Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Football developed in the United States, in what is commonly recognized as the first American football game between Rutgers and Princeton, on November 6, 1869.
Since its inception, over 1.5 million athletes participate today and contribute to football being considered the most popular sport in the United States.
There are well over 700 schools sponsoring varsity college football, which represent approximately 70,000 student-athletes involved in the sport.
The flying wedge was a V-shaped formation used by Harvard in a game against Yale in 1892 and was thought to be associated with significant brutality and injuries. This technique was banned in 1894, just 2 years later.
Years later, the National Collegiate Athletic Association (NCAA) was formed because of rising concerns of significant injuries associated with the sport.
There are different objectives for each team depending on which portion of their team is on the field. Offensively, the objective is to move the ball down the field and score. Defensively, the objective is to prevent the offense from doing so.
There are four “downs” per possession, each with the goal of moving the ball a minimum of 10 yards to acquire another set of “downs.”
Teams score by either moving the ball past the goal line (touchdown) or by kicking the ball through the goal post (field goal). The former is worth 6 points, and the latter is worth 3. After a touchdown, teams can opt for an additional point by kicking a point-after-touchdown (pat) or crossing the goal line again for a 2-point conversion.
Different rules regarding the length of the game, overtime, and possession are determined by the level of play (high school, college, and professional).
Football is a high-velocity collision sport with an increased risk of injury. Proper strength and conditioning are necessary to minimize injury.
All players, regardless of position, should maintain a good level of flexibility in conjunction with overall body strength.
Specific drills should be implemented based on the player’s position, but endurance work should also be emphasized as the foundation.
Explosive speed is needed and can be obtained by interval training, stair/stadium running, and hill training.
Increases in lean body mass by means of supervised weight-training programs are recommended.
The athlete should be counseled on the basic understanding of nutritional balance and their own specific needs based on their goals and the requirements of their position.
A healthy, natural, well-balanced diet should be emphasized. (See Chapter 5 : “Sports Nutrition.”)
The need for strength/weight gain often puts athletes at risk of potential abuse of performance-enhancing supplements. Therefore, the use of unsupervised nutraceuticals should be discouraged.
Fluids: A study in high school football players in a 50-play simulation scrimmage found no difference in aerobic performance with a 7% glucose polymer beverage containing electrolytes compared with water, but the beverage had a positive effect on maintaining plasma volume during recovery.
Purpose of the helmet is to prevent traumatic skull fractures.
Must meet National Operating Committee on Standards for Athletic Equipment (NOCSAE) specifications.
Construction
Outer shell is made of polymer plastic that is both lightweight and able to withstand high impact.
It is imperative to check for cracks in outer shell, as this can lead to loss of protection from the entire unit.
Inner shell is composed of padding, air/fluid-filled cells, or a combination of cells and pads.
Air cells can be inflated or deflated to provide a better fit.
Must check for leaks in the inner shell to prevent protective compromise.
Helmet fitting
Helmet should be donned by grasping ear holes and pulling apart with thumbs. Helmet should have minimal sliding/turning during rotation of the athlete’s head.
There should be no space between jaw pads and face or back of head.
There should be one to two fingerbreadths between bottom of forehead pad and athlete’s eyebrows. Helmet should not cover eyes when downward pressure is applied to the top of the helmet.
Base of skull should be fully covered, but helmet should not impinge on cervical spine with full neck extension.
Helmet should have NOCSAE label on outer shell warning of potential head or spine injury with inappropriate helmet size.
Hair should be the same length at time of fitting as it will be throughout the season. Long hair should be wet when fitting to simulate sweaty conditions.
Chin strap (four-point more secure than two-point) helps prevent forward and backward rocking of the helmet. These should always be appropriately fitted and secured during competition.
A plethora of face masks are available and are generally position-dependent. Ball carriers require masks that provide protection but are open enough to allow clear vision. Lineman require masks that provide additional protection from eye and facial injuries.
Helmet visors, made of clear plexiglass, are also available for those seeking additional eye protection. Tinted visors, of the same material, can be worn by players needing special assistance for elimination of sun because of a medical condition. They require a physician’s approval, and use is determined at the time of play by officiating staff.
Mouth guards (required in high school and college) can be custom-made, formed by the mouth with heating, or obtained in standard sizes. They help dissipate blows to the chin, reducing intraoral and mandible injuries.
Two standard types of shoulder pads: cantilever and noncantilever (flat) pads.
