Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Nerves are at risk of injury from:
Blunt force directed at the knee
Stretch/traction injury of the knee joint
Inversion sprain to the ankle
Open or arthroscopic knee surgery
Approach: knee pain that exists after musculoskeletal treatment is of neural origin.
Decide whether pain is coming from direct damage to the cutaneous nerves about the knee or from an injury to one of the nerves arising within the knee joint structures themselves.
Partial joint denervation is an approach in which the joint afferents that transmit a pain message are interrupted.
Nerves related to the knee include not only those that go in the skin about the surface of the knee joint but also mixed (motor and sensory) nerves that pass the knee on the way to their targets distal to this joint. In addition to these well-known nerves are those that innervate the knee joint. Each is at risk of injury when there is (1) blunt force directed at the knee, (2) a stretch/traction injury to the musculoskeletal system of the knee joint, or (3) an inversion sprain to the ankle or when (4) open or arthroscopic knee surgery has been performed. Although it is intuitively clear that a joint is innervated, the exact pathways of this innervation are curiously omitted from the classic and even the newer anatomy texts. For the human knee, the innervation pattern was not found to be described until 1994, during my search for an etiology of knee pain unrelated to musculoskeletal dysfunction. The approach to knee pain described in this chapter closely follows the approach developed for wrist pain, which preceded my interest in knee pain. This led to a subsequent similar approach to shoulder pain and ankle pain.
The approach described in this chapter considers knee pain that exists after musculoskeletal treatment to be of neural origin. The physician caring for these patients must consider whether the pain is coming from direct damage to the cutaneous nerves about the knee, such as a neuroma of the infrapatellar branch of the saphenous nerve, or from an injury to one of the nerves arising within the knee joint structures themselves. A further source of knee pain caused by nerve injury is an injury to a nerve far away from the knee, such as the lateral femoral cutaneous nerve, or a nerve that is simply going past the knee on its way to some other distal target. The concept of partial joint denervation is presented as an approach in which those joint afferents that transmit a pain message are interrupted, thereby stopping the pain and preserving the musculoskeletal components of the joint. A Charcot-type joint is not created because the deafferentation is partial instead of total.
Innervation of human knee joint
Innervation of proximal tibiofibular joint
Common peroneal nerve
Deep peroneal nerve
Superficial peroneal nerve
Proximal tibial nerve
Lateral femoral cutaneous nerve
Saphenous nerve
The innervation of the human knee joint is remarkably constant. On the medial aspect ( Fig. 39-1 ), the femoral nerve branch that innervates the vastus medialis continues past its motor point and exits deep and distal to the muscle. At this point, it lies deep within the medial retinaculum and becomes related to the medial recurrent geniculate artery and vein. This structure is termed the medial retinacular nerve . Both nerve and vessels continue directly adjacent to the vastus medialis and superficial to the synovium to enter the ligamentous structures of the medial aspect of the knee. These fibers also continue toward the midline of the knee to innervate the undersurface of the patella (see Fig. 39-1 ).
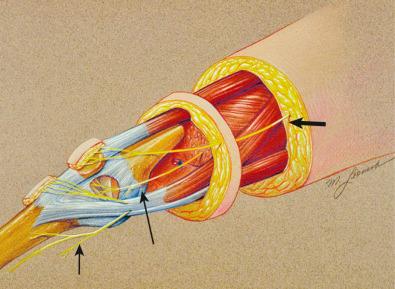
On the lateral aspect of the knee ( Fig. 39-2 ), a branch of the sciatic nerve leaves the popliteal fossa, travels laterally and anteriorly, emerges deep within the biceps tendon and enters the space beneath the lateral retinaculum. In this location, the nerve is adjacent to the superior lateral geniculate artery and vein. This structure is termed the lateral retinacular nerve . Both structures, the nerve and vessels, are immediately distal to the vastus lateralis and superficial to the synovium. The nerve enters the ligamentous structures of the lateral aspect of the knee (which have not yet been further defined histologically) and travels to the midline to innervate the undersurface of the patella.
