Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Preservation of the structure and function of the growth plate, or physis, is essential for normal growth. Physes are composed of cartilage. They may be weaker than surrounding bone and ligaments and therefore are prone to injuries in tension or shear. Different physes respond differently to injury, and each must be approached as a distinct entity; careful attention should be paid to the child’s age, the growth potential of the affected area, the location, and the type of injury. Long-term complications of physeal injuries include growth arrest and progressive angular deformities, and these are often best managed with early recognition.
The physis is the primary center for skeletal growth of long bones and should be distinguished from the epiphysis, or secondary ossification center. Physes have been described as either pressure (compression) or traction (tensile) responsive; the latter are also referred to as apophyses. Primary physes are initially discoid areas of rapidly maturing cartilage, but with increasing biomechanical stress, especially shear stress, they undergo changes in contour known as undulations. Planar physes contribute primarily to longitudinal growth, and spherical physes contribute almost exclusively to circumferential expansion of bone. The physes also differ in morphology according to their skeletal location. The rapidly growing distal femoral physis, for example, has elongated cell columns, in contrast to the shortened cell column formation in the slowly growing phalangeal physis.
Cartilage cells grow continually toward the side of the physis facing the epiphysis of a long bone, whereas on the metaphyseal side, cartilage is continually replaced by bone. When growth is complete, the physes are resorbed and replaced by primary spongiosa (bone) that fuses the epiphysis permanently to the metaphysis. In males, most physes are closed at about 18 years of age, although the medial clavicle physis may not close until age 25 years; in females, growth in the length of the bones ceases about 2 years earlier.
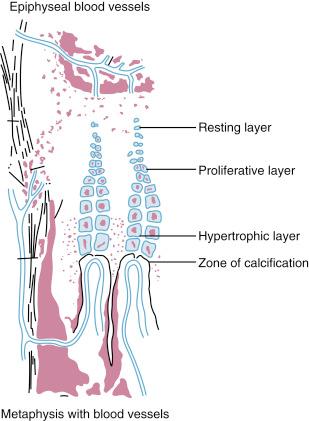
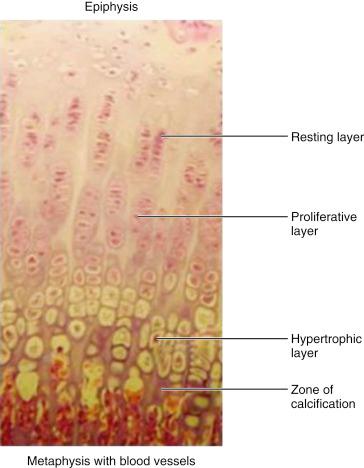
The physis can be divided into zones according to its function ( Fig. 2.1 ). In the resting and proliferative layers, the cells are relatively small and surrounded by a mechanically strong, thick layer of matrix. It is in the resting layer that germinal cells of stem cell origin are found. They exist in an area of low oxygen tension and respond to circulating hormones. As the cells proliferate, they appear as thin disks and palisades. In the extracellular matrix, longitudinal orientation of the collagen fibers occurs. This is an area of high oxygen tension. With hypertrophy of the chondrocytes (to 5–10 times their original size), there is physically less space for the extracellular matrix and its strengthening effect. The hypertrophic zone is therefore the weakest layer of the physis under tension, shear, and bending stress, and it is the most common area for fractures. In the zone of provisional calcification, metaphyseal vascular invasion allows mineralization of the matrix to occur, and programmed cell death of the chondrocytes is initiated. With the vascular invasion come osteoblasts and osteoclasts, allowing the formation of the primary spongiosa and its subsequent remodeling to more mature secondary spongiosa that no longer contains remnants of the cartilaginous precursor.
The physis is connected to the epiphysis and metaphysis peripherally via the zone of Ranvier and the perichondral ring of LaCroix. The zone of Ranvier is a circumferential notch containing cells (i.e., osteoblasts, chondrocytes, and fibroblasts), fibers, and a bony lamina located at the periphery of the physis. It also contributes to latitudinal or appositional growth. The periosteal sleeve is firmly attached to each end of a bone at the zone of Ranvier and the perichondrium of the epiphysis, and is thought to be an anatomic restraint to rapid, uncontrolled longitudinal growth. The perichondral ring of LaCroix is a strong, fibrous structure that secures the epiphysis to the metaphysis.
