Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Neurocutaneous disorders are congenital or hereditary conditions that feature lesions of both the skin and nervous system. Although each condition, or phakomatosis , is distinct and characterized by a unique pathophysiology, the concept of neurocutaneous disorders unifies those neurological disorders, whose identification depends primarily on simple visual diagnosis. These disorders may be inherited or sporadic; some of the sporadic disorders result from somatic mosaicism. Advances in clinical genetics have established the molecular basis for some of the disorders, although recognition and treatment still require an appreciation of the cutaneous and systemic symptoms. This chapter reviews the clinical features of the more common neurocutaneous syndromes.
Tuberous sclerosis complex (TSC) is a disorder of cellular differentiation and proliferation that can affect the brain, skin, kidneys, heart, and other organs. Many clinical features of TSC result from hamartomas, but true neoplasms also occur, particularly in the kidney and brain. Abnormal neuronal migration plays a major additional role in neurological dysfunction ( ; ).
Population-based studies suggest a prevalence of one per 6000 individuals. However, because of the striking variability of clinical expression, establishing the diagnosis of TSC can be difficult in individuals with subtle findings, and the true prevalence may be considerably higher. Cutaneous findings are usually the first clue that a patient has TSC, but other features may lead to the diagnosis. In infants, cardiac involvement and seizures frequently are presenting signs, whereas dermatological, pulmonary, or renal involvement may lead to diagnosis in older individuals. Updated guidelines have introduced genetic testing as the potential sole diagnostic criterion in addition to clinical findings ( Box 99.1 ).
The identification of a pathogenic mutation in either TSC1 or TSC2 is sufficient to make a definite diagnosis of TSC. A pathogenic mutation is defined as a mutation that clearly inactivates the function of the TSC1 or TSC2 proteins (e.g., out-of-frame indel or nonsense mutation), prevents protein synthesis (e.g., large genomic deletion), or is a missense mutation whose effect on protein function has been established. Other TSC1 or TSC2 variants whose effect on function is less certain do not meet these criteria and are insufficient to support a definite diagnosis of TSC. Note that 10%–25% of TSC patients have no mutation identified by conventional genetic testing, so a normal result does not exclude TSC or affect the use of clinical diagnostic criteria to diagnose TSC.
Hypomelanotic macules (≥3, at least 5-mm diameter)
Angiofibromas (≥3) or fibrous cephalic plaque
Ungual fibromas (≥2)
Shagreen patch
Multiple retinal hamartomas
Cortical dysplasias ∗
∗ Includes tubers and cerebral white-matter radial migration lines.
Subependymal nodules
Subependymal giant-cell astrocytoma
Cardiac rhabdomyoma
Lymphangioleiomyomatosis (LAM) †
† A combination of the two major clinical features (LAM and angiomyolipomas) without other features does not meet criteria for a definite diagnosis.
Angiomyolipomas (≥2) †
“Confetti” skin lesions
Dental enamel pits (≥3)
Intraoral fibromas (≥2)
Retinal achromic patch
Multiple renal cysts
Nonrenal hamartomas
Definite diagnosis: Two major features or one major feature with ≥2 minor features
Possible diagnosis: Either one major feature or ≥2 minor features
The inheritance of TSC is autosomal dominant with variable penetrance. The estimated spontaneous mutation rate for TSC varies from 66% to 86%, depending in part on the completeness of investigation of the extended family. Two genes are responsible for TSC: TSC1, coding for hamartin at chromosome 9q34.3; and TSC2, coding for tuberin adjacent to the gene for adult polycystic kidney disease at chromosome 16p13.3. The clinical features of TSC1 and TSC2 overlap, since the two gene products form a single functional unit that is an upstream modulator in the mammalian target of rapamycin (mTOR) signaling pathway. Both gene products downregulate small G-protein Ras-homolog enriched in brain (RHEB) activity in this pathway. However, genotype-phenotype studies indicate that individuals with a TSC2 mutation tend to have more severe disease, and the frequency of TSC2 mutations is greater among individuals with spontaneous mutations ( ). Multiple mutation types exist in different regions of each gene, and even individuals with identical genetic mutations can have different phenotypes. Molecular diagnostic testing—including prenatal testing—has been available since the early 2000s, and a disease-causing mutation is identified in about 85% of the individuals who meet the clinical diagnostic criteria. Some of the individuals with no mutation identified via routine gene analysis prove to have mosaicism ( ). Large genomic deletions and rearrangements are more common in the TSC2 gene than in TSC1, and more mutations have been identified for TSC2 than for TSC1. TSC2 mutations appear more commonly than TSC1 in patients with subependymal nodules (SENs), intellectual disability, renal angiomyolipomas, and retinal phakomas. Intellectual disability and other neuropsychiatric involvement are more likely in individuals with TSC2 than in those with TSC1 mutation ( ).
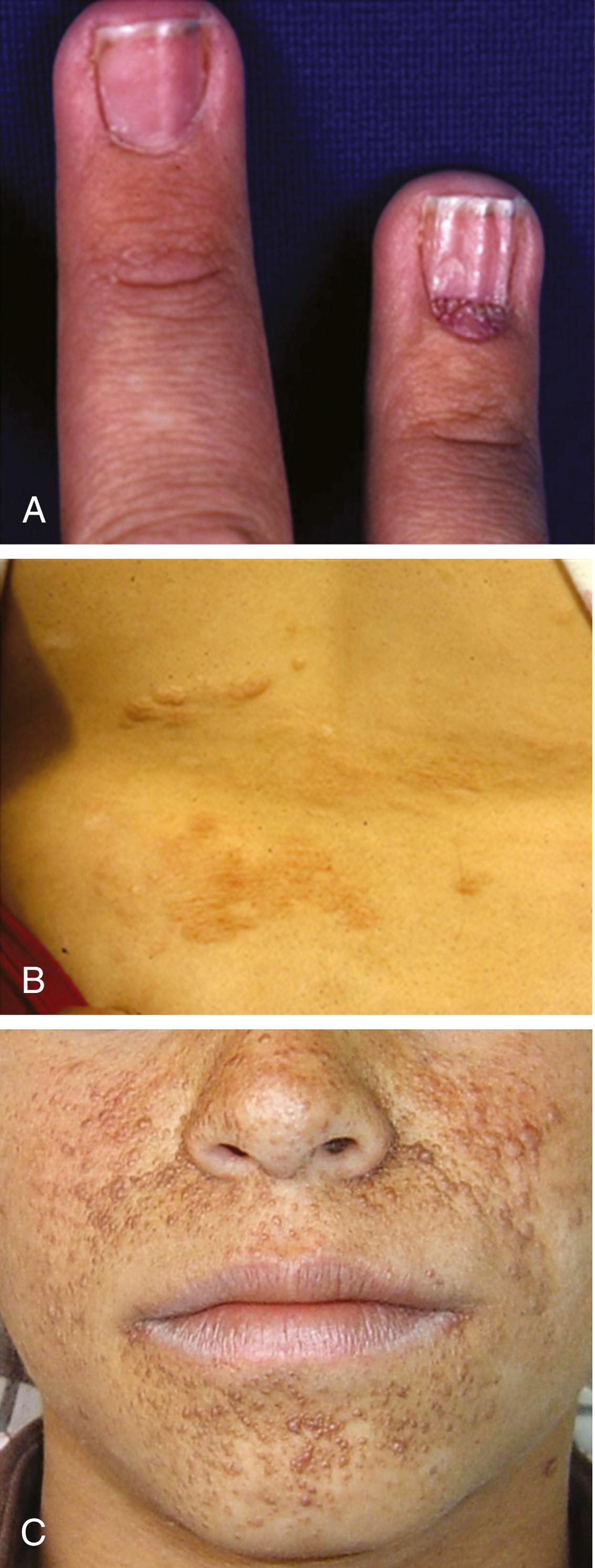
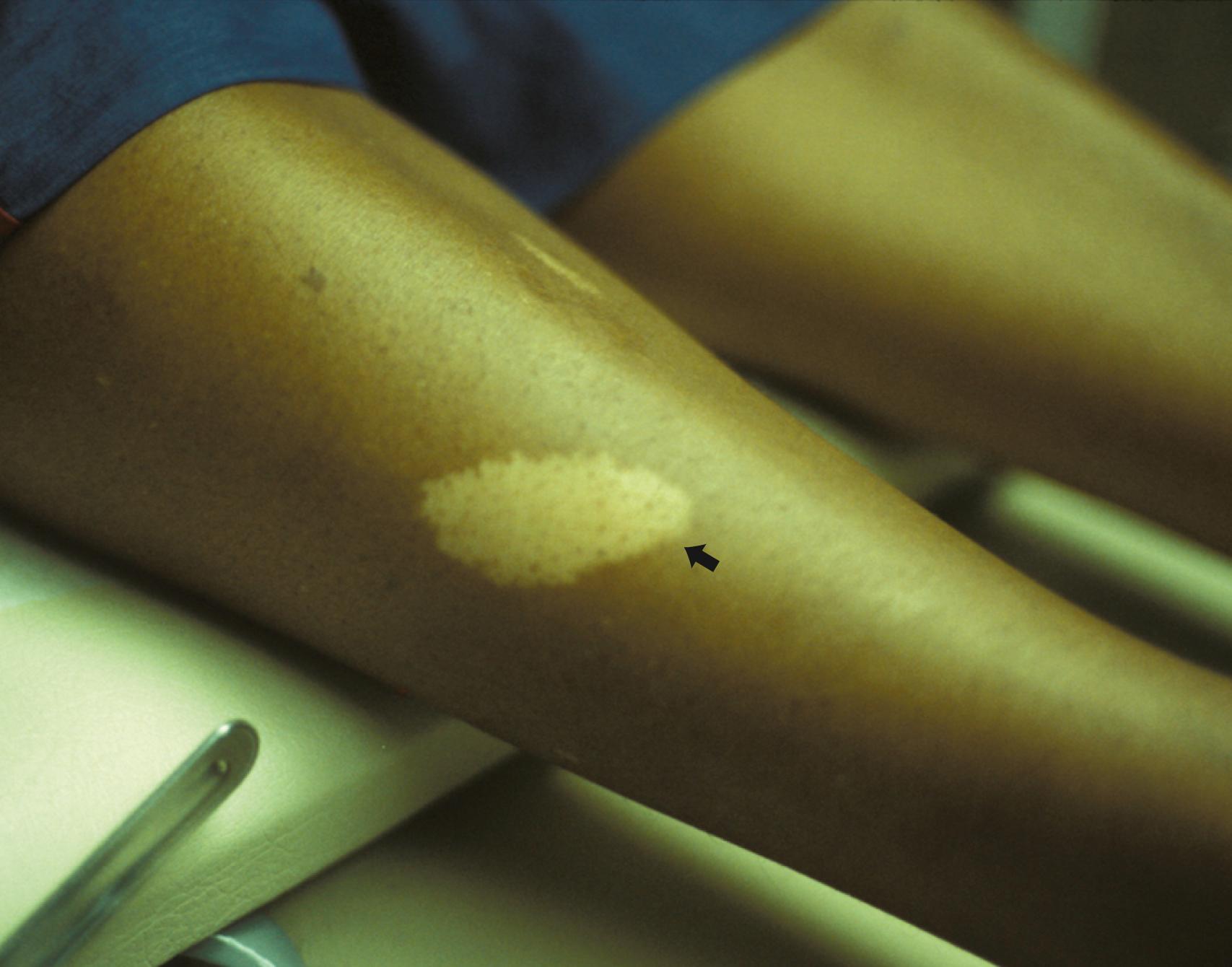
The cutaneous lesions of TSC include hypomelanotic macules, the shagreen patch, ungual fibromas, and facial angiofibromas ( Fig. 99.1 ). Hypomelanotic macules (ash leaf spots) occur in over 90% of affected individuals ( Fig. 99.2 ). The lesions usually are present at birth but may be evident in the newborn only with an ultraviolet light (Wood’s lamp). Other pigmentary abnormalities include confetti lesions (areas with stippled hypopigmentation, typically on the extremities) and poliosis (a white patch or forelock) of the scalp, hair, or eyelids. Hypomelanotic macules are common in normal individuals ( Table 99.1 ), but three or more hypomelanotic macules greater than 5 mm is a major diagnostic criterion for TSC.
