Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The large intestine extends from the ileocaecal junction to the anus ( Fig. 65.1 ). It begins as the caecum and vermiform appendix, which are usually located in the right iliac fossa. The ascending colon passes superiorly in the right lateral region to the right hypochondriac region, where it bends to the left to form the right colic flexure and become the transverse colon. This loops across the abdomen with an anteroinferior convexity until it reaches the left hypochondriac region, where it curves inferiorly to form the left colic flexure ( Fig. 65.2 ). From there, it descends in the left lateral region as the descending colon before continuing as the sigmoid colon in the left iliac region. The sigmoid colon descends into the lesser pelvis and becomes the rectum anterior to the third sacral vertebra. The rectum transitions to the anal canal at the level of the pelvic diaphragm. Embryologically, the large intestine is formed from the distal midgut, all of the hindgut and the anal pit (proctodeum) ( Ch. 22 and Figure 22.4, Figure 22.7E ). Knowledge of the development of the large intestine not only helps to explain its anatomy, relations (including peritoneal attachments) and neurovascular supply, but is also fundamental to understanding congenital large intestine disorders such as anorectal malformations and malrotation of the gut.
In the adult, the large intestine is approximately 1–1.5 m long in vivo , although there is considerable individual variation. It differs from the small intestine in several ways: it has a greater calibre; for much of its course it is more fixed in position; the outer longitudinal muscle layer of the colon is concentrated into three longitudinal bands, taeniae coli; small fatty projections, omental appendices, are scattered over its free surface (although these tend to be absent from the caecum, appendix and rectum); and the colonic wall is puckered into haustra, visible on plain radiographs as incomplete septations arising from the wall of the intestine ( Fig. 65.3 ; see Fig. 65.2 ). Its calibre is greatest near the caecum, gradually diminishes towards the sigmoid colon, and then increases again in the rectum, where the distal third is dilated to form the rectal ampulla. The mean internal diameter of the large intestine is 4.8 cm ( ).
During development, the large intestine is temporarily suspended by a midline dorsal mesentery. However, after rotation of the gut in utero , large portions of it come to lie adherent to the retroperitoneum, while other segments remain suspended by a mesentery within the abdominal cavity, i.e. an intermesenteric position. The mesenteries of the colon consist of two layers of visceral peritoneum enclosing adipose and connective tissues and surrounding vessels, nerves and lymphatics that run forward from retroperitoneal structures. The caecum may be firmly adherent to the retroperitoneum but is frequently suspended by a short mesentery, especially in infants. The ascending colon is usually adherent to the retroperitoneum, while the transverse colon is suspended by a mesocolon and is freely mobile within the upper abdomen. The left and right colic flexures may have a short mesentery. The descending colon is adherent to the retroperitoneum, usually down to the level of the iliac crest, and the sigmoid colon has a mesentery of variable length. The sigmoid mesentery shortens as it approaches the pelvis and practically disappears at the level of the rectosigmoid junction. The proximal third of the rectum is covered by peritoneum on its anterior and lateral aspects, and the middle third by peritoneum on its anterior aspect only; the distal third is below the peritoneum.
The microstructure of the large intestine corresponds to the general pattern of the gut wall, comprising a mucous membrane consisting of epithelium, lamina propria and muscularis mucosae, surrounded by inner circular and outer longitudinal layers of smooth muscle and a serosa (see Figs 65.3 , 65.50 , 65.51 ). The mucosa also contains scattered neuroendocrine cells derived from the amine precursor uptake and decarboxylation (APUD) cell lineage; these cells produce amines and/or peptides, which act as hormones or neurotransmitters. Unlike the small intestine, the mucosa of the large intestine lacks villi, and the intestinal glands contain a high proportion of goblet (mucin-secreting) cells. In the appendix, the intestinal glands are sparse and numerous lymphoid follicles are found in the mucosa and submucosa. Although it is not a vital organ, the primary function of the colon is transmission and elimination of intestinal contents, but it also has important absorptive and secretory roles. The large intestine has its own intrinsic (enteric) nerve supply, the activity of which is modulated by extrinsic innervation.
The haustra of the colon are frequently absent in the caecum and often relatively sparse in the ascending and proximal transverse colon. They become more pronounced beyond the middle of the transverse colon. The sigmoid colon often has marked haustra. Omental appendices are small, fat-filled pouches of peritoneum that project from the external surface of the colon and are supplied by blood vessels that perforate its wall. There are few, if any, omental appendices on the serosal surface of the caecum, and only a limited number scattered along the ascending colon. They are more common over the distal colon and particularly numerous on the surface of the sigmoid colon, where they can be large in the obese individual. The rectum has no omental appendices.
