Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Metatarsalgia in the athlete can be a debilitating disorder that can lead to loss of function. Forefoot disorders encompass lesser toe abnormalities such as claw toes, hammertoes, mallet toes, and hard and soft corns. More proximally, problems can include intractable plantar keratosis (IPK), bunionettes, neuromas, and metatarsophalangeal (MTP) joint capsulitis and instability.
For the athlete, repetitive activities can lead to repeated stress reactions in soft tissues, bones, and joints. Abrasions and repeated trauma over bony prominences can lead to callus formation and bursitis.
Ideally, avoiding the development of problems through the use of good footwear, proper training practices, and education should be the goal. Many of these problems may develop despite prophylactic care and thus require the intervention of the orthopedic surgeon either conservatively or surgically. Often, nonsurgical treatment is successful, leading to a rapid return to athletic activity.
The complaint of forefoot pain can be frustrating for the athlete and the physician. The pain must be differentiated in order to make a correct diagnosis. The accompanying algorithm ( Fig. 20.1 ) may prove useful in determining the specific forefoot diagnosis when a patient complains of metatarsalgia. Most important is the exact location of pain. In addition, the physician should ask the following questions: Which specific activities increase symptoms? Which activities alleviate discomfort? Is the pain dorsal or plantar, medial or lateral? Is there an associated neuritis symptom with the pain? Are enlarged exostoses or prominences associated with pain, swelling, or inflammation?
When a patient complains of metatarsalgia, the initial concern on physical examination is the presence of an associated callosity. This can be seen laterally over the fifth metatarsal head with a bunionette formation. It can be localized to the plantar metatarsal region with an IPK. A callosity may develop over the dorsal distal interphalangeal (DIP) joint (a mallet toe) or the dorsal proximal interphalangeal (PIP) joint (hammertoe). On occasion a patient may complain of a callosity both overlying the PIP joint and beneath the associated metatarsal head. With a concomitant contracture of this toe, the diagnosis of a claw toe is made based on these clinical findings.
Development of a callus between two toes (a soft corn) or over the lateral aspect of the fifth toe (a hard corn) can be extremely painful.
When a patient complains of metatarsalgia, but there is no callosity present, the patient should be carefully examined for nerve-related symptoms. When such a scenario is present (along with other specific symptoms), the diagnosis of an interdigital neuroma can be made. When neuritic symptoms are not present, but symptomatic pain is still localized to the forefoot, metatarsophalangeal joint capsulitis and/or instability should be considered. The presence of a positive drawer sign (dorsal plantar instability) or malalignment of the involved toe at the metatarsophalangeal joint aids in confirming the diagnosis of second toe instability. Although this algorithm is not all-inclusive, and much more goes into the specific diagnostic process than this flow sheet allows, it does offer a method of approaching the athlete with metatarsalgia. Sometimes symptoms overlap, frequently symptoms are vague—and repeated evaluation and clinical and radiographic examination are necessary to confirm a diagnosis. The cooperation of patients in defining their symptomatic complaints, and in defining their problem through varying their athletic activity, is highly important. Likewise, patient cooperation in modifying activities when conservative management is attempted is a critical factor in any successful treatment. When surgery is performed, patient cooperation in allowing adequate healing to occur before resuming athletic activity is instrumental not only in the recovery process but also in the avoidance of other associated problems or complications.
When evaluating forefoot pain, it can often be difficult to localize the exact location of a patient’s pain in order to make a correct diagnosis. Often, the physical examination is inconclusive, especially when the patient presents to clinic when asymptomatic. This is especially common in athletes whose complaints are often activity related. To identify the location of pain, instruct the patient to repeat the offending activity, recreating the patient’s symptoms. The patient is then instructed to mark the spot with a Sharpie marker. This “spot” will stay with the patient for the next clinical examination.
