Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The term multidirectional instability (MDI) was first described by Neer and Foster in their preliminary report in 1980, when they reported the results of open inferior capsular shift as a treatment for this condition. A few years later, they defined MDI as symptomatic subluxations or dislocations of the glenohumeral joint in three directions. On the basis of these studies, they concluded that patients with MDI had symptomatic laxity in anterior, posterior, and inferior directions. In 1998 Matsen et al. proposed the acronym AMBRI (Atraumatic, Multidirectional, Bilateral, good response to Rehabilitation, and sometimes requiring Inferior capsular shift) to describe this kind of instability. Although many years have passed, there is still confusion as to the definition of MDI. At present, Neer’s definition is most quoted, but other symptoms such as pathological capsular laxity, unidirectional instability with multidirectional laxity, or atraumatic laxity of anterior capsule and glenohumeral ligaments are also used to describe MDI , . Furthermore, many have traditionally equated laxity, a physical finding, with instability, a pathological condition, and thus comparative studies using strict definitions are lacking.
This lack of clarity also applies to shoulder instability classification. Even today, we do not have a generally accepted and approved system for assessing shoulder instability, thus complicating the classification of MDI. A number of new shoulder instability classification systems have been published, and typically MDI is considered to be one instability variant. , , However, there is still discrepancy in the use of the term “multidirectional” among the authors. In the United States, the International Classification of Diseases 9th Edition is considered to be the most frequently used system of instability classification, but its accuracy is still being questioned.
The etiology and pathomechanism of MDI are still being studied and are not clearly defined. Most reports accept the presumption that this condition is multifactorial. , , In the most recent reports, connective tissue intrinsic pathophysiology is believed to play the primary role in the development of MDI. Bony anomalies are also reported as being contributory, but their contributions are less clearly defined. Some studies have reported changes in the glenoid shape and its version, , and others have reported the presence of chondrolabral lesions in patients with posteroinferior instability. , The redundancy of capsule, mainly inferiorly, is considered to be the principal pathology for MDI. Finally, dynamic stabilizers, including the rotator cuff and periscapular musculature in patients with MDI, have been reported to have aberrant firing patterns, producing atypical scapular kinematics and periscapular muscle aberrancies , that can be observed in electromyographic studies.
The diagnostic workup for MDI can be very challenging. It is critical that one differentiates MDI from multidirectional laxity of the shoulder (MDL), which is also characterized by an excessive glenohumeral translation, but, unlike MDI, is asymptomatic. Chief complaints and clinical findings may differ widely among patients with MDI. Therefore the patient’s history and a very thorough clinical examination are essential for proper diagnosis and decision making. The most commonly reported problems are nonspecific pain during everyday activities and a feeling of muscle strength reduction. Patients may also complain of subluxation or dislocation incidents, but MDI more commonly presents itself as pain during shoulder function. Furthermore, most patients are unable to identify one particular traumatic event, as the onset is usually insidious and worsens with prolonged activity.
Joint laxity is a competitive advantage in many sports such as swimming and throwing events, but with prolonged use, the dynamic stabilizers of the shoulder can fatigue, moving an asymptomatic athlete with laxity to a symptomatic pathological laxity, leading to a diagnosis of MDI. , In athletes with MDL, care must be taken to ensure the dynamic stabilizers of the shoulder stay strong, to minimize this crossover from laxity to instability. Another key point in the diagnosis of MDI is to identify whether the instability is voluntary or not. The voluntary element of glenohumeral instability is rare, but the surgical treatment of these patients has a higher rate of failure, especially if they suffer from coexisting mental illness. , It is important that a distinction be made between voluntary instability that is “positional,” meaning patients can demonstrate the instability by moving their scapula and shoulder, from instability that is “volitional,” where the patient demonstrates this as a “party trick.” The former can often be corrected, whereas the latter is very difficult to treat surgically. The hallmark of MDI has traditionally been a symptomatic sulcus sign ( Fig. 28.1 ). This is a physical sign on examination which is significant for laxity, and if it reproduces the patient’s symptoms, it is consistent with instability.
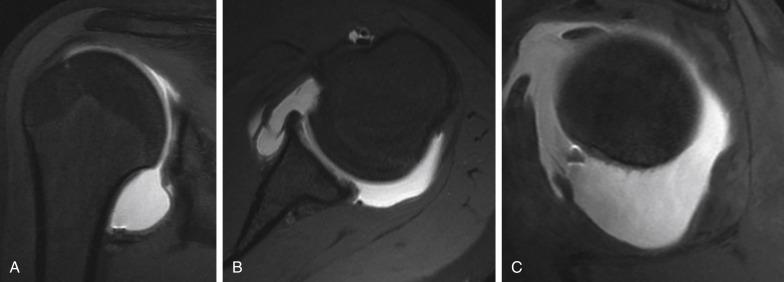
Imaging can be a very helpful tool in recognizing some of the critical findings in MDI. Radiographs, the most frequently used tool, should be taken in three views (anteroposterior Grashey view, scapular Y, axillary) and may be helpful in revealing bony lesions, or glenoid morphological changes such as hypoplasia. To identify soft tissue alterations like capsular redundancy or labral lesions, magnetic resonance imaging or, if possible, magnetic resonance arthrography (MRA), is recommended. MRA allows a more accurate assessment of the extended capsule, glenohumeral joint volume, and glenohumeral ligaments by filling the joint with intraarticular contrast ( Fig. 28.2A‒C ). However, it is crucial to note that radiology findings are not specific for MDI and may be present in other conditions.
Preoperative treatment complications can be defined as unsuccessful treatment outcomes based on incorrect diagnoses and a flawed decision-making process. One of the most typical mistakes is overlooking accompanying disorders. In the case of MDI, the most frequently misdiagnosed cases are conditions that may give a clinical presentation similar to MDI.
Generalized joint laxity, described as an increased range of joint motions, is a condition that should be given great attention owing to its high rate of coexistence with MDI. Moreover, differentiation between normal laxity and instability may be a great challenge, particularly because numerous patients with MDI have a symptomless contralateral shoulder, regardless of similar grade of laxity. It has been reported that 40% to 70% of MDI patients have generalized joint laxity. , In these patients, overstretched glenohumeral ligaments and joint capsule may predispose MDI development. Several methods have been described to diagnose generalized ligamentous laxity, although no single system of classification has emerged as the gold standard.
One of the most commonly used scales is the Beighton scale ( Table 28.1 ), which typically examines passive hyperextension of the metacarpophalangeal joint, thumb opposition to the forearm, and active elbow hyperextension and knee hyperextension. , Generalized laxity is said to be a main factor for worse results, including recurrent instability, in patients with traumatic onset of instability( Fig. 28.3 ).
| Characteristic | Score |
|---|---|
| Passive dorsiflexion of the little finger beyond 90 degrees | 1 point for each hand |
| Passive apposition of the thumb to the ipsilateral forearm | 1 point for each hand |
| Active hyperextension of the elbow beyond 10 degrees | 1 point for each hand |
| Active hyperextension of the knee beyond 10 degrees | 1 point for each hand |
| Forward flexion of the trunk with extended knees so that the palms of the hands rest flat on the floor | 1 point |
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here