| Lesion | Tuberous Sclerosis Complex | Other Individuals |
|---|---|---|
| Hypomelanotic macules | Occur in over 95% of TSC patients, often with many lesions | Occur in up to 5% of the population (but usually fewer than three lesions per person) |
| Facial angiofibromas | Eventually seen in 75% but less often in children | Seen in individuals with multiple endocrine neoplasia type 1 and in a few sporadic families |
| Shagreen patch | Up to 48% | Occasional |
| Ungual fibromas | Seen in 15% but often not until adulthood | Occasionally sporadic or after nail trauma (but typically one lesion) |
| Rhabdomyomas | One or more tumors seen in 47%–65% but much more common below 2 years Up to 51% of patients with rhabdomyomas have TSC |
In 14%–49% of rhabdomyoma patients, there are no other signs of TSC |
| Renal AML | Often multiple AML occur in up to 80% of TSC patients by age 10 | Sporadic AML occur but are typically solitary |
| Renal cysts | Polycystic kidneys occur in 3%–5% of TSC patients Smaller numbers of renal cysts are present in 15%–20% |
There are both dominant and recessive polycystic kidney diseases A few cysts are frequent sporadic findings in adults |
| Cortical dysplasia/tubers | 90%–95% and usually multiple lesions are present (magnetic resonance imaging yields highest detection rate) | Sporadic cortical dysplasia (typically one lesion) is common among individuals who have epilepsy not due to TSC |
| Subependymal nodules | 83%–93% | Rare, especially if calcified |
| Subependymal giant-cell tumors | Up to 15% (using radiographic criteria) | Rare in the absence of TSC |
Facial angiofibromas (previously termed adenoma sebaceum ) consist of vascular and connective tissue elements. Although multiple facial angiofibromas are relatively specific for TSC, they are found in only three-fourths of affected individuals and often appear several years after the diagnosis has been established by other means. The lesions typically become apparent during the preschool years as a few small red macules on the malar region; they gradually become papular, larger, and more numerous, sometimes extending down the nasolabial folds or onto the chin. Angiofibromas often become less prominent after starting an mTOR inhibitor, and topical application has been studied ( ). Forehead plaques or fibrous facial plaques resemble angiofibromas histologically, though they are not papular.
The shagreen patch most often is found on the back or flank area; it is an irregularly shaped, slightly raised, or textured skin lesion. About 20%–30% of patients with TSC have a shagreen patch, which may not be seen in young children.
Ungual fibromas are nodular or fleshy lesions that arise adjacent to (periungual) or underneath (subungual) the nails. The presence of two or more is considered a major criterion as a single lesion can develop after trauma in individuals without TSC. Ungual fibromas are among the latest cutaneous manifestation of TSC, present in up to 80% of older adults but only 20% overall ( ).
The predominant neurological manifestations of TSC are intellectual disability, epilepsy, and behavioral abnormalities, although milder forms of the disease with little or no neurological impairment are common. Impaired cellular interaction results in disrupted neuronal migration along radial glial fibers and abnormal proliferation of glial elements. Neuropathological lesions of TSC include SENs, cortical and subcortical hamartomas (tubers), areas of focal cortical dysplasia, and heterotopic gray matter. SENs commonly arise from germinal matrix progenitors in the caudothalamic groove near the foramen of Monro. These lesions can grow over time, but usually only into adolescence, after which time they calcify. These remain asymptomatic unless they transform into subependymal giant-cell astrocytomas (SEGAs). Tubers frequently extend from the ventricle wall to the cortical surface, with a linear or wedge-shaped distribution. Similar to normal brain, tubers develop between 14 and 16 weeks, gestation, such that the tuber load is established before birth, though they may not be visible on imaging until later childhood, given myelination status. These focal malformations of cortical development most frequently involve one gyrus at a time, but more diffuse involvement such as hemimegalencephaly can occur as well. Histology of these areas demonstrates disorganized cortical lamination and underlying abnormal myelination with indistinct gray-white-matter junction architecture. Calcification frequently is present. Dysmorphic neurons are often present, and other abnormal astrocytes similar to those seen in sporadic focal cortical dysplasias are termed balloon cells or giant cells for their abundant cytoplasm ( ).
Seizures of various types occur in 80%–90% of patients. Most develop during the first year of life, which is a poor prognosticator for autism and poor cognitive development. TSC is the most common cause of infantile spasms, and one-third of children with TSC develop them. Children with infantile spasms are more likely to have a high burden of cortical lesions demonstrated by magnetic resonance imaging (MRI) and are more likely to exhibit long-term cognitive impairment. For many, vigabatrin has been a more effective treatment option than adrenocorticotropic hormone (ACTH). Resective epilepsy surgery is a consideration in individuals with seizures localizing to one or two tubers. Corpus callosotomy is an option in some children. Some individuals with prolonged seizure freedom while taking medication can successfully discontinue anti-seizure medication ( ).
Many TSC patients have intellectual disability, but many have normal intelligence. As seen with early-onset epilepsy in general, intellectual disability in TSC often accompanies epilepsy that manifests earlier in life and that is refractory. The number of subependymal lesions does not correlate with the clinical severity of TSC, but MRI evidence of numerous cortical lesions is associated with more significant cognitive impairment and seizure intractability. The most abnormal regions seen on MRI tend to coincide with focal abnormalities of the electroencephalogram (EEG). The severity of intellectual disability ranges from borderline to profound intellectual disability. In addition to intellectual disability, many children with TSC have significant behavioral and psychiatric dysfunction. Autism, hyperkinesis, aggressiveness, psychosocial difficulties, and even psychosis can occur, either as isolated problems or in combination. The prevalence of autistic spectrum disorders is 25%–50% and equal between boys and girls. Behavioral problems are frequent and independent of intellectual ability. Mood disorders also are increased. De Vries and colleagues described the array of behavioral and psychiatric symptoms resulting from TSC as tuberous sclerosis associated neuropsychiatric disorders (TAND), and they developed a useful clinical screening tool ( ).
Computed tomography (CT) best demonstrates the calcified SENs that characterize TSC ( Fig. 99.3 ). CT sometimes shows superficial cerebral lesions, but they are far more obvious with brain MRI ( Fig. 99.4 ). T2-weighted sequences show evidence of abnormal neuronal migration in some patients as high-signal linear lesions running perpendicular to the cortex. SENs along the ventricular surface give the characteristic appearance of “candle guttering.” More than one-fourth of patients with TSC show cerebellar anomalies.
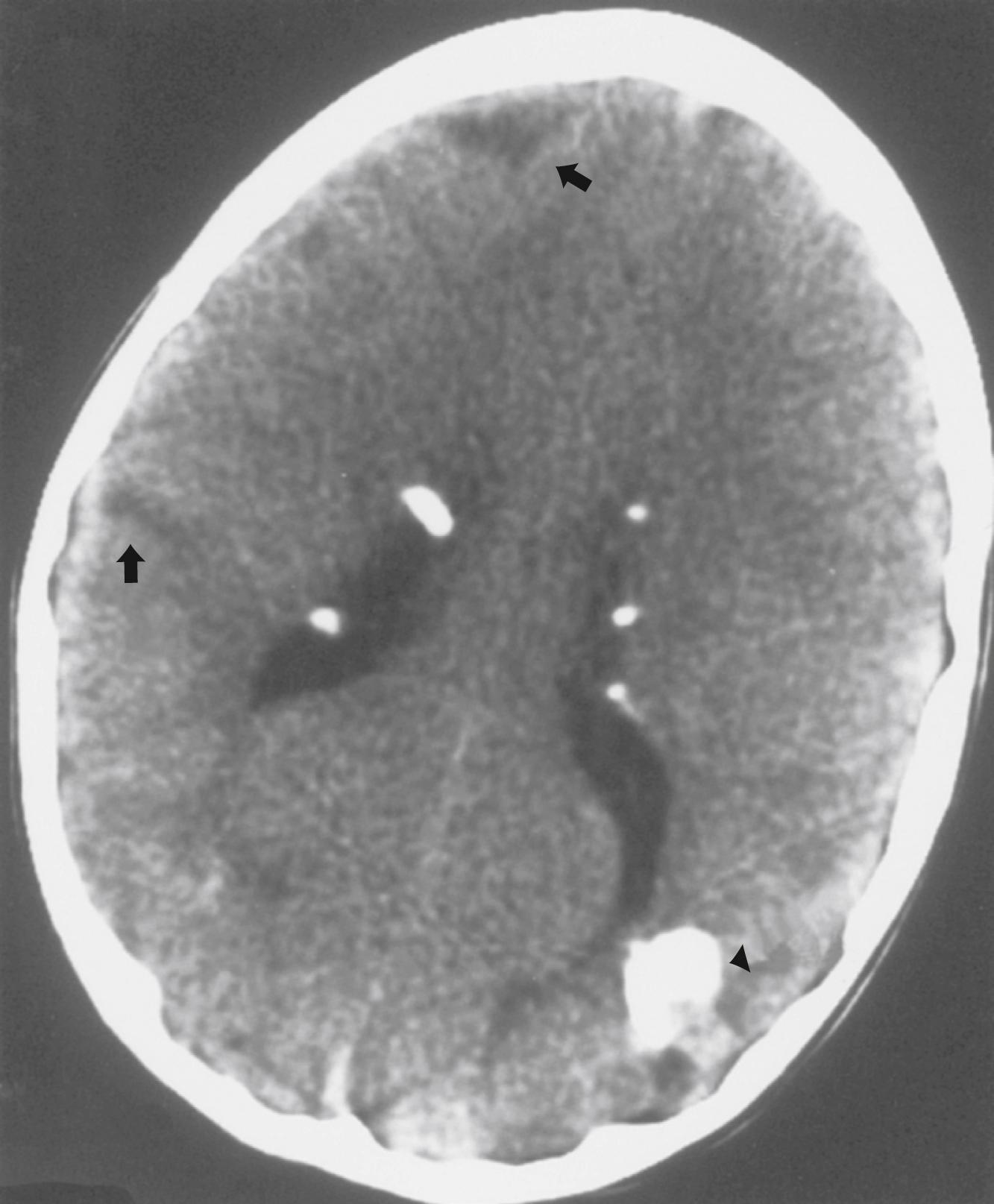
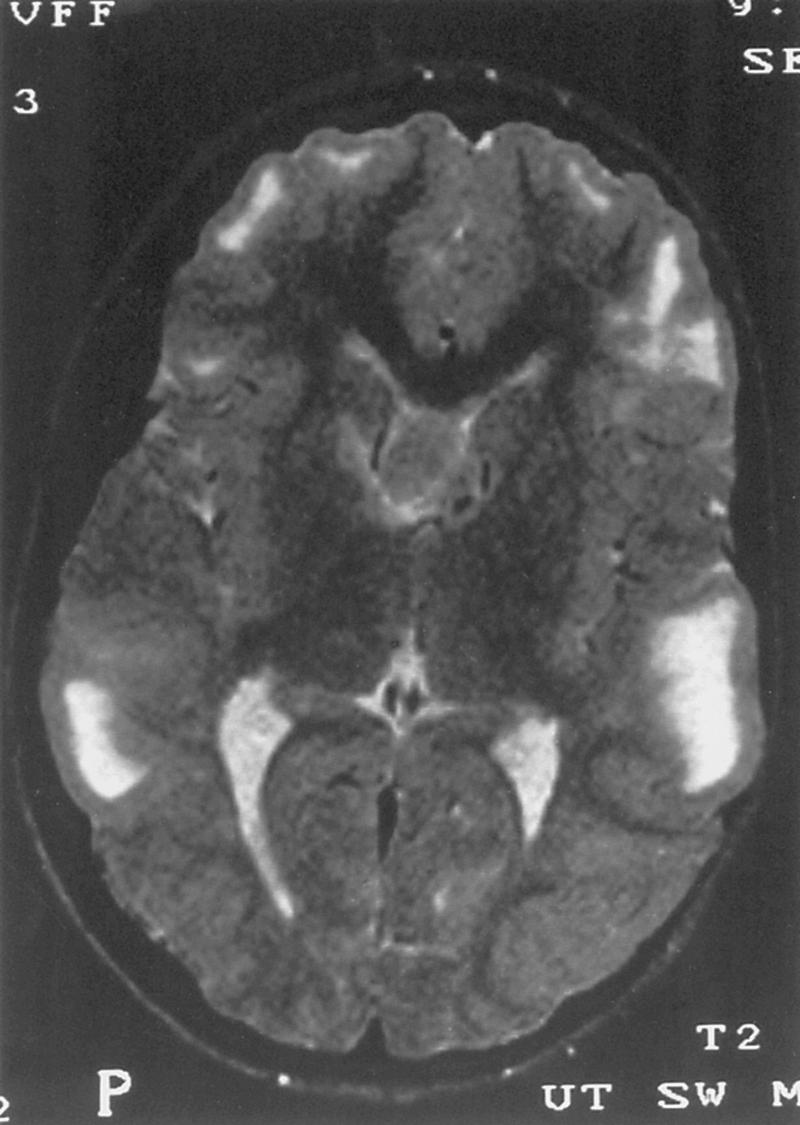
SEGAs develop in 6%–14% of patients with TSC. Unlike the more common cortical tubers and SENs, SEGAs can enlarge ( Fig. 99.5 ) and cause symptoms of increased intracranial pressure, particularly if extension into the lateral ventricles creates an obstructive hydrocephalus. Clinical features include new focal neurological deficits, unexplained behavior change, deterioration of seizure control, or symptoms of increased intracranial pressure. Acute or subacute onset of neurological dysfunction may result from sudden obstruction of the ventricular system by an intraventricular SEGA. Rarely, acute deterioration occurs because of hemorrhage into the tumor itself.
