Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Truncus arteriosus (persistent truncus arteriosus, truncus arteriosus communis, common aorticopulmonary trunk) is a congenital cardiovascular malformation in which one great artery arising from the base of the heart by way of a single semilunar (truncal) valve gives origin to the coronary, systemic, and one or two pulmonary arteries proximal to the origin of the brachiocephalic branches. It is one of several diagnoses within the phylum of common ventriculoatrial junction (see http://www.ipccc.net/ ). A ventricular septal defect (VSD) is almost always present beneath the truncal valve.
This definition excludes those hearts in which there are no true pulmonary arteries and in which the lungs are supplied only by large aortopulmonary arteries (Collett and Edwards type IV ), characteristic of tetralogy of Fallot and pulmonary atresia with absence of the pulmonary trunk and the central and hilar portions of the right and left pulmonary arteries (see “Morphology” under Tetralogy of Fallot with Pulmonary Atresia in Section II of Chapter 38 ). Excluded also from discussion in this chapter are hearts with a common arterial trunk but an intact ventricular septum. Whether hearts in which there is a VSD but no interventricular communication during diastole (because the semilunar cusps close against the crest of the ventricular septum) should be considered to have an intact septum is controversial.
The first well-documented case of truncus arteriosus was reported by Wilson in 1798, and existence of the entity was confirmed by accurate clinical and autopsy reports of a 6-month-old infant by Buchanan in 1864. In the early literature, there was frequent confusion with a single arterial trunk and, although Vievordt clarified this aspect in 1898 (quoted by Victoria and colleagues ), confusion existed as late as 1930 when Shapiro distinguished it from hearts with aortic and pulmonary atresia. Lev and Saphir proposed the basic morphologic criteria defining the anomaly in 1942, and in 1949 Collett and Edwards reviewed previously published cases and proposed a classification. An alternative classification was suggested by the Van Praaghs in 1965.
Surgical treatment was initially confined to banding of one or both pulmonary arteries. Intracardiac repair was first successfully accomplished in 1962 at the University of Michigan using a nonvalved polytetrafluoroethylene (PTFE) conduit; the patient was alive and well 11 years later. Experimental work using ascending aortic allografts including the aortic valve was reported from Japan by Arai and colleagues in 1965 and by Rastelli and colleagues at the Mayo Clinic in 1967. Before this, in 1966, Ross and Somerville had successfully used an ascending aortic allograft in reconstructing tetralogy of Fallot with pulmonary atresia.
McGoon and colleagues were the first to successfully repair truncus arteriosus using an ascending aortic allograft and valve conduit (cylinder) in September 1967. Weldon and Cameron reported a successful repair in 1967. Binet used a xenograft valve incorporated within a polyester cylinder in 1971 (see discussion of paper by Moore and colleagues ), and Bowman and colleagues reported use of a glutaraldehyde-treated porcine aortic valve in a polyester cylinder in 1973.
The first successful conduit repair in infancy was carried out in a 6-week-old infant by Barratt-Boyes in 1971, as reported by Girinath.
Deletion of chromosome 22q11 is present in a substantial number of patients with conotruncal abnormalities. About one third of subjects with truncus arteriosus have been found to have 22q11 deletion, and many of these have additional characteristic features of DiGeorge syndrome, velocardiofacial syndrome, or conotruncal face syndrome. As such, their natural history and also their course following operation may be complicated by hypocalcemia, palatal abnormalities, learning disability, and other noncardiac problems.
Truncus arteriosus is classified based on origins of the pulmonary arteries from the truncal artery (Collett and Edwards ) and also on degree of development of the ascending aorta and ductus arteriosus in cases with a single pulmonary artery (Van Praagh and Van Praagh ).
The arterial trunk (truncal artery) is larger than a normal aorta and is the only vessel arising from the base of the heart. It originates in part from both ventricles, but usually is more over the right than left ventricle. In an autopsy series of 56 cases, the trunk was equally balanced over both ventricles in 50%. In the remainder, it was either exclusively or predominantly over the right ventricle in 40% and over the left ventricle in 10%. In the unbalanced cases, the VSD was much more likely to be smaller (both shallower and narrower). From the truncal artery arise the coronary arteries and one or both pulmonary arteries.
