Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Radiation involves the direct emission or absorption of heat energy from the body (mostly infrared radiation).
Radiation is the largest source of heat loss from the body.
Clothed, sedentary individuals in a calm, temperate climate lose more body heat (approximately 60%) by radiation than active individuals (approximately 45%) in a thermoneutral environment where heat production equals heat loss.
The human body constantly radiates heat to nearby solid objects with a cooler temperature, and the rate of heat loss increases with the difference in temperature between the body and the object.
Radiant heat loss increases as temperature decreases but only becomes a significant concern in extremely cold environments.
Clothing does not markedly affect radiant heat loss.
Evaporation occurs when water or moisture is transformed into vapor.
Evaporation occurs with perspiration on the body’s surface and in respiratory passages as inspired air is warmed and moistened.
High altitude increases heat and water losses from the lungs because breathing deepens and the respiratory rate increases.
A small amount of “insensible” perspiration occurs at cold temperatures but may become significant in active individuals who are not appropriately dressed for that temperature.
Vigorous exercise with increased sweating leads to greater evaporative heat loss than with normal evaporative loss in sedentary individuals in a temperate climate (a difference of approximately 20%–30%).
Vapor barrier systems meant to decrease evaporative water loss are ineffective in physically active individuals because they trap perspiration between the barrier and the skin and lead to increased heat loss by convection when the sweat rate exceeds the rate of permeability ( Fig. 22.1 ).
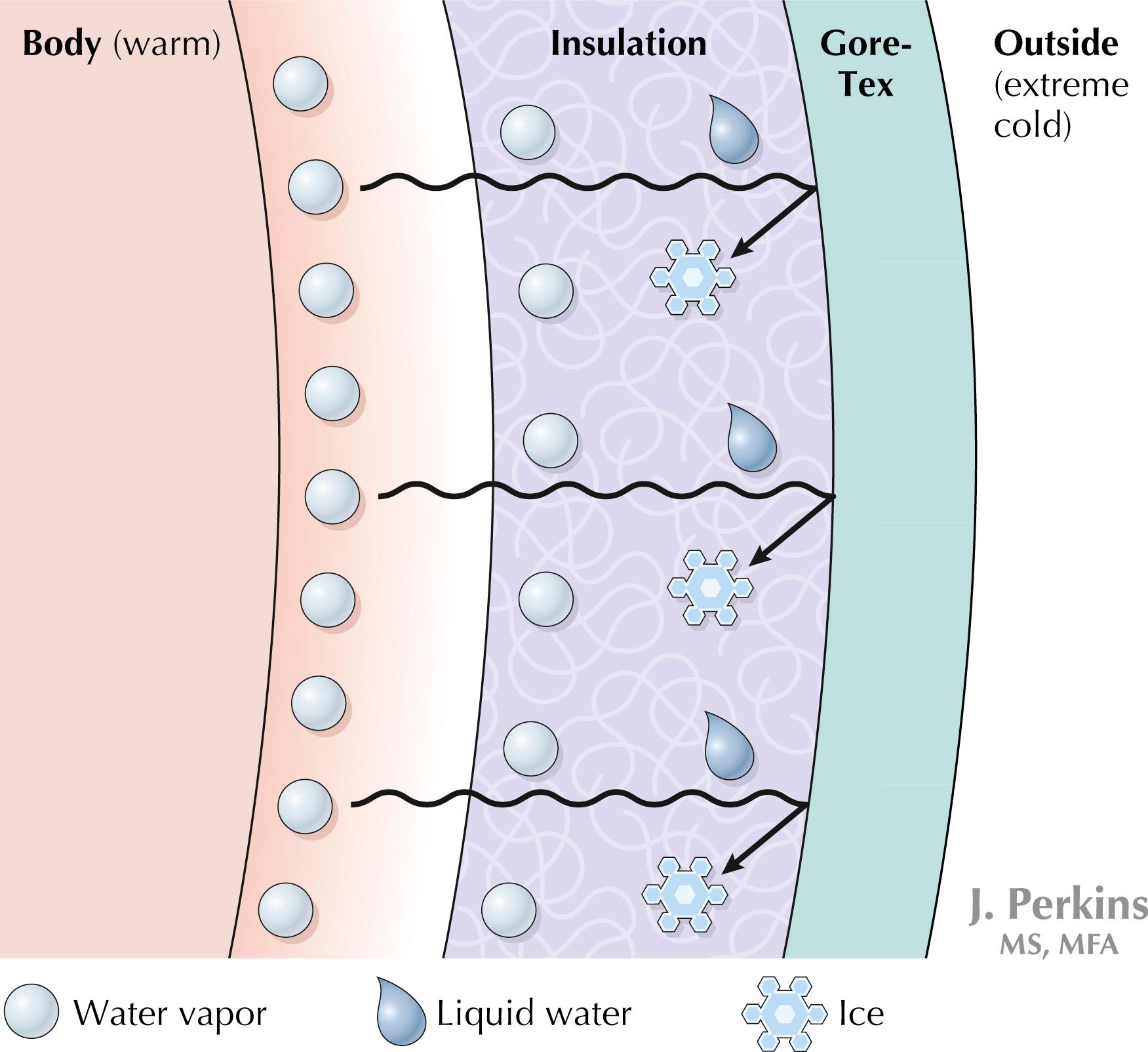
Wet clothing combined with wind leads to significant evaporative heat losses.
