Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Repair of a bilateral cleft lip deformity is challenging yet rewarding. Many surgeons find it hard to achieve results comparable to those of unilateral repairs. Poorly planned surgeries can leave noticeable residual deformities. There is a combination of genetic and environmental factors that may affect development of cleft lip in weeks 4 to 10 of gestation. These patients present along a spectrum of severity. Wide clefts, and those with a prominent premaxilla, may benefit from pre-surgical molding. The child must be of appropriate weight, size, and vigor before undergoing surgery. The operation can be performed with a relatively basic plastic surgery instrument set. Arguably the important part of the operation is the surgical marking, which is done before making any incision. This will be the blueprint for the entire repair. After marking, local anesthetic is injected, and the procedure begins in a stepwise fashion as detailed later. Post-operative management is simple, and major complications are rare.
Repair of the bilateral cleft lip deformity requires an understanding of the aberrant anatomy involved. The pre-operative nasolabial anatomy is often very distorted, and closure can bring a tremendous sense of relief to the patient's family. The surgical procedure, however, is nuanced and difficult; many surgeons feel that it is difficult to obtain results that compare favorably to those seen in unilateral repairs. A poorly designed and executed repair can leave residual deformities that are noticeable at conversational distance. It can also lead to significant restriction in maxillary growth. Older children or adult patients who have had an inadequately performed lip and/or palate repair often have significant maxillary retrusion. The primary goals of bilateral cleft lip repair are to achieve appropriate symmetry, address the nasal deformity, maintain continuity of the muscle, and design a philtrum/tubercle complex of appropriate size and shape. There are many techniques described in the literature; in this chapter we present one method that should allow a surgeon to achieve consistent and reliable outcomes.
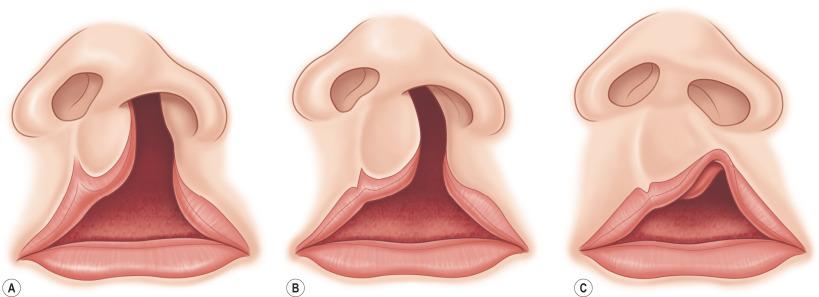
Much as in the unilateral cleft lip deformity, patients with bilateral clefts present within a spectrum of severity. About half of patients have a symmetrical and complete bilateral cleft deformity. The remaining half of patients are split between symmetrical incomplete deformities and asymmetrical incomplete deformities. Incomplete cleft defects can range from what is called a “microform” cleft to an essentially complete cleft deformity with just a residual cutaneous band present. In microform cleft lip deformities, there is a notch in the vermilion that is about 3 to 5 mm higher than is typical. On the other end of the “incomplete” spectrum is a deformity with essentially a small skin bridge, similar to a Simonart's band that is described in unilateral cleft lip anatomy.
The associated cleft palate deformity is typically dictated by the severity of the lip deformity. Therefore patients with bilateral complete clefts of the lip will most often have a bilateral complete cleft of the secondary palate. In general, bilateral cleft lips represent about 10% of all cleft lip deformities.
Patients present with a wide range of anatomy, including the width of each cleft, the prominence/angle of the premaxilla, and the severity of the nasal deformity as well as the ability to maintain food intake. Although the diagnosis of a patient with a cleft deformity is straightforward, it is important to appreciate the spectrum of the process, because this will guide the surgeon's ultimate repair.
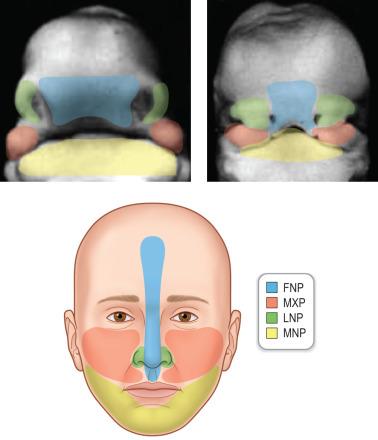
Cleft lip deformities are a result of incomplete fusion during embryological development. The basic foundational structure for facial shape is set early in gestation, within weeks 4 to 10. A number of prominences—including the frontonasal, maxillary, and mandibular—merge together to form the normal facial morphology. The lower portion of the frontonasal prominence divides into a medial nasal prominence and a lateral nasal prominence. (In various descriptions of this, the words “prominence” and “process” are used interchangeably.) Any disruption of this process can lead to craniofacial abnormalities.
Cleft lips form as a result of failure of the medial nasal process to contact the maxillary process. Lip formation is set largely during weeks 4 to 7 of human development. Cleft palates typically develop from a failure of fusion of the opposing palatine processes of the paired maxillary prominences.
There is a genetic contribution to the development of cleft lip and palate that is only partially understood. It is likely that there are environmental factors that can contribute as well. No single gene has ever been identified as leading to cleft lip or cleft palate. It does appear that isolated cleft palate is a unique process that differs from cleft lip with or without a cleft palate. A positive family history of cleft does increase the risk in subsequent births. Possible environmental contributors include the use of phenytoin or other anti-convulsants, smoking during the first trimester, and poor folic acid supply in the perinatal period.
The incidence of cleft lip (of any form) in birth is roughly 1 : 1000 for Caucasian babies. This rate is slightly lower in African Americans and higher in Asian populations. Roughly 10% of cleft lip deformities are bilateral.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here