Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Recent outbreaks of vaccine-preventable childhood infections have occurred secondary to unvaccinated individuals and travel to areas where disease is still endemic. Emergency clinicians should recognize the possibility of these once rare diseases.
Herpes simplex encephalitis is fatal if untreated. Clinicians should suspect this diagnosis when evaluating severely ill patients for suspected meningitis or encephalitis and promptly institute empirical therapy with IV acyclovir while awaiting diagnostic results.
Primary varicella can be dangerous in select populations, including older children, adults, and pregnant patients. These patients require treatment with acyclovir.
Zoster patients should be treated with acyclovir if they present within 72 hours of symptoms onset or if they are immunocompromised regardless of duration of illness. Disseminated zoster should be treated with IV acyclovir.
In healthy patients with influenza infection, the duration of illness can be shortened by almost 1 day if antiviral treatment is administered within 48 hours of symptom onset. Hospitalized patients with influenza infection should be treated with antiviral medication regardless of duration of symptoms, because it may decrease mortality and influenza complications.
Rabies has the highest case fatality rate of any recognized infectious disease.
Almost 60,000 deaths per year worldwide are caused by dog-mediated human rabies, and this burden falls disproportionately on children and the poor in rural areas.
Globally, human rabies results from bites by infected dogs. In North America human rabies results predominantly from wildlife exposures (bat, raccoon, and skunks).
Treatment is rarely effective once symptoms of human rabies occur.
Rabies postexposure prophylaxis (PEP) given strictly according to the World Health Organization (WHO) or US Centers for Disease Prevention and Control (CDC) guidelines is extremely effective. Discussion with public health officials is recommended to guide decisions regarding when PEP should be considered. The CDC clinician information line is 877-554-4625 or 800-CDC-INFO.
Many emerging viral infections, including SARS-CoV2 and Ebola, should be considered in febrile patients. It is important to identify patients at risk by determining travel history and exposure history to individuals with confirmed infection. Once a patient is deemed at risk, the patient should be promptly isolated according to established guidelines while further investigation occurs. It is also important to immediately inform the hospital infection control program and public health agencies.
The vast majority of viral infections, such as the common cold, are minor and self-limiting. However, some are highly pathogenic, contagious, and have the potential to cause devastating illness. In addition to centuries-old infections such as chicken pox, there are also newer infections such as avian influenza, Middle East respiratory syndrome (MERS), enterovirus D68 (EV-D68), as well as SARS-CoV2 (see Chapter 120 ). With increasing international travel, emergency clinicians should be familiar with emerging infections spreading beyond their endemic origins. In addition to recognizing symptoms and knowing the treatment for these infections, emergency clinicians should be familiar with isolation and reporting practices vital to preventing global pandemics.
Advances in molecular biology have increased our knowledge of these infections, improved our diagnostic ability, and allowed more treatment options. Viruses are classified according to the type and structure of nucleic acid, capsid, and presence or absence of an envelope ( Table 119.1 ). In practice, it is useful to group viruses based on clinical syndromes. This chapter reviews select viral illnesses with high morbidity and mortality, those with specific treatments, and those with major public health consequences. The chapter begins by reviewing several preventable diseases reemerging because of decreasing immunization rates caused by unfounded fears of complications or side effects.
| DNA Viruses | ||
| Poxviridae | Variola | Smallpox |
| Orf | Contagious pustular dermatitis | |
| Herpesviridae | HSV-1, HSV-2 | Mucocutaneous ulcers, herpes encephalitis |
| Cytomegalovirus | Pneumonitis in immunocompromised patients | |
| VZV | Chickenpox, shingles | |
| HHV-6 | Roseola infantum | |
| EBV | Mononucleosis | |
| Kaposi sarcoma herpesvirus | Kaposi sarcoma | |
| Adenoviridae | Adenovirus (50+ species) | Upper respiratory tract infections, diarrhea |
| Papillomaviridae | Papillomavirus (80+ species) | Warts (e.g., plantar, genital) |
| Polyomaviridae | JC virus | PML |
| Hepadnaviridae | Hepatitis B | Hepatitis |
| Parvoviridae | Parvovirus B19 | Aplastic anemia |
| RNA Viruses | ||
| Reoviridae | Colorado tick fever | Fever and rash |
| Rotavirus | Gastroenteritis | |
| Togaviridae | Eastern equine encephalitis | Epidemic encephalitis |
| Rubella | German measles | |
| Flaviviridae | Yellow fever | Hemorrhagic fever |
| Dengue Zika |
Dengue hemorrhagic fever Fever, rash, arthralgias |
|
| West Nile virus | West Nile encephalitis | |
| Hepacivirus, hepatitis C | Chronic hepatitis | |
| Coronaviridae | Coronavirus | Upper respiratory tract infections |
| SARS-CoV MERS-CoV SARS-CoV-2 |
SARS MERS COVID-19 |
|
| Paramyxoviridae | Respiratory syncytial virus | Bronchiolitis |
| Measles | Measles (rubeola), SSPE | |
| Parainfluenza | Croup | |
| Rhabdoviridae | Rabies | Rabies |
| Filoviridae | Ebola | Hemorrhagic fever |
| Orthomyxoviridae | Influenza A, B | Influenza |
| Bunyaviridae | La Crosse | Encephalitis |
| Hanta | Hemorrhagic fevers, ARDS | |
| Arenaviridae | Lassa | Hemorrhagic fever |
| Lymphocytic choriomeningitis virus | Meningoencephalitis | |
| Retroviridae | HIV | AIDS |
| Picornaviridae | Poliovirus | Polio |
| Coxsackie B | Myocarditis | |
| Hepatitis A | Enteric hepatitis | |
| Rhinovirus (115+ species) | Upper respiratory infections | |
| Caliciviridae | Norwalk virus | Gastroenteritis |
| Unclassified viruses | Hepatitis E | Enteric hepatitis |
Childhood immunization is among the most important public health measures globally. Immunizations save 2 to 3 million children per year from serious illness, disability, and death. However, there has been a troubling trend of people in industrialized nations refusing routine immunizations. These groups advocate for nonmedical exemptions from mandated school-entry vaccines in developed nations, and routine immunizations have been rejected by some over questions of safety and the lack of perceived threat for serious vaccine-preventable diseases. The emergency clinicians may therefore play a significant role in educating parents on the safety and efficacy of childhood immunizations. The United States (US) Advisory Committee on Immunization Practices (ACIP), the American Academy of Pediatrics (AAP), and the American Academy of Family Physicians recommend a specific childhood immunization schedule each year. Table 119.2 summarizes the currently available viral vaccines and recommended schedule.
