Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
History and physical examination, with additional testing as indicated, that is performed before participation in sport, that meets several objectives, and that is one of the most important functions provided by the sports medicine physician.
Often, this is the first interaction between the physician and the athlete; for many young adults, it may be the first exposure to the healthcare system.
It does not replace regular physical examinations, although many athletes think that it covers all healthcare needs.
It encompasses clearance for participation in the sport and provides education and information to athletes regarding issues such as nutrition, supplementation, training and conditioning, injury prevention, and rehabilitation.
Addition of a 12-lead electrocardiogram (ECG) examination as part of the standardized screening process is controversial.
Special considerations of PPPE include age specificity, sex specificity (special concerns for female vs. male athletes), sport specificity (specific demands of each sport should be considered), athletes with special needs, and athletes with physical or intellectual disabilities.
Emphasize cardiovascular, neurologic, and musculoskeletal issues
Identify any life-threatening or disabling conditions (e.g., underlying cardiovascular or neurologic abnormalities)
Identify any conditions that may put an athlete at risk of injury or illness (e.g., underlying ligamentous instability, musculoskeletal abnormalities, organomegaly, exercise-induced bronchospasm, or acute medical illness)
Assess an injury that has not been appropriately rehabilitated
Assess medical conditions and strength and flexibility deficits that put an athlete at risk of injury
Assess general health status (e.g., immunizations), fitness, and maturity
Meet insurance or legal requirements
Screen for menstrual dysfunction, stress fractures, or disordered eating (female athlete triad, disordered eating in male athletes)
Introduce athletes to the healthcare system and concepts of preventive medicine
Offer an opportunity to address issues such as recreational and performance-enhancing substance use and abuse, sexuality issues, mental health issues, and health promotional activities (alcohol and drug abuse, seat belts, helmets, and self-breast or self-testicular examination)
The PPPE should be performed at least 6 weeks before the beginning of the sport season to allow adequate time for further evaluation of identified problems and treatment or rehabilitation of any conditions or injuries.
If athletes are unavailable 4–6 weeks before the beginning of an early fall season, examinations performed at the end of the previous school year may be considered. Athletes should report any interval injuries, illnesses, and new medications between their examinations and the beginning of the fall season.
A detailed medical history may be completed by athletes and/or parents in advance, which may improve the accuracy of the information (e.g., immunization records) and examination efficiency. Internet resources can facilitate the history and interval injury reporting process. An electronic format (ideally a national database) has several benefits, including communication and administration of the PPPE.
Variable recommendations depend on individual athletes (i.e., age, gender, sport [single or multiple]; their health [underlying medical conditions or injury history], and cost); availability of records from past PPPEs (continuity of care); and requirements of state, city, or athletic governing body.
General guidelines (no consensus about optimal frequency)
Comprehensive baseline PPPE before initiating a new sport or attaining a new level (e.g., entry into high school, college, or professional level), and every 2–3 years thereafter.
Subsequent annual PPPEs may be limited to injuries or illnesses disclosed by an interim health questionnaire, which focuses on issues associated with heat, head, heart, and mental health; yearly evaluation of the cardiopulmonary system may be appropriate.
If an athlete is participating in multiple sports during the year, consider more frequent evaluations.
Several states require an annual full screening examination (no standard requirements).
The National Collegiate Athletics Association (NCAA) requires an initial comprehensive PPPE on entrance, followed by interim history in the intervening years; limited additional examinations focusing only on new problems.
The American Heart Association (AHA) recommends initial comprehensive PPPE on entrance for high school and college athletes. The AHA recommends another comprehensive PPPE after 2 years for high school athletes and follow-up interim history and blood pressure measurements annually, along with focused additional examinations for new problems for college student athletes.
The American Medical Society for Sports Medicine (AMSSM) emphasizes a shared decision-making process involving the athletes or their legal representatives and clinicians for any potential limitation for initial sports participation or return to play.
