Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Anesthetic management of endocrine surgical patients should consider not only the organ of interest but also the end-organ consequences of the endocrine dysfunction and possible rare syndromes.
Severe symptomatic hypercalcemia (especially > 14 mg/dL) constitutes a medical emergency, often mandating treatment before completing the diagnosis.
If rapid parathyroid hormone assay is contemplated intraoperatively (to determine effectiveness of resection), propofol use is discouraged and should be stopped at least 5 minutes before the assay is drawn.
Before thyroid surgery the anesthesiologist must know the gland's functional status; hyperthyroidism and hypothyroidism have significant preoperative implications. Imaging studies delineate anatomy, determine if other structures are involved, and help plan surgical management.
The major considerations regarding anesthesia for patients with thyroid disorders are (1) attainment of a euthyroid state preoperatively, (2) preoperative preparation and attention to disease characteristics, and (3) normalization of cardiovascular function and temperature perioperatively.
Thyroid storm is a medical emergency with significant mortality. Therapy includes blocking the synthesis of thyroid hormones with antithyroid drugs.
Myxedema coma is a rare complication associated with profound hypothyroidism and occasionally accompanied by pericardial effusion and congestive heart failure.
Pituitary adenomas are three to five times more common than previously reported (5%-20% of primary CNS tumors). Pituitary surgery treats the hyperfunctioning gland, cancer, or mass effect.
Pituitary surgical complications include temperature dysregulation and abnormalities of endocrine function, requiring immediate treatment of steroid deficiency, hypoglycemia, and excessive or deficient secretion of vasopressin.
Abnormalities of vasopressin (ADH) function that affect perioperative management involve a relative or absolute lack or an excess of vasopressin.
Special preoperative considerations for patients with Cushing's syndrome include regulating diabetes and hypertension, ensuring normal intravascular fluid volume and electrolyte concentrations, and careful patient positioning.
Withdrawal of steroids or suppression of their adrenal synthesis by steroid therapy is the leading cause of underproduction of corticosteroids. If not stressed, glucocorticoid-deficient patients usually have no perioperative problems.
Pheochromocytoma and paragangliomas are catecholamine- producing nervous system tumors. Preoperative α-blockade alleviates symptoms, with β-blockade and phenoxybenzamine for patients with persistent dysrhythmias or tachycardia.
Signs and symptoms in patients with insulinomas usually are directly related to prolonged hypoglycemic states.
Surgical mortality rates for diabetic patients average five times higher than for nondiabetic patients. Acute diabetic complications include hypoglycemia, diabetic ketoacidosis, and hyperglycemic hyperosmolar nonketotic coma.
For management of hyperglycemia in the ICU, recommended threshold to initiate insulin infusion is 180 mg/dL, then 140 to 180 mg/dL as the target range. Glucose control by insulin infusion is recommended preoperatively and for critically ill patients.
The endocrine system directly or indirectly influences many critical functions of the body, especially energy homeostasis, metabolism, and the cardiovascular system. Electrolyte and fluid balance and immune system function are intricately controlled by hormones. Disorders involving the endocrine system can present as primary disorders of the endocrine organ (common) or can be part of a syndrome (rare). The management of a patient who presents for surgery on endocrine organs should not only focus on the organ of interest, but also consider the end-organ consequences of the endocrine dysfunction and its possible relationship to rare syndromes. Perioperative outcome in many of these patients also involves the anesthesiologist's understanding of the surgery and the potentially dramatic pathophysiologic effects of removing the endocrine organ.
Parathyroid glands are intricately involved in calcium and phosphate metabolism. Disorders of serum calcium concentration are relatively common and often serve as a harbinger of underlying parathyroid disease. However, many diseases can cause hypercalcemia or hypocalcemia. Most surgeries on the parathyroid gland are performed for primary hyperparathyroidism. However, surgery may also be needed for secondary hyperparathyroidism, inherited parathyroid diseases, or familial hyperparathyroidism syndromes. Patients with primary carcinoma of the parathyroid gland, multiple endocrine neoplasia type I (MEN-I, parathyroid hyperplasia with lesions of pancreas and pituitary), and MEN-IIA (medullary thyroid cancer, pheochromocytoma, and primary hyperparathyroidism) may also present for parathyroid surgery. Other parathyroid syndromes that may require surgery include hereditary hyperparathyroidism–jaw tumor, familial isolated hyperparathyroidism, neonatal severe hyperparathyroidism, and familial hypocalciuric hypercalcemia ( Table 13-1 ). To appreciate perioperative considerations for patients undergoing parathyroid surgery, it is important to know about calcium metabolism.
| Syndrome | Clinical Features |
|---|---|
| Multiple endocrine neoplasia type I (MEN-I) | Primary hyperparathyroidism Enteropancreatic tumors Pituitary tumors Thymic or bronchial endocrine tumors Adrenocortical tumors |
| MEN-IIA | Medullary thyroid carcinoma Pheochromocytoma Parathyroid hyperplasia |
| Hereditary hyperparathyroidism–jaw tumor syndrome | Primary hyperparathyroidism Parathyroid carcinoma Ossifying fibromas of jaw Renal cysts Renal solid tumors Uterine fibromas |
| Familial isolated hyperparathyroidism | Associated with MEN-I |
| Neonatal severe hyperparathyroidism | Occurs in childhood Extreme hypercalcemia caused by: Diffuse chief cell hyperplasia Demineralization and pathologic fractures Multiglandular parathyroid hyperplasia vs. adenoma |
| Familial hypocalciuric hypercalcemia (FHH) | Mild to moderate hypercalcemia Most common cause of hereditary hypercalcemia Histologically, parathyroid glands removed from FHH patients are normal or occasionally hyperplastic. |
The calcium ion (Ca ++ ) plays a critical role in diverse cellular functions such as cardiac contractility, hormone secretion, blood coagulation, and neuromuscular signaling. Total (bound and free) serum calcium concentration is maintained at the normal level of 9.5 to 10.5 mg/dL through a series of feedback mechanisms that involve parathyroid gland, bone, kidney, and gastrointestinal (GI) tract ( Fig. 13-1 ). Approximately 50% of the serum calcium is bound to serum proteins (albumin), 40% is ionized, and the remaining 10% is bound to such chelating agents as citrate. If the serum protein concentration decreases, the total serum calcium concentration will also decrease. The rule of thumb is that for every 1-g decrement in albumin, a 0.8-mg/dL decrement in total serum calcium concentration occurs. Likewise, if the serum proteins increase (as in myeloma), total serum calcium will increase. Acidosis tends to increase the ionized calcium, whereas alkalosis tends to decrease it. Serum calcium tends to decrease slightly with age, with a concomitant elevation of the serum parathyroid hormone (PTH, parathormone), perhaps contributing to the osteoporosis associated with the aging process.
