Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
In the previous chapter, an orderly approach to the diagnosis of inflammatory skin lesions was discussed. This chapter records in list form some useful points that may assist in reaching a correct diagnosis. Many of the clues that follow produce diagnostic lists that are not necessarily related to tissue reaction, etiology, or pathogenesis.
Some of the clues that follow are original observations; many have been around for decades. An acknowledgment should be made here of the work of A. Bernard Ackerman, who has contributed more “clues” to diagnostic dermatopathology than anyone else.
Like all “shortcuts,” the following “clues” must be used with caution. They are not absolute criteria for diagnosis, and they are not invariably present at all stages of a disease. An attempt has been made to group the clues into several sections.
Dilated vessels in the upper dermis
Stellate fibroblasts/dendrocytes
Deep elastotic fibers
Deep extension of the infiltrate
Epidermal “sunburn” cells
Note: The duration of the process and the underlying nature of the light reaction will influence the response. Only one or two features may be present; for example, sunburn cells (apoptotic keratinocytes) are confined to phototoxic and photosensitive drug eruptions.

Acute, severe : Pale pink epidermis, sometimes with loss of cell borders; pinpoint erosions or larger ulcers; fibrin below the epidermis
Chronic, persistent : Psoriasiform epidermal hyperplasia; vertical streaks of collagen in the papillary dermis; stellate fibroblasts/dendrocytes; fibroplasia of varying amounts; enlarged follicular infundibula (as prurigo nodularis commences); compact orthokeratosis
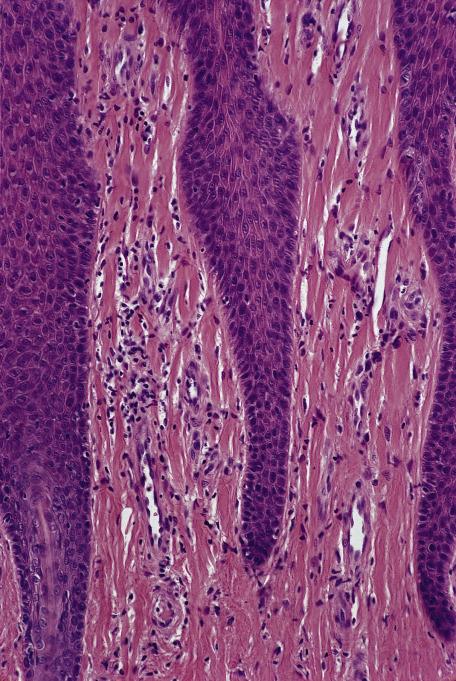
Superficial dermal edema
Activated lymphocytes
Eosinophils and/or plasma cells
Red cell extravasation
Endothelial swelling of vessels
Exocytosis of lymphocytes
Apoptotic keratinocytes.
The changes present will mirror the clinical types of reaction. In morbilliform reactions, lymphocytes extend into the lower epidermis and the apoptotic keratinocytes are in the basal layer.
Small blue coiled/clumped fibers (pseudoxanthoma elasticum)
Wavy epidermis (particularly in children)
Elastophagocytosis
Dispersed neutrophils (early cutis laxa)
Unusually thickened collagen (connective tissue nevus).
Confluent parakeratosis
Superficial epidermal necrosis and/or pallor
Mild psoriasiform hyperplasia
Hemorrhage (in pellagra and mixed deficiencies).
Basically, these features should prompt the performance of a periodic acid–Schiff (PAS) stain. Many simulants exist.
Compact orthokeratosis with no other explanation
Layering of epidermal cornification (“sandwich sign”)
Neutrophils in the epidermis/stratum corneum
Spongiosis, particularly palmoplantar
Suppurative folliculitis.

These signs refer to a likely folliculitis at deeper levels of the biopsy.
Neutrophils on top of the stratum corneum
Neutrophils at the edge of the tissue section
Uneven vasculitis (centered in one small area)—miliaria may do the same
Focal splaying of neutrophils and dust in mid dermis.
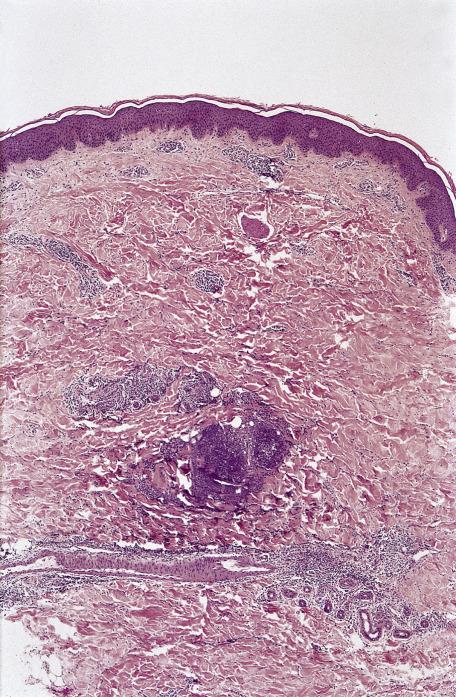
Last week's sign refers to a dermatosis, no longer active, that is “playing itself out.” It was presumably more active some days earlier.
