Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Burn injury to the axilla is caused by flame or direct contact. Ignition of clothing is the most common cause. Burns that will not heal within 2 weeks should be excised and skin grafted to prevent progressive scar contraction that will directly affect shoulder motion. Pain during acute burn management will limit abduction of the arm. The supple, concave quality of the axilla offers reduced resistance to burn contraction, subjecting the patient to potential long-standing painful, restricted motion.
Reconstruction of the burned axilla should be considered early as a pattern of functional loss of motion develops. The choice of reconstructive procedure depends on the extent of axillary involvement as well as on the quality of the peripheral tissue. Surgical treatment should reduce pain and maximize shoulder motion. Analysis of tissue deficiency, contraction patterns, and quality of tissue to be used for replacement will identify the proper treatment for each individual patient. As the contracture increases in complexity, knowledge of composite tissue transfer is essential to produce the best outcome while minimizing complications and recurrence.
The axilla is the area of skin and soft tissue underlying the shoulder joint. It is a supple, concave area defined by an anterior and posterior skinfold. The anterior fold is bordered by the lateral edge of the pectoralis major muscle; the posterior fold by the subscapularis, teres major, and latissimus muscles. The superior border consists of the first rib, clavicle, and scapula. The lower portion of the axillary skin is contiguous with the thorax. The contents of the axilla, deep to the subcutaneous tissue, include the axillary vessels, the brachial plexus, the long thoracic nerve, and axillary lymph nodes and lymphatic vessels. The skin of the axilla is of variable thickness. It is thinner at the cupola and thicker at the anterior and posterior folds. The density of hair follicles at the axillary cupola can be a potential source of increased healing by epithelialization in more superficial burn injuries to that protected area.
Burn injury to the axilla is often part of a larger chest/back burn in which loose clothing has caught fire, very often in cooking-related fires with direct injury to the torso and the outstretched arms. In regions where open, unprotected cooking fires are used in the home, burn injury to the axilla may be more common, especially in small children, who may fall or roll into the open fire. Explosions of stoves and ceramic cooking vessels are also a source of burns to the torso, upper extremities, and axillary areas.
Acute management of the axillary burn requires the assessment of burn depth and area of involvement. If third-degree burn is found over the majority of the axillary surface, early excision and grafting should be planned ( Fig. 4.6.1 ). Given the supple quality of the skin and the degree of concavity of the axilla, significant scar contraction will occur if the full-thickness burn is not excised. The resulting burn scar creates a skin deficiency that will limit motion of the shoulder. If partial-thickness injury is present and the expectation of healing by epithelialization is anticipated, conservative management with dressing changes may be considered ( Fig. 4.6.2 ). Splinting the arm in abduction both pre-operatively and post-operatively will be essential to reduce the potential for contraction. Early motion during the post–skin grafting or epithelializing period is extremely important.
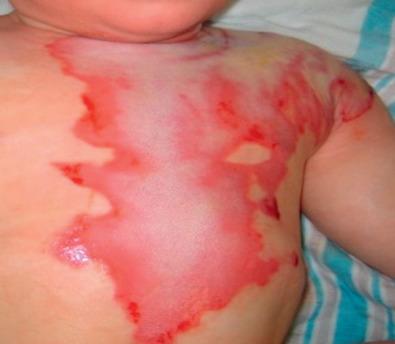
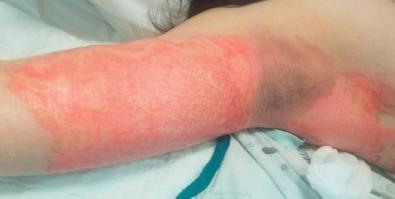
Burns of the axilla and shoulder are painful. Early excision of the deep burn with skin graft resurfacing replaces the anticipated contracting burn scar with better-quality tissue essential for early range-of-motion exercises. Axillary contractures and limitation of shoulder motion will be functionally significant in all deep axillary burns that go untreated. Even with optimum burn excision, skin grafting, or quality epithelialization in lesser-depth burn injuries, 27% of the patients will show axillary contractures when the scars have matured.
After healing of the grafted or epithelialized axillary burn, the surgeon will initiate a therapy plan to include scar massage, passive motion, and progressive stretch. Gains in abduction are maintained using splints between exercise periods and especially at nighttime. Splints and exercises opposing contraction are continued until scar maturation is complete and improvement in scar restriction occurs. Motion exercises are essential in preventing periarticular fibrosis of the shoulder joint. Limited shoulder motion is associated with a high degree of axillary contracture post-burn.
Continuous range-of-motion and stretch exercises of the shoulder after acute burn injury and resurfacing are essential to minimize contraction during the scar maturation period. As improvement of shoulder motion plateaus, identification of specific developing axillary contracture patterns will define the reconstructive stage of axillary burn management. Burn scar is synonymous with tissue deficiency. An appreciation of scar tension, direction of contraction, and timing of procedures associated with axillary contracture is important for the burn surgeon. Early intervention will be of great benefit to the patient.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here