The pulmonary arteries usually originate just downstream from the truncal valve on the left posterolateral aspect of the truncus artery, although their origin may lie truly laterally, truly posteriorly, or (rarely) anterolaterally ( Table 43-1 ). There is frequently a single orifice leading into a short pulmonary trunk (type I of Collett and Edwards), which then divides into left and right pulmonary arteries that follow a normal course ( Figs. 43-1 and 43-2 ). Alternatively and less commonly, the orifice is double, the left and right branches arising separately side by side ( Fig. 43-3 ) or occasionally with the orifice of the left pulmonary artery superior (anterior) to the right rather than to the left of it (type II of Collett and Edwards). Types I and II merge into each other and are best considered together. They comprise the majority of cases (89% of the Toronto surgical series).
| Site | No. | % |
|---|---|---|
| Single pulmonary trunk (I) b | 140 | 69 |
| Separate left and right pulmonary artery orifices close together (II) | 41 | 20 |
| Separate orifices at lateral aspects of truncus (III) | 14 | 7 |
| Common pulmonary orifice without a common trunk | 4 | 2 |
| Other arrangement | 3 | 1.5 |
a 148 patients underwent repair.
b I, II, and III refer to approximate type of Collett and Edwards.



Rarely, ostia of left and right pulmonary arteries may be widely separated and arise from opposite lateral walls of the truncal artery at either the same or different levels above the valve (type III of Collett and Edwards). This arrangement poses special problems for repair.
Occasionally, only one pulmonary artery originates from the truncal artery. The arterial vascular supply to the opposite lung arises either from a patent ductus arteriosus as a complete branch pulmonary artery or from large aortopulmonary collateral arteries, as in tetralogy of Fallot with pulmonary atresia. When the left pulmonary artery is the one that does not originate from the truncus (or is absent), the right often continues to arise from the left posterolateral surface of the proximal truncal artery. The term hemitruncus has been used to describe the condition of the common arterial trunk giving rise to only one branch pulmonary artery, but the term is more commonly used to describe the slightly more common “origin of right (or left) pulmonary artery from the aorta.” In the latter, of course, there are two separate semilunar valves (see Chapter 45 ).
Stenosis of the origin of one or both branch pulmonary arteries is more frequent than absence of the origin; it is probably underestimated in autopsy compared with cineangiographic studies. It was noted in five clinical cases (10%) in one series.
In truncus arteriosus, there is reciprocal development between ascending and transverse aortic arches (arising from fourth aortic arch) and ductus arteriosus (arising from sixth aortic arch). Thus, in the majority of cases the ascending aorta is a direct continuation of the truncus artery and of about the same diameter (see Fig. 43-1 ), whereas the ductus arteriosus is usually entirely absent. Rarely a ductus is present with a well-developed arch.
By contrast, when the ductus arteriosus is present, the transverse arch is usually absent (interrupted aortic arch) and the ascending aorta is underdeveloped. The ductus is a direct continuation of the truncus artery, arching leftward to join the descending aorta ( Fig. 43-4 ). In this situation, left and right pulmonary artery branches usually arise separately from superior and inferior (leftward and rightward) walls of the truncal artery (type III of Collett and Edwards). The ascending aorta now arises from the superior rightward aspect of the truncus artery as the relatively smaller branch. Usually the transverse aorta is interrupted beyond the origin of the left common carotid artery (type B interrupted aortic arch; see “Types” under Morphology in Section II of Chapter 48 ), or there is severe coarctation including tubular hypoplasia of the aortic isthmus and arch (see Fig. 43-4 ). This arrangement (Van Praagh type A4) was present in 12% of the cases of Van Praagh and colleagues and 14% (28 of 303) of the Toronto surgical series.