The three taeniae coli are located in fairly constant positions beneath the serosa of the colon, except in the transverse colon. They are found on the antimesenteric aspect of the colon directly opposite the mesentery (free taenia), posterolaterally (omental taenia) and posteromedially (mesocolic taenia) midway between the free taenia and the mesentery (see Fig. 65.3 ). In the ascending and descending colon, the omental taeniae are often hidden by the peritoneal reflection on to the colonic wall. In the transverse colon, the taeniae are rotated as a consequence of the dependent position of this segment of colon, so anterior becomes inferior, posteromedial becomes posterior, and posterolateral becomes superior. The width of the taeniae coli remains fairly constant throughout the colon but they broaden out in the distal part of the sigmoid colon and gradually merge to form a complete longitudinal muscle layer around the rectum, which therefore has no external haustra.
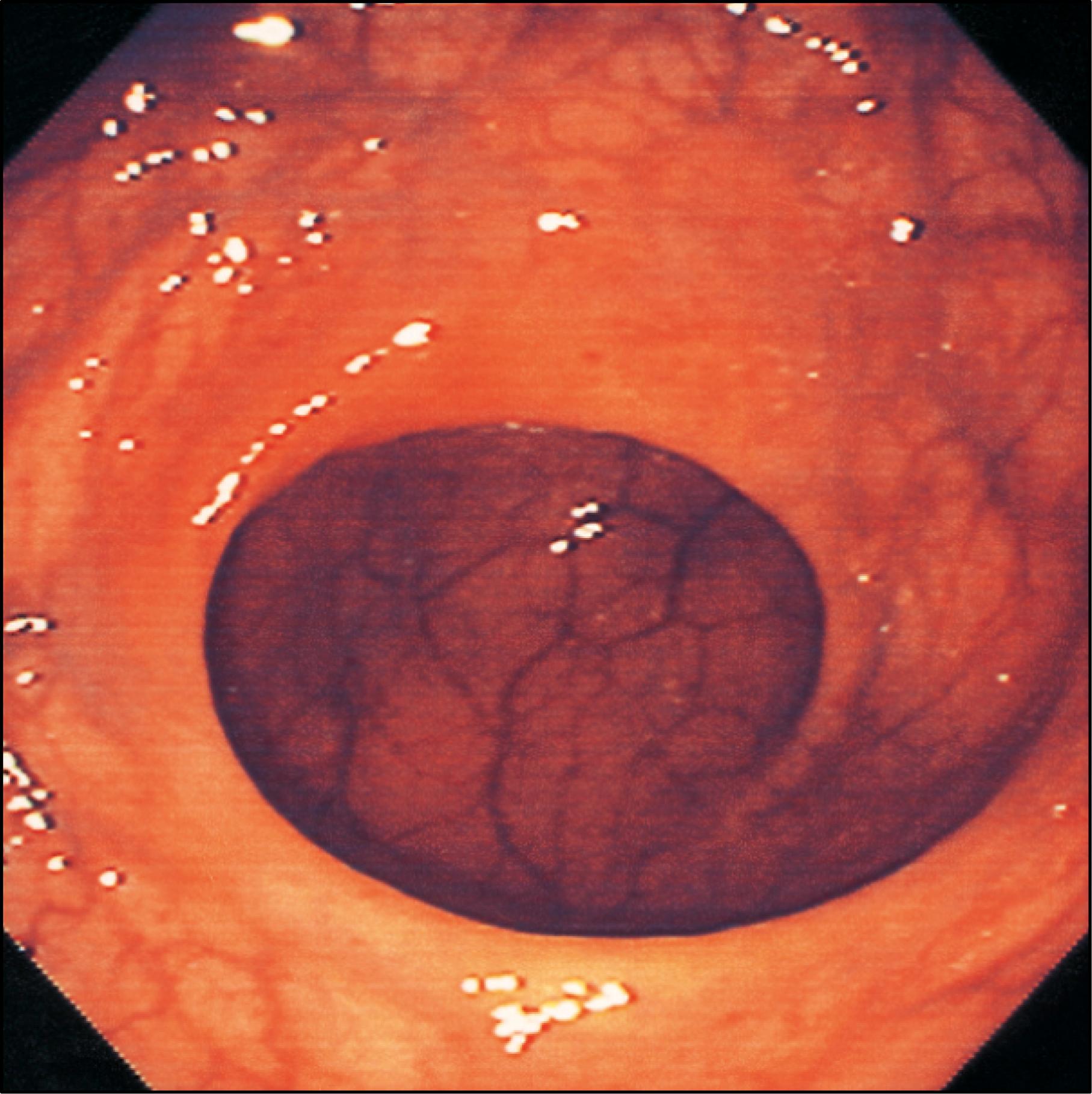
The haustra of the colon represent sites where the mucosa and submucosa of the colonic wall are infolded; these folds partially span the lumen of the colon but never form a complete circumferential ring. The pattern of haustra and appearance of the colonic mucosa help the clinician appreciate the level reached during flexible endoscopic examinations of the colon ( ). In the caecum, the three taeniae coli converge to form a characteristic ‘trefoil’ pattern on the caecal wall ( Fig. 65.4 ). The distal caecum is usually devoid of haustra, although a spiral mucosal pattern is often seen in the region of the orifice of the appendix ( Fig. 65.5 ). The ileal orifice can be identified as a thickened fold ( Fig. 65.6 ) and can be cannulated endoscopically to examine the terminal ileum. In the distal caecum and ascending colon, the haustra can extend across one-third of the lumen. In the transverse colon, the haustra often confer a triangular appearance to the cross-section of the lumen when it is viewed along its axis at colonoscopy ( Fig. 65.7 ). The haustra of the descending and sigmoid colon tend to be thicker and shorter, producing a more circular lumen cross-section ( Figs 65.8 – 65.9 ) . The wall of the colon is thinnest in the region of the caecum and ascending colon, where it is at risk of perforation during therapeutic endoscopic procedures. The overall luminal diameter is often smallest in the descending colon. The tortuosity of the sigmoid colon means that shorter lengths of it are visible during endoscopy than elsewhere in the colon. The haustra of the rectum usually form consistent and recognizable transverse rectal folds (spiral valves of Houston) and the submucosal vessels tend to be more pronounced than in the colon ( Fig. 65.10 ) . Most patients are found to have two or three folds and these are useful landmarks for planning rectal surgery ( ). Distinct veins are usually visible during endoscopy, and are most marked above the anorectal junction. FLOAT NOT FOUND FLOAT NOT FOUND FLOAT NOT FOUND FLOAT NOT FOUND






