Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Infective endocarditis (IE) is believed to occur only after one first develops what is termed nonbacterial thrombotic endocarditis (NBTE). According to the American Heart Association (AHA) statement on endocarditis, it is believed that turbulent blood flow produced by certain types of congenital or acquired heart disease traumatizes the endothelium. This turbulent blood flow may be the result of flow from a high- to a low-pressure chamber or across a narrowed orifice. This trauma of the endothelium then creates a predisposition for deposition of platelets and fibrin on the surface of the endothelium, resulting in what is called NBTE. If bacteremia (or fungemia) occurs, the organisms may then colonize this site, resulting in IE.
Important risk factors for the development of IE include the following:
Age >60 years.
Poor dentition or dental infection.
Rheumatic heart disease (in underdeveloped countries).
Prosthetic valves.
Many congenital heart diseases.
Previous history of endocarditis.
Intracardiac devices.
Intravenous drug abuse.
Immunocompromised state.
Diabetes mellitus.
Chronic hemodialysis.
IE has an annual incidence of 3 to 7 per 100,000 person-years in the most recent surveys. Although the overall IE incidence has remained stable, the incidence of IE caused by Staphylococcus aureus has increased and it is the most common causative organism in most countries.
Factors that should raise the suspicion for endocarditis include:
Bacteremia/sepsis of unknown cause.
Fever.
Constitutional symptoms, such as unexplained malaise, weakness, arthralgias, and weight loss.
Hematuria, glomerulonephritis, and suspected renal infarction.
Embolic event of unknown origin (to the brain, lungs, spleen, kidney).
New heart murmur (primarily regurgitant murmurs).
Unexplained new atrioventricular (AV) nodal conduction abnormality (prolonged PR interval, heart block).
