Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
NIH grant R01DK041274 is acknowledged for financial support.
Diarrhea is a global health concern ranked second only to respiratory diseases in worldwide occurrence. In 2015, UNICEF estimated that half a million deaths per year from diarrhea occur among children under 5 years of age worldwide, which corresponds to 1400 childhood deaths every day. It is especially prevalent in the developing world, where mortality is related to dehydration, malnutrition, electrolyte disturbance, and the resultant acidosis. The highest mortality rate (80%) occurs during the first 2 years of birth. In comparison to developing countries, diarrhea-related mortality and morbidity is significantly lower in developed countries. In the United States, CDC reported 47.8 million diarrheal episodes with 3100 deaths annually, which quantify economic burden of US$150 million to the health-care sector. Additional estimates of the burden of diarrhea and its etiologies are produced annually as part of the Global Burden of Diseases, Injuries, and Risk Factors Study. The latest study spanning years 1990–2015 has been recently summarized by Troeger et al. While the report was consistent with UNICEF data in terms of deaths under 5 years of age, the study also revealed encouraging trends with significant decreases in diarrheal diseases globally, albeit these improvement varied among countries. Among all the cases, the leading cause of diarrhea deaths was Rotavirus infection, followed by Shigella spp. and Salmonella spp., whereas in children under 5 years of age, the three most common etiologies responsible for childhood deaths were rotavirus, Cryptosporidium spp., and Shigella spp.
In the gastrointestinal tract, ionic balance, fluid absorption, and secretion are vital to maintain homeostasis allowing for the maintenance of a membrane potential, adequate nutrient intake, normal gut motility, protection against microbes, and epithelial cell viability. This homeostatic state relies on the normal physiological function of the small and large intestinal cells and a complex array of hormonal mechanisms that control gut motility as well as entry and exit of fluid into the gastrointestinal lumen. Although there is an individual variation in what can be considered a normal stool pattern, in health, infants pass 5–10 g/kg/24 h of stool output and adults range between 100 and 200 g/24 h. Any deviation from the norm will lead to fecal losses, deficits, and eventually disease. This chapter discusses the pathophysiology of different types of diarrhea, and reviews its various clinical manifestations.
Ingestion of fluids (~ 2 L) and secretion of salivary, gastrointestinal, biliary, and pancreatic juices (~ 6–7 L) result in 8–10 L of fluid containing 800 mmol sodium, 700 mmol chloride, and 100 mmol potassium passing through the small intestinal lumen daily. It is remarkable that in health, the small intestine absorbs all but 1.5 L and the colon absorbs the rest leaving approximately 100 mL of fluid to be lost in stool. The efficient mechanisms responsible for this absorptive capacity are due to the function of several transport proteins located at the brush border membrane of the small and large intestine ( Fig. 68.1 ).
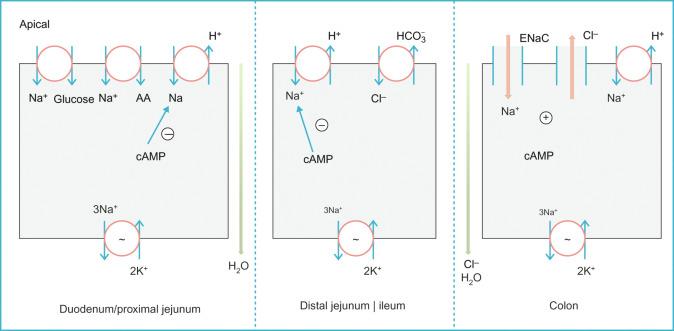
The intestinal tract separates its secretory and absorptive functions spatially. The tip of the villous, which is the functional unit of the small intestine, harbors the highly differentiated absorptive cells, whereas the crypt epithelia represent undifferentiated secretory cells. Both active absorption and active secretion of fluid result from the selective ion permeabilities of the plasma membranes of the cells lining the intestine. Irrespective of whether a subject ingests a hypotonic or a hypertonic meal, the permeable proximal small bowel allows movement of water and electrolytes into the lumen rendering the meal isotonic with plasma as it reaches the proximal jejunum; thus, allowing optimal absorption.