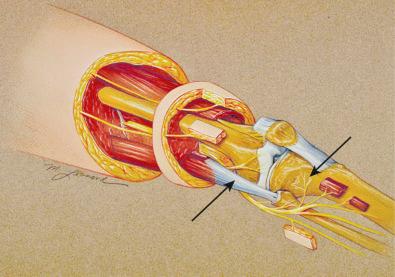
Anteriorly, another source of innervation is derived from the femoral nerve innervation of the vastus intermedius. This nerve continues on the surface of the periosteum to innervate the tissues around the prepatellar bursa. Finally, posteriorly, branches from the sciatic nerve enter the posterior knee joint capsule to provide innervation (see Fig. 39-2 ).
Although many patients complain of “knee pain,” they may be pointing or referring to the region distal and lateral to the knee, which is the articulation between the fibular head and the tibia. This joint space is likely to be injured from fractures of the fibula or lateral tibial plateau or from high tibial osteotomy or a Maquet operative procedure. It is innervated by the common peroneal nerve (see Fig. 39-2 ). As the common peroneal nerve travels from the popliteal fossa to the fibular head, it gives off a small (~1 mm in diameter) nerve that may enter the space posterior to the fibular head. The common peroneal nerve gives off a second innervating branch immediately as it curves anterior to the fibular head at the junction with the fibular neck. This branch is also approximately 1 mm in diameter. The next branch of the common peroneal nerve goes to the tibialis anterior, which is a critical motor branch. In the operating room, the only way to identify the branch to the joint is to stimulate it electrically. No motor function will be elicited when the branch is stimulated. This is a critical step. This small branch often looks like epineurium.
The common peroneal nerve is the lateral branch of the sciatic nerve. It can most often be identified as a distinct branch even to the sciatic notch. Therefore, in the thigh, there is clearly a common peroneal nerve even though it may be referred to as the sciatic nerve. In the distal thigh, the common peroneal nerve courses laterally, approaches the fibular head, and continues anteriorly to cross the fibular neck and enter the leg. As the common peroneal nerve approaches the fibular neck, it clearly divides into the superficial and the deep peroneal nerve, increasing in size as increased epineurium is required to ensheath these two branches ( Fig. 39-3 ). The critical anatomic sites that can cause compression have long been appreciated to occur where the common peroneal nerve crosses the fibular neck, requiring division of the fascia of the peroneus longus fascia. With increasing experience, it has become evident that three other anatomic factors must be considered. A fibrous band exists beneath the peroneus longus in 20% of cadavers, but this band is present (and ranges from 5 to 15 mm in width) in 80% of patients requiring neurolysis. The surgeon must identify the common peroneal nerve by elevating it from the fibular neck; determine whether or not fibrous thickening in the lateral gastrocnemius muscle fascia is present; and finally, be certain that the overall entrance into the anterior and lateral compartments is sufficiently large.
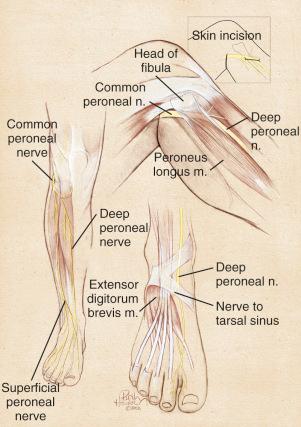
The deep peroneal nerve arises over the fibular neck as a discrete fascicle. It can be dissected proximally by microtechnique if necessary. Immediately after crossing the fibular neck, it gives off tiny branches to the tibialis anterior and the toe extensor muscles. In so doing, the deep peroneal nerve effectively tethers the common peroneal and its distal branches from having too much excursion. This predisposes the common peroneal nerve and its branches to stretch/traction injuries. The entrapment site for the deep peroneal nerve is at the ankle, the “anterior tarsal tunnel,” which is a rare site for compression unless there has been a direct injury at this location. A more common site for compression is over the dorsum of the foot where the tendon of the extensor hallucis brevis represents the anatomic structure causing the compression. A portion of the tendon of the extensor hallucis brevis is excised in the region of the deep peroneal nerve (see Fig. 39-3 ).