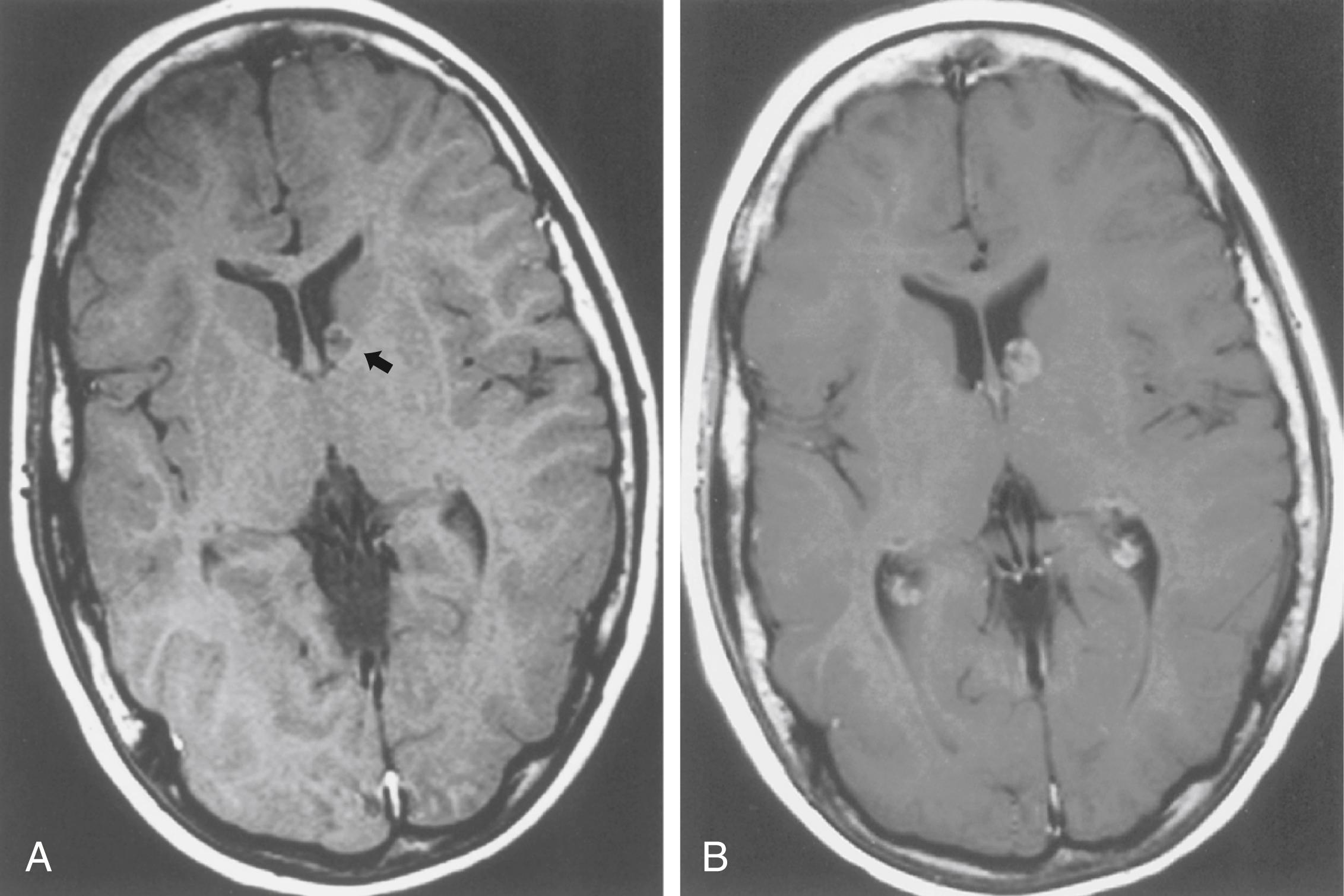
SEGAs are usually benign but locally invasive, and early surgery can be curative. Identification of an enlarging SEGA before the onset of symptoms of increased intracranial pressure or appearance of new neurological deficits is ideal. Periodic screening for identifying SEGA may improve surgical outcome. Recent work suggests that rapamycin and the oral mTOR inhibitor everolimus inhibit the growth of SEGAs. Everolimus has approval from the US Food and Drug Administration (FDA) for the treatment of SEGAs, renal angiomyolipomas, and, most recently, seizures due to TSC ( ). There also have been reports of improvement in pulmonary lymphangioleiomyomatosis (LAM) and facial angiofibromas ( ).
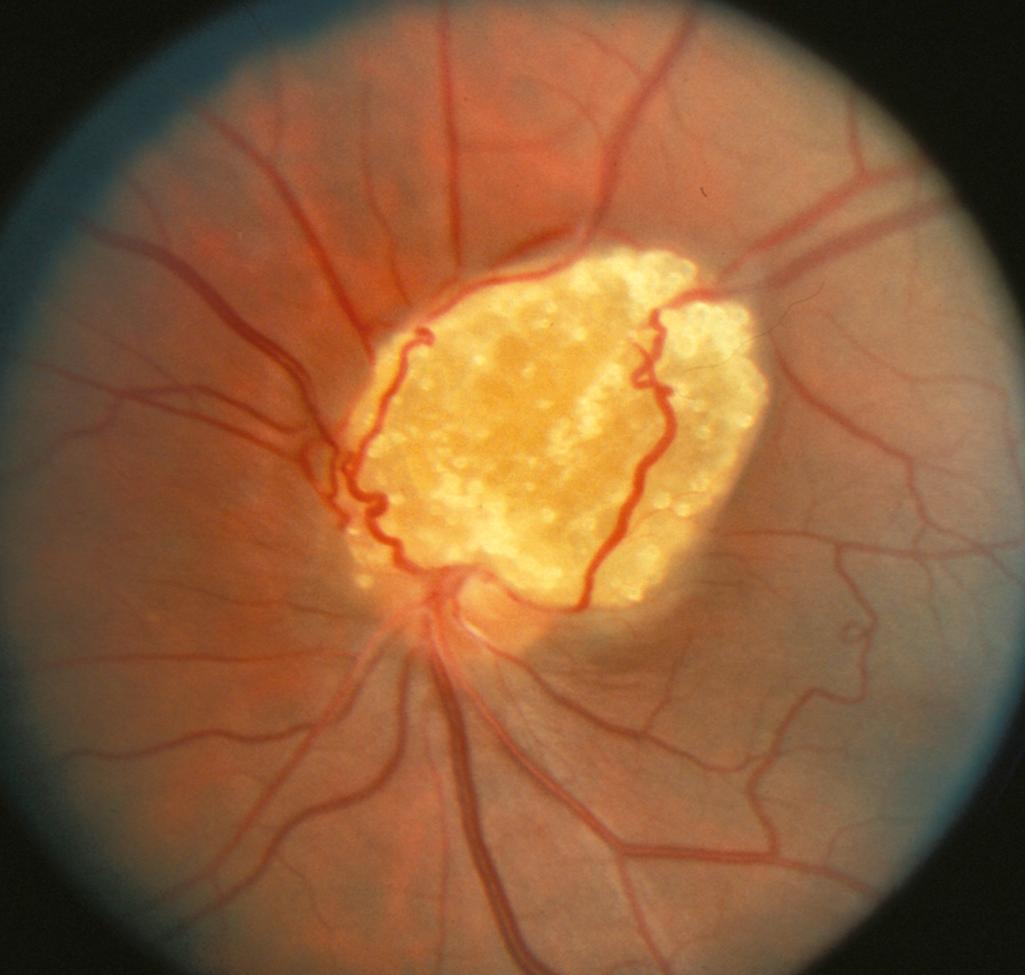
The frequency of retinal hamartomas in TSC varies from almost negligible to 87% of patients, probably reflecting the expertise and technique of the examiner. Pupillary dilatation and indirect ophthalmoscopy are important, particularly in children who may be uncooperative. Findings vary from classic mulberry lesions adjacent to the optic disc ( Fig. 99.6 ) to plaque-like hamartoma or depigmented retinal lesions. Most retinal lesions are clinically insignificant, but some patients have visual impairment caused by large macular lesions, and very few patients have visual loss caused by retinal detachment, vitreous hemorrhage, or hamartoma enlargement. Occasionally, patients have a pigmentary defect of the iris. Funduscopic examination is valuable at the time of diagnosis, to monitor existing abnormalities or to evaluate for new symptoms.
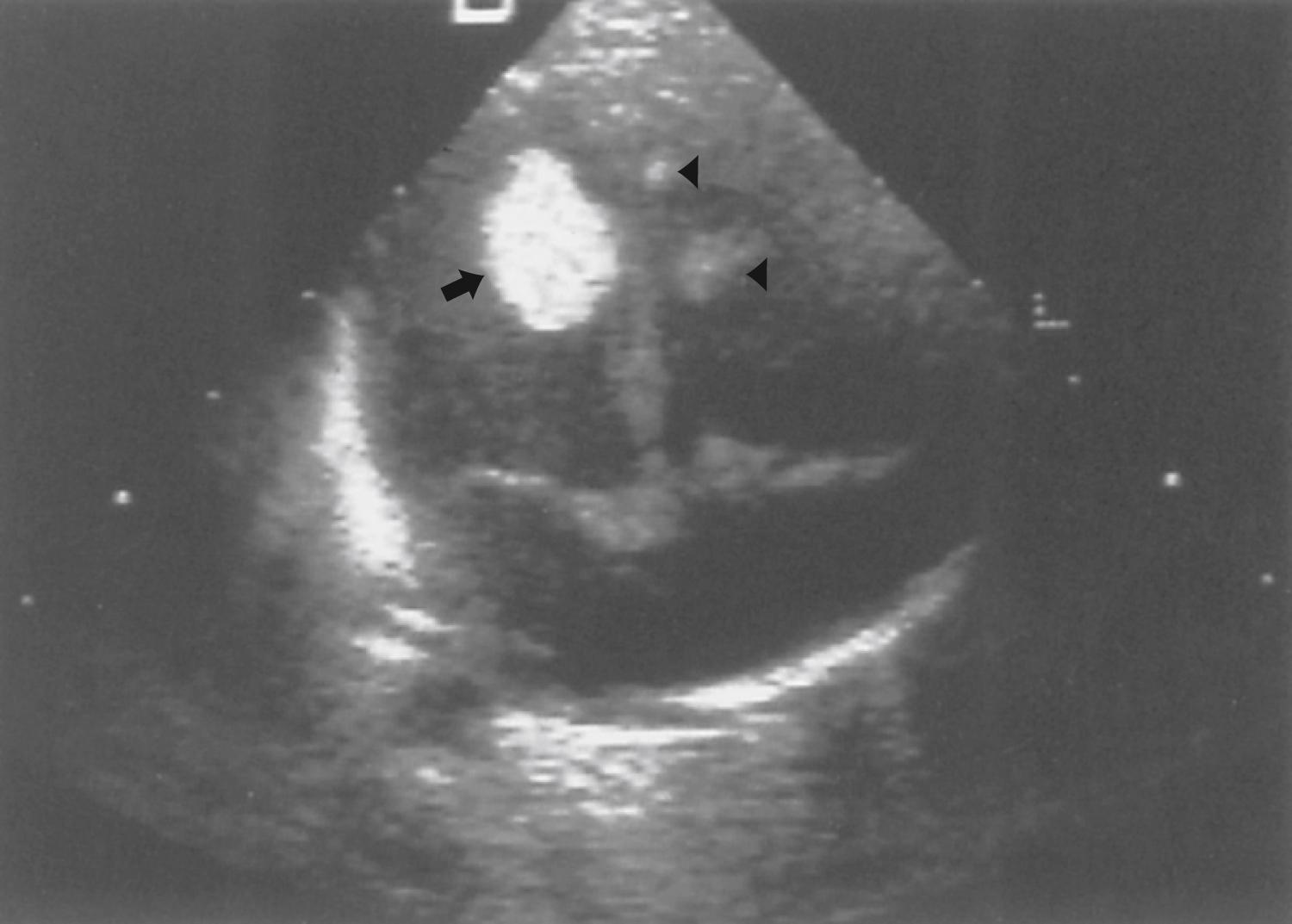
Approximately two-thirds of individuals with TSC have a cardiac rhabdomyoma, but few demonstrate clinical symptoms. Cardiac rhabdomyomas are hamartomas, tend to be multiple, and involute with time. These lesions sometimes are evident on prenatal ultrasound testing ( Fig. 99.7 ), usually after 24 weeks, gestational age. Most individuals who develop cardiac dysfunction present soon after birth with heart failure. A few children later develop cardiac arrhythmias or cerebral thromboembolism from the rhabdomyomas. The cause of congestive heart failure is either by obstruction of blood flow via intraluminal tumor or by lack of sufficient normal myocardium to maintain perfusion. Some patients stabilize after medical treatment with digoxin and diuretics and eventually improve; others require surgery. Echocardiography and electrocardiography (ECG) establish the diagnosis. Arterial aneurysms can occur. Surveillance studies every 6–12 months help monitor existing rhabdomyomas until stabilization or involution occurs. The size of these lesions may increase with hormone exposure—a consideration in the neonate, pubertal individual, and child treated with ACTH for infantile spasms.