Intestinal ion transport mechanisms play a significant role in determining overall fluid balance in the gut, namely chloride secretion, electroneutral sodium chloride absorption, and electrogenic sodium absorption. Intestinal chloride secretion is quantitatively the most important mechanism driving fluid secretion across the intestinal epithelium, which occurs primarily from the crypt cells throughout the gastrointestinal tract, and is stimulated by an increase in the intracellular level of cyclic adenosine monophosphate (cAMP), cyclic guanosine monophosphate (cGMP), and calcium. These mediators inhibit the neutral sodium chloride entry and permit the entry of chloride into the cells through the basolateral membrane via the NKCC1, a sodium-potassium-2 chloride transporter (Na + -K + -2Cl − ). This transporter takes advantage of the low levels of intracellular sodium that are established by the basolateral sodium-potassium-ATPase. Cotransported potassium ions are recycled to avoid cellular depolarization and to maintain the driving force for chloride exit across the apical membrane through one of the several chloride channels, mainly cystic fibrosis transmembrane conductor regulator (CFTR) channel. An alternative Ca 2 + -activated Cl − channel (CaCCs)-mediated, and cAMP-independent chloride secretion mechanism also exists in intestinal epithelia. Although the molecular identity of CaCC still remains controversial, TMEM16 proteins (anoctamin, Ano), bestrophins (Best), and ClC-2 have been postulated as the potential candidates for CaCC in the gut. The transcellular transport of chloride drives the paracellular movement of sodium and water via the tight junctions ( Fig. 68.2 ).
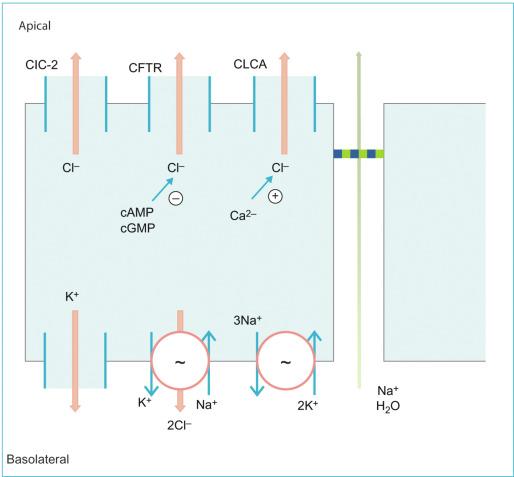
In addition to chloride secretion, the sodium-potassium-ATPase pump on the basolateral membrane of enterocytes provides the driving force for the net transcellular movement of sodium, potassium, and bicarbonate along the length of the small intestine. Sodium and chloride absorption occurs through an electroneutral pathway, which is achieved by the coordinated regulation of the apical membrane sodium-hydrogen exchangers (NHEs), mainly NHE-2, NHE-3, and NHE-8, and the anion exchangers SLC26A3 (DRA), SLC26A6 (PAT1), and SLC4A9 (AE4). These sodium-hydrogen and chloride-bicarbonate exchangers seem to work in parallel. Bicarbonate and protons needed to drive this process are believed to be generated intracellularly by the activity of carbonic anhydrase. Sodium then exits the cell via the basolateral sodium-potassium-ATPase pump, which leads to a subsequent absorption of water via the paracellular route. This pathway accounts for nutrient-independent fluid absorption in the small intestine and is also an important component of colonic fluid absorption, particularly in the proximal colon. Nonetheless, a sodium-hydrogen exchange in the absence of a parallel chloride-bicarbonate exchange is observed in the duodenum and proximal jejunum and is responsible for the absorption of large amounts of bicarbonate derived from biliary and pancreatic secretions. Sodium is also absorbed in the small intestine through cotransport with various nutrients, mainly sugars (glucose and galactose) and amino acids. This is the primary mechanism for postprandial fluid absorption and is not altered by increased levels of cAMP.
Sodium absorption by colonic epithelial cells mainly in the distal colon occurs through an electrogenic pathway, regulated by aldosterone. In this pathway, sodium, driven by a low intracellular sodium concentration, enters via sodium-selective ion channels (ENaC) and is followed by the paracellular chloride and water movement through tight junctions. In a state of salt restriction, aldosterone contributes to epithelial sodium channel upregulation which leads to an increased sodium permeability of the distal colon and hence, an increased active sodium absorption.