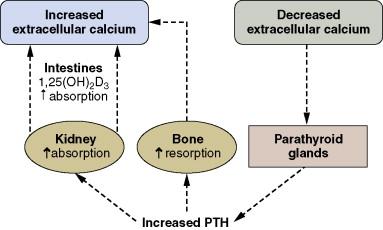
When the ionized calcium concentration decreases or the serum phosphate level rises, release of PTH is stimulated through activation of the calcium sensor receptor on parathyroid cells. PTH is secreted by the four parathyroid glands, which are usually located posterior to the upper and lower poles of the thyroid gland. PTH increases tubular reabsorption of calcium and decreases tubular reabsorption of phosphate to raise the serum calcium concentration. PTH also increases the resorption from the bone. Another effect of PTH on the kidney is the increase in active form of vitamin D, which in turn increases the absorption of calcium from the intestines. A renal phosphate leak is the result of excessive PTH secretion.
Vitamin D plays an important role in calcium homeostasis. Cholecalciferol is synthesized in the skin by the effects of ultraviolet light. Cholecalciferol is hydroxylated in the liver to form 25-hydroxycholecalciferol. The 25-hydroxy derivative is further hydroxylated in the kidney to form 1,25-dihydroxycholecalciferol (1,25[OH] 2 D 3 ). 1,25(OH) 2 D 3 stimulates absorption of both calcium and phosphorus from the GI tract. Thus, vitamin D provides the substrates for the formation of mineralized bone. 1,25(OH) 2 D 3 may also directly enhance mineralization of newly formed osteoid matrix in bone. Vitamin D derivatives also seem to work synergistically with PTH to increase resorption of bone. This is clinically important because immobilization alone increases bone resorption, and if the patient is receiving a vitamin D derivative, bone resorption may be increased further.
Hydroxylation of 25-hydroxycholecalciferol is controlled in the kidney by PTH and the phosphorus level. Elevated PTH and hypophosphatemia tend to accentuate the synthesis of 1,25(OH) 2 D 3 , whereas low levels of PTH and high levels of phosphate turn off the synthesis of 1,25(OH) 2 D 3 in the kidney. PTH maintains a normal calcium level in blood by increasing calcium reabsorption from bone and by promoting synthesis of 1,25(OH) 2 D 3 , which in turn enhances calcium reabsorption from the gut. Finally, PTH directly increases calcium reabsorption from the renal tubule. Thus, PTH accelerates the breakdown of bone by a complex mechanism that includes a fast component and a slow component (involving protein synthesis and cellular proliferation). In addition, PTH has an anabolic effect on bone formation, and in tissue culture it increases the number of active osteoblasts, the maturation of cartilage, and osteoid formation within the bone shaft.
The many causes of hypercalcemia can be grouped pathophysiologically into six broad categories ( Fig 13-2 ). Excessive PTH production is seen in (1) primary hyperparathyroidism, caused by adenoma, hyperplasia, or rarely carcinoma; (2) tertiary hyperparathyroidism, caused by long-term stimulation of PTH secretion in renal insufficiency; (3) ectopic PTH secretion (rare); (4) inactivation mutations at the calcium sensor receptor (CaSR), as seen in familial hypocalciuric hypercalcemia (FHH); and (5) alteration in CaSR function, as seen with lithium therapy.
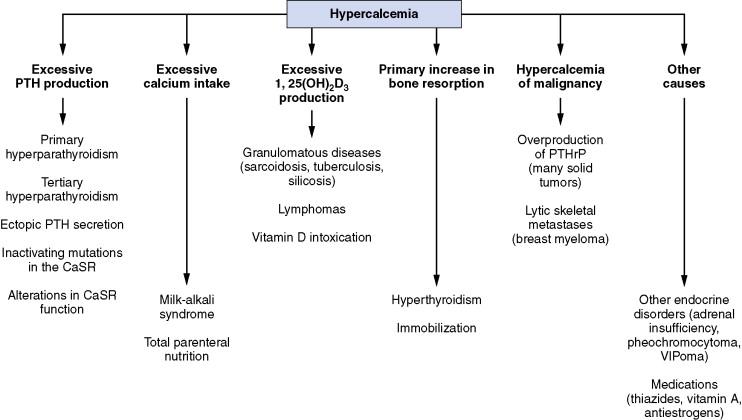
Parathyroid hyperplasia, usually involving all four parathyroid glands, may be a major cause of the hyperparathyroid syndrome. Carcinoma of the parathyroid glands is extremely rare. All adenomas might begin as hyperplasia; therefore, for the individual patient, where surgery occurs in the natural history of the disease may determine whether hyperplasia or an adenoma is found. Hypercalcemia can also be seen in solid malignancies caused by overproduction of PTH-related peptide (PTHrP) or lytic skeletal metastases, as seen in myeloma or breast cancer. Excessive 1,25(OH) 2 D 3 production can also cause hypercalcemia. This is typically observed with lymphomas, granulomatous diseases, or vitamin D intoxication. Primary increase in bone resorption, as seen with immobilization, Paget's disease, and hyperthyroidism, can also lead to hypercalcemia. Excessive calcium intake, which can occur with total parenteral nutrition (TPN) and milk-alkali syndrome, can also cause hypercalcemia. Hypercalcemia also results from other endocrine disorders (e.g., adrenal insufficiency, pheochromocytoma, VIPomas) and medications (e.g., antiestrogens, vitamin A, thiazides). Thiazides increase renal tubular reabsorption of calcium and may even enhance the PTH effects on the renal tubule. Most patients with significant hypercalcemia associated with thiazide diuretics have hyperparathyroidism.
