Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Multiple sclerosis (MS) is the most common disabling neurologic illness of North American and European young and middle-aged adults. It is also the primary example of a central nervous system (CNS) autoimmune demyelinating illness.
Neurologists base their diagnosis on the McDonald criteria , which were first published in 2011 and modified most recently in 2017 and named for the senior member of an international panel, Dr. W. Ian McDonald. The diagnosis of MS based on the McDonald criteria rests upon patients’ sustaining attacks of CNS dysfunction and having certain magnetic resonance imaging (MRI) findings. Medications may modify, although not reverse, the illness.
Although the manifestations of MS are mostly physical deficits, many patients have loss of cognitive capacity, depression, and medication-induced neuropsychiatric problems. In addition, MS greatly stresses the patient’s caregiver.
MS—usually a chronic recurring illness—typically begins with 1-mm to 3-cm patches of inflammation developing in the myelin sheaths of CNS axons. T cell-mediated inflammation strips myelin from (demyelinates) axons and eventually leaves sclerotic (Greek sklerosis , hard) plaques scattered throughout the CNS. The histologic and MRI signature of MS is plaques disseminated throughout the myelin or “white matter” of the cerebrum, cerebellum, spinal cord, brainstem, and optic nerves.
When denuded of their myelin insulation, axons transmit nerve impulses slowly or not at all. Some deficits resolve as myelin inflammation spontaneously subsides or anti-inflammatory medications, such as steroids, suppress it, after which Schwann cells are able to remyelinate affected axons. As plaques recur, develop in new areas, and accumulate, MS evolves from an acute inflammatory to a chronic degenerative condition. Sooner or later, the plaques leave permanent neurologic deficits.
Although MS acts primarily as a CNS demyelinating disorder, its pathology includes prominent axon degeneration. In contrast to demyelination associated with plaques, axon degeneration regularly produces permanent mental and physical disabilities.
The mean age at onset of MS is 33 years, with 70% of cases developing between 21 and 40 years. Some studies have reported many patients who suffer their first or a subsequent MS attack after a medical insult, such as infection, childbirth, head or spine trauma, intervertebral disk surgery, or electrical injury. Other studies have reported psychologic stress preceding the first or subsequent attacks. However, most carefully controlled prospective studies have found these factors do not play a major role in either causing or exacerbating MS.
A cause remains unknown, but in view of the protean symptoms, different courses, and variable responses to treatment, there may be many causes. Studies have found that genetic susceptibility and environmental factors—or, more likely, their interaction—allow MS to develop. Epidemiologic studies show the power of genetic risk factors. For example, compared to its incidence in the general population, MS occurs 20 to 40 times more frequently in first-degree relatives of MS patients. MS occurs at a rate of 5% in a dizygotic twin and of 25% in the monozygotic twin of an MS patient. Still, the concordance rates in twins, while striking, are far smaller than if the illness resulted from conventional genetic inheritance. Moreover, affected twins often display different symptomatology and follow different disease courses. Also, studies have linked several chromosome mutations to the development of MS but none seems to be necessary or sufficient.
Although genetic factors clearly confer susceptibility, they do not constitute the entire explanation. MS occurs three to four times as frequently in women than men. Environmental factors present during childhood years are also risk factors. In general, because the prevalence of MS increases with the distance from the equator, there is a high incidence of MS among people born and raised in cool climates. The incidence of MS is higher in individuals born and raised in Boston than New Orleans and higher in Scandinavian countries than in Italy and Spain. As the inverse pattern naturally applies in the Southern Hemisphere, the incidence is relatively high in Australia's cool, southern regions. As a corollary, the incidence is relatively low in the tropical areas of Asia, Latin America, and sub-Saharan Africa.
Studies have found that lack of sun exposure in late childhood, little ultraviolet exposure, and vitamin D deficiency are risk factors for developing MS. With these factors’ close relationship to each other and to the northern latitudes, they partly account the influence of geography. Other risk factors include Epstein-Barr virus infection, obesity, and exposure to tobacco smoke.
The initial episode of MS may range from a single trivial impairment lasting several days to a group of debilitating deficits that remain for several weeks and never fully recede. Subsequent episodes vary considerably in their manifestations, severity, and permanence. Relapse rates are highly variable among individuals, but most untreated patients will have a clinical relapse approximately every 1 to 2 years. During exacerbations, the initial symptoms, accompanied by additional ones, generally reappear.
