Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
A 42-year-old, 70-inch-tall, 95-kg man with chronic obstructive pulmonary disease and hypertension is undergoing a laparoscopic appendectomy. A satisfactory rapid-sequence induction with propofol and succinylcholine is performed, appropriate antibiotics are administered, and the abdomen is insufflated. Fifteen minutes into the procedure, the low oxygen pressure alarm sounds, the Fi o 2 displays 16%, and oxygen saturation by pulse oximetry (Sp o 2 ) reads 99% but steadily declines. Peak and plateau pressures, tidal volumes, and minute ventilation are minimally changed.
The authors wish to thank Dr. John C. Boncyk for his contribution to the previous edition of this chapter.
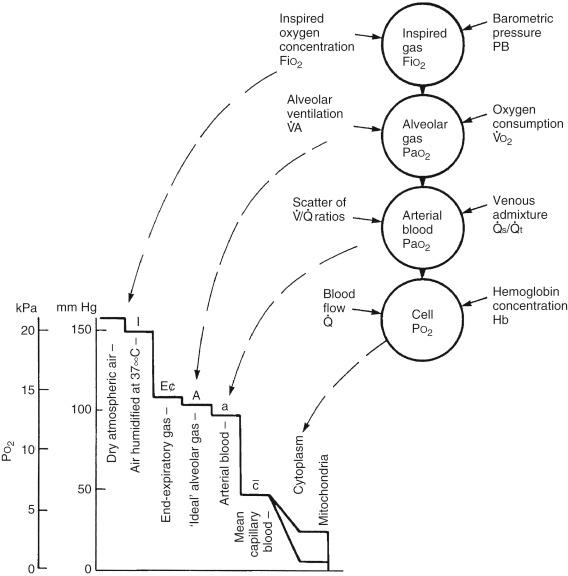
Hypoxia, or hypoxation, is abnormally low oxygen content in a tissue or organ that is unable to meet the needs of the body. The oxygen cascade depicts the declining partial pressure of oxygen from the atmosphere to the mitochondria ( Fig. 159.1 ). A disruption anywhere along the oxygen cascade results in insufficient oxygenation of end organs. Hypoxia can be subdivided into hypoxemia (hypoxic hypoxia), anemic hypoxia, circulatory hypoxia, and histiocytic hypoxia.
Hypoxemia is the failure of oxygen (O 2 ) to bind to hemoglobin or dissolve in plasma resulting in decreased blood O 2 content. Fig. 159.2 lists the causes of hypoxemia. The alveolar gas equation predicts the partial pressure of oxygen in the alveoli and is useful for calculating the A-a gradient to identify causes of hypoxemia:
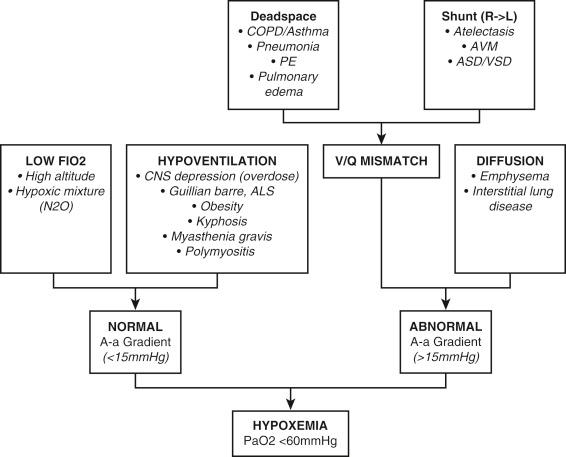
Pa o 2 and Pa co 2 are alveolar partial pressures of O 2 and CO 2 , respectively; Fi o 2 is the fraction of inspired O 2 ; PB is atmospheric (barometric) pressure; PiH 2 O is saturated H 2 O vapor pressure; and RQ is the respiratory quotient (0.8).
A normal gradient exists as oxygen diffuses down from the alveoli into the blood.
PA o 2 is the partial pressure of O 2 in the alveoli; Pa o 2 is the partial pressure of O 2 in the blood.
The A-a gradient increases with age approximately 1 mm Hg for every decade of life.