Parakeratosis overlying basket-weave orthokeratin (the key feature)
Mild hyperplasia of the epidermis
Mild dermal inflammation.
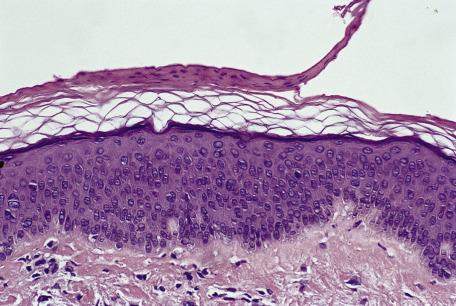
Lagging history refers to several conditions in which the clinical appearances may be striking in comparison to the histology.
Sclerodermoid graft-versus-host disease (GVHD) may have “rock-hard skin” but only subtle collagen deposition.
Cicatricial alopecia can be similar.
Urticaria: Histology underestimates the edema because of dehydration during tissue processing.
Prurigo nodularis: There may be clinical nodules but no histological swollen infundibula, only psoriasiform hyperplasia of lichen simplex chronicus.
Pauci-cellular photodermatoses: There may be striking clinical changes but only telangiectasia and sparse inflammatory cells on histology.
The presence of a superficial and deep inflammatory cell infiltrate within the dermis should trigger the mnemonic “8Ls + DRUGS.”
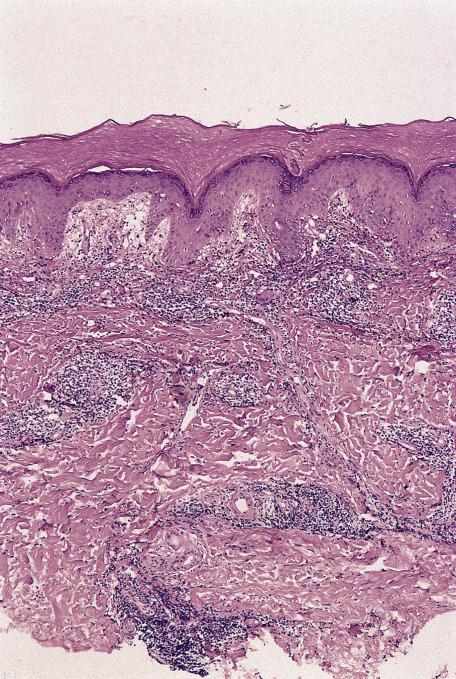
Light reactions
Lymphoma
Leprosy
Lues
Lichen striatus
Lupus erythematosus
Lipoidica (necrobiosis)
Lepidoptera (and other arthropods)
Dermatophyte
Reticular erythematous mucinosis
Urticarial stages (bullous pemphigoid)
Gyrate erythemas
Scleroderma (localized)
And, of course, drug reactions
Busy refers to a dermis that appears focally hypercellular on scanning magnification and is not usually due to the usual inflammatory infiltrates.
Incomplete form of granuloma annulare
Interstitial granulomatous dermatitis
Interstitial granulomatous drug reaction
Resolving vasculitis (increased mucin also)
Chronic photodermatoses
Folliculitis—at deeper levels (cells are neutrophils and dust)
Subtle breast carcinoma recurrence
Desmoplastic melanoma (also perivascular lymphocytes)
Kaposi's sarcoma (early stage)
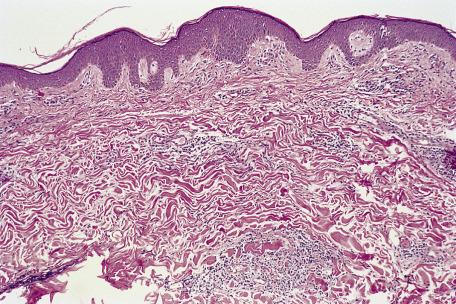
Staphylococcal scalded skin syndrome
Pemphigus foliaceus
Peeling skin syndrome
Psoriatic erythroderma (psoriasiform hyperplasia present)
Artifacts
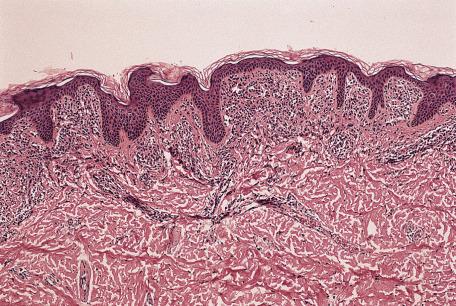
The low power impression is that of a variably hypercellular papillary dermis. Excluded from consideration are nodular and diffuse infiltrates also involving the reticular dermis. The “LUMP” mnemonic covers most cases: l ichenoid, u rticaria pigmentosa, m ycosis fungoides, p igmented purpuric dermatoses. Expressed differently they are as follows:
Most of the lichenoid tissue reactions
Pigmented purpuric dermatoses
Cutaneous T-cell lymphoma
Parapsoriasis (if not included earlier)
Some mastocytomas
Early lichen sclerosus et atrophicus.