There are three sources of blood supply to the physis: the epiphyseal, metaphyseal, and perichondral circulations. The epiphyseal vessels (arteries, veins, and capillary network) disperse throughout the chondroepiphysis, except for the avascular articular cartilage region, within cartilage channels, occasionally communicating with the metaphyseal circulation. The pattern of this vascular network may be of two types. In type A epiphyses, which are covered almost entirely by articular cartilage, the blood supply enters from the metaphyseal side of the physis and is therefore prone to injury during epiphyseal separation. The proximal femur and proximal radius are the only two type A epiphyses. In type B epiphyses, which are only partially covered by articular cartilage, the blood supply enters from the epiphyseal side of the physis and is therefore protected from injury during epiphyseal separation.
The metaphysis contributes to the strength of the physis by way of its trabeculae, although these are susceptible to compressive forces. When the epiphysis is mainly cartilaginous, it acts as a shock absorber. As the epiphysis ossifies, its shock-absorbing ability diminishes.
Physeal injuries have been reported to occur in approximately 30% of children’s long bone fractures. They are twice as common in boys as in girls, possibly because the physes are open for a longer period of time in boys, and boys participate in more risk-taking behavior and athletics. Most physeal injuries occur between the ages of 12 and 16 in boys and between the ages of 10 and 12 in girls. The most common physeal fractures involve the phalanges of the fingers, distal radius, and distal tibia. Distal physes tend to be injured more frequently than proximal physes. Injuries occur approximately equally on right and left limbs, and upper limbs tend to be more commonly injured than lower limbs.
The mechanism depends on the age of the child. The physis is relatively thick in infancy and childhood and is therefore more prone to injury secondary to shear or tensile forces. In older children and adolescents, a fracture–separation of the physis is more common and occurs as the result of a combination of shear and compressive forces. Intraarticular fractures may also be caused by transient or near dislocation of a joint secondary to a tensile or shear force. Compressive forces may be transmitted to the physis secondary to severe abduction or adduction, angular forces applied to a joint that normally only flexes and extends.
Repetitive microtrauma can also injure the physis, as seen in examples such as Little League elbow and gymnast wrist. Other mechanisms of injury include iatrogenic causes (e.g., insertion of hardware, medications, or irradiation), diseases including infections and neoplasms, vascular insults, and thermal injuries such as those caused by frostbite or lightning.
The most characteristic consequence of a physeal injury is the disruption or cessation of longitudinal bone growth. Complete growth arrest can result in significant limb length inequality with functional impairment. Partial growth arrest can lead to angular deformities. Other consequences of physeal injuries include nonunion (e.g., after a lateral humeral condylar fracture), malunion, and avascular necrosis.
The prognosis for future growth is dependent on the type and mechanism of injury and on the location of the injury within the physis ( Fig. 2.2 ). If the fracture is limited to the hypertrophic layer, healing is usually uncomplicated. If the fracture line involves the resting zone or affects multiple zones of the physis, growth disturbance is far more likely. Although the exact mechanism that leads to physeal bar formation is unclear, Gruber et al hypothesize that injury to the basement plate of the physis results in an inability of the physis to heal itself and thus to subsequent physeal bar formation. Also, physeal bar formation may occur when the layers of the physis are not realigned properly, leading to bony bar formation between the bone of the metaphysis and that of the epiphysis.
Neurovascular and ligamentous structures adjacent to the physis may be injured as a result of physeal fractures. Ligamentous injuries that result in physeal avulsion occur most often at the tibial spine, at the ulnar styloid, and in the phalanges. Combinations of physeal injury and ligamentous disruption are most common in the knee, such as tibial spine avulsion associated with anterior cruciate ligament avulsion.