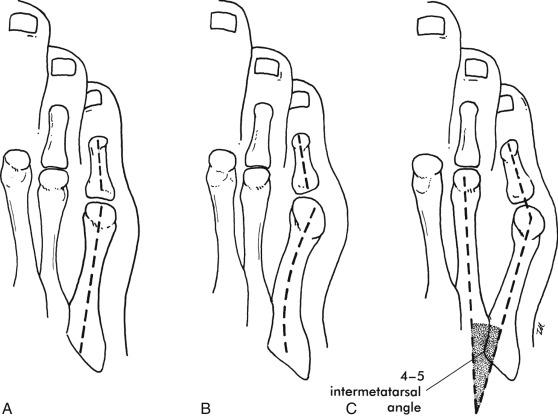
The development of inflammation, an enlarged bursa, or a callus over a prominent fifth metatarsal head may lead a physician to diagnose a bunionette ( Fig. 20.2 ). Just as bunions can present with differing magnitude and different characteristics, so too can a bunionette. A bunionette may appear radiographically as an enlarged fifth metatarsal head (type I). A flare in the metaphysis may cause bowing of the fifth metatarsal (type II), leading to symptoms, or a widened 4‒5 intermetatarsal angle (type III) characteristic of a splayfoot may lead to pain and callus formation ( Fig. 20.3 ).
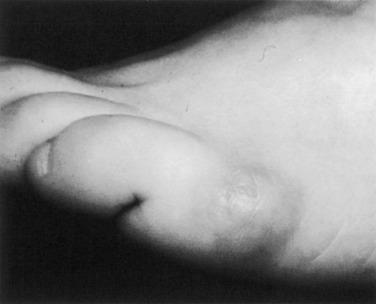
Initially an athlete may complain of pain directly lateral over the fifth metatarsal head, but the examiner should be aware of plantar symptoms as well. Neuritic symptoms involving the fifth toe may occur due to pressure over the lateral digital nerve to the fifth toe. Complaints of pain, inflammation, blistering, ulceration, or infection may be noted by the athlete.
On physical examination, significant callus formation may be observed on the lateral, plantar, or lateral-plantar position overlying the fifth metatarsal head. Any pronation of the longitudinal arch should be noted, as should any restriction in hindfoot motion.
Radiographic evaluation may demonstrate an enlarged metatarsal head, outflaring of the fifth metatarsal metaphysis, or widening of the 4‒5 intermetatarsal angle. Widening of the 4‒5 intermetatarsal angle is the most common. Abduction of the fifth toe in relation to the fifth metatarsal head may also be demonstrated.
Early treatment involves attempting to relieve pressure on the underlying bony prominence. Stretching of shoes or obtaining shoes with a soft upper that is more forgiving will relieve overlying pressure. Seams or stitching directly over the bunionette should be avoided. Moleskin applied to a blister may promote healing and protect the area while athletes continue their activities. Altering running and/or training activity may also diminish symptoms. Nonimpact activities such as stationary cycles or swimming can be integrated into the training program. A reduction in total miles per day/week may be required. Trimming the callus may significantly relieve symptoms. Physicians may teach their patients how to pare the callus appropriately. The callus is shaved in thin layers with the scalpel parallel to the toe. A pumice stone may also be used to pare down the callus. A pumice stone is safer and often more acceptable to patients for home use than using a scalpel.
When athletic activity is significantly impaired after conservative efforts, surgical intervention may be considered (see Case Study 20.1 ). The type of osteotomy selected is dependent upon the location of the callosity, as specific osteotomies of the fifth metatarsal can be used to direct the metatarsal head in different directions. Surgical intervention in treating forefoot callosities should be tailored to the patient. Extensive soft-tissue stripping, unsecured osteotomies, and multiple metatarsal osteotomies should all be avoided in athletes. Although a surgical procedure may relieve the painful callosity, athletic performance of the patient may be diminished, and thus the procedure would be considered unsuccessful. The two surgical procedures presented here fulfill the requirements of less surgical exposure, employ internal fixation, and appear better suited to athletes.
A 30-year-old skier developed pain and swelling over the plantar lateral aspect of the fifth metatarsal head. An increased callosity was observed over the plantar lateral aspect of the bunionette. A painful inflamed bursa developed during the middle of ski season that was partially relieved by grinding down the inner aspect of the ski boot overlying the bunionette. Likewise, the area overlying the fifth metatarsal head was relieved in the athlete’s everyday footwear by stretching the leather surface.