Potential advantages: patient-centered, physician–patient familiarity, privacy, and continuity of care
Potential disadvantages: greater cost, limited appointment time, limited physician interest/experience, and lack of communication of pertinent information to school athletic staff
Potential advantages: specialized personnel, time and cost efficiency, and good communication with school athletic staff
| Required Stations | Personnel |
| Sign-in, height and weight (BMI a ), blood pressure, and vision | Ancillary personnel (coach, nurse, and community volunteer) |
| History review, physical examination b , and clearance | Physician |
| Optional Stations | Personnel |
| Nutrition | Dietitian |
| Dental | Dentist |
| Injury evaluation c | Physician |
| Flexibility | Trainer or therapist |
| Body composition | Physiologist |
| Strength | Trainer, coach, therapist, and physiologist |
| Speed, agility, power, balance, and endurance | Trainer, coach, and physiologist |
a Body mass index (BMI) can be calculated from height and weight (for specific age- and gender-adjusted categories, see www.cdc.gov/growthcharts ).
b Physical examination can be subdivided if more than one physician is present.
c A musculoskeletal injury evaluation station may be used to provide a more complete evaluation when a musculoskeletal injury is detected during the required musculoskeletal screening examination.
Potential disadvantages: rushed examinations, lack of privacy, and inadequate follow-up of identified problems
Two types of group PPPEs: multistation (multiple physicians, each at a specialized station) and “locker room” (single or multiple physicians performing complete examinations individually, each in their own area [e.g., locker room]).
At the final station of a station-based examination, an experienced team physician should be available to review all data and to determine clearance or provide appropriate recommendations.
Communication between other primary or consulting physicians, athletic trainers, coaches, and parents may be enhanced by carefully documenting the problems and specific recommendations in the clearance section of the PPPE form.
Cases of special concern may warrant a telephone conversation between the team physician and other involved healthcare providers.
The 2019 Preparticipation Physical Evaluation monograph (see “Recommended Readings”) considers “gymnasium examination” to be inadequate to achieve the goals and objectives of the PPPE process.
PPPEs should be performed by an MD/DO physician, nurse practitioner, or physician assistant, with final clearance by an MD or DO physician.
Regulations by certain states at the high school level allow other practitioners (e.g., chiropractors or naturopathic clinicians) to perform PPPEs.
Primary care physicians perform a majority of PPPEs because of their ability to evaluate all organ (i.e., cardiopulmonary, musculoskeletal, neurologic, ophthalmologic, gastrointestinal, genitourinary, and dermatologic) systems.
Specialists such as orthopedic surgeons, cardiologists, and ophthalmologists or optometrists are key consultants and may be present on site during the screening-station format examination.
Medical staff, including athletic trainers, physical therapists, nurses, exercise scientists, dietitians, and sports psychologists, may be involved, particularly during the screening-station format PPPE.
Nonmedical staff, including coaches, school administrators, and community volunteers, are particularly helpful during the screening-station format PPPE.
There is an emphasis on screening for cardiovascular and musculoskeletal problems, prior head injuries and other neurologic problems, and significant recent illnesses. In addition, prior heat illness, pulmonary problems, medication problems, inadequate immunizations, allergic reactions, skin problems, and menstruation abnormalities and eating disorders in female athletes should be addressed (PPPE: History Form in English and in Spanish available at https://services.aap.org/en/community/aap-councils/council-on-sports-medicine-and-fitness/preparticipation-physical-evaluation; accessed January 2021). The medical history is an essential component of the PPPE that detects abnormalities in a majority of athletes.
Joint completion of history forms by athletes and parents/guardians is recommended when possible, particularly if the athlete is unclear about family or personal history. In addition, the parent/guardian should be present or available during the PPPE for additional questions that may arise. However, athletes should be alone with the provider when questions regarding high-risk behaviors and mental health are addressed.