Dermatitis herpetiformis
Linear immunoglobulin A (IgA) disease
Cicatricial pemphigoid
Localized cicatricial pemphigoid
Bullous lupus erythematosus
Epidermolysis bullosa acquisita
Drugs
Hypersensitivity vasculitis (rare)
Rheumatoid neutrophilic dermatosis
Pemphigoid gestationis (eosinophils)
Deep lamina lucida pemphigoid
Generalized exanthematous pustulosis (rare)
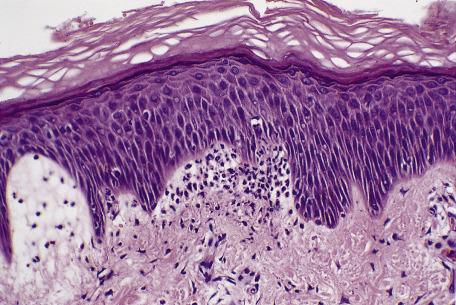
In some conditions, neutrophils are relatively sparse or less conspicuous than in vasculitis, a neutrophilic dermatosis, or cellulitis.
Erythema marginatum
Still's disease
Neutrophilic urticaria
Mild periodic fever syndromes
Early or subsiding neutrophilic dermatoses
Neutrophilic erythemas of infancy
Some flea bites
Lupus erythematosus
Dermatomyositis (less so)
Lichen sclerosus et atrophicus
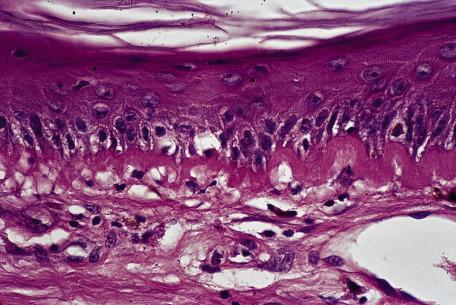
Cutaneous lupus erythematosus
Reticular erythematous mucinosis (REM)
Jessner's lymphocytic infiltrate
Other signs will usually allow these diagnoses, but sometimes REM will present with very little deep infiltrate. Biopsies appear to have a “mid-dermal plexus.” Dermatomyositis can have mucin, but the infiltrate is only superficial. Perifollicular mucin can be seen in Carney's complex. REM and Jessner's infiltrate (no longer used) are both patterns of expression of cutaneous lupus erythematosus.
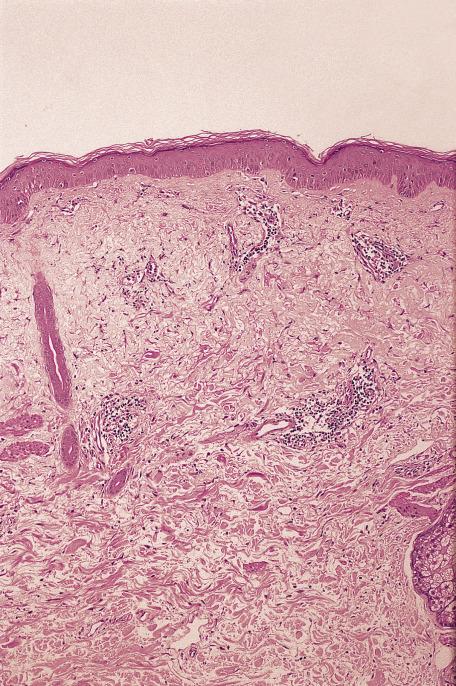
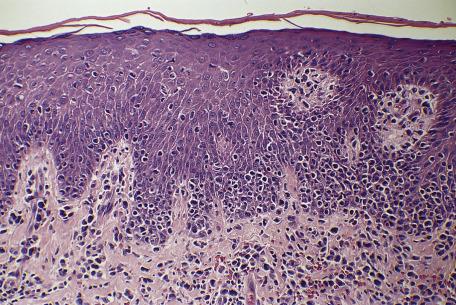
The terms epidermotropism and exocytosis are often used interchangeably. It is best to restrict them as follows:
Exocytosis : Random emigration of inflammatory cells through the epidermis; some cells will reach the surface. It is common in inflammatory dermatoses. In the spongiotic tissue reaction, it may be a striking feature in nummular dermatitis and spongiotic drug reactions.