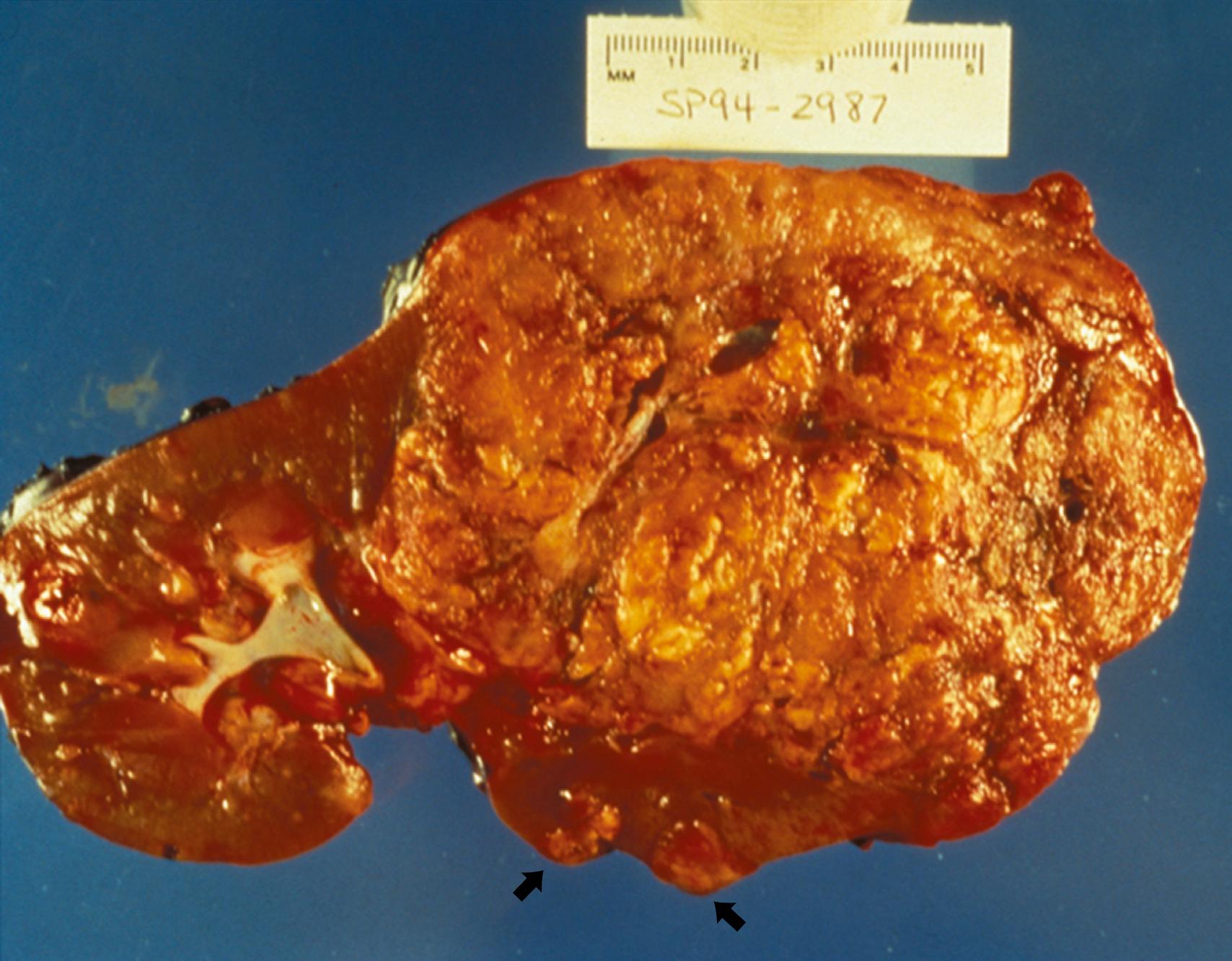
Renal angiomyolipomas occur in up to three-fourths of patients with TSC, usually presenting by 10 years of age. Most of these lesions are histologically benign tumors with varying amounts of vascular tissue, fat, and smooth muscle ( Fig. 99.8 ). Bilateral tumors and multiple tumors in a kidney are common. The prevalence and size of renal tumors increase with age, and tumors larger than 4 cm are much more likely to become symptomatic than smaller tumors. Renal cell carcinoma or other malignancies can affect TSC patients less commonly and at younger ages than the general population. Coalescing angiomyolipomas can contribute to end-stage renal disease. Endovascular embolization of the larger renal angiomyolipomas prevents hemorrhage and other complications ( ). Rapamycin and everolimus limit the growth of these tumors, at least transiently.
Single or multiple renal cysts are also a feature of TSC; these tend to appear earlier than the renal tumors. Ultrasound or cranial CT easily identifies larger cysts, and the combination of renal cysts and angiomyolipomas is characteristic of TSC. Individual renal cysts may disappear. Surveillance imaging is recommended, at least every 2–3 years—more frequently in those with existing or symptomatic renal involvement.
Pulmonary disease presents after puberty in the form of LAM and is five times more common in females than in males. Pulmonary lesions, symptomatic or asymptomatic, can be demonstrated in almost half of women with TSC who undergo chest CT. Baseline pulmonary function testing, 6-minute walk test, and high-resolution CT of the chest are recommended in all symptomatic patients and asymptomatic females at age 18 years. Spontaneous and recurrent pneumothorax, dyspnea, cough, and hemoptysis are typical symptoms of pulmonary TSC. Of those who develop symptoms, 10%–12% die within 10 years of symptom onset from complications of pulmonary TSC ( ). Tamoxifen and progesterone may be helpful in some patients, and mTOR inhibitors have been additional treatment options.
Neurofibromatosis type 1 (NF1), or von Recklinghausen disease, is the most common of the neurocutaneous syndromes, occurring in approximately 1 in 3000 people. Inheritance is autosomal dominant, but approximately half of NF1 cases result from a spontaneous mutation. The clinical features are highly variable.
A mutation of the 60-exon NF1 gene on chromosome 17q11.2 causes NF1. The NF1 gene product, neurofibromin, is a tumor-suppressor GTPase-activating protein functioning to inhibit Ras-mediated cell proliferation. Despite identification of approximately 100 mutations of NF1 in various regions of the gene, none correlates to a specific clinical phenotype ( ).
Several patients have developed a somatic NF1 mutation affecting only a limited region of the body. With this mosaic NF1, one extremity may have café-au-lait lesions, subcutaneous neurofibromas, and other signs of NF1, but the rest of the body is unaffected ( ). Similarly, some patients with germline mosaicism have no outward manifestations of NF1 but have multiple affected offspring.
If several characteristics are present and the physician is astute, the diagnosis of NF1 is obvious, especially when another family member is affected. The diagnosis is difficult when the clinical features are atypical and the family history is negative. Very young children may have fewer apparent lesions, making definitive diagnosis difficult. Diagnostic criteria ( Box 99.2 ) help to resolve some of these questionable cases, but specific gene testing is replacing the use of clinical criteria. Screening for the NF1 gene is technically difficult because the gene is large and several different mutations are causative. Commercially available studies have a 30% false-negative rate.
Six or more café-au-lait lesions more than 5 mm in diameter before puberty and more than 15 mm in diameter afterward
Freckling in the axillary or inguinal areas
Optic glioma
Two or more neurofibromas or one plexiform neurofibroma
A first-degree relative with neurofibromatosis type 1
Two or more Lisch nodules
A characteristic bony lesion (sphenoid dysplasia, thinning of the cortex of long bones, with or without pseudoarthrosis)
Bilateral eighth nerve tumor (shown by magnetic resonance imaging, computed tomography, or histological confirmation)
A first-degree relative with neurofibromatosis type 2 and a unilateral eighth nerve tumor
A first-degree relative with neurofibromatosis type 2 and any two of the following lesions: neurofibroma, meningioma, schwannoma, glioma, or juvenile posterior subcapsular lenticular opacity
Cutaneous lesions of NF1 ( Fig. 99.9 ) include café-au-lait spots, subcutaneous neurofibromas, plexiform neurofibromas, and axillary freckling. Café-au-lait spots are flat, hyperpigmented areas that vary in shape and size. They typically are present at birth but increase in size and number during the first few years of life. Later in childhood, skin freckling, 1–3 mm in diameter, often occurs symmetrically in the axillae (Crowe sign) and other intertriginous regions. Most children with six or more café-au-lait spots as their only diagnostic criterion will go on to meet diagnostic criteria, usually by age 6 years.
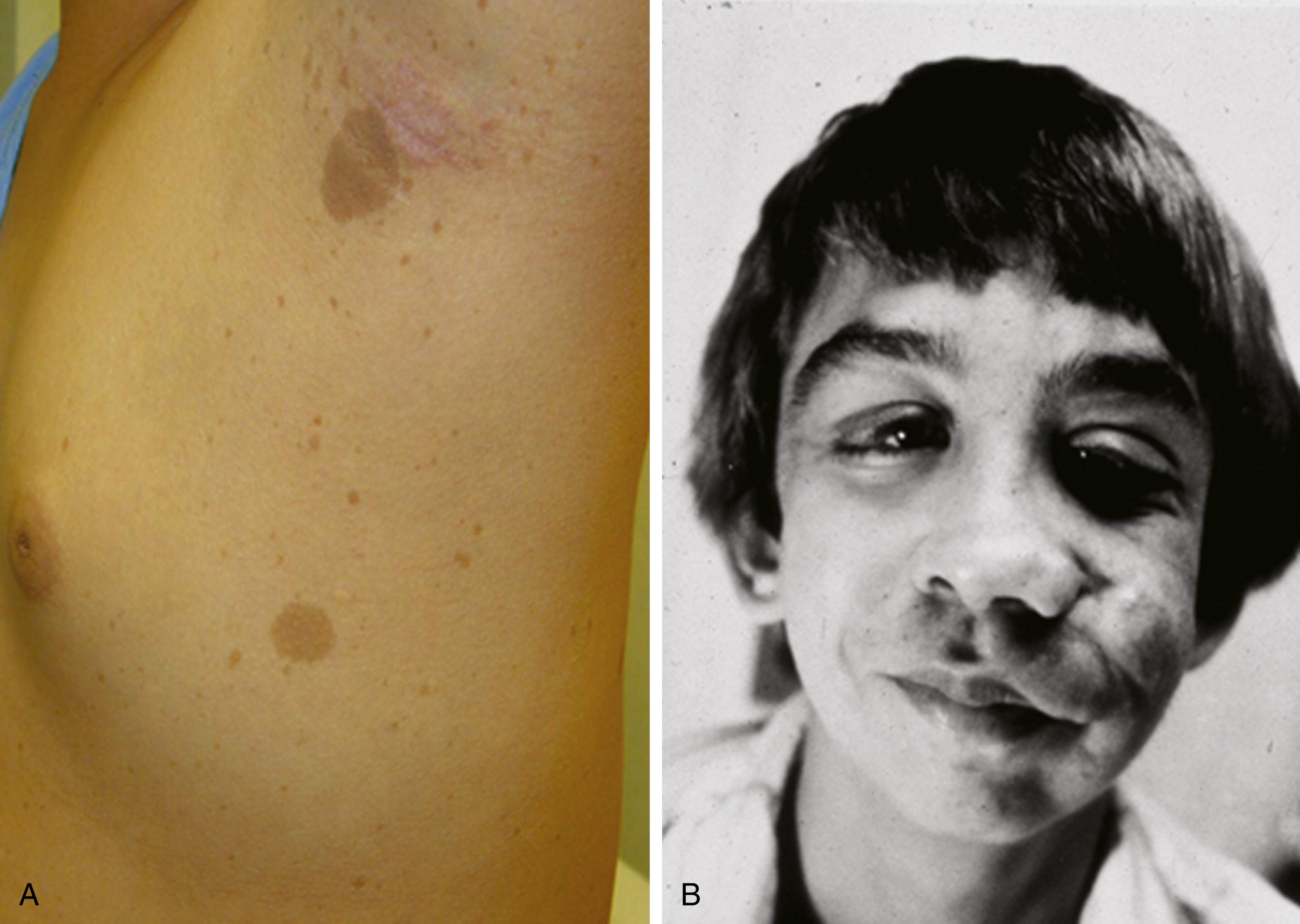
Neurofibromas are benign tumors arising from peripheral nerves. These tumors are composed predominantly of Schwann cells and fibroblasts but contain endothelial, pericyte, and mast cell components. Neurofibromas can develop at any time; their size and number often increase after puberty.