Compartment syndrome is not commonly associated with physeal fractures but has been reported with proximal and distal tibial fractures. A displaced distal radius physeal injury can lead to acute carpal tunnel syndrome. Joint dislocation or an ipsilateral shaft fracture is seen most frequently with medial epicondylar fractures about the elbow, approximately half of which are associated with partial or complete elbow dislocation.
A number of classification systems have been described for physeal fractures, including those by Aitken, Li et al, Ogden, and Poland. The most widely used classification, however, is the Salter–Harris (SH) system described in 1963. It is based on the relationship of the fracture line to the layers of the physis, and it has prognostic value with respect to subsequent growth disturbance. Five types of fractures are described in the classification. The first four types are, in fact, combinations of those injuries described by Poland (types I to III) and Aitken (types I to III), and the last type was added by Salter and Harris.
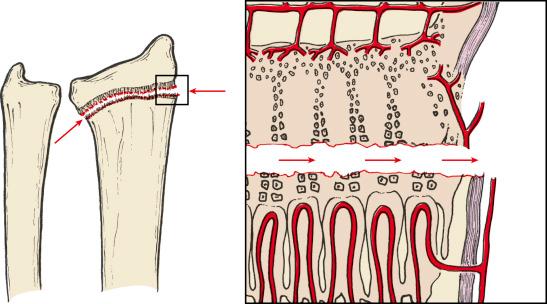
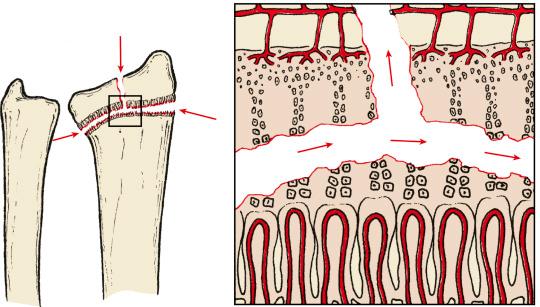
An SH type I (SH I) fracture occurs entirely through the zone of hypertrophic cells, but the surrounding bone is not fractured. This may result in complete separation of the epiphysis from the metaphysis ( Fig. 2.3 ). Because the resting layer remains with the epiphysis, growth is usually undisturbed unless there is damage to the epiphyseal blood supply (e.g., proximal femoral epiphyseal traumatic separation).
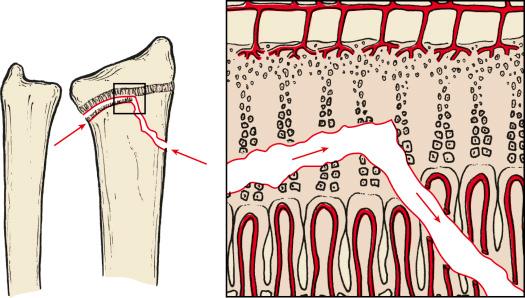
SH II injuries are similar to type I, except that the fracture line exits through the metaphysis on the compression side of the fracture (Thurston–Holland fragment) ( Fig. 2.4 ). The periosteum remains intact on the metaphyseal side of the fragment and provides stability once the fracture has been reduced. Again, growth disturbance is unusual because the resting layer is intact. This pattern is the most common type.
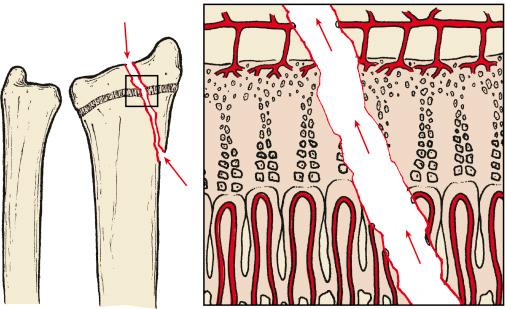
SH III fractures are intraarticular injuries with a fracture line running through the epiphysis and exiting through the physis ( Fig. 2.5 ). There is a high risk of growth arrest, and any displacement needs to be corrected.
