Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Science of processes and mechanisms of skeletal muscle contraction and the corresponding interaction of other body systems that facilitate and respond to skeletal muscle contraction.
Skeletal muscle contraction that exceeds physiologic limits, is inappropriate in duration or intensity, or for which the musculoskeletal system has been inadequately prepared can lead to injury or poor performance and adaptation to training.
Clinical relevance lies in identification of the pathology; what triggered it; and how to correct, alleviate, and/or prevent this in both individuals and populations of active people.
Metabolic equivalents (METs): expression of metabolic cost of exercise in terms of oxygen consumption
Rest defined as 1 MET, which is an oxygenation of 3.5 mL O 2 /kg/min
MET chart ( Table 17.1 )
| Sport | METs |
|---|---|
| Basketball (comp) | 7–12 |
| Biking (rec) | 3–8 |
| Dancing | 3–7 |
| Football | 6–10 |
| Golf (cart) | 2–3 |
| Jogging (5–6 mph) | 7–15 |
| Skiing (downhill) | 5–8 |
| Soccer | 5–12 |
| Tennis | 4–9 |
| Volleyball | 3–6 |
VO 2 max: maximal oxygen utilization
Gold standard for evaluating cardiorespiratory fitness
Measured in mL O 2 /kg/min
Anaerobic threshold: point at which oxygen demand exceeds oxygen availability
Workload: amount of energy required to complete a specific task ( Table 17.2 )
| Workload | Miles | Minutes |
|---|---|---|
| 5 METs | 1 | 15–18 |
| 6 METs | 1.5 | 21–25 |
| 8 METs | 2 | 24–29 |
| 10 METs | 4 | 50–54 |
| 12 METs | 5 | 70–80 |
The sarcomere, which is the basic unit of muscle, is composed of actin and myosin filaments ( Fig. 17.1 ).
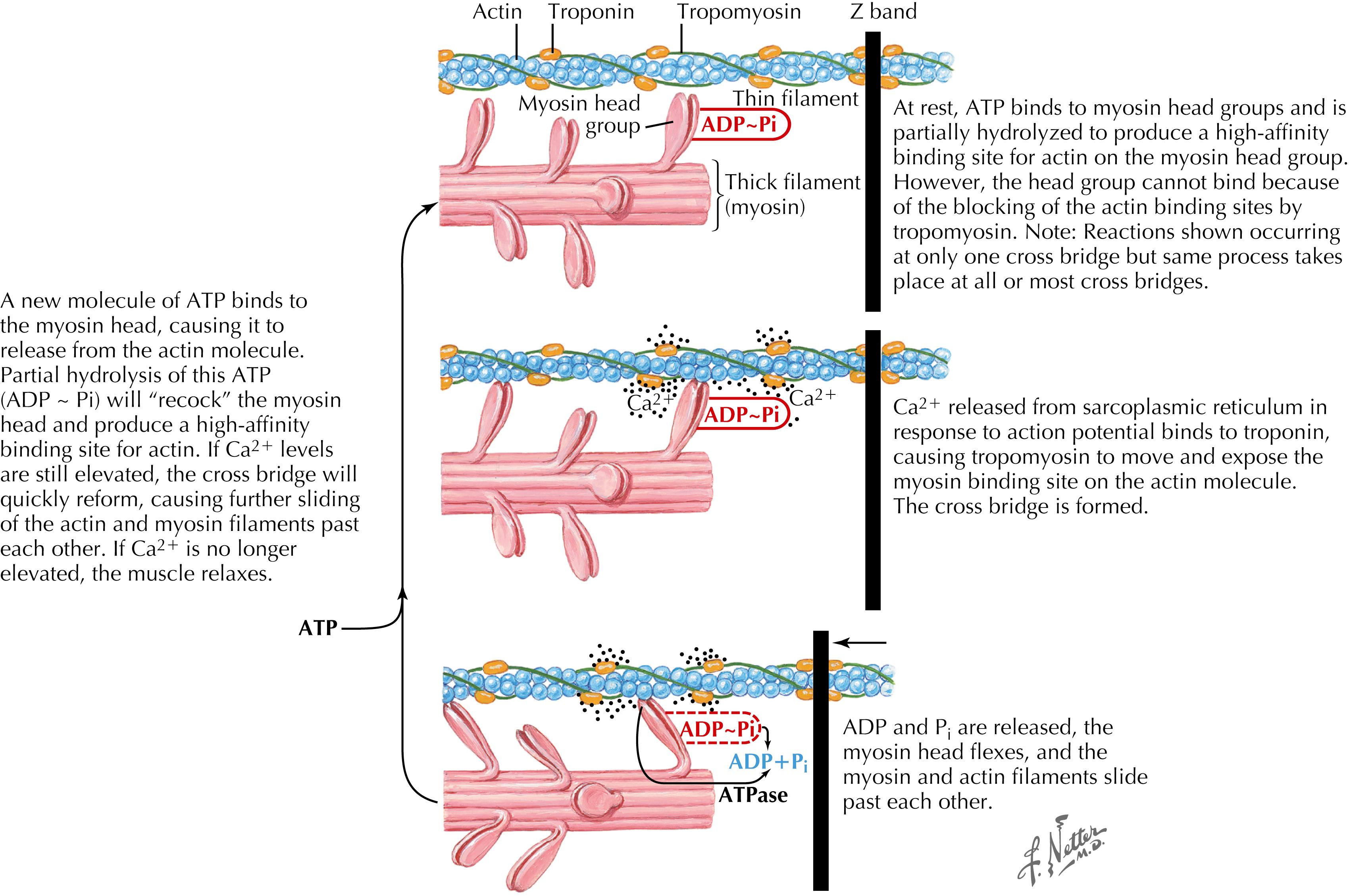
This linkage between actin and myosin is facilitated via acetylcholine release at the motor endplate, which triggers depolarization and subsequent release of calcium from the sarcoplasmic reticulum; this is followed by a series of reactions, causes formation of an adenosine triphosphate (ATP)–myosin complex, a subsequent change in myosin unit conformation, and ultimately, traction on the actin filament. This pulls on the sarcomere’s connective tissue components, resulting in muscle contraction ( Fig. 17.2 ) and movement.
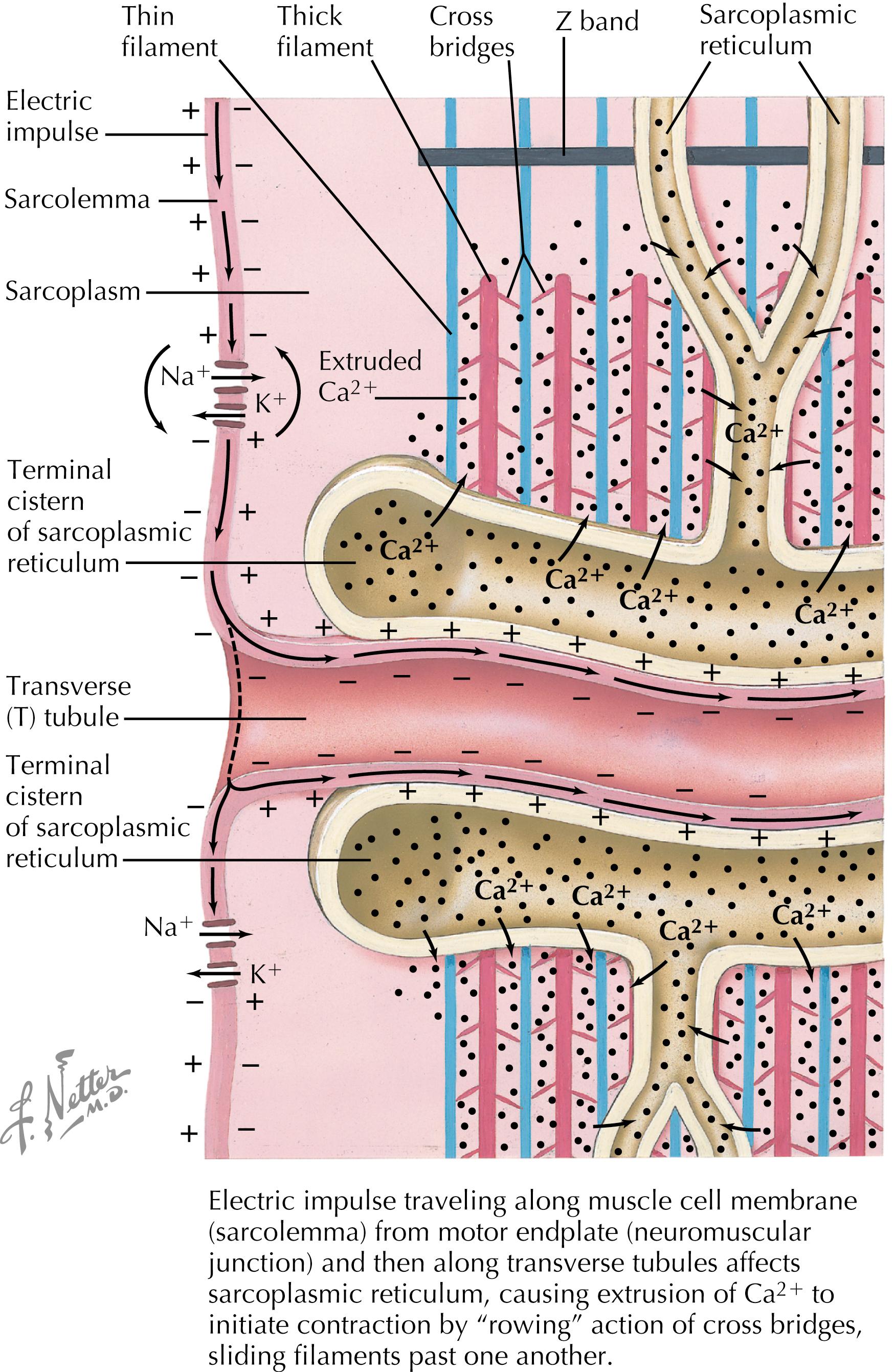
The motor nerve center directs the timing and sequencing of motor unit recruitment and firing, which facilitates coordinated movement.