MS patients tend to follow one of four reasonably distinct courses characterized by either a single attack (clinically isolated syndrome) , multiple attacks followed by partial or complete recovery (relapsing-remitting MS) , several attacks followed by steady deterioration (secondary progressive MS) , or unremitting, steady deterioration from the onset (primary progressive MS) . These categories reflect patients’ clinical status as a function of time unrelated to the severity of attacks. About 85% of cases follow a relapsing-remitting course. In addition to being descriptive, these patterns imply a patient's prognosis and likely response to immunomodulating treatments.
Lesions in the white matter tracts of the CNS cause various symptoms during a patient's illness ( Fig. 15.1 ). Moreover, simultaneous involvement of two separate CNS areas often produces combinations of disparate symptoms. For example, plaques may simultaneously develop in the cerebellum and thoracic spinal cord, which would cause ataxia and spastic paraparesis. The three most frequent presentations of MS are ataxia (from cerebellar involvement), visual impairments (optic neuritis and internuclear ophthalmoplegia), and spastic paraparesis (spinal cord inflammation [i.e., transverse myelitis]).
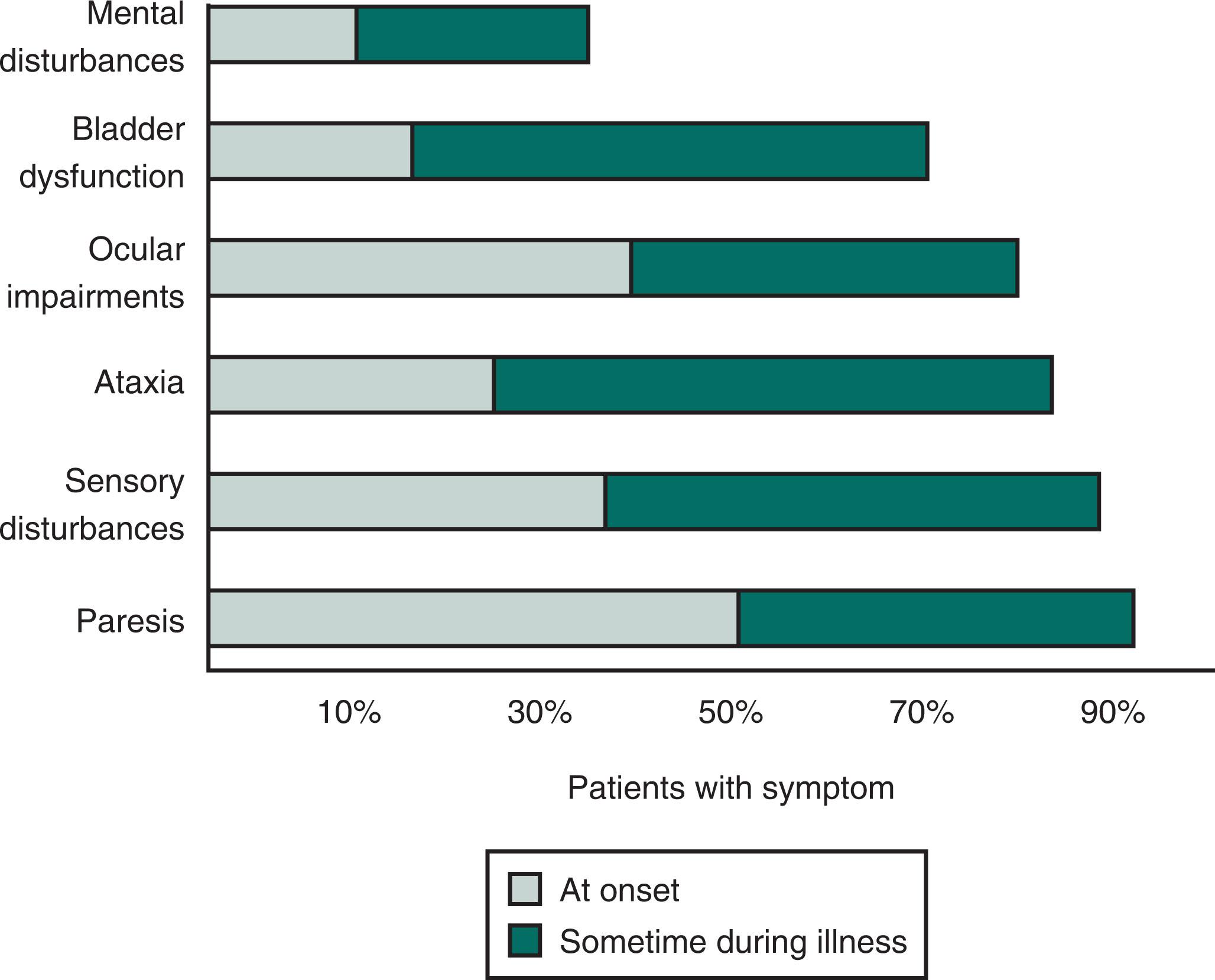
As some of their earliest and recurrent manifestations, MS patients typically develop gait ataxia (see Fig. 2.13 ), intention tremor (see Fig. 2.11 ), dysdiadochokinesia, scanning speech, and sometimes a head tremor (titubation) . Of those impairments, the gait ataxia is the most debilitating because it forces patients into wheelchairs or confines them to bed.