Plexiform neurofibromas often occur on the face and can cause substantial deformity. Patients with plexiform tumors of the head, face, or neck and those who presented before 10 years of age are more likely to do poorly ( ). Plexiform neurofibromas have a 5%–13% lifetime risk of malignant degeneration into malignant peripheral nerve sheath tumors (MPNSTs). MPNSTs carry poor 5-year survival rates despite treatment with surgery, chemotherapy, and radiation. PNFs and MPNSTs are difficult to distinguish radiographically and sometimes even pathologically.
NF1 affects the nervous system in several ways, but the clinical features vary even within the same family. Tumors occur in the brain, spinal cord, and peripheral nerves. Compared to the general population, there is higher incidence of learning disability and attention disorders. Accompanying moyamoya syndrome predisposes to stroke.
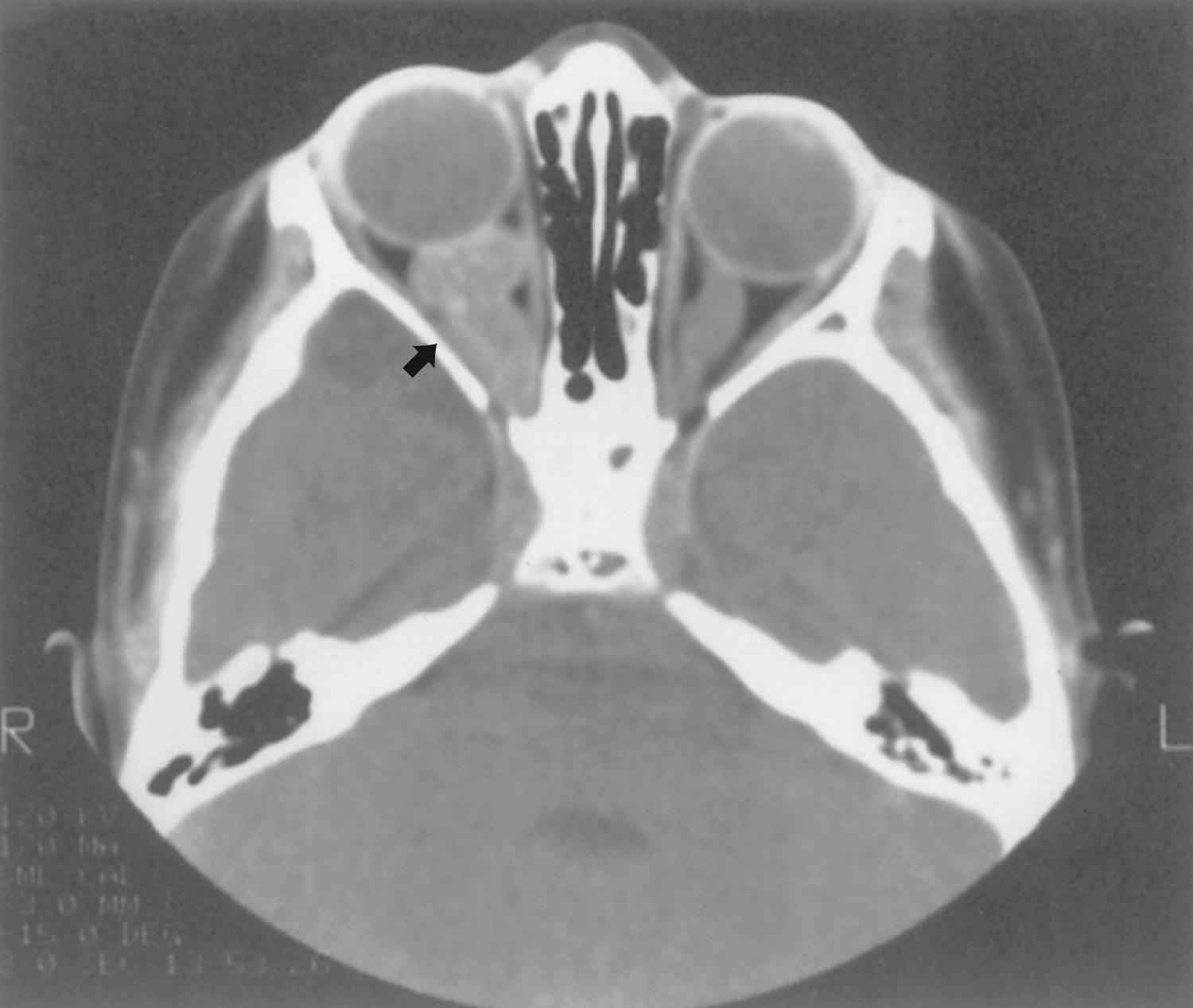
Optic nerve glioma ( Fig. 99.10 ) is the most common CNS tumor caused by NF1. Approximately 15% of patients with NF1 have unilateral or bilateral optic glioma. The growth rate of these tumors varies, but they tend to behave less aggressively in patients with NF1 than those without NF1. When symptomatic, the presenting features are optic atrophy, progressive vision loss, pain, or proptosis. Precocious puberty is a common presenting feature of chiasmatic optic nerve tumors in children with NF1. Management options include observation with serial brain MRI or treatment with radiation, chemotherapy, or small-molecule therapies that specifically target signaling pathways downstream of activated Ras. Radiation is less favored, especially given possible exacerbation of vasculopathy in this population.
Ependymomas and meningiomas of the CNS occur in patients with NF1 less often than in patients with neurofibromatosis type 2. Neurofibromas and schwannomas are common but not always symptomatic; they develop on either cranial nerves or spinal nerve roots. The symptoms from these tumors (discomfort, pain, numbness, weakness, and bowel/bladder dysfunction) reflect their size, location, and rate of growth.
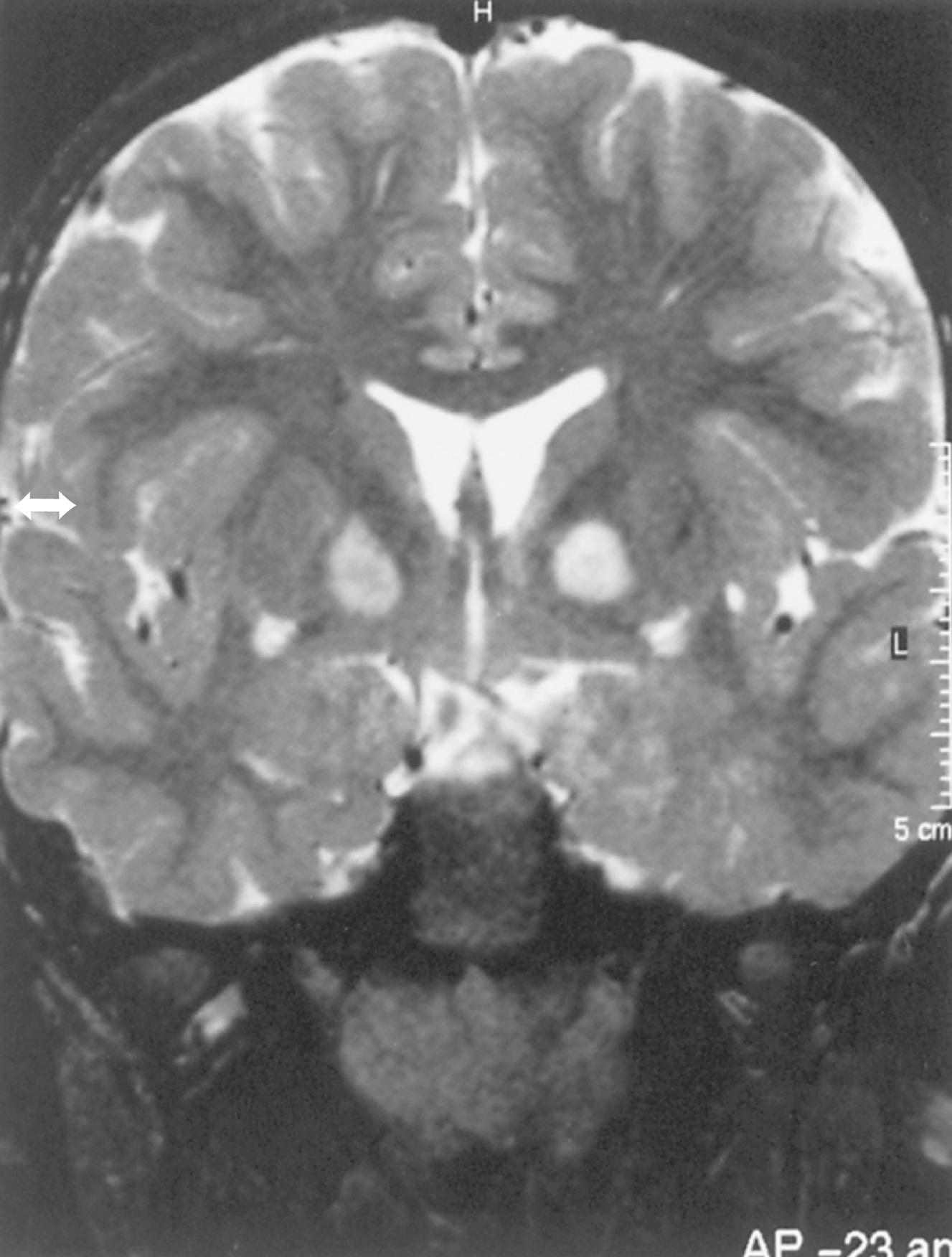
Macrocephaly is seen in half of NF1 patients, typically attributable to megalencephaly related to increases in white-matter volume. Macrocephaly is independent of hydrocephalus accompanying aqueductal stenosis, which also occurs in this disorder. Approximately 60%–78% of patients with NF1 have increased signal lesions within the basal ganglia, thalamus, brainstem, and cerebellum on T2-weighted MRIs ( Fig. 99.11 ). These areas are not routinely visible with CT. The origin and significance of these radiographic lesions are unclear, and they are referred to at times as unidentified bright objects (UBOs). Whether these MRI lesions correlate with the likelihood of cognitive impairment is still debatable; radiographic findings do not correlate with neurological deficits. Patients with NF1 tend to have full-scale intelligence quotient (IQ) scores within the low-normal range and to exhibit behavioral problems. Deep gray-matter radiological findings tend to decrease with time, while cortical and subcortical findings do not decrease or increase.