Cross-sectional imaging of the colon can be performed with computed tomography (CT) and magnetic resonance imaging (MRI). On axial images, the colon may be filled with particulate faeces and flatus ( Fig. 65.11 ). The wall in normal individuals is thin. The caecum and ascending colon often contain faecal residue. The transverse colon may contain faeces or flatus and lies in a variable position, suspended by its mesentery. The descending colon lies in the retroperitoneum on the left and seldom contains much faecal residue. The volume data sets produced by multislice CT can generate virtual colonoscopic mucosal images of the distended and cleaned colon, and surface-rendered images of the internal surface of the colon ( ).

The arterial supply of the large intestine is derived from both the superior and the inferior mesenteric arteries ( Fig. 65.12 ) ( ). The caecum, appendix, ascending colon and proximal two-thirds of the transverse colon (derived from the midgut) are supplied from ileocolic, right colic and middle colic arteries, branches of the superior mesenteric artery. The distal third of the transverse colon, descending and sigmoid colon, rectum and proximal anal canal (hindgut derivatives) are supplied predominantly from the inferior mesenteric artery via the left colic, sigmoid and superior rectal arteries, with a small contribution from branches of the internal iliac artery (the middle and inferior anorectal arteries).

The arteries of the midgut- and hindgut-derived intestine contribute to an anastomotic vessel, the marginal artery (of Drummond), which runs in the mesentery along the inner margin of the colon and gives off short terminal branches to the wall of the intestine. These divide into vasa brevia, which pass directly through the muscular layer of the colonic wall, and vasa longa, which travel through the subserosa for a short distance before running through the circular muscle, giving off branches to the omental appendices ( Fig. 65.13 ). The marginal artery is formed by the main branches and arcades arising from the ileocolic, right colic, middle colic and left colic arteries. It is most apparent in the ascending, transverse and descending colons ( Fig. 65.14 ) but poorly developed in the sigmoid



colon. The marginal artery in the region of the left colic flexure can be absent or too narrow to be of functional significance. Nevertheless, it can dilate considerably when one of the main visceral arteries is compromised since it then provides a collateral arterial supply to the colon. The most susceptible part of the chain of anastomosing vessels is at the junction of midgut- and hindgut-derived intestine in the distal transverse colon near the left colic flexure. However, the arterial supply to this region may be augmented by an inner arterial arc (of Riolan), which runs a meandering course in the colonic mesentery between the main trunk of the middle colic artery and the ascending branch of the left colic artery ( , ). When present, this vessel is usually only prominent when there is occlusion of the superior or inferior mesenteric artery.
