Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
When there is sustained occlusion of arterial blood supply or venous drainage, a type of necrosis can occur called infarction . Common clinical examples of infarction are myocardial infarction (affecting the heart) and cerebral infarction or stroke (affecting the brain). In these situations, the myocardial or cerebral vessels are affected by atherosclerosis, thrombosis or embolism. If the blood supply is temporarily altered, then this can lead to ischaemia of the tissues; sustained ischaemia leads to infarction.
In most situations, infarction arises as a consequence of thrombotic or embolic events in the arterial system, though occlusion of venous drainage may also result in infarction.
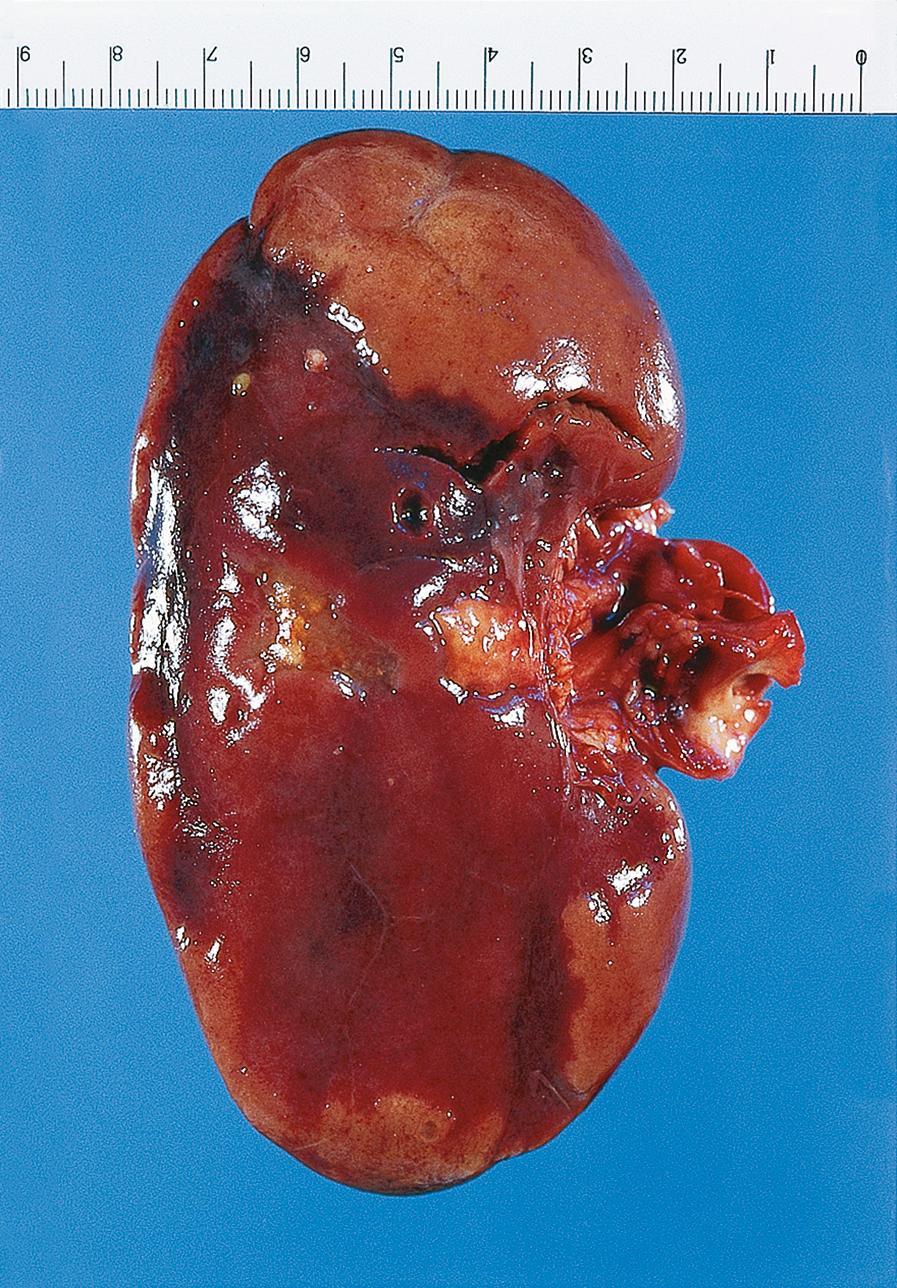
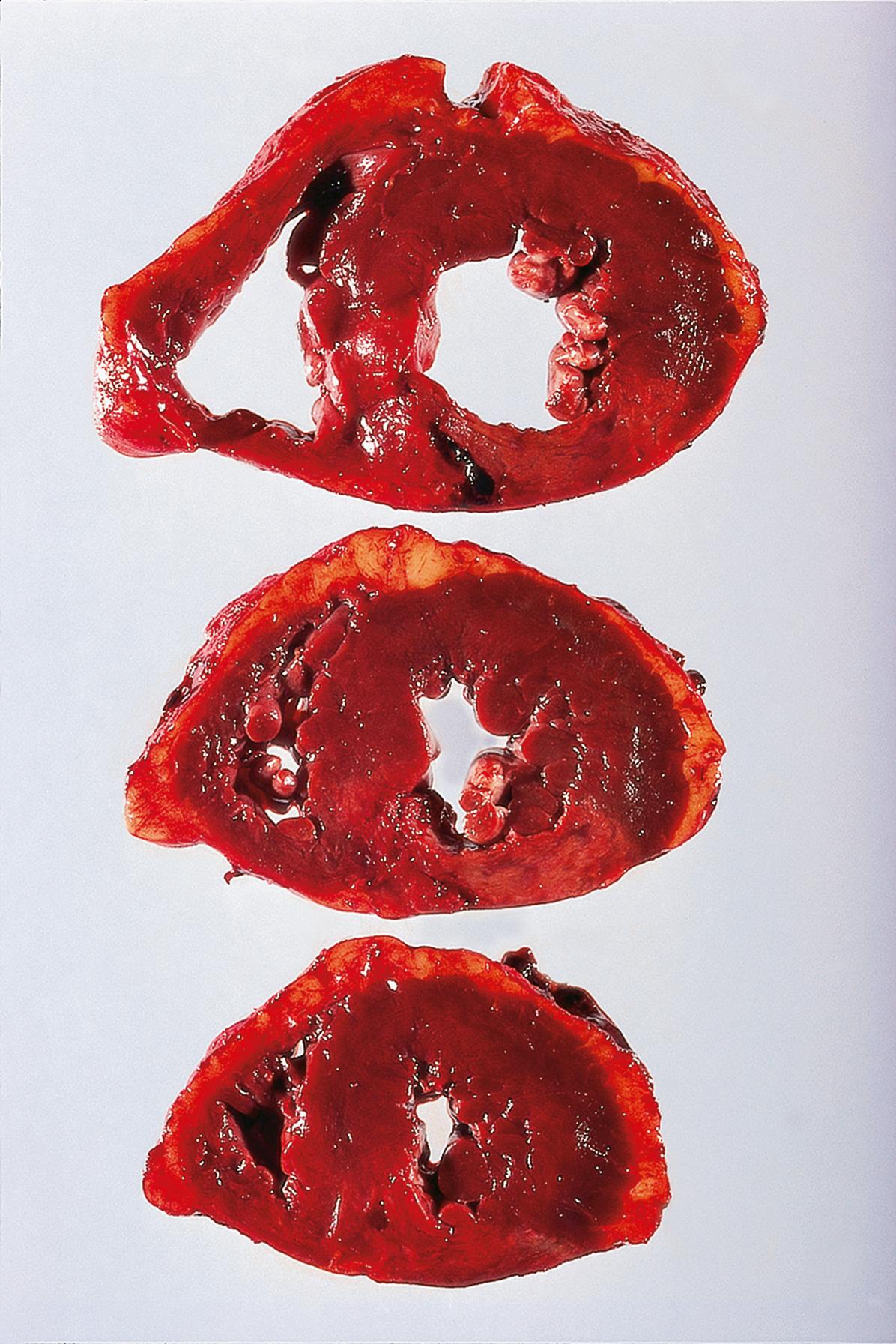
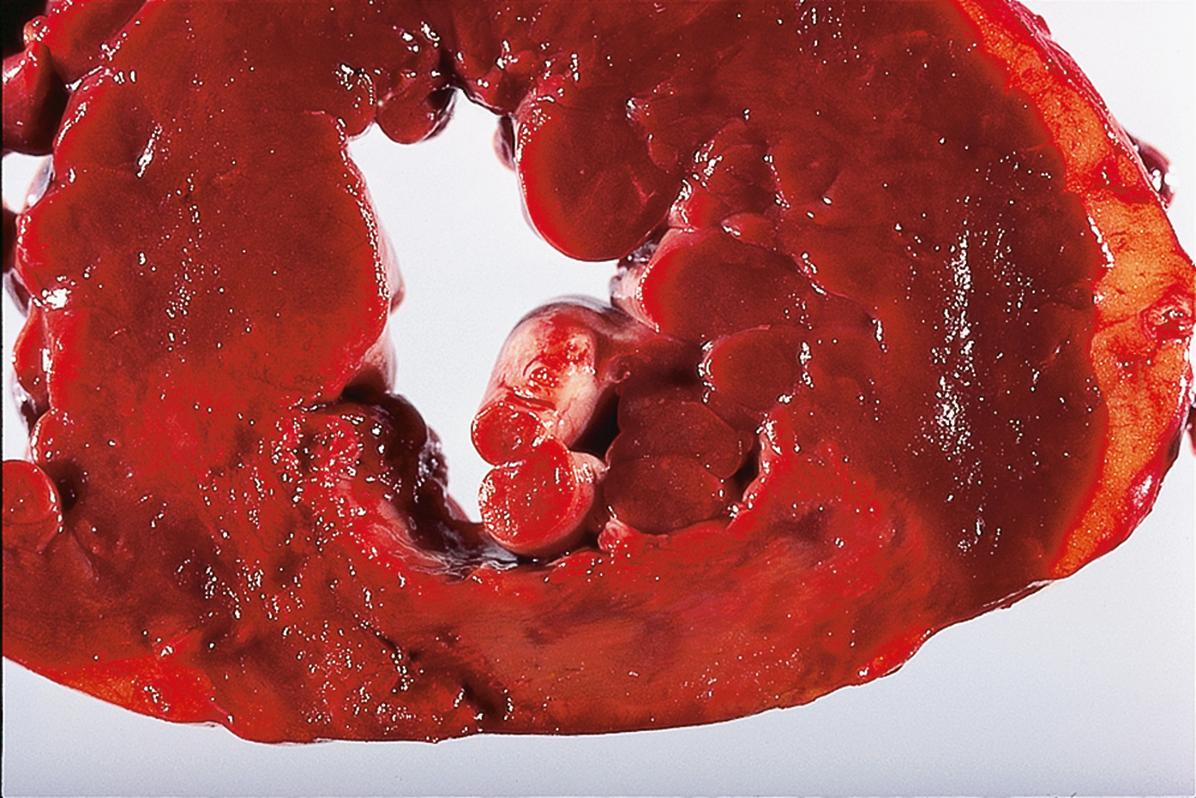
Arterial infarction is usually due to complete blockage of an artery by thrombosis or embolism. Arterial thrombosis is generally a complication of pre-existing atheroma (see Ch. 8 ). Embolisation in the arterial system is most commonly from the heart, either from mural thrombus (see Fig. 9.3) or thrombus occurring on heart valves ( vegetations ; see Figs 11.16 and 11.17) or from thrombosis and/or atheroma of arteries. Examples of infarcts from the kidney and myocardium are shown in Figs 10.1 and 10.2 , respectively, and from the cerebellum in Fig. 23.2.