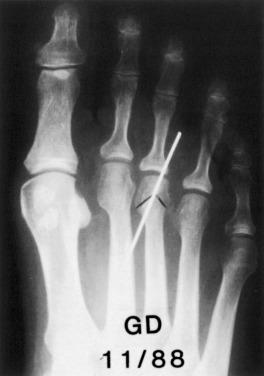
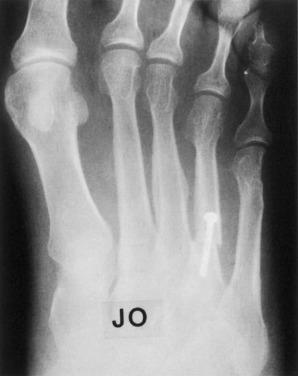
On physical examination, a normal neurologic and vascular examination was noted. Prominence of the fifth metatarsal head was characterized by a callosity both on the plantar and lateral aspects. Radiographic evaluation demonstrated an enlarged fifth metatarsal lateral condyle ( Fig. 20.4A ).
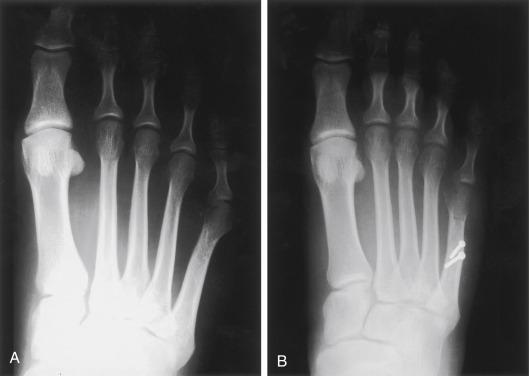
Conservative care, stretching of shoes, and padding were all recommended.
At the end of ski season, the patient requested surgical treatment due to continued symptoms. An oblique osteotomy was performed and fixed with screws. At 8 weeks following surgery, the osteotomy was healed and the patient began advancing gradually over a 2-month period. Fig. 20.4B shows the correction obtained. The patient skied the following season without symptoms.
The foot is prepped and draped in the routine sterile fashion. An Esmarch bandage is used to exsanguinate the foot. The ankle is carefully padded and the Esmarch is used as a tourniquet.
A longitudinal lateral incision is centered directly over the bunionette, extending from the midproximal phalanx to 1 cm above the metatarsal head. Care is taken to protect the neurovascular bundles.
The metatarsophalangeal joint capsule is detached on the dorsal and proximal aspect and retracted plantarly, exposing the prominent lateral condyle ( Fig. 20.5 ).
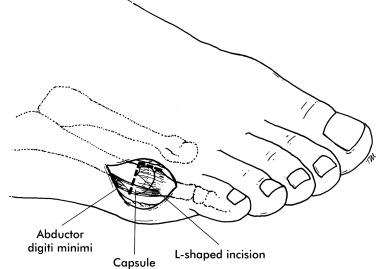
A sagittal saw is used to resect the lateral condyle in line with the diaphyseal shaft of the fifth metatarsal. (At this point, a decision must be made regarding the type of osteotomy to be performed. For a pure lateral callus, a chevron osteotomy is performed. For a combined plantar lateral callus, a distal oblique osteotomy is performed.)
Chevron osteotomy : A lateral to medial drill hole is placed in the center of the fifth metatarsal head, marking the apex of the chevron osteotomy. A 60-degree angled osteotomy based proximally is directed in a lateral to medial plane. The metatarsal head is translated medially and fixed with a percutaneous 0.045 K-wire ( Fig. 20.6 ).