The superficial peroneal nerve arises over the fibular neck from the common peroneal nerve. It can be dissected proximally by microdissection if required. The motor innervation to the foot everters arises within the first 1 to 2 cm distal to the neck of the fibula. The known site of entrapment for this nerve is the region where it transitions from deep fascia into the subcutaneous tissues in the distal third of the leg. The typical division into its dorsomedial and dorsolateral branches occurs just proximal to the ankle in approximately 75% of patients (see Fig. 39-3 ). In my experience, it is now clear that in at least 25% of cadavers and patients coming to surgery, this division can occur in the proximal third of the leg. This creates the situation in which the superficial peroneal nerve may be found in both the anterior and its most usually described location, the lateral compartment. Indeed, the superficial peroneal nerve may be present in just the anterior compartment or within the septum between the two compartments. The anatomic variability means that any surgical approach to this nerve must open both the anterior and the lateral compartments.
Although the tibial nerve (like the common peroneal nerve) arises at the sciatic notch as the medial component of the sciatic nerve and is often clearly a distinct nerve in the thigh, the only well-described site for tibial nerve compression was at the medial ankle in the tarsal tunnel. It is now evident that the tibial nerve can be compressed in a site more proximal than the tarsal tunnel, and this site (just distal to the knee) is best described as the proximal tibial nerve, to distinguish it from the tarsal tunnel region. Tibial nerve compression in the popliteal fossa has been described related to the presence of compartment syndrome or space-occupying masses, such as a popliteal artery or a Baker cyst. Although anatomy texts clearly depict a fibrous arch or soleal sling from which the soleus muscle arises, only recently has there been an anatomic study describing the relationship of this sling to the proximal tibial nerve (unpublished data). This sling lies at a mean distance of 9.3 cm (range, 7-13 cm) from the middle of the popliteal fossa and causes a visible narrowing of the tibial nerve over a length of 1.5 cm in 55% of the cadavers, with a severe constriction being found in 2% of the specimens. With injury to the knee, especially one associated with postoperative bleeding into the popliteal fossa, tibial nerve compression at this proximal site must be considered as a source of symptoms of numbness in the plantar aspect of the foot, with proximal referral to the knee region.
The lateral femoral cutaneous nerve has a great deal of anatomic variability related both to its location at the anterior superior iliac crest and to its innervated skin territory. If the location is within the inguinal ligament instead of inferior to it, the lateral femoral cutaneous nerve is at risk for compression or stretch/traction injury during falls, while wearing tight belts, during a seatbelt injury, or during manipulation of the knee with the patient on the operating room table. From Figure 39-4 , it can be noted that compression of the lateral femoral cutaneous nerve can produce symptoms that include numbness or pain about the lateral aspect of the knee. This nerve, or the femoral nerve itself, can be injured during regional anesthesia given for knee surgery.
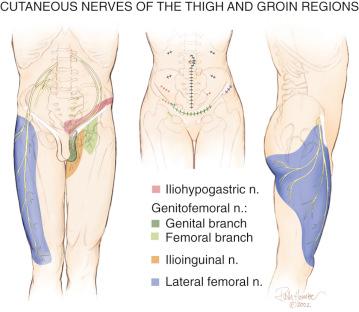
The saphenous nerve is a branch that arises from the femoral nerve in the proximal thigh. Its cutaneous branches to the skin below the knee are well described and lie in a position to be injured directly from either a medial ankle arthroscopy portal or the midline incisions used for many surgical approaches to the knee. These branches can be directly injured by blunt trauma as well. Less well recognized is the nerve to the skin overlying the patellar itself. This is a branch of the femoral nerve, which may include sensory contribution from the obturator nerve joining within Hunter's canal. The medial cutaneous nerve of the thigh (see Fig. 39-1 ) approaches from the medial aspect of the knee compared with the vertical approach taken by the anterior femoral cutaneous nerves. Even less well appreciated is that the saphenous nerve can be compressed in the distal thigh within Hunter's canal. This is called adductor canal syndrome , which is rare in the absence of direct trauma to the region. Entrapment of the saphenous nerve in this location can present as medial knee pain.
History is critical.
Determine whether pain is made worse by certain positions of the body or leg or by certain activities.