The marginal artery of the colon can become massively dilated when there is chronic stenosis or occlusion of the superior or inferior mesenteric artery. The latter may occur, for example, in association with an abdominal aortic aneurysm, when the descending colon remains viable because the marginal artery continues to receive an adequate blood supply from left branches of the middle colic artery and the sigmoid colon gains its blood supply from the middle anorectal and inferior anorectal arteries. When colonic ischaemia does occur, it is usually maximal in the region of the left colic flexure and proximal descending colon because this segment is farthest from the collateral arterial supplies. Occlusion of the common iliac arteries can also result in dilation of the marginal and inferior mesenteric arteries, which become an important collateral supply to the lower limbs via dilated middle anorectal arteries commonly arising from either the internal pudendal or inferior gluteal artery ( ).
The venous drainage of the large intestine is primarily into the hepatic portal vein via the superior mesenteric and inferior mesenteric veins, although some drainage from the rectum occurs via middle anorectal veins into the internal iliac veins, and inferior anorectal veins into the internal pudendal veins. Those parts of the colon derived from the midgut (caecum, appendix, ascending colon and proximal two-thirds of the transverse colon) drain into colic branches of the superior mesenteric vein, while hindgut derivatives (distal third of the transverse colon, descending and sigmoid colon, rectum and proximal anal canal) drain into the inferior mesenteric vein ( Fig. 65.15 ).

Lymph drainage from the large intestine follows the course of the arteries. Thus, lymphatic vessels of the caecum and the ascending and proximal transverse colon drain ultimately into lymph nodes related to the superior mesenteric artery, while those of the distal transverse colon, descending colon, sigmoid colon and rectum drain into nodes following the course of the inferior mesenteric artery ( Fig. 65.16 ). In cases where the distal transverse colon or left colic flexure is predominantly supplied by vessels from the middle colic artery, most of the lymphatic drainage of this area may be to superior mesenteric nodes.

Lymph nodes related to the colon form four groups: epicolic, paracolic, intermediate colic and preterminal colic. Epicolic nodes are minute whitish nodules on the serosal surface of the colon, sometimes within the omental appendices. Paracolic nodes lie along the medial borders of the ascending and descending colon and along the mesenteric borders of the transverse and sigmoid colon. Intermediate colic nodes lie along the named colic vessels (the ileocolic, right colic, middle colic, left colic, sigmoid and superior rectal arteries). Preterminal colic nodes lie along the main trunks of the superior and inferior mesenteric arteries and drain into pre-aortic nodes at the origin of these vessels.
Ascending mesocolic nodes are significantly larger than sigmoid mesocolic ones; this is relevant to lymph node retrieval and examination after resection for colonic cancer ( ).
Radical lymphadenectomy during resection of colorectal cancer requires removal of the highest possible lymph nodes draining the region of colon in which the tumour is located. In cases of cancer of the rectum or sigmoid colon, this usually involves excision of the preterminal colic nodes along the inferior mesenteric artery with ligation of the artery at its root or just below the origin of the left colic artery. At least 12 lymph nodes must be excised in an oncologically resected partial colectomy for cancer.
This blind pouch, approximately 6 cm long, lies below the level of the ileocaecal junction ( Fig. 65.17 ) , anterior to the right iliac and psoas fasciae, with the lateral femoral cutaneous nerve interposed. The caecum usually lies adjacent to the anterior abdominal wall unless the greater omentum or loops of small intestine are interposed. It is often completely covered by peritoneum, which is reflected posteriorly and inferiorly to the floor of the right iliac fossa. The three taeniae coli lie anteriorly, posteromedially and posterolaterally and converge on the base of the appendix. During childhood, the lateral wall of the caecum outgrows the medial wall such that the orifice of the appendix, which is originally at the distal caecum, usually comes to lie slightly posteromedially.

Fluid and electrolyte reabsorption by the large intestine begins in the caecum but occurs mostly in the ascending and transverse colon. The distensible ‘sac-like’ morphology of the caecum allows large volumes of semi-liquid chyme from the small intestine to be stored. Its relatively large diameter makes it liable to distension with increased intracolonic pressure and it is the region of the large intestine at greatest risk of perforation secondary to colonic distension (from obstruction or other pathology).