Cardiovascular history ( Box 3.1 ):
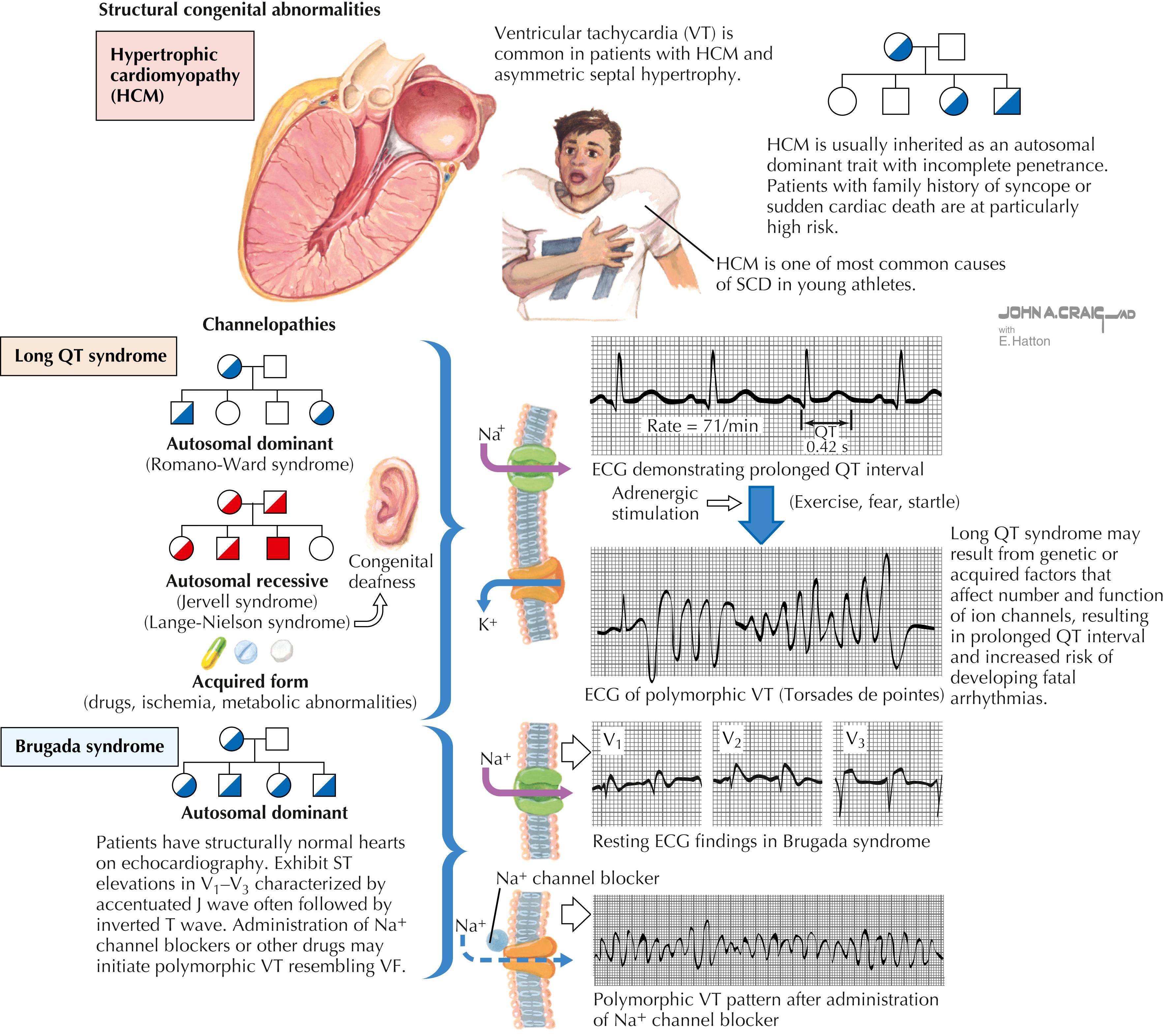
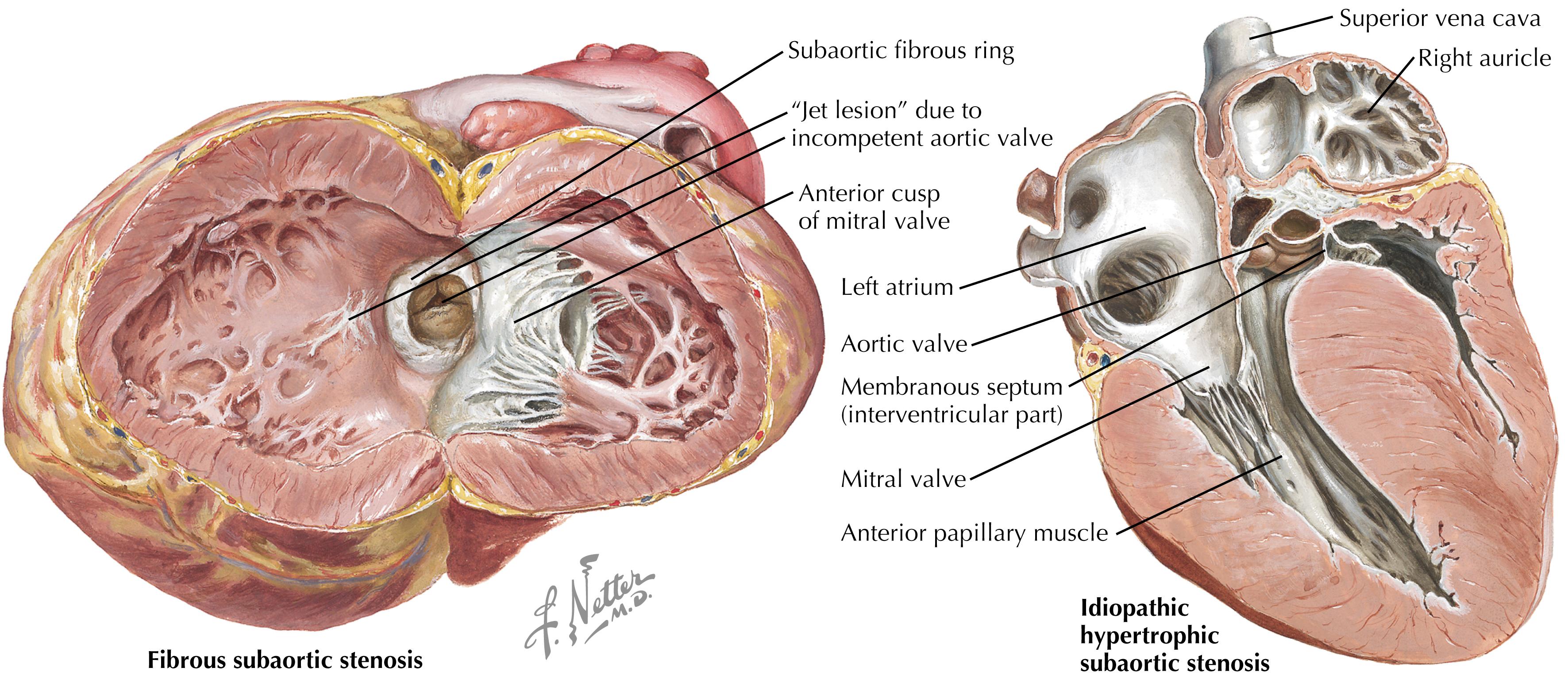
Screen for causes of sudden cardiac death (SCD; Fig. 3.1 ). The most common cause in people aged <35 years is hypertrophic cardiomyopathy (HCM; Fig. 3.2 ); in people aged ≥35 years, the most common cause is coronary artery disease (CAD). The PPPE is scrutinized by certain physicians for its ability to detect underlying causes of SCD, particularly in younger patients. However, the AHA states that a certain form of preparticipation screening for high school and college athletes is justifiable and compelling based on ethical, legal, and medical grounds.