Patients with hypercalcemia present with a variety of symptoms. The level of blood calcium is frequently related to the degree and severity of symptoms. Mild hypercalcemia (up to 11-11.5 mg/dL) is usually asymptomatic and detected on routine calcium measurement. Patients may have vague complaints of depression, poor concentration, and personality changes. Other patients may present with nephrolithiasis or peptic ulcer disease. Nephrolithiasis occurs in 60% to 70% of patients with hyperparathyroidism. Sustained hypercalcemia can result in tubular and glomerular disorders. Polyuria and polydipsia are common complaints. Patients with calcium levels above 12 to 13 mg/dL, especially developing acutely, have anorexia, nausea, vomiting, abdominal pain, constipation, polyuria, tachycardia, and dehydration.
Hypercalcemia can also result in significant echocardiographic (ECG) changes, including bradycardia, atrioventricular block, and short QT interval. Psychosis and obtundation are usually the end results of severe and prolonged hypercalcemia. Band keratopathy is a most unusual physical finding. Bone disease in hyperparathyroidism, such as subperiosteal resorption, can also be seen in radiographs of the teeth and hands in patients with prolonged hypercalcemia. Severe bone disease in hyperparathyroidism, such as osteitis fibrosa cystica, is only rarely seen and usually in older patients with long-standing disease (up to 20 years). The older patient with severe osteopenia, and perhaps vertebral compression fractures, should prompt suspicion of hyperparathyroidism.
Patients with hyperparathyroidism have elevated calcium and low serum phosphate levels. Very mild hyperchloremic acidosis may be present. The PTH level is usually elevated, particularly with respect to the level of calcium concentration, and PTH reduction is the hallmark of successful surgery. The only two situations in which hypercalcemia would be associated with a high PTH level are hyperparathyroidism and the ectopic PTH syndrome (usually secondary to a tumor of the lung or kidney that produces a biologically active fragment of PTH). All other causes of hypercalcemia are associated with either “normal” or, more appropriately, low levels of PTH. When a patient presents with an extremely high blood calcium level (> 14 mg/dL), the patient likely has a distant cancer rather than hyperparathyroidism. Overall, about 50% of all cases of hypercalcemia are caused by cancer invading bone. In these patients, prognosis is poor; more than 50% die within 6 months. Treating hypercalcemia does not prolong survival but usually improves quality of life.
Evaluation for bony metastases includes a technetium diphosphonate bone scan, which is positive in a large percentage of cancers that have metastasized. In addition to serum calcium and phosphate, the bony fraction of alkaline phosphatase, creatinine, electrolyte, and urinary calcium levels are obtained, as well as the appropriate skeletal radiographs and isotope bone scan (by endocrinologist) to aid diagnosis.
Severe symptomatic hypercalcemia, especially levels greater than 14 mg/dL, constitutes a medical emergency, and often treatment must be begun before the diagnosis is complete. The signs and symptoms in any one patient cannot be related to serum calcium level. One patient with total calcium of 14 mg/dL may be almost asymptomatic, whereas another may have severe polyuria, tachycardia, dehydration, and even psychosis. Age seems to be a factor; that is, for any given calcium level, the older patient is more likely to be symptomatic than younger patients.
The first step in the management of hypercalcemia is hydration. Infusion of 4 to 6 L of intravenous (IV) saline may be required in the first 24 hours. Loop diuretics may be required to enhance sodium and calcium excretion. Complications of these interventions include hypomagnesemia and hypokalemia. Extreme care must be exercised in the use of digitalis derivatives for patients with hypercalcemia. Digitalis intoxication occurs quite readily in the presence of hypercalcemia, and dysrhythmias from digitalis toxicity are common ( Box 13-1 ).
Provide hydration: 4-6 L of IV saline in first 24 hours.
Administer loop diuretics to enhance sodium excretion.
Inhibit bone resorption by bisphosphonates (zoledronic acid, pamidronate, etidronate).
Rarely, plicamycin may be indicated.
Correct hypokalemia and hypomagnesemia that may develop with treatment of hypercalcemia.
Correct hypovolemia.
Correct electrolyte disorders.
Note risk of aspiration if patient has altered mental status.
Take special care in positioning (risk of pathologic fractures).
Avoid or discontinue propofol if rapid PTH assay is going to be conducted intraoperatively.
Postoperatively, note risk of recurrent laryngeal nerve injury, glottic edema, hypocalcemia, hypophosphatemia and hypomagnesemia.
IV, Intravenous; PTH, parathormone.
If there is increased calcium mobilization from bone, as in malignancy or severe hyperparathyroidism, drugs that inhibit bone resorption should be considered. Zoledronic acid (e.g., 4 mg intravenously [IV] over 30 minutes), pamidronate (e.g., 60–90 mg IV over 2-4 hours), and etidronate (e.g., 7.5 mg/kg/day for 3-7 consecutive days) can be used in the treatment of hypercalcemia of malignancy in adults. Onset of action is within 1 to 3 days, with normalization of serum calcium levels occurring in 60% to 90% of patients. Because of their effectiveness, bisphosphonates have replaced calcitonin and plicamycin, which are rarely used in current practice for the management of hypercalcemia. In rare cases, dialysis may be necessary. Finally, although IV phosphate chelates calcium and decreases serum calcium levels, this therapy can be toxic because calcium-phosphate complexes may deposit in tissues and cause extensive organ damage.
In patients with 1,25(OH) 2 D 3 -mediated hypercalcemia, glucocorticoids are the preferred therapy because they decrease 1,25(OH) 2 D 3 production. IV hydrocortisone (100-300 mg daily) or oral prednisone (40-60 mg daily) for 3 to 7 days are used most often. Other drugs, such as ketoconazole, chloroquine, and hydroxychloroquine, may also decrease 1,25(OH) 2 D 3 production and are used occasionally.