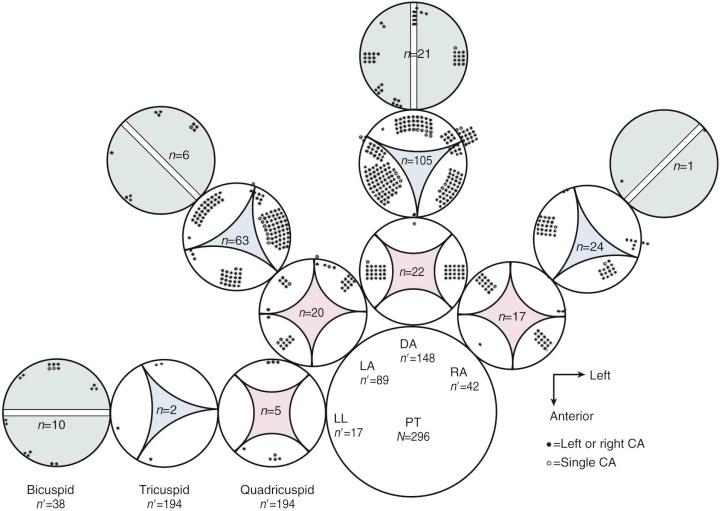
Orifices of the coronary arteries have a variable relationship to the sinuses of Valsalva above the truncal cusps ( Fig. 43-5 ). A minority (≈20%) arise centrally (more or less normally) within the sinuses; about 80% (whether the usual two or a single orifice) are at the margin of the sinus or at the upper margin of a commissure. In at least a third of cases, one coronary orifice (usually the left) is displaced cephalad above the sinutubular ridge and must be differentiated from the pulmonary artery orifices at the time of repair. In about two thirds of cases, the left coronary artery arises from the left posterior aspect of the truncal artery, and the right coronary artery from the right anterior aspect in a position similar to normal. Deviations from this pattern occur in the remainder of cases and include a single ostium (found in 18% of hearts reported by de la Cruz and colleagues ), closely approximated right and left ostia, and small, slitlike, or stenotic and kinked proximal left coronary artery.
Rarely, a coronary artery may arise from a pulmonary artery rather than the truncal artery; Daskalopoulos and colleagues report the circumflex artery's origin from the right pulmonary artery in a patient in whom pulmonary artery banding was not tolerated. The proximal part of the left anterior descending coronary artery is frequently displaced to the left of the interventricular sulcus and does not reach it until about halfway down the front of the heart. It tends to be small. Larger-than-normal diagonal branches from the right coronary artery cross the anterior right ventricle inferior to conal branches, contributing to the blood supply of the upper interventricular septum and occasionally part of the left ventricle. Damage to these vessels during surgical repair can seriously compromise the myocardium.
The single truncal valve is posterior and inferior in position, similar to the normal aortic valve, although it points more anteriorly. There is fibrous continuity between its posterior cusps and the anterior mitral leaflet, as in the normal heart ( Fig. 43-6 ). It has three cusps in half to two thirds of cases, and four cusps in most of the remainder. Rarely the valve is bicuspid. Not infrequently a raphe is present and partially divides a cusp into two, but it is doubtful whether there are ever more than four well-formed cusps. There may be variations in length and width of individual cusps, but in most patients who survive infancy, the cusps are well formed (see Figs. 43-2 and 43-6 ). However, in all cases, details of the structure of the truncal valve are different from those of the normal aortic valve.

In autopsy material, obvious severe myxomatous thickening of the cusps is present in a third of cases and is much more common in those dying as neonates ( Fig. 43-7 ). Less severe myxomatous changes are present in two thirds of older infants ( Fig. 43-8 ), and microscopic increase in thickness of the distal portions of the cusps is apparent in many more. Severe myxomatous changes often are associated with severe truncal valve regurgitation, and their frequency in autopsy specimens from neonates and young infants corresponds to the high prevalence of truncal valve regurgitation in neonates and young infants who develop severe heart failure or die. These morphologic changes are also reminiscent of those seen in congenital valvar aortic stenosis in the neonate (see “Morphology” in Section I of Chapter 47 ) and may make the valve stenotic. Rarely, stenosis is contributed to by commissural fusion. A redundant truncal valve leaflet may obstruct the pulmonary trunk ostium during ventricular ejection when the ostium is proximally placed.


The VSD is high, anterior, usually large, and juxtatruncal in position. It is typically stated that the truncal valve forms its superior margin (see Figs. 43-2 and 43-6 ). Consistent with this observation is the fact that the infundibular septum is absent in truncus arteriosus, so there is no infundibular structure to form the superior margin of the VSD, leaving the superior margin to be formed by the valve itself. Another way to characterize the VSD is to describe it as U shaped —that is, with no superior margin. This perspective can be best appreciated if one examines a specimen with the truncal valve leaflets opened to the position they occupy during systole. Inferiorly and anteriorly, the VSD is bounded by the two divisions of the septal band (trabecula septomarginalis [TSM]) and posteriorly by the free wall muscle band that separates the semilunar from the tricuspid valve (the ventriculoinfundibular fold) (see Fig. 43-2 ).
