Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Rhinoplasty surgery requires a robust understanding of the surgical anatomy and physiology of the nose and nasal airway. Only by building on this solid foundation can a rhinoplasty surgeon adjust and tailor surgical techniques to fit unique individual patient needs. By balancing the patient's concerns with the surgeon's diagnosis after a complete examination, the surgeon can determine which set of techniques are most suitable to accomplish the surgical goals set out for each individual patient.
There is valuable information to be gained from inspection and palpation of the patient's nasal structures, including the skin, cartilage, bone, and dynamic interplay of these structures in animation during the preoperative assessment. There are features of each individual nose that the surgeon will want to preserve; it may be the dorsal height for one patient or the ala–columellar relation for another. The preoperative analytical and diagnostic aspects of rhinoplasty surgery are at least as important as the execution of any given technique outlined in the remainder of this book.
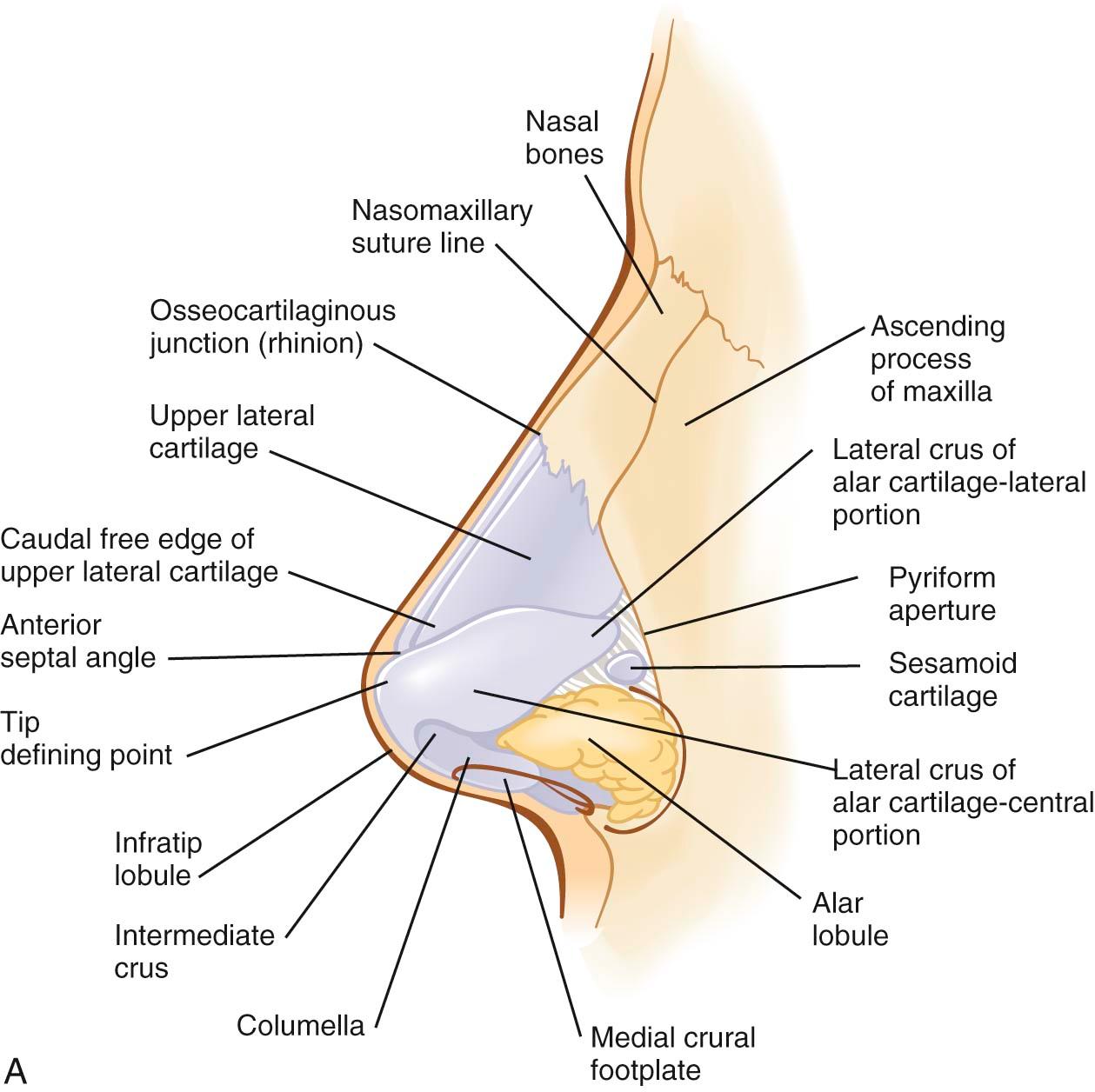
The scope of this chapter is to serve as a practical clinical reference to applied surgical anatomy and physiology as related to rhinoplasty. For the purposes of clarifying preferred directional anatomical references, these have been depicted in Figure 2-1 .
