Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Surgical treatment of spinal disorders at the cervicothoracic junction is challenging because of the complex anatomy and biomechanical properties of this region. Access to the cervicothoracic junction is complicated by important vascular, visceral, and soft-tissue structures, and knowledge of these structures and surgical landmarks is essential for decompression and stabilization.
Cervicothoracic pathologies are relatively uncommon but include bacterial and tuberculous infections, fractures from primary bone disease, primary bone tumors, meningeal tumors, vascular malformations, congenital connective tissue and skeletal disorders, trauma, and thoracic disc herniations ( Table 178.1 ). Up to 15% of patients with spinal neoplasms have lesions of the upper thoracic vertebrae, and 10% of spinal metastases arise from the T1 to the T4 region. One group reported that 8% of patients undergoing tumor resection required posterior instrumentation at the cervicothoracic junction. Additionally, as many as 9% of traumatic injuries can involve the cervicothoracic junction.
| Metastatic tumors |
|---|
| Primary tumors of bone |
| Primary lymphoma |
| Intradural, extramedullar tumors |
| Intradural, intramedullary tumors |
| Bacterial infections |
| Tuberculous infections |
| Vascular malformations |
| Pathologic fracture (primary metabolic disease of bone) |
| Connective tissue and skeletal disorders |
| Traumatic vertebral fractures |
| Disc herniations |
Up to 80% of unstable cervicothoracic pathologies can have neurologic compromise, and many of these lesions require surgical treatment. Unfortunately, injuries to this area are often overlooked on routine radiographic studies. , The surgical goals include neural decompression, immediate stabilization, restoration of anatomic spinal alignment, and early rehabilitation. Appropriate treatment is necessary because acute unstable lesions of the cervicothoracic junction can have severe consequences including poor rates of recovery and significant mortality from cardiopulmonary-related complications.
Posterior approaches, such as laminectomy and pediculectomy, are common approaches to many diseases of the spine. When treating anterior spinal element diseases, these techniques might not be adequate, can have a higher complication rate, and can disrupt spinal stability. , For these reasons, a variety of anterior and posterolateral surgical approaches have been developed.
The first detailed description of a posterolateral approach to the anterior elements was the costotransversectomy. Although this technique gave adequate exposure of the middle and lower thoracic spine, it was less useful in the upper thoracic region. In 1954, Capener described a more-extensive posterolateral exposure, the lateral rhachotomy. In 1976, Larson and colleagues reported a modification of the lateral rhachotomy, the lateral extracavitary approach, which provided improved exposure of the middle and lower thoracic spine with less morbidity. However, these new additions were still limited at the cervicothoracic junction owing to the shoulder girdle. The lateral parascapular extrapleural operation, a modification of the lateral extracavitary approach, eliminates those obstructions and provides exposure of the thoracic vertebrae up to the inferior end plate of C7.
Purely anterior, supraclavicular approaches to the cervicothoracic junction were initially described by Jonnesco and Brunig in 1923 and later used by Royle for spastic paralysis, by Gask for Raynaud disease, and by Ochsner and DeBakey for thoracic sympathectomy. However, exposure of the thoracic area was restricted by the clavicle, so the transmanubrial and transclavicular approach was developed by Sundaresan and colleagues in 1984 and modified by Birch and colleagues in 1990.
Another approach to the anterior thoracic vertebral elements, the anterolateral thoracotomy, was first described by Hodgson and colleagues. This approach involves resection of the third rib and requires transpleural mobilization of the lung with ligation and division of the intercostal arteries, intercostal veins, and the hemiazygos vein.
The following sections discuss the clinical features of cervicothoracic junction diseases, including preoperative evaluation, anesthetic considerations, relevant regional surgical anatomy, biomechanics of the cervicothoracic junction, surgical approaches, and options for surgical reconstruction and stabilization.