A variety of hormones and neurotransmitters are synthesized locally in the intestinal mucosa and modify intestinal ion transport either directly by binding to receptors on the basolateral membrane of enterocytes or indirectly via the release of other effectors. Serotonin (5-hydroxytryptamine; 5-HT) and prostaglandin E 2 (PGE 2 ) are potent intestinal secretagogues. 5-HT plays a role in a local reflex that controls chloride secretion in response to epithelial mechanical stimulation. Activated enterochromaffin cells residing in the epithelium release 5-HT in response to epithelial deformation which in turn affects epithelial transport directly as well as indirectly through the activation of sensory nerves that release substance P, acetylcholine, and purine nucleotides. PGE 2 is synthesized by subepithelial elements and acts by increasing levels of cAMP, which mediates the secretory effect. Among the various neurotransmitters released in the intestinal mucosa, vasoactive intestinal polypeptide (VIP), acetylcholine (ACh), and substance P are predominantly secretory, whereas norepinephrine, somatostatin, neuropeptide Y, and enkephalins are mainly absorptive. Both norepinephrine and somatostatin activate the inhibitory G-protein Gi, which interferes not only with the activation of adenylate cyclase but also with one or more calcium-mediated events. A recent study revealed region-specific contributions of the pro-secretory neurotransmitters ACh, VIP, NO, substance P, ATP, and adenosine to the neural control of the epithelial ion transport. ACh was primarily involved in nerve-evoked secretion in the small intestine, whereas VIP and NO were more dominant in the large intestine.
Recent studies also indicate that the multifaceted calcium sensing receptor (CaSR), G protein-coupled cell surface receptor of class C type, is a key player in the regulation of intestinal fluid homeostasis. Highly expressed in GI tract, including both villus and crypt cells, CaSR impedes Cl − secretion and promotes Na + absorption when activated by extracellular cations, mainly by Ca 2 + and some amino acids. This antisecretory and proabsorptive effect of CaSR is attributed to the degradation of cyclic nucleotides (cAMP, cGMP) due to the activation of Ca 2 + -sensitive phosphodiesterases.
In certain pathophysiologic states, the finely tuned ionic-fluid exchange becomes dysfunctional as a result of the failure of compensatory pro-absorptive/antisecretory mechanisms. The excessive secretion of sodium and chloride ions followed by the release of a large amount of water into the colonic lumen results in diarrhea. Definitions of diarrhea include increased volume, altered consistency, and increased frequency of defecation. A stool output in excess of 10 g/kg/day in infants and children and 200 g/day in an adolescent or adult is considered abnormal. However, the measurement of stool fluid content is impractical and assessment of frequency is preferred for diagnostic purposes. Word Health Organization (WHO) defines diarrhea as the passage of more than three loose or watery stools in a 24 h period, but emphasizes the importance of change in stool consistency rather than frequency.
Diarrhea can further be divided into acute and chronic, allowing some categorization of causes and associated management. Acute diarrhea, the most common form, has an abrupt onset, usually due to infection. It is self-limited and resolves typically within 2 weeks with proper medication. When diarrhea persists for more than 14 days, the condition is referred to as chronic. Chronic diarrheas usually manifest secondary to inflammation in the digestive tract (e.g., inflammatory bowel diseases; IBD) or to functional bowel disorders such as irritable bowel syndrome (IBS), food allergies or intolerance, or parasitic infections ( Cryptosporidium , Giardia ). Different pathophysiological mechanisms causing diarrhea have been elucidated and often several mechanisms work simultaneously.