Both lack of sensation and abnormal sensations occur frequently and prominently. MS patients often describe hypesthesia, paresthesias, or dysesthesias in their limbs or trunk or below a particular spinal cord level. Neurologists consider spontaneous painful sensations as neuropathic pain (see Chapter 14 ). Sensory symptoms, at their onset, may not conform to expected neurologic patterns or be unaccompanied by objective findings. Physicians may understandably misinterpret atypical sensory symptoms as a psychogenic disturbance.
Impaired visual acuity and disordered ocular motility are reliable signs of MS. In fact, their absence in patients believed to have MS prompts neurologists to reconsider that diagnosis (see later).
The optic nerve is involved in MS because its covering consists of CNS myelin. (Oligodendrocytes produce CNS myelin, but Schwann cells produce peripheral nervous system [PNS] myelin.) The auditory nerve (cranial nerve VIII) is only partially covered by CNS myelin and is rarely involved in MS.
Neurologists usually attribute visual acuity impairment in MS to inflammation in the optic nerve (optic neuritis) . When inflammation is restricted to the portion of the nerve behind the optic disk, neurologists apply the more specific term, retrobulbar neuritis (see Fig. 12.5 ). Optic neuritis typically causes an irregular area of visual loss in one eye, a scotoma , which classically includes the center of vision ( Fig. 15.2 ). Optic neuritis also leads to color desaturation , in which colors—especially red—lose their intensity.
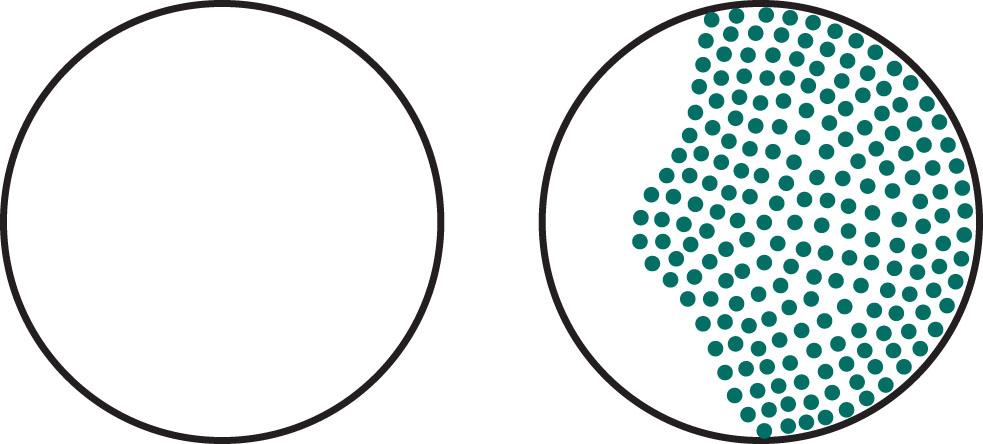
In addition to reducing vision, optic neuritis characteristically causes pain in the affected eye, probably because ocular movement puts traction on an inflamed optic nerve, eye pain increases when patients look from side to side.
Optic neuritis, as well as other lesions of the optic nerve, causes a readily identifiable pupillary light reaction (see Fig. 4.2 ). In the “swinging flashing test,” shining a flashlight first into the normal eye and then into the eye with optic neuritis will lead to dilation, rather than continued constriction, of both pupils. This dilation results from less stimulation transmitted by the defective optic nerve compared to when light is shined into the normal eye. Because the abnormality lies in the afferent limb of the light reflex pathway, neurologists call this response a “relative afferent pupillary defect” or “Marcus Gunn pupil” and recognize it as a sign of optic neuritis or other optic nerve disease.