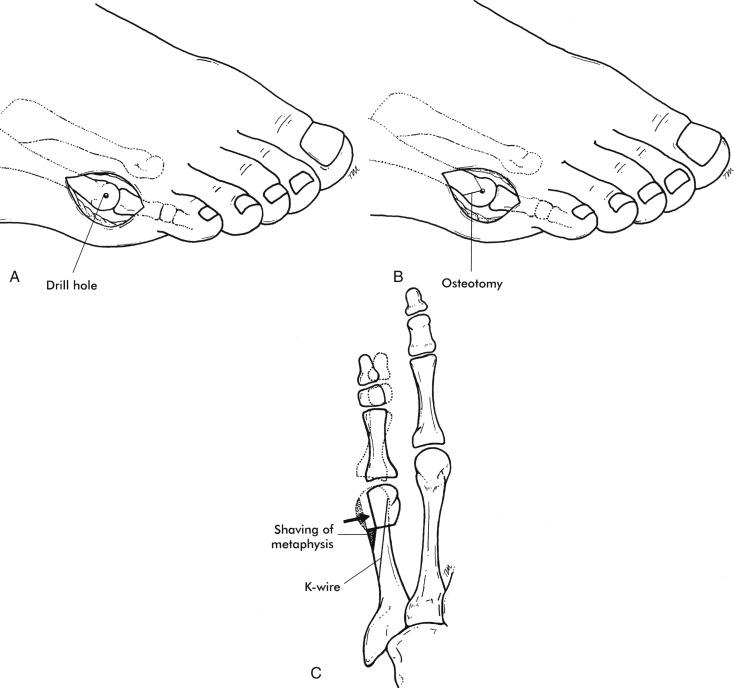
Distal oblique osteotomy : After exposing the metatarsal head and metaphysis, an oblique osteotomy is performed from a distal lateral to proximal medial direction. The metatarsal head is displaced medially and slightly proximally and is allowed to “raise up” approximately 3 mm to decrease plantar pressure beneath the fifth metatarsal head. The osteotomy is fixed with a percutaneous 0.045 K-wire ( Fig. 20.7 ).
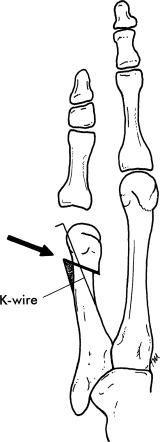
Midshaft osteotomy : After a distal lateral eminence resection is performed, in the case of an increased 4‒5 intermetatarsal angle, a diaphyseal midshaft osteotomy may be necessary to achieve correction. A subperiosteal dissection is performed at the midshaft of the fifth metatarsal with care to protect the distal capsular tissue and attachments. Care must also be taken to prevent overdissection of the metatarsal by dissecting no more than 50% of the circumference of the metatarsal shaft. This preserves as much medial-based blood supply as possible. The osteotomy may be performed, but prior to completing the oblique osteotomy, which generally runs from plantar‒proximal to dorsal‒distal, fixation is considered. Two screws are generally sufficient for fixation, and the more proximal of the two screws is drilled and placed. After completing the osteotomy, with a depth gauge placed in the hole, this drill hole acts as the center of rotation of the osteotomy and allows easier placement of the screw for definitive fixation after correction has been achieved.
Any remaining prominent metaphysis is shaved with the sagittal saw. A drill hole is placed in the dorsal proximal metaphysis, and the capsule is anchored with an interrupted suture. Remaining interrupted sutures are placed to reinforce the capsular repair ( Fig. 20.8 ).
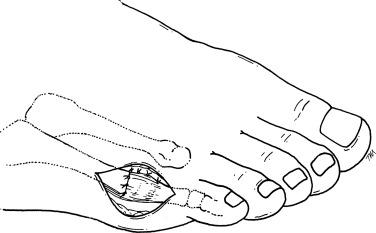
The skin is closed in a routine fashion. A gauze and tape dressing is applied and changed on a weekly basis. The patient is allowed to ambulate in a stiff postoperative shoe.
Athletic activity is increased as swelling and pain diminish. Patients are allowed to heel weight bear as soon as pain and swelling permit. Radiographic confirmation of healing should be present before aggressive activity such as jogging, running, or jumping is considered. In general, a patient can return to nonimpact activities at 2 months and progress as tolerated thereafter.
The development of a keratosis beneath one or more of the metatarsal heads is referred to as an IPK. A callus may be a localized discrete lesion or a diffuse keratotic buildup ( Fig. 20.9 ). Callus formation in athletes is not uncommon and, if asymptomatic, rarely requires medical intervention. With significant buildup, painful symptoms may occur requiring evaluation and treatment.