The skin and soft tissue envelope drapes the nasal skeleton, composed of the nasal bones, corresponding to the upper third of the nasal pyramid, and the lower two thirds, represented by the paired upper lateral cartilages (ULCs), paired lower lateral cartilages (LLCs), and septum in the midline. It is through the modification of these supporting structures that the rhinoplasty surgeon will be able to build the foundation onto which the skin and soft tissue envelope (S-STE) will rest, giving a pleasant appearance. Careful consideration should be given to the structural integrity of this foundation, as it will need to overcome both the natural aging process and the contractile forces associated with the cicatricial healing process following surgery. No compromises on nasal function need to be made in the name of accomplishing an aesthetically pleasing result.
The thickness, elasticity, and general characteristics of the S-STE can be confirmed by palpation of the nose. However, clues to its thickness are present on inspection. The presence of acne or adnexal structures such as fine hair in the supratip region, as seen in some patients, will provide insight into the skin thickness and the vascular supply that accompanies it. Topographic analysis of the nose is useful to discuss and accurately describe different anatomic landmarks ( Figures 2-2 through 2-6 ).
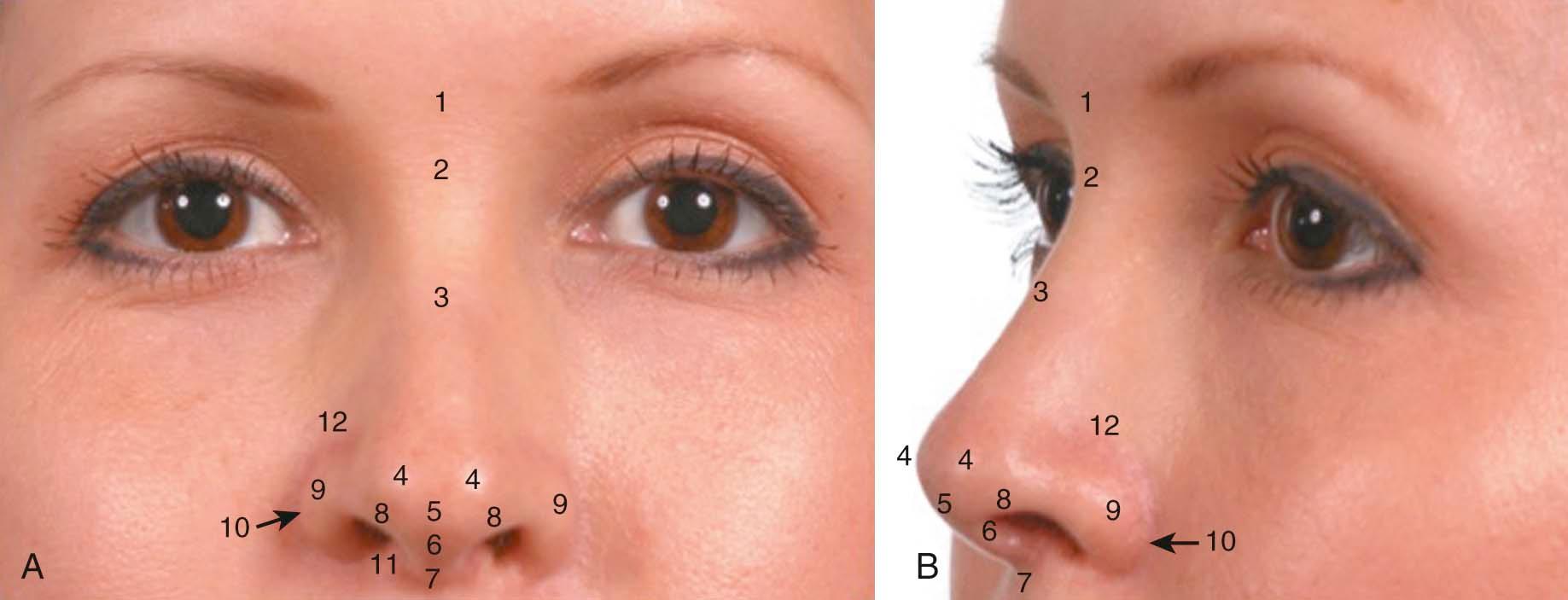
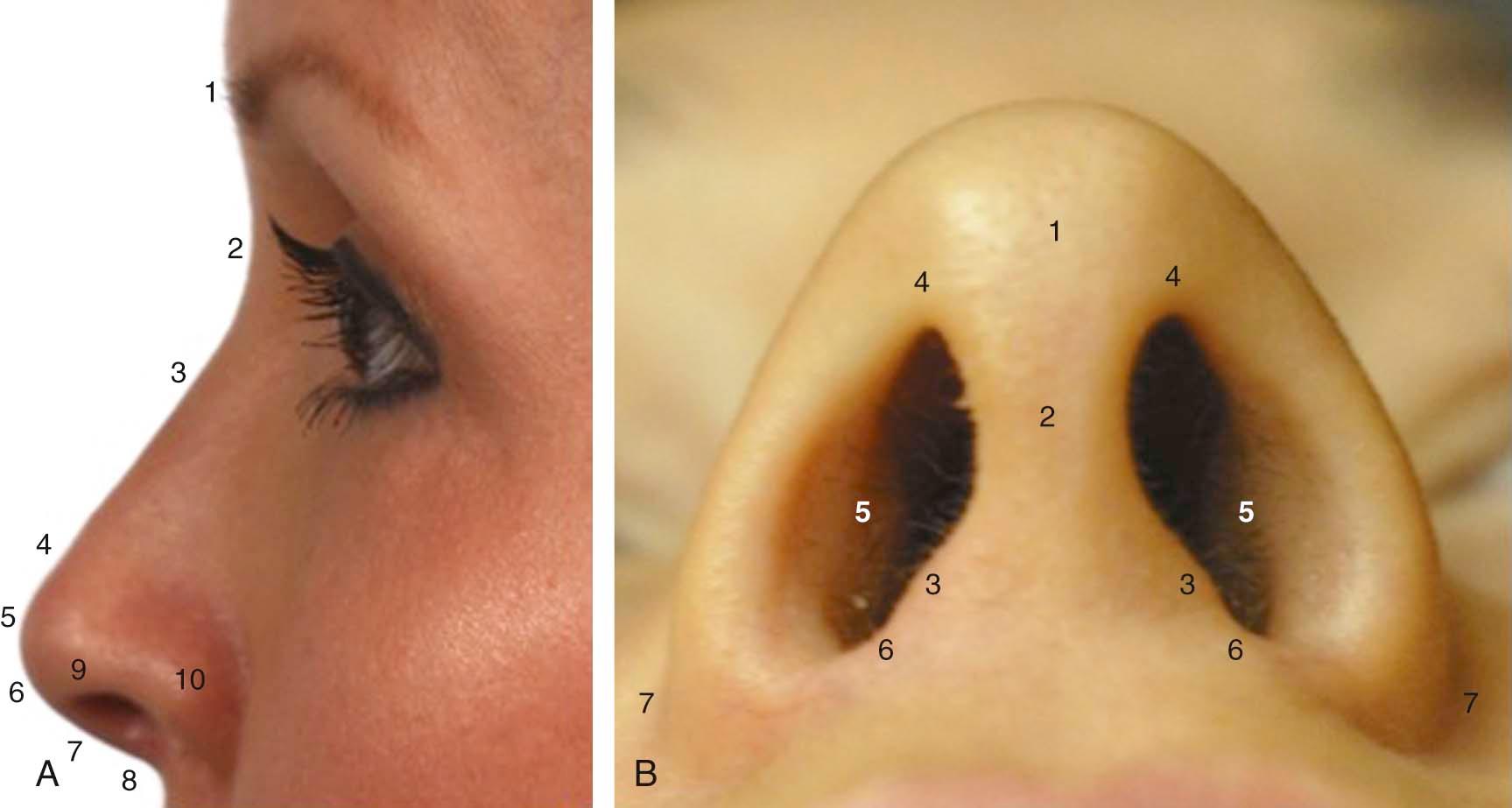
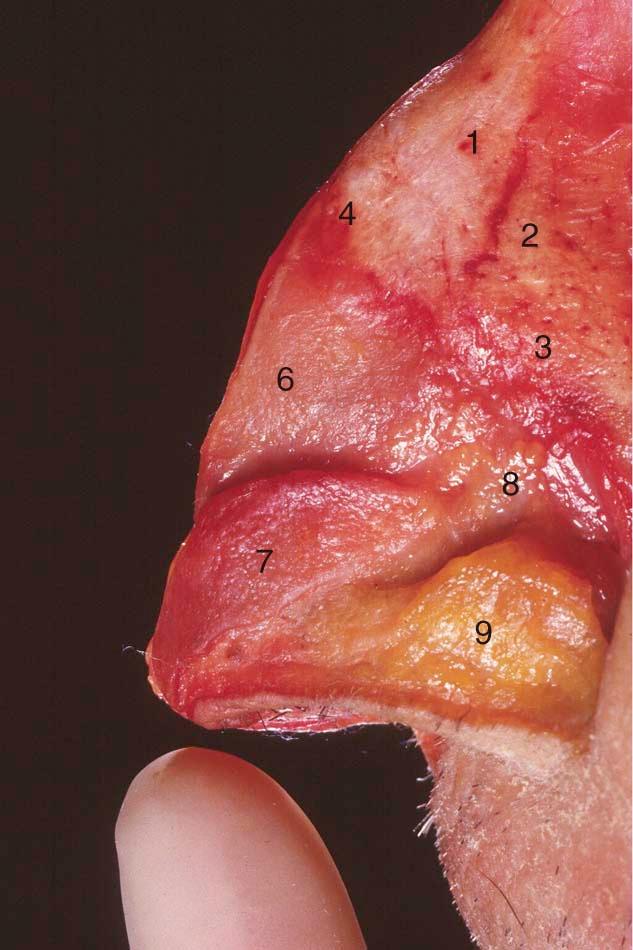
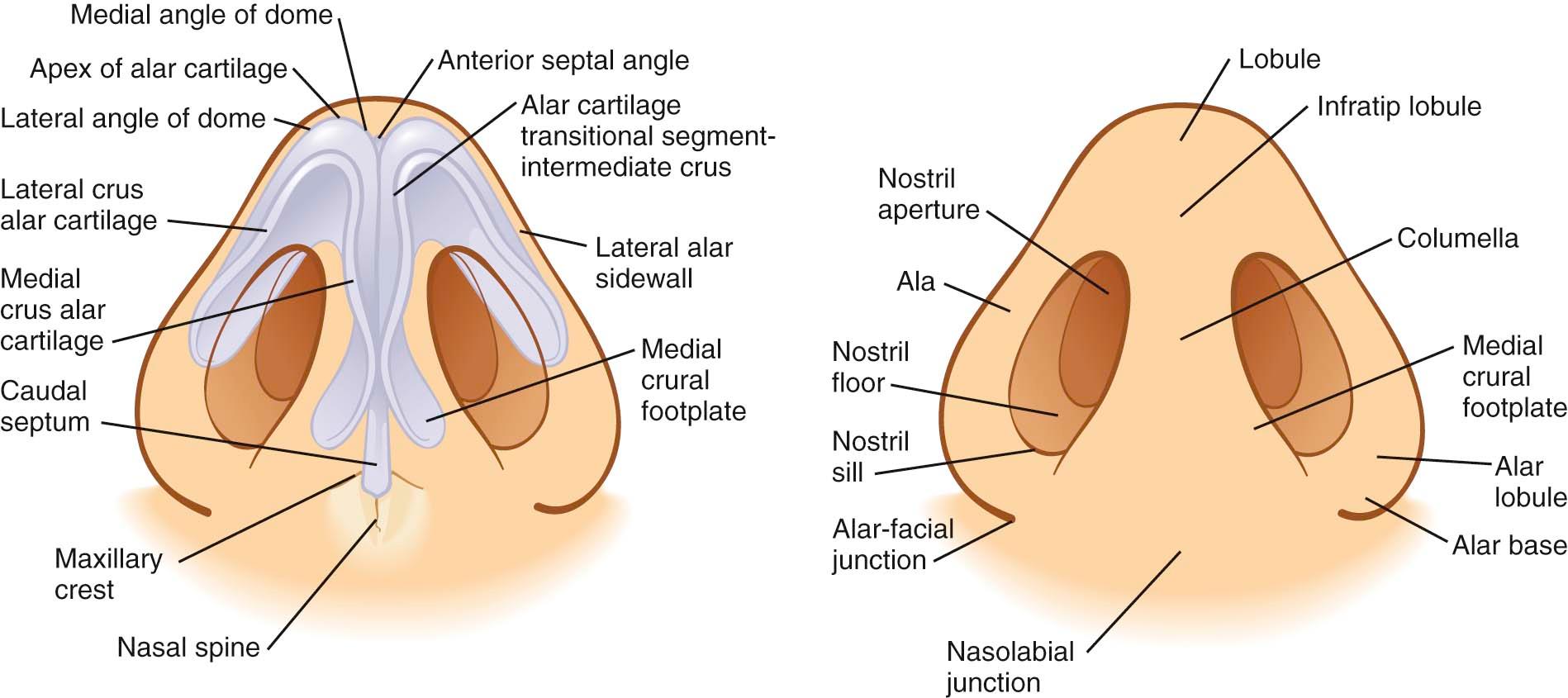
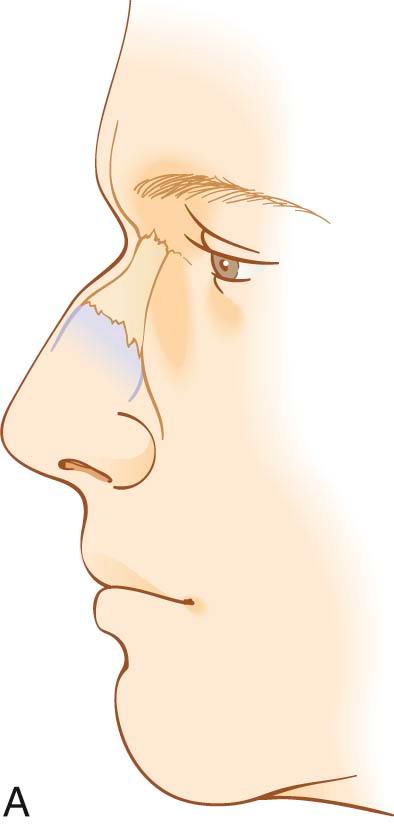
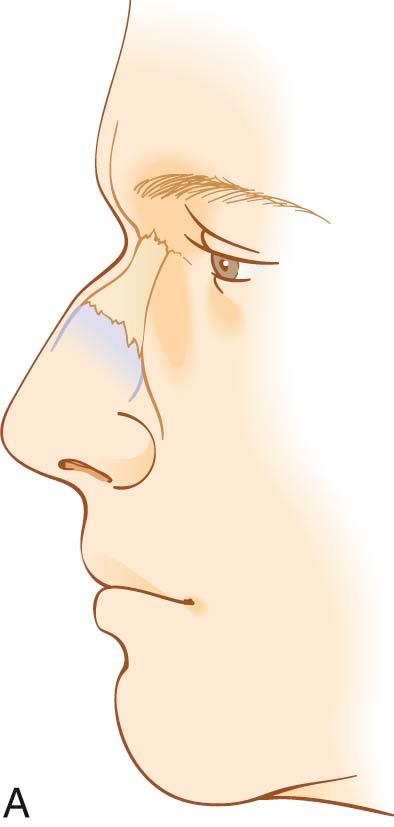
When divided into upper, middle, and lower thirds, the middle third of the nose, or that part covering the rhinion (osteocartilaginous juncture of the nose), will be the thinnest. In adults, the upper third of the S-STE will be the thickest, followed by the lower third. Adolescents and patients of ethnicity other than Caucasian will tend to have thicker S-STE on the supratip region of the lower third of the nose. However, the area of skin overlying the nasal domes will typically remain very