Unless the optic disk is swollen, routine ophthalmoscopic examination usually reveals no abnormality. This discrepancy between visual loss and the normal appearance of the disk has given rise to the saying, “The patient sees nothing and the physician sees nothing.” As an optic neuritis attack subsides, most vision returns and pain subsides. However, with repeated attacks, progressive visual loss ensues, and the disk becomes pale and atrophic. Optical coherence tomography—a new technique—can measure MS-induced damage to retinal nerve fibers.
Statistics vary on the relationship of optic neuritis to MS. They indicate approximately 25% of MS patients present with optic neuritis as their initial symptom and 50% of MS patients suffer an optic neuritis attack during their illness. A single attack of optic neuritis with no other neurologic symptoms and an MRI showing no brain lesions means the individual has only about a 25% likelihood of developing MS in the following 15 years; however, when one or more MRI lesions accompany optic neuritis, the individual's likelihood increases to about 70% during the same period.
Either brainstem or cerebellar MS lesions can cause nystagmus. Although it is clinically indistinguishable from nystagmus induced by other conditions (see Chapter 12 ), MS-induced nystagmus classically occurs in combination with dysarthria and tremor (Charcot's triad) . Whatever the underlying illness, nystagmus often causes images in the patient’s vision to move back and forth, creating the symptom of oscillopsia .