Multifocal or rapid changing pulmonic infiltrates.
Peripheral abscesses.
Cutaneous lesions (Osler’s nodes, Janeway’s lesions).
Ophthalmic manifestations (Roth’s spots).
Osler’s nodes are small, tender red-purple nodules. They most commonly occur in the fingers, hands, toes, and feet. They may be caused by circulating immunocomplexes.
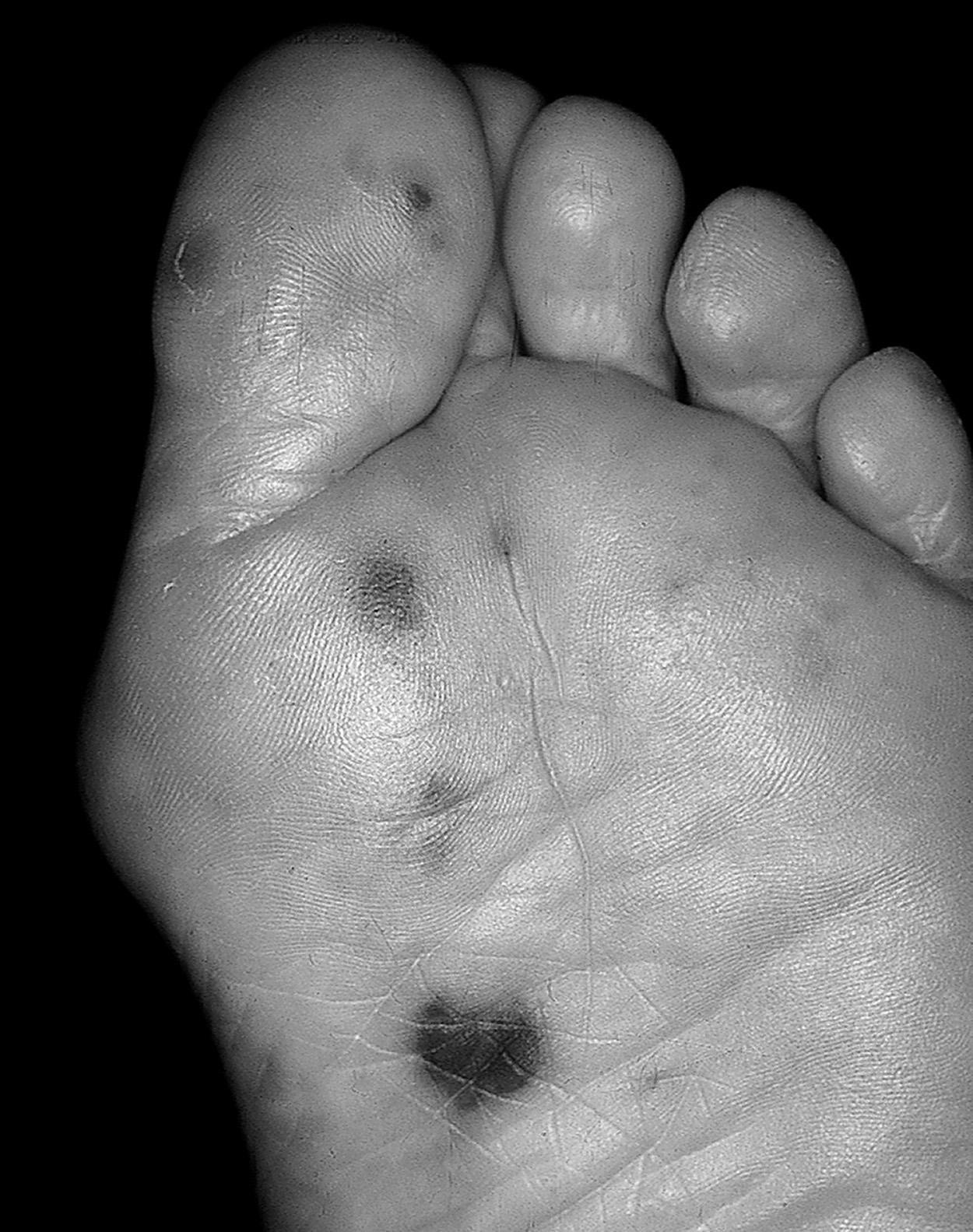
Janeway’s lesions are irregular macules located on the hands and feet. As opposed to Osler nodes, they are painless ( Fig. 34.1 ).
The Duke criteria is a set of criteria proposed for the definite and possible diagnosis of IE, published in 1994 (see Bibliography), based on both pathologic and clinical criteria. These criteria were a modification of previously proposed criteria (the Von Reyn criteria ). These criteria were then slightly modified in 2000, with the criteria incorporating the value of transesophageal echo, special recognition of Coxiella burnetii , and several other issues (see Bibliography). These revisions became known as the “modified Duke criteria” and are presented in Tables 34.1 and 34.2 .
| Definite Infective Endocarditis |
|
| Possible Infective Endocarditis (see Table 34.2 ) |
|
| Rejected |
|
| Major Criteria |
|
| Minor Criteria |
|
A classic history and Oslerian manifestations of endocarditis (bacteremia, active valvulitis, peripheral emboli, and immunologic phenomena) are present in a minority of patients. In most patients, these “textbook” findings may be absent. Hence, a high index of suspicion and low threshold for investigation are essential in these high-risk groups. Patients in particular who can present with endocarditis in an atypical manner include:
Those with right-sided endocarditis.
Elderly and immunocompromised patients.
Patients with pacemakers, implantable cardioverter defibrillators (ICDs), or central venous catheters.
Intravenous drug users, especially if with concomitant immunosuppression.