The differential diagnosis for cervicothoracic pathologies is listed in Table 178.1 . Disease processes in this region can manifest as pain without neurologic deficit, thoracic myelopathy, C7 or T1 radiculopathy, or a combination of these signs and symptoms. Table 178.2 lists the presenting findings in our series of patients with pathologic processes of the cervicothoracic junction (C7 to T4). Of these patients, 93% had decreased sensation, 83% presented with generalized upper thoracic back pain, and 58% had leg weakness. C7 and T1 lesions were less common, and consequently, 33% of patients presented with radicular symptoms and 35% demonstrated hand weakness on examination. Other, less common findings included ataxia (25%) and bowel or bladder dysfunction (17%).
| Signs and Symptoms | Percentage of Patients with Signs or Symptoms |
|---|---|
| Back pain | 83 |
| Radicular pain | 33 |
| Leg weakness | 58 |
| Decreased sensation | 92 |
| Hand weakness | 35 |
| Bowel or bladder dysfunction | 17 |
| Ataxia | 25 |
| Babinski sign | 58 |
Radiologic evaluation begins with anteroposterior and lateral plain radiographs, and evidence of pathology includes malalignment, vertebral collapse, and widening of the pedicles. These radiographs can demonstrate traumatic or pathologic vertebral fractures, infections, tumors, and deformities.
Infections such as osteomyelitis or discitis have a variety of characteristics on plain radiographs. The earliest and most consistent finding of infection is narrowing of the disc space, which is present in 74% of patients. After 3 to 6 weeks, destructive changes in the body can be noted, which usually begin as lytic areas in the anterior aspect of the body adjacent to the disc and end plate. Active bone formation and sclerosis is also present in 11% of patients.
Metastatic disease of the bone has several classic signs including unilateral erosion of a pedicle, fishmouthing (cephalad and caudad end plate concavity within the vertebral body), osteoblastic changes, and vertebral body collapse. These findings can occur late in the disease process because 30% to 70% of the bone must be destroyed before changes are visible on plain radiographs.
Radionucleotide bone scintigraphy is a sensitive but not specific method for detecting metastatic disease and infections. , However, false negatives have been reported with lung cancer, renal cell carcinoma, myeloproliferative diseases, and regional ischemia, and in patients with leukopenia.
Myelography is primarily used to evaluate the patency of the subarachnoid space. Thus, myelography can demonstrate the level of a metastatic lesion by indentation or complete blockage of the myelographic dye column as it flows through the spinal canal. Additionally, myelography can demonstrate the presence of intradural extramedullary or intramedullary tumors, disc herniations, retropulsed vertebral fragments from pathologic or traumatic fractures, and vascular malformations.
Computed tomography (CT) also aids in the evaluation of diseases of the thoracic spine. These pathologies include metastatic disease, intradural tumors, disc herniations, and vascular malformations. Additionally, CT aids in defining the extent of paraspinal soft-tissue involvement for tumor staging and surgical planning, and also helps determine the extent of bone destruction. In addition, CT scans can help distinguish between osteoporosis and tumor as a cause of vertebral body collapse.
Magnetic resonance imaging (MRI) is the most important diagnostic tool for evaluating diseases of the thoracic spine. MRI permits early diagnosis of infection and recognition of paravertebral or intraspinal abscesses without the risk associated with myelography. MRI is also effective in demonstrating the extent of metastatic disease, primary tumors of bone, primary lymphoma, intradural tumors, thoracic disc herniations, and vertebral fractures. Additionally, this modality may be helpful in spinal vascular malformations, and when assessing metastatic disease, MRI has been found to be at least as sensitive and accurate as gallium and bone scanning combined. Finally, MRI provides anatomic detail, especially of soft tissue and nervous structures, not available with any other imaging studies.
Metabolic evaluation of cervicothoracic junction pathology should include complete blood count, kidney profile (electrolytes, blood urea nitrogen, and creatinine), liver profile, and erythrocyte sedimentation rate. Other helpful metabolic evaluations include calcium, phosphorus, alkaline phosphatase, serum protein electrophoresis, and serum transferrin analysis. Antinuclear antibody and rheumatoid factor analysis assist in the evaluation for rheumatoid arthritis. Additionally, bone marrow aspiration may be helpful in the diagnosis of blood-borne dyscrasias, and antigenic markers for specific tumors include carcinoembryonic antigen, serum acid phosphatase, and prostate-specific antigen.
The lateral parascapular extrapleural approach is a posterolateral surgery that allows nearly lateral access to the cervicothoracic junction vertebral bodies. The anterolateral thoracotomy is a transthoracic approach through the third rib that allows access to the anterior and lateral aspects of the vertebrae and for control of the mediastinal vasculature. The relevant anatomy may be summarized in three major areas: scapula and parascapular anatomy, posterior thoracic cage, and retromediastinal space and spinal anatomy.