Another source of visual impairment in MS is the characteristic internuclear ophthalmoplegia (INO) , also known as the medial longitudinal fasciculus (MLF) syndrome . In MS-induced INO, a plaque in the MLF interrupts nerve impulse transmission from the pontine conjugate gaze centers to the oculomotor nuclei in the midbrain ( Figs. 12.11 , 15.3 , and 15.4 ). The primary symptom of INO is diplopia on lateral gaze, while looking to the side opposite the lesion, due to paresis of the adducting eye. In addition—due to nystagmus in the abducting eye—oscillopsia may also be present.
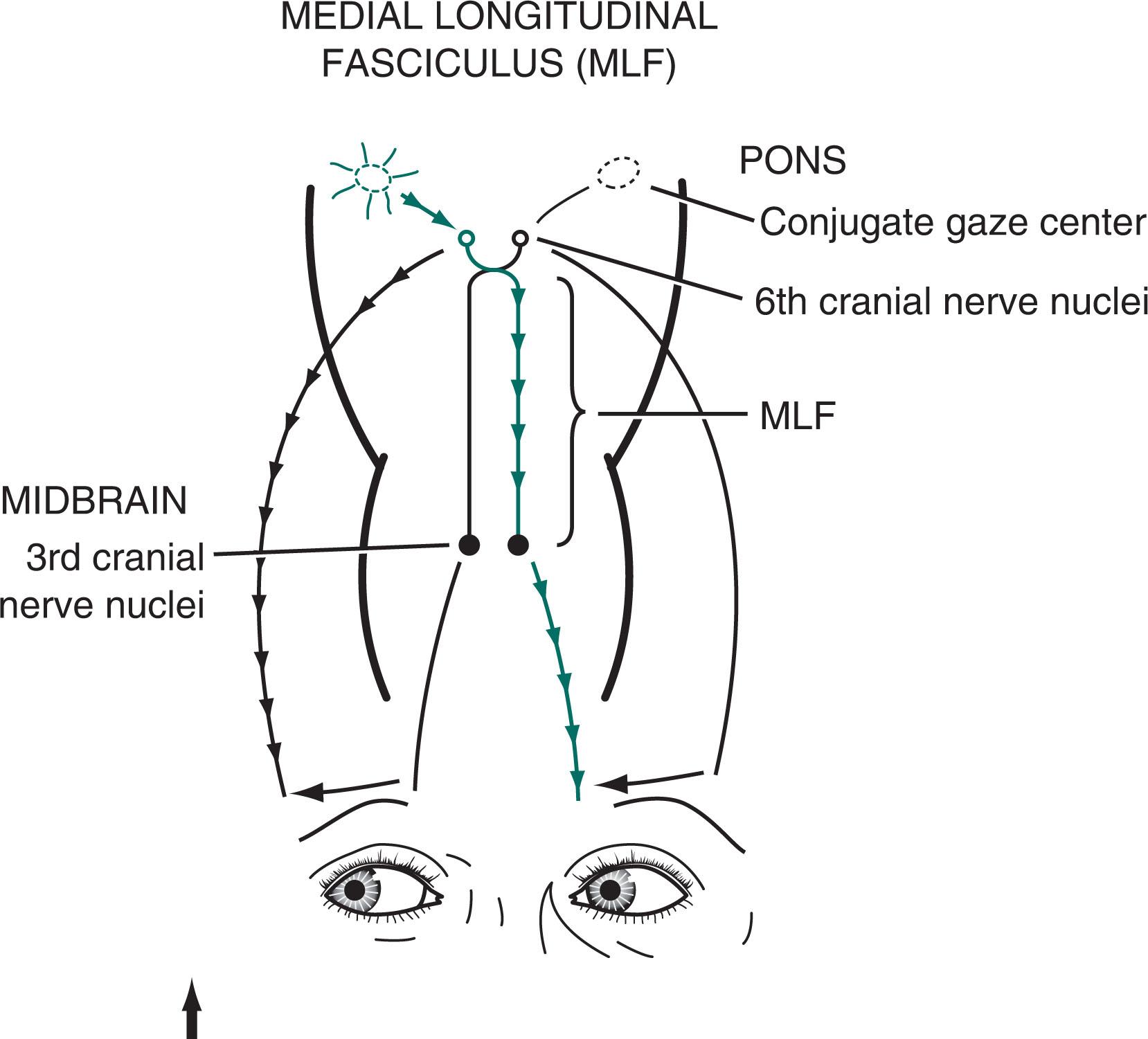
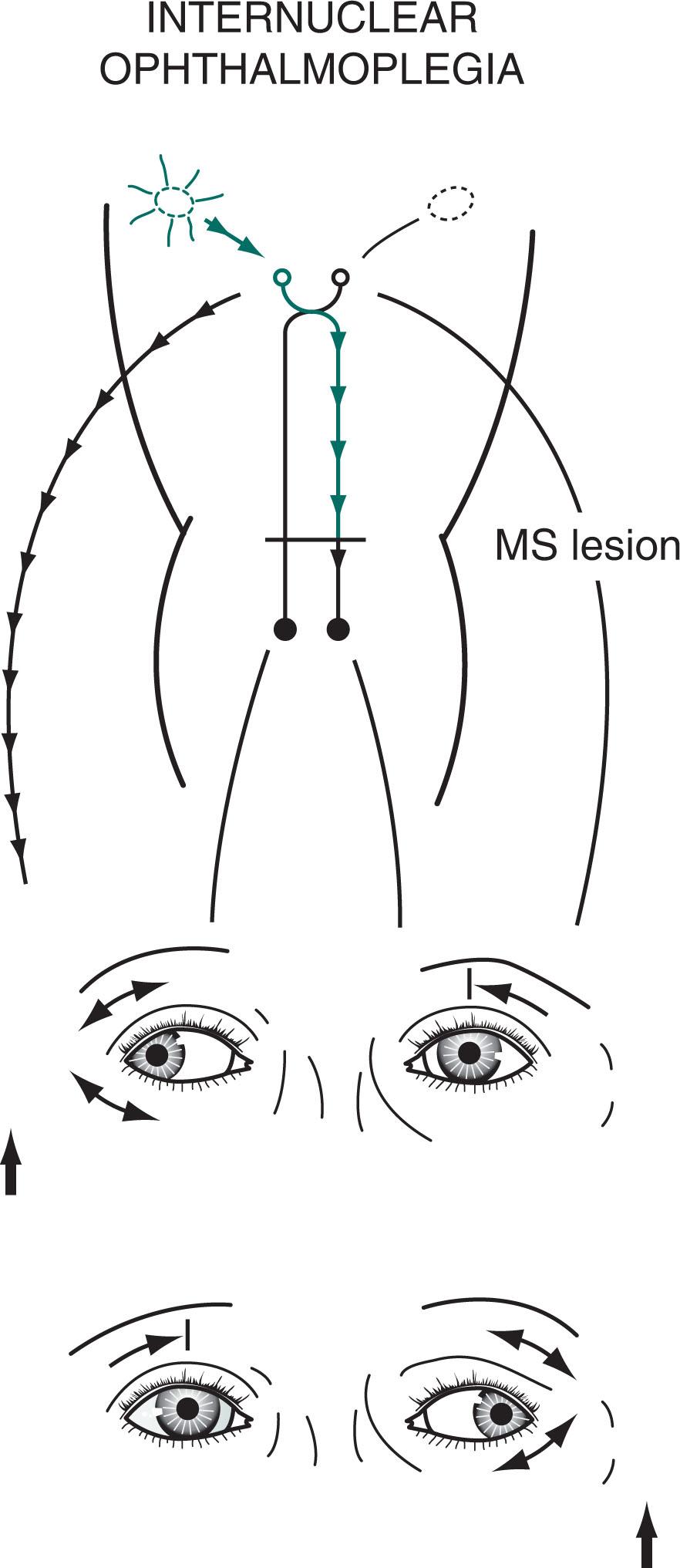
INO is a classic sign of MS; however, it may also be a sign of systemic lupus erythematosus (SLE) or a small basilar artery stroke. In addition, Wernicke–Korsakoff syndrome, myasthenia gravis, and botulism can produce patterns of ocular muscle weakness that mimic INO. From a physiologic viewpoint, INO is analogous to a disconnection syndrome, such as conduction aphasia, in which communicating links are severed, but each neurologic “center” remains intact (see Chapter 8 ).