Hypoxemia can be due to a normal A-a gradient (<15 mm Hg) or high A-a gradient (>15 mm Hg) ( Table 159.1 ).
| Cause | P(A-a) o 2 | 100% O 2 | Pa co 2 |
|---|---|---|---|
| Low Fio 2 | Normal | Increased Pao 2 | Normal |
| Hypoventilation | Normal | Increased Pao 2 | Increased |
| V/Q mismatch | Increased | Increased Pao 2 | Normal |
| Shunt (V s /Q t ) | Increased | No change | Normal |
| Diffusion limitation | Increased | Increased Pa o 2 | Normal |
Normal A-a gradient (<15 mm Hg) hypoxemia is caused by the following:
Low a fraction of inspired oxygen (Fi o 2 ) such as inspiring a hypoxic mixture (Fi o 2 <21%) due to excessive nitrous oxide or nitrogen, incorrect flowmeter settings, a faulty tank or hose connection, central gas distribution error, or inspiring at a barometric pressure below 760 mm Hg.
Hypoventilation whether central (central nervous system toxicity from drug overdose) or peripheral (obesity, kyphosis, myasthenia gravis) results in an accumulation of arterial and alveolar CO 2 . In the setting of constant O 2 , consumption hypoxia results.
High A-a gradient (>15 mm Hg) hypoxemia is caused by the following:
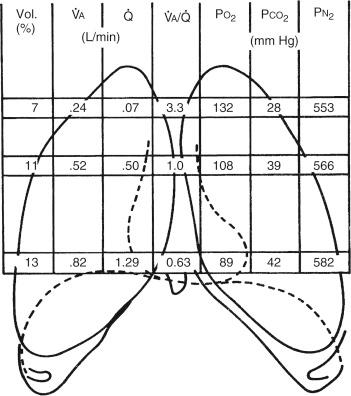
Ventilation (V)/perfusion (Q) mismatch is the most common cause ( Fig. 159.3 ). Blood flows through well perfused, poorly perfused, or entirely bypasses the alveoli. The resulting arterial oxygen content is the summed average of all of these compartments. Extremes of V/Q mismatch are known as deadspace and shunt.
Deadspace (V > Q), a product of ventilation without perfusion, is more frequently in the apex of the lungs and seen with COPD or a pulmonary embolism. In the apex, PA > Pa > Pv. Distended alveoli cause capillary collapse, wasted ventilation, and minimal to no gas exchange with blood. This is corrected with supplemental O 2 , but further widens the A-a gradient ( Fig. 159.4 ). These areas have high P o 2 and low P co 2 .
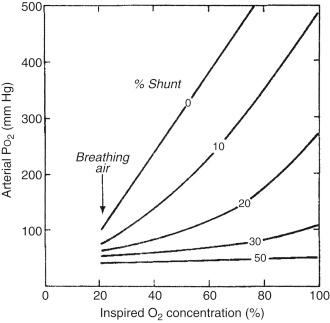
Shunt Q > V, perfusion without ventilation, occurs most frequently at the lung bases. Here Pa > Pv > PA and most commonly a result of postoperative atelectasis, pneumonia, or pulmonary edema. The venous and pulmonary capillary oxygen content is nearly equivalent (low P o 2 and O 2 content). At the bases, the mixed venous blood traverses the pulmonary capillary bed without being oxygenated, further exacerbating the V/Q mismatch. These areas have low Po 2 and high Pco 2 content. Supplemental Fio 2 will not improve oxygenation.
Diffusion problems occur if the alveolar to capillary P o 2 gradient is lost by way of a saturated or poorly functioning Hb molecule, reduction of the surface area available for gas exchange, or thickening of the diffusion barrier. These are commonly encountered during interstitial lung disease, emphysema, fibrosis, or acute respiratory distress syndrome. Alveolar-capillary gas exchange is limited by the diffusing capacity of a particular gas across the alveolar-capillary membrane (D). Diffusing capacity for O 2 ( Do 2 ) varies from 21 mL/min per mm Hg P(A-a )o 2 at rest to 65 mL/min per mm Hg P(A-a )o 2 during exercise. The Pa o 2 /Fi o 2 ratio is a common measure of oxygenation used for ventilated patients. A normal ratio is 300 to 500 mm Hg. A ratio less than 300 mm Hg indicates abnormal gas exchange; less than 200 mm Hg indicates severe hypoxemia. In a vented patient, the a-A oxygen ratio is a useful ratio for weaning. A normal a/A ratio (Pa o 2 /PA o 2 ) is greater than 0.75, and a ratio greater than 0.25 is predictive of successful weaning from the vent. In patients with central access, a mixed venous saturation (SV o 2 ) is useful to rule out anemia or low cardiac output as causes of an increased A-a gradient.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here