Posterolateral access to the thoracic cage and vertebral elements is hindered by the scapular and the parascapular shoulder musculature ( Fig. 178.1 ). Mobilization of the scapula anterolaterally is necessary and requires the disruption of the posteromedial shoulder musculature.
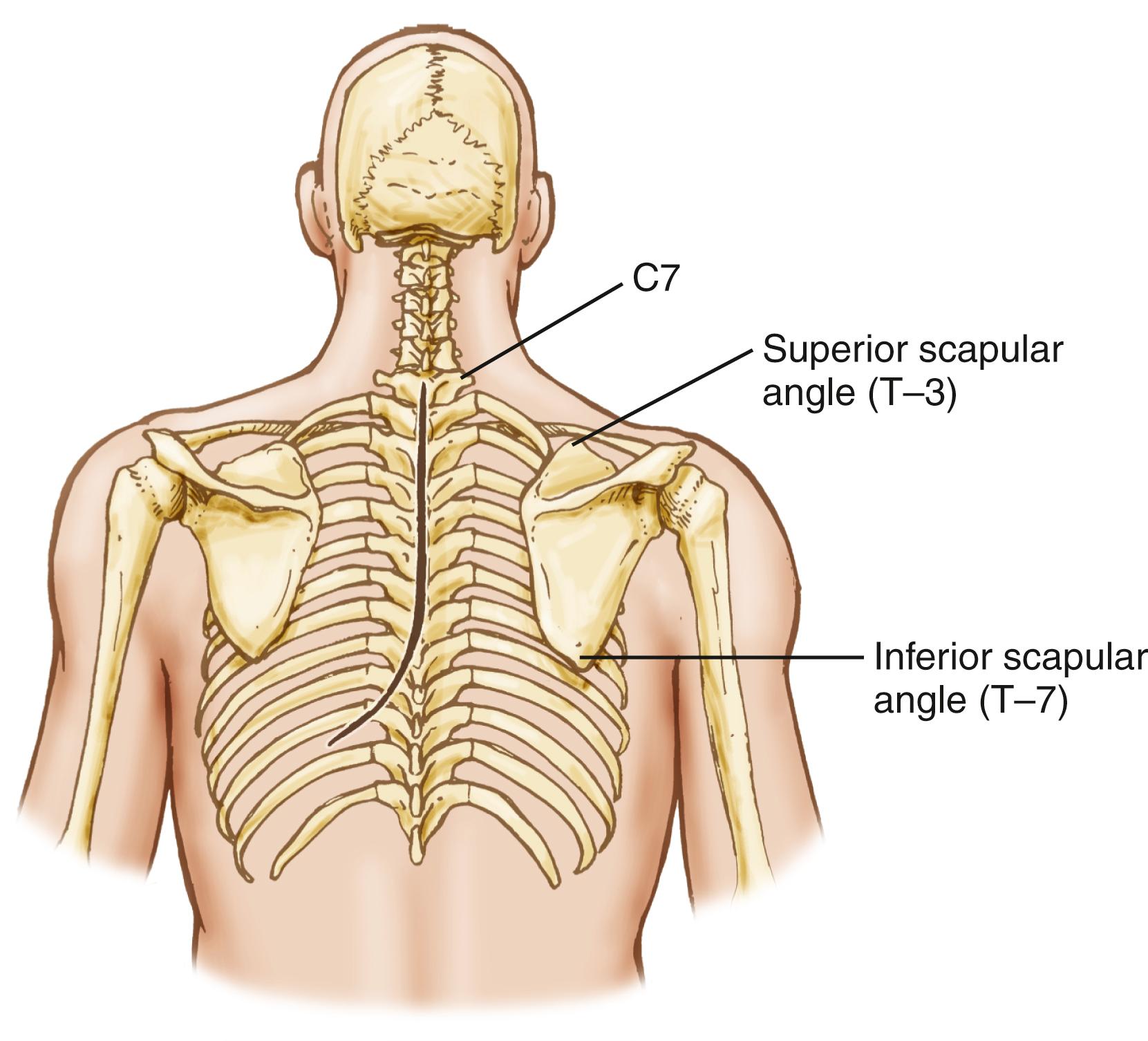
The first muscle encountered after skin incision is the trapezius muscle, which inserts medially at the superior nuchal line and external occipital protuberance and at the spinous processes of C1 through T12. This muscle extends laterally as the upper, intermediate, and lower divisions to the lateral third of the clavicle, the acromion, and the scapular spine. The trapezius muscle stabilizes and abducts the shoulder by the insertion of the lower fiber aponeurosis to the tubercle of the lower lip of the scapular spine. The trapezius muscle is innervated by the ventral rami of C3 and C4 of the spinal accessory nerve, which lies deep to the trapezius muscle and superficial to the levator scapulae. The arterial supply is from branches of the dorsal scapular artery.
