Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Postinfarction ventricular septal defects (VSDs) are classified as occurring in three locations—apical, anterior, and posteroinferior ( Fig. 8.1 ). Most common is an anterior or apical defect caused by anterior septal myocardial infarction after occlusion of the left anterior descending coronary artery. In about one-third of patients, the rupture occurs in the posterior septum after an inferior septal infarction. The inferior septal infarction is usually due to occlusion of a dominant right coronary or, less frequently, of a dominant circumflex artery. An apical septal defect can be considered a variant of an anterior defect, but it presents the opportunity for a modified, and less involved, surgical technique.
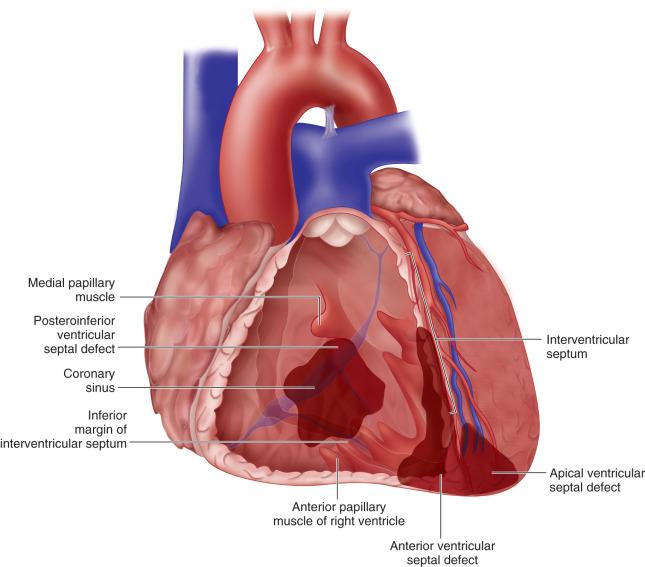
Associated with the septal defect is a variable amount of adjacent myocardial damage, both septal and free wall. In addition, the posterior papillary muscle is often involved in a posterior postinfarction septal defect. When the free wall infarction involves the papillary muscle, special techniques must be used to anchor the repair, or a mitral valve replacement should be undertaken.
Without surgery, 50% of patients with a postinfarction VSD will die within 24 hours, and 80% will die within 4 weeks. Therefore, the presence of this defect is considered an urgent indication for operation. The goal of preoperative management is to reduce the left-to-right shunt by reducing both the systemic vascular resistance and left ventricular pressure.
In addition, efforts are made to maintain cardiac output and arterial pressure to aid in end-organ perfusion. Placement of an intraaortic balloon pump is greatly beneficial and should be done as soon as the diagnosis is made. Patients in severe failure who are deemed hopeless candidates for immediate operation can be managed with an intraaortic balloon pump or with mechanical circulatory support in an attempt to delay surgery.
The use of a ventricular assist devices and extracorporeal membrane oxygenation (ECMO) with staged repair of the postinfarct VSD has been described. Left ventricular assist devices may result in a greater degree of right-to-left shunting; therefore, biventricular assist devices are preferred. ECMO may allow for support and resuscitation of critically ill patients in cardiogenic shock. ECMO can be instituted using central or peripheral cannulation. The type of cannulation should be determined on a case by case basis. Mechanical circulatory support for a short amount of time can be used to reverse end-organ damage. In addition, it can provide some time for infarct maturation, allowing for firmer tissue at the time of surgical repair.
In select patients, percutaneous closure is possible. The primary limitation is the friable condition of the surrounding septal muscle and proximity to the mitral valve or papillary muscles. Given reports of frequent early failure, this approach may best be used as an interim measure before surgery. The approach is more likely to be successful in delayed presentations or as treatment for recurrent defects that may occur between a repair patch and adjacent noninfarcted myocardium. The advent of the Amplatzer Muscular VSD Occluder (St. Jude Medical, St. Paul, MN) has shown potential for being an effective percutaneous treatment for extremely high-risk patients with postinfarct VSD.
Controversy exists over the role of preoperative coronary angiography and concomitant bypass surgery. Those who argue against preoperative catheterization have noted that there is no survival benefit and that it is a time-consuming procedure. In addition, because all patients present with a completed full-thickness infarction, revascularization of the infarcted territory is of limited value. A selective approach is appropriate, with catheterization performed in the subset of patients who are not in shock or severe failure before surgery, because some patients may benefit from revascularization to noninfarcted territories in which flow-limiting coronary lesions exist.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here