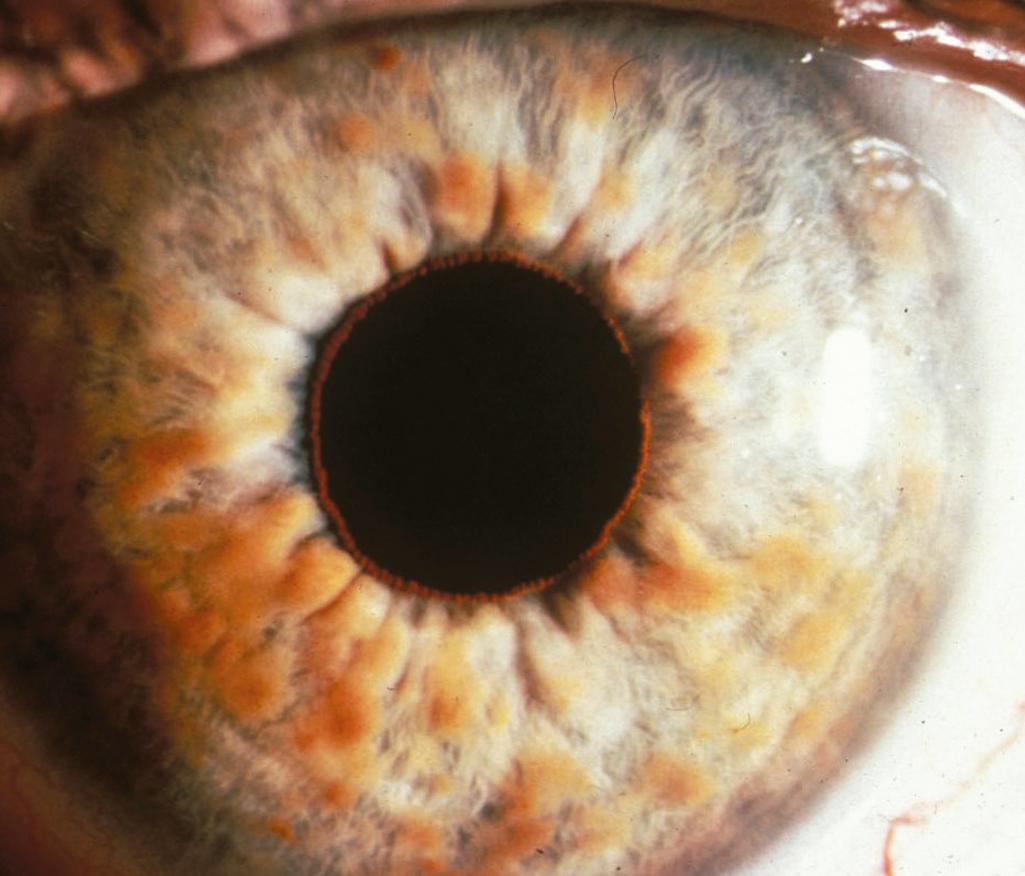
Lisch nodules are pigmented iris hamartomas ( Fig. 99.12 ). They are pathognomonic for NF1. Lisch nodules do not cause symptoms; their significance lies in their implications for the diagnosis of NF1. Lisch nodules are often not apparent during early childhood, so their absence does not exclude the diagnosis of NF1. Rarely, children with NF1 have retinal hamartomas, but these usually remain asymptomatic.
Dysplasia of the renal or carotid arteries occurs in a small percentage of patients with NF1. Renal artery stenosis causes systemic hypertension. Another potential cause of hypertension is pheochromocytoma. Several forms of cerebral artery dysplasia occur, most commonly moyamoya syndrome, which promotes cerebral infarction in children and brain hemorrhage in adults. Arterial aneurysms occur as well.
The most common skeletal manifestations in NF1 consist of short stature and macrocephaly. Other skeletal abnormalities include long-bone dysplasia (resulting in pathological fractures and subsequent pseudoarthrosis), scoliosis, and bony erosion secondary to adjacent tumor. Dysplasia of the sphenoid wing is common.
A mimic of NF1 is LEOPARD syndrome ( l entigenes, E CG conduction abnormalities, o cular hypertelorism, p ulmonary stenosis, a bnormal (male) genitalia, r etardation of growth, d eafness) is an autosomal dominant disorder whose features also include café-au-lait spots and obstructive cardiomyopathy. The café-au-lait spots and cardiac abnormalities may suggest NF1. Legius syndrome is another autosomal dominant NF-like syndrome; it is characterized by similar cutaneous features but little tumorigenesis.
Designated fully a separate entity from NF1 in the late 20th century, neurofibromatosis type 2 (NF2) is characterized by bilateral vestibular schwannomas and often is associated with other brain or spinal cord tumors. Similar to NF1, the inheritance is autosomal dominant. Some suggest the diagnosis of NF2 based on multiple meningiomas or nonvestibular schwannomas even without family history or classic bilateral vestibular schwannomas. NF2 occurs in only 1 in 35,000 to 50,000 people.
A mutation of the NF2 gene on chromosome 22 causes NF2. The NF2 protein product is schwannomin or merlin, moesin-ezrin-radixin-like protein. The NF2 gene is a tumor suppressor. Dysfunction of the NF2 gene accounts for the occurrence of multiple central nervous system (CNS) tumors in patients with NF2. Several different mutations have been documented in the NF2 gene. The clinical severity may be related to the nature of the NF2 mutation; missense mutations that allow some protein function tend to produce milder clinical forms, whereas frameshift and nonsense mutations that produce stop codons preventing the production of any protein often cause severe disease ( ).
Patients with NF2 have few cutaneous lesions, and these tend to be subtle. Instead, patients often have multiple types of CNS tumors (thus, the designation of central NF ). Café-au-lait spots and subcutaneous neurofibromas are less common than in NF1. Some patients exhibit presenile posterior subcapsular cataracts.
Most patients who meet established diagnostic criteria for NF2 (see Box 99.2 ) eventually develop bilateral vestibular schwannomas, previously termed acoustic neuromas ( Fig. 99.13 ). Symptoms of NF2 typically develop in adolescence or early adulthood but can begin in childhood. Common complaints with large acoustic tumors include hearing loss, tinnitus, vertigo, facial weakness, poor balance, and headache. Unilateral hearing loss is relatively common in the early stages. Consider screening with annual auditory brainstem responses or brain MRI.
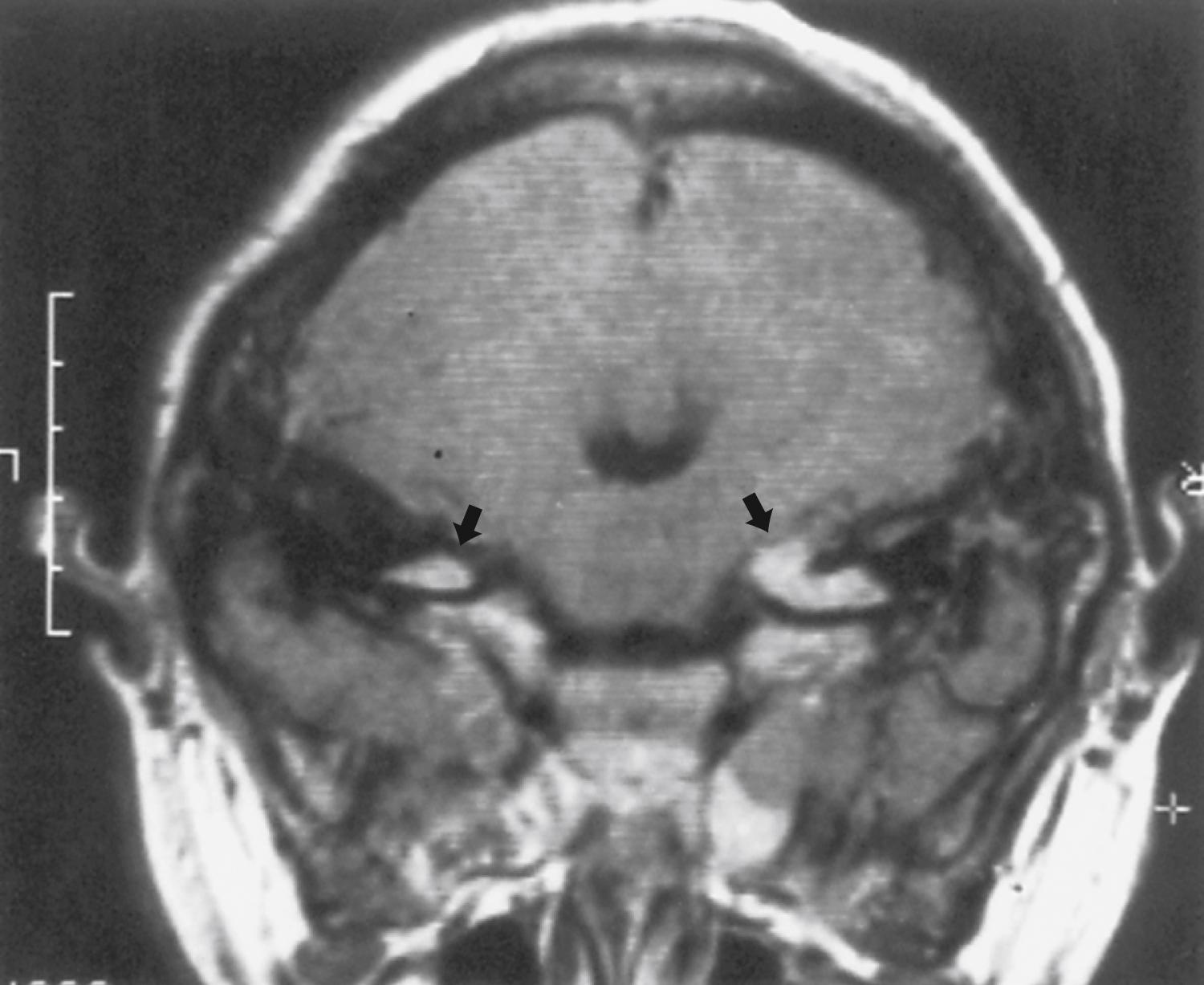
Other CNS tumors occur much less often than vestibular schwannomas. The term MISME syndrome ( m ultiple i nherited s chwannomas, m eningiomas, and e pendymomas) applies to this disorder. The clinical features of these tumors depend primarily on their location within the brain and spinal cord. Schwannomas of other cranial nerves occur in some patients. Meningiomas, ependymomas, and astrocytomas also occur with increased frequency. Patients with NF2 may develop multiple simultaneous tumor types, and baseline imaging at the time of diagnosis should include the brain and spinal cord.
Merlin is a novel regulator of TSC/mTORC1 signaling, so mTOR inhibitors are being evaluated in the management of NF2 tumors ( ) and also have been under study for the treatment of plexiform neurofibromas in NF1.