The rhomboid major, rhomboid minor, and levator scapulae muscles are deep to the trapezius muscle. The ligamentum nuchae of the spinous processes provides the insertion site for the rhomboid major (T1–T4) and the rhomboid minor (C6–C7). Similarly, both of these muscles insert along the vertebral edge of the scapula: the rhomboid minor above and the rhomboid major below the scapular spine. The dorsal scapular artery supplies all three muscles, and the dorsal scapular nerve innervates the rhomboids. The levator scapulae muscle is innervated via branches from C3, C4, and C5. Both the artery and nerve lie deep to the muscle bodies, are located medially under the scapula, and are rarely seen during a routine exposure. The serratus posterior superior muscle lies deep to the trapezius muscle from C6 through T2, and the splenius arises ventral to this muscle at the ligamentum nuchae and upper thoracic spine, dividing into the splenius capitis and splenius cervicis. The splenius capitis inserts on the superior nuchal line and mastoid process, and the splenius cervicis joins the levator scapulae to insert on the transverse processes of C1 through C4. These muscles stabilize and rotate the skull.
During exposure of the cervicothoracic junction, the spinous process insertions of the trapezius, rhomboid, serratus posterior superior, splenius capitis, and splenius cervicis are laterally retracted as a single group. As these muscles are taken down, the scapula can be rotated anterolaterally out of the operative field. This maneuver exposes the posterior and posterolateral rib cage.
The deep or intrinsic muscles including the erector spinae and transversospinalis muscles are next encountered ( Fig. 178.2 ). The erector spinae muscles originate from the sacrum as a dense aponeurotic band and divide into three columns below the last rib as they proceed superiorly. The iliocostalis muscle is located laterally and inserts from the angles of the ribs and into the cervical transverse processes from C4 through C6 as series of related muscular bundles. Each bundle extends over approximately six segments, with the more medial bundles extending more cephalad.
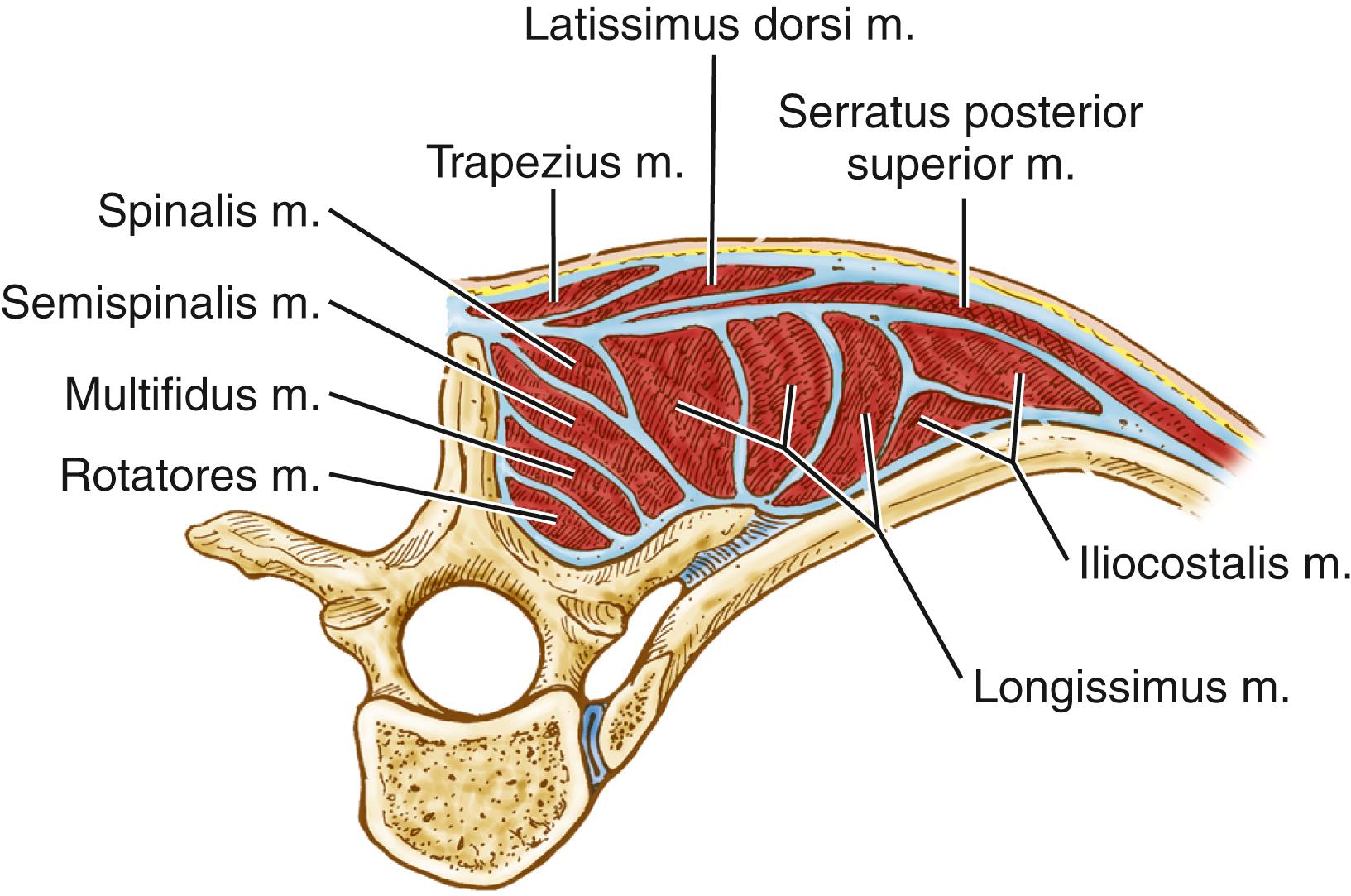