Usually the junction of the right posterior division of the TSM and ventriculoinfundibular fold forms a muscle bridge that separates the defect from the tricuspid valve and right trigone (see Fig. 43-1 ) and therefore from the bundle of His. Occasionally, this muscle bridge is absent (see Fig. 43-2 ) or poorly formed (see Fig. 43-8 ); the lower margin of the defect then approaches the tricuspid anulus, or the VSD becomes juxtatricuspid in position, in which case the His bundle is at risk of damage during repair. In these hearts, there may be fibrous truncal-tricuspid-mitral valve continuity. Part of the membranous ventricular septum may still be present at the posteroinferior margin of the VSD.
The infundibular (conal) septum is absent from the right ventricular outflow tract. Contrariwise, it has been asserted that the infundibular septum can be recognized fused to the distal anterior (free) right ventricular wall; rarely, there is a persistent blind right ventricular outflow pouch in front of it. The right ventricle is nearly always hypertrophied and enlarged.
In contrast to the right ventricular outflow tract, the left ventricular outflow tract is relatively normal in hearts with truncus arteriosus (see Fig. 43-6 ), and flow from this chamber into the truncal artery is restricted only in the unusual situation when the truncal artery originates mainly from the right ventricle and the VSD is small. A pressure gradient demonstrable on catheter withdrawal from left ventricle to aorta in such rare instances will lie at the VSD level rather than at the truncal valve. Although a moderate-sized VSD is not restrictive before surgical repair, it may prove so afterward and thus may need to be enlarged at operation (see Technique of Operation later).
The most common associated cardiac and noncardiac anomalies are shown in Tables 43-2 and 43-3 . About 10% to 20% of patients with truncus arteriosus have coexisting interrupted aortic arch or coarctation with patency of the ductus arteriosus. Truncus arteriosus is rarely associated with atrioventricular discordant connection, situs inversus, asplenia or polysplenia, or dextrocardia. Double inlet ventricle is also rare, although mitral stenosis or atresia with left ventricular hypoplasia occurs.
| Anomaly | No. of Patients | Percent |
|---|---|---|
| Cardiac | ||
| VSD | 29 | 100 |
| Truncal valve, regurgitation (mild/moderate) | 15 (9/5) | 51.7 |
| Truncal valve, stenosis (mild/moderate) | 8 (6/2) | 27.6 |
| Secundum ASD/PFO | 11 | 37.9 |
| Right aortic arch | 7 | 24.1 |
| Coronary anomalies | 4 | 13.8 |
| Persistent LSVC | 3 | 10.3 |
| IAA: | 2 | 6.9 |
| Type A | 1 | |
| Type B | 1 | |
| PDA | 2 a | 6.9 |
| Noncardiac | ||
| DiGeorge syndrome | 9 | 31 |
| Hypocalcemia | 3 | 10.3 |
| von Willebrand disease | 2 | 6.9 |
| Hypothyroidism | 1 | 3.1 |
| Esophageal atresia + tracheoesophageal fistula | 1 | 3.1 |
| Anovestibular fistula | 1 | 3.1 |
| Other | 4 | 13.8 |
| Patients | ||
|---|---|---|
| Anomaly | Number | Percentage |
| Major | ||
| Truncal stenosis/regurgitation (severe) | 7 | 12 |
| IAA | 6 | 10 |
| Non-confluent pulmonary arteries | 4 | 7 |
| TAPVR | 1 | 2 |
| Minor | ||
| Secundum ASD/PFO | 15 | 25 |
| Other (right aortic arch, coarctation, anomalous systemic-venous connection, DiGeorge syndrome | 13 | 22 |
| Other than three truncal leaflets | 15 | 25 |
| Coronary anomaly | 6 | 10 |
Frequent total absence of the ductus arteriosus has already been mentioned together with association of a widely patent ductus arteriosus in patients in whom there is also aortic arch interruption or, less often, aortic coarctation or atresia. When hearts with aortic arch interruption are excluded, right aortic arch is as common in truncus arteriosus as in tetralogy of Fallot (25%-35%). Anomalous aortic branch origins occur frequently, usually of the subclavian arteries (10%). A persistent left superior vena cava drains to the coronary sinus in about 10% of patients, and occasionally there is partial anomalous pulmonary venous connection. Patent foramen ovale is common, and atrial septal defect of moderate or large size is found in about 10% of patients. Mitral valve anomalies of various types are present with similar frequency. Other rare lesions include atrioventricular septal defect, double aortic arch, and according to Bharati and colleagues, tricuspid stenosis and (rarely) atresia.