Continued muscle contraction relies on an adequate supply of ATP in each sarcomere.
ATP is provided by three interlinked, overlapping energy systems that synthesize ATP for both short periods of intense vigorous activity and longer periods of lower-level sustained activity.
Exercise results in increases in protein synthesis within muscle, with long-term/cumulative changes to the steady-state level of protein synthesis with repetitive exercise.
Body weight and glucose control are influenced by the energy requirements of muscle contraction.
Anaerobic system used in maximum-intensity exercise lasting only seconds
Composed of ATP and creatine phosphate stored in the cytoplasm of each sarcomere
Phosphagens provide rapid resynthesis of ATP on myosin heads, facilitating brief, high-intensity bursts of muscle activity.
Particularly important during very high-intensity exercise and at the beginning of exercise
Anaerobic process that degrades muscle glycogen to pyruvate
Pyruvate is an essential substrate that can be oxidized to ATP via the aerobic energy system (see “Oxidative System”).
Also directly provides some ATP, which becomes part of the phosphagen pool.
Energy source in high-intensity, short-burst exercise (typically ≤3 minutes).
Pyruvate can be reversibly converted to lactate, which can be transported out of the cell for use by other tissues.
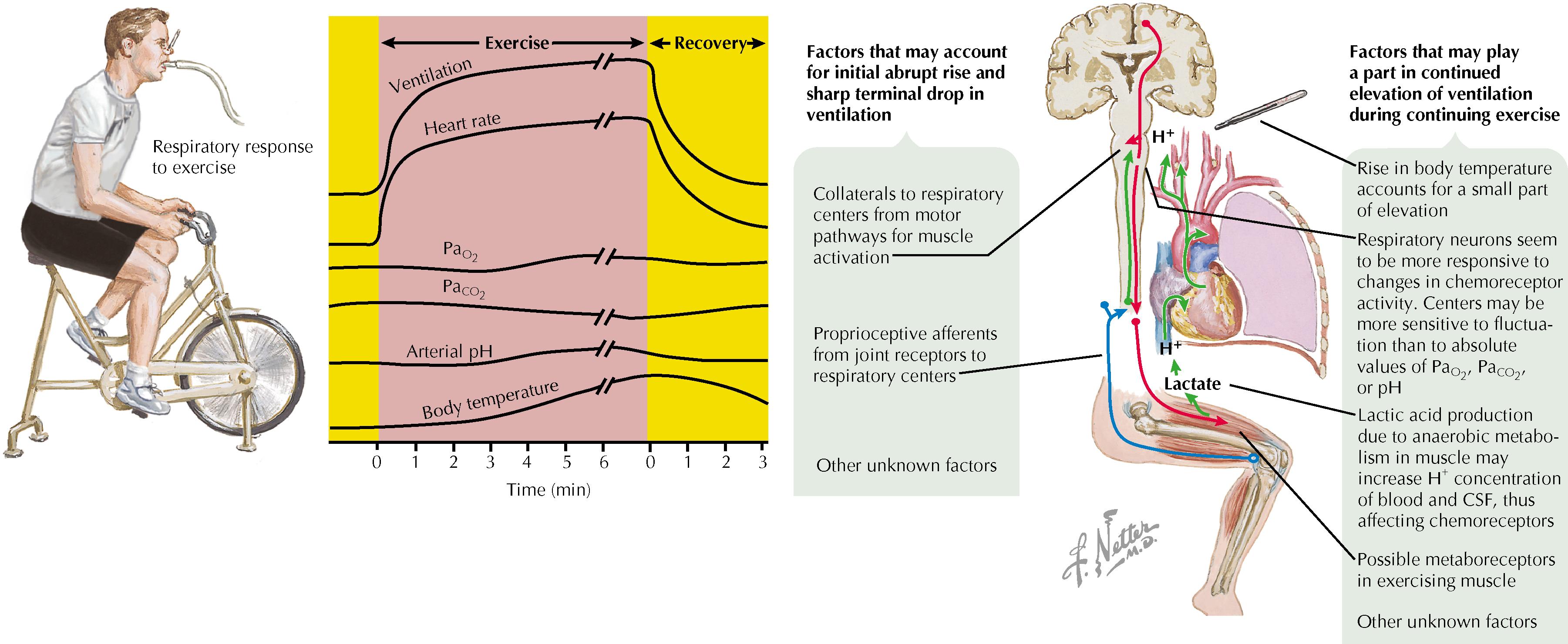
Also serves as a negative feedback loop because increased lactate causes metabolic acidosis, which increases the rate of ventilation and causes muscle discomfort; these reactions will eventually encourage the individual to reduce the intensity of exercise.