Epithelial cells’ ion transport processes, in secretory diarrhea, are turned into a state of active secretion. Features of secretory diarrhea include a high stool volume output, a lack of response to fasting, absence of blood in stools, and a normal stool ion gap (100 mOsm/kg or less), indicating that nutrient absorption is intact ( Table 68.1 ). The mechanisms in this type of diarrhea include activation of intracellular mediators such as cAMP, cGMP, and intracellular calcium, which stimulate active chloride secretion from crypt cells and inhibit neutral coupled sodium chloride absorption ( Table 68.2 ). These mediators alter the paracellular ion flux because of toxin-mediated injury to the tight junctions. The most common cause of acute-onset secretory diarrhea is a bacterial infection of the gut. Several mechanisms may be at work. After colonization, enteric pathogens may adhere to or invade the epithelium; they may produce enterotoxins or cytotoxins. They may also trigger release of cytokines attracting inflammatory cells, which, in turn, contribute to the activated secretion by inducing the release of agents such as prostaglandins or platelet-activating factor. Coupled transport of sodium to glucose and amino acids is largely unaffected. Contrary, recent studies suggest rotavirus toxin NSP4 induce secretory diarrhea by inhibiting Na + absorption by the epithelial Na + channel ENaC and the Na + /glucose cotransporter SGLT1.
| Osmotic Diarrhea | Secretory Diarrhea | |
|---|---|---|
| Stool volume | < 200 mL/day | > 200 mL/day |
| Response to fasting | Stops | Continues |
| Fecal Na + | < 70 mEq/L | > 70 mEq/L |
| Fecal Cl − | < 35 mEq/L | > 40 mEq/L |
| Fecal pH | < 5.6 | > 6.0 |
| Fecal osmotic gap | > 100 mOsm/kg | < 50 mOsm/kg |
| Fecal reducing substances | Positive | Negative |
| Activation of cyclic adenosine monophosphate |
| Bacterial toxins: Salmonella, Shigella, Campylobacter , Pseudomonas aeruginosa , Escherichia coli (heat-labile), enterotoxins of cholera |
| Hormones: vasoactive intestinal peptide, gastrin, secretin |
| Anion surfactants: bile acids, ricinoleic acid |
| Activation of cyclic guanosine monophosphate |
| Bacterial toxins: Escherichia coli (heat-stable), Yersinia |
| Calcium-dependent |
| Bacterial toxins: Clostridium difficile |
| Neurotransmitters: acetylcholine, serotonin |
| Paracrine agents: bradykinin |
Occasionally, intestinal crypts undergo hyperplasia where the number of immature cryptal secretory cells increases to replace loss of absorptive cells. This cause of secretory diarrhea is noted in cases of enterocyte destruction and villous atrophy such as viral enteritis, celiac disease, and allergic enteropathy.
Osmotic diarrhea is caused by the presence of nonabsorbable solutes in the gastrointestinal tract ( Table 68.3 ). As such, stool output is proportional to the intake of these substrates and is usually not massive; diarrheal stools promptly regress with discontinuation of the offending nutrient, and the stool ion gap is high, exceeding 100 mOsm/kg ( Table 68.1 ). In fact, the fecal osmolality in this circumstance is accounted for not only by the electrolytes but also by the unabsorbed nutrient(s) and their degradation products. Because electrolyte absorption (Na + , K + , Cl − , HCO 3 − ) is unaffected by the osmotically active substances, stool water contains minute amounts of unabsorbed Na + and K + . This is the basis for the measurement and calculation of the fecal osmotic gap, a diagnostic test in the evaluation of patients with osmotic diarrhea.
| Malabsorption of water-soluble nutrients |
| Glucose-galactose malabsorption |
| Fructose malabsorption |
| Lactase deficiency (congenital or acquired) |
| Sucrase-isomaltase deficiency |
| Excessive intake of nonabsorbable solutes |
| Sorbitol |
| Lactulose |
| Magnesium hydroxide |
| Excessive intake of carbonated beverages |
Malabsorption and maldigestion can result due to the presence of osmotically active molecules within the intestinal tract. These molecules draw water into the lumen at a rate directly proportional to their concentration. This is further exacerbated in the colon where bacterial digestion of these molecules and fermentation to short-chain organic acids propagate the osmotic load and interfere with sodium absorption. A classic example is lactose malabsorption due to lactase deficiency.
Osmotic laxatives act via this mechanism. Polyethylene glycol 3350 (PEG) is poorly absorbed, not digested by human or bacterial enzymes, carries no electrical charge, and causes pure osmotic diarrhea. On the other hand, lactulose, a synthetic therapeutic disaccharide composed of galactose and fructose seems to be fermented at doses lower than organic acids, resulting in an osmotic load, but with higher doses diarrhea is mainly caused by a combination of organic acids and undigested carbohydrate.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here