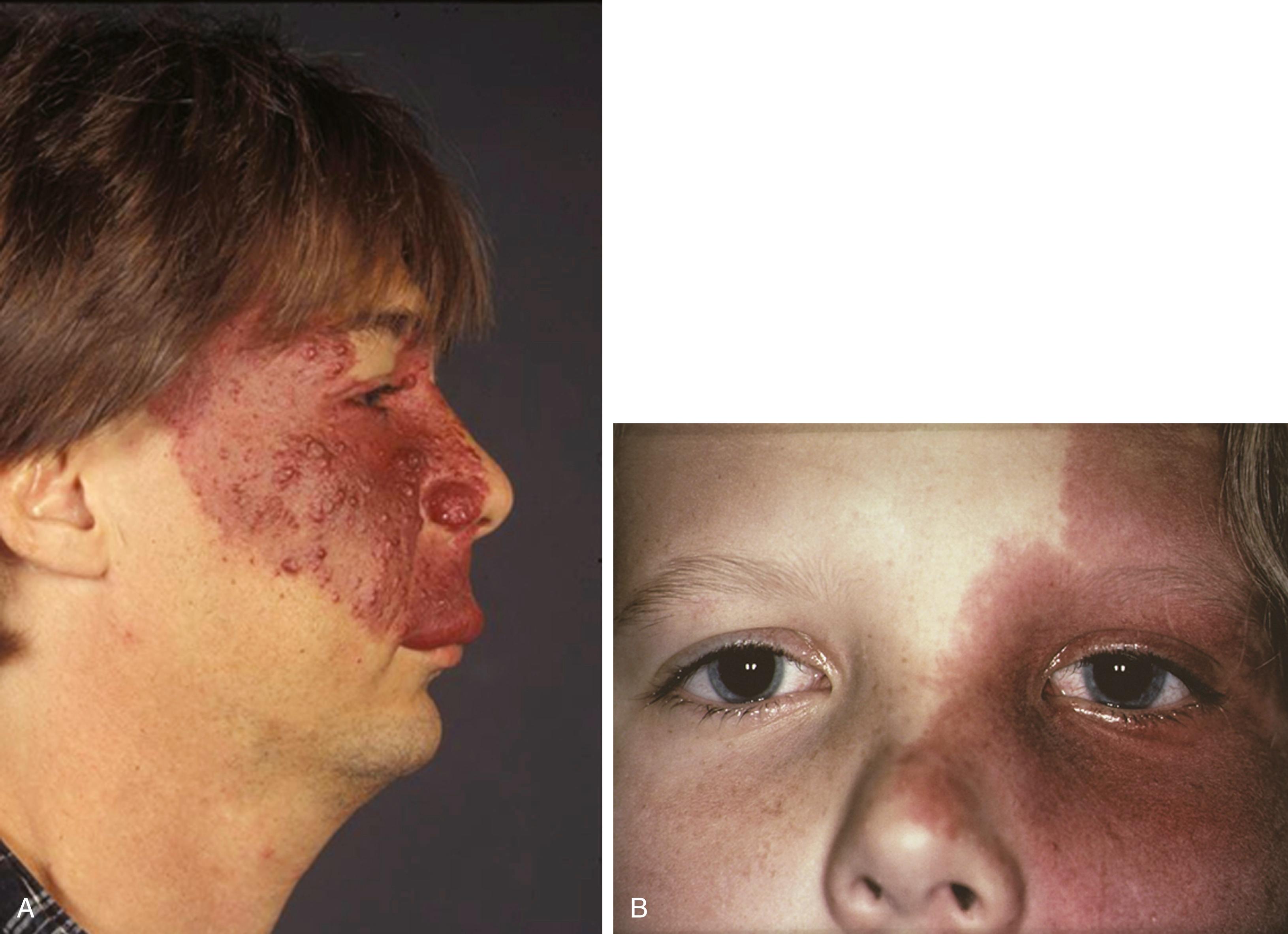
The characteristic features of Sturge-Weber syndrome (SWS) are a facial cutaneous angioma (port-wine nevus) and an associated leptomeningeal and brain angioma. The findings usually are ipsilateral but can be bilateral or even contralateral. In addition to the facial nevus, other findings include intellectual disability, seizures, contralateral hemiparesis and hemiatrophy, and homonymous hemianopia ( ). However, the clinical features are variable, and individuals with cutaneous lesions and seizures but with normal intelligence and no focal neurological deficits are common. The syndrome occurs sporadically and in all races. A somatic mutation in GNAQ has been identified in patients with port-wine stains with or without SWS. This activating mutation disrupts the q class of G-protein alpha subunits and contributes to reduced GTPase activity; this results in increased cell signaling activity ( ).
The nevus typically involves the forehead and upper eyelid but also may involve both sides of the face and extend onto the trunk and limbs ( Fig. 99.14 ). Nevi that involve only the trunk, or facial nevi that spare the upper face, rarely are associated with an intracranial angioma. The facial angioma is usually obvious at birth; it may thicken over time and develop a nodular texture. Reactive hypertrophy of adjacent bone and connective tissue may occur. Some children have the characteristic neurological and radiographic features of SWS, yet have no skin lesions. More frequently, the typical cutaneous and ophthalmic findings are present without clinical or radiographic evidence of an intracranial lesion. Only 10%–20% of children with a port-wine nevus of the forehead have a leptomeningeal angioma. Although the leptomeningeal angioma is typically ipsilateral to a unilateral facial nevus, bilateral brain lesions occur in at least 15% of patients, including some with a unilateral cutaneous nevus.
Glaucoma is the main ophthalmological condition associated with SWS. The risk of developing glaucoma has two age peaks, the first in infancy and the second in late childhood. Amblyopia and buphthalmos (enlarged globe) are present in some newborns. In others, the glaucoma becomes symptomatic later and, if untreated, causes progressive blindness. Periodic measurement of the intraocular pressure is mandatory, particularly when the nevus is near the eye. Patients with SWS also may develop choroid angiomas or heterochromasia of the iris ipsilateral to the nevus.
Epilepsy, intellectual disability, and focal neurological deficits are the principal neurological abnormalities of SWS. Seizures often begin in conjunction with hemiparesis or other focal deficits. Seizure onset before age 2 years increases the likelihood of future intellectual disability and refractory epilepsy. Intellectual disability is likely in children with refractory seizures, whereas children who never experience seizures usually have normal intelligence. Few children who have normal cognition at age 3 years will later develop severe intellectual impairment.
Epilepsy eventually develops in 72%–80% of patients with SWS with unilateral lesions and in 93% of patients with bihemispheric involvement. Although some begin in adult life, 75% of seizures begin during the first year, 86% by age 2, and 95% before age 5. Focal motor seizures or generalized tonic-clonic seizures are the most typical seizure type initially associated with SWS. Other initial seizure types are infantile spasms, myoclonic seizures, and atonic seizures. The first few seizures are often focal, even in patients who later develop generalized tonic-clonic seizures or infantile spasms. Seizures can be refractory or may remain well controlled with medication for long intervals.
The neurological impairment caused by SWS depends in part on the site of the intracranial vascular lesion. Because the occipital region frequently is involved, visual-field deficits are common. Hemiparesis often develops acutely in conjunction with the initial flurry of seizures. Although often attributed to postictal weakness, hemiparesis may be permanent or persist longer than typical of a postictal deficit. Some children develop sudden weakness without seizures, either as repeated episodes of weakness similar to transient ischemic attacks or as a single stroke-like episode with persistent neurological deficit. Not all patients have permanent focal neurological signs.
Early developmental milestones may be normal, but mild to profound mental deficiency eventually develops in approximately half of patients. Only 8% of the patients with bilateral brain involvement are intellectually normal. Behavioral concerns are frequent, even in patients who are not intellectually disabled. The clinical condition eventually stabilizes, resulting in residual hemiparesis, hemianopia, intellectual disability, and epilepsy, but without further deterioration.
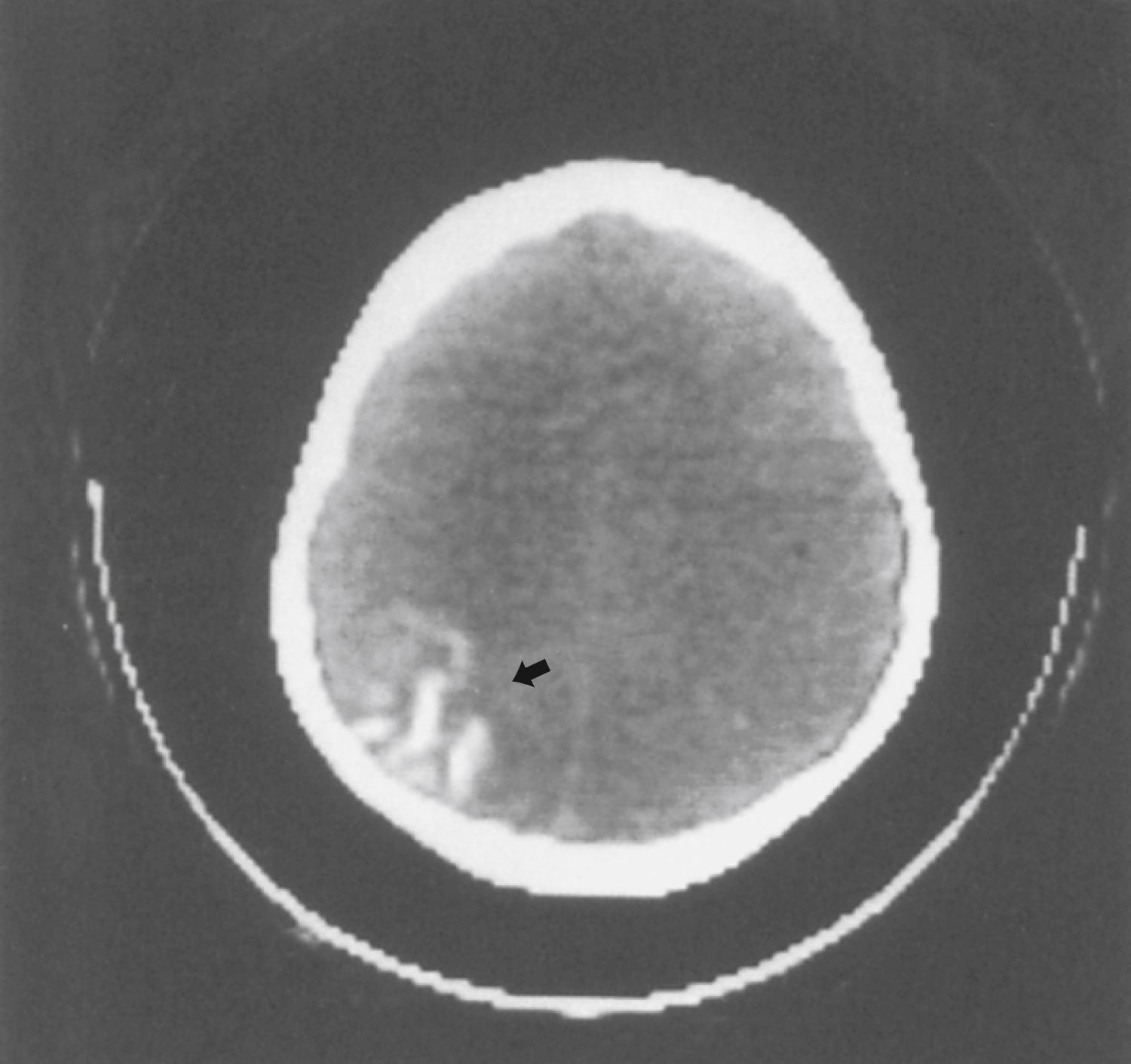
Most children with a facial port-wine nevus do not have an intracranial angioma. Neuroimaging studies help distinguish children with SWS from those with isolated cutaneous lesions. Although gyral calcification is a typical feature of SWS, the tram-track appearance first described on standard radiographs is uncommon and is almost never present in neonates. CT shows intracranial calcification much earlier ( Fig. 99.15 ) than standard skull radiographs. Extensive cerebral atrophy is apparent even with CT, but MRI more readily shows subtle atrophy.
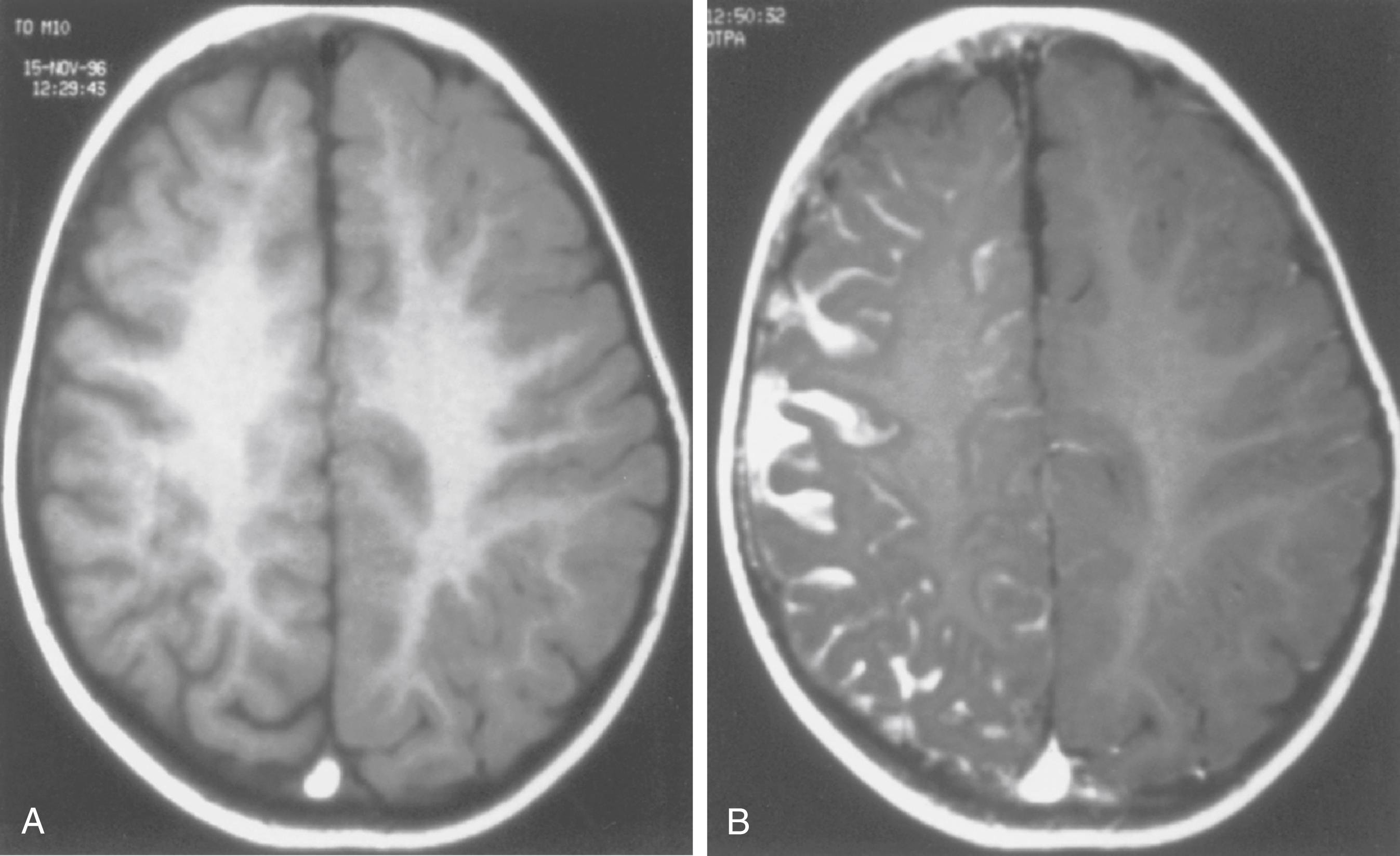
MRI with gadolinium contrast ( Fig. 99.16 ) effectively demonstrates the abnormal intracranial vessels in most patients with SWS. Positron emission tomography (PET) demonstrates reduced metabolism of the brain adjacent to the leptomeningeal lesion. However, patients with recent-onset seizures may have increased cerebral metabolism near the lesion. Single-photon emission computed tomography (SPECT) shows reduced perfusion of the affected brain. Both PET and SPECT often reveal vascular changes extending well beyond the area of abnormality depicted by CT ( ). Although functional imaging is not necessary for all patients, it may help initially to establish a diagnosis and may help characterize the extent of abnormality before surgery.