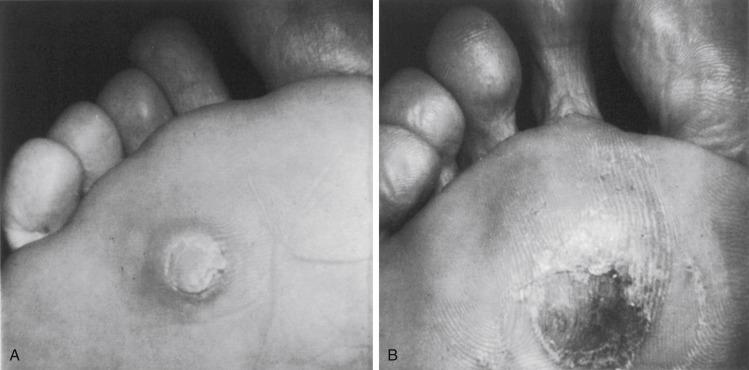
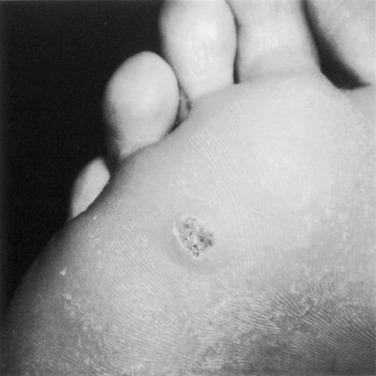
A diffuse callus may be due to repetitive abrasion associated with athletic activity. It also may be associated with a long second metatarsal or long second and third metatarsal. A discrete callus may occur beneath a single metatarsal head. It is typically associated with an enlarged plantar metatarsal condyle. It is important to distinguish this from a wart ( Fig. 20.10 ). Although warts (plantar verrucae) typically are not found beneath a metatarsal head, on occasion they can occur in this region and thus must be differentiated from an IPK. Trimming of a wart will uncover end arterioles in the lesion characterized by punctuate hemorrhages. Evaluation of the athlete with an IPK involves determining the significance of the symptoms, length of duration, and association, if any, with specific athletic activity. A patient with minimal symptoms requires no treatment.
Radiographic evaluation entails weight-bearing films with markers to determine the exact location of the IPK (a long metatarsal may be associated with an IPK; likewise, a marker may be located directly beneath the plantar condyle of a metatarsal head).
A Harris mat is invaluable in identifying abnormal pressure points on the plantar surface of a patient’s foot. The patient is instructed to walk in a normal manner, stepping on the Harris mat. The test is repeated with the contralateral foot. Abnormal pressures are illustrated as unusually dark regions and will aid in making the correct diagnosis and appropriate treatment.
Conservative treatment revolves around paring the IPK and padding it to relieve the pressure ( Fig. 20.11 ). A patient can be instructed to trim the lesion every 7 to 10 days, and this will significantly relieve discomfort. Placement of a metatarsal pad just proximal to the IPK can transfer pressure to the metatarsal diaphysis and relieve symptoms (see Case Study 20.2 ). Custom or prefabricated orthotic devices also can be a significant help in relieving symptoms. Athletes may consider altering their workout, or change sporting activities, or change duration or intensity of the workout.

A 50-year-old tennis player developed a painful callus beneath the second and third metatarsals. It was a diffusely thickened callus that began to limit his sports activities. On initial evaluation the diffuse callus was trimmed, and the patient instructed in how to care conservatively for the IPK. A pumice stone was used to pare the callus. The patient also obtained disposable scalpels to shave his thickened callosity. When he returned for further follow-up, radiographs demonstrated a long second and third metatarsal in relationship to the adjacent metatarsals. A soft pad was placed in his shoe just proximal to the callosity. Between shaving the callosity and padding it, symptoms were completely relieved, and he returned to full sports activities. Later, a soft orthotic device was fabricated to relieve pressure beneath the second and third metatarsals.
When all methods of conservative treatment have been exhausted, surgical intervention may be considered. Caution is advised in considering any metatarsal osteotomy in a high-level athlete. The possibility of delayed union, nonunion, or malunion can significantly impair athletic activity. The development of a transfer lesion beneath another metatarsal head is not uncommon. Multiple metatarsal osteotomies are to be discouraged.
The foot is prepped and draped in a routine sterile fashion. An Esmarch bandage is used to exsanguinate the foot. It is carefully padded at the ankle and used as a tourniquet.
A longitudinal incision is centered over the metatarsal head with a “hockey stick” extension distal into the adjacent interspace if needed. (The extensor tendon may be temporarily released to aid exposure and is repaired at the conclusion of the procedure.)
