Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Whatever its underlying psychology, sexual function depends on two complex and delicate neurologic pathways: (1) a connection between the brain and the genitals and (2) a reflex loop between the genitals and spinal cord. Both involve the central nervous system (CNS), peripheral nervous system (PNS), and autonomic nervous system (ANS).
In the pathway between the brain and the genitals, the brain converts various stimuli, including sleep-related events, into neurologic impulses that are usually excitatory, although occasionally inhibitory. These impulses travel down the spinal cord, some descending all the way down to its sacral region (S2–4), where they exit through the sacral nerve roots to travel through the pudendal nerve . Upon exiting the spinal cord, they leave the CNS to join the PNS ( Fig. 16.1 ). Other impulses also travel through the sacral nerve roots but through the parasympathetic division of the ANS. Meanwhile, as if diverted to a parallel route, some impulses leave the spinal cord at its low thoracic and upper lumbar regions (T11-L2) to travel through the sympathetic division of the ANS.
Excitatory descending stimuli increase parasympathetic ANS activity, which reduces (relaxes) tone in the wall muscles of the genital arteries. As the relaxed arteries dilate, they allow increased blood flow. In men, increased blood flow inflates the penis and produces an erection. In women, it produces clitoral engorgement.
With continued excitatory stimulation, a complex series of predominantly sympathetic ANS-mediated events produce an orgasm. Afterward, normal muscle tone reduces blood flow. The resultant reduced vascular engorgement results in detumescence.
Although the sympathetic and parasympathetic components of the ANS are complementary, they depend on different neurotransmitters—acetylcholine in the parasympathetic and monoamines in the sympathetic. Moreover, the ANS components have different roles. An admittedly crude mnemonic describes the p arasympathetic and s ympathetic ANS roles in sexual response: “ p oint and s hoot.” (The mnemonic also reflects that current knowledge of sexual function rests primarily on male physiology, evaluation, and treatment.)
The other pathway—the genital-spinal cord reflex—is shorter and simpler. In it, erotic impulses from genital stimulation pass through the pudendal nerve to the spinal cord. Most impulses synapse in the sacral region of the spinal cord and return, via the ANS, to the genitals.
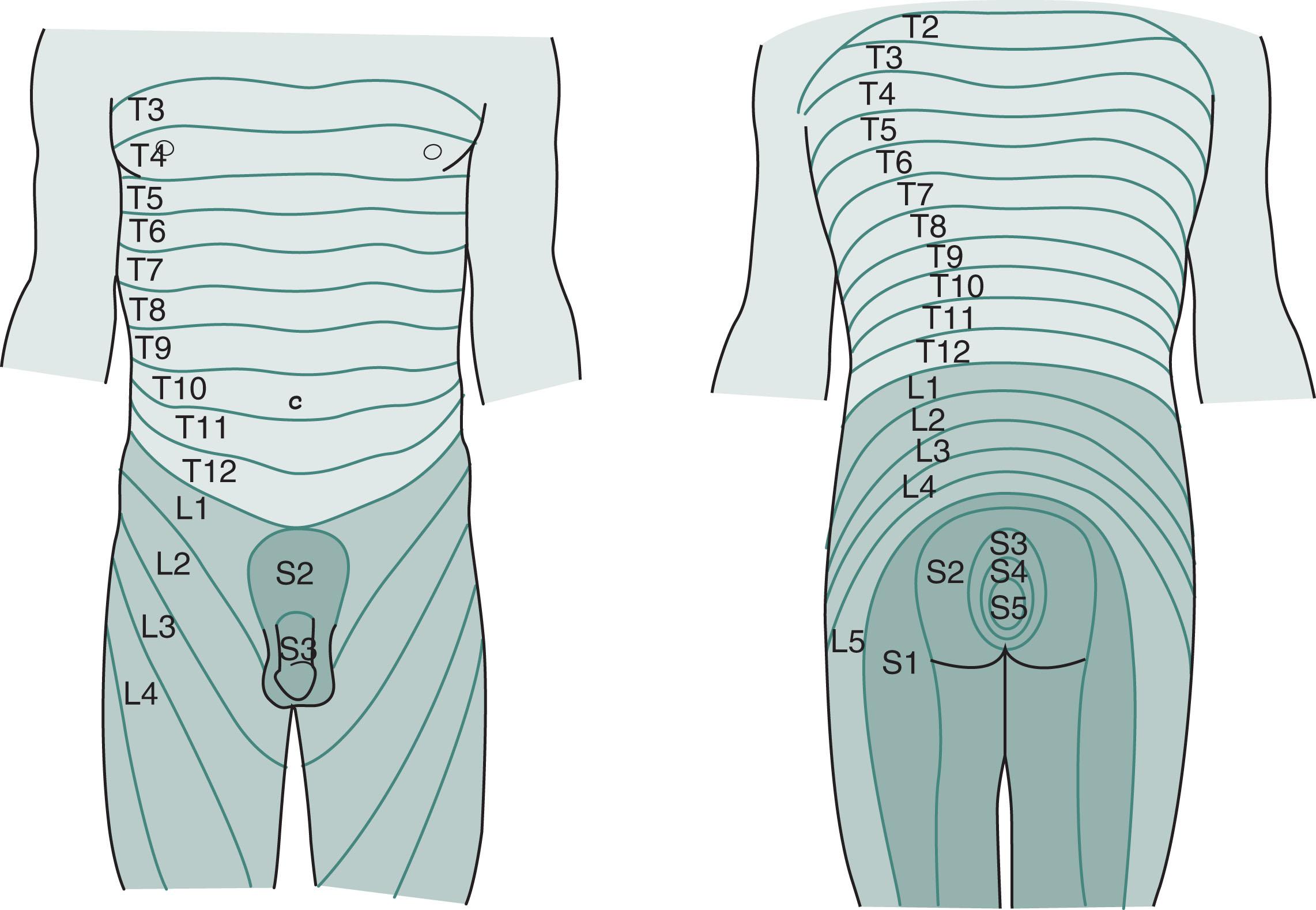
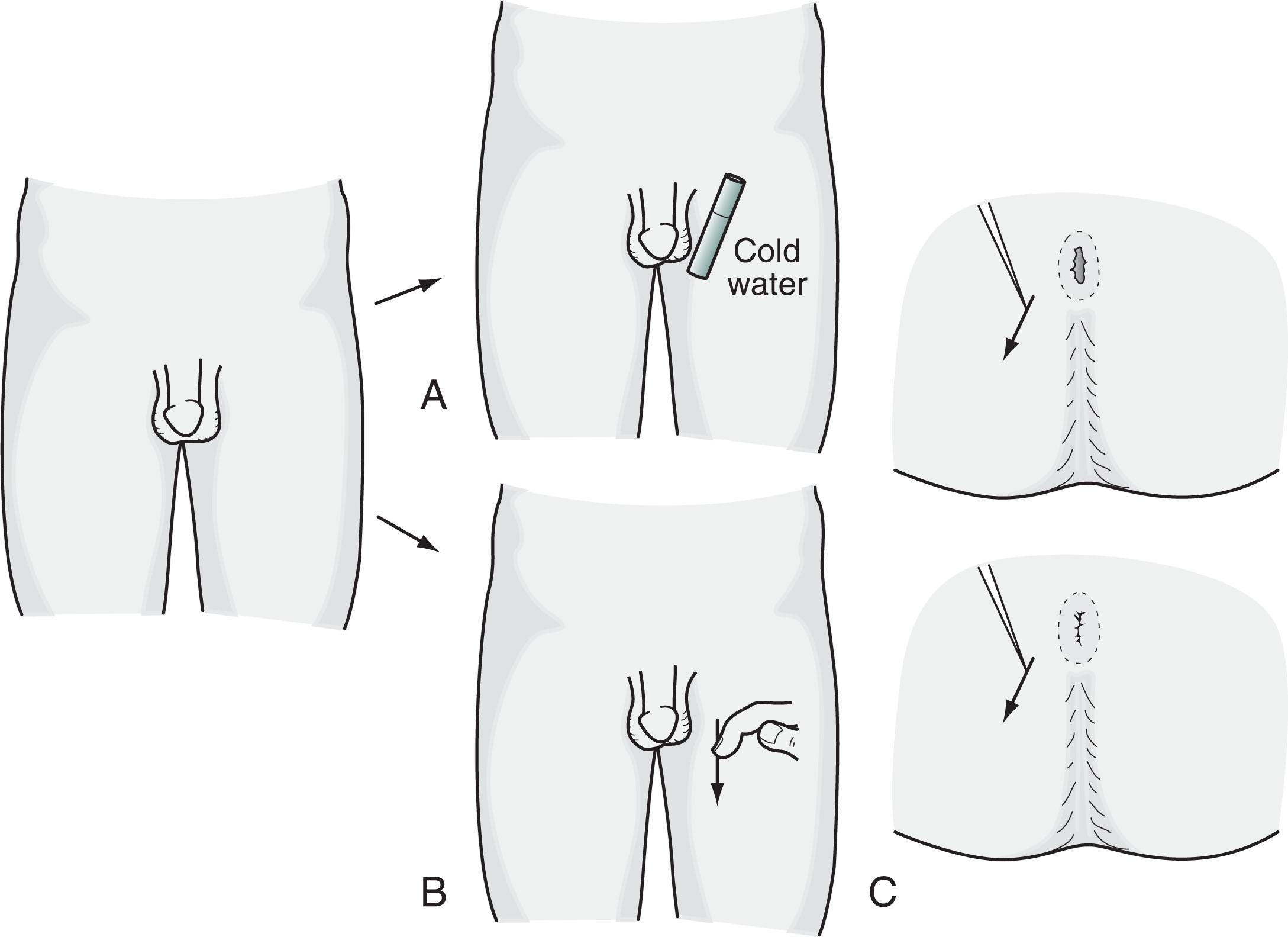
Without accepting a complete distinction between neurologic and psychologic sexual impairment, certain elements of the patient’s history ( Box 16.1 ) and neurologic examination ( Box 16.2 ) reliably indicate a neurologic origin. For example, either spinal cord or peripheral nerve injury might lead to a pattern of weakness and sensory loss below the waist or only around the genitals, anus, and buttocks—the “saddle area” ( Fig. 16.2 ). Plantar and deep tendon reflex (DTR) testing will indicate which system is responsible: spinal cord injury causes hyperactive DTRs and Babinski signs, whereas peripheral nerve injury causes hypoactive DTRs and no Babinski signs. Both CNS and PNS impairment lead to loss of the relevant “superficial reflexes”: scrotal, cremasteric, and anal ( Fig. 16.3 ).
Continual erectile dysfunction
Absence of morning erections
No erection or orgasm during masturbation or sex with different partners
Related somatic complaints
Sensory loss in genitals, pelvis, or legs
Urinary incontinence
Certain neurologic conditions
Spinal cord injury
Diabetic neuropathy
Multiple sclerosis
Herniated intervertebral disk
Use of many medications
Signs of spinal cord injury
Paraparesis or quadriparesis
Leg spasticity
Urinary incontinence
Signs of autonomic nervous system injury
Orthostatic hypotension or lightheadedness
Anhidrosis in groin and legs
Urinary incontinence
Retrograde ejaculation
Signs of peripheral nervous system injury
Loss of sensation in the genitals, “saddle area,” and legs
Paresis and areflexia in legs
Scrotal, cremasteric, and anal reflex loss
Although often subtle, signs of ANS impairment, as might result from diabetes, medications, or idiopathic systemic conditions, carry considerable diagnostic weight. For example, orthostatic hypotension , usually defined as a fall of 20 mm Hg in systolic blood pressure upon standing, and lack of sweating (anhidrosis) indicate ANS impairment.
