Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
This chapter includes an accompanying lecture presentation that has been prepared by the authors: ![]() .
.
Optimal positioning provides the most direct safe trajectory to the surgical target; affords safety to the patient; eliminates the need for brain retraction; reduces intracranial pressure; and allows the surgeon to operate comfortably.
Patient positioning for the majority of procedures should involve the most direct trajectory from the entry point to the surgical target ( Fig. 24.1 ).
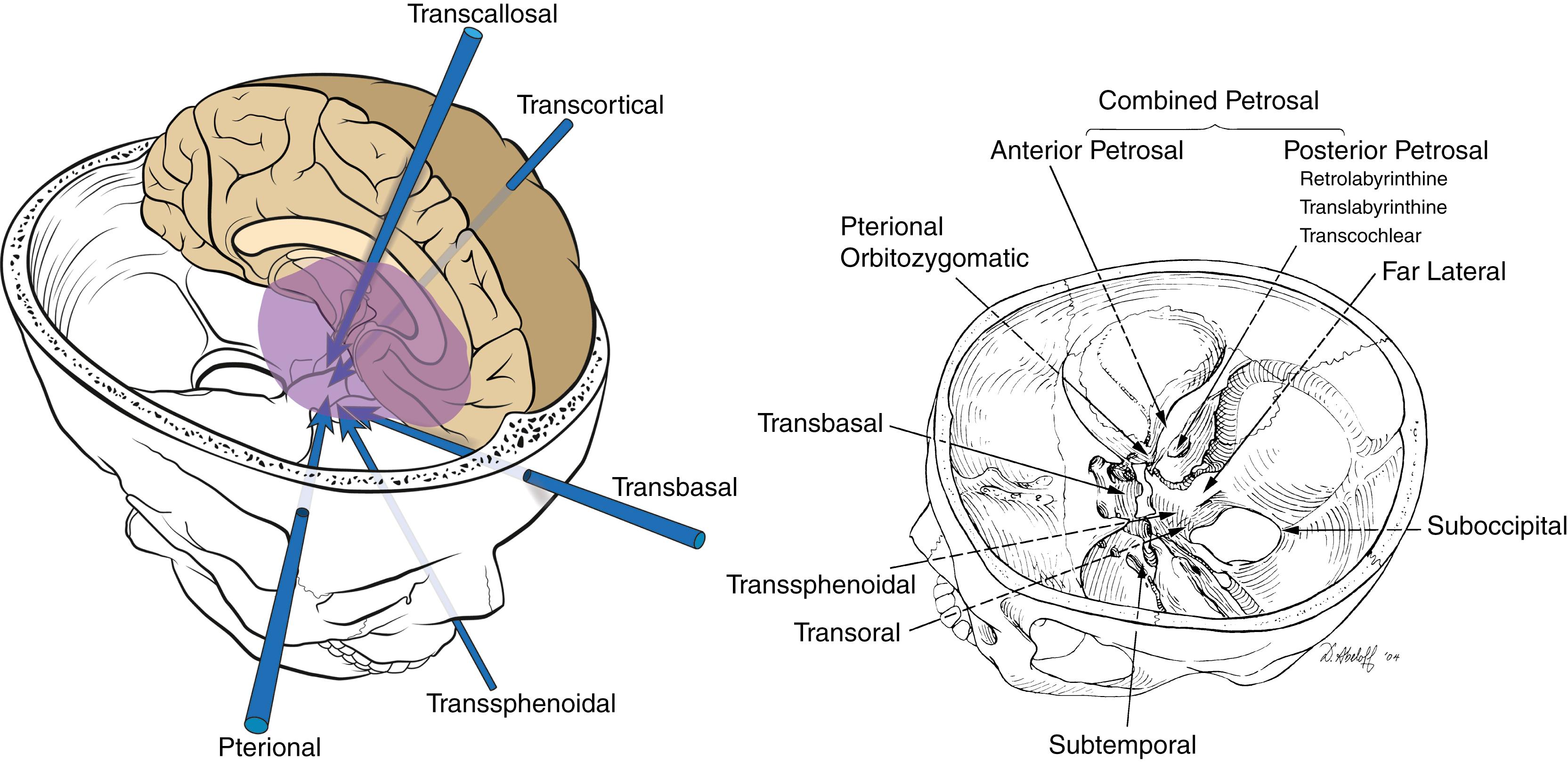
The ideal trajectory will also consider tumor projection and avoiding eloquent areas, even if it requires a longer trajectory.
Patient positioning that exploits the effects of gravity can significantly reduce the need for brain retraction and aid in visualization.
Appropriate placement of head fixation pins is important to avoid obstruction of the surgical field and inappropriate motion of the head during the procedure.
Patient positioning is also important to avoid other potential complications, such as the risk for air emboli in choosing a sitting versus a semisitting position.