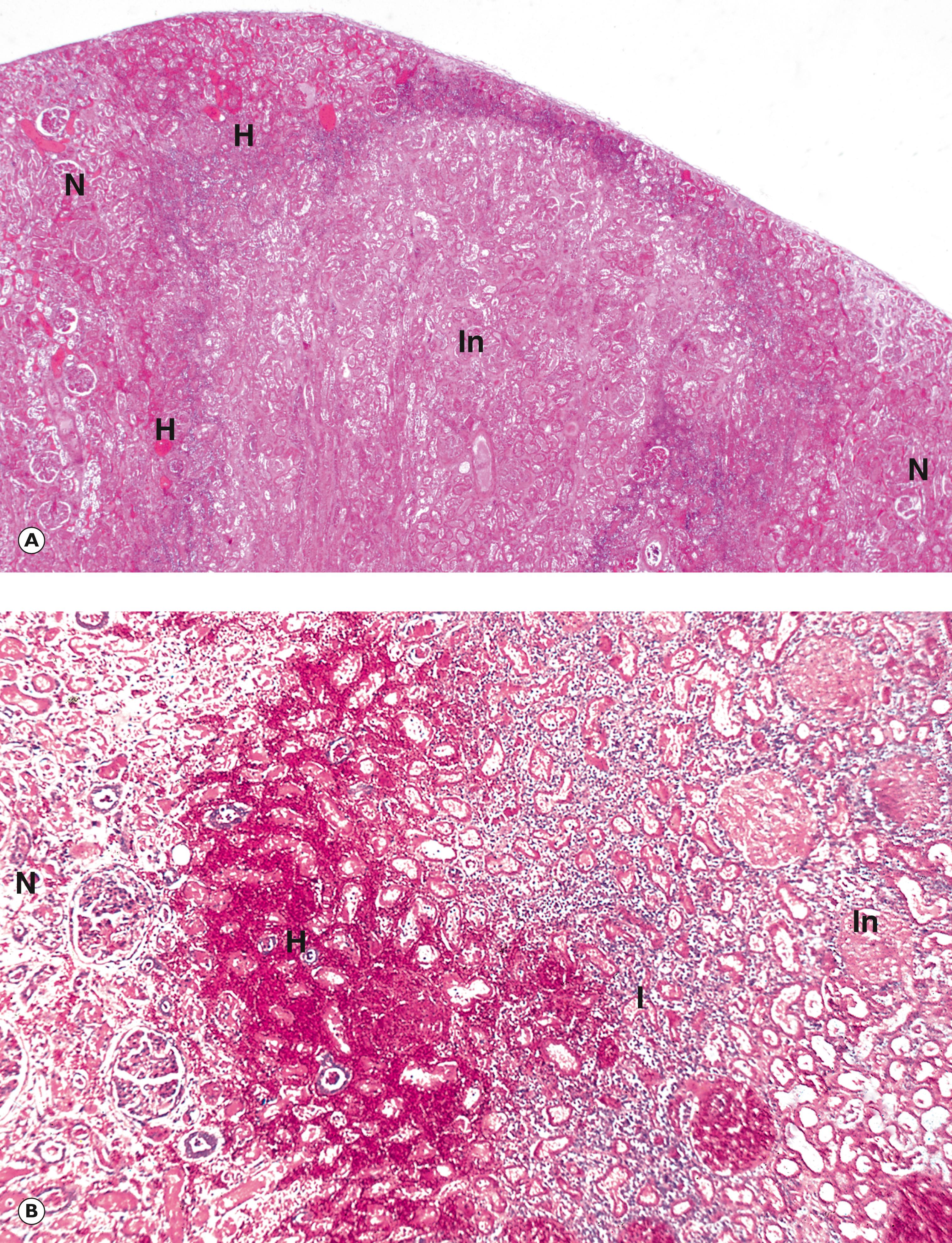
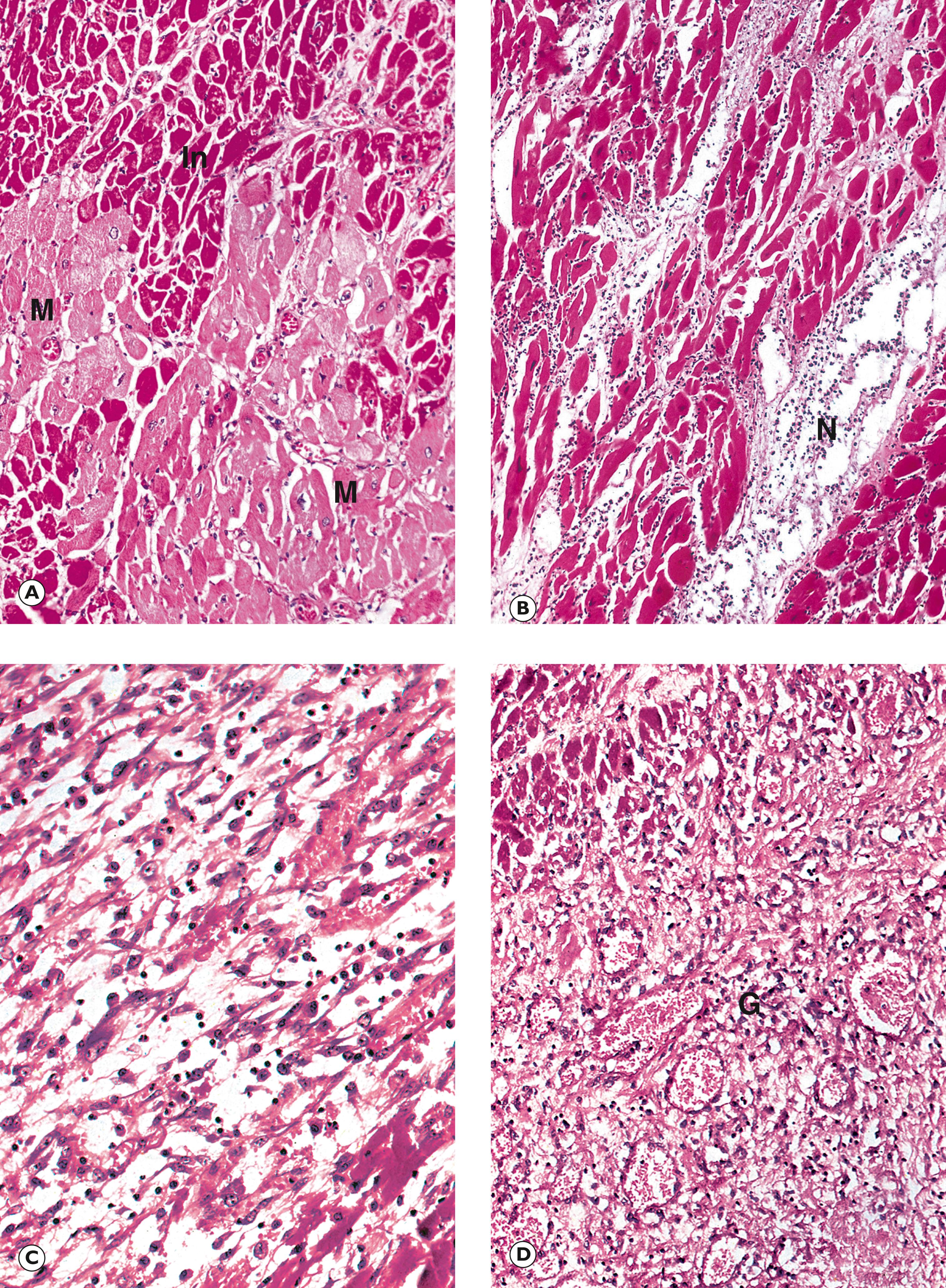
Venous infarction most commonly arises as a consequence of mechanical compression of blood vessels, particularly in organs that receive their blood supply via a vascular pedicle. Such organs may become infarcted if the pedicle becomes twisted, for example torsion of the testis (see Fig. 19.1), or constricted by becoming entrapped in a narrow space, for example bowel infarction caused by hernial strangulation ( Fig. 10.5 ). In such cases, venous obstruction occurs as extrinsic pressure compresses the thin-walled, low-pressure veins without initially compromising the arteries. As a consequence, tissues become massively suffused with red cells and prolonged venous obstruction eventually causes the tissue to become ischaemic owing to stasis of blood. The resulting cessation in tissue perfusion results in infarction. Venous infarction may also occur in the brain as a complication of dural sinus thrombosis.