Patients with moderate hypercalcemia who have normal renal and cardiovascular function present no special preoperative problems. ECG findings can be examined preoperatively and intraoperatively for shortened PR or QT interval. Because severe hypercalcemia can result in hypovolemia, normal intravascular volume and electrolyte status should be restored before anesthesia for elective surgery. Aspiration precautions must be taken because the hypercalcemic patient with altered mental status may have a full stomach or may be unable to protect the airway. Radiographs of the cervical spine should be taken to rule out lytic lesions when hypercalcemia results from cancer. Laryngoscopy in a patient with an unstable cervical spine may result in quadriplegia.
There have been significant advances in parathyroid surgery. With newer imaging and radionuclide techniques and rapid intraoperative PTH assay, it is no longer necessary to remove all four parathyroid glands. Unilateral removal of the glands is now possible with less invasive techniques. Surgery can be performed under general, regional, or local anesthesia based on institutional approach. Although no controlled study has demonstrated clinical advantages of one anesthetic over another, if rapid intraoperative PTH assessment is contemplated (to determine the effectiveness of resection), propofol use is discouraged. If propofol is used, it should be stopped at least 5 minutes before the assay is drawn.
Maintenance of anesthesia usually presents little difficulty. No special intraoperative monitoring for hyperparathyroid patients is required. Because of the proximity of surgical retraction to the face, however, meticulous care is taken to protect the eyes. The possibility of lytic or pathologic fractures warrants careful positioning. Response to neuromuscular blocking agents may be unpredictable when calcium levels are elevated; reversal of the effects may be difficult. Failure to remove all the parathyroid adenomas may necessitate single or multiple reoperations. Sestamibi scanning and venous sampling of PTH levels in thyroidal venous beds may provide useful information to the surgeon at reoperation. Unusual sites of parathyroid adenoma include areas behind the esophagus, in the mediastinum, and within the thyroid.
Of the many possible postoperative complications (nerve injuries, bleeding, metabolic abnormalities), bilateral recurrent nerve trauma and hypocalcemic tetany are most serious. Bilateral recurrent laryngeal nerve injury (from trauma or edema) causes stridor and laryngeal obstruction as a result of unopposed adduction of the vocal cords and closure of the glottic aperture. Immediate endotracheal intubation is required in these patients, usually followed by tracheostomy to ensure an adequate airway. This rare complication of bilateral recurrent nerve injury occurred only once in more than 30,000 operations at the Lahey Clinic (Tufts University School of Medicine, Burlington, Mass). Unilateral recurrent laryngeal nerve injury often goes unnoticed because of compensatory overadduction of the uninvolved cord. Because bilateral injury is rare and clinically obvious, laryngoscopy after thyroid or parathyroid surgery need not be performed routinely; however, the clinician can easily test vocal cord function after surgery by asking the patient to say “e” or “moon.” Unilateral nerve injury is characterized by hoarseness, and bilateral nerve injury is characterized by aphonia. Selective injury of adductor fibers of both recurrent laryngeal nerves leaves the abductor muscles relatively unopposed, and pulmonary aspiration is a risk. Selective injury of abductor fibers, on the other hand, leaves the adductor muscles relatively unopposed, and airway obstruction can occur.
Bullous glottic edema is edema of the glottis and pharynx, which occasionally follows parathyroid surgery. This is an additional cause of postoperative respiratory compromise; it has no specific origin, and there is no known preventive measure.
Unintended hypocalcemia during surgery for parathyroid disease occurs in rare cases, usually from the lingering effect of vigorous preoperative treatment. This effect is especially important for patients with advanced osteitis because of the calcium affinity of their bones. After parathyroidectomy, magnesium or calcium ions may be redistributed internally (into “hungry bones”), thus causing hypomagnesemia, hypocalcemia, or both. Risk factors for the development of hypocalcemia (and hypocalcemic tetany) after parathydroidectomy include subtotal or 3½-gland parathyroidectomy, bilateral neck exploration, removal of the parathyroids together with thyroid glands, or history of previous neck dissection. In high-risk situations, management after parathyroid surgery should include serial determinations of serum calcium, inorganic phosphate, magnesium, and PTH levels. Serum calcium levels fall by several milligrams per deciliter in the first 24 hours. The lowest level usually is reached within 4 or 5 days. In some patients, hypocalcemia may be a postoperative problem. Causes include insufficient residual parathyroid tissue, surgical trauma or ischemia, postoperative hypomagnesemia, and delayed recovery of function of normal parathyroid gland tissue. It is particularly important to correct hypomagnesemia in patients with hypocalcemia because PTH secretion is diminished in the presence of hypomagnesemia. Potentially lethal complications of severe hypocalcemia include laryngeal spasm and hypocalcemic seizures.
In addition to monitoring total serum calcium or ionized calcium postoperatively, the clinician can test for Chvostek and Trousseau signs. Because Chvostek sign is present in 10% to 20% of individuals who do not have hypocalcemia, an attempt should be made to elicit this sign preoperatively. Chvostek sign is a contracture of the facial muscles produced by tapping the ipsilateral facial nerves at the angle of the jaw. Trousseau sign is elicited by application of a blood pressure (BP) cuff at a level slightly above the systolic pressure for a few minutes. The resulting carpopedal spasm, with contractions of the fingers and inability to open the hand, stems from the increased muscle irritability in hypocalcemic states, which is aggravated by ischemia produced by the inflated BP cuff. Because a postoperative hematoma can compromise the airway, the neck and wound dressings should be examined for evidence of bleeding before a patient is discharged from the recovery room.
Hypophosphatemia may also occur postoperatively. It is particularly important to correct this deficiency in patients with congestive heart failure (CHF). In a group of patients with severe hypophosphatemia, correction of serum phosphate concentration from 1.0 to 2.9 mg/dL led to significant improvement in left ventricular contractility at the same preload. Other complications of hypophosphatemia include hemolysis, platelet dysfunction, leukocyte dysfunction (depression of chemotaxis, phagocytosis, and bactericidal activity), paresthesias, muscular weakness, and rhabdomyolysis. In patients with both hypocalcemia and hypomagnesemia, correction of the hypomagnesemia may cause greatly increased PTH secretion, resulting in dramatic hypophosphatemia. Serum phosphate levels should be monitored closely in such patients.
