Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Cardiac denervation is an unavoidable consequence of heart transplantation, and reinnervation is at best partial and incomplete.
Drugs acting directly on the heart are the drugs of choice for altering cardiac physiology after heart transplantation.
Allograft coronary vasculopathy remains the greatest threat to long-term survival after heart transplantation.
Broadening of donor criteria has decreased time to lung transplantation.
Air trapping in patients with severe obstructive lung disease may impair hemodynamics and require deliberate hypoventilation.
Newly transplanted lungs should be ventilated with a low tidal volume and inspiratory pressure and as low an inspired oxygen concentration as can be tolerated.
Reperfusion injury is the most common cause of perioperative death.
The frequency of heart-lung transplantation has decreased as the frequency of lung transplantations has increased.
The history of heart transplantation spans almost a century. Canine heterotopic cardiac transplantation was first reported in 1905, but such efforts were doomed by ignorance of the workings of the immune system ( Box 19.1 ). Further research in the late 1950s and early 1960s set the stage for the first human cardiac transplant by Barnard in 1966. However, there were few long-term survivors in this era because of continued deficiency in understanding and modulating the human immune system, and the procedure fell into general disfavor. Continued research at selected centers (such as Stanford University) and lessons learned from renal transplantation led to greater understanding of the technical issues and immunology required, and by the early 1980s, cardiac transplantation gained widespread acceptance as a realistic option for patients with end-stage cardiomyopathy.
Frequency of transplantation remains limited by donor supply
Pathophysiology before transplantation is primarily that of end-stage ventricular failure
Pathophysiology after transplantation reflects the effects of denervation
Allograft coronary vasculopathy is a frequent long-term complication
Heart transplantation experienced explosive growth in the mid-to-late 1980s, but the annual number of heart transplants worldwide plateaued by the early 1990s at approximately 3500 per year. The factor limiting continued growth has been a shortage of suitable donors. As of February 2015, there were slig htly more than 4000 patients on the United Network for Organ Sharing (UNOS) cardiac transplant waiting list (includes all US candidates), an increase of 25% compared with 2004. During that same time period the frequency of heart transplantation also increased (by approximately 17%) but failed to keep pace with the increase in the size of the waiting list. Only 2431 heart transplants were performed in the United States during the 2014 calendar year, slightly above the average of 2290 heart transplants per year over the preceding decade. The median waiting time for a cardiac graft varies widely according to blood type (approximately 52 days for type AB recipients in contrast with 241 days for type O recipients listed for the period 2003–2004, based on Organ Procurement and Transplantation Network [OPTN] data as of February 1, 2015). Of those patients listed for heart transplantation in 2009, 27.5% had spent more than a year waiting for a transplant. Adult patients on the heart transplant waiting list are assigned a status of 1A, 1B, or 2. Status 1A patients require mechanical circulatory support, mechanical ventilation, high-dose or multiple inotropes, with continuous monitoring of left ventricular filling pressure. Status 1B patients require mechanical circulatory support beyond 30 days or inotropic support without continuous monitoring of left ventricular filling pressure. All other patients are classified as Status 2. The most frequent recipient indications for adult heart transplantation remain either idiopathic or ischemic cardiomyopathy. Other less common diagnoses include viral cardiomyopathy, systemic diseases such as amyloidosis, and complex congenital heart disease (CHD).
The 1-year survival rate after heart transplantation has been reported to be 79%, with a subsequent mortality rate of approximately 4%/year. There has been only slight improvement in the survival statistics over the past decade; the OPTN reports that the 1- and 3-year survival rates after heart transplantation for those transplanted in the United States during the period 1997 to 2004 were approximately 87% and 78%, respectively. One-year survival rate after repeat heart transplantation more than 6 months after the original procedure is slightly lower (63%) but substantially worse if performed within 6 months of the original grafting (39%). Risk factors for increased mortality have been associated with recipient factors (prior transplantation, poor human leukocyte antigen matching, ventilator dependence, age, and race), medical center factors (volume of heart transplants performed, ischemic time), and donor factors (race, sex, age), and have remained relatively unchanged over the past two decades. Early deaths most frequently are caused by graft failure, whereas intermediate-term deaths are caused by acute rejection or infection. Late deaths after heart transplantation most frequently are due to allograft vasculopathy, posttransplant lymphoproliferative disease or other malignancy, and chronic rejection.