Chest pain/discomfort/tightness/pressure related to exertion
Unexplained syncope/near-syncope a
a Judged not to be neurocardiogenic (vasovagal) in origin; is of particular concern when occurs during or after physical exertion.
Excessive and unexplained dyspnea/fatigue or palpitations associated with exercise
Prior recognition of a heart murmur
Elevated systemic blood pressure
Prior restriction from participation in sports
Prior heart testing ordered by a physician
Premature death (sudden and unexpected or otherwise) in ≥1 relative aged <50 years attributable to heart disease
Disability from heart disease in a close relative aged <50 years
Hypertrophic or dilated cardiomyopathy, long QT syndrome, or other ion channelopathies or Marfan syndrome or clinically significant arrhythmias; specific knowledge of genetic cardiac conditions in family members
Heart murmur b
b Refers to heart murmurs judged likely to be organic and unlikely to be innocent; auscultation should be performed in both supine and standing positions (or with Valsalva maneuver), specifically to identify murmurs of dynamic left ventricular outflow tract obstruction.
Femoral pulses to exclude aortic coarctation
Physical stigmata of Marfan syndrome
Brachial artery blood pressure (sitting position) c
c Preferably taken in both arms.
Personal history is important.
History of exertional chest pain, tightness, or chest pressure; any unexplained syncope or near-syncope; and excessive and unexplained dyspnea/fatigue or palpitations associated with exercise are all significant.
Prior recognition of a heart murmur.
Determine past history of invasive or noninvasive cardiac tests ordered by a physician.
Prior history of hypertension or prehypertension noted during examinations.
Family history is important.
Twenty-five percent of first-degree relatives of patients with HCM exhibit morphologic evidence of HCM in ECG.
Other known genetic cardiac conditions associated with SCD (e.g., long QT syndrome, other ion channelopathies, Marfan syndrome, clinically or significant arrhythmias).
Premature death (sudden and unexpected or otherwise) before 50 years of age attributable to heart disease in ≥1 relative.
Disability from heart disease in close relatives aged <50 years.
Hypertension.
It is important to ask questions about previous head or neck injury, concussion, neurologic symptoms, exercise-related syncope, stingers/burners, and seizure disorder.
The NCAA has a recommended symptom score, cognitive examination, and balance assessment as “best practices” for every athlete as part of his or her baseline physical examination.
Concussion history, including the number, symptoms, and time out of activity, as well as a history for “modifiers” for concussion (e.g., migraine history, learning disability history, or history of depression/anxiety) should be considered as part of the baseline PPPE.
Any positive response mandates a more thorough history, physical examination, and evaluation.
Complete history is essential.
History of previous ligamentous injuries, documentation of surgery, rehabilitation, and time out of play
History of prior advanced imaging (e.g., radiographs, magnetic resonance imaging [MRI], computed tomography [CT], or bone scan) for a musculoskeletal problem
Any positive response mandates careful attention during physical examination, including assessment of ligamentous instability, strength and flexibility deficits/mismatches, and completeness of rehabilitation, as well as consideration for obtaining medical records related to the evaluation.
If an athlete has had prior surgery, obtain medical records related to the evaluation and a documentation that the operating surgeon has cleared the athlete to return to competition and/or determine the athlete’s rehabilitation status.
Heat exhaustion/illness
Infectious mononucleosis
Hepatitis
HIV disease
Diabetes
Sickle cell disease/hemoglobinopathy
Asthma
Allergic reactions
Kawasaki disease
Menstrual history:
Age of menarche
Date of last menstrual period
Number of periods in the past 12 months
Bone health history:
History of stress fractures
History of bone injuries
Risk factors for osteoporosis
Nutrition history and risk factors for disordered eating:
Discrepancies between ideal versus current body weight
Body image concerns
Pathologic eating behaviors
Additional concerns not always included on the PPPE form may be addressed on an individual basis. If you do not ask, you might never find out.