The aerobic energy system
Quantitatively the most important system
Typically used in activities lasting >3 minutes
Dependent on oxygen availability at the cellular level
The body’s physiology is structured to facilitate the transport of O 2 to tissues via the cardiorespiratory system
Dependent on oxidation of pyruvate , acetyl-CoA (formed directly from glucose), or free fatty acids
A low-power but extremely high-capacity energy system
Mitochondrial volume and density may increase up to 40% to accommodate increase in aerobic exercise.
Musculoskeletal and cardiorespiratory systems are highly adaptable to regularly performed exercise.
Adaptation to repetitive exercise can be understood in terms of several factors, which can be represented by the mnemonic P-ROIDS.
P rogression: Gradual increase in intensity, duration, and difficulty of physical activity to improve strength, endurance, and sport-specific skills
R eversibility: Training is generally continuous or cyclic in nature, because of the rapid loss of benefits from conditioning when people stop exercising
Inactivity for as little as several days can lead to reduction in work capacity secondary to a decrease in protein synthesis from baseline with loss of exercise stimulus
O verload: Exercising above normal levels through combinations of type of activity, intensity, duration, and/or frequency
I ndividual D ifferences
S pecificity: Specific training develops specific adaptations beneficial to a particular sport/activity
Training should focus on energy system that is most important to that sport (e.g., distance runners spend more time working on oxidative system)
Modern training programs typically incorporate cross-training because training focused on optimizing all energy systems can improve sport-specific performance (e.g., dry-land and weight training can improve the performance of skiers)
Concurrent training: integration of both aerobic/endurance and resistance training into the training plan
Lower-volume, high-intensity interval training can improve aerobic fitness in sedentary subjects
Ratio of acute to chronic training load can be used to monitor response to exercise and mitigate injury risk
Acute training load: workload performed over 7 days
Chronic training load: 28-day average of acute training load
Aerobic/endurance exercise: fueled by an oxidative energy system and in place when oxygen supply/delivery to tissues is adequate for sustained low- to moderate-intensity exercise
Increased lipid mobilization and oxidation by skeletal muscle
Increased number of mitochondria with adaptation
Anaerobic exercise: typically high-intensity, shorter-duration exercise that exceeds capacity of oxidative system and is fueled primarily by phosphagens and glycogen to pyruvate energy systems
Resistance exercise: training for maximal contractile force and muscle hypertrophy
Range of motion/stretching/warm-up/cool-down exercises ( Fig. 17.3 )
Flexibility exercise: increases ability to lengthen muscle–tendon units and improve motion around specific joints
“Lifestyle activity”: cumulative, nonstructured, moderate-intensity physical activities that individuals do during a typical day (e.g., taking stairs and walking from parking lot)
Ten minutes of moderate-intensity exercise three times a day facilitates changes comparable to health benefits of 30 minutes of continuous exercise
Increasing lifestyle activity is as effective as structured activity for improving cardiorespiratory fitness and reducing cardiovascular disease (CVD) risk factors.
A tool to teach, coach, and educate patients regarding opportunities to improve overall health and well-being
Can also enhance exercise and sport-specific performance
Exercise is safe for a majority of patients and has numerous health/fitness benefits
Written exercise prescription has been demonstrated to increase activity levels more compared with verbal advice alone
Prescription should include exercises to improve aerobic fitness, strength, and mobility
Identify those who would benefit from exercise prescription
Identify conditions amenable to exercise therapy
Assess patient’s activity level
Educate patient about the benefits of exercise
Assess patient interest, motivation, and goals
Strive to find activities that are sustainable
Monitor progress; assess barriers
Encourage use of measurement tools such as pedometers, accelerometers, and smart phone applications
Start slowly and allow fitness level to improve
Goal is long-term lifestyle change
Initially, prescribe shorter periods of light- to moderate-intensity exercise and build in duration, frequency, and intensity over time
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here