In many conditions, such as spinal cord injury or severe ANS damage, urinary and fecal incontinence accompany neurologic-induced sexual impairment because the bladder, bowel, and genitals share many elements of innervation. The anus, like the bladder, has two sphincters (see Fig. 15.5 ). Its internal sphincter, more powerful than the external one, constricts in response to increased sympathetic activity and relaxes to parasympathetic activity. The external sphincter of the anus is under voluntary control through the pudendal nerves and other branches of the S3 and S4 nerve roots. Thus, to produce a bowel movement, individuals must deliberately relax their external sphincter while the internal sphincter, under involuntary parasympathetic control, simultaneously relaxes.
As could be anticipated, excess sympathetic ANS activity, as in the “fight and flight” response, inhibits both urinating and defecating by constricting the sphincters. Moreover, excess ANS activity, typically caused by anxiety, often impairs sexual arousal, inhibits an erection, and precipitates premature ejaculation.
From infancy to old age, normal men have erections and other signs of ANS activity during their rapid eye movement (REM) periods of sleep. Erections develop during REM sleep, regardless of dreams’ overt content. Thus, normal men have three to five erections per night, each lasting about 20 minutes. In a nocturnal penile tumescence (NPT) study, a device monitors a man’s erections and correlates them with REM periods over one to three nights.
Because NPT studies take place in a secluded setting, the testing frees men with erectile dysfunction from most social and psychological influences. During NPT studies, some men casually diagnosed as having erectile dysfunction actually develop erections. Those who develop no erections usually have a physiologic disturbance; however, some of them instead suffer from depression, a sleep disorder, or a test-induced artifact.
Depending on the circumstances—peripheral vascular disease, atherosclerosis, diabetes, or pelvic injuries—physicians may assess men with erectile dysfunction and other sexual impairments by measuring the blood pressure and blood flow in the dorsal artery of the penis using a small blood pressure cuff, Doppler ultrasound apparatus, and other devices. Barring vascular disease, an injection of a vasodilator into the penis (i.e., an intracorporeal vasodilator injection) produces an erection. In fact, such injections provide a treatment option.
If physicians suspect polyneuropathy, pudendal nerve damage, or spinal cord injury, neurologists may perform electrophysiologic studies, such as peripheral nerve conduction velocity, penile nerve conduction velocity, and somatosensory evoked potentials for women as well as men. These tests help in the diagnosis of patients with diabetic neuropathy, prostate cancer, pelvic or spine trauma, or multiple sclerosis (MS) (see later).
Individuals with an endocrinologic basis of their sexual dysfunction usually have other signs of hormone imbalance. Relevant screening tests usually measure blood glucose, prolactin, testosterone, estrogen, and gonadotropic hormone concentrations. Other tests may reveal hypogonadism, hypothyroidism, diabetes, or a disruption of the hypothalamic-pituitary-gonadal axis.
For psychiatric patients who have no systemic medical illness, the determination of serum prolactin and testosterone levels are important measures. These two hormones have a reciprocal relationship. Increased levels of prolactin, often induced by antipsychotic agents or tricyclic antidepressants, suppress testosterone levels, which lead to sexual dysfunction. Similarly, dopamine precursors or agonists (Parkinson disease medicines), which increase dopamine activity, suppress prolactin levels, raise testosterone levels, and enhance sexuality.
Several medications can produce erections adequate for sexual intercourse despite neurologic injury or vascular insufficiency. In addition, they may help restore erections in men with psychogenic erectile dysfunction and in those taking psychotropic medication.
Physicians may prescribe yohimbine, a centrally acting α-2 adrenergic antagonist (see Chapter 21 ). This medicine may modestly increase sympathetic vasomotor activity and create an aphrodisiac effect. Although yohimbine may alleviate psychogenic erectile dysfunction, it often causes anxiety. Moreover, it does not help in cases of sexual function due to medical or neurologic illness.