Familiarity with various positions allows the surgeon to be flexible by tailoring what is most appropriate for each patient and pathology.
Positioning of the patient for intracranial procedures is a crucial step to completing a successful surgery. Optimal positioning is key to providing the most direct trajectory to the surgical target but also must afford safety for the patient. Optimal positioning can achieve many surgical benefits by eliminating the need for brain retraction, providing a clear and bloodless field, reducing intracranial pressure, presenting the anatomy and pathology in the ideal perspective for the surgeon, and minimizing the chance for avoidable complications. Here we review the fundamental principles of positioning for the most common approaches to cranial disease.
Like all surgical considerations, the planning of patient positioning should take place ahead of time. On the day of surgery, after safe and effective anesthetic induction and securing of adequate monitoring and access, the patient should be positioned on the operating table. The body should always be positioned before the head is secured to minimize the risk for cervical injury. A prone, supine, lateral, or sitting position is chosen to maximize exposure of the surgical target and minimize damage to surrounding structures. The imaginary trajectory from the highest point on the skull to the lesion in the brain should be the shortest distance between two points if possible, but should also consider tumor projection and avoiding eloquent areas. Optimal positioning can significantly reduce the need for brain retraction and thereby minimize brain pressure. If possible, the use of gravity for retraction is considered when approaching intracranial targets. A cranial fixation apparatus, such as the Mayfield head clamp, is used to prevent inappropriate motion of the head during the procedure; the pins are placed to avoid obstructing the surgical field and to minimize visible cosmetic scarring. Head positioning requires a combination of flexion, rotation, and neck extension maneuvers to achieve the ideal surgical trajectory. After the head is positioned, final padding is placed, and the patient is secured to the bed. When well planned and executed, the patient positioning will ensure patient safety, provide optimal access to the surgical target, and allow the surgeon to operate comfortably.
The pterional, or frontotemporal, craniotomy is known as the “workhorse” of cranial approaches. It is extremely versatile, making it a key component of the neurosurgeon’s armamentarium. The pterional craniotomy, as well as its variations such as the orbitozygomatic approach, is the craniotomy of choice for many procedures, including those accessing supratentorial aneurysms, pathologies of the anterior and middle cranial fossae, the parasellar region, and to a certain extent, the central skull base and upper posterior cranial fossa with the anterior petrosal approach.
The patient is placed supine on the operating table ( Fig. 24.2A ). The table is reflexed to minimize downward shifting of the patient as the tilt is adjusted. The patient’s legs are elevated and placed in compression devices to minimize venous pooling. Placing the patient in the reverse Trendelenburg position promotes brain relaxation and increases venous return. We prefer to use a shoulder roll or a wedge under the ipsilateral shoulder along the long axis of the patient to assist with head rotation (see Fig. 24.2B ). It is important to minimize the amount of torque on the neck, especially in older adult patients, in whom the vertebral artery and the cervical rootlets can be at risk for tension.