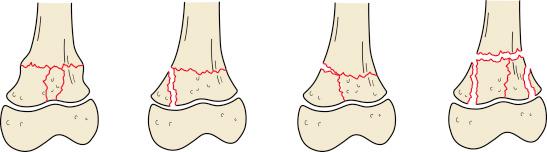
SH IV injuries involve a fracture through the metaphysis, physis, and epiphysis ( Fig. 2.6 ). Because the fracture line crosses the resting layer and enters the joint, anatomic reduction is necessary to prevent articular incongruity and osseous bridging across the physis. The risk of growth arrest is high.
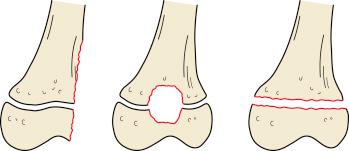
SH V fractures involve a compression or crushing injury to the physis. They are rare and cannot be immediately diagnosed because of the lack of radiographic signs. These fractures are recognized once a growth disturbance occurs.
Certain physeal injuries do not fit into the SH classification scheme. Rang described an injury to the perichondral ring of LaCroix, naming it a type VI physeal injury. This is most often seen in injuries about the medial malleolus caused by lawnmowers or after an individual has been dragged along the street by a motor vehicle. Peterson introduced a novel classification in 1994 based on a review of 951 fractures. Although there are similarities to the SH scheme, two previously undescribed injury types were added. In a Peterson type I fracture, seen commonly in the distal radius, a transverse fracture of the metaphysis occurs with longitudinal extension into the physis ( Fig. 2.7 ). In a Peterson type VI fracture, an open injury occurs, associated with loss of a portion of the physis. Peterson recommended emergent treatment in the form of débridement, often with wound packing, and secondary closure, occasionally with a skin graft or flap closure for this type of fracture. This fracture type may also require later reconstructive surgery as a result of premature physeal closure and bar formation on the exposed bone surface ( Fig. 2.8 ).
Most children with physeal injuries can recall a specific traumatic event and can localize their symptoms to a specific anatomic region. The most common symptoms are pain and localized tenderness; swelling and effusion are variable signs depending on the severity of the injury. Nontraumatic physeal injuries, such as infection, neoplasia, or congenital conditions, are usually evident from the history.
Orthogonal radiographs, most often anteroposterior and lateral, are usually sufficient to diagnose the physeal injury and plan treatment. Some physeal injuries may not be visible on standard views because of the irregular contour and chondro-osseous nature of the physis. Slight physeal widening may be the only sign of minimal displacement of an epiphyseal fragment. The Thurston–Holland metaphyseal fragment may sometimes be difficult to appreciate. Comparison radiographs of the contralateral extremity may be helpful for diagnosis, particularly for nondisplaced or minimally displaced SH type I and II fractures. Occasionally, stress views can help to demonstrate gapping between the epiphysis and metaphysis, particularly in injuries about uniplanar joints such as the knee, ankle, and elbow. However, alternatives such as magnetic resonance imaging (MRI) ( Fig. 2.9 ) or repeated radiographs 10 days after immobilization and protection can allow the diagnosis to be made without causing the patient discomfort.
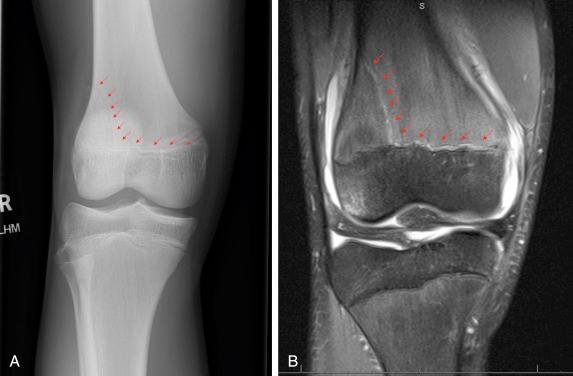
Imaging modalities that can be used for diagnosis include arthrography, MRI, ultrasound, and computed tomography (CT). Arthrography can be helpful in diagnosing fractures in areas where there is a large volume of cartilage, such as the distal humerus, although MRI and ultrasound are increasingly being used to evaluate such injuries. MRI is particularly useful in diagnosing occult fractures about the physis when plain radiography is negative. In a prospective study evaluating injuries to the elbow, distal femur, and distal tibia in children age 3 to 15 years with negative plain radiographs, MRI was able to detect a fracture in 34.8% of patients. Ultrasound may also be used to document soft tissue injury without fracture and has also been shown to be a safe and effective tool for evaluating SH I fractures with subperiosteal hematoma as well as other pathologies involving periosteal reaction, including infection and tumor. CT is helpful in complex fracture patterns, such as triplane ankle fractures. Furthermore, MRI and CT are particularly helpful in assessing the size and location of bony bars after growth arrest.