| Virus | Vaccine | Type | Indication | Recommended Schedule |
|---|---|---|---|---|
| Smallpox | Vaccinia | Live | For persons at risk or for emergency responders | Once, before anticipated risk of exposure |
| Polio | Oral polio vaccine (Sabin) | Live | During outbreaks Unvaccinated travelers |
Inactivated polio vaccine preferred in almost all cases |
| Inactivated polio vaccine (Salk) | Inactivated | All children | At 2, 4, 6–18 months, and at 4–6 years | |
| Measles | Measles, mumps, rubella (MMR) | Live | All normal children | At 12–15 months and 4–6 years |
| Mumps | MMR | Live | All normal children | Same as for measles |
| Rubella | MMR | Live | All normal children | Same as for measles |
| Hepatitis A | HAV vaccine | Inactivated | Persons at risk (e.g., travelers, persons living in areas of high prevalence) | Two doses, 6 months apart. Ideally should be given one month prior to travel. Immune globulin should be given if travel is imminent |
| Hepatitis B | HBV vaccine | Inactivated or recombinant | All children | At birth, 1–2 months, and 6–18 months |
| Persons at risk of exposure (e.g., health care workers) | Hepatitis B immune globulin (HBIG) should be given in addition in case of high-risk exposure | |||
| Influenza A and B | Influenza vaccine | Inactivated | In 2010, CDC expanded recommendation for annual influenza vaccination to include all persons aged 6 months and older | One dose yearly in the fall or winter |
| Intranasal vaccine | Live, cold adapted | As above, for persons 2–49 years of age. Avoid if pregnant, immunosuppressed, young children with asthma, allergic to eggs | As above | |
| Rabies | Human diploid cell vaccine (HDCV) | Inactivated | Postexposure prophylaxis or for preexposure prophylaxis in high-risk individuals | Postexposure: HDCV or PCEC 1.0 mL IM in the deltoid region on days 0, 3, 7, and 14. Rabies immune globulin (RIG) 20 IU/kg should be administered around the wound site, as possible, with the remainder given IM at an anatomically distant site. Preexposure: HDCV or PCEC 1.0 mL IM in the deltoid region on days 0, 7, 21, and 28. |
| Purified chick embryo cell (PCEC) | Inactivated | Postexposure prophylaxis or for preexposure prophylaxis in high-risk individuals | As above | |
| Yellow fever | 17D virus strain | Live | Persons 9 months to 59 years of age traveling to endemic areas. Contraindicated in children younger than 6 months of age, precaution in age 6–8 months and 60 years or older | Boosters every 10 years |
| Rotavirus | RV1 | Live | All healthy children | 2 dose series, at 2 months and 4 months of age |
| RV5 | Live | All healthy children | 3 dose series, at 2, 4, and 6 months of age | |
| Varicella | Varicella | Live | All healthy children | At 12–15 months and 4–6 years |
| At-risk adults (those without evidence of immunity and high risk for exposure or transmission) | Persons older than 13 years should receive two doses 4–8 weeks apart | |||
| Zoster | Zoster | Live | Anyone 60 years of age and older, contraindicated in severe immunodeficiency | A single one time dose in adults aged 60 years or older |
Mumps is an RNA virus that is a member of the Paramyxoviridae family. It causes a febrile illness with swelling and tenderness of the parotid gland. Since the advent of the mumps vaccine in 1967, there has been a 99% decrease in mumps in the United States. Despite the vaccine, recent outbreaks in industrialized nations, even in vaccinated individuals, raised concerns about resurgence of mumps.
Mumps is spread via infected respiratory secretions that enter a susceptible respiratory tract. The incubation period is typically 16 to 18 days, ranging from 12 to 25 days. Infected patients are most contagious 1 to 2 days before onset of disease but can be contagious as early as 7 days before symptoms and up to 9 days after symptoms start.
Parotitis, either unilateral or bilateral, is the hallmark of this infection, occurring in over 95% of symptomatic patients ( Fig. 119.1 ). Other salivary glands are not commonly affected. Symptoms usually begin with fever, malaise, and headache, but about one-third of mumps infections are asymptomatic. Up to 30% of mumps infections cause orchitis, which usually occurs 1 week after the onset of parotitis and is more commonly seen in older patients. Orchitis is usually unilateral but can occur in both testes in up to one-third of the cases. There is a high incidence of cerebrospinal fluid (CSF) pleocytosis in patients with mumps, but less than 10% have symptomatic meningitis, and less than 1% have encephalitis. The mortality from mumps is very low, and the majority of morbidity and mortality associated with mumps occurs in cases complicated by encephalitis.

During an outbreak, mumps can be easy to diagnose. Other viral infections that can cause parotitis (Epstein-Barr virus [EBV], parainfluenza, influenza A virus, coxsackievirus, adenovirus, parvovirus B19, lymphocytic choriomeningitis virus, and human immunodeficiency virus [HIV]), bacterial infections, facial cellulitis, and tumor are all other diagnoses that should be considered.
Mumps can be confirmed by detection of viral RNA, via reverse transcription polymerase chain reaction (RT-PCR), detection of the virus itself from clinical specimens, or detection of antibodies (immunoglobulin M [IgM] or a fourfold rise in immunoglobulin G [IgG] between acute and convalescent serum specimen). This entails collecting a buccal or oral swab specimen for virus isolation and blood sample for serologic testing. Collecting samples early improves yield as virus isolation greatly diminishes after the first week of symptoms.
The mainstay of treatment is supportive care with antipyretics and analgesics. There is no specific antiviral treatment. Most cases have a benign, self-resolving course and do not require admission to the hospital. In the hospital setting, these patients should have droplet precautions observed. Patients should be isolated for 5 days after the onset of parotid swelling. Individuals with close contact with the infected patient should receive vaccinations if not immunized.