Testosterone injections are popular mostly because they may increase muscle mass, especially in bodybuilders, and provide psychological stimulation. Testosterone injections increase libido but otherwise have no effect on sexual function. Moreover, in high doses for long periods, they may induce prostate cancer.
In contrast, intracorporeal injections of vasoactive medicines—although briefly painful—are effective. They induce erections in men with spinal cord damage, peripheral neuropathy, or vascular disease. The most effective medicines are papaverine, a nonspecific smooth muscle relaxant; phentolamine, an α-adrenergic antagonist; and alprostadil, a synthetic prostaglandin E1. A man with erectile dysfunction can inject these medicines—individually or as a mixture—into the base of his corpus cavernosum (the vascular erectile tissue of the penis) to induce a serviceable erection.
Phentolamine-induced erections illustrate an important physiologic distinction. In contrast to adrenergic antagonists , such as phentolamine, causing erections, adrenergic agonists , such as epinephrine (see later), soften erections—by respectively increasing or reducing blood flow into the penis.
Using an alternative treatment, men can insert an alprostadil suppository into the urethra. Although initially uncomfortable, it leads to an erection by greatly promoting blood flow into the penis. This method, unlike treatment with sildenafil (Viagra), does not require physical stimulation to achieve an erection and causes few side effects.
Sildenafil and related medicines—tadalafil (Cialis), vardenafil (Levitra), and avanafil (Stendra)—have simplified the treatment of erectile dysfunction and dispensed with expensive and lengthy testing. To a greater or lesser degree, they assist men with erectile dysfunction from age-related changes, diabetes, MS, spinal cord injury, and nerve damage from prostate surgery. Furthermore, they often correct erectile dysfunction associated with anxiety, decreased libido, depression, or other psychiatric disturbances. They also partially or completely reverse sexual dysfunction caused by psychotropic medications in both sexes (see later).
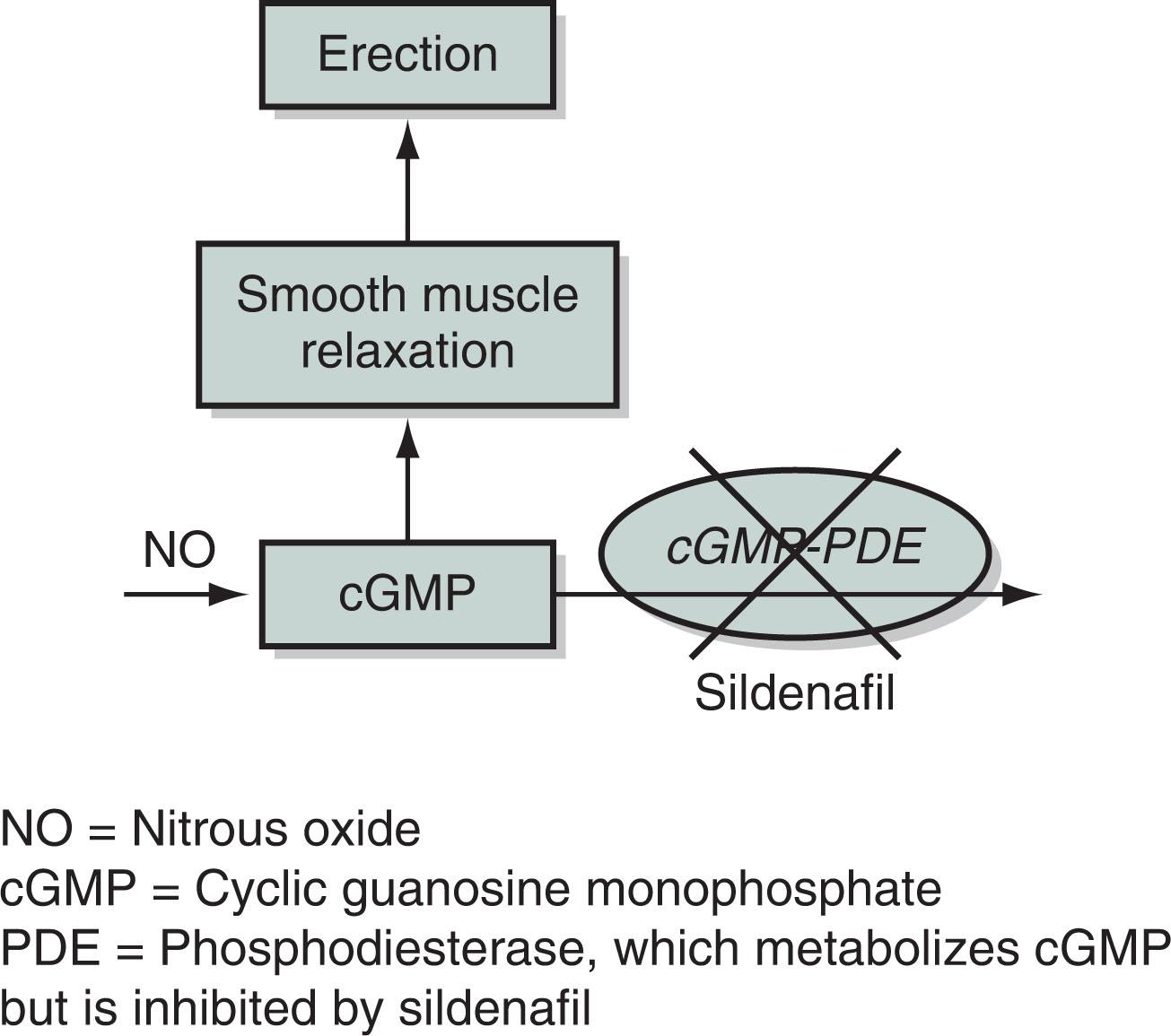