Potential candidates for heart transplantation generally undergo a multidisciplinary evaluation, including a complete history and physical examination, routine hematology, chemistries (to assess renal and hepatic function), viral serology, electrocardiography, chest radiography, pulmonary function tests, and right- and left-heart catheterization. Ambulatory electrocardiography, echocardiography, and nuclear gated scans are performed if necessary. The goals of this evaluation are to confirm a diagnosis of end-stage heart disease that is not amenable to other therapies and that will likely lead to death within 1 to 2 years, as well as to exclude extracardiac organ dysfunction that could lead to death soon after heart transplantation. Patients typically have New York Heart Association (NYHA) class IV symptoms and a left ventricular ejection fraction less than 20%. Although most centers eschew a strict age cutoff, the candidate should have a physiologic age younger than 60. Detecting pulmonary hypertension and determining whether it is due to fixed elevation of pulmonary vascular resistance (PVR) is crucial; early mortality because of graft failure is threefold greater in patients with increased PVR (transpulmonary gradient >15 mm Hg or PVR >5 dynes•sec•cm −5 ). If increased PVR is detected, a larger donor heart, a heterotopic heart transplant, or a heart-lung transplant (HLT) may be more appropriate. Active infection and recent pulmonary thromboembolism with pulmonary infarction are additional contraindications to heart transplantation. The results of this extensive evaluation should be tabulated and available to the anesthesia team at all times because heart transplantation is an emergency procedure.
Once a brain-dead donor has been identified, the accepting transplant center must further evaluate the suitability of the allograft. Centers generally prefer donors to be free of previous cardiac illness and younger than 35 years because the incidence of coronary artery disease markedly increases at older ages. However, the relative shortage of suitable cardiac donors has forced many transplant centers to consider older donors without risk factors and symptoms of coronary artery disease. If it is necessary and the services are available at the donor hospital, the heart can be further evaluated by echocardiography (for regional wall motion abnormalities) or coronary angiography, to complement standard palpation of the coronaries in the operating room. The absence of sepsis, prolonged cardiac arrest, severe chest trauma, and a high inotrope requirement also are important. The donor is matched to the prospective recipient for ABO blood-type compatibility and size (within 20%, especially if the recipient has high PVR); a crossmatch is performed only if the recipient's preformed antibody screen is positive.
Donors can exhibit major hemodynamic and metabolic derangements that can adversely affect organ retrieval. Most brain-dead donors will be hemodynamically unstable. Reasons for such instability include hypovolemia (secondary to diuretics or diabetes insipidus), myocardial injury (possibly a result of catecholamine storm during periods of increased intracranial pressure), and inadequate sympathetic tone because of brainstem infarction. Donors often also have abnormalities of neuroendocrine function such as low T 3 and T 4 levels.
Donor cardiectomy is performed through a median sternotomy, usually simultaneously with recovery of other organs such as lungs, kidneys, and liver. Just before cardiac harvesting, the donor is heparinized and an intravenous cannula is placed in the ascending aorta for administration of conventional cardioplegia. The superior vena cava (SVC) is ligated and the inferior vena cava (IVC) transected to decompress the heart, simultaneous with the administration of cold hyperkalemic cardioplegia into the aortic root. The aorta is cross-clamped when the heart ceases to eject. The heart also is topically cooled with ice-cold saline. After arrest has been achieved, the pulmonary veins are severed, the SVC is transected, the ascending aorta is divided just proximal to the innominate artery, and the pulmonary artery (PA) is transected at its bifurcation. The heart is then prepared for transport by placing it in a sterile plastic bag that is placed, in turn, in another bag filled with ice-cold saline, all of which are carried in an ice chest. Of all the regimens tested, conventional cardioplegia has proved most effective in maintaining cardiac performance. The upper time limit for ex vivo storage of human hearts appears to be approximately 6 hours.