Measles is an RNA virus thought to be the most contagious infection known to humans. It was a common childhood illness, causing 3 to 4 million cases per year in the United States the 1960s, but the number of cases has dramatically decreased since the advent of the measles vaccine. Despite introduction of the measles vaccine in the 1960s, measles remains common in developing countries, mostly in parts of Africa and Asia. Global health initiatives aimed at eliminating measles focus on reaching and maintaining over 95% coverage with two doses of measles-containing vaccination. Progress has been made toward measles elimination; the World Health Organization (WHO) reported that from 2000 to 2018, the annual measles incidence decreased by 66% and measles-related deaths decreased by 73%.
Measles still occurs in the United States and other developed nations, mostly among unvaccinated or incompletely vaccinated individuals who have exposures to individuals infected from an endemic region. In 2011, France had a measles outbreak with nearly 15,000 cases. A recent outbreak in New York City was linked to an unvaccinated child returning home from Israel with measles with over 600 cases occurring.
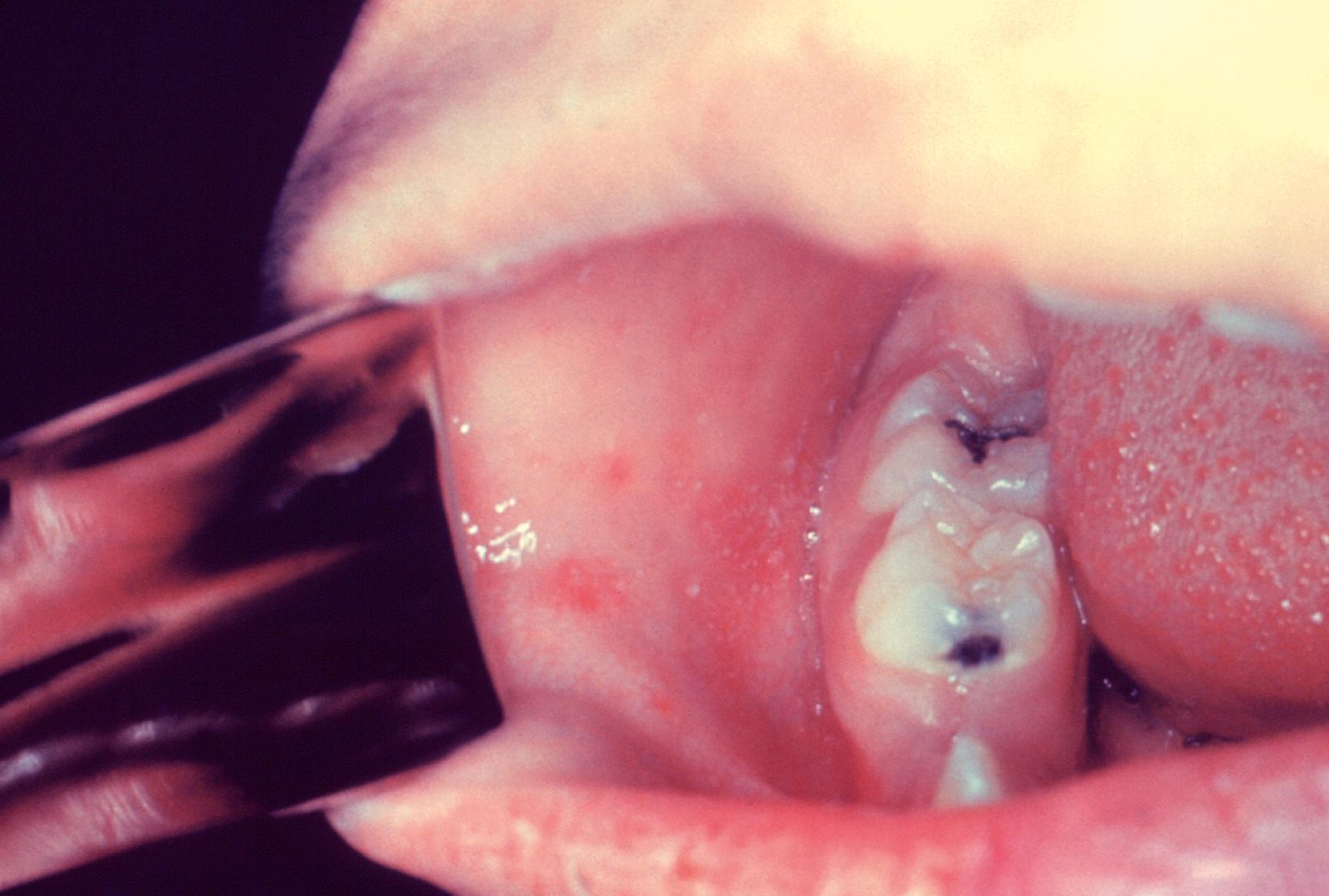
The incubation period for measles is 7 to 21 days. The first symptoms manifest during the prodromal phase, which lasts approximately 3 days. During this phase patients have fever, malaise, and the classically taught three Cs (cough, coryza, and conjunctivitis). Koplik spots, small raised bluish white spots on the buccal mucosa, often opposite the lower first and second molars, or the roof of mouth ( Fig. 119.2 ), are pathognomonic for the diagnosis and can be seen during the prodromal phase. The patient will then develop the typical rash; a nonpruritic maculopapular rash beginning on the head and face and spreading down the entire body over the next 2 to 3 days ( Fig. 119.3 ). Patients are contagious 4 days before and 4 days after the onset of the rash.

Complications of measles include otitis media, laryngitis, tracheobronchitis, bronchiolitis, pneumonitis, severe diarrhea, and acute encephalitis. The virus itself can also cause pneumonia. Bacterial superinfection can also occur. The populations that are at high risk for severe disease or complications include children younger than 5 years old, adults older than 20 years old, pregnant women, and the immunocompromised.
Subacute sclerosing panencephalitis (SSPE) is a rare but fatal complication of measles. SSPE is a slow progressive infection of the central nervous systems (CNS) that results from a prior measles infection. It is thought to be due to continual measles infection of the CNS. The mean time of onset of SSPE is 7 years after measles infection. Symptoms include behavior change, decreased intellect, ataxia, and myoclonic seizures followed by progressive neurologic deterioration and death. Since the development of measles vaccine, this disease has almost disappeared in the United States.
