Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The incidence of tendon ruptures after distal radius fracture is rare, currently 1%–3%, and generally occur within the first year after surgery. The extensor pollicis longus (EPL) or flexor pollicis longus (FPL) are most often involved tendons, and rupture of flexor or extensor tendons to the fingers were also reported.
The key to prevent flexor tendon rupture is to properly position the plate, and Soong classification offers practical guide to ideal plate position.
The key to prevent extensor tendon rupture is to avoid too long screws that dorsally protrude. The dorsal tangential/horizon/skyline or carpal shoot-through view offers a reliable verification intraoperatively, and/or a CT scan, postoperatively.
Once clinical diagnosis is established, surgical exploration should proceed and hardware should be removed before proceeding to tendon reconstruction.
Tendon transfer or grafting are two common option of surgical treatment and prognosis of these surgeries are believed to be reliable in achieving a satisfactory result.
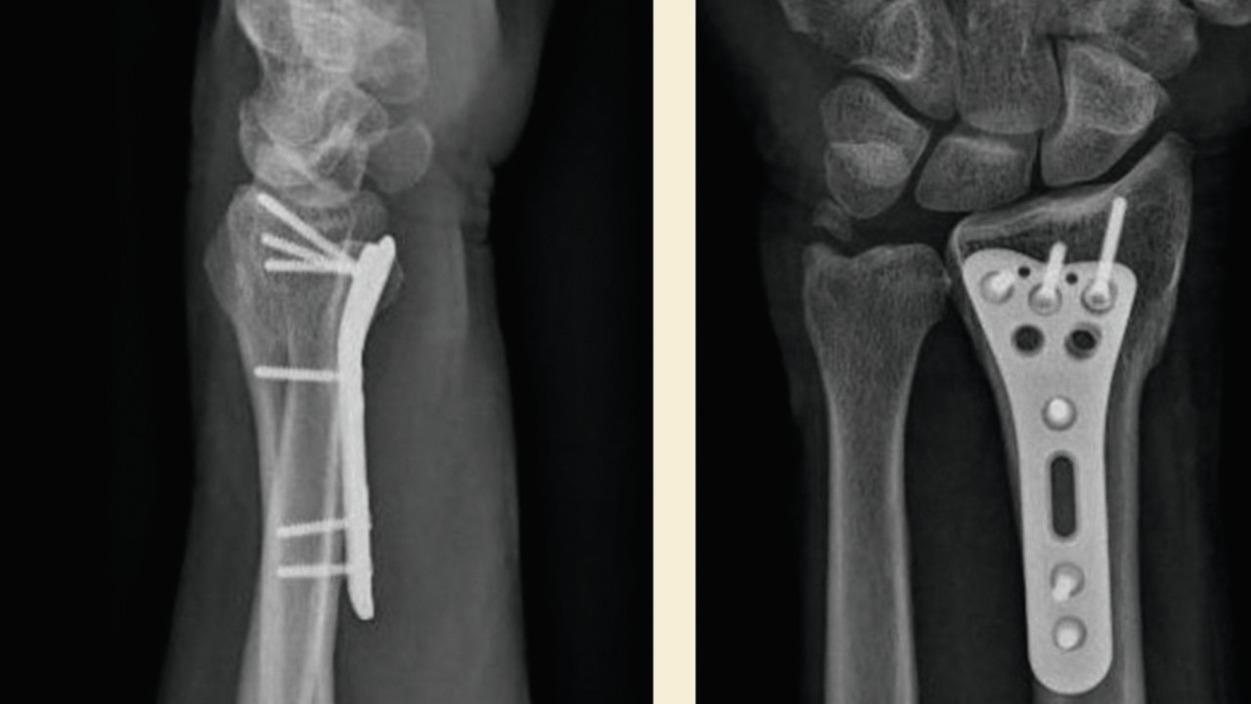
A 63 year-old, right hand dominant male presents with a spontaneous inability to flex his thumb after several months of pain along the course of the FPL. His medical history include a volar plate osteosynthesis of a distal radius fracture 2 years earlier after a skiing trauma ( Fig. 1 ). Clinical examination confirms an FPL tendon rupture and ultrasound identifies a rupture at the CMC-1 joint with a retracted proximal tendon stump that cannot be localized. What is the most effective approach for management of his rupture and how could it have been prevented?
Tendon rupture after distal radius fractures were found with or without surgical treatment. The timing of the tendon rupture varies from days or months after fracture or many years after surgical treatment. The most common incidence is associated with open reduction and internal fixation when the plate is not placed in a correct position and most commonly involved tendons are extensor tendons. DeGeorge et al. reported among 647 cases of distal radius fractures (636 patients) with open treatment of extra-articular and intraarticular distal radius fractures with internal fixation between May 2000 and May 2015, there is 2 extensor pollicis longus (EPL) ruptures and 1 flexor pollicis longus (FPL) tendon rupture. The mean time to tendon rupture was 481 days with a range from 21 to 1599 days. This is a rather uncommon complications compared with other complications such as loose or painful hardware (48 cases) and tendinopathy (flexor tendon irritation in 16 cases, extensor tendon irritation in 11 cases). In a survey of distal radius fractures treated with volar plating in a prefecture in Japan, Naito et al. reported 10 FPL ruptures (0.35%), 8 EPL ruptures (0.29%), 1 rupture of the flexor digitorum profundus (FDP) tendon to index finger (0.04%) and 1 rupture of the extensor digitorum communis (EDC) (0.04%) out of a total of 2787 cases. Thorninger et al. followed 576 patients with distal radius fractures treated with volar plating and found 5 flexor tendon ruptures and 12 extensor tendon ruptures. The incidence of tendon rupture was 2.9%.
In a systematic review of the 56 studies (6278 patients) before 2017, Azzi et al. reported overall tendon-related adverse events were recorded in 420 patients (6.8%). The incidence of tendon ruptures (EPL, FPL, FDP plus flexor digitorum superficialis, or EDC) was 1.5% with volar plates and 1.7% with dorsal plates. The incidence of tenosynovitis was 4.5% with volar plates and 7.5% with dorsal plates. Other reported detailed the ruptures of the flexor carpi radialis tendon or all finger flexors, or patients with late ruptures or the ruptures in nonoperative patients.
The incidence of tendon rupture was reported in 1%–3% of the cases with volar or dorsal plating according to the recent large patient cohorts, which appears not differ from the data in earlier publications (1%–2%). Though tendon rupture was seen in distal radius fracture without open reduction and surgical plating, our chapter will focus on questions and evidence of tendon rupture relating to surgical treatment.
How are tendon ruptures after distal radius fracture most effectively prevented, diagnosed, and treated?
Tendon rupture secondary to conservatively treated distal radius fractures are excessively rare and may go unnoticed if a high index of suspicion is not maintained. The vast majority of tendon ruptures following distal radius fractures are related to hardware malposition, have an insidious onset postoperatively after surgery and are preventable.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here