Hypomagnesemia may occur postoperatively. Clinical sequelae of magnesium deficiency include cardiac dysrhythmias (principally ventricular tachydysrhythmias), hypocalcemic tetany, and neuromuscular irritability independent of hypocalcemia (tremors, twitching, asterixis, seizures). Both hypomagnesemia and hypokalemia augment the neuromuscular effects of hypocalcemia. Often, just restoring the magnesium deficit corrects the hypocalcemia. It is preferable to use oral calcium (1 or 2 g of calcium gluconate four times daily) when the patient is able to take oral fluids.
During the first week or 10 days after surgery, vitamin D derivatives are avoided to allow the suppressed parathyroid tissue (if present) to function. Vitamin D derivatives are always started if the patient has significant hypocalcemia 2 weeks after surgery. The management of hypoparathyroidism is not easy, and careful follow-up of patients is mandatory. Oral calcium and vitamin D analogs are used for long-term management.
Probably the most common cause of hypocalcemia is hypoalbuminemia, followed by surgical removal of the parathyroids. However, causes of hypocalcemia can be differentiated based on high or low PTH levels. Low PTH levels (hypoparathyroidism) are associated with (1) parathyroid agenesis (DiGeorge syndrome); (2) parathyroid gland destruction from surgery, radiation, autoimmune disease, or infiltration by metastatic or inflammatory diseases; and (3) reduced parathyroid function caused by hypomagnesemia or activating calcium sensor receptor mutations ( Fig. 13-3 ).
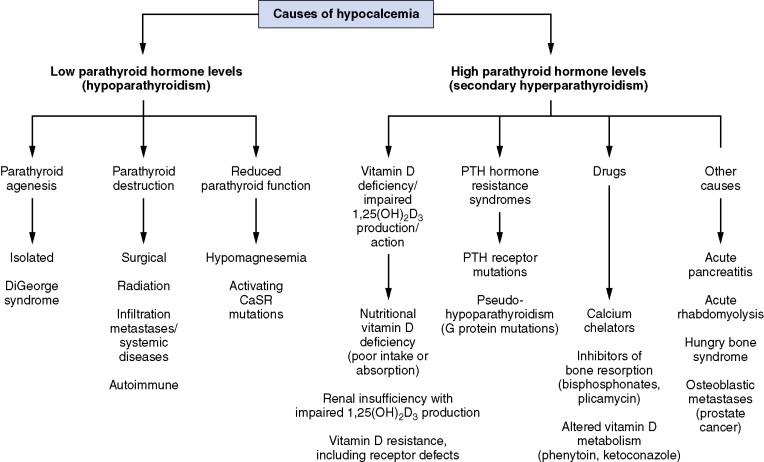
Hypocalcemia can lead to a compensatory increase in PTH levels (secondary hyperparathyroidism). The causes for hypocalcemia in patients with high PTH level include the following:
Vitamin D deficiency or impaired 1,25(OH) 2 D 3 production or action, as seen in nutritional deficiency, renal insufficiency with impaired 1,25(OH) 2 D 3 production, or resistance to vitamin D, including receptor defects.
Parathyroid hormone resistance syndromes, including PTH receptor mutations and G-protein mutations (pseudohypoparathyroidism).
Drugs such as calcium chelators, inhibitors of bone resorption, and agents that alter vitamin D metabolism (e.g., phenytoin, ketoconazole).
Acute pancreatitis, acute rhabdomyolysis, “hungry bone” syndrome after parathyroidectomy, or osteoblastic metastases with marked stimulation of the bone (prostate cancer).
In DiGeorge syndrome, thymic hypoplasia is associated with hypoparathyroidism. Pseudohypoparathyroidism is an unusual entity associated with short stature, round facies, and short metacarpals, as well as parathyroid hyperplasia. It represents in part as end-organ resistance to the action of PTH resulting from G-protein defects. 1,25(OH) 2 D 3 levels are low in pseudohypoparathyroidism, and replacement of this vitamin D derivative can partially reverse the end-organ resistance.
Hypomagnesemia impairs PTH release and thus can cause profound hypocalcemia. Hypomagnesemia is common in patients with alcoholism, malnutrition, or chronic severe malabsorption states. The calcium level may be restored by replacing magnesium. The vitamin D deficiency of the malabsorption syndrome, osteomalacia (adults) and rickets (children), is associated with a low serum phosphorus concentration. In all other causes of hypocalcemia, serum phosphorus tends to be elevated. It is disproportionately elevated in chronic renal failure. Cataracts and basal ganglion calcification are seen in both hypoparathyroidism and pseudohypoparathyroidism. Subperiosteal resorption, the hallmark of excessive PTH secretion, is seen mainly in chronic renal failure associated with secondary hyperparathyroidism and in some forms of pseudohypoparathyroidism.
Most of the clinical manifestations of hypoparathyroidism are attributable to hypocalcemia. Hypocalcemia occurs because of a fall in the equilibrium level of the blood-bone calcium relationship, in association with a reduction in renal tubular reabsorption and GI absorption of calcium. PTH inhibits renal tubular reabsorption of phosphate and bicarbonate; thus, serum phosphate and bicarbonate levels are elevated in patients with hypoparathyroidism.
The manifestations of acute hypoparathyroidism are discussed earlier in the context of the postoperative management of hypercalcemia. A nerve exposed to low calcium concentration has a reduced threshold of excitation, responds repetitively to a single stimulus, and has impaired accommodation and continuous activity. Tetany usually begins with paresthesias of the face and extremities, which increase in severity. Spasms of the muscles in the face and extremities follow. Pain in the contracting muscle may be severe. Patients often hyperventilate, and the resulting hypocapnia worsens the tetany. Spasm of laryngeal muscles can cause the vocal cords to be fixed at the midline, leading to stridor and cyanosis. Chvostek and Trousseau signs are classic signals of latent tetany, and manifestations of spasm distal to the inflated BP cuff should occur within 2 minutes (see earlier discussion).