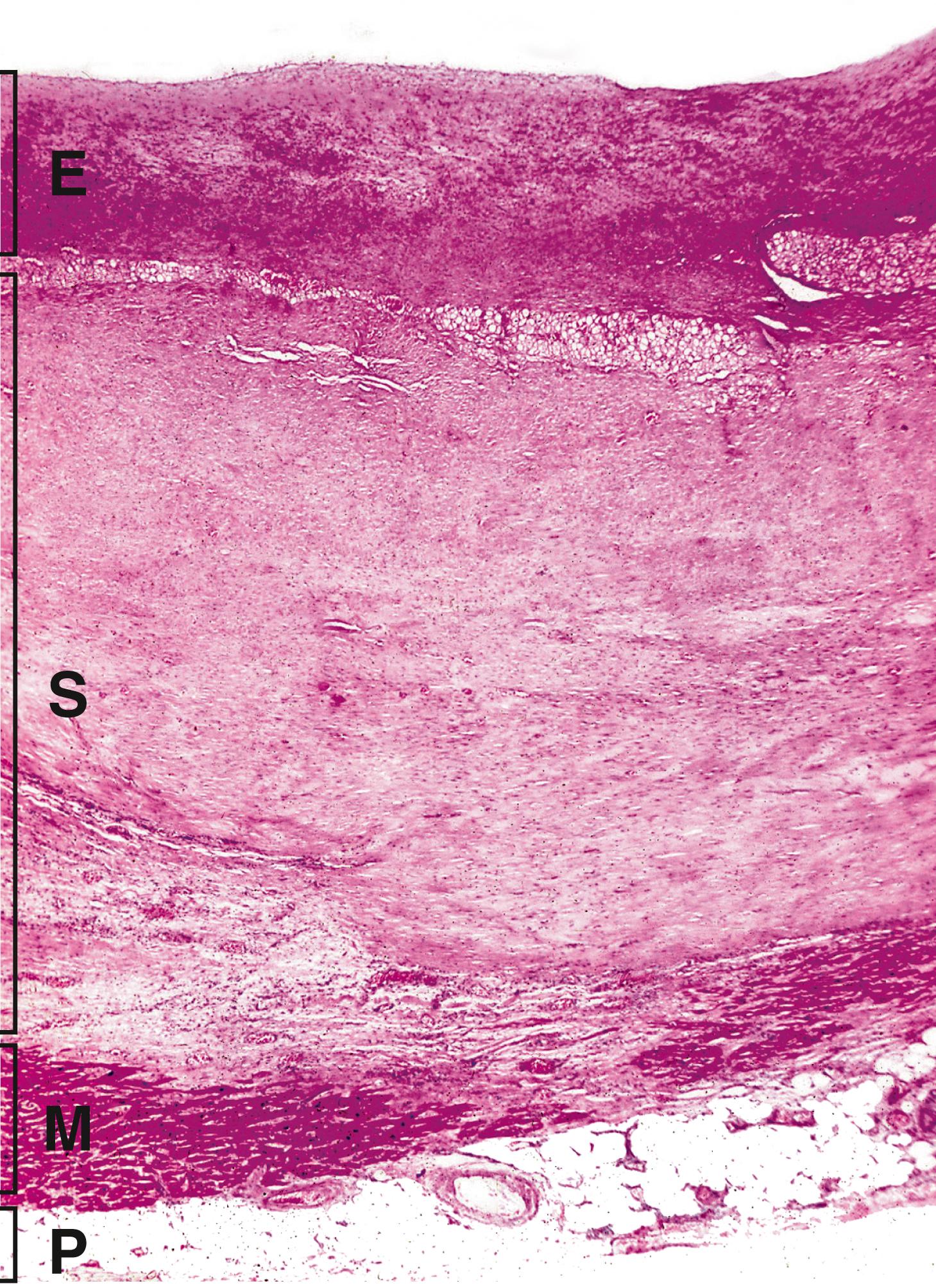
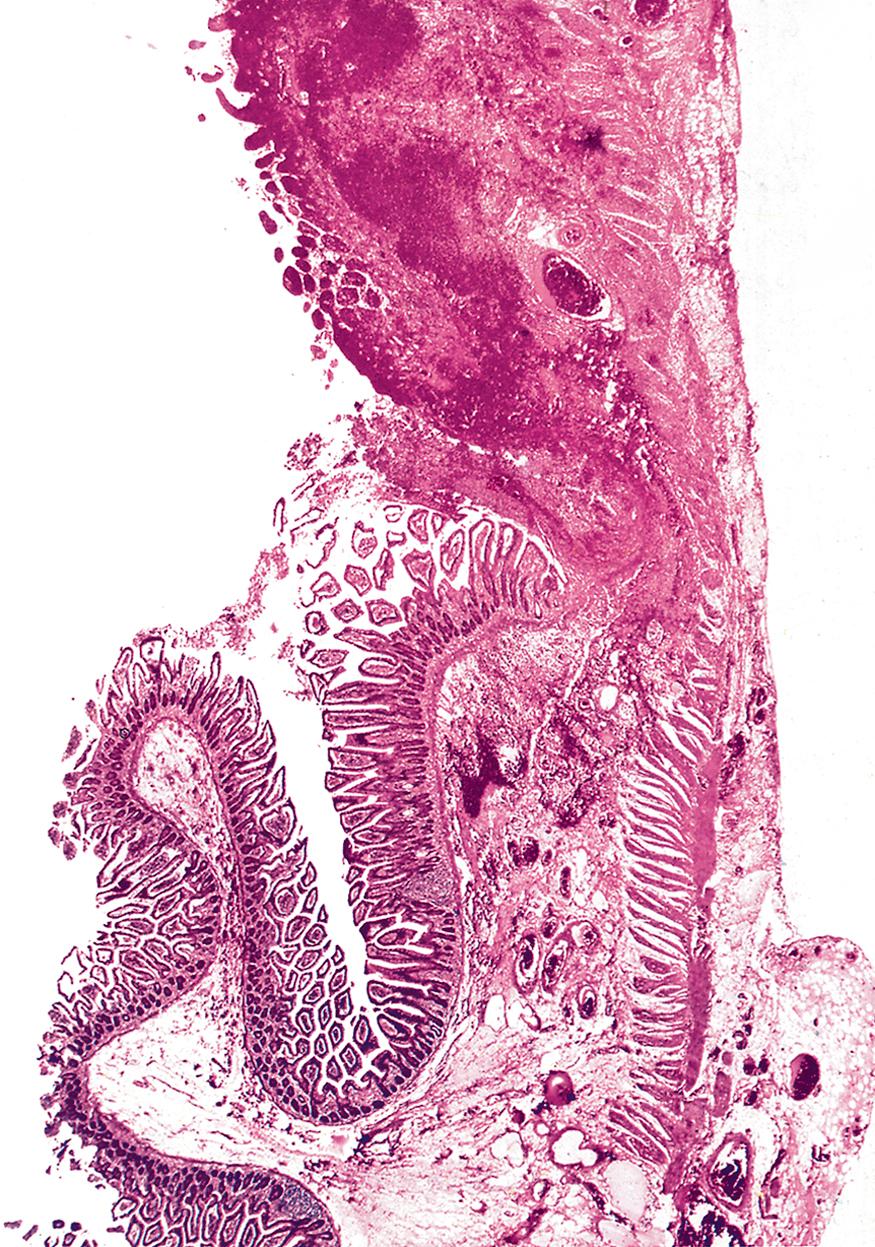
When infarction is due to simple cessation of arterial supply, the shape of the infarct reflects the arterial territory involved. In most organs (e.g. kidney, spleen or brain), the infarct appears wedge-shaped in section, with the broad part of the wedge at the periphery ( E-Fig. 10.1 G ). In contrast, infarcts in the heart are not wedge-shaped, but are classified as subendocardial or transmural depending on the underlying cause ( E-Figs 10.2 and 10.3 ). Transmural infarctions, i.e. those involving the full thickness of the ventricle, are caused by an obstruction of one of the coronary artery territories. As the coronary arteries are end arteries , blockage of a major coronary artery branch