The MTP joint capsule is released and the toe is flexed to 90 degrees at the MTP joint.
A McGlamry elevator is used to release the plantar plate from the plantar metatarasal head in order to prevent damage during the resection.
An osteotome is used to remove 25% of the plantar condyle. Care is taken to avoid fracture to the metatarsal head ( Fig. 20.12 ). The condyle is removed.
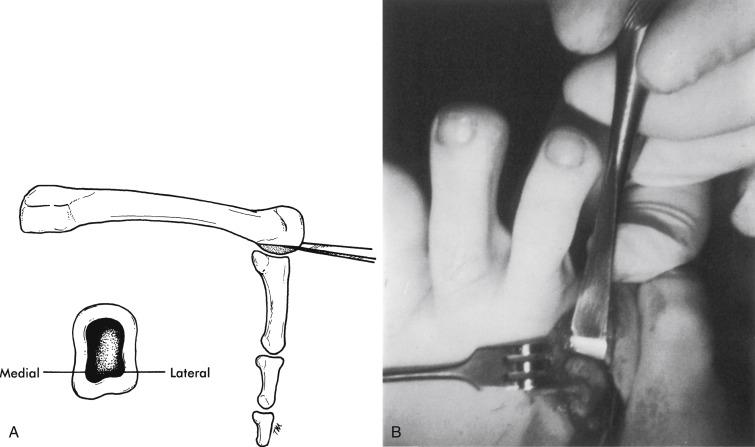
A 0.045 K-wire introduced at the MTP joint is driven distally out the tip of the toe. With the MTP joint reduced, the pin is driven in a retrograde fashion stabilizing the joint.
The extensor tendon (if released) is repaired. The skin is closed in a routine fashion.
A gauze and tape dressing is applied and changed on a weekly basis. The patient is allowed to heel weight bear in a wooden-soled shoe.
At 3 weeks the K-wire is removed.
Athletic activity is permitted as swelling and pain decrease. The toe is protected for 6 weeks following surgery with taping immobilization. In general, a patient can return to nonimpact activities at 1 month, limited impact activities such as jogging at 6 weeks, and may progress as tolerated.
The foot is prepped and draped in a routine sterile fashion. An Esmarch bandage is used to exsanguinate the foot. It is carefully padded at the ankle and used as a tourniquet.
A dorsal longitudinal incision is centered over the involved metatarsal.
If a distal oblique osteotomy is performed ( Fig. 20.13 ), the cut is directed in a vertical direction. The metatarsal head is displaced upward 3 mm and fixed with a 0.045 K-wire.
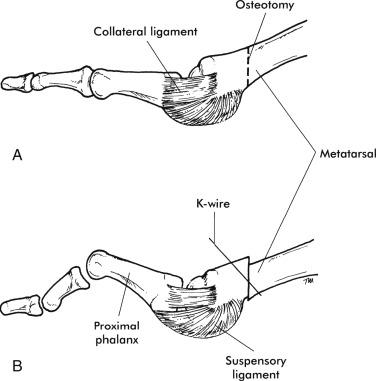
If a vertical chevron osteotomy is performed ( Fig. 20.14 ), the V-shaped osteotomy is directed in a vertical direction. (This has more coronal stability than a transverse osteotomy.) The metatarsal head is displaced upward 3 mm and fixed with a 0.045 K-wire.
If a proximal transverse osteotomy is performed ( Fig. 20.15 ), a dorsally based closing wedge osteotomy is performed. The further proximal the osteotomy is located, the more sagittal plane elevation is achieved with wedge removal. (Care must be taken not to overcorrect at the osteotomy site in order to prevent transfer metatarsalgia.) The wedge may be removed with a sagittal saw or with a small rongeur. Internal fixation is recommended. A plate-and- screw construct, screw-only construct, or K-wire is used.
The wound is closed in a routine fashion. A gauze and tape dressing is applied and changed on a weekly basis. The patient is allowed to heel weight bear in a wooden-soled shoe.
Sutures are removed 3 weeks following surgery. Percutaneous K-wires are removed 3 to 4 weeks following surgery. The forefoot is then strapped with tape and gauze until symptoms resolve.
Radiographic union is important before aggressive athletic activity can begin.