Hypocalcemia delays ventricular repolarization, thus increasing the QTc interval (normal, 0.35-0.44). With electrical systole thus prolonged, the ventricles may fail to respond to the next electrical impulse from the sinoatrial (SA) node, causing 2:1 heart block. Prolongation of the QT interval is a moderately reliable ECG sign of hypocalcemia, not for the population as a whole but for individual patients. Thus, following the QT interval as corrected for heart rate is a useful but not always accurate means of monitoring hypocalcemia. CHF may also occur with hypocalcemia, but this is rare. Heart failure in patients with coexisting heart disease can be improved when calcium and magnesium ion levels are restored to normal, and these levels should be normal before surgery. Sudden decreases in blood levels of ionized calcium (as with chelation therapy) can result in severe hypotension.
Patients with hypocalcemia may have seizures. These may be focal, jacksonian, petit mal, or grand mal in appearance, indistinguishable from those that occur in the absence of hypocalcemia. Patients may also have a type of seizure called cerebral tetany, which consists of generalized tetany followed by tonic spasms. Therapy with standard anticonvulsants is ineffective. In long-standing hypoparathyroidism, calcifications may appear above the sella, representing deposits of calcium in and around small blood vessels of the basal ganglia, and may be associated with various extrapyramidal syndromes.
Other common clinical signs of hypocalcemia include clumsiness, depression, muscle stiffness, paresthesias, dry scaly skin, brittle nails, coarse hair, and soft tissue calcifications. Patients with long-standing hypoparathyroidism sometimes adapt to the condition well enough to be asymptomatic.
The symptoms related to tetany seem to correlate best with the level of the ionized calcium. If alkalosis is present, the total calcium level may be normal, but the ionized calcium may be low. This can result in symptoms of neuromuscular irritability (i.e., hyperventilation syndrome). With slowly developing chronic hypocalcemia, the symptoms may be very mild despite severe hypocalcemia, which may partly result from adaptive changes in the level of the ionized calcium. Even with calcium levels of 6 to 7 mg/dL, minor muscle cramps, fatigue, and mild depression may be the only symptoms. Many patients with a calcium level of 6 to 6.5 mg/dL are asymptomatic aside from some mild depression of intellectual function.
The approach to treatment of patient with hypocalcemia depends on the rate of decline and clinical presentation. For example, seizure and laryngospasm require acute treatment. Acute, symptomatic hypocalcemia is initially managed with calcium gluconate, 10 mL 10% wt/vol (90 mg or 2.2 mmol) IV, diluted in 50 mL of 5% dextrose or 0.9% sodium chloride, IV over 5 minutes. Continuing hypocalcemia often requires a constant IV infusion (typically 10 ampules of calcium gluconate or 900 mg of calcium in 1 L of 5% dextrose or 0.9% NaCl administered over 24 hours). Accompanying hypomagnesemia, if present, should be treated with appropriate magnesium supplementation ( Box 13-2 ).
Chronic hypocalcemia from hypoparathyroidism is treated with calcium supplements (1000-1500 mg/day of elemental calcium in divided doses) and either vitamin D 2 or vitamin D 3 (25,000-100,000 U daily) or calcitriol (1,25[OH] 2 D 3 , 0.25-2 μg/day). Other vitamin D metabolites (dihydrotachysterol, alfacalcidiol) are now used less frequently. Vitamin D deficiency, however, is best treated using vitamin D supplementation, with the dose depending on the severity of the deficit and the underlying cause. Thus, nutritional vitamin D deficiency generally responds to relatively low doses of vitamin D, 50,000 U two or three times per week for several months, whereas vitamin D deficiency caused by malabsorption may require much higher doses (≥ 100,000 U/day). The treatment goal is to bring serum calcium into the low-normal range and to avoid hypercalciuria, which may lead to nephrolithiasis.
Because treatment of hypoparathyroidism is not surgical, hypoparathyroid patients require surgery for an unrelated condition. Their calcium, phosphate, and magnesium levels should be measured both preoperatively and postoperatively. Patients with symptomatic hypocalcemia should be treated with IV calcium gluconate before surgery, as previously detailed. Initially, 10 to 20 mL of 10% calcium gluconate may be given at a rate of 10 mL/min. The effect on serum calcium levels is of short duration, but a continuous infusion with 10 mL of 10% calcium gluconate in 500 mL of solution over 6 hours may help to maintain adequate serum calcium levels.
The objective of therapy is to have symptoms under control before surgery and anesthesia. In patients with chronic hypoparathyroidism, the objective is to maintain the serum calcium level in at least the lower half of the normal range. A preoperative electrocardiogram (ECG) can be obtained and the QTc interval calculated. The QTc value may be used as a guide to the serum calcium level if a rapid laboratory assessment is not possible. The choice of anesthetic agents or techniques does not appear to influence outcome, with the exception of avoidance of respiratory alkalosis, because this tends to decrease ionized calcium levels further.
These patients can have congenital thymic hypoplasia and hypoparathyroidism; associated anomalies are usually vascular, such as tetralogy of Fallot, persistent truncus arteriosus, or right aortic arch. Furthermore, airway abnormality and compression of the trachea by abnormal vessels are possibilities. Thorough preoperative workup to rule out lower airway abnormalities and cardiovascular anomalies is warranted before elective surgery. These patients are also prone to sepsis caused by depressed cellular immunity, so leukocyte-depleted, irradiated blood is indicated for such patients.
Thyroidectomy is typically performed (1) to treat benign and malignant thyroid tumors or establish definitive diagnosis of a thyroid nodule; (2) to alleviate pressure symptoms or respiratory difficulties associated with a benign or malignant process (e.g., large or substernal goiters); or (3) as therapy for hyperthyroidism (thyrotoxicosis) in some patients, both those with Graves' disease and others with hot nodules. Thyroid tumors can be part of rare familial syndromes such as phosphatase and tensin homolog (PTEN) hamartoma tumor syndrome, familial adenomatous polyposis syndrome, Carney's complex, Pendred's syndrome, and Werner's syndrome ( Table 13-2 ).
