Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
With an increased number of adults and adolescents participating in fitness programs and competitive sports, there has been an increase in thoracic and lumbar spinal problems.
Most injuries are soft tissue injuries, and appropriate training and avoidance of aggravating activities may allow participation while the pain resolves.
Treatment of an athlete can be complicated by his or her competitiveness and the fact that the athlete will be returning to the activity that precipitated the injury.
The primary treatment objective is the protection and preservation of the nervous system.
Spine injuries occur with a reported incidence of 7%–27% among sports-related injuries.
The use of biologic injections (platelet-rich plasma [PRP], stem cells) for treatment of spinal issues is controversial at this time.
The spine is a mechanical structure consisting of bones, joints, ligaments, and muscles surrounding and distributing neural elements.
The thoracic spine is more stable than the lumbar and cervical spine and is less mobile because of the thoracic cage.
The spinal column is composed of 33 vertebrae divided into five sections: cervical (7), thoracic (12), lumbar (5), sacral (5), and coccygeal (4) ( Fig. 53.1 ).
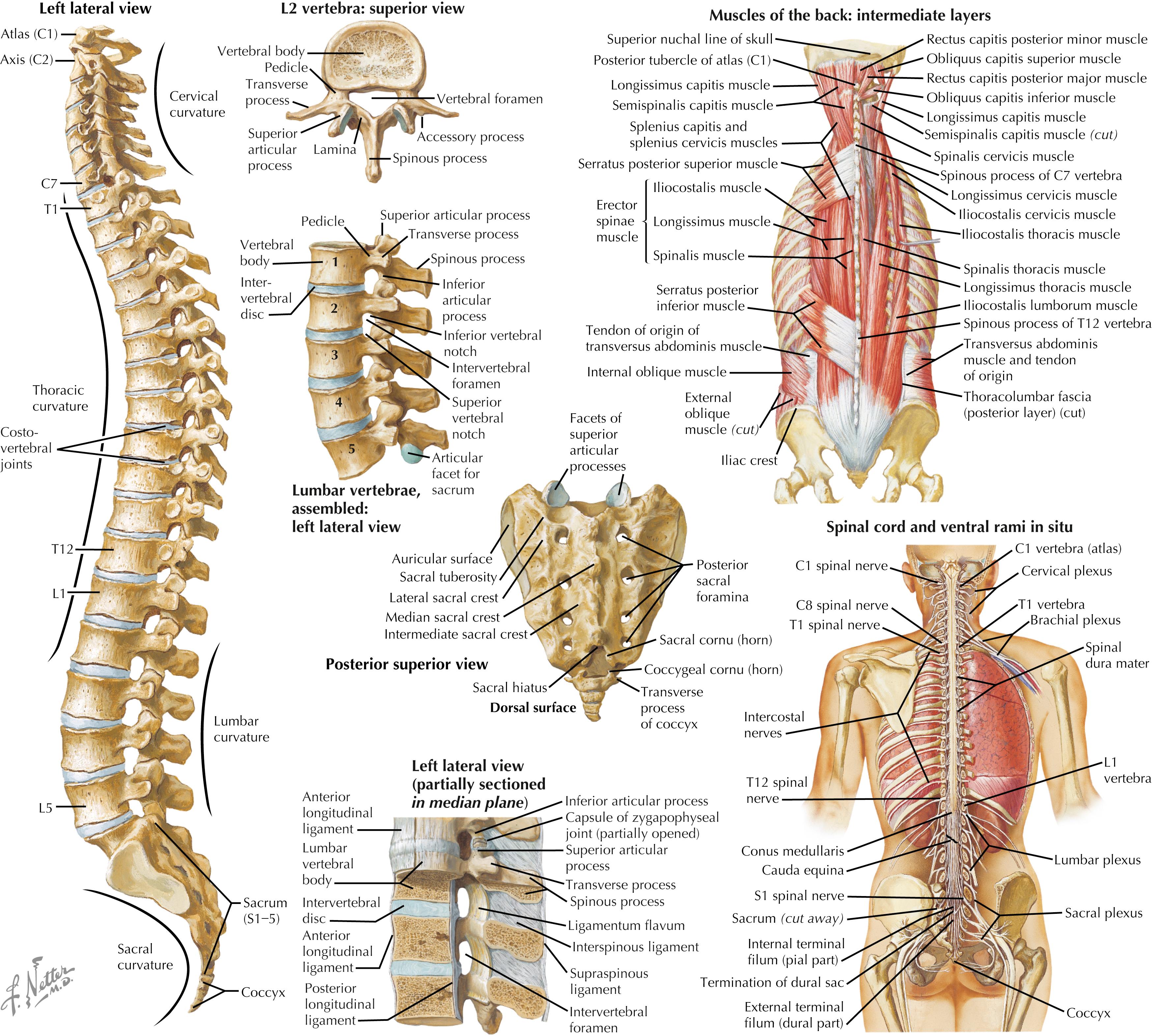
Vertebral body: Large, strong, anterior weight-bearing structure (see Fig. 53.1 )
Posterior vertebral arch: Semicircular-shaped structure surrounding the central canal, above and below the vertebral foramen through which the roots pass; composed of pedicles, which project dorsally off the body, one on each side, and the lamina, which connects the pedicles; from the pedicles and lamina, project the transverse process ; from the lamina, project the spinous process ; these are locations for muscular attachments. Each lamina articulates with the lamina above and the lamina below through facet joints. These synovial-lined facet joints are formed by a superior articular process from the lamina below and an inferior articular process from the lamina above and are surrounded by a facet capsule or ligament (see Fig. 53.1 ).
Pars interarticularis: Literally, the “part between the joints,” or the area between these facet joints; relevant because it is the weak link anatomically and is susceptible to injury and stress fracture
Sacrum: Coalesced lower segments of the spine that articulate with the pelvis
Costovertebral joints: Area of articulation of the thoracic vertebrae with its rib
Disc: Major ligament connecting each vertebral body; composed of two types of tissue: annulus fibrosus (outer layer of fibers that functions to hold the nucleus pulposus and restrains the vertebral bodies) and nucleus pulposus (gelatinous structure located in the annulus)—both are responsible for load-bearing