Nutritional issues: fluids, game-day nutrition, and general nutrition
Supplements and performance-enhancing agents
Sexuality concerns: pregnancy, sexually transmitted diseases, and sexual orientation (best addressed in a private setting)
Recreational drugs and alcohol use
Preventive medicine (e.g., seat belts, helmets, self-breast or self-testicular examination, cholesterol screening, and gynecologic examinations/Pap smear)
Mental health and psychosocial issues: stress management, anxiety, depression, suicide (consider including screening questionnaires such as the Patient Health Questionnaire-9 [PHQ-9] or Generalized Anxiety Disorder-7 [GAD-7] for depression and anxiety, respectively)
The physical examination should be comprehensive. It should focus on areas of greatest importance in sports participation and address any problems uncovered while recording an athlete’s history.
Height
Weight
Eyes: visual acuity and pupil size
Oral cavity
Ears
Nose
Lungs
Cardiovascular system: blood pressure; femoral and radial pulses; and heart rate, rhythm, and murmurs
Abdomen: masses, tenderness, and organomegaly
Skin: rashes and lesions (infectious)
Musculoskeletal system: contour; range of motion; and symmetry of neck, back, shoulder/arm, elbow/forearm, wrist/hand, hip/thigh, knee, leg/ankle, and foot
Adequate exposure during the examination is important.
The physical examination form (PPPE: Physical Examination Form available at https://downloads.aap.org/AAP/PDF/PPE-Physical-Examination-Form.pdf , copyright 2019, accessed January 2021) is generally comprehensive and covers the scope of such examination, but it should not limit the clinician if additional examination is deemed pertinent.
In athletes with excessive weight change, explore the possibility of eating disorders or steroid abuse.
Body mass index (BMI) should be calculated (gender and age specific; see www.cdc.gov/growthcharts ). Understand the indications and limitations of using BMI.
Underweight (<5th percentile)
Overweight (85th–94th percentile)
Obese (≥95th percentile)
Optical examination is important: check visual acuity in all athletes, pupils for anisocoria, conjunctiva for anemia.
Certain athletes may have a predilection for ear issues (e.g., swimmers [otitis externa], scuba divers [otic barotrauma], and wrestlers [auricular hematoma]).
Allergy sufferers and athletes with history of nose trauma need nasopharyngeal examinations.
Smokeless tobacco users need oropharyngeal examinations.
A cardiovascular assessment is essential for both the initial PPPE and annual reevaluations (see Box 3.2 ).
Brachial artery blood pressure measurement (with appropriate cuff size and ideally in both arms): if elevated, recheck after the athlete rests quietly for 15 minutes and later, if needed ( Table 3.2 ). The following are blood pressure categorizations for children and adolescents according to the 2017 American Academy of Pediatrics (AAP) guidelines.
| Age and Phase | 90th–94th Percentile b High Normal a Prehypertensive c |
95th–99th Percentile b Significant HTN a Stage 1 HTN c |
>99th Percentile b Severe HTN a Stage 2 HTN c |
|---|---|---|---|
| 6–9 yr | |||
| Systolic b | 104–121 | 108–129 | >115–129 |
| Diastolic b | 68–81 | 72–89 | >83–89 |
| 10–12 yr | |||
| Systolic b | 112–127 | 116–135 | >123–135 |
| Diastolic b | 73–83 | 77–91 | >84–91 |
| 13–15 yr | |||
| Systolic b | 117–135 | 121–142 | >128–142 |
| Diastolic b | 76–85 | 80–93 | >87–93 |
| 16–17 yr | |||
| Systolic b | 121–140 | 125–147 | >132–147 |
| Diastolic b | 78–89 | 82–97 | >90–97 |
| ≥18 yr | |||
| Systolic c | 120–139 | 140–159 | ≥160 |
| Diastolic c | 80–89 | 90–99 | ≥100 |
a American Academy of Pediatrics, Task Force on Blood Pressure in Children. Report of the Second Task Force Control on Blood Pressure in Children—1987. Pediatrics . 1987;79:1-25. Updated in 1996;98(4 Pt 1):649-658.