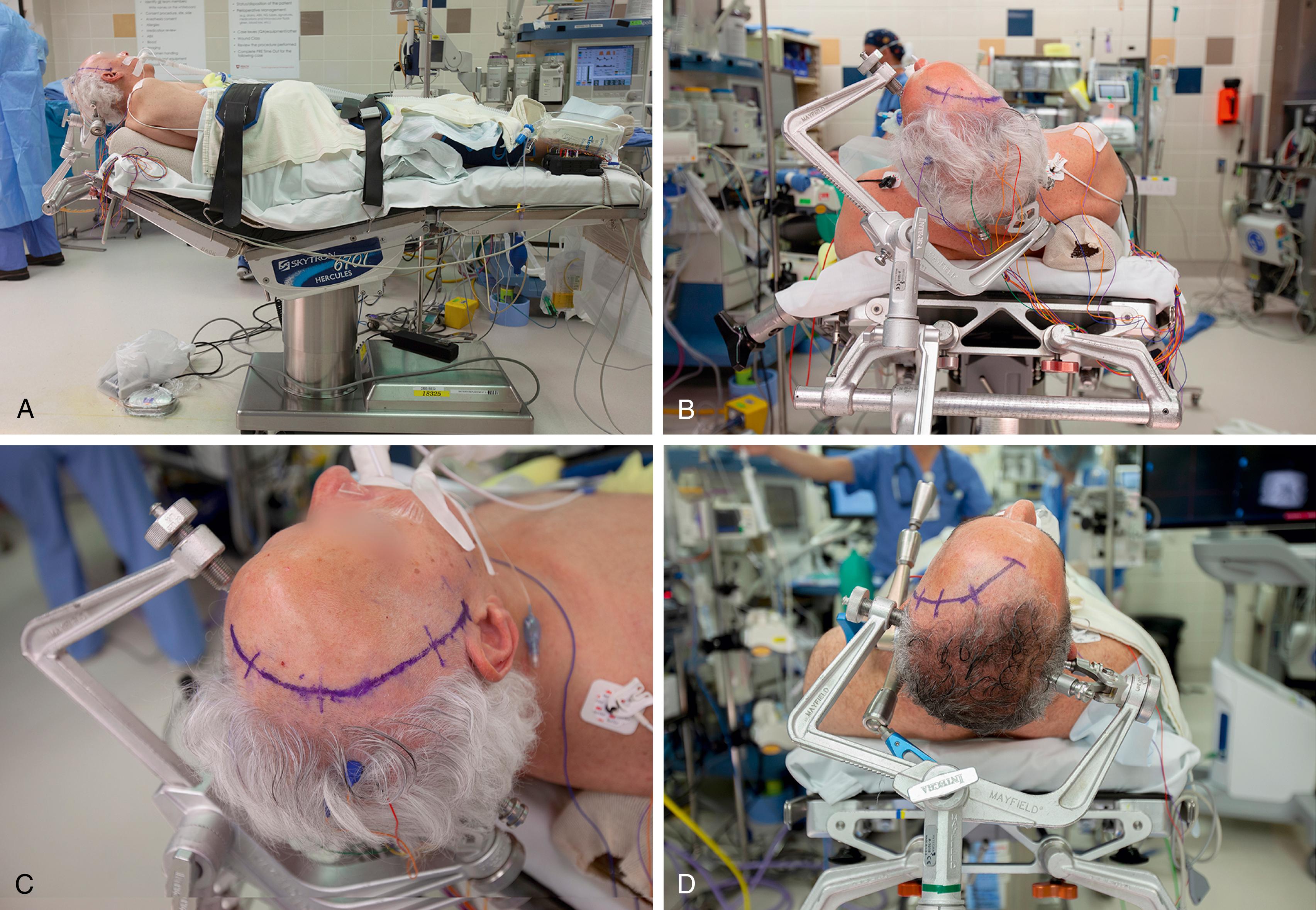
The patient’s head is secured in the Mayfield cranial fixation apparatus or a similar device (see Fig. 24.2C–D ). We prefer to place the pins in a biparietal location, usually with the twin pins opposite the side of surgery (see Fig. 24.2D ). To avoid an epidural hematoma from a temporal bone fracture, the pins should not be placed in the area of the temporalis muscle. , Alternatively, the single pin can be placed in the frontal bone contralateral to the operative target, above the brow to avoid the frontal sinus and ideally behind the hairline to minimize potential cosmetic scarring from the pin site (see Fig. 24.2C ). If a frontal pin is placed, the dual pins are positioned in the occipital bone on the ipsilateral side to the operative target above the attachment of neck musculature. It is important to place the pins inferior to the “equator” of the axial plane to avoid the disastrous complication of the head falling from pins that are placed above the “equator.”
After pinning, the patient’s head is placed into the optimal position. This requires a combination of flexion, rotation, and neck extension maneuvers, the goal of which is to provide the ideal surgical trajectory while minimizing brain retraction. First, the head is rotated to the contralateral side, with the degree of rotation being affected by location of the surgical target. Internal carotid artery disease is often approached fairly vertically, requiring about 5 to 30 degrees of contralateral rotation, whereas anterior communicating artery aneurysms require up to 50 to 60 degrees of rotation to visualize the circle of Willis complex. For pathologies requiring wide opening of the sylvian fissure, such as middle cerebral artery aneurysms, head rotation is minimized to avoid obstruction of the surgical corridor by the temporal bone. Once the desired degree of rotation is obtained, the head is laterally flexed slightly and the neck extended. This should bring the malar eminence to the highest point, allowing gravity to pull the frontal lobe away from the skull base and aid with visualization. More extension is used in approaching subfrontal targets, such as anterior communicating aneurysms, and less with skull base targets along the sphenoid ridge, cavernous sinus, or middle cranial fossa.
Once the optimal positioning is achieved, the head fixation device is secured to the table. The patient’s arm that is closest to the scrub nurse or the technician is padded, while the contralateral arm is rested on an arm board abducted to less than 90 degrees to aid with unobstructed access for the anesthesiologists. Pillows and padding are used under the knees and feet, and the patient is secured to the bed with a padded safety belt or tape (see Fig. 24.2A ).
Temporal, subtemporal, or middle fossa craniotomies may be performed alone (e.g., accessing disease at the petrous apex, basilar tip aneurysms, lesions in the middle fossa, and internal auditory canal) or in conjunction with the pterional or retrosigmoid approaches for more complex cranial disease.
We prefer to perform the subtemporal craniotomy with the patient in the supine position, with a large shoulder roll to facilitate a full 90 degrees of head rotation. In older adult patients, or if the patient’s neck flexibility does not allow for this, we perform this approach in the lateral position. The lateral position is also indicated if concurrent placement of a lumbar needle or drain is desired, as for a subtemporal approach to a basilar apex aneurysm.