The terminal ileum joins the posteromedial aspect of the large intestine at the junction of the caecum and colon, where it projects into the lumen of the large intestine as the ileal papilla ( Fig. 65.18A ). This projection consists of two lips and its precise shape and form varies from slit-like to an oval mucosal rosette, depending, in part, on the state of contraction or distension of the caecum. The ileocolic lip is approximately horizontal and is at the junction between the ileum and colon; the ileocaecal lip is longer and more concave, and is at the junction between the ileum and caecum. At their bases, the lips fuse and continue as the frenulum of the ileal orifice.

The ileal papilla is formed by the mucosa, submucosa and external muscle layers of the ileum, continuing through the wall of the large intestine and combining with corresponding layers from the caecum inferiorly and the colon superiorly ( Fig. 65.18B ). Its internal surface is lined by small intestinal mucosa and its large intestine surface is covered by large intestine mucosa; these epithelial surfaces meet near the tip of the ileal papilla. A localized thickening of the muscle at the base of the ileal papilla is consistent with physiological data that suggest the presence of an intrinsic anatomical sphincter ( ). In addition, the bilabial configuration of the ileal papilla could confer a valvular function. The ileocaecal junction performs several roles: it provides partial mechanical and functional separation of the luminal environments of the small and large intestine, which differ in composition, pH and bacterial content; it impedes reflux from the colon; and it helps to regulate antegrade small intestine transit.
If the caecum and ascending colon are attached to the posterior abdominal wall by a narrow mesentery, the ileocaecal region is at risk of twisting about its mesenteric pedicle, creating a caecal volvulus. In such cases, the caecum becomes markedly distended because of the strangulating closed loop intestinal obstruction that develops. Non-anatomical factors such as caecal distension can also contribute to the pathogenesis of caecal volvulus ( , ).
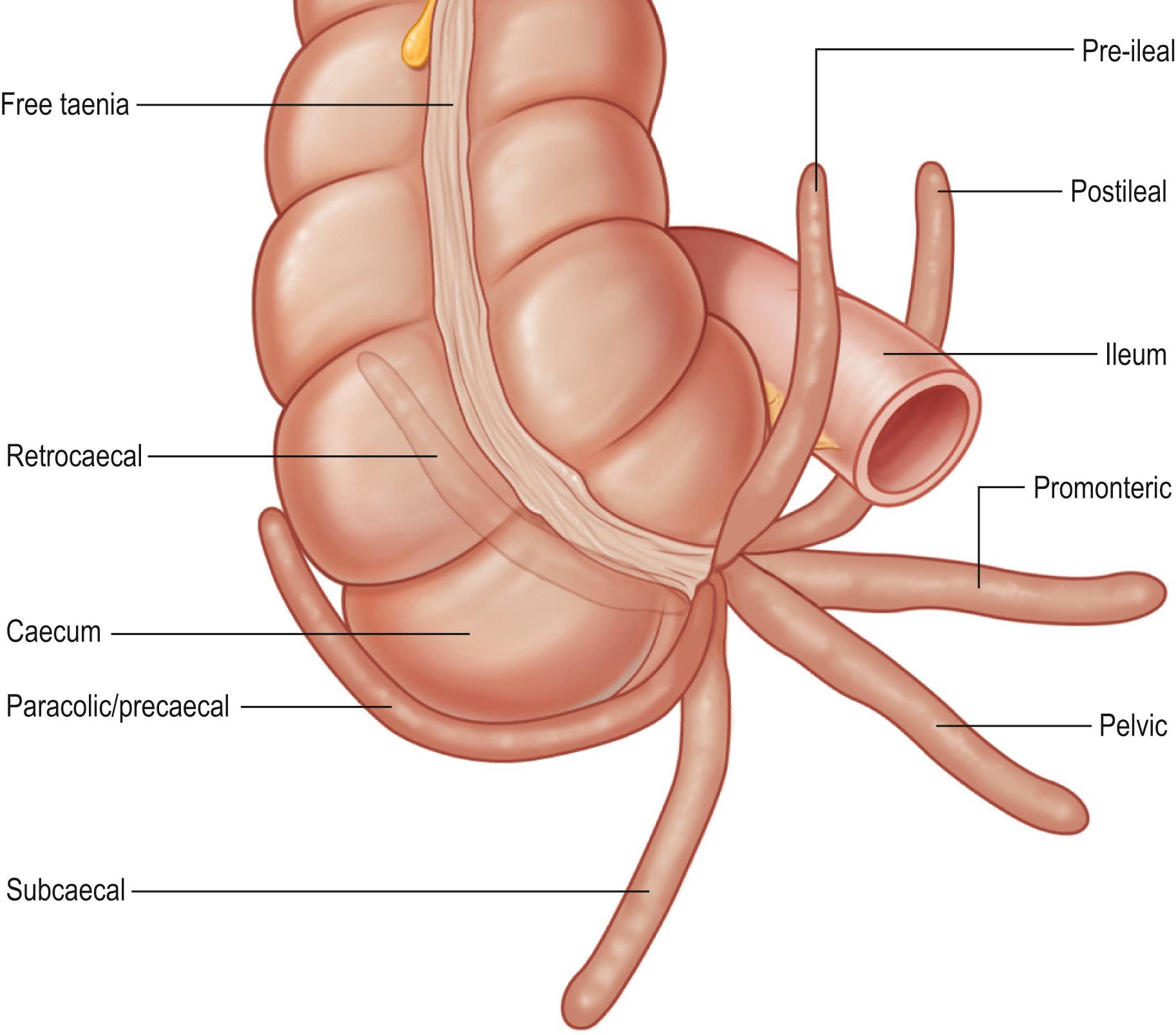
The appendix is a narrow, blind-ending tube, usually 6–10 cm long in the adult. It joins the posteromedial wall of the caecum below the ileocaecal junction. The appendix grows in length and diameter during early childhood, reaching almost mature dimensions by about three years of age ( ). It usually lies in the right iliac fossa but its distal end may occupy one of several positions ( Fig. 65.19 ) ( ). In clinical practice, the tip is most commonly retrocaecal or retrocolic (behind the caecum or proximal ascending colon, respectively, anterior to iliacus and psoas major), or pelvic (when the appendix descends over the linea terminalis, close to the right uterine tube and ovary in females). Other positions include subcaecal, and pre- or post-ileal (anterior or posterior to the terminal ileum, respectively), especially when a long meso-appendix allows greater mobility. The surface marking for the base of the appendix has traditionally been described by McBurney’s point (two-thirds of the way along a line between the umbilicus and right anterior superior iliac spine) but its position is variable and is affected by posture, caecal distension and other factors ( ).