The longissimus muscles (thoracis, cervicis, and capitis) insert into the lumbar and thoracic transverse processes and ribs between T2 and T12. Medially, the muscle bundles extend from T1 through T4 to the transverse processes of C2 through C6. Medial to the cervical insertions, other bundles extend superiorly to the mastoid process deep to the splenius capitis and sternocleidomastoid muscles. Thus, the longissimus is the only erector spinae muscle to reach the skull. Finally, the aponeurotic spinalis muscle extends from the upper lumbar to the lower cervical spinous processes.
The transversospinalis muscle group passes cephalad from the transverse processes to the spinous processes immediately deep to the erector spinae muscles in three layers. The most superficial layer, the semispinalis, arises from the tips of the transverse processes and inserts at the tips of the spinous processes approximately five vertebral levels cephalad. At the cervicothoracic junction, this muscle is primarily composed of the semispinalis capitis. This muscle passes from the upper thoracic transverse processes and lower cervical articular processes (C4–T4) to the occipital bone between the superior and inferior nuchal lines. The muscle fibers run vertically and attach to the ligamentum nuchae. The intermediate layer, the multifidus, originates from the erector spinae aponeurosis and from the transverse processes up to C4 and extends to the lower border of each spinous process. This muscle spans approximately three levels. The deepest muscles of this group, the rotatores, are muscles that bridge one interspace. They pass from one transverse process root to the spinous process root immediately above.
These muscle groups extend the vertebral column or can bend and rotate the vertebrae. The erector spinae and transversospinalis muscles are typically dissected off the spinous processes, laminae, facets, and transverse processes as a single muscular mass. This dissection exposes all the vertebral elements from the spinous processes to the transverse processes, as well as the costotransverse ligaments, joints, and ribs.
Each rib articulates with its own vertebral body and transverse process, the vertebra above, and the intervertebral disc between them ( Fig. 178.3 ), but the first rib articulates only with its own vertebral body. Each of these articulations forms separate synovial joints, and the joints of the posterolateral vertebral body surface are separated by an intra-articular ligament that attaches to the intervertebral disc. An articular capsule surrounds the joints and attaches to the vertebral body anteriorly via the radiate ligament.