Measles can be mistaken for other acute respiratory viral illnesses with rash or even noninfectious illnesses that present with fever and rash. Other diagnoses to consider include rubella, roseola, dengue, Kawasaki disease, and drug rash. Measles should be considered in patients that have traveled to endemic regions and return with fever and rash.
The diagnosis was usually made clinically by visualizing both Koplik spots and the characteristic rash along with cough, coryza, and conjunctivitis. However, the disease is not common in the developed world, and it may be mistaken for other illnesses. Clinicians suspecting a diagnosis of measles should contact local health departments. They can help instruct practitioners to obtain the necessary samples for diagnosis and surveillance. The most common methods of confirmation are serologic testing for measles-specific IgM antibody and detection of measles RNA from a nasopharyngeal specimen, blood, or urine by RT-PCR.
The mainstay of treatment is supportive care. Bacterial superinfection should be treated appropriately. Postexposure prophylaxis is important in individuals who do not have evidence of measles immunity and have a measles exposure, because it can provide protection or lessen the severity of disease. Postexposure prophylaxis consists of either the measles, mumps, and rubella (MMR) vaccine within 72 hours, or immunoglobulin within 6 days. Healthy infants should receive 0.25 mL/kg of immunoglobulin intramuscularly, and immunocompromised children should be given 0.5 mL/kg intramuscularly, up to 15 mL. Children and malnourished patients who are hospitalized with severe measles may benefit from vitamin A.
Patients with measles require admission to the hospital based on the severity of illness. Uncomplicated measles patients should be treated at home to prevent spread of the disease. It is important, however, to observe appropriate isolation precautions in the hospital setting. All suspected cases of measles should be evaluated with airborne isolation precautions in place. Infected individuals should have airborne isolation for 4 days after they develop the rash, and those who are immunocompromised should remain on airborne precautions until complete recovery.
Rubella is a single-stranded RNA virus that is a member of the Togaviridae family. Since the wide-scale implementation of the vaccine, cases have dropped by greater than 99%. As a result, rubella is no longer endemic in the United States. The virus is spread via contact with respiratory droplets. In pregnant patients, the virus spreads to the placenta with subsequent infection of fetal organs.
Acquired rubella is a mild febrile illness associated with a diffuse maculopapular rash, malaise, headache, and arthritis. Encephalitis and thrombocytopenia are rare complications. Rubella is generally a mild disease, but consequences in pregnant patients can be devastating. It can cause miscarriage, intrauterine death, premature delivery, or congenital rubella syndrome. Congenital rubella syndrome is characterized by severe birth defects, including hearing impairment, cataracts, retinopathy, developmental delay, microcephaly, and a variety of congenital heart defects.
The diagnosis of rubella on a clinical basis can be difficult because of the overlap with many other illnesses. Diseases that share common features include measles, roseola, erythema infectiosum (fifth disease), toxoplasmosis, and scarlet fever.
The diagnosis of rubella can be made by virus detection or serologic testing. The most common method is detection of IgM antibodies or fourfold increase in IgG antibody titer between acute and convalescent specimen. Virus culture and RT-PCR can also be isolated from blood or the nasopharynx.
There is no specific antiviral treatment for rubella. The management centers on symptom control with antipyretics and analgesics. The course of this disease is short and benign. These patients can generally be treated at home but should be educated about the risks to pregnant women.
Herpes simplex virus type 1 (HSV-1) and herpes simplex virus type 2 (HSV-2) are double-stranded DNA viruses of the Herpesviridae family. Herpes simplex infections primarily involve the skin or mucosal surfaces with occasional severe involvement of organs. Herpes simplex virus (HSV) infections range in acuity from asymptomatic to life-threatening. HSV-1 typically causes orofacial infections but can affect liver, lung, eye, genitalia, and the CNS. HSV-2 typically causes genital herpes but can also affect the other systems as well. HSV infections are common; the seroprevalence of HSV-1 has been reported to be 57.7% in persons aged 14 to 49 years old in the United States, and the seroprevalence of HSV-2 has been reported to be 17.0% in the same population.
Initial HSV-1 infection usually occurs in childhood. HSV gains entry via breaks in the skin or mucosal surfaces. Viral replication is then initiated in epidermal and dermal cells. The infection then spreads to the nervous system, where it lays latent in the sensory nerve ganglia. Any stressor such as acute illness, emotional stress, trauma, intense sunlight, or fever can trigger reactivation of the virus. Recurrence rates are high for herpes infections. HSV-2 infections usually are acquired in adolescence or adulthood through sexual contact. Neonatal HSV-2 infections occur during childbirth via contact with the infected mother’s birth canal.
The first episode of HSV-1 infections usually occurs early in life and manifests as a gingivostomatitis and pharyngitis. Symptoms include fever, malaise, and vesicular lesions anywhere in the mouth or oropharynx. Infections typically last between 10 to 14 days. Reactivation is usually much less severe and occurs as herpes labialis, small vesicles at the vermilion border of the lip ( Fig. 119.4 ). These vesicles usually crust over within 48 hours.

This infection is characterized by painful vesicles and ulcers on the external genitalia. The first infection is usually the most severe and can be accompanied by systemic symptoms like fever, headache, malaise, and myalgias. It is also common to have dysuria and tender inguinal lymphadenopathy. Infections can also spread to the perianal and rectal region as well.
HSV-1 is a common cause of infectious encephalitis; it causes necrotizing hemorrhagic encephalitis, typically involving the temporal lobes. Herpes simplex encephalitis is characterized by acute onset of symptoms, including fever, headache, altered mental status, seizures, and focal neurologic deficits resulting from frontal and temporal lobe necrosis. If left untreated, mortality is greater than 70%. HSV-2 can cause meningitis in over 25% of patients with primary infection, more commonly in women. In contrast to HSV encephalitis, HSV meningitis has a benign course. Neonatal HSV encephalitis is caused by HSV-2 acquired during vaginal delivery of an infected mother.