This should be done as soon as possible. Ideally less than 12 hours after initial evaluation. Echocardiographic evidence of an oscillating intracardiac mass or vegetation, an annular abscess, prosthetic valve dehiscence, and new valvular regurgitation are major criteria in the diagnosis of IE. Transthoracic echocardiography (TTE) has a sensitivity of 60% to 75% in the detection of native valve endocarditis. It can detect 70% of vegetations larger than 6 mm but only 25% of vegetations less than 5 mm. In cases where the clinical suspicion of endocarditis is low, a good-quality TTE is usually adequate. In cases where the suspicion of endocarditis is higher, a negative or nondiagnostic TTE should be followed by transesophageal echocardiography (TEE), which has a sensitivity of 88% to 100% and a specificity of 91% to 100% for native valves. Sometimes TEE may be unrevealing when performed early in a patient’s illness. Thus if a high clinical suspicion persists, a repeat TEE is recommended in 3 to 5 days or sooner depending on clinical findings. TTE is not considered a sensitive test when a prosthetic valve or intracardiac device is present, and a TEE is recommended in such cases. Figs. 34.2 and 34.3 demonstrate a mitral valve vegetation visualized by TEE.
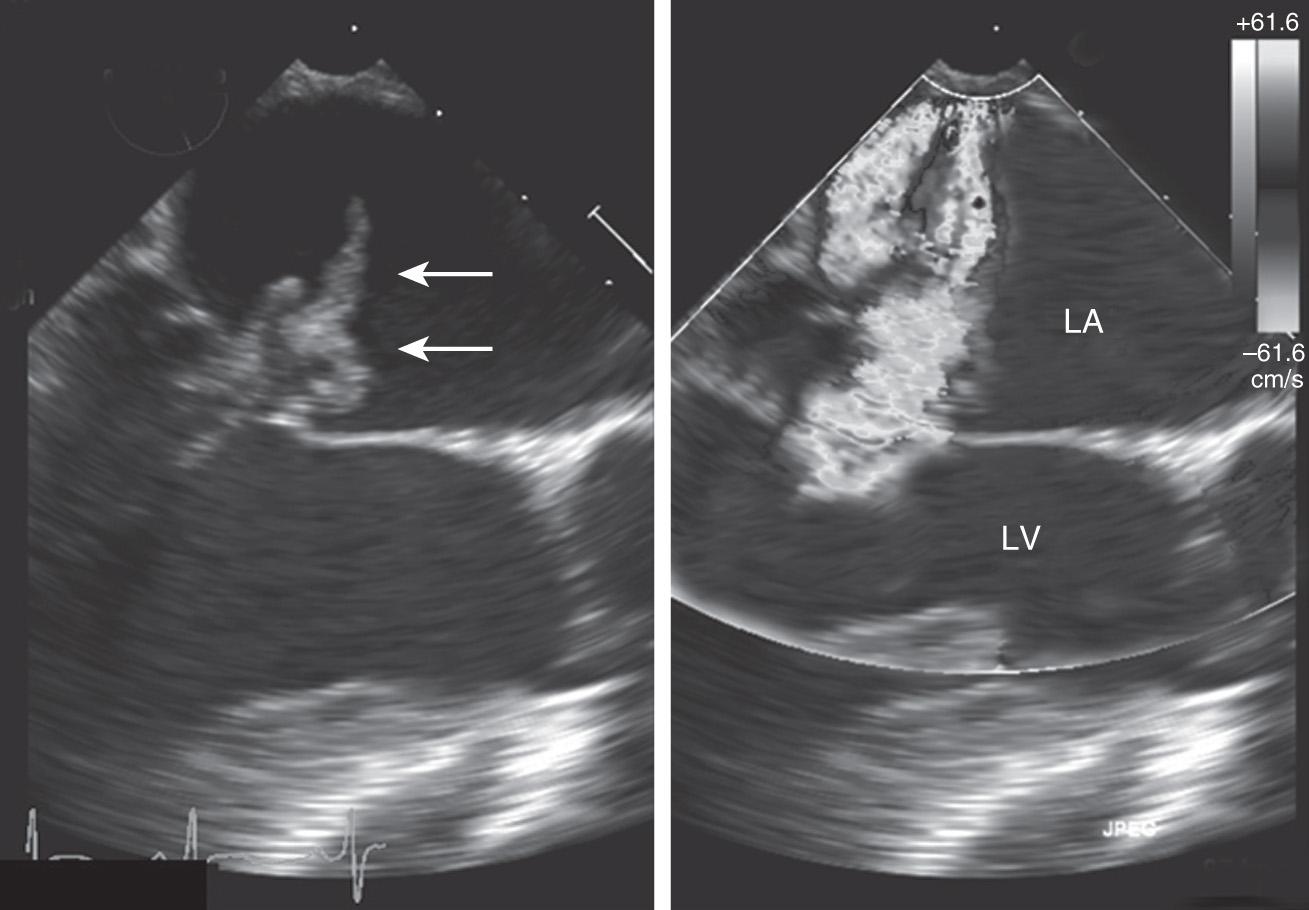
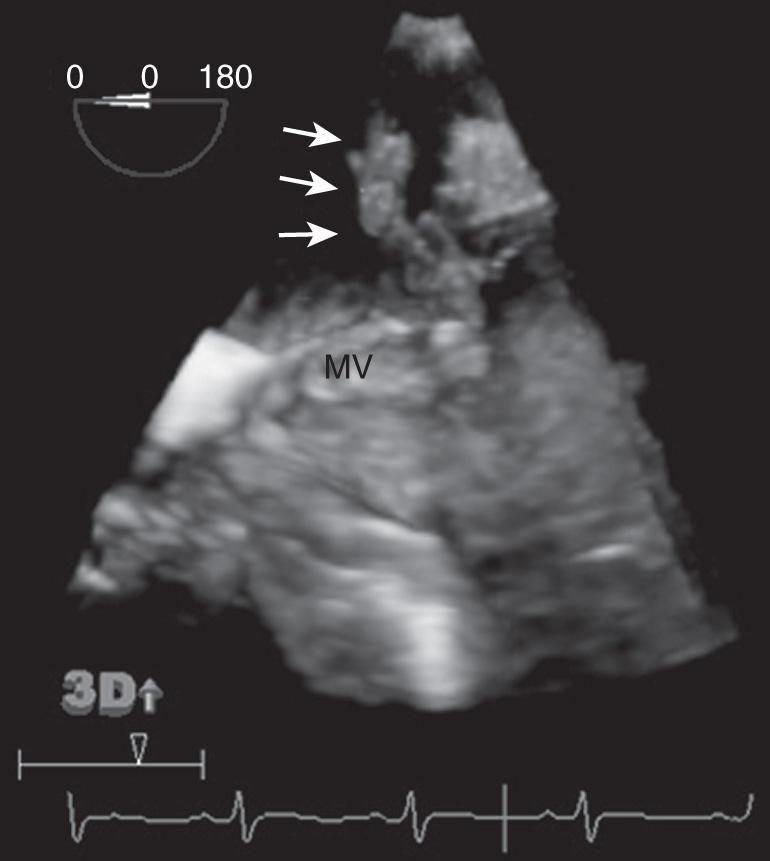
Repeat TTE is indicated with acute changes in the patient’s signs and symptoms. Examples include development of a new murmur, embolic phenomena, or AV conduction blocks. Persistence of fever despite adequate antibiotic therapy is also an indication for repeat imaging. Repeat echocardiography can also be considered during follow-up of uncomplicated IE at the time of antimicrobial therapy completion to establish baseline features such as vegetation size and severity of valvular dysfunction.
Multislice computed tomography scan (MSCT) can be used to detect abscesses/pseudoaneurysms when the diagnosis is not secured by TEE and may be superior to echo in providing information on the extent of the perivalvular extension. It is also helpful to diagnose embolic complications to the spleen, kidney, and brain. Coronary CT can assess the coronary arteries in patients who are undergoing cardiac surgery complications of IE. MRI is more sensitive than CT scan to diagnose neurological complications of IE. F-18 fluorodeoxyglucose positron emission tomography ( 18 F-FDG PET)/CT significantly improves diagnostic accuracy in patients with prosthetic valve IE or cardiac device-related IE and has been used in patients with IE to identify peripheral embolization and extracardiac manifestations.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here