If pain persists beyond a reasonable timeframe of 3 to 6 months, diagnosis is most consistent with pain of neural origin.
Distinguish whether any skin territories are dysesthetic; observe for trigger spot.
Joint afferents: palpate medial and lateral retinacular nerves. To determine whether knee pain is because of an injury to one or both of the joint afferents, conduct diagnostic nerve block. Determine whether effective.
If block is not effective, look for more rare sources of nerve pain: anterior femoral cutaneous nerve, another branch of the infrapatellar saphenous nerve, Tinel's sign over lateral femoral cutaneous nerve, or motor function of the common peroneal nerve.
It is critical to obtain the history of knee pain. Knee pain does not arise de novo but because of a history of some type of sports event, overuse activity, new activity, or actual direct injury to the knee. The knee injury may be blunt or open. Surgery should also be considered as a source of trauma. Many patients with knee pain caused by musculoskeletal problems awake from their reconstructive knee surgery to have a different pain or paralysis. These are known complications of knee surgery that should be recognized as such and referred for appropriate treatment in a timely manner. The determination of whether or not the pain is made worse by certain positions of the body or leg or by certain activities is important for a correct diagnosis. Certainly, most knee pain unrelated to structural impairment will be relieved by nonoperative treatment. But when pain persists beyond a reasonable timeframe of 3 to 6 months, the diagnosis is most consistent with pain of neural origin.
The physical examination is directed at identifying one or more sources of neural origin of the pain. First, the clinician should try to distinguish whether any skin territories are dysesthetic or painful when touched lightly. If so, these areas should be outlined. The most common distribution is that of the infrapatellar branch of the saphenous nerve; the second most common is the skin over the patella itself. These areas might be numb, indicating loss of sensation ( Fig. 39-5 ). Once the pattern is identified, examine proximally along the course of the given nerve, observing for a trigger spot, which is either a true end-bulb neuroma or an in-continuity nerve lesion. The hypothesis is made that this nerve or these nerves are the source of the cutaneous pain; a diagnostic nerve block will be required to confirm this hypothesis.
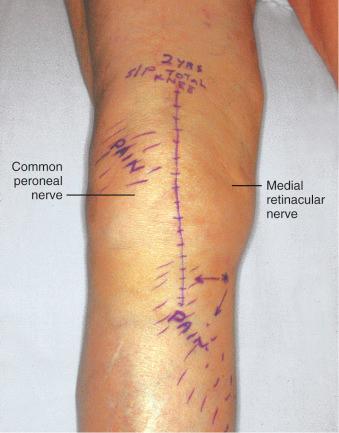
The physical examination is then directed to the joint afferents. Palpation is done deeply on the spot located just distal to the vastus medialis muscle, through the medial retinaculum to elicit pain from the medial retinacular nerve. Next, palpation is repeated on the area located just distal to the vastus lateralis muscle, through the lateral retinaculum, to elicit pain from the lateral retinacular nerve ( Fig. 39-5 ). The hypothesis is made that the knee joint pain is caused by an injury to one or both of the joint afferents; a diagnostic nerve block will be required to confirm this hypothesis. The medial cutaneous nerve to the thigh and the medial retinacular nerve can be blocked at the same area. Ten minutes after the nerve blocks, the patient is instructed to walk in the hallway, climb and descend a few steps, and even kneel on a padded chair ( Fig. 39-6 ). A reduction of 5 points on a visual analog scale, for example, from 10 to 5, where 10 represents the worst pain, is confirmation that sufficient relief of pain has occurred to permit surgery for partial knee denervation and resection of cutaneous neuromas.