Noncantilever pads are worn by those with positions that have a greater need for glenohumeral circumduction (quarterbacks, receivers, kickers).
Cantilever pads are worn by those in positions that require constant contact, thus needing additional protection (lineman and linebackers).
Modifications can be made to pads depending on position and preference (e.g., linebackers hit from a standing position so pads can be slightly tilted forward and larger anteriorly).
Appropriate fitting can be done by measuring from acromioclavicular (AC) joint to AC joint and comparing with manufacturer’s size chart.
Neck opening should be large enough to prevent impingement when lifting arm overhead, but not so large that excessive sliding occurs.
Lateral aspect of pad should be just lateral to the shoulder, with epaulets large enough to cover the deltoid region.
Axilla straps should be adjusted snugly, but comfortably, to distribute impact across the entire chest area of pads.
When laced, anterior pads should meet but not overlap.
Bottom of chest plate and posterior plate should end just below the nipple line anteriorly and 1 cm below the scapula posteriorly, respectively.
Standard equipment
Hip pads are used to protect iliac crest and tailbone from injury.
Thigh and knee pads are inserted into the pants. These should fit snug and not allow easy slippage. These pads have become smaller in size over the past decade and often do not cover much of the anterior knee or thigh.
Special equipment
Neck rolls and collars are frequently used by players who have experienced “stingers” or those who seek prevention from this. The efficacy in these for prevention remains debatable. Neck rolls in high school are often ineffective because of inappropriate fit of shoulder pads.
Shoulder restraint harnesses restrict abduction and external rotation in chronic shoulder dislocations. The downside is that these devices may affect the capabilities of the athlete in several positions.
Padded gloves and upper extremity accessories are worn to prevent finger injuries, contusions, and myositis ossificans.
Flak jackets are commonly worn by quarterbacks to prevent rib injuries.
Mandatory knee bracing is not recommended for prophylactic prevention of knee injuries.
At the college level, in a report published by the Centers for Disease Control and Prevention (CDC) reviewing sport-related injuries from 2009 to 2014, football accounted for the largest annual estimated number of injuries per year, the highest competition injury rate (39.9 per 1000 athlete-exposures [AEs]), and the third highest overall injury rate (9.2 per 1000) ( Table 66.1 ). Football also accounts for the largest proportion of injuries requiring >7 days before return to full participation (26.2%), surgery (40.2%), or emergency transport (31.9%).
| Sport | Practice | Game |
|---|---|---|
| Football | 5.8 | 39.9 |
| Wrestling | 9.0 | 38.5 |
| Men’s Ice Hockey | 3.2 | 26.3 |
| Men’s Soccer | 5.2 | 17.9 |
| Women’s Soccer | 5.3 | 17.2 |
| Men’s Basketball | 5.8 | 15.0 |
| Men’s Lacrosse | 4.9 | 13.7 |
| Women’s Gymnastics | 2.9 | 13.2 |
| Women’s Ice Hockey | 3.2 | 11.2 |
| Women’s Field Hockey | 5.1 | 10.5 |
| Women’s Basketball | 4.9 | 10.4 |
| Men’s Tennis | 2.9 | 10.0 |
| Women’s Lacrosse | 4.2 | 9.7 |
| Women’s Cross-Country | 3.4 | 7.7 |
| Women’s Tennis | 3.1 | 7.6 |
| Men’s Baseball | 3.0 | 6.8 |
| Men’s Indoor Track | 3.1 | 6.5 |
| Women’s Softball | 3.5 | 5.9 |
| Women’s Volleyball | 5.6 | 5.9 |
| Men’s Outdoor Track | 2.3 | 5.4 |
| Men’s Cross-Country | 3.2 | 5.2 |
| Women’s Outdoor Track | 2.7 | 5.1 |
| Women’s Indoor Track | 3.8 | 4.4 |
| Men’s Swimming and Diving | 2.1 | 2.0 |
| Women’s Swimming and Diving | 2.1 | 1.9 |
Between 1988–1989 and 2003–2004, preseason injury rates were higher than both in-season and postseason injury rates (7.05 vs. 2.02 and 7.05 vs. 1.70 per 1000 AEs, respectively). Preseason, therefore, is a critical time to emphasize appropriate warmups, fluid and nutrition replacement, technique, stretching, and recovery.