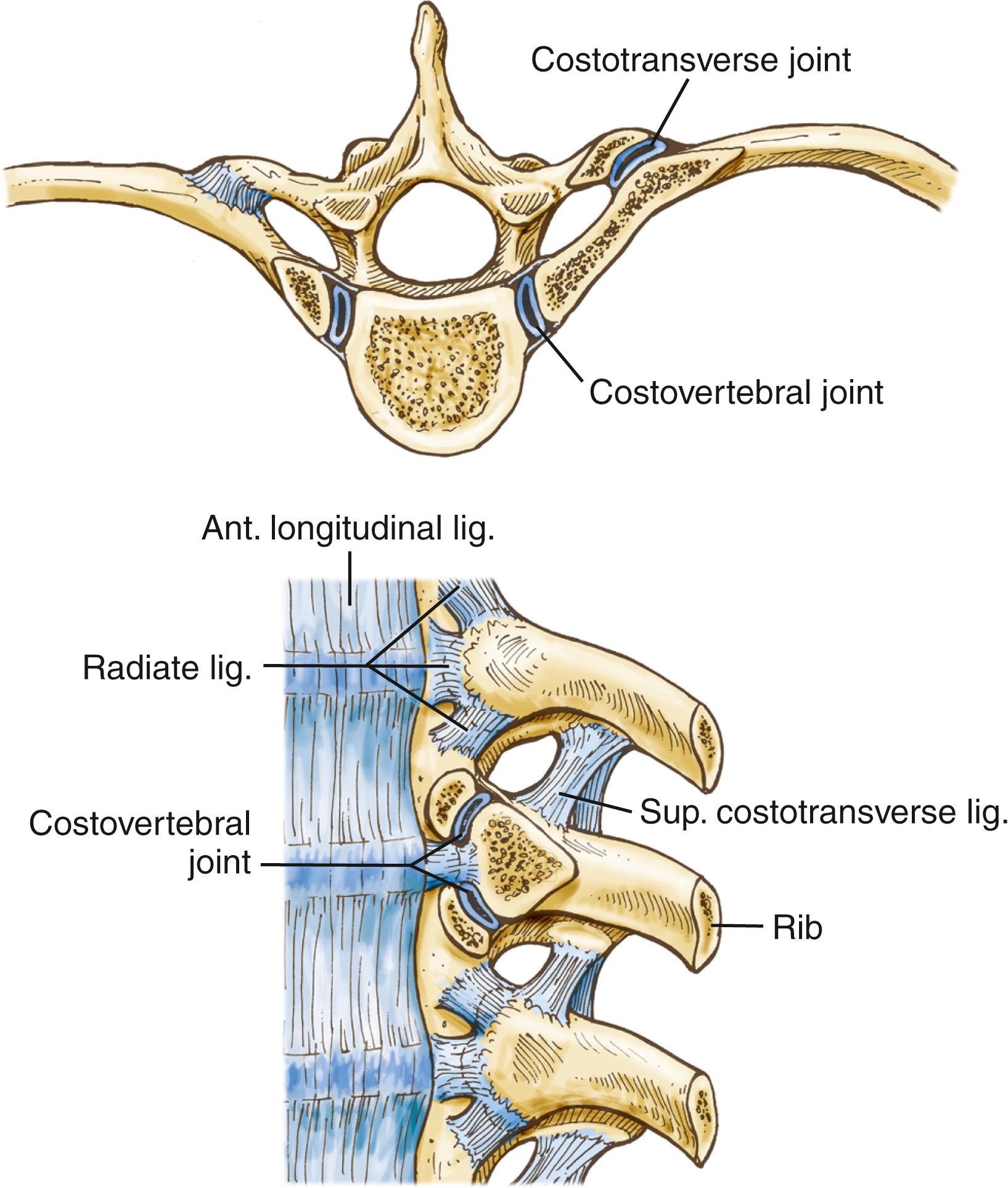
The costotransverse joint is surrounded by an articular capsule and is strengthened laterally by the lateral costotransverse ligament and the costotransverse ligament. The superior costotransverse ligament joins the neck of the rib to the transverse process immediately above. The canal formed between this ligament and the vertebral column contains the dorsal ramus of the spinal nerve and the dorsal branch of the intercostal artery. Finally, the ribs are attached to one another through the intercostal musculature, which originates medially on the superior rib and inserts laterally on the inferior rib.
The intercostal musculature contains the intercostal nerve, artery, and vein as they pass between the internal intercostal membrane and the pleura and between the internal and innermost intercostal muscles. Most commonly, the intercostal vein is cephalad and the intercostal artery is more caudad. The intercostal nerve may be separate from these structures and is located most caudad. The pleura lies ventral to the intercostal bundle and the intercostal muscles.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here