b The blood pressure range is obtained from the Fourth Report on the Diagnosis, Evaluation, and Treatment of High Blood Pressure in Children and Adolescents . For specific blood pressure levels by age, gender, and height, see http://www.nhlbi.nih.gov/files/docs/guidelines/child_tbl.pdf .
c From the Seventh Report of the Joint National Committee on Detection, Evaluation, and Treatment of High Blood Pressure , 2003.
Classification categories of hypertension in children aged 1–13 years old:
Normal (<90th percentile for age, sex, and height)
Elevated blood pressure (≥90th but <95th percentile for age, sex, and height or 120/80 mmHg to <95th percentile, whichever is lower)
Stage 1 hypertension (≥95th percentile for age, sex, and height to <95th percentile + 12 mmHg or 130/80 to 139/89 mmHg, whichever is lower)
Stage 2 hypertension (≥95th percentile for age, sex, and height + 12 mmHg or ≥140/90 mmHg, whichever is lower)
Classification categories of hypertension in children aged ≥13 years old:
Normal (<120/80 mmHg)
Elevated blood pressure (systolic blood pressure [SBP] between 120 and 129 with diastolic blood pressure [DBP] <80 mmHg)
Stage 1 hypertension (130/80 to 139/89 mmHg)
Stage 2 hypertension (blood pressure ≥140/90 mmHg)
Palpate radial and femoral pulses:
Decreased or nonpalpable femoral pulses should raise suspicion for coarctation of the aorta.
Irregular pulse should raise suspicion for arrhythmia and requires ECG evaluation.
Heart auscultation in supine and standing positions: note the presence and character of any murmurs
HCM murmur: systolic murmur heard best at lower left sternal border in the standing position; increases with maneuvers that decrease venous return to the heart
Provocative maneuvers help differentiate functional murmurs from pathologic murmurs.
To decrease venous return: Valsalva maneuver and squat-to-stand
To increase venous return: deep inspiration, stand-to-squat, and isometric hand grip
