Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Three groups of patients benefit from implant augmentation of the mandibular body, angle, and ramus. These include patients with normal, deficient, or surgically altered anatomy.
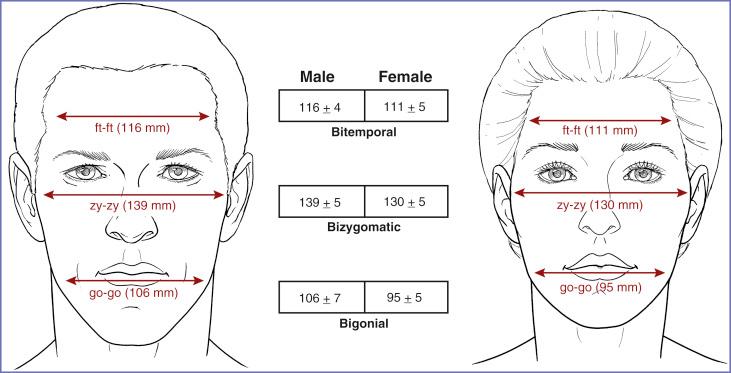
Most patients who desire mandible augmentation have lower face horizontal dimensions that relate to the upper and middle thirds of the face within a normal range ( Figs. 12.1 and 12.2 ). These patients, usually males, perceive a wider lower face as desirable. This group benefits from implants designed to augment the ramus and posterior body of the mandible and, in so doing, increase the bigonial distance. Other patients desire more definition and angularly to the mandibular border. Implants that augment the anterior mandible back to the ramus can achieve this goal.
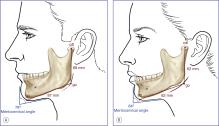
Another group of patients who benefit from mandible augmentation are those with skeletal mandibular deficiency ( Fig. 12.3 ). It has been estimated that approximately 5% of the total US population has skeletal mandibular deficiency resulting in a class II occlusal problem. The majority of these patients (approximately 80%) can have their dental relationships normalized through orthodontic tooth movement. The remaining 20%, or 1% of the total population, have mandibular deficiency that is so severe that surgical mandibular advancement would be needed to correct it.
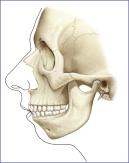
The classic method of correcting class II dental malocclusion in patients with significant mandibular deficiency, in addition to preoperative and postoperative orthodontic treatment, includes sagittal split ramus osteotomy and sliding advancement genioplasty, with possible Le Fort I maxillary impaction. This combination of procedures can provide a class I dental relationship while normalizing the skeletal contour. In patients with mandibular deficiency who have had their malocclusion corrected through orthodontics alone, mandibular osteotomy would disturb these dental relationships, requiring extensive perioperative orthodontic treatment. This type of treatment is both costly and time consuming. Alloplastic augmentation of the mandible can provide a visual effect similar to and, in my opinion, superior to that of sagittal osteotomy with advancement. Implant augmentation involves a less surgical procedure that avoids any further dental manipulation. Mandible implants can address the obtuse mandible angle with steep mentocervical angle, as well as the decreased vertical (go–cdl) and transverse ramus (go –gn) dimensions. An extended chin implant will camouflage the poorly projecting chin.
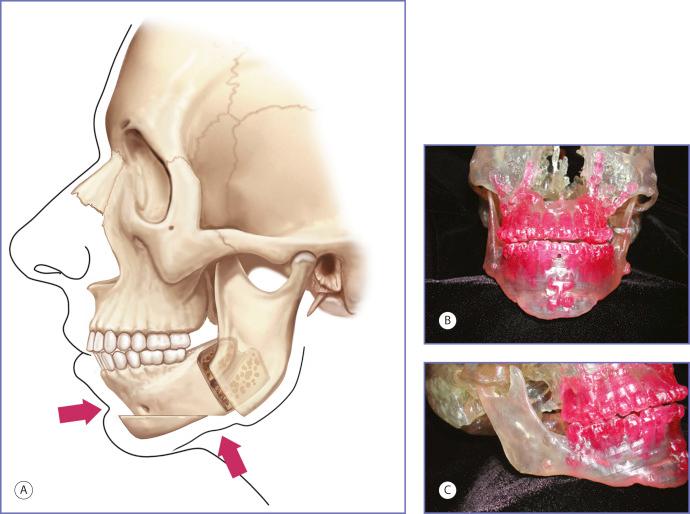
A third group of patients who may benefit from alloplastic augmentation of the mandible are patients who have had their class II dental malocclusion due to mandibular deficiency corrected by sagittal split osteotomy with advancement of the distal segment. This procedure splits or separates the tooth-bearing symphysis and adjacent bodies from the non-tooth-bearing but articulating rami. Requisites for positioning the resultant anterior and posterior segments to improve occlusion, allow bone healing, and continue joint function may result in a displeasing postoperative contour. The advancement of the distal, or tooth-bearing, segment is dictated by occlusal relations. It inevitably creates a contour irregularity at the site of the body osteotomy and distal segment advancement. This area of narrowing may be visible, and even disfiguring, in certain individuals. Positioning of the posterior segment requires that the condyle be seated in the glenoid fossa and that there be sufficient segment contact to allow bone healing. Fulfillment of these requisites dictates the position of the ramus and its angle. This may result in an aesthetically displeasing position of the ramus angle with insufficient height, insufficient width, or asymmetry ( Fig. 12.4 ). Mandible implants can be used to improve contour in these patients. Computer-aided design and manufacture (CAD/CAM) implant augmentation has proven to be a more precise method to treat the contour irregularities and asymmetries in this group of patients. The use of CAD/CAM implants is presented in Chapter14, Chapter15 .
Mandibular body and ramus augmentation in women with normal-dimensioned mandibles should be conservative with the intention of providing definition. The anthropometric measurements provided by Farkas ( Fig. 12.1 ) help in understanding our visual interpretation of male and female patients with normal mandibular morphology and dimensions who undergo mandibular augmentation. These data show that all transverse facial dimensions are greater in men than in women and that the bigonial distance is the transverse facial dimension that has the greatest difference between sexes. In other words, the lower third of women’s faces tends to be absolutely and relatively narrower than that of men. Hence, when normal male mandibles undergo augmentation, they may be perceived as stronger. However, when normal female mandibles undergo aggressive augmentation, they may be perceived as less feminine.
Aggressive augmentation of the female mandible risks its masculinization.
Physical examination is the most important element in preoperative assessment and planning. Reviewing life-size posteroanterior and lateral photographs with the patient can be helpful when discussing aesthetic concerns and goals. To allow the patient to understand the scale and scope of augmentation, it is useful to have sample implants available to demonstrate on a model skull and to apply these implants to the relevant area of the patient’s face.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here