Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The brachial plexus is the name given to the plexus of nerves formed by the lower four ventral cervical roots (C5-C8) and the first thoracic ventral root (T1) as they emerge from the spinal cord, intermingle, realign, and emerge from the plexus as defined distal nerves. C4 and T2 may contribute axons to the plexus with little effect on the clinical location of the lesion. The brachial plexus is responsible for the motility and sensitivity in the upper extremities.
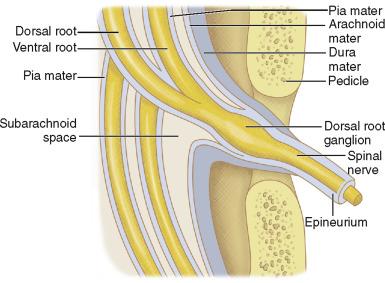
At each spinal level, the ventral and dorsal rootlets emerge from the spinal cord and unite distal to the dorsal ganglia to form the root proper. This root then divides into dorsal and ventral portions designated the dorsal and ventral roots of each level. The dorsal portions of the lower cervical roots do not contribute to the brachial plexus; they pass dorsally to innervate the skin and muscles of the neck and upper back. The ventral roots form the brachial plexus. First, the ventral roots realign into three trunks. The ventral root of C5 joins the ventral root of C6 to form the upper trunk. The ventral root of C7 remains alone and forms the middle trunk. The ventral root of C8 joins the ventral root of T1 to form the lower trunk. Each trunk then splits into an anterior and a posterior division, which reunite to form three cords (posterior, lateral, and medial) that finally end as the branches (peripheral nerves) ( Fig. 26-1 ).
The ventral cervical roots descend toward the first rib, whereas the ventral T1 root ascends over the first rib to form the brachial plexus. The brachial plexus emerges between the anterior and middle scalene muscles (the interscalenic triangle), where sympathetic fibers controlling vasoconstriction and sweat gland activity join the nerve roots. The sympathetic contributions to C5 and C6 arise from the inferior cervical ganglion. The sympathetic contributions to C7, C8, and T1 arise from the stellate ganglion. T1 nerve roots also contribute parasympathetic fibers to the ganglion, which, when injured, cause Horner syndrome ( Fig. 26-2 ).
MRI is the most widely accepted imaging modality used to evaluate the brachial plexus. Sequences that are usually employed include the following:
T1-weighted (T1W) imaging is used to evaluate the regional anatomy and fatty post-traumatic denervation changes of the muscle.
T2-weighted (T2W) imaging with fat suppression can highlight the pathologic signal changes within the nerves. Fat suppression sequences such as short tau inversion recovery (STIR) or frequency-selective fat saturation are necessary so that abnormal signal is not obscured by adjacent fat. STIR offers a consistent and uniform suppression of fat signal with excellent T2 contrast but has a low signal-to-noise ratio (SNR), greater sensitivity to blood flow artifacts, and no T1 tissue contrast images. Frequency-selective fat saturation methods have a higher SNR (resulting in better image quality), have fewer blood-flow–related artifacts, and can generate T1W images. The greatest disadvantage of frequency-selective fat saturation is the variable completeness of fat suppression across the field of view and consequent signal inhomogeneity.
Constructive interference in steady-state (CISS)/fast imaging employing steady-state acquisition (FIESTA) show pools of cerebrospinal fluid (CSF) associated with nerve root avulsions and small schwannomas.
Contrast-enhanced T1W imaging is done with a standard dose of 0.1 mmol/kg of gadolinium-based contrast material to display neoplasms, radiation injury, inflammation/abscess, or other enhancing disease processes. Contrast enhancement is not indicated in trauma, although acute denervated muscles enhance. Contrast-enhanced studies must be performed with frequency-selective fat saturation to better visualize enhancing structures.
The study is performed to maximize information from the symptomatic side and obtain basic information from the normal side for comparison.
Imaging planes and methods include the following:
Symptomatic side
T1, T2, CISS/FIESTA true or oblique coronal
T1 true or oblique sagittal
T1 and T2 axial
T1 images repeated after gadolinium administration with fat suppression
Asymptomatic side (to enable comparison with normal structures)
T1 and T2 true or oblique coronal
CT cannot visualize the brachial plexus directly, but it is helpful for evaluating neighboring structures to detect post-traumatic clavicle fractures, cervical ribs, lung masses, and so on.