Extracardiac congenital defects are not uncommon and may occasionally contribute to death. DiGeorge syndrome (thymic and parathyroid aplasia or hypoplasia) is known to be associated with truncus arteriosus.
Presenting symptoms are almost always tachypnea, tachycardia, irritability, and unwillingness to take either breast or bottle feedings during the early weeks of life, all manifestations of heart failure. Rarely, respiratory distress is aggravated by compression of the left upper lobe bronchus between an anteriorly placed left pulmonary artery and the posterior aortic arch. Even more rarely, an aneurysmal truncal artery associated with interrupted aortic arch may severely compress the right main bronchus and produce total right lung collapse. Mild cyanosis accompanies these symptoms in about one third of cases but rarely is the presenting feature. By contrast, in those infants who survive for longer periods, recurrent respiratory infections, dyspnea, and failure to thrive are usually present, and cyanosis is more apparent secondary to rising pulmonary vascular resistance. Older children may occasionally present with increasing cyanosis (Eisenmenger syndrome) and fail to give a history of heart failure in infancy.
On examination, signs of heart failure are accompanied by a jerky to collapsing arterial pulse produced by rapid runoff from the truncal artery into the pulmonary arteries. The heart is overactive, and a prominent left parasternal systolic murmur and often thrill are appreciated. There is frequently an ejection click coinciding with full opening of the truncal valve, and an apical gallop rhythm may be present, although it is surprisingly rare in neonates. An aortic early diastolic murmur (from truncal valve regurgitation) is highly suggestive of truncus arteriosus, particularly when it is accompanied by pulmonary plethora on chest radiograph and right aortic arch. The second heart sound is usually single but split in about one third of cases. A continuous murmur is noted occasionally and is most often due to stenosis at the origin of one or both pulmonary arteries. Important truncal valve stenosis is a confusing feature and usually results in diminished peripheral pulses accompanied by a harsh ejection systolic murmur and thrill, maximal in the right upper intercostal spaces.
Chest radiography shows marked cardiomegaly as well as plethoric lung fields in neonates and infants. The pulmonary trunk segment is deficient (as in transposition), but a high origin or arching of the left pulmonary artery may be evident in older children as a “comma” sign on the left upper mediastinal border. A solitary right pulmonary artery arising from the left side of the truncus artery may give a similar appearance. The hemithorax may be smaller and vascularity less on the side of the “absent” branch pulmonary artery (when this lung is supplied by bronchial collaterals or by a relatively small patent ductus arteriosus). In truncus arteriosus with aortic arch interruption, the descending aorta is often prominent in the chest radiograph. In those few infants who survive without treatment, pulmonary plethora subsides, as does cardiomegaly, from increasing pulmonary vascular disease.
Electrocardiography (ECG) usually shows combined ventricular hypertrophy and a normal or slightly rightward axis, although left ventricular hypertrophy is usually dominant in the tracing (occasionally it is absent). P pulmonale can occur.
Two-dimensional echocardiography can be diagnostic and is usually definitive, with infrequent occurrence of only minor errors ( Fig. 43-9 ). It demonstrates a single vessel overriding the ventricular septum and reveals abnormalities in the truncal valve cusps. In addition, origins of pulmonary arteries can be predicted with some accuracy, and presence of major associated abnormalities, particularly interrupted aortic arch, can be determined.
Cardiac catheterization and angiography may still be performed in the occasional neonate or young infant to define the pulmonary arteries, and hemodynamic state when there is an atypical physiologic presentation, such as severe cyanosis, or when there is suspicion on echocardiography that the pulmonary artery morphology is complex (e.g., unilateral aortopulmonary collaterals). Magnetic resonance imaging (MRI) and computed tomography (CT) compete with traditional angiography when structural details and some physiologic details require definition (see “ Computed Tomography Angiography and Magnetic Resonance Imaging ” later). There is an absolute indication for catheterization in patients who present after 6 months of life to define the status of the pulmonary microvasculature.