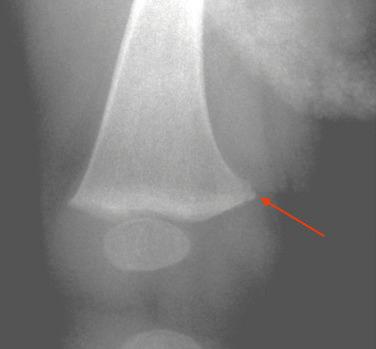
Nonaccidental injury may be suspected from the history and examination and, occasionally, on radiographs. The pathognomonic sign of a “corner fracture” of the metaphysis (also known as a bucket-handle fracture when seen “en face”) indicates the application of torsional or shear forces (such as severe twisting or wrenching) to a limb ( Fig. 2.10 ). Note that although this finding may indicate nonaccidental trauma, it may also be a normal finding in some. Nonaccidental trauma is discussed in more detail in Chapter 20 .
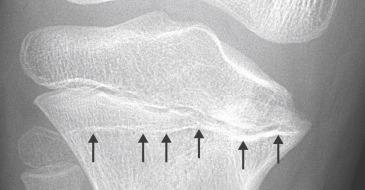
Previous injury to the physis may be evident by the presence of Harris growth arrest lines, which are transverse striations in the metaphysis thought to represent a period of slowing or cessation of growth. These lines may be present in either a single long bone after an isolated traumatic injury, or all long bones after a significant systemic illness. If the Harris growth arrest lines run parallel to the physis and continue to move away from the physis with time, the physis can be assumed to be growing normally after the injury. If they are asymmetric or oblique moving toward the physis, partial growth arrest is likely to have occurred ( Fig. 2.11 ). No growth arrest lines are seen after complete physeal arrest.
As with all patients with fractures, a child must be fully assessed with use of the basic ABCs (airway, breathing, and circulation) of trauma management, and all life- and limb-threatening injuries should be identified and treated. The goal of treating any physeal fracture is to obtain and maintain an acceptable reduction by closed or open means without causing any further injury to the resting cell layer of the physis. The specific treatment of physeal injuries is dictated by several factors, such as the severity of the injury, the anatomic location, the degree of residual deformity, the amount of time elapsed from the injury, and the age of the child.
Neurovascular and open injuries can coexist with physeal fractures and must be managed first on an emergent basis before attention is turned to the physeal injury. With respect to anatomic location, the capacity for remodeling is dependent on the location of the injury within a respective long bone. For example, the proximal humeral physis contributes 80% of the longitudinal growth of the humerus and therefore has great remodeling potential.
There is no exact degree of deformity that can be defined as acceptable in children’s fractures. In general, more valgus deformity can be tolerated than varus deformity, and more flexion deformity can be tolerated than extension deformity. In the lower extremity, more deformity can be tolerated proximally than distally. Angular deformities correct to the greatest extent when they are in the plane of motion of a nearby hinge joint, whereas angulation in other directions may persist to some extent. Rotational deformities do not tend to remodel.
The following numbers are approximate but worth remembering as a general guide when treating skeletal injuries in children. Most children’s fractures heal twice as fast as adult fractures, and most epiphyseal separations heal in half the time of a child’s long bone fracture. For example, in the tibia, an adult fracture may need 12 to 18 weeks to heal, a child’s fracture may only need 6 to 9 weeks, and a pure epiphyseal separation (SH I injury) heals in only 3 to 5 weeks.