The appendix has a continuous outer layer of longitudinal muscle formed by the coalescence of the three taeniae coli. Its lumen is irregularly narrowed by submucosal lymphoid tissue. The meso-appendix is a triangular mesentery running between the terminal ileum and appendix; it contains a variable amount of fat and frequently ends short of the distal end of the appendix. A fold of peritoneum runs between the terminal ileum and the anterior layer of the meso-appendix (the ‘bloodless fold of Treves’), and another fold of peritoneum containing the anterior caecal vessels extends from the terminal ileal mesentery to the anterior wall of the caecum (and contains the anterior caecal artery). The luminal orifice is sometimes partially covered by a mucosal fold forming an asymmetric ‘valve’ (see Fig. 65.5 ). The lumen can be widely patent in early childhood but is often partially or wholly obliterated in the elderly. Agenesis and duplication of the appendix are exceptionally rare ( , ).
The layers of the wall of the appendix are similar to those of the large intestine in general but with some notable differences. The serosa forms a complete covering, except along the mesenteric attachment. The outer longitudinal muscle is a complete layer of uniform thickness, except in a few small areas where the muscularis externa is deficient, allowing the serosa to come into contact with the submucosa.
Microscopic examination of the appendix reveals the epithelial layer, prominent lymphoid tissue of the mucosa, and the underlying submucosa, muscularis propria, serosa and subserosal connective tissue. The conspicuous (and often confluent) lymphoid aggregates are a characteristic feature of the appendix that can involve both the mucosa and the submucosa ( Fig. 65.20 ). The mucosa is covered by columnar epithelium, which contains M cells where it overlies the mucosal lymphoid tissue. Intestinal glands are similar to those of the colon but are fewer and less densely packed. They penetrate deep into the lamina propria. The submucosal lymphoid tissue frequently exhibits germinal centres within its follicles, indicative of B cell activation. Lymphoid follicles are absent at birth but accumulate during the first 10 years of life to become prominent. In adults, the lymphoid follicles gradually atrophy; in the elderly, the lumen of the appendix can be partially obliterated by fibrous tissue ( ).

Acute appendicitis can develop if the lumen is obstructed by inspissated material, a faecolith (appendicolith) or lymphoid swelling. This can lead to suppuration, infarction and necrosis. Appendicoliths are more common in children than adults but their prevalence is variable, reflecting differences among populations, definitions and methods of detection. In one radiographic study of normal appendices removed incidentally at surgery or at autopsy, calcified faecoliths were identified in 2.7% ( ). The increased size of the appendicular orifice in early childhood and the decreased size of the lumen in the elderly could explain why acute appendicitis is less common in these age groups. Low suspicion can lead to delayed diagnosis in the elderly resulting in higher morbidity and mortality ( ). Although the appendix is well supplied by arterial anastomoses at its base, the appendicular artery is an end artery; its close proximity to the wall of the appendix makes it susceptible to thrombosis during acute appendicitis, which explains the high frequency of gangrenous perforation seen in the disease.