Convection involves the transfer of heat from the body to cold air or water in contact with the body surface.
Ongoing heat loss occurs when warmed air or water is continually displaced from the body surface and is replaced by air and water of colder temperatures.
The amount of heat loss that occurs by convection is determined by the temperature difference between the air and the body surface and by the speed of the air moving over the body.
Convective heat loss increases greatly with wind moving over the body surface, particularly with submersion in cold water.
“Wind chill” is wind combined with cold that causes a lower “equivalent” temperature ( Fig. 22.2 ) than current environmental temperature and greatly accelerates heat loss by convection; wind chill is most significant with the first 20-mph increase in wind speed, with some additional effects at higher wind speeds.
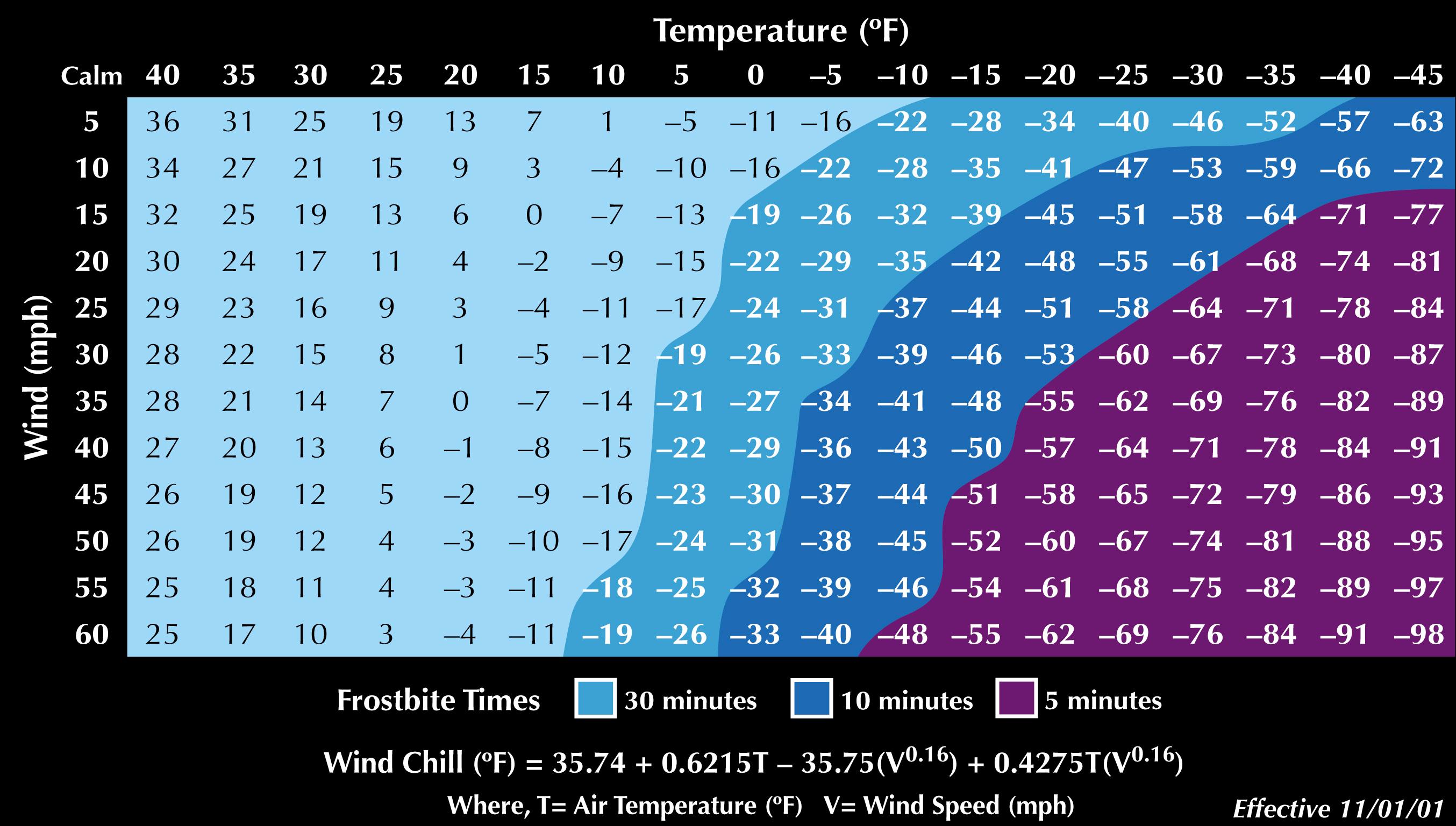
In addition to natural wind, wind moving over the body surface created by cycling, skiing, running, windsurfing, or other activities that increase air flow over the body can cause marked heat loss, particularly at cold temperatures sustained over prolonged periods.