causes necrosis of the segment of heart muscle supplied by that branch. Subendocardial infarctions can be seen in cases of global poor perfusion, such as in cases of systemic shock. As their name suggests, they do not affect the thickness of the muscle wall and are confined to the innermost aspect of the heart muscle, as this region receives its blood supply from the lumen of the ventricle.
Like most forms of tissue damage, infarction excites an acute inflammatory response followed by replacement of necrotic tissue by granulation tissue, which then undergoes fibrous repair and scarring (see Ch. 3 ). The appearance of infarcts histologically and to the naked eye thus depends on how far this sequence has progressed. One important exception to this process is the brain, which does not normally show the usual processes of granulation tissue formation and fibrous repair. Cerebral infarcts undergo central liquefaction known as colliquative necrosis (see Ch. 2 ) with reactive gliosis at the margins of the lesion (see Ch. 23 ). Old cerebral infarcts are usually marked by a cystic area surrounded by a zone of gliosis; brain infarction is illustrated in Figs 2.7B and 23.2.
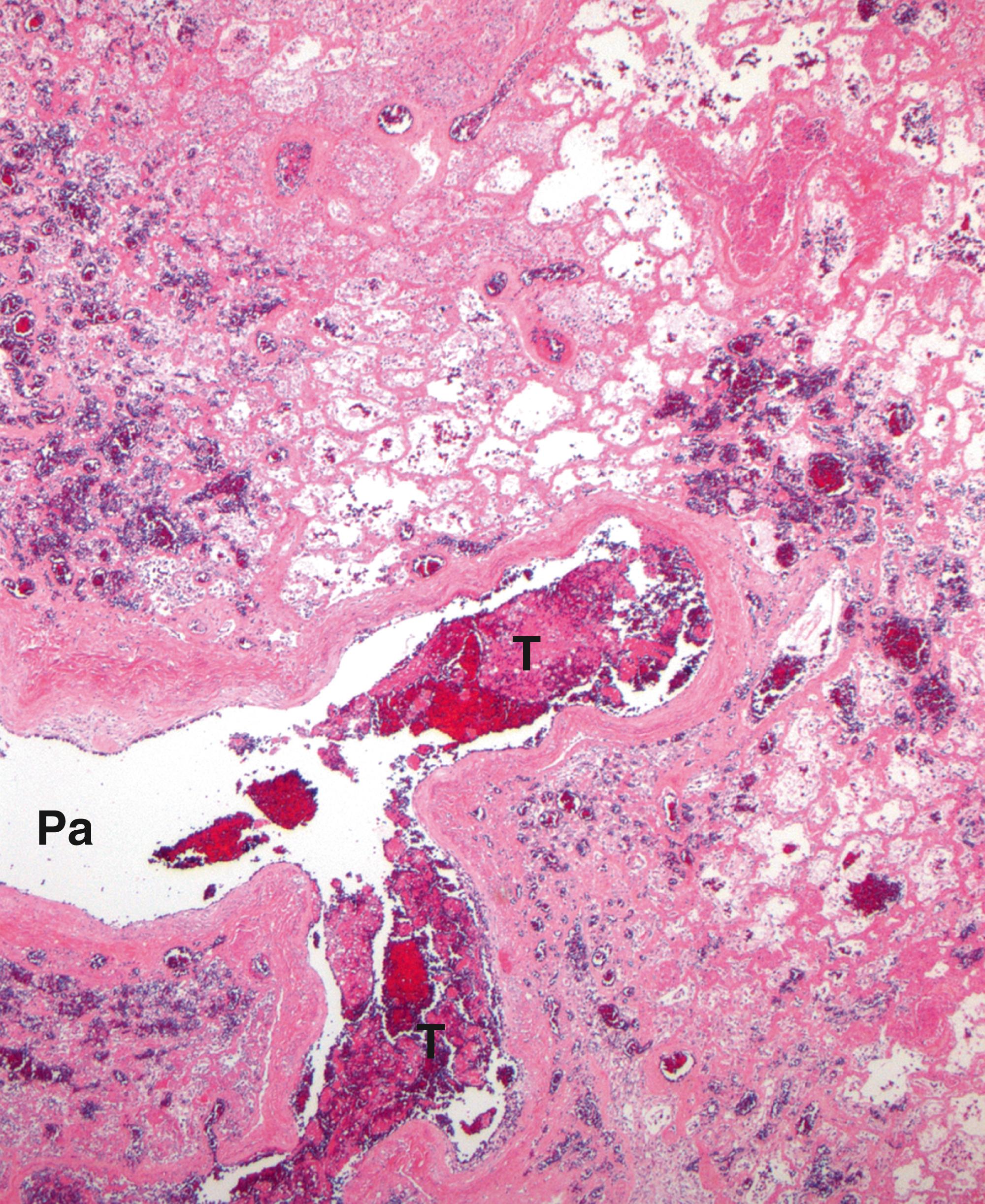
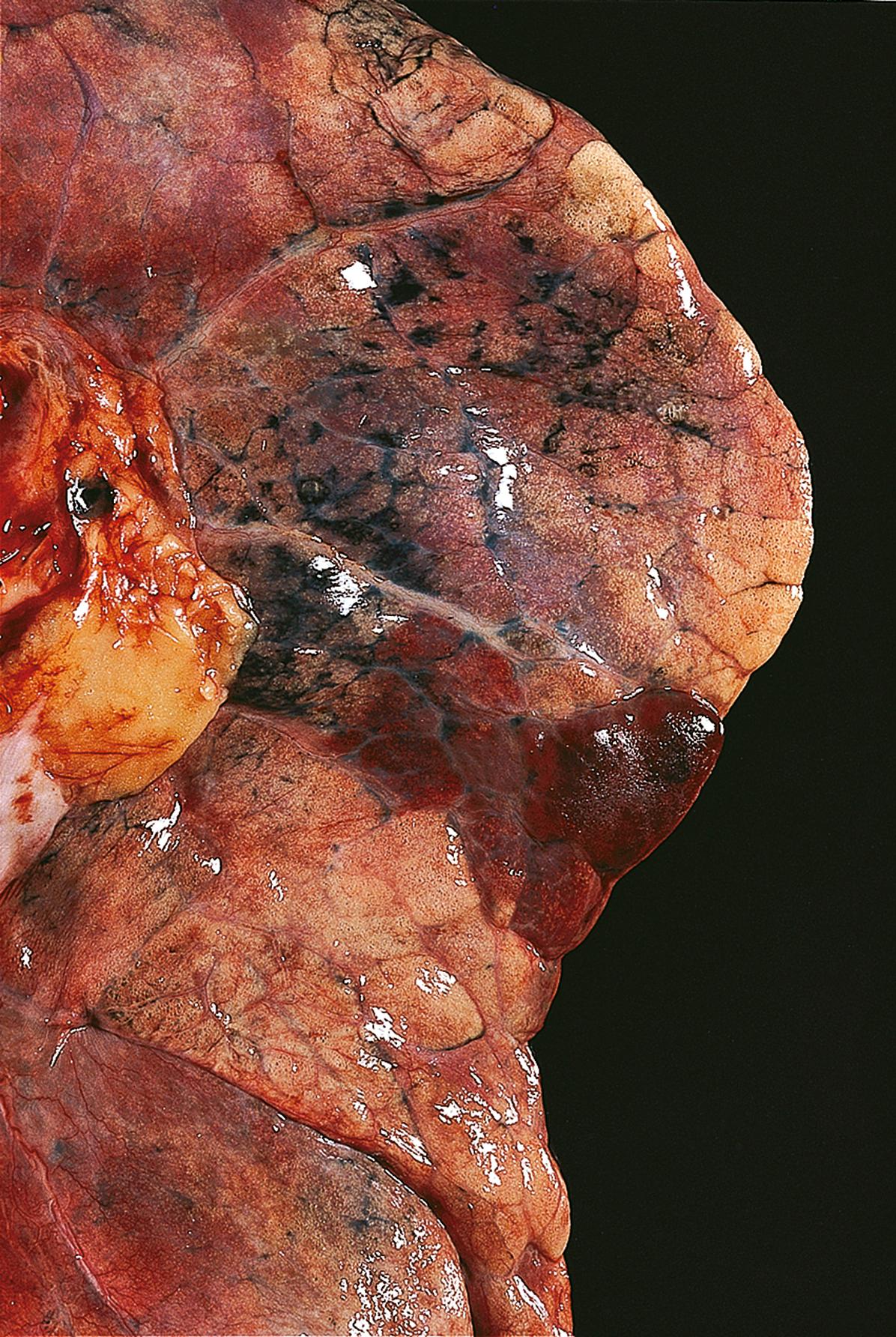
Organs in which there are extensive capillary, sinusoidal or arteriovenous anastomoses often have infarcts that are dark red in their early stages because of congestion with blood and haemorrhage (from the Latin, infarcire , meaning to stuff). Important examples are the lung ( Fig. 10.4 ) and spleen.