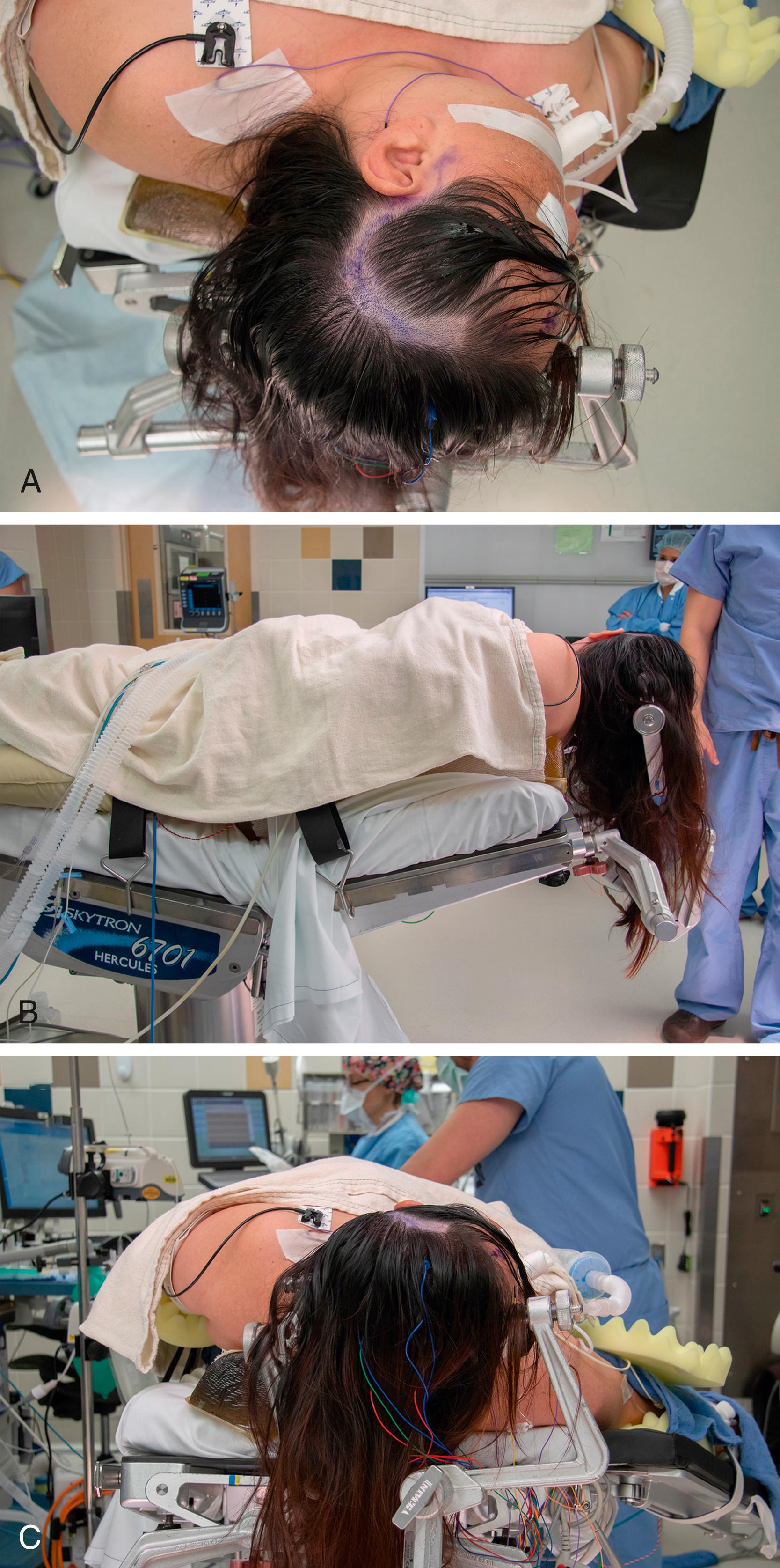
The patient’s head is secured in a Mayfield head fixation apparatus with the single pin in the frontal bone above the ipsilateral brow and the dual pins at the midline in the occipital bone ( Fig. 24.3A ). The bed is placed in the reflex position to facilitate stability and to elevate the knees to prevent venous pooling (see Fig. 24.3B ). The head is rotated so the sagittal sinus is parallel and the middle cranial fossa is perpendicular to the floor and then secured to the bed. The patient is placed in the reverse Trendelenburg position, and the neck is flexed laterally to allow gravity to facilitate gentle retraction of the temporal lobe. Finally, the patient is secured to the bed with belts and tape ( Fig. 24.3B–C ).
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here