CT myelography may be helpful when nerve root avulsion is suspected. It has greater sensitivity and specificity than a simple myelogram but is less sensitive than MRI for identification of pseudomeningoceles.
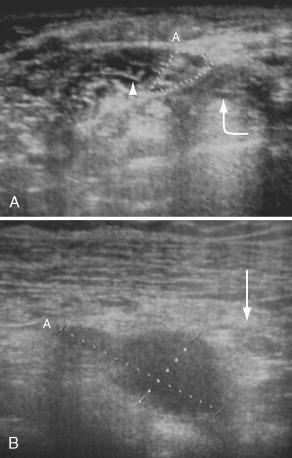
Ultrasonography is highly useful for guiding placement of local anesthesia and evaluating the echo texture of a mass before biopsy (e.g., subclavian aneurysm vs. nerve sheath tumor vs. adenopathy) ( Fig. 26-3 ).
Indications for the different techniques are as follows:
Trauma: radiography, MRI, and CT myelography
Tumor: MRI and CT
Thoracic outlet syndrome: radiography, MRI, CT, and angiography
Plexitis and suspected inflammatory processes: MRI
The components of the brachial plexus normally have intermediate signal intensity, similar to muscle in both T1W and T2W images. Distal to the dorsal root ganglia there is no normal enhancement. All of the portions of the brachial plexus (roots, trunks, divisions, cord, and branches) are uniform in size (within groups) and are separated by fat. The roots are located in the neural foramina, the trunks within the fat of the interscalene triangle (between the anterior and middle scalene muscles), and the divisions behind (posterior to) the clavicle. The lateral and medial cords lie anterior to the subclavian artery, whereas the posterior cord lies dorsal to the artery. Their branches wrap around the axillary artery.
Artifacts may be associated with this technique:
Inhomogeneity of fat saturation in frequency-selective fat saturation images may lead to varying signal intensities in the brachial plexus, simulating edema.
The “magic angle” effect in STIR images results in an isolated hyperintensity of portions of the plexus. It results from T2 anisotropy attributed to densely packed and hydrated collagen and from the fact that the brachial plexus is oriented at 55 degrees to the main B° magnetic field (the magic angle).
Flow artifacts arise from the artery or aneurysms.
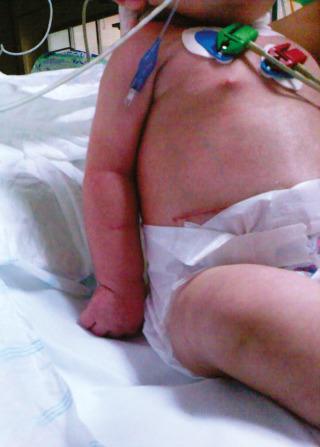
Obstetric trauma to the brachial plexus occurs in 0.4 to 2.5 per 1000 live births. Plexus injuries are mainly associated with shoulder dystocias, which are the most frequent cause of obstetric brachial plexus palsies. There are two major presentations of obstetric trauma to the brachial plexus: an upper root injury at C5-C6 (Erb's palsy), which is more frequent, and an isolated lower root injury at C8-T1 (Dejerine-Klumpke palsy). The typical posture of Erb's palsy consists of shoulder adduction and internal rotation, elbow extension, forearm pronation, wrist flexion, and finger flexion ( Fig. 26-4 ). Extended Erb's palsy includes C7, leading to additional paralysis of elbow and finger extension. Klumpke's palsy should be suspected if Horner syndrome is present. Because limited external rotation may also be due to a concomitant shoulder dislocation and the humeral head of a newborn is neither ossified nor visible on radiographs, ultrasonography or MRI may be required to rule out this differential possibility.
Stab wounds or gunshot wounds can transect portions of the brachial plexus directly or produce vascular injuries with expanding hematomas or pseudoaneuryms that compress the nerves secondarily ( Fig. 26-5 ). In these conditions, brachial plexus imaging is necessary to sort out which lesions are present, which specific therapies they require, and their prognoses.