General recommendations for murmurs requiring further evaluation before the athlete can participate:
Any systolic murmur grade ≥III/VI in severity
Any diastolic murmur
Any murmur that gets louder with Valsalva maneuver
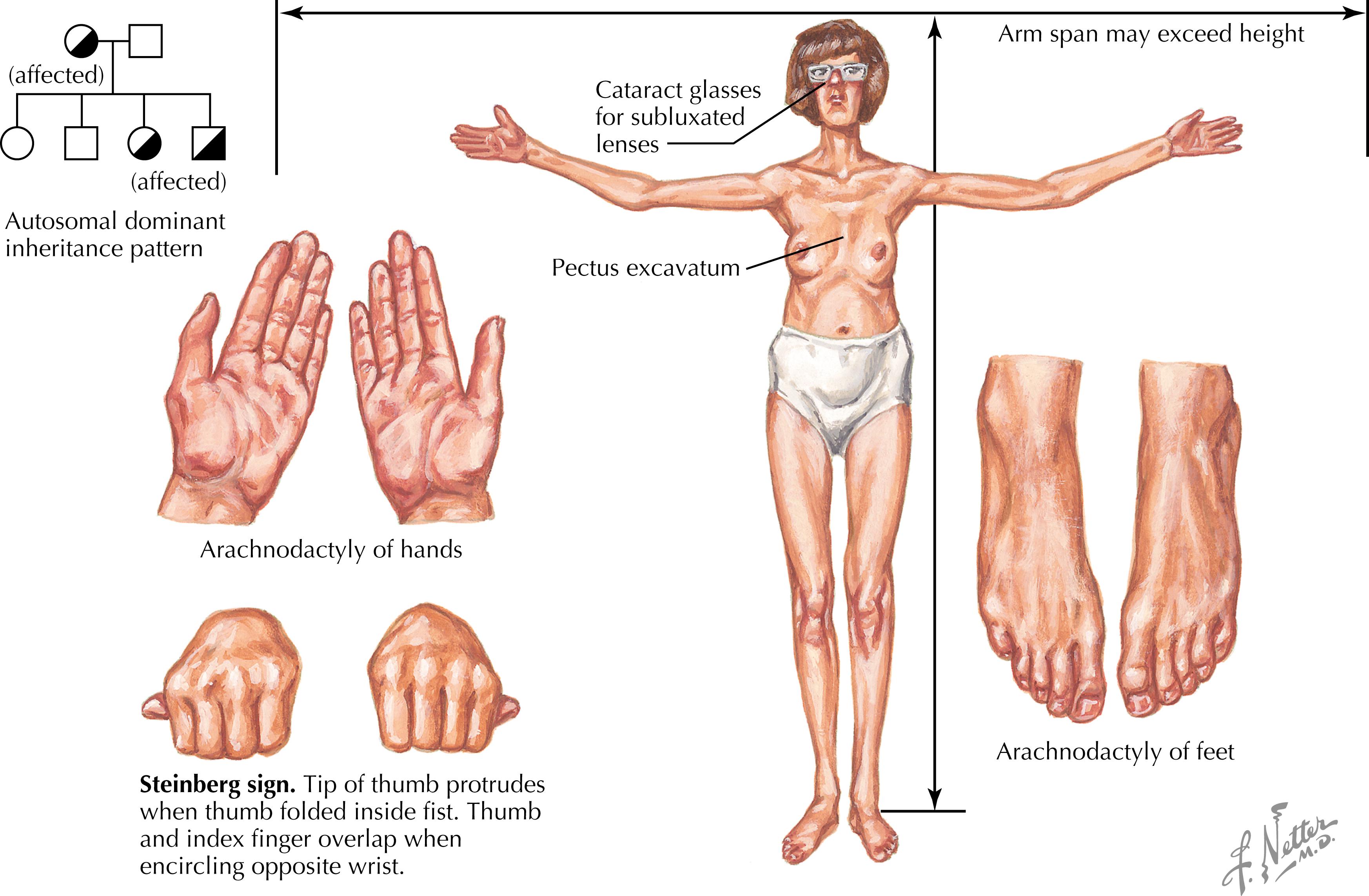
Marfan syndrome stigmata ( Fig. 3.3 ): Tall stature, arachnodactyly, kyphoscoliosis, anterior chest deformity, arm span greater than height, decreased upper body length to lower body length ratio, heart murmur or midsystolic click, ectopic lens, thumb sign (the thumbs protrude from the clenched fists), wrist sign (the distal phalanges of the first and fifth digits of one hand overlap when wrapped around the opposite wrist), and family history of Marfan syndrome
Focus on detecting abnormal breath sounds: wheezes, crackles, rubs, and abnormal inspiratory to expiratory ratio
Asthma screening (e.g., exercise challenge test) has been suggested but is impractical in most preparticipation settings.
Should be performed with athlete in the supine position. Examples of problems requiring further evaluation before participation include organomegaly (liver and spleen), masses, bruits, tenderness, and/or rigidity and possible pregnancy in females.
Male: Per the fifth PPPE Monograph. Indications for performing the male genital examination include history of groin pain, inguinal bulge, possible testicular lump, or possible undescended testicle. If warranted by history or other findings, examine in a private setting. Chaperones may be present during this part of the examination per patient and/or provider preference.
Female: routine examination is not recommended; if warranted by history or other findings, examine in a private setting.
Tanner staging is no longer recommended in PPPE monograph as a standard element; however, it may be useful for counseling on growth and development and anabolic steroid use.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here