Anterior longitudinal ligament: Strong bond of fibrous tissue that runs the entire length of the spine along the anterior vertebral bodies (see Fig. 53.1 )
Posterior longitudinal ligament: Weaker than the anterior ligament; runs along the posterior surface of the vertebral bodies
Ligamentum flavum: Very strong ligament attaching the lamina above to the lamina below
Facet capsule: Connects each superior articulating process with its corresponding inferior articulating process
Interspinous ligament: Connects each spinous process to the one below
Supraspinous ligament: Runs along the dorsal surface of the tips of the spinous processes
Costotransverse ligaments: Thoracic area
Thoracolumbar fascia: Investing tissue that separates the muscular compartments and fuses with the aponeuroses of several muscles (see Fig. 53.1 )
Anterior groups of muscles: Anterior to the transverse processes; include psoas, intertransversalis, quadratus, and levator costae
Posterior groups of muscles: Posterior to the transverse process; include superficial muscles, erector spinae (semispinalis, longissimus, and iliocostalis), deep muscles, multifidus, rotares, and interspinalis
Accessory group of muscles: Includes abdominal muscles, latissimus dorsi, rhomboids, and gluteus maximus
Neural elements of the spine include the spinal cord from the occiput to about L1, the conus medullaris or lower portion of the cord thickened by the mass required to innervate the lower extremities located from T11 to L1, and the cauda equina from L1 to the sacrum; the nerve roots exit at each level on both sides of the canal via the vertebral foramina (see Fig. 53.1 ).
Vascular elements of the spine include a complex system of intradural and extradural arteries and veins that supply the neural elements.
The spinal column has five principal functions:
Support of the head
Support of the abdominal contents and pelvic girdle
Point of attachment for the thoracic cage and muscles
Protection of the spinal cord and the neural elements within while allowing motion
The biomechanical transfer of the weight and bending movements of the head and trunk to the pelvis
Understanding several basic concepts of biomechanics helps us understand how specific activities can exacerbate symptoms in certain syndromes:
In the spine, flexion of the lumbar spine increases the size of the intervertebral canal and the intervertebral foramina.
Extension decreases the size of the intervertebral canal and the intervertebral foramina.
Flexion increases dural sac and nerve root tension.
Extension decreases dural sac and nerve root tension.
Front flexion, axial loading, and an upright posture increase intradiscal pressure: pressure is greater while sitting, less while standing, and least while lying down.
With flexion, the annulus bulges anteriorly.