| Syndrome | Clinical Features |
|---|---|
| MEN-IIB | Pheochromocytoma Mucosal neuromas Ganglioneuromatosis of intestine Marfanoid habitus |
| Carney's complex (syndrome, triad) | Mucocutaneous pigmented lesion Myxomas Multiple thyroid follicular adenomas Primary pigmented nodular adrenocortical disease Pituitary growth hormone-producing adenoma |
| PTEN hamartoma tumor syndrome | Multiple adenomatous nodules Lymphocytic thyroiditis |
| Familial adenomatous polyposis syndrome | Papillary thyroid carcinoma Adrenal adenomas Colon polyps Desmoid tumors Osteomas Hepatoblastomas Retinal pigmented epithelial hypertrophy |
| Pendred's syndrome | Thyroid goiter Bilateral sensorineural hearing loss |
| Werner's syndrome | Papillary thyroid carcinoma Follicular thyroid carcinoma Anaplastic thyroid carcinoma Premature aging Skin atrophy Bilateral cataracts |
| Cowden's disease (multiple hamartoma syndrome) | Thyroid cancer Breast cancer Hamartomas Uterine leiomyoma Megacephaly Thyroid adenoma Benign breast disease Mucocutaneous lesions Endometrial carcinoma Lhermitte-Duclos disease |
As with other endocrinopathies, two themes guide anesthesia for patients with thyroid disease. First, the organ system that most influences the anesthetic management of patients with endocrinopathy is the cardiovascular system. Second, in almost all emergency situations, and certainly in all elective situations, stabilization of any endocrine abnormality affecting the patient's preoperative state may improve outcome.
Thyroid hormone biosynthesis involves five steps : (1) iodide trapping, (2) oxidation of iodide and iodination of tyrosine residues, (3) hormone storage in the colloid of the thyroid gland as part of the large thyroglobulin molecule, (4) proteolysis and release of hormones, and (5) conversion of less active prohormone thyroxine (T 4 ) to the more potent 3,5,3- tri-iodothyronine (T 3 ). The first four steps are regulated by pituitary thyroid-stimulating hormone (TSH, thyrotropin). Proteolysis of stored hormone in the colloid is inhibited by iodide ( Fig. 13-4 ).
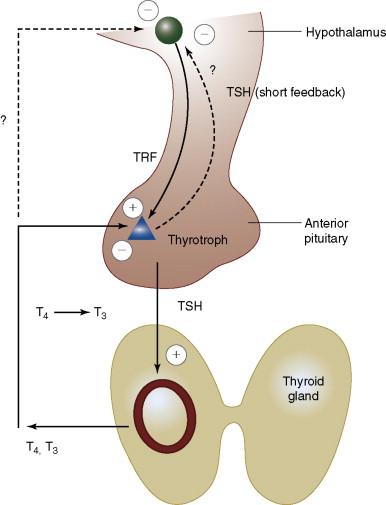
The major thyroid products are the prohormone T 4 , a product of the thyroid gland, and T 3 , a product of both the thyroid and the extrathyroidal enzymatic deiodination of T 4 . Approximately 85% of T 3 is produced outside the thyroid gland. Production of thyroid hormones is maintained by secretion of TSH by the pituitary gland, which in turn is regulated by secretion of thyrotropin-releasing hormone (TRH) in the hypothalamus. The production of thyroid hormone is initiated by absorption of iodine from the GI tract, where the iodine is reduced to an iodide and released into plasma. It is then concentrated up to 500-fold by the thyroid gland.
Once in the gland, the iodide is oxidized by a peroxidase to iodine (organification) and then bound to tyrosine, forming either monoiodotyrosine or di-iodotyrosine. Both these are then coupled enzymatically to form T 4 or T 3 . The T 3 and T 4 are bound to the protein thyroglobulin and stored as colloid in the gland. A proteolytic enzyme releases T 3 and T 4 from the thyroglobulin as the prohormones pass from the cell to the plasma. T 3 and T 4 are transported through the bloodstream on thyroxine-binding globulin (TBG) and thyroxine-binding prealbumin. The plasma normally contains 4 to 11 μg of T 4 and 0.1 to 0.2 μg of T 3 per deciliter (dL; 100 mL). Secretion of TSH and TRH appears to be regulated by T 3 in a negative feedback loop. Most of the effects of thyroid hormones are mediated by T 3 ; again, T 4 is both less potent and more protein bound, thus having lesser biologic effect, and is considered a prohormone.
In peripheral tissues there exists a ubiquitous deiodinase that converts T 4 to T 3 . Thus, T 4 appears to be a prohormone for T 3 . Monodeiodination can remove either the iodine at the 5′ position to yield T 3 or the iodine at the 5 position to yield reverse T 3 (rT 3 ), which is totally inactive biologically. In general, when T 3 levels are depressed, rT 3 levels are elevated. In several situations, rT 3 levels are increased, such as during gestation, malnutrition, chronic disease, and surgical stress. A feedback circuit exists between the pituitary gland and the circulating thyroid hormones. High levels of thyroid hormones reduce release of pituitary TSH, whereas low levels result in more TSH release (see Fig. 13-4 ).
Energy-dependent transport systems move T 3 across the target cell membrane into the cytoplasm. It then diffuses to receptors in the cell nucleus, where its binding to high-affinity nuclear receptors (TRα and TRβ) alters the production of specific messenger ribonucleic acid (mRNA) sequences, resulting in physiologic effects. Thyroid hormone has anabolic effects, promotes growth, and advances normal brain and organ development. Thyroid hormone also increases the concentration of adrenergic receptors, which may account for many of its cardiovascular effects. They also bind to specific target genes that code for structural and regulatory proteins (myosin, β-receptors, Ca ++ -activated adenosine triphosphatase, phospholamban) and for calcium, sodium, and potassium channels in the heart, which are important for systolic contractile function and diastolic relaxation.
Before undertaking surgery on the thyroid gland, it is important to know its functional status. Hyperthyroidism and hypothyroidism both have significant preoperative implications. Furthermore, imaging studies are undertaken to delineate the anatomy of the gland, determine if other structures are involved, and plan the best possible surgical management.