In neonates and young infants with typical physiology, there is left-to-right shunting at the ventricular level with a high pulmonary-to-systemic blood flow ratio ( ![]() ) and systemic pressures in the right ventricle and pulmonary artery. The high pulmonary blood flow keeps aortic oxygen saturation at 85% or more. Pulmonary vascular resistance is mildly raised (2-4 units · m 2 ). Atypical physiology may occur. Rarely, when the VSD is restrictive and the truncal origin is mainly from the right ventricle, left ventricular pressure may exceed that in the right. When there is truncal valve stenosis, there is a withdrawal gradient across it. The site of stenosis may be difficult to identify preoperatively. Pulmonary artery pressure is often slightly below systemic pressure, but it is importantly reduced when there is stenosis at the origin of one or the other artery.
) and systemic pressures in the right ventricle and pulmonary artery. The high pulmonary blood flow keeps aortic oxygen saturation at 85% or more. Pulmonary vascular resistance is mildly raised (2-4 units · m 2 ). Atypical physiology may occur. Rarely, when the VSD is restrictive and the truncal origin is mainly from the right ventricle, left ventricular pressure may exceed that in the right. When there is truncal valve stenosis, there is a withdrawal gradient across it. The site of stenosis may be difficult to identify preoperatively. Pulmonary artery pressure is often slightly below systemic pressure, but it is importantly reduced when there is stenosis at the origin of one or the other artery.
The progressive rise in pulmonary vascular resistance that occurs in virtually all children who survive infancy is associated with a fall in ![]() and therefore in arterial oxygen saturation. Arterial oxygen saturations less than 80% are usually an indication that pulmonary vascular resistance is beyond the operable range.
and therefore in arterial oxygen saturation. Arterial oxygen saturations less than 80% are usually an indication that pulmonary vascular resistance is beyond the operable range.
Cineangiography with contrast injections into both ventricles and ascending aorta demonstrates the exact site of origin of the pulmonary arteries and differentiates this lesion from patent ductus arteriosus. Special views are required to demonstrate the origin of right and left pulmonary artery branches to assess any proximal stenosis. Should one pulmonary artery fail to outline after routine contrast injections, the origin and distribution of the blood supply to the other lung must be identified. This is usually possible by injections into the upper descending thoracic aorta and its branches, defining either a ductus or large collaterals. In addition, a pulmonary vein wedge injection can be used to retrogradely fill true pulmonary arteries that fill either inadequately or not at all from an aortic injection.
These studies also provide information on alignment of the truncal artery and truncal valve with the two ventricles, truncal valve cusp thickening, and truncal valve stenosis or regurgitation. A bicuspid or quadricuspid valve may show doming in systole without stenosis being present. Site of the VSD is demonstrated, as are the two ventricles.
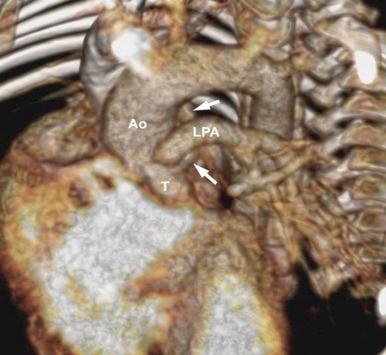
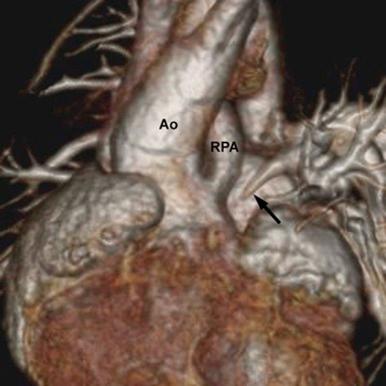
CT angiography (CTA) and MRI are not routinely indicated, but these imaging modalities may be indicated in specific circumstances in both neonates and older children. CTA provides excellent spatial resolution ( Fig. 43-10 ). When echocardiography suggests complex pulmonary artery problems such as stenosis or discontinuity, but there is no concern about pulmonary vascular resistance, CTA can define the morphologic details, and cardiac catheterization can be avoided ( Fig. 43-11 ). MRI can quantify the regurgitant fraction of an abnormal truncal valve, providing objective data for longitudinal follow-up and decision making ( Fig. 43-12 ).


Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here