With extension, the annulus bulges posteriorly.
Nuclear shift in an injured disc is poorly documented, but the disc probably shifts in the direction of the annular bulge.
Rotation and torsion produce annular tears and disc herniations.
Information obtained during history taking and physical examination is critical. The following questions are particularly relevant.
When and how did your symptoms start? Mechanism of injury can help locate the damage. Onset can be telling because a gradual onset can be more related to a stress injury, and a rapid severe onset may indicate a more acute injury.
What is the location of the pain? Neurologic involvement is likely when a patient perceives more pain in the leg than in the back. The percentage of back to leg pain is relevant. Associated neurologic symptoms such as numbness, dysesthesia, weakness, or spasticity are important to note. There are multiple nociceptive sources in the spine.
When does it hurt? Night pain may be more ominous and associated with tumors. Pain with motion and relieved by rest implies mechanical pain. Constant pain unaffected by rest may indicate an inflammatory component.
What makes it worse? Discogenic pain is usually worse with flexion or prolonged sitting and increases with a Valsalva maneuver (cough or strain with defecation). Pain from a spondylolysis is worse than that with hyperextension. Pain from spinal stenosis (pseudoclaudication) is worse with ambulation or prolonged standing. Sacroiliac (SI) joint dysfunction can be worse with hyperextension.
What makes it better? Discogenic pain can be improved by lying down with knees and hips flexed (opens foramina and unloads disc). Spinal stenosis symptoms can improve by bending forward (as in walking over a grocery cart) or by sitting.
How do you train? This may reveal a voluntary restriction that helps with a diagnosis or reveals a training error compatible with a specific syndrome.
Do you have any of these factors? Bowel, bladder, or sexual dysfunction may indicate significant neurologic involvement of the cord, conus, or cauda equina. Weight loss, anorexia, night pain, and pain at rest may suggest neoplasia. Fever may indicate infection. A visceral type of pain with referral may indicate kidney, prostate, bowel, or vascular pathology.
Should address inspection, palpation, and percussion and identify:
Exact location of tenderness, dysesthesias, or numbness
Maneuvers that reproduce the pain
Presence of neural tension signs
Deficits in range of motion (ROM)
Any neurologic deficit
Inspection of posture and stance: Patients in a sitting position may tend to tripod or lean back to unload the spine. When standing, a list to one side may suggest nerve root compression. The appearance of a flat back with a vertical sacrum may be seen in advanced spondylolisthesis. Scoliosis may be detected in a standing position.
Inspection of gait: Myelopathic patients may walk with spasticity. A forward flexed posture can be seen in stenosis. Patients with discitis may have a rigid short-stride gait.
Inspection of ROM: May be limited by painful conditions; extension may be limited in stress fractures and facet syndromes. Discogenic pain may limit flexion.
Palpation: May detect muscle spasm, deformity with a palpable mass, scoliosis, spondylolisthesis, or a gibbus deformity; tenderness may be present at the sciatic notch.
Percussion: May elicit tenderness in trauma or infection, and costovertebral angle tenderness may imply a kidney problem
Neurologic: Most critical portion of the examination ( Table 53.1 and Fig. 53.2 ); upper motor neuron findings of spasticity, weakness, numbness, hyperreflexia, and clonus may indicate spinal cord pathology; lower motor neuron findings of flaccid muscles, weakness, numbness, and hyporeflexia may indicate cauda equina or root injury. Sensory levels on the trunk will help determine the level of spinal cord injury, if present. A rectal and cremasteric reflex examination is recommended with any spinal cord injury.