thin. This underscores the importance of concentrating on avoiding irregularities to the middle third and around the area of the domes of the nose, so as to prevent its long-term collapse or irregularities, after soft tissue swelling subsides and the aging process ensues. The skin thickness of the soft tissue envelope of the nose will play a significant role in the degree of postoperative edema seen. Thin-skinned patients are found to have less edema that resolves faster than the greater, persistent edema found in patients with thicker skin.
The importance of these anatomic issues is evident when making surgical decisions. A straight-line removal of a nasal hump can result in an overreduced profile. Differential reduction of the cartilaginous and bony profile must be calibrated depending on the individual thickness of the overlying S-STE ( Figure 2-7 ). It is equally important to adequately analyze the depth of the radix, as it can provide a natural balance to the nose. Significant deepening of the radix will accentuate any dorsal prominence. Conversely, in a carefully selected setting, a radix graft will balance the nasal profile, decreasing the amount of resection necessary to balance the nasal dorsum ( Figure 2-8 ).
The nasal ala is composed of fibrofatty tissue and is devoid of cartilaginous structure, except for its attachments with the sesamoid cartilages through which it relates to the ULC, LLC, and the pyriform aperture.
The major mimetic muscles of the nose include the levator labii superioris–alaeque nasi, depressor septii nasi, alar nasi, and transverse nasalis muscle. These are encased and interconnected throughout by a fibrous fascia referred to as the nasal superficial musculoaponeurotic system (SMAS). Maintaining the integrity of this vascularized layer is important when placing grafts and implants to maximize engraftment and minimize infections. Significant ptosis of the nasal tip or deformity occurring during animation will respond to addressing these muscles by either Botulinum toxin use or by surgical ablation.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here