MS that involves the spinal cord (myelitis) typically causes hyperactive deep tendon reflexes (DTRs) and Babinski signs. Even with mild paraparesis, spasticity impairs patients' gait and triggers painful leg muscle spasms. Patients with cervical myelitis also often have a Lhermitte's sign : when neurologists flex their neck, the movement triggers electrical sensations that radiate downward from their neck.
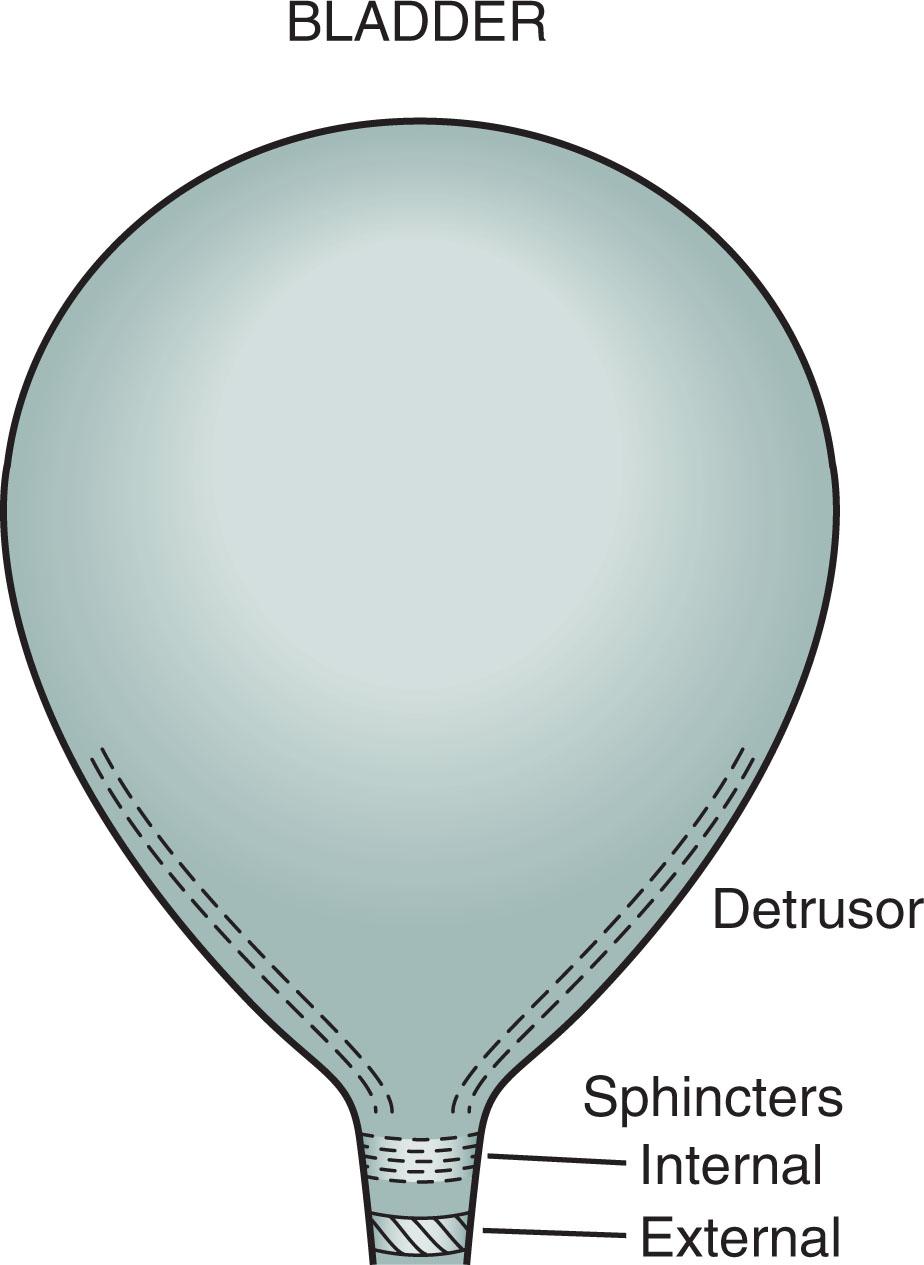
Spinal cord involvement also leads to urinary incontinence from bladder sphincter muscle spasticity, paresis, and incoordination (dyssynergia) ( Fig. 15.5 ). MS patients may initially have incontinence only during sleep and sexual intercourse. As the disease progresses, they develop intermittent urinary retention and often complete loss of control. They may require intermittent or continuous catheterization that puts them at risk of urinary tract infections. With or without urinary incontinence, sexual dysfunction occurs in most MS patients (see Chapter 16 ).
An inexplicable, constant sense of fatigue affects up to 80% of MS patients. While some patients and physicians describe it as “lassitude” (weariness of body or mind), fatigue is entirely subjective and does not correlate with patients' age or degree of paresis. It reduces MS patients' quality of life, ability to work, and compliance with medical regimens and has a close relationship with depression and cognitive impairment. It is also a physiologic cause of the chronic fatigue syndrome (see Chapter 6 ). Although many studies found that depression with or without anxiety is comorbid with fatigue in MS patients, antidepressants do not alleviate fatigue. Instead, amantadine may be helpful. Other effective therapies reportedly include stimulants, modafinil, and exercise. However, some medicines—certain anticonvulsants, psychotropics, and anti-MS drugs—exacerbate MS fatigue.