Herpes can cause a variety of cutaneous manifestations. They typically present with the classic painful grouped vesicles on an erythematous base on the affected area. Herpetic whitlow refers to these vesicles occurring on the finger. Herpes gladiatorum is a skin infection that can arise anywhere on the body and is associated with contact sports. Herpes can also cause ocular infections, including keratitis, conjunctivitis, and acute retinal necrosis. Immunocompromised patients are at risk for rare infections like HSV pneumonitis, esophagitis, or hepatitis.
When suspecting orofacial HSV infection, considerations include other diseases with vesicles and ulcers, such as aphthous ulcers, coxsackievirus infections (herpangina and hand-foot-and-mouth disease), infectious mononucleosis, Stevens-Johnson syndrome, or Behçet disease. The differential diagnosis for genital herpes infection should include other sexually transmitted infections with ulcers and vesicles, such as syphilis or chancroid or noninfectious diseases like Behçet disease. HSV encephalitis can be difficult to distinguish from other acute CNS emergencies like bacterial meningitis, brain abscess, other viral encephalitides, brain tumor, or stroke.
Frequently, clinicians diagnose oral or genital HSV infections clinically, given the classic appearance of the vesicles and ulcers. However, because of the risk of transmission and the impact of this diagnosis on a patient, testing should be performed if possible. Definitive diagnosis can be made by viral culture, direct fluorescent antibody (DFA), or polymerase chain reaction (PCR) from vesicles, ulcers, or mucocutaneous sites. PCR is more sensitive than viral culture. Tzanck smear has a low sensitivity and specificity and is mainly of historical interest. Serology can differentiate between acute infection and reactivation.
The diagnosis of HSV encephalitis is made by PCR from the CSF. The routine laboratory tests sent after a lumbar puncture (LP) to assess for bacterial meningitis do not adequately assess for HSV encephalitis. Classically, CSF analysis shows an elevated white blood cell (WBC) count, with lymphocyte predominance. Depending on the degree of brain necrosis, an elevated red blood cell (RBC) count can also be seen. Although it is rare, CSF results can be normal in HSV encephalitis, particularly in immunocompromised individuals. This underscores the importance of waiting for PCR results before considering discontinuation of treatment in suspected cases of HSV encephalitis. In cases of negative CSF PCR with a high suspicion of HSV encephalitis, especially those with who present early in their illness, we recommend continuing empirical treatment and resending CSF PCR in 72 hours. Neuroimaging with computed tomography (CT) or magnetic resonance imaging (MRI) can be highly suggestive of HSV encephalitis, but imaging can be negative early in the course of illness ( Fig. 119.5 ).

Antiviral agents are the mainstay of treatment. The treatment dose and duration for herpes simplex depends on the clinical syndrome that is present. Acyclovir, valacyclovir, and famciclovir are the commonly used antiviral drugs with activity against HSV. These drugs are nucleoside analogues that work by inhibiting viral DNA synthesis. Acyclovir is the only agent that is available in an intravenous (IV) formulation.
Herpes gingivostomatitis or labialis: First episodes are treated with oral acyclovir 200 mg five times a day (alternative regimen: 400 mg three times a day), valacyclovir 1 g twice daily, or famciclovir 250 mg three times a day for 7 days. Recurrent infections are treated with acyclovir 400 mg five times a day for 5 days, valacyclovir 2 g twice daily for 1 day, or famciclovir 1500 mg as a single dose.
Genital herpes: First episodes are treated with oral acyclovir 200 mg five times a day (alternative regimen: 400 mg three times a day), valacyclovir 1 g twice daily, or famciclovir 250 mg three times a day for 7 to 10 days. A shorter course is usually adequate for treatment of recurrence. For suppression of recurrent episodes, acyclovir 400 to 800 mg twice daily or valacyclovir 500 mg daily can be used.
Herpetic whitlow and other mucocutaneous manifestations: Administer acyclovir 200 mg five times a day or 400 mg three times a day for 5 days.
Herpes keratitis: Administer acyclovir 400 mg five times a day or valacyclovir 500 mg three times a day. Topical antiviral therapy with trifluridine, acyclovir, or ganciclovir are all equally effective.
HSV encephalitis: Administer IV acyclovir 10 mg/kg every 8 hours for 14 to 21 days. Given the high mortality associated with this condition, antiviral therapy should be started as soon as the diagnosis is suspected.
The majority of herpes infections can be treated with oral antiviral therapy on an outpatient basis. Patients who are immunocompromised and have severe mucocutaneous disease or disseminated disease benefit from inpatient admission with IV acyclovir treatment. All patients with suspected encephalitis should be admitted for empirical treatment and diagnostic testing. Intensive care unit (ICU) admission may be necessary depending on the severity of neurologic symptoms. For HSV encephalitis patients, we recommend early involvement of infectious disease consultants to help guide treatment and neurology for management of cerebral edema and severe neurologic symptoms.
The varicella-zoster virus (VZV) is another double-stranded DNA virus that is a member of the Herpesviridae family. VZV causes two common infections: varicella (chicken pox) and zoster (shingles). Transmission occurs via the respiratory tract through respiratory droplets and also by direct contact with virus present in the fluid-filled vesicles. VZV initially infects the nasopharynx and spreads to the lymphoid tissue. The virus is present in vesicles that develop on the skin and then infects the nerve endings in the skin and migrates to the dorsal ganglia where it lays latent.
Primary infection of VZV occurs as varicella (chicken pox). Varicella is highly contagious and historically occurred year round with a predilection for winter and spring months. Prior to the development of the varicella vaccine in 1995, most people would develop this infection in childhood. After widespread uptake of the vaccine, the incidence of varicella has decreased by 90%, with a subsequent decline in mortality. Zoster (shingles) is a result of reactivation of the latent virus. Risk factors for developing shingles include older age and immunosuppression.
