Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Paraneoplastic syndromes in the context of hematologic malignancies have been reported among multiple organ systems, including the nervous system, skin, bone marrow, and kidneys. Paraneoplastic glomerular injury has been demonstrated to be the result of tumoral production of cytokines, monoclonal and amyloid proteins, cryoglobulins, and the development of autoimmune diseases. Direct leukemic or lymphomatous infiltration of the kidney will not be included in this discussion, because paraneoplastic glomerulopathy (PNGN) refers to renal disease that is not a direct result of tumor burden, invasion, or metastasis.
Box 23.1 illustrates the 2016 World Health Organization classification of hematologic malignancies. The major subtypes are grouped by lineage into lymphoid, myeloid, and histiocytic/dendritic neoplasms. This chapter will focus on the lymphoid and myeloid lineages, because there are no reports of PNGN with the latter subgroup. The prevalence and types of PNGN can vary significantly among the two major subtypes. Overall, the reported incidence of PNGN related to hematologic malignancies is quite rare, with the total number of case reports in the literature only slightly in excess of 200. When compared with myeloid neoplasias, PNGN has been reported relatively more frequently in patients with the lymphoid malignancies, specifically Hodgkin lymphoma (HL), non-Hodgkin lymphoma (NHL), and chronic lymphocytic leukemia (CLL). Among the lymphoid neoplasias, paraneoplastic minimal change disease (MCD) and focal segmental glomerular sclerosis (FSGS) are more frequently reported with diseases of the T-cell lineage like HL, whereas paraneoplastic membranoproliferative glomerulonephritis (MPGN) and membranous nephropathy (MN) are more commonly reported with B-cell lineage tumors like CLL.
Hodgkin lymphoma
Non-Hodgkin lymphoma, which includes
Mature B-cell neoplasms
Mature T and natural killer cell neoplasms
Posttransplant lymphoproliferative disorders
Myeloproliferative neoplasms
Chronic myeloid leukemia
Polycythemia vera
Primary myelofibrosis
Essential thrombocythemia
Myeloid/lymphoid neoplasms with eosinophilia and rearrangement
Myelodysplastic/myeloproliferative neoplasms
Chronic myelomonocytic leukemia
Myelodysplastic syndrome
Acute myeloid leukemia and related neoplasms
B- and T-cell lymphoblastic leukemia
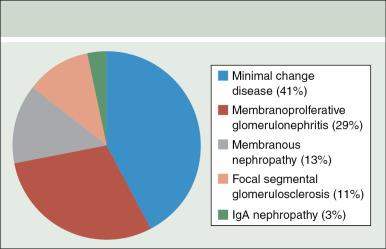
The frequency of renal involvement with lymphoid neoplasia ranges from 16% to 33%, depending upon the case series. , Varied patterns of glomerular lesions have been reported with the lymphoid malignancies, but there seems to be predilection for specific lesions. The following subsections present the paraneoplastic lesions associated with lymphoid neoplasia in their order of reported relative frequency. Fig. 23.1 illustrates the relative distribution of the patterns of PNGN based on case reports and case series in the literature. MCD and FSGS, which are glomerular lesions characterized by podocyte injury, account for more than 50% of case reports. Proliferative lesions like MPGN account for about one-third of the reported cases. Most of the discussion in this section will focus on HL, NHL, and CLL because most of the cases of PNGN have been linked with these diseases. Lymphoid neoplasias that have been less frequently associated with a PNGN are discussed in the final portion of this section.
MCD and FSGS are discussed together in this section because both entities present with podocyte injury, proteinuria, and minimal immune deposits. PNGN in patients with HL has been reported in up to 0.4% of cases. MCD is the most commonly reported glomerular lesion with HL. It is more frequently seen in the classic form of HL, including the mixed cellularity and the nodular sclerosing subtypes. The secondary MCD associated with HL exhibits a high degree of steroid and cyclosporine resistance, but generally goes into remission with successful treatment of the HL. The occurrence of nephrotic syndrome (NS) can precede the development of malignancy by several years, and recurrence of NS can often herald relapse of the lymphoma. The incidence of paraneoplastic FSGS is about one-tenth that of MCD. This form of secondary FSGS will also respond to chemotherapy administered for treatment of the primary lymphoma. Among patients with NHL, mantle cell lymphoma (MCL) has been reported in association with FSGS in two cases, and in both, the glomerular disease responded well to chemotherapy for the MCL. ,
The pathogenesis of paraneoplastic MCD and FSGS remains poorly defined. Both lesions are essentially the sequela of injury and dysfunction of the glomerular podocyte. As such, paraneoplastic MCD and FSGS may result from abnormal tumoral expression of proteins, which are involved with cytoskeleton organization and podocyte signaling. There are several tumoral proteins of interest in this regard. Paraneoplastic MCD in patients with HL may be related to the increased production of the T-helper 2 cell (Th2) cytokine interleukin (IL)-13. In patients with HL, T-cells tend to expand towards the Th2 cell, and IL-13 levels are increased in the serum of patients with MCD. In a rat model, increased production of IL-13 produces an MCD-type nephropathy. Another putative protein is c-mip (c-maf inducing protein). Increased expression of c-mip switches off the interaction between nephrin and tyrosine kinase-fyn. This in turn leads to defects in cytoskeleton organization and proximal podocyte signaling that may lead to the development podocyte disease. Increased production of vascular endothelial growth factor (VEGF) has also been associated with the development of podocyte dysfunction. There are cases of paraneoplastic FSGS with HL and NHL in which altered T-cell function led to abnormal secretion of VEGF, which in turn led to increased glomerular permeability. A similar pattern of podocyte injury has been observed with the tumoral cytokine, transforming growth factor beta (TGF-β). ,
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here