Internal knee derangements, ankle sprains, and concussion account for most injuries in games (17.8%, 15.6%, and 6.8%, respectively).
Internal knee derangements, ankle sprains, and upper leg muscular injuries account for most injuries in practice (12%, 11.8%, and 10.7%, respectively).
Cervical spine injuries can have catastrophic potential, but the prevalence has decreased since the induction of rule modifications, improved athlete fitness, and substantial equipment upgrades.
Direct player-to-player contact is the most common mechanism for injury in football. This holds true regardless of competitive environment (practice, scrimmage, or games).
Player position plays a factor in the likelihood of injury. Running backs are the most injured position during games (19.6%), followed by quarterbacks (17.5%), linebackers (15.5%), wide receivers (14.4%), defensive backs (11.7%), defensive linemen (11.3%), then offensive linemen (9.9%).
Fatalities have been reported in both high school and collegiate football players. From 1990 to 2010, 243 fatalities were reported to the National Center for Catastrophic Sports Injury Research. Of these 243, 164 were indirectly related and 79 were related. The most common causes of fatalities in the review were cardiac failure (41.2%), brain injury (25.5%), heat illness (15.6%), sickle cell trait (4.5%), asthma and commotio cordis (2.9%), blood clot (2.1%), and cervical fracture (1.7%). Intra-abdominal injury, infection, and lighting completed the remaining causes, each accounting for 1.2%.
This section will describe various common injuries encountered in the sport of football. The treatment and return to play for many of the musculoskeletal conditions may vary by the position that the athlete plays on the football field. A right thumb injury to an offensive lineman can likely be treated differently than the same injury in a quarterback’s throwing hand, and the injury will affect the athlete with a much different level of significance. In this example, the lineman might be able to return to the same game in a cast, whereas the quarterback might take several weeks to return, as their ability to hold a football is severely affected. Thus, the treatment and return to play of many of the conditions need to be evaluated on an individual and position-specific basis.
Description: A transient change in neurologic function secondary to an acute force being applied to the head and/or neck. In sports, a concussion is usually the most common form of a traumatic brain injury. Football has a high rate of head injuries as monitored at the collegiate level ( Table 66.2 ).
| Concussion a | |||
| Game | Practice | Overall | |
| Sports With No Head Protection | |||
| Field hockey | 11.10 | 1.77 | 4.02 |
| Women’s lacrosse | 13.08 | 3.30 | 5.21 |
| Men’s soccer | 9.69 | 1.75 | 3.44 |
| Women’s soccer | 19.38 | 2.14 | 6.31 |
| Women’s basketball | 10.92 | 4.43 | 5.95 |
| Men’s basketball | 5.6 | 3.42 | 3.89 |
| Wrestling | 55.46 | 5.68 | 10.92 |
| Sports With Head Protection | |||
| Men’s ice hockey | 24.89 | 2.51 | 7.91 |
| Football | 30.07 | 4.20 | 6.71 |
| Women’s ice hockey | 20.10 | 3.00 | 7.50 |
| Men’s lacrosse | 9.31 | 1.95 | 3.18 |
| Women’s softball | 5.61 | 1.75 | 3.28 |
| Baseball | 1.20 | 0.72 | 0.90 |
a Concussion as a subset of all head injuries; rates are per 10,000 athlete-exposures.
History: In football, player-to-player contact is the primary mechanism of action. A forceful blow to the head by another person or solid object (turf, goalpost, benches) elicits axonal damage and neurotransmitter release, leading to direct brain injury and concussive symptoms. Other mechanisms for concussion would be a “whiplash” injury to the cervical spine.
Physical examination: Acutely, primary evaluation of the athlete should ensue, taking into careful consideration the ABCs of emergency management (Airway, Breathing, Circulation). Secondary assessment once the player is off the field would consist of neurocognitive testing with a Standardized Concussion Assessment Tool (SCAT5).
Diagnostic considerations: Usually not necessary for concussion. If concerns for neurologic deterioration exist, emergent Computed Tomography (CT) should be obtained to rule out cerebral hemorrhage.
Treatment: Rest until asymptomatic. Postconcussion complications are discussed in Chapter 45 .
Return to play: If there are concerns for concussion, the athlete should be promptly removed from the field of play. General agreed-upon consensus is that no athlete should be allowed to resume play on the same day that a concussion has been suffered. Graded return to activity based on symptom severity has been used to assist athletes in obtaining level of function before injury. Special consideration should be measured with football players and specific positions. Graded return to play may be earlier for sport-specific drills in noncontact positions (quarterbacks, kickers, punters) than in contact positions (defensive linemen, offensive linemen, running backs).