Traction injuries are the most common cause of brachial plexus injury in young adults, with most of them resulting from motorcycle accidents in males. Some call these injuries “burners or stingers” when they are due to minor stretch traumas common in contact sports such as football. Clinically, they cause a burning pain and paresthesias that radiate from the supraclavicular area into the arm with transient weakness and sensory abnormalities. They usually resolve spontaneously over a few minutes and do not require imaging. If there is incomplete recovery or restricted neck motion, diagnostic imaging is required to rule out a cervical spine injury or other important pathology.
All traumatic lesions of the brachial plexus may be classified as postganglionic or preganglionic. The prognosis and treatment planning are different for the two types, so it is essential to differentiate between them.
Postganglionic injuries are treated surgically to reestablish local nerve continuity and afford a better prognosis. Preganglionic avulsions are usually irreparable and require alternative techniques to restore function or to at least decrease the patient's pain (nerve transfer and more recent reimplantation or graft insertion).
Preganglionic lesions may be root stretches or partial/complete root avulsions. The most common pattern of injury (69% of partial avulsions) is partial avulsion of a ventral rootlet with an intact dorsal rootlet. If the motor rootlet is avulsed, the motor cell body in the spinal cord is separated from its axons. The axons then undergo wallerian degeneration. If the dorsal rootlet is avulsed, the sensory cell bodies in the dorsal root ganglia remain connected to their axons, so sensory fibers are spared from wallerian degeneration. In these cases, therefore, electrodiagnostic studies reveal abnormal motor findings with intact sensory conduction. Avulsion occurs more frequently at the C8-T1 rootlets. These rootlets lack fibrous attachments to the transverse processes, so they are prone to avulsions.
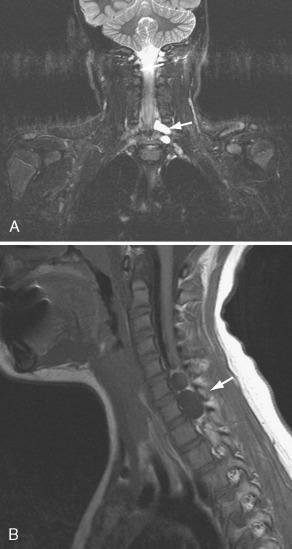
MRI and CT myelography may both help to identify fluid-filled pseudomeningoceles. Traumatic tears of the meningeal sleeves of brachial plexus rootlets permit CSF to leak into the soft tissue, forming fluid pouches termed pseudomeningoceles . Pseudomeningoceles are almost pathognomonic preganglionic rootlet avulsions ( Fig. 26-6 ). MRI demonstrates pseudomeningoceles better than CT, simple myelography, or even CT-myelography, because swelling and early granulation tissues may block free communication between the intraspinal CSF and the pseudomeningoceles. In this situation, no contrast agent fills the pouch, so the pouch will not be demonstrated. However, MRI demonstrates even noncommunicating fluid collections in the paraspinal soft tissue and often shows an alignment of their long axes that defines the specific rootlets affected. The T2 signal intensity of pseudomeningoceles is characteristically higher than normal CSF, owing to absent CSF pulsations or higher protein/blood content ( Fig. 26-7 ). Complications associated with pseudomeningoceles include spinal cord herniation and displacement ( Fig. 26-8 ), hematoma formation, and even superficial siderosis. Twenty percent of patients with root avulsions show abnormal signal intensity within the spinal cord. Areas of T2 hyperintensity suggest edema in the acute phase and myelomalacia in the chronic phase. T2 hypointensity suggests hemorrhage in the acute phase and siderosis from repeated hemorrhages in the chronic phase. Enhancement of intradural nerve rootlets and paraspinal muscles suggests functional impairment.

In postganglionic injuries, the stretching or tearing of the nerves may separate them from the cell bodies of the motor and sensory neurons, leading to wallerian degeneration.
For surgical purposes, postganglionic lesions can be classified by their relationships to the clavicle. Supraclavicular lesions involve the roots and trunks of the brachial plexus. Seventy-five percent of these are Erb-Duchenne (extended upper brachial plexus) palsies, Dejerine-Klumpke (lower brachial plexus) palsies, or complete palsies. Retroclavicular lesions predominantly affect the divisions of the brachial plexus. They are relatively rare and generally result from clavicular fracture (acute period) or prominent callus formation (chronic period). Infraclavicular lesions predominantly affect the cords and branches. The axillary nerve is particularly susceptible to traction injury as it traverses the quadrangular space because this tight space anchors or fixes it in position.