Orthotopic heart transplantation is carried out via a median sternotomy, and the general approach is similar to that used for coronary revascularization or valve replacement. Frequently, patients will have undergone a prior median sternotomy; repeat sternotomy is cautiously performed using an oscillating saw. The groin should be prepped and draped to provide a rapid route for cannulation for cardiopulmonary bypass (CPB) if necessary. After the pericardium is opened, the aorta is cannulated as distally as possible and the IVC and SVC are individually cannulated via the high right atrium. Manipulation of the heart before institution of CPB is limited if thrombus is detected in the heart with transesophageal echocardiography (TEE). After initiation of CPB and cross-clamping of the aorta, the heart is arrested and excised ( Fig. 19.1 ). The aorta and PA are separated and divided just above the level of their respective valves, and the atria are transected at their grooves. A variant of this classic approach totally excises both atria, mandating bicaval anastomoses. This technique may reduce the incidence of atrial arrhythmias, better preserve atrial function by avoiding tricuspid regurgitation, and enhance cardiac output (CO) after transplantation.
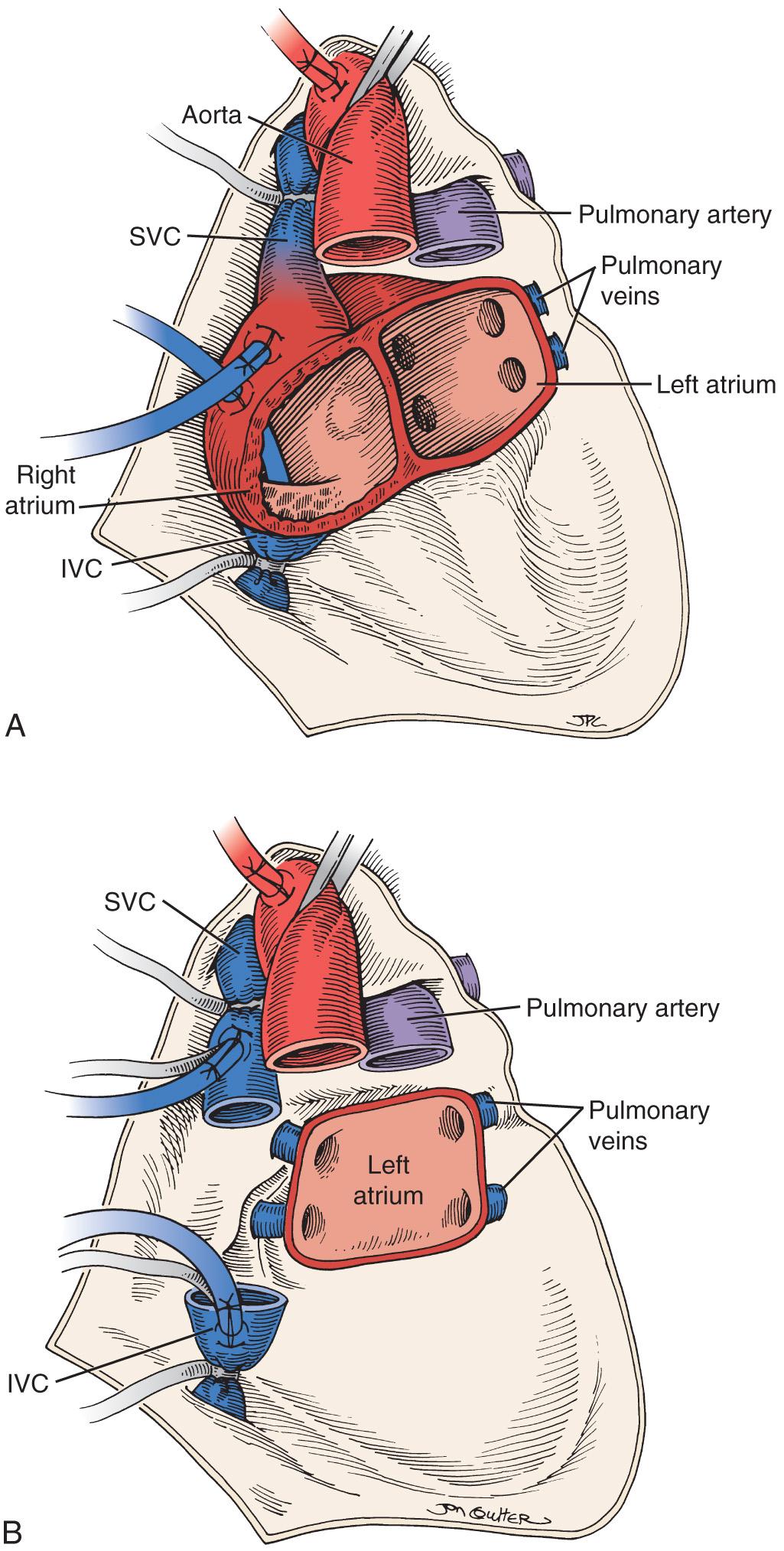
The donor graft then is implanted with every effort to maintain a cold tissue temperature, beginning with the left atrial (LA) anastomosis. If the foramen ovale is patent, it is sutured closed. The donor right atrium is opened by incising it from the IVC to the base of the right atrial (RA) appendage (to preserve the donor sinoatrial node), and the RA anastomosis is constructed. Alternatively, if the bicaval technique is used, individual IVC and SVC anastomoses are sewn. The donor and recipient PAs are then brought together in an end-to-end manner, followed by the anastomosis of the donor to the recipient aorta. After removal of the aortic cross-clamp, the heart is de-aired via a vent in the ascending aorta. Just before weaning from CPB, one of the venous cannulae is withdrawn into the right atrium and the other removed. The patient is then weaned from CPB in the usual manner. After hemostasis is achieved, mediastinal tubes are placed for drainage, the pericardium is left open, and the wound is closed in the standard fashion.