Cold-water swimmers lose significant heat by convection because continuous motion prompts the ongoing displacement of water away from the body, resulting in constant exposure of a “warm” body to cold water.
Windproof clothing, particularly combined with appropriate insulation layers, can greatly reduce convective heat loss in most environments by trapping warm air and minimizing air displacement.
Conduction involves the direct transfer of heat from the body when it is in contact with a surface colder than the body’s temperature (e.g., fuel, water, snow, ice, or rocks).
Water is an excellent conductor, and it has an exponentially greater volumetric heat capacity than air, which can lead to significant heat losses for anyone immersed in cold water, particularly without protective clothing.
Wet clothing increases conductive heat losses.
Metabolic and biochemical reactions (slight increase)
Muscular activity
Involuntary shivering (increases heat production 2–6 times the basal levels; subsides after several hours when core temperature drops below 86°F [30°C])
Voluntary exercise (increases heat production up to 10 times the basal levels)
Nonshivering thermogenesis
Increases thyroxine, epinephrine, and norepinephrine and a subsequent slight increase in overall tissue metabolism
Relatively ineffective in preventing cold injury; may increase heat production by 10%–15% in adults
The hypothalamus is the thermoregulatory center for maintenance of body temperature and physiologic response to cold.
The body needs to stay between 95°F and 105°F (34°C and 40.5°C) to maintain normal organ function; core temperature normally ranges between 97.7°F and 99.5°F (36.5°C and 37.5°C).
The body dissipates heat relatively efficiently but is less effective at compensating for cold.
The body initially responds to cold by regulating the core (brain and other major organs) and shell (skin, muscle, and extremities).
Exposure to cold stimulates thermoreceptors in the skin that signal the hypothalamus to activate shivering and nonshivering thermogenesis, constrict peripheral or “shell” circulation, and decrease sweating in an effort to increase heat production and maintain core temperature.
The body shell acts as an interface between the body and environmental stresses—shell temperature may vary widely in contrast to core temperature.
Athletic performance may be decreased with shell cooling as cold weakens and slows muscle contractions, decreases tissue elasticity, and slows nerve conduction.
Prolonged cooling causes body core temperature to drop and results in several physiologic changes:
When core temperature falls below 95°F (35°C), rates of essential biochemical reactions decelerate.
Shivering gradually ceases at approximately 88°F–90°F (31°C–32°C) as muscles become cooler and stiffer.
Severe cold may affect all organ systems, particularly the central nervous system (CNS) and the cardiovascular system ( Table 22.1 ).
| System | Mild Hypothermia (95°F–90°F [35°C–32°C]) | Moderate Hypothermia (90°F–82.4°F [32.2°C–28°C]) | Severe Hypothermia (<82.4°F [28°C]) |
|---|---|---|---|
| Central nervous system | Confusion, slurred speech, impaired judgment, amnesia | Lethargy, hallucinations, loss of papillary reflex, EEG abnormalities | Loss of cerebrovascular regulation, decline in EEG activity, coma, loss of ocular reflex |
| Cardiovascular system | Tachycardia, increased cardiac output, and systemic vascular resistance | Progressive bradycardia (unresponsiveness), decreased cardiac output, BP, atrial and ventricular arrhythmias, J (Osborn) wave on ECG | Decline in BP and cardiac output, ventricular fibrillation (82.4°F [28°C]) and asystole (68°F [20°C]) |
| Respiratory system | Tachypnea, bronchorrhea | Hypoventilation (decreased RR and tidal volume), decreased oxygen consumption and CO 2 production, loss of cough reflex | Pulmonary edema, apnea |
| Renal | Cold diuresis | Cold diuresis | Decreased renal perfusion and GFR, oliguria |
| Hematologic | Increase in hematocrit, decreased platelet and white blood cell counts, coagulopathy, and DIC | ||
| Gastrointestinal | Ileus, pancreatitis, gastric stress ulcers, hepatic dysfunction | ||
| Metabolic/endocrine | Increased metabolic rate, hyperglycemia | Decreased metabolic rate, hyperglycemia or hypoglycemia | |
| Musculoskeletal | Increased shivering | Decreased shivering (89.6°F [32°C]) | Patient appears dead “pseudorigor mortis” |
As temperature decreases, heart rate and cardiac output reduce, and arrhythmias may occur secondary to myocardial irritability.
Cerebral blood flow decreases, leading to dilated pupils, obtundation, stupor, and eventually coma.
Respiratory rate reduces and so does oxygen consumption.
Diuresis occurs secondary to shunting of blood volume to the body core from the periphery.
Lactic acidosis develops secondary to decreased shell tissue perfusion (decreased tissue oxygenation) and subsequent anaerobic glycolysis combined with carbon dioxide retention that occurs with reduced respiratory rate.
Insulin activity reduces and hyperglycemia develops.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here