Tumors are an important cause of brachial plexopathies, particularly in older individuals. They cause sensory deficits with patchy and incomplete distribution more frequently than motor symptoms (which tend to be related to trauma). Tumors may be primary or secondary (typically metastases). Primary neurogenic tumors are rare but usually treatable. They consist of neurofibromas (most frequent), schwannomas, malignant peripheral nerve sheath tumors, and post-traumatic neuromas.
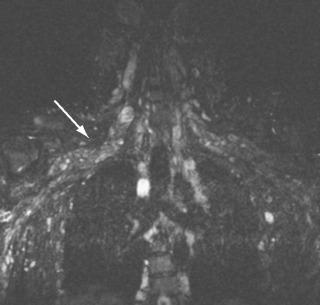
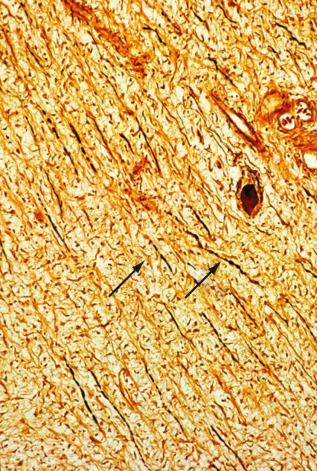
One third of patients with neurofibromas have localized or plexiform neurofibromas, associated with neurofibromatosis type 1. In these patients the nerves of the brachial plexus show diffuse and gross enlargement resembling a “bag of worms” ( Fig. 26-9 ). Sporadic neurofibromas are typically solitary and more commonly found in the supraclavicular region. They are more often seen in females than males (3 : 1). Histologically, these lesions are unencapsulated tumors that appear to arise from the nerve fascicles. The tumor cells penetrated into the nerve deeply and diffusely ( Fig. 26-10 ). Complete resection is not possible and results in neurologic deficits.
The second most common neural tumors of the brachial plexus are encapsulated eccentric nerve sheath masses that arise from Schwann cells. Schwannomas are slightly more common in the upper brachial plexus and tend to displace the nerve fascicles instead of invading them. Therefore, surgical excision is often complete and is not associated with a high level of neurologic deficits. Multiple schwannomas suggest the diagnosis of neurofibromatosis type 2. When they are malignant (very rare) they may also be associated with neurofibromatosis type 1.
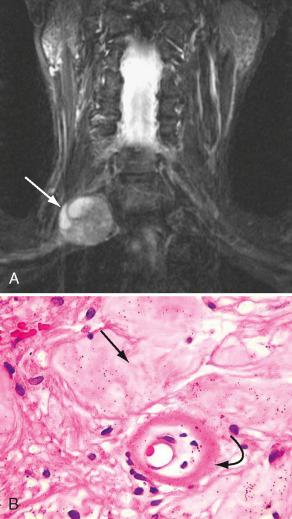
The imaging features of neurofibromas and schwannomas may be very similar, so they may be very difficult to differentiate successfully. Plain radiographs show foraminal enlargement and well-defined bony remodeling. Ultrasonography demonstrates well-defined oval hypoechoic masses with posterior acoustic enhancement. Absence of a central echogenic hilum differentiates these lesions from cervical lymph nodes (see Fig. 26-3B ). On CT, neurofibromas and schwannomas both have attenuations similar to muscle and both enhance variably after administration of a contrast agent. On MRI, both appear isointense to muscle on T1W imaging, have a characteristic high signal on T2W imaging, and enhance intensely after gadolinium is given intravenously. Neurofibromas often show a central area of low signal intensity within the area of high T2 signal, giving the appearance of a “target” sign. On histology, the “target sign” is created by a central core of nonenhancing collagenous and fibrillary tissue and a peripheral, less densely cellular, enhancing myxoid tissue ( Fig. 26-11 ). Cystic and necrotic regions exhibit high T2 signal but do not enhance after contrast agent administration.