Although orthotopic placement of the cardiac graft is optimal for most patients, certain recipients are not candidates for the orthotopic operation, and instead the graft is placed in the right chest and connected to the circulation in parallel with the recipient heart. The two primary indications for heterotopic placement are significant irreversible pulmonary hypertension and gross size mismatch between the donor and recipient. Heterotopic placement may avoid the development of acute right ventricular (RV) failure in the unconditioned donor heart in the face of acutely increased RV afterload.
Donor harvesting for heterotopic placement is performed in the previously described manner, except that the azygos vein is ligated and divided to increase the length of the donor SVC; the PA is extensively dissected to provide the longest possible main and right PA; and the donor IVC and right pulmonary veins are oversewn, with the left pulmonary veins incised to create a single large orifice. The operation is performed via a median sternotomy in the recipient, but the right pleura is entered and excised. The recipient SVC is cannulated via the RA appendage, and the IVC via the lower right atrium. After arresting the recipient heart, the LA anastomosis is constructed by incising the recipient left atrium near the right superior pulmonary vein and extending this incision inferiorly and then anastomosing the respective left atria. The recipient RA-SVC is then incised and anastomosed to the donor RA-SVC, after which the donor aorta is joined to the recipient aorta in an end-to-side manner. Finally, the donor PA is anastomosed to the recipient main PA in an end-to-side manner if it is sufficiently long; otherwise, they are joined via an interposed vascular graft ( Fig. 19.2 ).