Visceral afferent fibres within adjacent nerves are responsible for the initial symptoms of acute appendicitis (colicky pain with or without emesis) that are caused by distension and inflammation of the appendix. Abdominal pain from appendicitis is poorly localized initially and referred to the umbilical region of the abdomen, consistent with the midgut derivation of the appendix. It is not until parietal peritoneum adjacent to the appendix becomes involved in the inflammatory process that somatic nociceptors are stimulated, resulting in localization of pain to the right iliac fossa. Removal of the appendix is not in itself associated with any discernible long-term sequelae but this does not mean it is an entirely vestigial organ. There is some evidence that it acts as a reservoir for normal gut flora, enabling the large intestine flora to recover more rapidly after severe gastroenteritis ( ).
The ascending colon is 15–20 cm long and passes upwards from the ileocaecal junction to the right colic flexure, separated posteriorly by loose connective tissue from the iliac fascia, iliolumbar ligament, quadratus lumborum, transversus abdominis and the renal fascia anterior and inferolateral to the right kidney. The lateral femoral cutaneous nerve, usually the fourth lumbar artery, and sometimes the ilio-inguinal and iliohypogastric nerves lie posteriorly as they cross quadratus lumborum ( Fig. 65.21 ). Both the lateral and anterior surfaces of the ascending colon are covered by peritoneum which is composed of two layers of mesothelium containing fat embedded within a connective tissue lattice, vessels and nerves; it is attached to the retroperitoneum via a layer of connective tissue ( , ) known as Toldt’s fascia, which forms the plane of dissection when a right hemicolectomy is performed.

The right colic flexure, forming the junction between the ascending and transverse colon, is variable in position and has a less acute angle than the left colic flexure. It overlies the anterior surface of the inferior pole of the right kidney, abutting the inferior surface of the right lobe of the liver above (see Fig. 65.21 ; Fig. 65.22B ), the descending part of the duodenum medially, and the fundus of the gallbladder anteromedially. The posterior aspect of the right colic flexure is not covered by peritoneum and is in direct contact with renal fascia. The greater omentum often extends from its attachment to the transverse colon on to the right colic flexure.

The transverse colon is highly variable in both length (approximately 50 cm on average) and the extent to which it hangs down anterior to the small intestine between sites of attachment at the right and left colic flexures. The greater curvature of the stomach and the gastrocolic ligament, which fuses with the transverse colon anteriorly and continues inferiorly as the greater omentum, are superior. The transverse colon is suspended by the transverse mesocolon, which is attached from the inferior pole of the right kidney, across the descending part of the duodenum and pancreas, to the superior pole of the left kidney. The left colic flexure lies at a more superior level than the right colic flexure, often abutting the spleen under the lower ribs. Because of the disposition of the transverse colon and the more posteriorly sited flexures, the free taenia of the ascending and descending colon is positioned inferiorly. The transverse mesocolon affords considerable mobility to the transverse colon. Occasionally, the colon is interposed between the liver and the diaphragm, when it can be mistaken for free intraperitoneal flatus on imaging; when this is associated with gastrointestinal symptoms it is referred to as Chilaiditi’s syndrome ( ).
The artery of the midgut is the superior mesenteric artery, which arises from the anterior surface of the aorta at the level of the lower border of the body of the first lumbar vertebra. It runs steeply downwards, posterior to the splenic vein and body of the pancreas, with the superior mesenteric vein on its right, and directly anterior to the left renal vein, the uncinate process of the pancreas and the horizontal part of the duodenum. It then enters the root of the mesentery of the small intestine and passes obliquely downwards and to the right, giving off several branches to the large intestine.
The ileocolic artery arises from the superior mesenteric artery near the root of the mesentery of the small intestine, descending within that mesentery to the right towards the caecum, and crossing anterior to the right ureter, gonadal vessels and psoas major. It usually divides into superior and inferior branches, the superior branch running up along the left side of the ascending colon to anastomose with the right colic artery (or right branch of the middle colic artery) ( ). The inferior branch runs to the ileocaecal junction and divides into anterior and posterior caecal arteries, the appendicular artery and an ileal branch that passes to the left in the ileal mesentery to anastomose with a terminal ileal branch of the superior mesenteric artery ( Fig. 65.23 ). The latter therefore provides a collateral arterial supply to the caecum. The ileocolic artery provides the major arterial supply to the caecum; traction on the caecum in the direction of the anterior superior iliac spine will cause the artery to tent up the mesentery, allowing the vessel to be easily identified.