Prevention: Efforts have been made throughout collegiate and professional levels to reduce the number of concussions obtained. In 1976, spearing became officially banned in football, with the goal of reducing brain trauma and catastrophic cervical injuries. Head-to-head injuries remained after the rule change, and in 2008 officials were able to label these as fouls. The NCAA (Safety in College Football Summit) and the NFL Foundations, USA Football (HeadsUpFootball) have made strides to decrease the amount of contact exposures, increase education about proper tackling mechanics, and have a formal concussion plan in place that brings the signs and symptoms of a concussion to the forefront.
Description: Musculotendinous injury to the cervical spine. Typically, the most common form of neck injury.
History: Athlete will present with paravertebral pain with or without spasm, depending on acuity, and decreased range of motion. Radicular and neurologic symptoms are usually absent.
Physical examination: Decreased range of motion on the contralateral side to the soft tissue injury (inability to side-bend head to the left or rotate the head to the left would indicate a cervical strain to the posterior right paravertebral muscles). Hypertonic paravertebral muscles would be palpable, with tenderness to palpation of the same soft tissue region.
Diagnostic considerations: Usually not indicated unless noticeable midline tenderness or bony prominence, feelings of instability from the athlete, or neurologic deficits associated. If necessary, plain radiographs should be used to rule out instability or fracture.
Treatment: Nonsteroidal anti-inflammatory drugs (NSAIDs), rest, and physical therapy using soft tissue treatment and stretching.
Return to play: Full, unrestricted range of motion without pain. Normal posture, physical examination, and absence of neurologic deficits should be obtained before returning to competition.
Prevention: Typically acute in nature. Maintain proper conditioning and posture. Thorough warm-up before intense practice or competition.
Description: Typically occurs from acute traumatic distraction of the neck or shoulder, leading to stretching or pinching of the brachial plexus.
History: Can be seen from a player landing on the superior aspect of the shoulder or from a direct blow to the side of the helmet leading to excessive side-bending of the cervical spine. Athlete will present with electric shocklike radiating pain from neck to arm. May also experience numbness or paralysis in the affected extremity. Careful consideration should be taken for bilateral symptoms, as this could be suggestive of transient quadriparesis.
Physical examination: Athlete may hold arm adducted and flexed, close to body. May also notice athlete “shaking” arm in attempt to regain sensation or correct paresthesia. Full neurologic assessment for strength and sensation should take place to isolate nerve root affected.
Diagnostic considerations: Usually not necessary unless recurrent, physical examination yields bony tenderness, or symptoms are bilateral. Plain radiographs should be the test of choice if these symptoms are present.
Treatment: NSAIDs, rest, and physical therapy focusing on stretching hypertonic neck muscles and strengthening the same muscles that may have been weakened during the injury.
Return to play: Once full strength and resolution of neurologic symptoms have been obtained. Athlete should be reexamined 24 hours after injury because of phenomenon of delayed weakness.
Prevention: Protective equipment with a neck roll or soft collar. Shoulder pads must be well-fitting, as loose pads diminish the effect of the neck roll.
Description: Fracture of either the spinous process or transverse process of the cervical vertebrae.
History: Less frequent since “spearing” has been removed. Can still inadvertently happen with secondary hyperflexion and compression of the cervical spine, as seen when one player encounters another by using the crown of the helmet.
Physical examination: Athlete will have pain in the neck, noticeably worse with cervical flexion. Assess for neurologic injury!
Diagnostic considerations: Imaging needed. Plain radiographs AFTER immobilization and transfer. Magnetic Resonance Imaging (MRI) if neurologic symptoms.
Treatment: Removal from play. Immobilization of the spine must be obtained. Pads and helmet should not be removed until spine is immobilized. Face mask should be cut if airway management is necessary. Be aware of emergency action plan and emergency personnel guidelines.