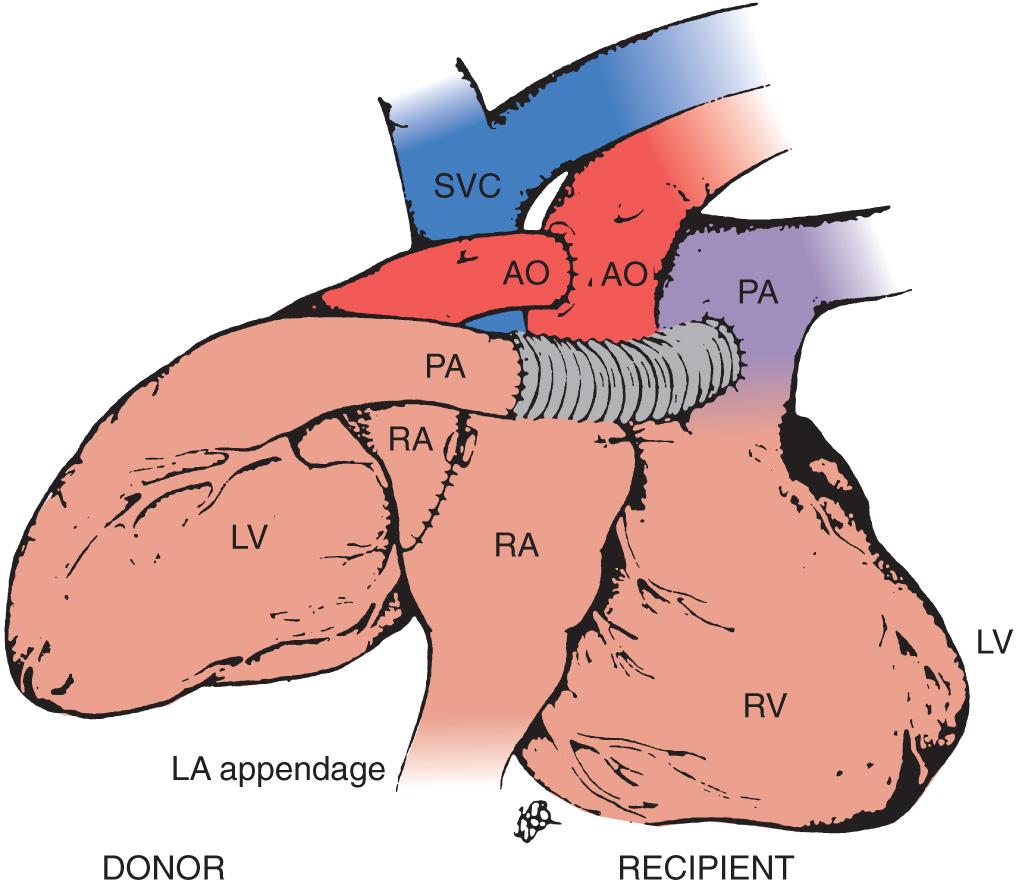
Mechanical ventricular assist devices have been used successfully to bridge patients who would otherwise die of acute heart failure awaiting transplantation. Although ventricular assist devices may improve the survival of patients awaiting transplantation, complications associated with their use may negatively impact survival after transplantation. The technique of transplantation is virtually identical in such patients to that for ordinary orthotopic transplantation. However, repeat sternotomy is obligatory, and repeat sternotomy is associated with higher morbidity and mortality, as well as higher intraoperative blood use, postoperative length of intensive care unit (ICU) and hospital stays, and frequency of reoperation for bleeding after subsequent heart transplantation.
Rarely, patients will present for cardiac transplantation combined with transplantation of the liver. The cardiac allograft usually is implanted first to better enable the patient to survive potential hemodynamic instability associated with reperfusion of the hepatic allograft. Large-bore intravenous access is mandatory. Conventional full heparinization protocols or low-dose heparin with heparin-bonded circuits may be used. A venous cannula can be left in the right atrium at the completion of the heart transplant procedure to serve as a return site for subsequent venovenous bypass during liver transplantation.