The appendicular artery usually arises directly from the ileocolic artery and descends posterior to the terminal ileum to enter the meso-appendix a short distance from the base of the appendix (see Fig. 65.23 ). Here, it gives off a recurrent branch that anastomoses at the proximal appendix with a branch of the posterior caecal artery. The appendicular artery approaches the distal end of the organ, at first near to and then in the edge of the meso-appendix. Its terminal part lies on the wall of the appendix and can become thrombosed in appendicitis, resulting in distal gangrene or necrosis. Less commonly, the appendicular artery arises from the posterior caecal artery or an ileal artery ( ) (see Fig. 65.12 ). Accessory appendicular arteries are common; two or more arteries may supply the appendix.
The right colic artery is relatively small and variable in its anatomy ( , ). It usually arises as a common trunk with the middle colic artery, but can originate directly from the superior mesenteric artery or from the ileocolic artery (when it is referred to as an accessory right colic artery) ( Fig. 65.24 ). It passes to the right, across the right psoas major and quadratus lumborum, crossing the right gonadal vessels and ureter. Near the left side of the ascending colon it divides into a descending branch, which runs down to anastomose with the superior branch of the ileocolic artery, and an ascending branch, which passes up across the inferior pole of the right kidney to the right colic flexure, where it anastomoses with a branch of the middle colic artery. Together, these anastomoses form the marginal artery at the right colic flexure.

The middle colic artery arises from the right side of the superior mesenteric artery, either separately or in common with the right colic artery, just inferior to the neck of the pancreas, and passes anteriorly and superiorly within the transverse mesocolon, just to the right of the midline. As it approaches the colon, it usually divides into right and left branches. The right branch anastomoses with the ascending branch of the right colic artery. The left branch supplies the terminal part of midgut derivatives and anastomoses with a branch of the left colic artery near the left colic flexure. The marginal artery thus formed lies a few centimetres from the mesenteric edge of the transverse colon. Sometimes, the middle colic artery divides into three or more branches within the transverse mesocolon, in which case the most lateral branches form the arterial anastomoses. An accessory, or rarely a replaced, middle colic artery can arise directly from the abdominal aorta ( ), dorsal pancreatic, hepatic, inferior mesenteric or left colic arteries ( Fig. 65.25 ). In addition, an accessory middle colic artery is occasionally found arising from the superior mesenteric artery proximal to the origin of the actual middle colic artery ( ).

All the branches of the superior mesenteric artery are accompanied by correspondingly named veins. These tributaries drain into the superior mesenteric vein, which ascends to the right of the artery, crossing the horizontal part of the duodenum and uncinate process of the pancreas. Behind the neck of the pancreas, at the level of the transpyloric plane (the inferior border of the body of the first lumbar vertebra), it joins the splenic vein to form the hepatic portal vein, which ascends behind the superior part of the duodenum to reach the liver. The right colic vein is highly variable: it can drain either directly into the superior mesenteric vein, or into the right gastro-omental or inferior pancreaticoduodenal veins to form a ‘gastrocolic trunk’ that drains into the superior mesenteric vein, or it can be entirely absent ( , ). Several tributaries draining into one or more middle colic veins are highly variable in extent and position. The middle colic veins drain either into the superior mesenteric vein, just before its junction with the splenic vein, or directly into the hepatic portal vein. The appendicular vein usually joins the caecal vein to become the ileocolic vein; infection from the appendix can therefore be carried directly to the liver via the hepatic portal vein.
Lymphatic vessels originate from both anterior and posterior aspects of the colon. Lymph drainage from midgut derivatives follows the course of the superior mesenteric artery. Thus, lymph from the caecum and appendix drains to nodes associated with the ileocolic artery, and lymph from the distal ascending colon and right colic flexure drains to nodes along the right colic artery (see Fig. 65.16 ). When the distal transverse colon and left colic flexure are predominantly supplied by the middle colic artery, lymph drainage of this segment is also largely to superior mesenteric nodes. Lymphatic vessels in the appendix are numerous and combine to form vessels that ascend in the meso-appendix, occasionally interrupted by one or more nodes. They unite to form three or four larger vessels that anastomose with lymphatic vessels draining the ascending colon into ileocolic nodes.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here