Malignant nerve tumors are less common than neurofibromas and schwannomas and mostly consist of fibrosarcomas and neurogenic sarcomas. They are more frequent in patients with neurofibromatosis type 1, especially after radiation therapy. Their imaging features are similar to their benign counterparts, which makes it difficult to differentiate between them. The diagnosis of a malignant nerve sheath tumor is suggested by a progressively enlarging mass in a patient with neurofibromatosis, concurrent bone destruction, poorly defined margins with infiltration into neighboring soft tissues, heterogeneous contrast enhancement, and a lack of the “target sign.” Although diffusion-weighted MRI and fluorodeoxyglucose-labeled positron emission tomography (FDG-PET) have been used with some success for diagnosing malignant change in plexiform neurofibromas, a biopsy should always be performed whenever the question of a malignancy is considered.
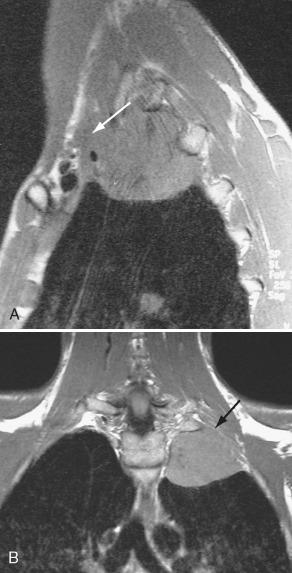
The main primary tumors that affect the brachial plexus are lymphoma, lung apex carcinoma, and skeletal soft tissue tumors, especially desmoid tumors and lipomas ( Fig. 26-12 ). Head and neck tumors may also extend to involve the brachial plexus. Primary cancers arising from the apex of the lung may invade into the brachial plexus and other para-apical structures to cause Pancoast syndrome. This syndrome consists of pain around the shoulder and arm (the most common initial symptom) produced by neoplastic involvement of C8 and T1-T2 nerve roots. Horner syndrome is seen in 20% of patients and muscle atrophy of the hand and rib destruction are also common. MRI displays these tumors and their relationship to the brachial plexus well ( Fig. 26-13 ). Tumor invasion of the brachial plexus may preclude surgery.

Secondary tumors involve the brachial plexus more often than primary nerve tumors do. The most common lesions to metastasize to the region of the brachial plexus are breast carcinoma (from axillary drainage of metastases), lung carcinoma, and head and neck tumors. True hematogenous metastases are rare.
MRI evaluation of tumors affecting the brachial plexus must define two important factors: (1) does the tumor lie adjacent to the brachial plexus or actually invade it; and (2) are the findings observed the result of prior therapy, particularly surgery and radiation therapy, or are they due to residual or recurrent tumor?
The most reliable signs to differentiate tumor from radiation fibrosis are the presence of a soft tissue mass and clinical and imaging evidence of a progressive abnormality. Clinical features suggestive of radiation-induced brachial plexopathy are little or no pain, lymphedema, cutaneous radiation changes, and known radiation doses of more than 60 Gy. Imaging features suggestive of radiation-induced brachial plexopathy include upper trunk involvement (from its longer course through the radiation field and lesser protection by thinner layers of soft tissue within the occipital triangle), thickening of the brachial plexus and stranding of the neighboring fat within the irradiated field, and low signal intensity on both T1W and T2W images. However, radiation therapy can also cause high T2 signal intensity (edema) in the brachial plexus and enhancement after gadolinium administration.
Thoracic outlet syndrome refers to clinical manifestations attributable to impingement on the brachial plexus and the subclavian vessels as they pass from the thoracic cavity to the axilla. Congenital bony or fibromuscular anomalies, trauma, and posture may contribute to the compression or elongation of the neurovascular bundle. Movements such as raising the arms above the head may further compromise the thoracic outlet. Symptoms are variable and nonspecific. Whereas nearly all patients with thoracic outlet syndrome have compression of the brachial plexus, only a minority have symptoms or sequelae due to arterial or venous impingement.