Cerebral arteriography is no longer routine in the evaluation of SWS but is sometimes useful in atypical patients or prior to surgery for epilepsy. The veins are more abnormal than the arteries, with enlarged, tortuous, subependymal, and medullary veins and sparse superficial cortical veins. Failure of the sagittal sinus to opacify after ipsilateral carotid injection may be due to obliteration of the superficial cortical veins by thrombosis; the abnormal deep venous channels probably have a similar origin as they form collateral conduits for nonfunctioning cortical veins. Microscopic hemorrhages are sometimes evident on pathology specimens, although significant intracranial hemorrhage is rare.
Generally, the more extensive the intracranial lesion, the more difficult it is to control seizures with medication. Resection of a localized brain vascular lesion or hemispherectomy can often improve seizure control and may promote better intellectual development ( ). Despite general agreement on the efficacy of surgical resection, debate remains concerning patient selection and the timing of surgery. Almost one patient in five has bilateral cerebral lesions, limiting the surgical options unless one hemisphere is clearly responsible for most of the seizures. Often the patient selected for surgery is one with refractory seizures, clinical dysfunction (e.g., hemiparesis, hemianopia) of the area selected for resection, and failure to respond to an adequate trial of anticonvulsants. Patients with less extensive lesions should have a limited resection rather than a complete hemispherectomy. The limited resection preserves as much normal brain as possible, even at the risk of having to do another operation later. Corpus callosotomy is useful for patients with refractory tonic or atonic seizures and extensive disease. In effect, the surgical considerations in children with SWS are similar to those used with other patients with epilepsy. Low-dose aspirin has been offered to patients with SWS in an effort to minimize the burden of stroke-like episodes, seizures, or cognitive impairment ( ). Aspirin is generally well-tolerated, but its efficacy has not been established.
Von Hippel-Lindau (VHL) syndrome is an autosomal dominant inherited disorder characterized by hemangioblastomas arising in the retina and CNS, as well as visceral cysts and tumors. Hemangioblastomas may occur sporadically but are usually multiple and more likely to occur in young persons. Current prevalence estimates of this disorder are approximately 1 in 40,000.
Hemangioblastomas are benign slow-growing vascular tumors that cause symptoms from hemorrhage or local mass effect. Histologically, hemangioblastomas are composed of endothelium-lined vascular channels surrounded by stromal cells and pericytes. Mast cells are present and may produce erythropoietin.
The initial symptoms of VHL usually arise from effects of the vascular anomalies in the CNS, but some patients may present with pheochromocytoma or renal, pancreatic, hepatic, or epididymal tumors. One classification system categorizes patients according to whether pheochromocytoma is present. The most common pattern of VHL findings includes retinal and CNS hemangioblastomas and pancreatic cysts ( ).
In the CNS, the most common site of hemangioblastomas is the cerebellum in approximately half of patients ( Fig. 99.17 ), followed by spinal and medullary sites. Cerebral hemangioblastomas are present in less than 5% of patients with VHL. The cerebellar hemispheres are affected far more frequently than the cerebellar vermis. Cerebellar hemangioblastomas typically present in the second decade of life.
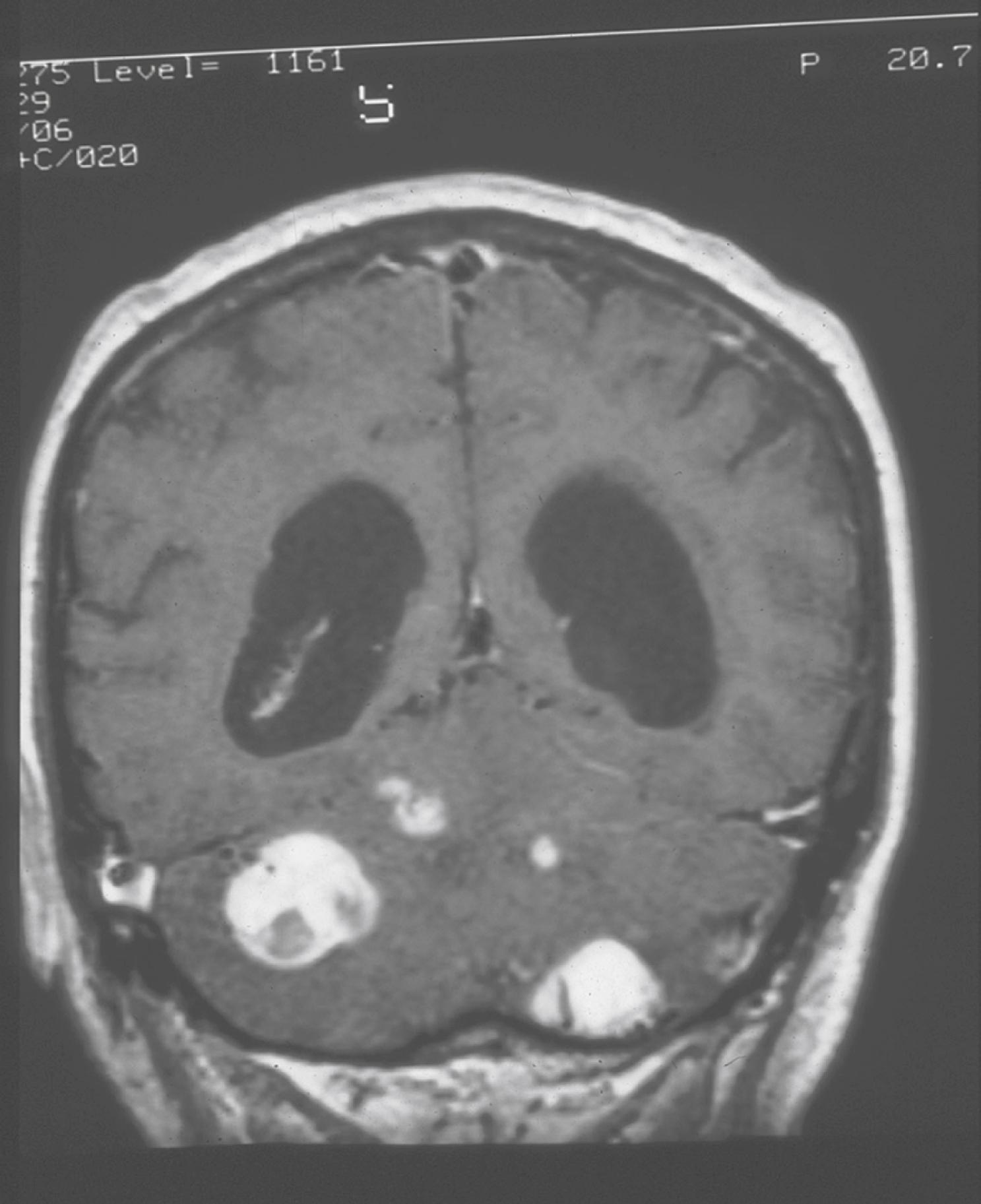
Early symptoms of cerebellar and brainstem hemangioblastomas include headache, the most common symptom, followed by ataxia, nausea and vomiting, and nystagmus. Symptoms are often intermittent or slowly progressive, but up to 20% of patients have an acute onset of symptoms following mild head trauma. Spinal hemangioblastomas typically present with focal back or neck pain and sensory loss or weakness. Because of their typical intramedullary location, spinal hemangioblastomas frequently lead to syringomyelia. The conus medullaris and the cervicomedullary junction are the most common sites. Brainstem hemangioblastomas tend to arise in the area postrema in the medulla, where they may be associated with syringobulbia. Occasionally, hemangioblastomas occur in the cerebral hemispheres or sites near the third ventricle, such as the pituitary gland or its stalk, the hypothalamus, or optic nerve. The incidence of cerebellar hemangioblastomas increases with age, and 84% of patients with VHL will develop at least one such tumor by age 60 years ( ).
Hemangioblastomas are best visualized using contrast-enhanced MRI. Routine screening of the brain and spinal cord should include precontrast and postcontrast T1-weighted images with thin sections through the posterior fossa and spinal cord and surface coil imaging of the entire spinal cord. Arteriography is not necessary for diagnosis but is valuable in demonstrating the feeding vessels if surgical resection is planned.
Endolymphatic sac tumors occur in 10%–15% of these individuals. Sometimes they are bilateral. Presenting symptoms can be abrupt change in hearing accompanying hemorrhage or vertigo and tinnitus ( ).
Childhood onset of symptoms is unusual, but retinal hemangioblastomas may occur in children as young as 1 year. Retinal hemangioblastomas may be asymptomatic, especially if they occur in the periphery of the retina. Vision loss occurs when the lesions are large and centrally located, even in the absence of hemorrhage. Arteriovenous shunting leads to fluid extravasation. Hemorrhage may lead to retinal injury and detachment, glaucoma, uveitis, macular edema, and sympathetic ophthalmitis.
Renal cysts are present in more than half of individuals with VHL, although, as with CNS and retinal hemangioblastomas, the patients may be asymptomatic. Extensive renal cysts rarely lead to renal failure. Of greater concern is renal cell carcinoma, which develops in more than 70% of patients and is the leading cause of death. These tumors are usually multiple and tend to occur at a younger age than sporadic renal cell carcinoma ( ). Simple renal cysts arise from distal tubular epithelium, whereas renal cell carcinoma tumors arise from proximal tubular epithelium.
Pheochromocytomas occur in 7%–19% of patients and may be the only clinical manifestation of VHL, even in carefully screened individuals. Tumors may be bilateral and occur outside the adrenal glands. Symptoms of pheochromocytoma include episodic or sustained hypertension, severe headache, and flushing with profuse sweating—or even hypertensive crises, stroke, myocardial infarction, and heart failure. Diagnostic laboratory investigation demonstrates excessive catecholamine concentrations in serum and urine.
Cysts and tumors of the pancreas and epididymis are also features of VHL. Pancreatic tumors include nonsecretory islet cell tumors, simple cysts, serous microcystic adenomas, and adenocarcinomas. Pancreatic cysts are the most common of these lesions and are asymptomatic unless they obstruct the bile duct or become numerous enough to cause pancreatic insufficiency. Islet cell tumors coincide frequently with pheochromocytomas, possibly because both tumors derive from neural crest cells. Epididymal cystadenomas also may be asymptomatic but palpable and cause discomfort.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here