Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
A 95-kg, 70-year-old man is scheduled to have a left internal carotid endarterectomy. He takes amlodipine (5 mg/day) and irbesartan (150 mg/day), an angiotensin II receptor antagonist, for hypertension. He took his usual doses of both medications on the morning of surgery. Preoperative tests included a transthoracic echocardiogram that showed normal left ventricular systolic function and septal hypertrophy. Blood pressure and heart rate immediately before induction of anesthesia were 150/70 mm Hg and 56 beats per minute, respectively. After receiving 900 mL of crystalloid, he was induced with sufentanil (10 μg), propofol (150 mg), and rocuronium (50 mg), with subsequent endotracheal intubation and anesthetic maintenance with oxygen and air (40:60) and desflurane (0.7 minimum alveolar concentration [MAC]). Two minutes after induction, his blood pressure fell to 80/44 mm Hg. Despite repeated intravenous blouses of ephedrine (50 mg total), his blood pressure was 47/30 mm Hg 4 minutes after induction.
Renin-angiotensin system (RAS) antagonists include both angiotensin-converting enzyme (ACE) inhibitors and angiotensin II receptor antagonists. These drugs are used to treat hypertension and heart failure in selected patients. ACE inhibitors and angiotensin II receptor antagonists cause a blockage of the RAS that can adversely affect hemodynamics during anesthesia and surgery. Although anesthesia is not invariably associated with hemodynamic instability in RAS-blocked patients, unexpected episodes of refractory hypotension have been reported. Also, RAS antagonists, specifically ACE inhibitors, have been associated with potentially life-threatening angioedema of the head and neck.
The RAS plays an essential role in the regulation of vascular tone and extracellular fluid volume. As shown in Fig. 8.1 , sympathetic stimulation via β 1 -adrenergic receptors, renal artery hypotension, and decreased sodium delivery to the distal tubules stimulate the release of renin by the kidney. Renin is a proteolytic enzyme that cleaves to the circulating substrate angiotensinogen to form angiotensin I, which has little intrinsic pharmacologic activity. Angiotensin I is converted immediately to angiotensin II via a reaction catalyzed by ACE, which is present in vascular endothelium and lung tissue.
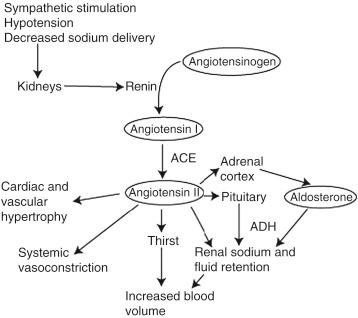
In the short term (i.e., intraoperatively), angiotensin II contributes to vascular homeostasis by increasing vascular (especially arteriolar) tone. It acts directly on angiotensin II receptors and indirectly by enhancing sympathetic adrenergic function to increase vascular tone, which is necessary to maintain adequate perfusion pressure in patients with hypovolemia or reduced cardiac output. In the longer term (e.g., hours to days), angiotensin II contributes to vascular homeostasis by its effect on extracellular fluid volume. It causes the adrenal cortex to release aldosterone, a hormone that acts on the kidneys to increase sodium and fluid retention. Angiotensin II also stimulates the release of vasopressin (i.e., antidiuretic hormone) from the posterior pituitary, which causes the kidneys to increase fluid retention. Blocking angiotensin II–mediated increased vascular tone and relative reduction of intravascular volume in patients receiving RAS antagonists chronically may cause refractory hypotension after induction of anesthesia.
Angioedema of the oropharynx or larynx has been recognized as an unusual complication of ACE inhibitor therapy. ACE inhibitor–induced angioedema usually manifests spontaneously within hours to days of initiation of treatment and has been described in association with anesthesia and endotracheal intubation. Edema of the tongue is commonly the presenting symptom, with involvement of the face, lips, floor of the mouth, pharynx, glottis, or larynx frequently observed.
The precise mechanism of angioedema formation is uncertain. Because it is likely mediated by the kallikrein-bradykinin system, it is probably a biochemical rather than an immunologic phenomenon. Bradykinin is a potent vasodilator that increases vascular permeability and produces tissue edema. Kinase II (which is identical to ACE) is the major tissue enzyme responsible for the breakdown of bradykinin. ACE inhibitors inhibit kinase II to prevent bradykinin breakdown. Angioedema associated with ACE inhibitor therapy may therefore be a result of inhibition of bradykinin inactivation by kinase II.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here