The delay between injury and treatment is an important factor. Ideally, all reductions should be performed as soon after the injury as possible. If there is a delay, the decision to perform a reduction is dependent on the age of the child and the plane and severity of the deformity. The younger the patient, the more likely the correction will be through remodeling, particularly if the angulation is in the plane of motion of the adjacent joint. If the delay is more than 7 to 10 days in an SH I or II fracture, it is safer to perform an osteotomy later on to correct the deformity than to risk damaging the physis through a traumatic reduction of a healing physeal fracture. In intraarticular SH III and IV injuries with significant intraarticular displacement, anatomic reduction must be performed regardless of the amount of time elapsed from the injury.
With respect to age, the same injury that may lead to disabling sequelae in a young child, in whom injury to the physis has a longer time to negatively impact normal growth, may result in little disability in an adolescent nearing skeletal maturity. On the other hand, if a child has several years of growth remaining and the physis has not been damaged, the majority of deformities in the plane of motion of the joint will remodel.
Treatment of specific physeal injuries is discussed in the relevant chapters by anatomic location, but several general principles are worth considering. If displacement is minimal or absent, or if the diagnosis is in doubt, the extremity should be immobilized and the injury reexamined in 1 or 2 weeks for a periosteal reaction indicating an SH I fracture. When a physeal fracture is reduced, traction rather than forceful manipulation is preferred, and care should be taken not to “grate” the physis on metaphyseal or epiphyseal fragments. The rule of thumb of 90% traction and 10% translation is useful. Multiple attempts at reduction may cause further physeal damage. If the fracture cannot be reduced after a few attempts with the patient under local or regional anesthesia, closed reduction under general anesthesia is the next step. If significant deformity persists after closed reduction, especially in SH III and IV fractures, open reduction and internal fixation is indicated.
Some of the anatomic landmarks surrounding the physis should be taken into consideration. The periosteum in particular is of interest. It has been shown that the periosteum around the epiphysis may be resected or reflected for more accurate exposure and reduction, but care should be taken to ensure that the fragment is not completely denuded of its soft tissue attachments, through which it receives its blood supply. Bright recommended careful resection of about 1 cm of periosteum on either side of the physis to prevent bony bridge formation between the epiphysis and metaphysis; however, there is no definitive evidence to support this concept. The role of interposed periosteum in bony bridge formation is controversial. Although histologic studies in a rat model showed that in the presence of interposed periosteum the physis was able to repair itself, clinical studies have shown that interposition of periosteum may be associated with an increased incidence of growth arrest for fractures around the ankle.
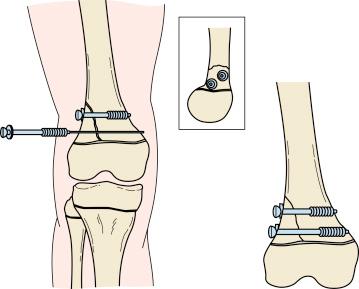
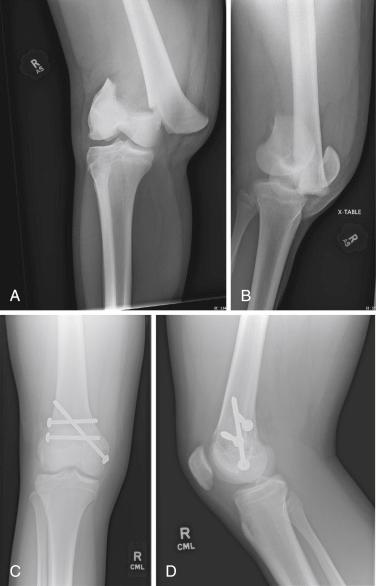
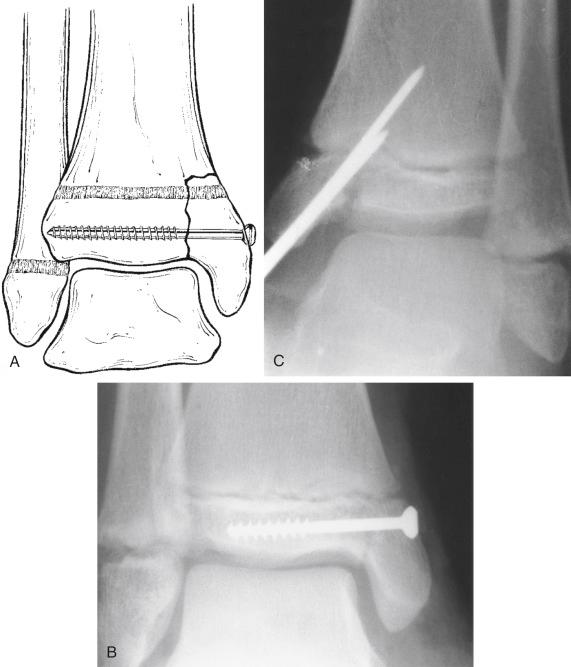
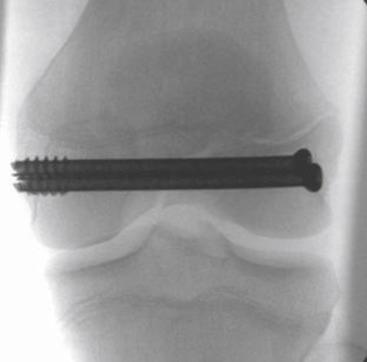