Epidermotropism : Refers to directed emigration of lymphocytes; it usually involves only the lower one-third to half of the epidermis. The cells tend to aggregate. There is little, if any, accompanying spongiosis. It is a feature of mycosis fungoides.
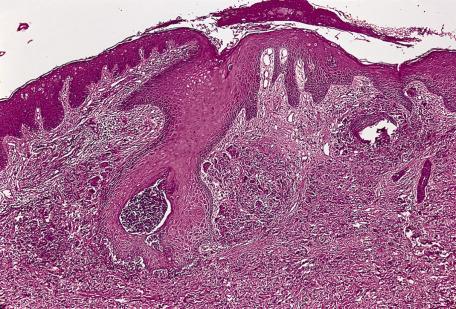
The epidermal/follicular “vacuum cleaner” is the author's term for the irregular epidermal hyperplasia ± enlarged follicular infundibula, associated with the transepidermal elimination of material from the dermis. It can be subtle after cryotherapy to sun-damaged skin; it may be the cause of a persistent lesion at the site, often mistaken as a clinical recurrence.
Lipping : See later
Spongiosis : Pityriasis rosea, erythema annulare centrifugum, seborrheic dermatitis, other spongiotic diseases
Neutrophils : Psoriasis (neutrophils in “summits” of mounds), seborrheic dermatitis, dermatophyte infection, necrolytic erythema, secondary bacterial infection
In tiers : Porokeratosis, verruca vulgaris, palmoplantar psoriasis
With interface change : Lichenoid drug, lichen planus–like keratosis, pityriasis lichenoides, lupus erythematosus (more often orthokeratosis)
Overlying orthokeratosis : Healing lesion or intermittent activity, particularly a spongiotic process
Alternating : Alternating orthokeratosis and parakeratosis in a horizontal direction is seen in ILVEN, and actinic keratosis, and in a horizontal and vertical direction in pityriasis rubra pilaris
Broad thick zones : Psoriasis, glucagonoma and deficiency states (epidermal pallor is not invariable), pityriasis lichenoides, granular parakeratosis.
Seborrheic dermatitis
Pityriasis rubra pilaris (follicular lesions)
Spongiotic processes, or psoriasis, on the face. The large number of follicles on the face means that they are more likely to be involved incidentally in any condition with parakeratosis.
Large atypical lymphoid cells within a heavy mixed infiltrate occur in lymphomatoid papulosis. The cells have been likened to “chunks of coal.”
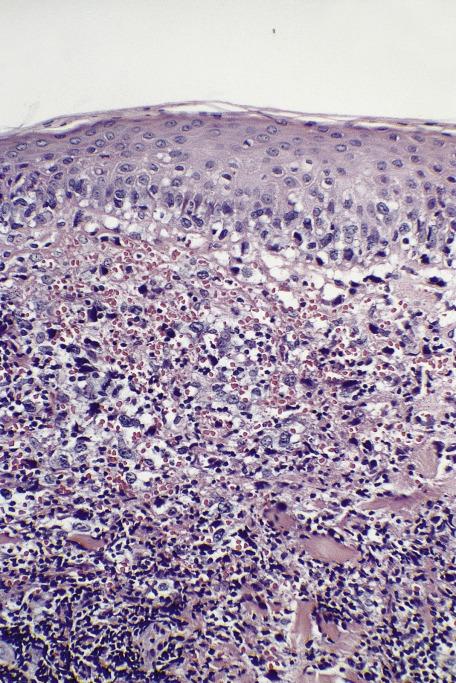
Interstitial eosinophils refers to the presence of eosinophils between collagen bundles and away from vessels. Perivascular eosinophils are also present.
Arthropod bites
Cnidarian contact
Other parasite infestations
Drug reactions
Toxic erythema of pregnancy
Annular erythemas of infancy
Wells’ syndrome
Dermal hypersensitivity
Hypereosinophilic syndrome
Urticaria
Urticarial stages of bullous pemphigoid, pemphigoid gestationis
Internal malignancy (rare)
Large numbers of eosinophils in suspected bite reactions suggest scabies or a hypersensitive state to the arthropod. Prebullous pemphigoid also has numerous eosinophils.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here