Return to play:
Absolute contraindications for return to collision sports
Any C1–C2 injury with ligamentous instability or fusion
Unstable ligamentous injuries to C2–C7
Vertebral body fractures with displacement into the spinal canal
Healed fractures with residual instability
Disc herniation with neurologic findings or limited motion
Postoperative fusion of more than three levels
Relative contraindications for return to collision sports
Full, pain-free range of motion without neurologic deficits with a healed vertebral body compression fracture or neural ring fracture
Postoperative fusion of two to three levels
No contraindication for return to collision sports
Full, pain-free range of motion without neurologic deficits and a healed, stable compression fracture of spinous process
Postoperative fusion of one level after a discectomy of a vertebrae at or higher than C3
Description: Fracture to the clavicle from direct or indirect trauma. Roughly 90% occur in the middle third of the clavicle.
History: Most common from a direct blow to the clavicle. Also occurs while falling directly on to lateral aspect of shoulder with an adducted arm.
Physical examination: Bruising and tenderness to palpation over the clavicle. If severe enough, may notice tenting of the overlying skin.
Diagnostic considerations: Plain radiographs should be obtained.
Treatment: Majority can be treated nonsurgically with arm sling and immobilization. If fragments are overlapping >1.5 cm (Bayonet deformity), surgical fixation is recommended.
Return to play: Faster healing time and return to play with surgical fixation, usually 8–12 weeks. Athlete should have full range of motion, strength, and imaging evidence of healed fracture.
Prevention: Sudden injury without much anticipation. Ensuring athletes are wearing all proper protective equipment is first line.
Description: Referred to as grade I and II AC strains. Coracoclavicular ligaments may be intact or sprained without disruption. (See Chapter 49 : “Shoulder Injuries.”)
History: Most commonly results from fall onto the point of the shoulder ( Fig. 66.1 ).
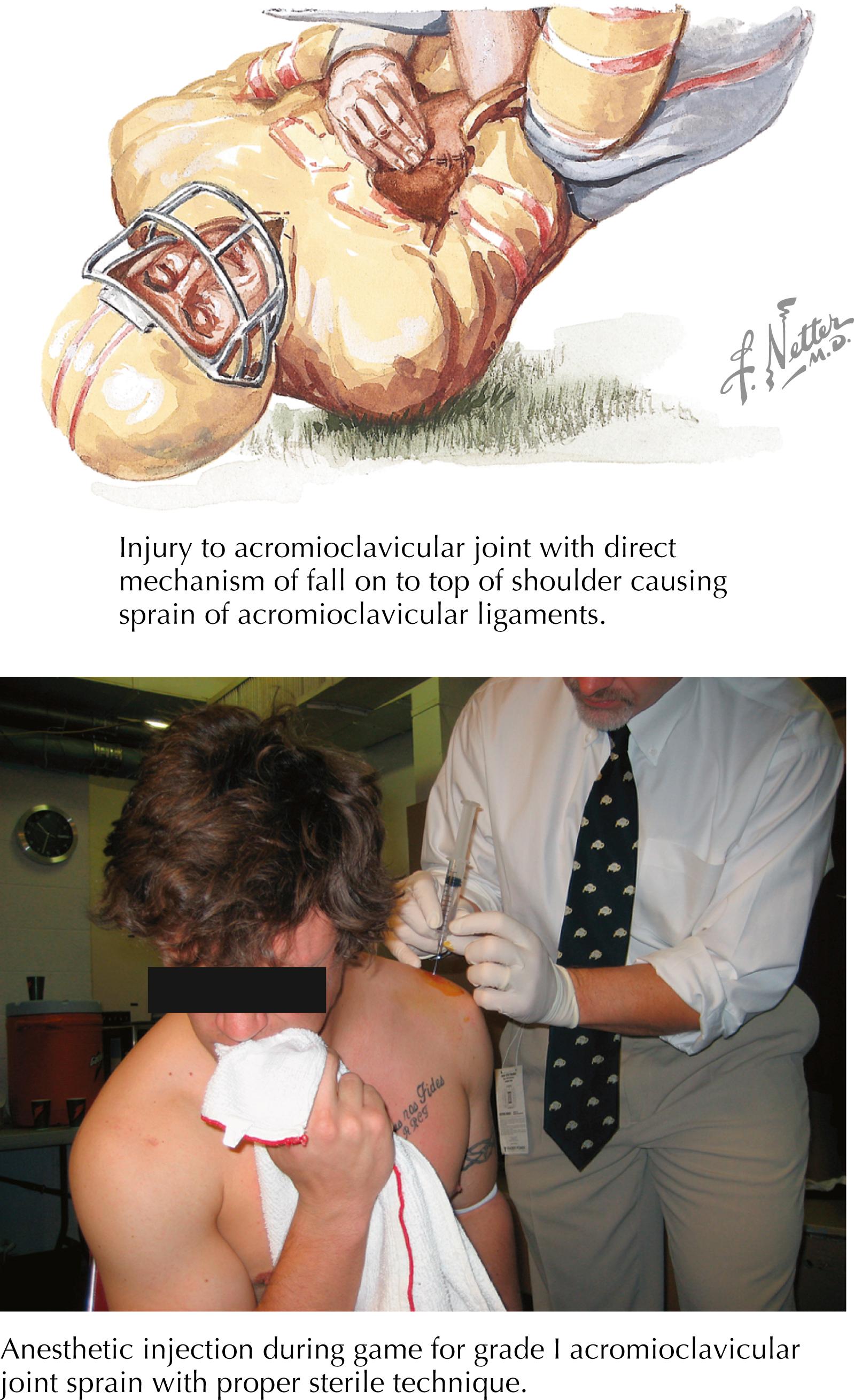
Physical examination: Athlete will have tenderness over AC joint. Will notice pain with cross-body test (resisted adduction of arm across the chest).