When a growth plate warrants fixation for adequate stability, ideally, the fixation should be inserted parallel to the physis in the epiphysis and metaphysis ( Fig. 2.12 ). However, at times, the need for stability will warrant transphyseal fixation ( Fig. 2.13 ). If the patient has growth remaining, transphyseal fixation should be performed with the use of smooth rather than threaded pins ( Fig. 2.14 ). Every physeal fracture should be closely monitored to ensure that there is no loss of reduction. SH I and II fractures do not tend to redisplace after the second week; however, SH III and IV fractures are unstable and may redisplace up to 3 weeks after the injury.
For every growth plate injury, adequate counseling is essential. The family should be informed of the possibility of complications, which can be as high as 40% after physeal fractures of the distal femur, with 85% to 100% of SH IV and V fractures experiencing complications. Follow-up should occur for at least 6 to 12 months after the injury to evaluate for growth arrest. During follow-up, Harris growth arrest lines should be examined closely to ensure that they remain parallel to the physis.
SH I fractures are generally treated by closed reduction and immobilization without internal fixation. Healing usually occurs within 3 to 4 weeks, and complications are rare. The same is generally true of SH II injuries. The intact hinge of periosteum in SH II injuries usually aids reduction. Often, the reduction is stable because of the presence of the metaphyseal fragment and its associated intact periosteum. If reduction is unstable, the orthopedist may use pins or screws to fix the metaphyseal fragment to the metaphysis, avoiding the physis. When closed reduction is performed in the operating room, fixation is generally used to prevent loss of reduction. In distal femoral physeal fractures, fixation should always be used for any fracture requiring reduction. Thomson et al demonstrated that 43% of distal femoral physeal fractures treated without internal fixation displaced, whereas no fractures with internal fixation displaced. If the metaphyseal fragment is too small, smooth pins can be used across the physis. Growth arrest is more likely in SH II fractures with larger physeal fragments, with larger degrees of displacement, in irregular undulating physes such as the distal femur and proximal tibia, and after repeated attempts at reduction.
Anatomic reduction is essential for SH III injuries, and it is most often achieved by open reduction so that the articular surfaces can be visualized. Fixation may be achieved by fixing the epiphyseal fragment across the fracture site parallel to the physis within the epiphysis ( Fig. 2.15 ). There needs to be a high index of suspicion for an intraarticular injury in adolescents with an injury mechanism and pain because plain radiographs may show a large effusion, but the SH III fracture may be difficult to diagnose, with as many as 39% of these injuries being missed on initial plain imaging and the amount of displacement being greater than 3 versus 6 mm on further advanced imaging. In SH IV injuries, open reduction and internal fixation are again usually required for alignment of the physis and articular surface if there is any displacement. Fixation is best achieved from epiphysis to epiphysis or metaphysis to metaphysis, and long-term follow-up is needed because the growth arrest rate is very high. SH V injuries are rarely diagnosed immediately, and treatment is usually delayed until growth arrest is evident.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here