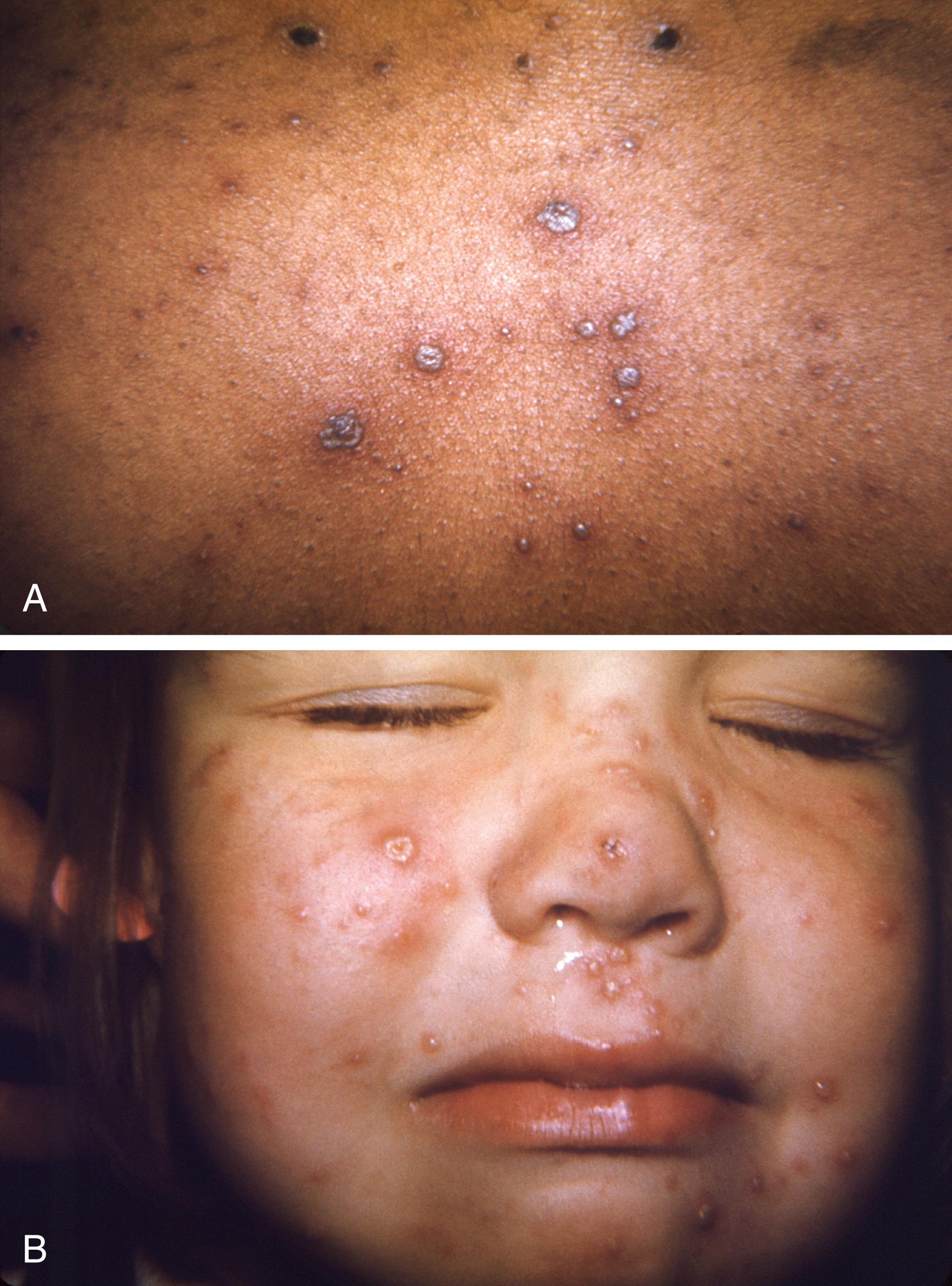
Chicken pox is a febrile illness characterized by malaise and rash. The rash begins first on the scalp and face and then spreads to the trunk and extremities. The lesions start as maculopapular, and progress to fluid-filled vesicles that eventually crust over and form scabs ( Fig. 119.6 ). The lesions occur as crops at various stages of development. Patients are contagious until all lesions are scabbed over, which can typically take 1 to 2 weeks.
This disease typically has a benign course, although adults have a more severe course than children. The most common complication is a secondary bacterial infection of the skin lesions. VZV has been associated with invasive group A streptococcal infections and necrotizing fasciitis. Immunocompromised patients are at risk for disseminated disease and visceral organ involvement. Pregnant patients are also at risk for severe disease. Varicella pneumonia accounts for most of the morbidity related to this disease. Neurologic complications are rare but can include encephalitis, aseptic meningitis, transverse myelitis, and Reye syndrome. Although exceedingly rare, it is important to recognize the association of aspirin use with Reye syndrome, a progressive encephalopathy with acute liver injury. Thus aspirin and other salicylates should be avoided in varicella treatment, especially in children.
Herpes zoster typically causes a vesicular rash with an erythematous base that occurs unilaterally in a single dermatome ( Fig. 119.7 ). The rash is often painful and preceded by paresthesias or hypesthesia. In immunocompetent individuals, the rash crusts in 7 to 10 days, and at that time patients are no longer contagious. Post-herpetic neuralgia, defined as pain that persists for more than 90 days, is the feared complication. Risk factors for post-herpetic neuralgia include older age and severity of pain at onset.

Herpes zoster ophthalmicus is viral reactivation within the trigeminal nerve ganglion. Ocular involvement occurs in over 50% of these cases. The Hutchinson sign, a vesicle on the tip of the nose, is associated with ocular involvement. Herpes zoster oticus (Ramsay Hunt syndrome) is characterized by facial nerve palsy, pain, and vesicular rash on the ear and in the auditory canal. Disseminated zoster involving multiple dermatomes can occur in immunocompromised patients.
Classic varicella is distinctive, but the other major diagnoses to consider are other febrile illnesses with rashes like disseminated HSV infection, coxsackievirus infection, measles, or rickettsialpox. Prior to eradication, smallpox was a consideration, presenting with lesions in the same stage of development. The rash of zoster is also usually very characteristic. Other diagnoses to consider include herpes simplex infection or contact dermatitis.
The majority of chickenpox and shingles diagnosis is made clinically. Confirmatory diagnosis can be made through viral culture, DFA, or PCR testing of the vesicle fluid.