Diagnostic considerations: Plain radiographs with weight in arm to distinguish grade III from grade IV.
Treatment: Conservative therapy with rest, ice, compression, and elevation (RICE). Physical therapy also beneficial.
Return to play: After full strength and range of motion have been obtained. Pain tolerance is a key factor in regaining strength and motion and then returning to play. Pain tolerance is variable across all athletes. AC padding after restoration of strength. In resolving semiacute phase, local anesthetic injection can be used judiciously to allow in-game return or to enable play.
Prevention: Sudden and unexpected. Ensure athletes are wearing all properly fitted protective equipment.
Description: Referred to as grade III–grade VI AC sprains. Coracoclavicular ligaments are disrupted. (See Chapter 49 : “Shoulder Injuries.”)
History: Same mechanisms of action as incomplete AC joint separations.
Physical examination: Tenderness at AC joint. Palpable step-off between clavicle and acromion.
Diagnostic considerations: Plain radiographs.
Treatment: Grade III separations are controversial. Unless extensive muscle injury present or distal clavicle has penetrated the trapezius, conservative measures are appropriate. Grade IV–VI separations require surgical fixation.
Return to play: Once athlete has full restoration of strength and motion. Again, as in incomplete AC separations, pain tolerance will be a factor in return to play. AC padding should take place with return.
Prevention: Sudden and unexpected. Ensure athletes are wearing all properly fitted protective equipment.
Description (common football injury usually seen as either anterior or posterior):
Anterior: Most common secondary to abduction/external rotation force; can result from inappropriate tackling technique.
Posterior: Traumatic posterior dislocation is uncommon. However, instability/labral tears are common in offensive linemen.
History:
Anterior: Occurs secondary to a fall on an outstretched hand. Also can happen when an athlete lunges for a tackle with the arm abducted forcibly.
Posterior: Athlete will have pain in posterior shoulder after arms have been extended forward and presented with a direct posterior force (offensive lineman when blocking or an athlete performing a heavy bench press), leading to posterior displacement of the shoulder.
Physical examination:
Anterior: Athlete will have a prominence in the anterior of the shoulder. Arm will be visibly held in abduction and external rotation, with limited internal rotation. Be sure to assess neurovascular function.
Posterior: Athlete will visibly hold arm in adducted, internally rotated position with lack of external rotation. Palpation of an anterior prominent coracoid. Posterior jerk test will reproduce symptoms.
Diagnostic considerations:
Anterior: Plain radiographs to evaluate for reduction, Hill–Sachs, or Bankart lesions. MRI recommended to evaluate extent of cartilage injury.
Posterior: Plain radiographs are needed to avoid a missed diagnosis.
Treatment:
Anterior: On field, acute injury can be treated by experienced physician using gentle reduction. Early rehabilitation is important. Immobilization after acute injury is controversial. Bracing can control external rotation/abduction movement and allow earlier return to play ( Fig. 66.2 ). Neither immobilization nor therapy has been shown to decrease the redislocation rate in young people. Arthroscopic stabilization has been shown to decrease the dislocation rate, but decision-making on surgery is case-dependent. Factors include timing, risk factors, and career goals.