| Root | Strength | Sensation, Dermatomal Distribution | Reflex |
|---|---|---|---|
| L1–L2 | Iliopsoas | Inguinal area and upper two-thirds of anterior thigh | |
| L3 | Quadriceps | Oblique band of distal third of anterior thigh immediately above patella | |
| L4 | Tibialis anterior and quadriceps | Medial side of lower leg and foot | Patellar tendon |
| L5 | Extensor hallucis longus and tibialis anterior | Anterior aspect of lower leg and dorsum of foot | Not reliable (posterior tibialis reflex present in only 40%–50% of population) |
| S1 | Peroneus longus and brevis gastrocnemius | Lateral aspect of lower leg and lateral foot | Achilles tendon reflex |
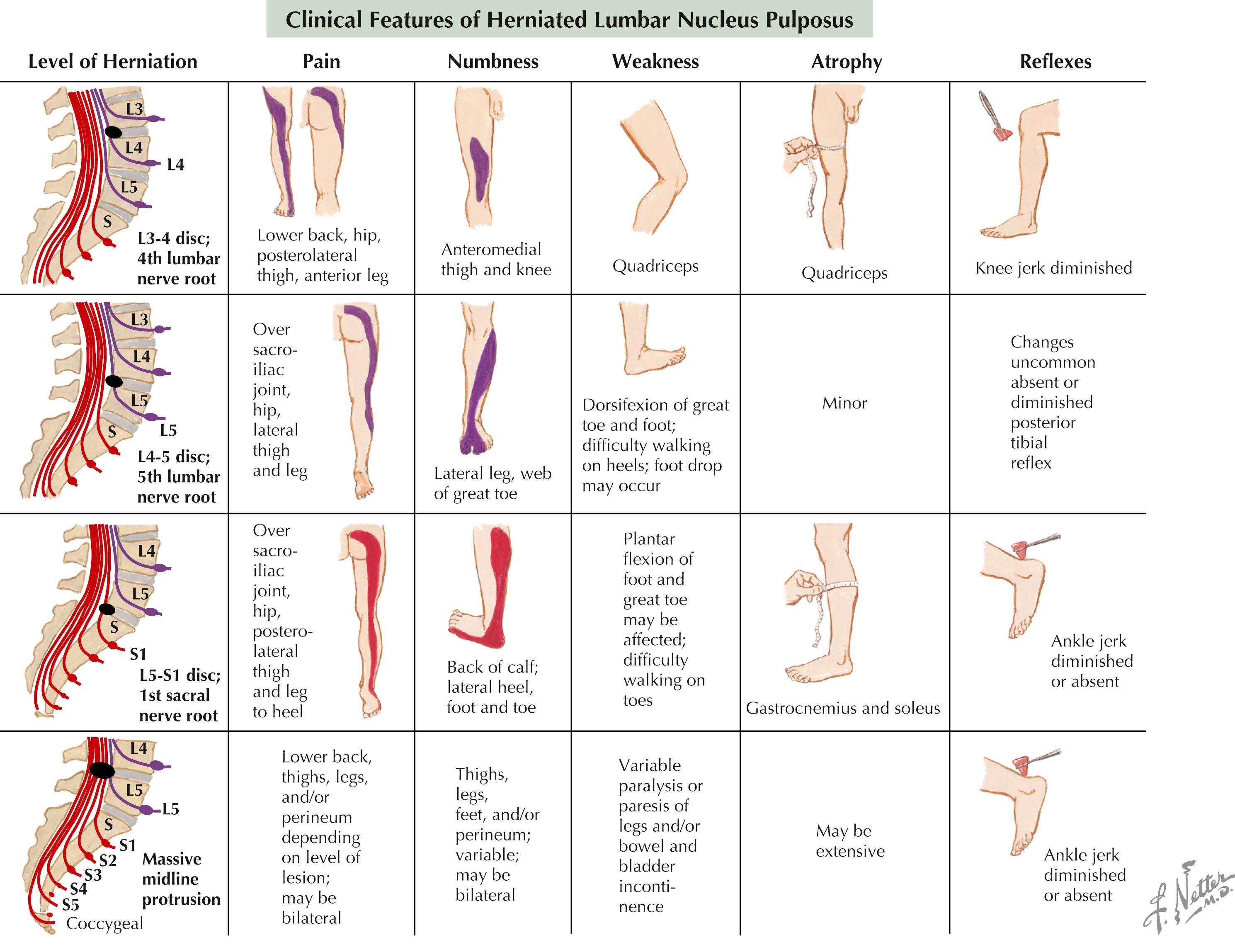
Straight leg raise (SLR) test: Tension test that indicates nerve irritation in the sciatic nerve if positive with radicular pain at <60–70 degrees of leg elevation ( Fig. 53.3 )