Sildenafil and related medicines have a well-established mechanism of action. Under normal circumstances, psychologic or tactile sexual stimulation provokes parasympathetic neurons to produce and release the neurotransmitter nitric oxide (NO) within the penis. NO, in turn, promotes the production of cyclic guanylate cyclase monophosphate (cGMP). Then cGMP dilates the arteries that promote blood flow and creates an erection. When the enzyme cGMP-phosphodiesterase metabolizes cGMP, the erection subsides.
As their primary mechanism of action, these medicines— phosphodiesterase inhibitors —inhibit cGMP-phosphodiesterase and thus preserve cGMP. The resulting cGMP concentration promotes blood flow in the penis ( Fig. 16.4 ).
Hardly a panacea, phosphodiesterase inhibitors help only about 60% of men with erectile dysfunction. They are often ineffective in men older than 70 years, with diabetes (especially when it is uncontrolled), undergoing cancer chemotherapy, or who smoke. In addition, men taking nitroglycerin, other nitrates, doxazosin, or most α 1 -adrenergic antagonists should not also take phosphodiesterase inhibitors because excess vasodilation may lead to orthostatic hypotension. Phosphodiesterase inhibitors routinely cause headaches and mild visual disturbances.
Invasive treatments are rarely satisfactory. Delicate and tedious arterial reconstructive procedures are usually disappointing except in men with localized vascular injuries. Surgically implanted devices, such as rigid or semirigid silicone rods or a balloon-like apparatus, can mimic an erection. Silicone penile implants are costly, unaesthetic, and prone to infections and mechanical failures.
Curiously, although NO and cGMP mediate clitoral blood flow and engorgement in women, the use of phosphodiesterase inhibitors in women has not shown success for female sexual dysfunction. Flibanserin (Addyi), a multifunctional agonist at some serotonin receptors and antagonist at others, was approved in 2015 for the treatment of hypoactive sexual desire disorder (HSDD) in women. Of note, the DSM-5 now classifies HSDD as part of Female Sexual Interest/Arousal Disorder .
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here