Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Injuries to the hallux metatarsophalangeal (MTP) joint are not uncommon, particularly in the running athlete, and may result in chronic pain and deformity. Causes of hallux injuries range from soft-tissue disruption to overuse and degeneration. Trainers and physicians may fail to recognize the potential dysfunction of these injuries, thus providing inadequate care and protection from further injury. Long-term sequelae of even isolated soft-tissue injury include flexor hallucis longus (FHL) tendon tears, hallux valgus or varus, cock-up deformity with or without interphalangeal (IP) joint contracture, and degenerative joint disease (DJD), i.e., hallux rigidus.
Clanton and Ford found that foot injuries rank third behind ankle and knee injuries as the most common time-loss injury among university athletes. Of these foot injuries, a large proportion were sprains of the forefoot and, more specifically, the hallux MTP joint. Hunt and colleagues demonstrated that the incidence of turf toe injures was 0.062 per 1000 athlete exposures, but were 14 times more likely to occur during games than practice and more common in running backs and quarterbacks. In the author’s practice, we have seen a number of professional athletes with a broad range of injuries to the great toe and base this chapter on our experiences.
Great-toe injuries can lead to significant functional disability, especially when not recognized early. In the short term, these injuries can result in difficulties with push-off strength and running. Long-term sequelae typically involve pain due to progressive degeneration. Physicians involved in the treatment of foot and ankle injuries, especially those caring for athletes, must become familiar with the spectrum of injuries about the hallux MTP joint, the biomechanical implications, the conservative and operative treatments for these injuries, and the late sequelae encountered in these athletes.
The provider responsible for the care of athletes with great-toe injuries must have a keen knowledge of the anatomy of the hallux MTP joint. In the simplest of terms, the motion of the joint consists of rolling, sliding, and compression. More specifically, the morphology of this joint allows for plantarflexion and dorsiflexion but very limited abduction and adduction. The fact that there is more than one center of motion contradicts the theory of a simple, hinged joint. Instead, the joint is a dynamic acetabulum or “hammock” as described by Kelikian. The joint articulation provides little of the overall stability because of the shallow, glenoid-like cavity of the proximal phalanx. Most of the stability comes instead from the capsular-ligamentous-sesamoid complex, which is described in detail later.
There are two sets of ligaments that contribute to the stability of the metatarsal (MT) head as it articulates with the proximal phalanx: the medial and lateral collateral ligaments and the metatarsosesamoid suspensory ligaments. The fan-shaped medial collateral ligament is composed of the medial MTP ligament and the medial metatarsosesamoid ligament ( Fig. 21.1 ). The lateral collateral ligament is structured in a similar fashion.
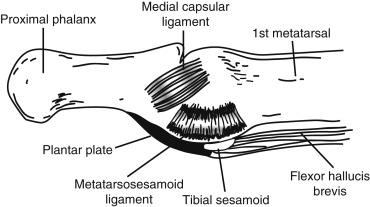
In addition to the collateral ligaments, the strong, fibrous plantar plate (see Fig. 21.1 ) also affords structural support. The capsular ligamentous complex of the hallux MTP joint, distal to the sesamoids, is actually a confluence of structures including the plantar plate, collateral ligaments, the flexor hallucis brevis (FHB), the adductor hallucis, and abductor hallucis tendons. This plantar plate is attached firmly to the base of the proximal phalanx and only loosely attached at the MT neck through the capsule.
The split tendon of the FHB runs along the plantar aspect of the hallux and envelops the sesamoids before inserting at the base of the proximal phalanx as the capsular-ligamentous complex ( Fig. 21.1 ). The two sesamoids are united by a thick, intersesamoid ligament, all of which help to maintain the course of the FHL tendon. Adding to the stability of the hallux MTP joint are three other intrinsic muscles of the great toe. The extensor hallucis brevis (EHB) originates at the fascia overlying the sinus tarsi and runs obliquely to attach into the extensor mechanism on the dorsum of the MTP joint. It functions primarily as an extensor of the hallux MTP joint. On the plantar aspect, the abductor and adductor hallucis tendons insert on the medial and lateral aspects of the hallux MTP joint, respectively. These tendons blend into the capsular-ligamentous complex, as well as the sesamoids, to provide additional structural support ( Fig. 21.2 ).
Not a simple, hinged joint.
Most of the stability comes instead from the capsular-ligamentous-sesamoid complex.
Capsular ligamentous complex: plantar plate, collateral ligaments, FHB, adductor hallucis, and abductor hallucis tendons.
Collateral ligaments have phalangeal and sesamoid insertions.
Split tendon of the FHB runs along the plantar aspect of the hallux and envelopes the sesamoids before inserting at the base of the proximal phalanx.
The hallux MTP joint lies in an intricate balance of opposing tendons and ligaments. The anatomy outlined previously, especially with regard to the plantar plate, is important when considering the biomechanical demands placed on the first MTP joint. During normal gait, the great toe typically supports twice the load of each of the lesser toes and accommodates forces reaching 40% to 60% of body weight. During athletic activity, including jogging and running, the peak forces may approach two to three times body weight, and the forces increase to eightfold when a running jump is performed.
The range of motion (ROM) in the normal foot has been studied extensively; it is noted to be highly variable and to decrease with aging. In the resting position, the first MTP joint is in a mean resting position of 16 degrees of dorsiflexion. The passive arc of motion was noted by Joseph to be from 3 to 43 degrees of plantarflexion and from 40 to 100 degrees of dorsiflexion. The mean passive MTP joint dorsiflexion during push-off was 84 degrees. One study found that at least 60 degrees of dorsiflexion is considered normal in barefoot walking on a level surface. Athletes may accommodate up to 50% reduction in MTP joint motion resulting from acute injury to the plantar plate or hallux rigidus by various gait adjustments such as foot/leg external rotation, shortened stride, and increased ankle, knee, or hip motion. In addition, a stiff-soled shoe is capable of decreasing MTP joint dorsiflexion to 25 to 30 degrees without significantly affecting gait.
The effects on the push-off power of the great toe following sesamoidectomy have been studied in vitro by Aper et al. They confirmed the importance of this seemingly insignificant bone to the function of the toe, particularly in the athlete, in whom even a small loss of power will affect overall performance. The study noted that the isolated excision of the tibial sesamoid equated to an 11% loss of flexor power, there was 19% loss for a fibular sesamoidectomy, and 32% when both are excised.
Great toe supports twice the weight of each lesser toe.
Hallux dorsiflexion during gait/running is 60 to 84 degrees.
Up to 50% reduction in ROM can be accommodated through gait adjustments such as foot/leg external rotation, shortened stride, and increased ankle, knee, or hip motion.
Sesamoidectomy: tibial excision results in 11% loss of flexor power, fibular 19% loss, and 32% when both are excised.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here