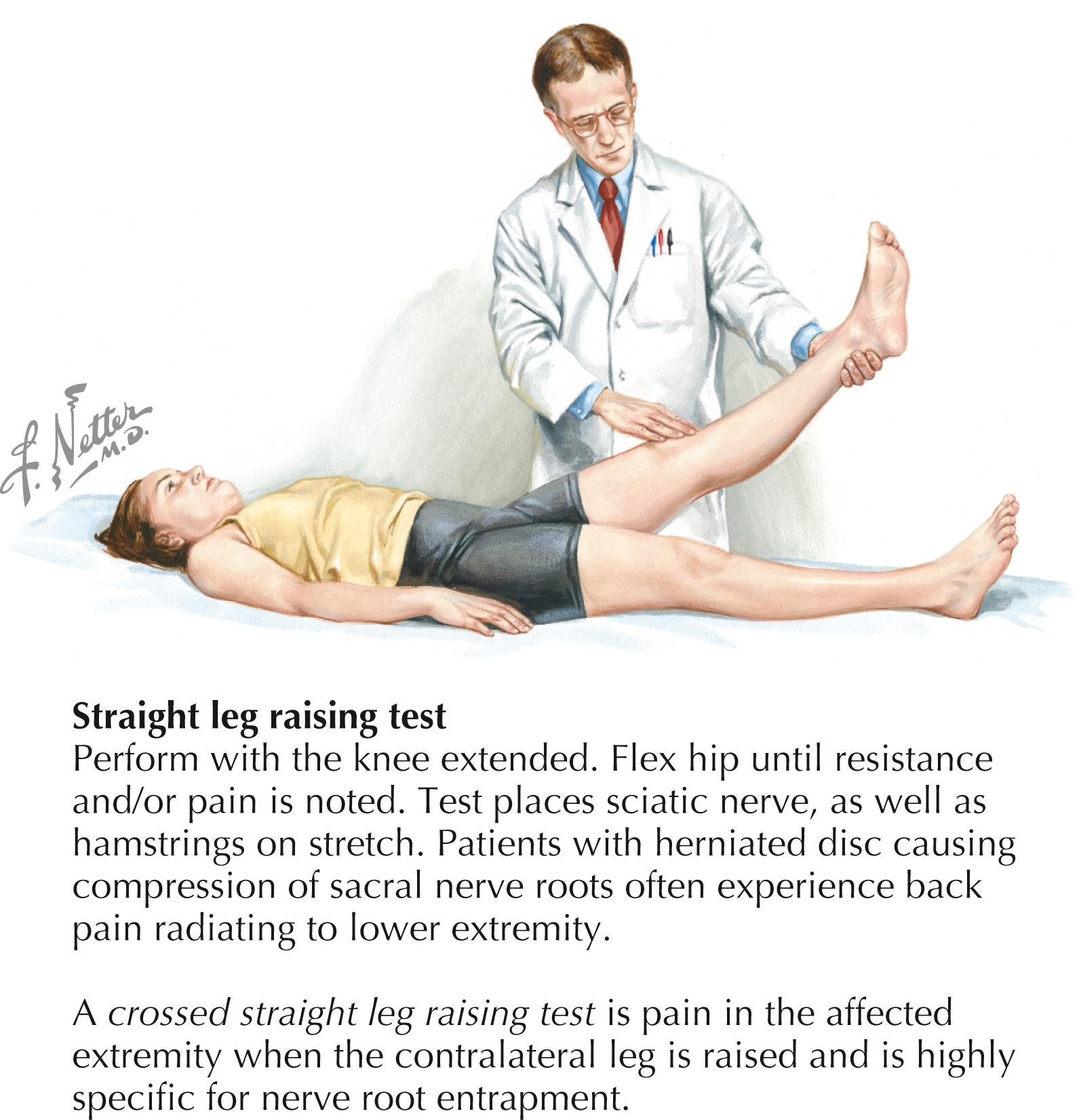
SLR test with foot dorsiflexion (Lasègue test): Tension test suggesting sciatic nerve irritation if painful
SLR test while sitting: Positive when extending the knee while patient is sitting causes radicular pain; patient may lean back to gain relief. A positive and a negative SLR test while sitting can be inconsistent and suggest other etiologies.
Crossed SLR test: Positive test may be pathognomonic for a herniated disc. With the patient sitting, the examiner lifts the unaffected leg; in the presence of a herniated disc, this may produce pain in the affected leg.
Femoral stretch test: In a side-lying position with knee flexed 90 degrees, the hip is extended, stretching the femoral nerve. Pain on the anterior thigh suggests femoral nerve or upper lumbar root irritation.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here