Various pain syndromes commonly occur in MS. For example, approximately 2% of MS patients suffer from trigeminal neuralgia (see Chapter 9 ). Many MS patients have ill-defined dysesthesias or frank pain in their limbs or trunk. These sensations probably arise from MS plaques that irritate pain-transmitting fibers in the brainstem and cervical spinal cord. As with other forms of neuropathic pain, tricyclic antidepressants and antiepileptic drugs, particularly gabapentin and carbamazepine, provide some relief.
Because MS attacks generally spare CNS structures that contain little or no myelin, symptoms that originate in gray matter injury rarely complicate the early stages of illness. For example, MS patients seldom develop signs of focal cerebral cortical dysfunction, such as seizures or aphasia. Similarly, because the basal ganglia, like the cerebral cortex, lack myelin, MS patients almost never develop parkinsonism or other movement disorders (see Chapter 18 ).
Using newly introduced imaging techniques, however, neurologists are able to detect gray matter injury in chronic MS patients. Gray matter involvement helps explain the global cerebral atrophy and progression of cognitive symptoms that cannot be attributed solely to white matter involvement.
Women with MS remain fertile. Oral contraceptives do not influence MS. If women with MS conceive, they do not have an increased rate of miscarriage, obstetric complications, or fetal malformations. Throughout pregnancy, the rates of both first MS attacks and MS exacerbations fall. In fact, during the third trimester, the exacerbation rate drops to 70% of its baseline. If MS exacerbations occur, they do not affect the pregnancy. After delivery, breastfeeding extends the protection afforded by pregnancy.
As for delivery, MS patients require cesarean sections for only the usual indications. Epidural anesthesia usually has no effect on the course of MS.
Although the pregnancy and delivery pose little threat, during the first 3 postpartum months, up to 30% of these new mothers with MS have an exacerbation. Postpartum exacerbations are more incapacitating than those that strike before conception. In the long run, the number of pregnancies does not worsen the course of MS, and the rate of MS attacks remain low during successive pregnancies.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here