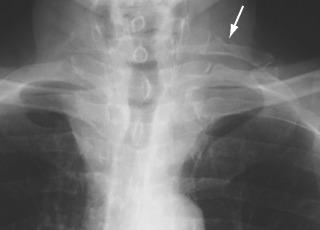
One frequent cause of brachial plexus compression in thoracic outlet syndrome is a cervical rib (or hypertrophied C7 transverse process), sometimes with an associated fibrous band. Cervical ribs are present in 6% of the normal population and in 13% of patients with thoracic outlet syndrome ( Fig. 26-14 ). The rib or transverse process can be diagnosed with plain radiographs. MRI better displays the fibrous bands that attach to the first rib and narrow the thoracic outlet. MRI also helps to display hypertrophied musculature, such as the scalene muscles, which may also cause thoracic outlet syndrome. Hyperabduction of the ipsilateral upper extremity accentuates the degree of compression on the neurovascular structures. Therefore, it can be important to image the thoracic outlet during hyperabduction of the ipsilateral extremity to detect subtle cases and define the severity of the rest. The hyperabduction maneuver can by employed during conventional angiography, CT, CT angiography, MRI, and MR angiography. Ultrasonography and Doppler sonography may also be helpful, particularly when venous obstruction is suspected. Positive electrophysiologic nerve conduction studies are useful in selecting patients for surgical decompression of neurogenic thoracic outlet syndrome. Resection of the first rib—the standard surgical treatment for thoracic outlet syndrome—usually fails to improve long-term function in neurogenic thoracic outlet syndrome but helps patients with vascular thoracic outlet syndrome.
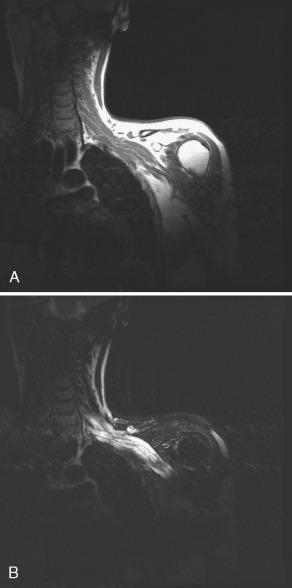
Hypertrophic polyneuropathies may result in a grossly enlarged brachial plexus with expansion of the intervertebral foramina and scalloping of the vertebral bodies. The hypertrophic polyneuropathies are a heterogeneous group of diseases that include the hereditary motor-sensory neuropathies (HMSN type I or Charcot-Marie-Tooth, HMSN II, and HMSN III or Dejerine-Sotas), amyloidosis, leprosy, sarcoidosis, chronic inflammatory demyelinating polyradiculoneuropathy, and acromegaly. The clinical presentation, CSF analysis, nerve conduction studies, sural nerve biopsies, and genetic studies are needed to make an exact diagnosis because the imaging features of these disorders overlap and may even be confused with neurofibromatosis. MRI reveals abnormal thickening and enhancement of all components of the brachial plexus. Their signal intensity may remain normal on T1W imaging ( Fig. 26-15A ) but slightly hyperintense on T2W imaging (see Fig. 26-15B ).
Sudden, unexplained brachial plexus plexopathy may be called neuralgic amyotrophy, Parsonage-Turner syndrome, brachial neuritis, or brachial plexitis. Patients usually experience sudden onset of severe, constant pain in the lateral neck, shoulder, and upper arm, followed by a profound weakness and atrophy of the painful muscles. The serratus anterior is most frequently affected. The condition may (1) be idiopathic, (2) be the result of a primary viral infection, especially in older individuals, (3) be a complication of prior infection (herpes) or serum vaccine, antibiotic, or other drug administration, or (4) have a heredofamilial prevalence. Symptoms usually resolve, partially or completely, but recovery may not begin until 6 months after the onset of symptoms and may require up to 3 years. The MRI findings are frequently normal, but MRI may also show diffusely enlarged brachial plexus nerves with increased T2 signal ( Fig. 26-16 ). Newer MRI techniques such as MR neurography are particularly useful for confirming the diagnosis of this entity, which has previously been a diagnosis of exclusion.

Sample reports are presented in Boxes 26-1 to 26-3 . See also Box 26-4 for pitfalls and limitations of the brachial plexus imaging and Figures 26-17 to 26-19 for examples.
A young male adult involved in a motorcycle accident presented with upper arm and shoulder palsy and pain.
Bilateral noncontrast T1W spin-echo axial MR study ( Fig. 26-17A ) was done with a large field of view. Axial (see Fig. 26-17B ) and left parasagittal (see Fig. 26-17C ) T2W spin-echo MR studies were also obtained.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here