The pathophysiology of heart transplant candidates is predominantly end-stage cardiomyopathy. Normally, such patients will have both systolic dysfunction (characterized by decreased stroke volume and increased end-diastolic volume) and diastolic dysfunction, characterized by an increased intracardiac diastolic pressure. As compensatory mechanisms to maintain CO fail, the increased left ventricular (LV) pressures lead to increases in pulmonary venous pressures and development of pulmonary vascular congestion and edema. A similar process occurs if RV failure also occurs. Autonomic sympathetic tone is increased in patients with heart failure, leading to generalized vasoconstriction, as well as salt and water retention. Vasoconstriction and ventricular dilation combine to substantially increase myocardial wall tension. Over time, the high levels of catecholamines lead to a decrease in the sensitivity of the heart and vasculature to these agents via a decrease in receptor density (ie, downregulation) and a decrease in myocardial norepinephrine stores.
Therapy of heart failure seeks to reverse or antagonize these processes. Almost all candidates will be maintained on diuretics; hypokalemia and hypomagnesemia secondary to urinary losses are likely, and the anesthesiologist must be alert to the possibility that a patient is hypovolemic from excessive diuresis. Another mainstay of therapy is vasodilators (such as nitrates, hydralazine, and angiotensin-converting enzyme inhibitors), which decrease the impedance to LV emptying and improve cardiac function and survival in patients with end-stage heart failure. Paradoxically, slow incremental β-blockade with agents such as the β 1 -antagonist metoprolol also can improve hemodynamics and exercise tolerance in some patients awaiting heart transplantation. Patients who are symptomatic despite these measures often will require inotropic therapy. Digoxin is an effective but weak inotrope, and its use is limited by toxic side effects. Phosphodiesterase inhibitors such as amrinone, milrinone, and enoximone are efficacious, but chronic therapy is restricted by concerns about increased mortality in those receiving these agents. Therefore inotrope-dependent patients often are treated with intravenous infusions of β-adrenergic agonists such as dopamine or dobutamine. Patients refractory to even these measures may be supported with intraaortic balloon counterpulsation, but its use is fraught with significant vascular complications and essentially immobilizes the patient. Many patients with low CO are maintained on anticoagulants such as warfarin to prevent pulmonary or systemic embolization, especially if they have atrial fibrillation.
The physiology of patients after heart transplantation is of interest not only to anesthesiologists in cardiac transplant centers but to the anesthesiology community at large because a substantial portion of these patients return for subsequent surgical procedures.
Cardiac denervation is an unavoidable consequence of heart transplantation. Many long-term studies indicate that reinnervation is absent, or at best partial or incomplete, in humans. Denervation does not significantly change baseline cardiac function, but it does substantially alter the cardiac response to demands for increased CO. Normally, increases in heart rate can rapidly increase CO, but this mechanism is not available to the transplanted heart. Heart rate increases only gradually with exercise, and this effect is mediated by circulating catecholamines. Increases in CO in response to exercise are instead mostly mediated via an increase in stroke volume. Therefore maintenance of adequate preload in cardiac transplant recipients is crucial. Lack of parasympathetic innervation probably is responsible for the gradual decrease in heart rate after exercise seen in transplant recipients, rather than the usual sharp decline.
Denervation has important implications in the choice of pharmacologic agents used after cardiac transplantation. Drugs that act indirectly on the heart via either the sympathetic (ephedrine) or parasympathetic (atropine, pancuronium, edrophonium) nervous systems generally will be ineffective. Drugs with a mixture of direct and indirect effects will exhibit only their direct effects (leading to the absence of the normal increase in refractory period of the atrioventricular node with digoxin, tachycardia with norepinephrine infusion, and bradycardia with neostigmine). Thus agents with direct cardiac effects (such as epinephrine or isoproterenol) are the drugs of choice for altering cardiac physiology after transplantation. However, the chronically high catecholamine levels found in cardiac transplant recipients may blunt the effect of α-adrenergic agents, as opposed to normal responses to β-adrenergic agents.