H hyperaemic zone I acute inflammation In infarcted region N normal S scar
Acute myocardial infarctions can be subdivided by the pattern of ECG changes noted at initial presentation, as ST elevation myocardial infarction (STEMI) and non-ST elevation myocardial infarction (NSTEMI). STEMIs tend to occur secondary to acute coronary artery thrombosis and are usually treated by a minimally invasive surgical procedure to remove the thrombus ( percutaneous coronary intervention or PCI ) generally followed by medical therapy. NSTEMIs may be caused by a less severe blockage of a coronary artery and, in general, can be treated with up-front medical therapy and subsequent coronary intervention.
There are other ways to describe myocardial infarctions, notably type 1 myocardial infarction and type 2 myocardial infarction. Type 1 myocardial infarction can be diagnosed when clinical features of myocardial infarction – chest pain, arm/neck pain, sweating, nausea – are present, together with a rise in troponin, a blood test finding indicative of myocyte damage, and ECG changes. A type 2 myocardial infarction may not present with the typical clinical features of myocardial infarction and is better termed secondary ischaemic cardiac injury.
Ischaemic heart disease is a major cause of death in all industrialised countries. Atherosclerosis of coronary arteries accounts for the vast majority of cases, hence the alternative term coronary artery disease (CAD) . Three main clinical syndromes are recognised:
Stable angina pectoris (from the Latin for ‘choking pain’ of the ‘chest’). Angina describes a complex of symptoms arising from paroxysmal, often recurring and brief episodes of reversible myocardial ischaemia. Symptoms arise as a consequence of increased load on the heart (e.g. during exercise) in the face of coronary artery stenosis through atheroma. Thus, there is insufficient perfusion of the myocardium as coronary artery blood flow is limited by atheroma. Stable angina may progress to acute myocardial infarction with increasing atheromatous occlusion and/or thrombosis.
Acute myocardial infarction (heart attack). Two main pathological forms are recognised:
Transmural infarction . This involves the full thickness of a segment of the ventricular wall and is associated with complete blockage of a main coronary artery by thrombosis, often superimposed on an area of atherosclerotic narrowing (see Ch. 8 ). Complications of an acute transmural infarction include death, cardiac dysrhythmia, ventricular aneurysm, acute valve dysfunction and pericarditis.
Subendocardial myocardial infarction . In this case, myocardial necrosis is limited to cells in the inner third of the ventricular wall. The pathogenesis of infarction is limitation of flow to the end arteries supplying the inner part of the ventricular wall, rather than complete occlusion of the main arterial trunks.
Sudden cardiac death (immediately fatal myocardial infarction or dysrhythmia due to acute ischaemia resulting in death).
The histological changes following infarction are illustrated in Figs 10.2 and 10.3 .
G granulation tissue In infarcted fibres M normal fibres N neutrophils
| Disorder | Definition/example | Features | Figure |
|---|---|---|---|
| Arterial infarction | Renal infarction | Common and often asymptomatic. Typically wedge-shaped, base towards capsular surface In initial stages demarcated from surrounding, non-infarcted tissue by hyperaemic zone. Heals leaving fibrous scar. |
10.1 |
| Myocardial infarction | Earliest histological changes detected within 4 hours; established by 12 to 24 hours. | 10.2 10.3 |
|
| Pulmonary infarction | Initial stage, firm, dark red, wedge-shaped. Sharp pleuritic pain plus pleural rub. Can result in sudden death. |
10.4 | |
| Cerebral infarction | Earliest changes within hours of infarction; established at 6 to 12 hours. | 2.7 23.2 |
|
| Venous infarction | Torsion of testis | Twisting of spermatic cord leads to compression of thin-walled veins and subsequent infarction. | 19.1 |
| Small bowel volvulus | Initially intensely congested with blood. Bowel becomes progressively ischaemic. Necrosis unless venous obstruction relieved. |
10.5 |
E endocardium M surviving myocardium P pericardium Pa pulmonary artery branch S scar T thrombus
A man dies two weeks following an acute myocardial infarction. At post mortem examination, a histological section of the infarct shows that the necrotic myocardium has largely been replaced by capillaries, fibroblasts and collagen. Which of the inflammatory cells in this lesion has the most important role in the healing process?
Macrophages
Plasma cells
Neutrophil polymorphs
Eosinophils
Lymphocytes
Which ONE of the following processes is unlikely to result in infarction?
Thrombosis
Venous obstruction
Embolism
Atherosclerosis
Dissection
Which of the following processes is involved in the pathogenesis of cerebral infarction?
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here