The management is mainly supportive care with antipyretics and antihistamines to decrease the pruritus caused by the skin lesions. Salicylates should be avoided in children because of the association with Reye syndrome. Antiviral therapy with acyclovir has been shown to decrease the duration of fever and total number of lesions in healthy children. It does not reduce the number of varicella-related complications, however. Therefore, we typically do not recommend treatment of otherwise healthy children with varicella. We recommend treating high-risk groups with acyclovir, including those older than 12 years old, pregnant patients, persons with chronic cutaneous or pulmonary disorders, persons on long-term salicylate therapy, persons on aerosolized corticosteroids, and immunocompromised patients. The treatment should be initiated within 24 hours after the rash appears for the most benefit. The dose of acyclovir for VZV treatment is higher than that of HSV, 800 mg orally four times a day for 5 days. If the patient is immunocompromised and has severe disease, IV acyclovir should be administered.
The goals of treatment for zoster are to treat the viral infection and control the pain that occurs with the rash. Uncomplicated zoster in the immunocompetent host can be treated with the following regimens for 1 week: acyclovir 800 mg five times a day, famciclovir 500 mg three times a day, or valacyclovir 1 g three times a day. Antiviral treatment should be initiated within 72 hours of the onset of rash because the efficacy beyond 72 hours is unclear. Immunocompromised patients should be treated regardless of time of onset of rash. Zoster involving more than one dermatome or disseminated zoster should be treated with IV acyclovir. The disease is often painful enough to require opioid agents. Currently, there are no treatments that have reliably shown a reduction in the occurrence of post-herpetic neuralgia. Antiviral treatment has shown mixed results and is likely not useful in preventing post-herpetic neuralgia. Corticosteroids have been studied extensively, but a recent review did not support their use in preventing post-herpetic neuralgia.
Most patients with varicella and zoster can be treated at home. Patients with varicella are highly contagious and should be instructed to avoid people who have not been fully vaccinated or never had the disease, immunocompromised persons, or pregnant individuals until all of their lesions have crusted over. Immunocompromised patients, patients with disseminated zoster, or patients with complications require admission to the hospital.
In general, patients with varicella should be under contact and airborne precautions until all of the lesions have crusted over. An immunocompetent localized zoster patient only requires standard precautions, whereas an immunocompromised or disseminated zoster patient is treated like a patient with varicella, requiring contact and airborne precautions.
EBV is a member of the Herpesviridae family. It is classically known for causing infectious mononucleosis. It is also associated with several types of cancer, including Burkitt lymphoma, nasopharyngeal carcinoma, Hodgkin disease, and B cell lymphoma. EBV is ubiquitous, with most individuals testing positive for antibodies by adulthood. One British study demonstrated that 70% of 0- to 5-year-olds had antibodies to EBV, whereas 95% of 20- to 25-year-olds tested positive. EBV is spread via salivary secretions. The virus infects the oropharynx and then spreads through the bloodstream and infects B lymphocytes resulting in proliferation of infected B lymphocytes and T lymphocytes, leading to enlargement of lymphoid tissue.
EBV infection in young children is usually asymptomatic or presents as mild pharyngitis. Adolescents and young adults tend to have the classic infectious mononucleosis (fever, exudative pharyngitis, lymphadenopathy, myalgias, and fatigue). Splenomegaly is common, seen in up to 50% of cases. Hepatomegaly and jaundice occur less than 10% of the time. The symptom duration is typically 1 to 3 weeks, with some cases having malaise and fatigue for several months. Splenic rupture is rare, occurring in less than 0.5% of patients. It should be suspected in patients with left upper quadrant pain and is more common during the first 3 weeks of illness. Airway obstruction occurs in less than 5% of children with mononucleosis and is one of the common causes of hospital admission. Rare neurologic complications include encephalitis, aseptic meningitis, transverse myelitis, Guillain-Barré syndrome, retrobulbar neuritis, and peripheral neuropathies. Patients treated with amoxicillin or ampicillin for presumed streptococcal pharyngitis may develop a nonallergic maculopapular rash.
EBV causes 90% of infectious mononucleosis; the remaining 10% is caused by cytomegalovirus (CMV). Acute HIV infection, streptococcal pharyngitis, toxoplasmosis, and other viral pharyngitis causes should be considered in potential mononucleosis patients.
It is difficult to diagnose mononucleosis based on history and physical examination alone. Laboratory data can help confirm the diagnosis. Historically, the heterophile antibody test (monospot) has been the test of confirmation for primary EBV infection. The test has a sensitivity ranging from 63% to 84% and specificity ranging from 84% to 100%. The test is often not positive in younger children. The WBC count typically demonstrates lymphocyte predominance with many atypical lymphocytes. A lymphocyte count less than 4 × 10 9 /L in adults is highly predictive of a negative monospot test. Health care providers can test for antibodies to EBV viral capsid and nuclear antigen if other testing is equivocal.
Infectious mononucleosis typically has a self-limiting course. The treatment is supportive care with rest, antipyretics, and analgesia. Glucocorticoids have been used to decrease severity of symptoms, but there is insufficient evidence to support this practice. Antiviral treatment with acyclovir does not reduce the clinical symptoms of the disease. It is important to advise patients to avoid contact sports for at least 3 weeks to avoid the feared complication of splenic rupture. Abdominal ultrasound for assessment of spleen size may have a role in determining when it is safe to return to sports.
The majority of patients can be treated at home. Admission is necessary for airway obstruction and in patients with significant complications, such as splenic rupture.
CMV is a double-stranded DNA virus that belongs to the Herpesviridae family. Depending on geographic location, the seroprevalence ranges from 66% to 90%. The spectrum of illness caused by CMV ranges from asymptomatic to severe disseminated disease in the immunocompromised patient. CMV is particularly harmful in pregnant patients because it can lead to congenital infection, causing profound neurologic defects and permanent hearing loss. CMV is present in breast milk, saliva, feces, urine, semen, cervical secretions, and blood. The virus spreads via prolonged exposure to these body fluids. After primary infection, CMV establishes a lifelong latent infection.