The current generation of the TSH assay is very sensitive and now considered the single best test of thyroid hormone action at the cellular level. Small changes in thyroid function cause significant changes in TSH secretions. Most of the T 4 is bound to the plasma protein TBG; changes in TBG can affect the total T 4 level. Estrogens, infectious hepatitis, and genetic factors can elevate TBG level and thus secondarily raise total T 4 . Androgens, nephrosis, hypoproteinemia, and genetic factors can lower TBG and thus secondarily lower total T 4 . Thus, it is more important to know the value of free T 4 and free T 3 . The normal level of TSH is 0.4 to 5.0 mU/L. A TSH level of 0.1 to 0.4 with normal levels of free T 3 and free T 4 is diagnostic of subclinical hyperthyroidism. A TSH level less than 0.03 mU/L with elevated T 3 and T 4 is diagnostic of overt hyperthyroidism. Overt hypothyroidism is diagnosed if TSH levels are more than 20 mU/L (even as high as 200-400 mU/L) with reduced levels of T 3 and T 4 . Subclinical hypothyroidism is defined by TSH levels in the range of 5 to 10 mU/L, with normal levels of free T 3 and free T 4 . Ultrasound, radioactive iodine uptake, magnetic resonance imaging (MRI), and thin-slice computed tomography (CT) thyroid scan can be useful in the diagnosis and management of thyroid masses. Functioning thyroid nodules are rarely malignant, whereas “cold” or hypofunctioning nodules have a greater probability of malignancy.
The diagnosis of pituitary or hypothalamic disease can be complicated. The procedure is often aided by the use of TRH. This tripeptide is the hypothalamic factor that brings about release of TSH from the pituitary. It may also be used to confirm the diagnosis of hyperthyroidism. Thyroid antibodies (antithyroglobulin and antimicrosomal) are useful in arriving at the diagnosis of Hashimoto's thyroiditis. Serum thyroglobulin levels tend to be elevated in patients with thyrotoxicosis. Painless thyroiditis is associated with transient hyperthyroiditis. Measurement of the α subunit of TSH has been helpful in identifying the rare patients who have a pituitary neoplasm and who usually have increased α-subunit concentrations. Some patients are clinically euthyroid in the presence of elevated levels of total T 4 in serum. Certain drugs, notably gallbladder dyes, corticosteroids, and amiodarone, block the conversion to T 3 to T 4 , thus elevating T 4 levels. Severe illness also slows the conversion of T 4 to T 3 . Levels of TSH are often high when the rate of this conversion is decreased. In hyperthyroidism, cardiac function and responses to stress are abnormal; the return of normal cardiac function parallels the return of TSH levels to normal values.
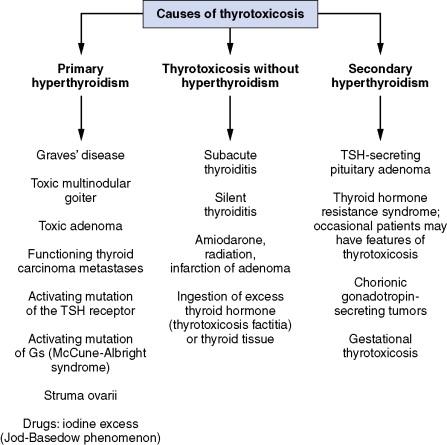
Hyperthyroidism is usually caused by multinodular diffuse enlargement of the gland, as in Graves' disease, which is also associated with disorders of the skin and eyes. Hyperthyroidism may be associated with pregnancy, thyroiditis (with or without neck pain), thyroid adenoma, choriocarcinoma, or TSH-secreting pituitary adenoma ( Fig. 13-5 ).
Major manifestations of hyperthyroidism are weight loss, diarrhea, warm moist skin, weakness of large muscle groups, menstrual abnormalities, nervousness, intolerance of heat, tachycardia, cardiac dysrhythmias, mitral valve prolapse, and heart failure. When the thyroid is functioning abnormally, the cardiovascular system is most threatened. Severe diarrhea can lead to dehydration, which can be corrected before surgery. Mild anemia, thrombocytopenia, increased serum alkaline phosphatase, hypercalcemia, muscle wasting, and bone loss frequently occur in patients with hyperthyroidism.
Muscle disease usually involves proximal muscle groups; hyperthyroidism has not been reported to cause respiratory paralysis. In the “apathetic” form of hyperthyroidism, seen most often in persons over age 60, cardiac effects dominate the clinical picture. The signs and symptoms include tachycardia, irregular heartbeat, atrial fibrillation, heart failure, and occasionally, papillary muscle dysfunction. Atrial fibrillation of unknown origin is a special concern in patients with apathetic hyperthyroidism because “thyroid storm” can occur when they have surgery for other diseases.
Although β-adrenergic receptor blockade can control heart rate, its use is fraught with hazards in a patient already experiencing CHF. However, decreasing heart rate may improve the cardiac pump function. Thus, hyperthyroid patients who have high ventricular rates, who have CHF, and who require emergency surgery are given propranolol in doses guided by changes in pulmonary artery wedge pressure and the overall clinical condition. If slowing the heart rate with a small dose of esmolol (50 μg/kg) does not aggravate heart failure, additional esmolol (50-500 μg/kg) is administered. The aim is to avoid imposing surgery on any patient whose thyroid function is clinically abnormal. Therefore, only “life or death” emergency surgery should preclude making the patient pharmacologically euthyroid, a process that can take 2 to 6 weeks.
A number of patients refuse radioactive iodine treatment and undergo surgery for hyperthyroidism. However, it is important to make these patients euthyroid before surgery. Typical treatment for hyperthyroidism includes the antithyroid drug methimazole or propylthiouracil (PTU). These drugs inhibit both thyroid hormone synthesis and the peripheral conversion of T 4 to T 3 . A usual dose takes full effect in about 6 to 8 weeks, although it may take much longer in a patient with a large thyroid gland. About 10 days before surgery, the patient typically receives a potassium iodide saturated solution (3 drops three times daily) to decrease gland vascularity and block release of stored hormone. A β-blocker, typically propranolol, is added to control adrenergic symptoms ( Box 13-3 ).
Treat with antithyroid medication (e.g., methimazole, propylthiouracil/PTU) for 6-8 weeks.
Prescribe potassium iodide, 3 drops three times daily for 10 days before surgery.
Treat sympathetic symptoms with beta-adrenergic blockers (e.g., propranolol).
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here