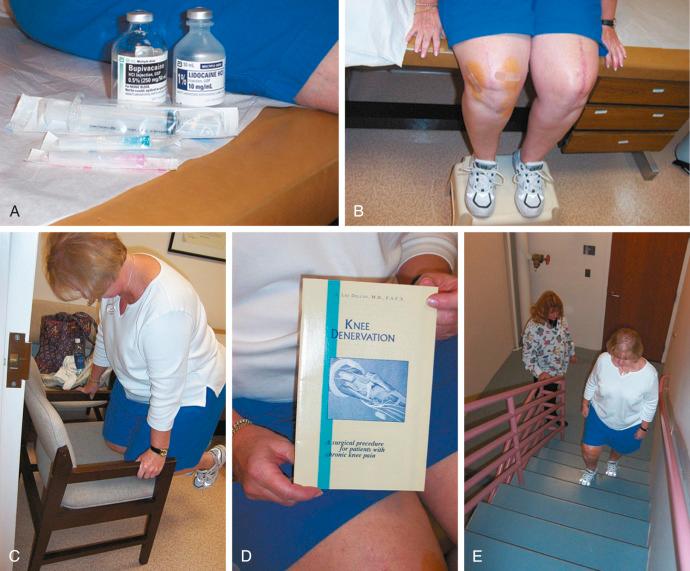
If the nerve blocks just described have not reduced the pain level to less than 5 points or the blocks were not effective, the physical examination should proceed to include other more rare sources for the nerve pain. In a patient with a knee replacement, the remaining pain may stem from an anterior femoral cutaneous nerve found in the proximal portions of the incision or another branch of the infrapatellar saphenous nerve, which can have many branches, including more distal branches.
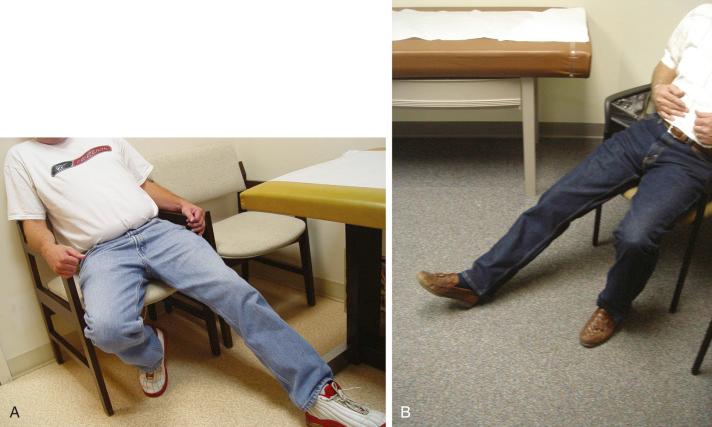
Finally, the groin should be examined to search for Tinel's sign over the lateral femoral cutaneous nerve. The patient will be noted to sit with the lower extremity extended at the hip joint ( Fig. 39-7 ). The midthigh should be examined to search for Tinel's sign over Hunter's adductor canal. This is most effectively done with the patient supine and the affected leg externally rotated at the hip, leaving the knee bent. This stretches the adductor muscle group over the saphenous nerve. Then gentle palpation over the canal produces a distal radiating painful response ( Fig. 39-8 ).
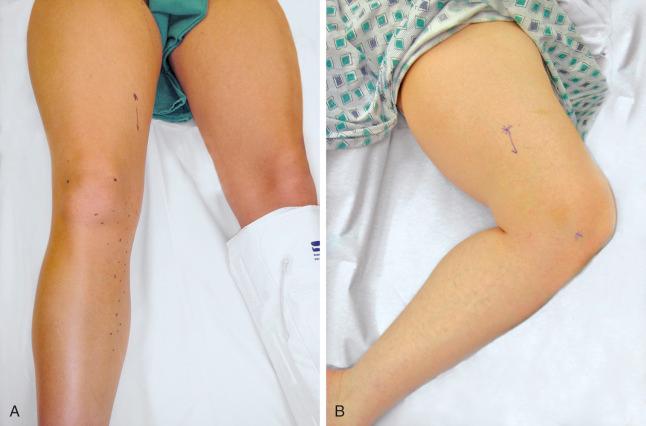
If the pain is below the knee joint and located laterally, examine for tenderness in the proximal tibiofibular joint space. If this is present, a nerve block can be done directly into this space without blocking the common peroneal nerve.
If pain is accompanied by complaints of the leg “giving out,” the foot dragging, or a “footdrop,” the motor function of the common peroneal nerve must be evaluated by manual muscle testing. The common peroneal nerve must be palpated or percussed at the fibular neck, with tenderness (even without distal radiation) considered a positive sign for nerve entrapment.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here