The primary CMV infection is subclinical in most individuals. Some immunocompetent adults develop a mononucleosis-like syndrome. The illness can last from 2 to 6 weeks and is characterized by fever, fatigue, malaise, myalgia, and headache. Unlike EBV mononucleosis, exudative pharyngitis and lymphadenopathy are less common. Although it is rare, CMV can cause severe disease in the immunocompetent individual. CMV colitis and CNS infection (meningitis, encephalitis, transverse myelitis) are the most frequent forms of severe CMV infection in the immunocompetent host. Up to one-third of critically ill immunocompetent patients have evidence of CMV reactivation.
The majority of newborns who are infected with congenital CMV appear healthy or normal at birth. Common problems caused by congenital CMV infection include premature birth, intrauterine growth retardation, microcephaly, seizures, thrombocytopenia, hepatosplenomegaly, or pneumonitis. Sequelae of congenital CMV infection can present up to 2 years after birth. Frequent complications that occur are hearing loss, neurologic impairment, and ocular disturbances.
CMV can cause life-threatening disease in immunocompromised patients. CMV infection occurs in over 40% of solid organ transplant patients during the first 3 months when immunosuppressive therapy is the strongest. Transplant patients that are CMV seronegative and receive a CMV seropositive donor are at highest risk. HIV patients with CD4 count less than 100/μL are at high risk of CMV infection as well. In the immunocompromised host, CMV manifests initially as fever, malaise, and myalgias. The infection can then progress to cause leukopenia, pneumonia, esophagitis/gastritis, hepatitis, colitis, encephalitis, polyradiculopathy, and retinitis. CMV retinitis is the most common cause of blindness in patients with AIDS.
It is difficult to make the diagnosis of CMV infection solely on a clinical basis. Infectious mononucleosis caused by EBV presents very similarly. In the perinatal phase, infants with apparent infections should be evaluated for the other common congenital infections: toxoplasmosis, rubella, herpes simplex, syphilis, VZV, and parvovirus B19. Because the CMV infection can cause a wide array of disease in the immunocompromised host, the differential diagnosis should be broad and include other viral pathogens, bacterial infections, Pneumocystis infection, and fungal infections.
Making the diagnosis of CMV is unlikely in the ED. Confirmation of this diagnosis centers on either virus isolation, serologic testing, or histopathology. Common methods involve PCR, viral culture, or antibody testing. The WBC count may show lymphocyte predominance with more than 10% atypical lymphocytes, much like EBV infections.
For the most part, CMV infection in the immunocompetent host only requires symptomatic care for the mononucleosis-like syndrome. The treatment recommendations for critically ill immunocompetent patients with CMV infection are less clear. Immunocompromised patients with CMV infection are treated more aggressively. Antiviral treatment is necessary in sight and life-threatening infections.
Ganciclovir is an IV agent that is used to treat CMV infections. The treatment for CMV retinitis is induction therapy: 5 mg/kg/dose every 12 hours for 14 to 21 days followed by 5 mg/kg/dose once daily maintenance therapy for a prolonged course. Fever, diarrhea, and thrombocytopenia are common adverse reactions. Valganciclovir is an oral prodrug that is metabolized to ganciclovir. The treatment regimen is induction: 900 mg twice daily for 21 days followed by maintenance of 900 mg once daily. Foscarnet and cidofovir are IV agents used to treat CMV resistant to ganciclovir, and both can also be used to treat HSV resistant to acyclovir. The primary limiting toxicity of these drugs is renal toxicity.
Most immunocompetent patients with CMV infection can be managed at home. In contrast, immunocompromised patients with CMV infection will usually require admission to the hospital, and depending on the extent of end-organ damage, may require ICU admission.
Enteroviruses are a group of single-stranded RNA viruses that can multiply within the gastrointestinal tract. Most infections are asymptomatic or mild undifferentiated illnesses. Despite their name, their major manifestation is not gastroenteritis. There are many enteroviruses; common ones include poliovirus, coxsackievirus A and B, echovirus, and enterovirus. These viruses are found globally and are transmitted via the fecal-oral route. Vaccination exists for poliovirus; in the United States and other industrialized nations, the disease has been declared eradicated.
Most of the infections caused by enteroviruses are asymptomatic or self-limiting febrile illnesses. More of the severe infections are discussed in the following sections.
The poliovirus causes a nonspecific febrile illness with malaise, myalgias, headache, and sore throat. The most feared presentation of the poliovirus infection is paralytic poliomyelitis. This manifests as aseptic meningitis followed by back, neck, and muscle pain and then the development of motor weakness. The paralysis is usually asymmetrical and affects proximal muscles more. Usually some recovery of motor function occurs months later, but approximately two-thirds of patients have some form of permanent weakness.
Most enterovirus infections are subclinical, but they can also cause a variety of symptoms and syndromes. Enteroviruses account for most causes of viral meningitis and encephalitis. Enteroviruses commonly cause pericarditis and myocarditis, particularly coxsackievirus B. Symptoms usually include chest pain, fever, dyspnea, and can progress to severe heart failure. Enteroviruses are a common cause of viral exanthems as well. Herpangina is caused by coxsackievirus A and presents with fever, sore throat, odynophagia, and vesiculopapular lesions on the cheeks and soft palate ( Fig. 119.8 ). Hand-foot-and-mouth disease is caused by coxsackievirus A or enterovirus 71 and commonly manifests as fever and malaise, followed by vesicles in the mouth, and vesicles on the hands and feet ( Fig. 119.9 ). Pleurodynia is a painful illness characterized by fever and spasms of the chest wall and abdomen that occur in paroxysms.


In 2014, there was an outbreak across the United States of EV-D68. The virus affected mostly children and was severe in children with asthma. Typically EV-D68 causes mild respiratory illness, rhinorrhea, sneezing, cough, and myalgias but occasionally causes severe disease with wheezing and respiratory distress. There has also been an association with flaccid paralysis with anterior myelitis with EV-D68 infection.
Clinicians should consider other diagnoses depending on the specific symptoms and syndrome caused by enterovirus infection. For the diseases with skin and oropharyngeal lesions, herpes simplex, aphthous stomatitis, mononucleosis, and bacterial pharyngitis should be considered. The diseases with primary neurologic manifestation present similarly to bacterial meningitis and other causes of viral meningitis or encephalitis, including herpes simplex encephalitis. Myopericarditis can present similar to pulmonary embolism, myocardial infarction, or pneumonia (see Chapter 68 ).
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here