Allograft coronary vasculopathy remains the greatest threat to long-term survival after heart transplantation. Allografts are prone to the accelerated development of an unusual form of coronary atherosclerosis that is characterized by circumferential, diffuse involvement of entire coronary arterial segments, as opposed to the conventional form of coronary atherosclerosis with focal plaques often found in eccentric positions in proximal coronary arteries. The pathophysiologic basis of this process remains elusive, but it is likely due to an immune cell-mediated activation of vascular endothelial cells to upregulate the production of smooth muscle cell growth factors. More than half of all heart transplant recipients have evidence of concentric atherosclerosis 3 years after transplant, and more than 80% at 5 years. Because afferent cardiac reinnervation is rare, a substantial portion of recipients with accelerated vasculopathy will have silent ischemia. Noninvasive methods of detecting coronary atherosclerosis are insensitive for detecting allograft vasculopathy. Furthermore, coronary angiography often underestimates the severity of allograft atherosclerosis; other diagnostic regimens such as intravascular ultrasound and dobutamine stress echocardiography may detect morphologic abnormalities or functional ischemia, respectively, in the absence of angiographically significant lesions. Therefore the anesthesiologist should assume that there is a substantial risk for coronary vasculopathy in any heart transplant recipient beyond the first 2 years, regardless of symptoms, the results of noninvasive testing, and even angiography.
The preoperative period often is marked by severe time constraints because of the impending arrival of the donor heart. Nevertheless, a rapid history should screen for last oral intake, recent anticoagulant use, intercurrent deterioration of ventricular function, or change in anginal pattern; a physical examination should evaluate present volume status, and a laboratory review (if available) and a chest radiograph should detect the presence of renal, hepatic, or pulmonary dysfunction. Many hospitalized patients will be supported with inotropic infusions and/or an intraaortic balloon pump, and the infusion rates and timing of the latter should be reviewed.
Equipment and drugs similar to those usually used for routine cases requiring CPB should be prepared. A β-agonist such as epinephrine should be readily available both in bolus form and as an infusion to treat ventricular failure rapidly, and an α-agonist such as phenylephrine or norepinephrine is useful to compensate for the vasodilatory effects of anesthetics because even small decreases in preload and afterload can lead to catastrophic changes in CO and coronary perfusion in these patients.
Placement of invasive monitoring before induction will facilitate rapid and accurate response to hemodynamic events during induction. In addition to standard noninvasive monitoring, an arterial catheter and a PA catheter (PAC, with a long sterile sheath to allow partial removal during graft implantation) are placed after judicious use of sedation and local anesthetics. Placing the PAC in a central site rather than the radial artery will avoid the discrepancy between radial and central arterial pressure often seen after CPB, but it also may be necessary to cannulate a femoral artery for arterial inflow for CPB if there has been a prior sternotomy. Floating the PAC into correct position may be difficult because of cardiac chamber dilation and severe tricuspid regurgitation. Large-bore intravenous access is mandatory, especially if a sternotomy has been previously performed, in which case external defibrillator/pacing patches also may be useful. The overall hemodynamic picture should be evaluated and optimized insofar as possible just before induction. If the hemodynamics seem tenuous, then starting or increasing an inotrope infusion may be advisable.
Most patients presenting for heart transplantation will not be in a fasting state and should be considered to have a full stomach. Therefore the induction technique should aim to rapidly achieve control of the airway to prevent aspiration while avoiding myocardial depression. A regimen combining a short-acting hypnotic with minimal myocardial depression (etomidate, 0.3 mg/kg), a moderate dose of narcotic to blunt the tachycardic response to laryngoscopy and intubation (fentanyl, 10 µg/kg), and succinylcholine (1.5 mg/kg) is popular; high-dose narcotic techniques with or without benzodiazepines also have been advocated. Vasodilation should be countered with an α-agonist. Anesthesia can be maintained with additional narcotic and sedatives (benzodiazepines or scopolamine).
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here