Athletic activity is permitted as swelling and pain diminish. In general, a patient can return to nonimpact activities at 2 months, limited impact activities such as jogging at 3 months, and progress as tolerated.
In general, with a partial plantar condylectomy, satisfactory results are attained for relieving the symptoms of a discrete well-localized IPK. Likewise, a distal osteotomy may be efficacious for a similar lesion. A diffuse callus in the athlete is probably best padded and shaved, as a more extensive procedure involving a diaphyseal osteotomy may require prolonged healing time and place the athlete at greater risk for delayed healing, malunion, and transfer metatarsalgia. A proximal closing wedge osteotomy may be used to elevate a symptomatic long second or third metatarsal.
An interdigital neuroma may be a source of ill-defined forefoot pain. Most commonly located in the third intermetatarsal space (IMS), a neuroma is rarely isolated to the first, second, or fourth interspace. Rarely (less than 3% of cases) do two neuromas occur in the same foot simultaneously.
Typically an athlete initially describes ill-defined forefoot pain, often exacerbated with running or sports activities, which is relieved by rest or removal of shoes.
Although ill-defined forefoot discomfort is common, the treating physician needs to help patients define the exact area of pain. With time and education, athletes may be able to pinpoint the exact area of pain from the dorsal and plantar aspect of the forefoot. Neuritic symptoms or numbness in either the second or third common digital nerve distribution may be observed. Intermetatarsal space neuromas are located in the third intermetatarsal space about 85% of the time and in the other intermetatarsal spaces less commonly. It is important to appreciate that more generalized neuritic symptoms in the toes may have other causes. Neuritis may cause irritation of all of the intermetatarsal spaces. Alternatively, tarsal tunnel syndrome or compression of Baxter’s nerve proximally at the ankle can cause generalized neuritis or, in the case of compression of Baxter’s nerve, may preferentially cause symptoms in the distribution of the lateral plantar nerve.
On physical examination, care is taken to observe for signs of peripheral neuropathy, vascular insufficiency, or neuritic symptoms at the ankle. Peripheral neuropathy is characterized by a loss of cutaneous, positional, and vibratory sensation. The Semmes-Weinstein 5.07 monofilament is the classic test for protective sensation. Vascular insufficiency is characterized by a loss of distal hair, lack of pulses, dependent rubor, varicose veins, atrophic skin, and delayed capillary refill. The toes are examined for fixed deformity. Any callus or IPK is noted, and the adjacent MTP joints are evaluated for pain or instability (see section on Metatarsophalangeal Instability). MTP capsular instability symptoms closely mimic those of an interdigital neuroma, especially in the second intermetatarsal space. This is thought to occur because the second intermetatarsal space nerve is near the plantar-lateral second MTP joint capsule, which is commonly inflamed in both second MTP instability as well as second MTP joint capsulitis. In all three diagnoses, palpation of the involved interspace usually elicits pain. Grasping and compression of the transverse arch at the level of the metatarsal heads may elicit a click (Mulder’s sign), which occurs when the neuroma subluxates below the metatarsal head and transverse metatarsal ligament (TML).
When a patient has difficulty isolating the location of pain, a 1% lidocaine injection may be used to determine the site of pain. During serial office visits 1 week apart, the physician may inject the second IMS, then the third IMS, then the second MTP joint, then the third MTP joint. Fluoroscopy and injectable contrast may be used to verify an intraarticular injection. It is important to use small volumes (1‒3mL) to prevent extravasation of anesthetic agent to adjacent structures. The patient is asked to repeat the activity that causes the most discomfort while anesthetized and keep a “pain diary” carefully describing how much of their symptoms improved and for how long. Within 1 or 2 hours the anesthetic wears off. When temporary relief is achieved with the injection, followed by recurrent symptoms, an anatomic diagnosis can be confirmed.
Early conservative treatment may alleviate symptoms in the athlete. With intermittent symptoms exacerbated by intense athletic activity, or sports of significant duration, a change in the type of activity or its duration may completely relieve symptoms.
Placing a small metatarsal pad just proximal to the symptomatic interspace may relieve symptoms. Change in athletic shoes may also alleviate pain.
When conservative methods including the modification of sports activities have not relieved symptoms, surgical intervention may be considered.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here