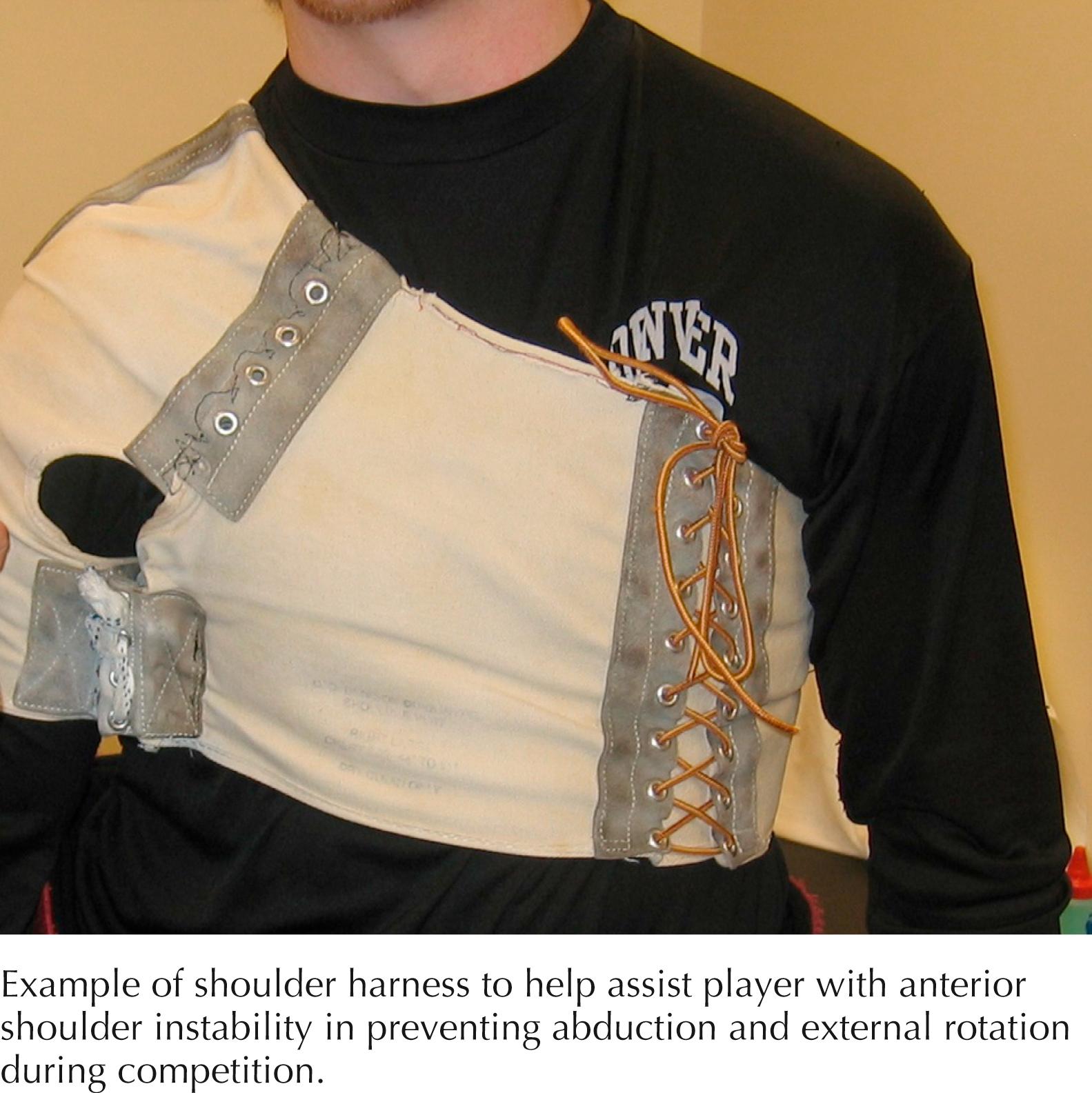
Posterior: Should consist of rehabilitation. There is no bracing that can control a posterior-directed force on the shoulder. If athlete remains symptomatic, then surgical stabilization is the treatment of choice. Usually a labral tear is associated, and players have been shown to have a successful return to football after surgery.
Return to play: Once athlete has regained full strength and range of motion with minimal apprehension, but little evidence exists for a formal recommendation as to return criteria. Athletes with previous instability episodes have a high rate of recurrence.
Prevention: Sudden and unexpected on first attempt. Educate on proper tackling technique. Surgical referral for episodes of repeat instability.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here