Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Double outlet right ventricle (DORV) is a congenital cardiac anomaly in which both great arteries arise wholly or in large part from the right ventricle. 1 It is a type of ventriculoarterial connection (see “Cardiac Connections” under Terminology and Classification of Heart Disease in Chapter 1 ).
1 The adjectives left and right used to modify atrium or ventricle mean morphologically left and right, respectively. Position of the chamber is referred to as right-sided or left-sided .
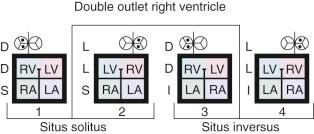
In this chapter, DORV with atrioventricular (AV) concordant connection is discussed in detail. DORV also occurs in other settings ( Fig. 53-1 ), but when the AV connection is discordant, that becomes the surgically more important feature, and patients with this combination (commonly called congenitally corrected transposition of the great arteries ) are better considered along with others with AV discordant connection (see Chapter 55 ). DORV may also occur in patients with univentricular AV connections (see “Ventriculoarterial Connections” under Morphology in Chapter 56 ). It is a frequent occurrence in patients with atrial isomerism (see “Ventriculoarterial Connections” under Morphology in Chapter 58 ).
One or both great arteries may directly overlie the ventricular septal defect (VSD) and thus arise biventricularly. For purposes of categorization, the great artery so arising is assigned to the ventricle it overlies by more than 50% on morphologic examination. Thus, when one great artery arises wholly or nearly so from the right ventricle (RV) and the other more than 50% from it, the condition is termed DORV. Uncommonly, both great arteries arise biventricularly in association with a doubly committed juxta-arterial VSD (see Chapter 35 , Fig. 35-8, Fig. 35-9 ). One option is to arbitrarily assign each great artery to the ventricle above from which more than 50% arises and categorize the anomaly accordingly; the alternative is to term the malformation double outlet both ventricles.
Tetralogy of Fallot is an entity characterized by a variable amount of dextroposition of the aorta. When the aorta arises more than 50% from the RV, the anomaly may be categorized as tetralogy of Fallot with DORV or as DORV with pulmonary stenosis . Edwards uses still different criteria for distinguishing between these two conditions. Taussig-Bing heart (see description under Morphology later in this chapter) is an entity with variability in the origin of the pulmonary artery . This diagnosis may be made when the pulmonary artery arises wholly or nearly so from the RV (in which case, it is a type of DORV), equally from right and left ventricles, or more than 50% but not entirely from the left ventricle (LV; in which case, it is not a type of DORV). When it arises entirely or essentially so from the LV, the assignment is to transposition of the great arteries with VSD .
Because of this differing terminology, surgical reports must clearly describe the entities under discussion.
When Kirklin performed the first repair of DORV (which was of the simple type with a subaortic VSD) in May 1957 at the Mayo Clinic, the anomaly was virtually unknown, and the preoperative diagnosis was large VSD with high pulmonary blood flow. Diagnosis was correctly made at operation, the term double outlet right ventricle or origin of both great vessels from the right ventricle coined in the operating room, position of the His bundle deduced, and intraventricular tunnel repair performed in much the same manner as is done today. An identical sequence occurred at GLH in September 1958. Earlier, in 1952, Braun and colleagues reported what was clearly a case of DORV with pulmonary stenosis and used the phrase double outlet ventricle , but the title of their paper was confusing, and it escaped notice. About the time of the first repair, the first morphologic paper with the title “Double Outlet Right Ventricle” was published by Witham ; subsequently, other early descriptions of the morphology appeared. In 1963, Redo and colleagues also reported repair of this entity.
Taussig-Bing heart was described in 1949, but its place in the spectrum of DORV was not recognized until later. Many early papers understandably referred to it under the heading Transposition . Lev and colleagues recognized it as a form of DORV with subpulmonary VSD. They and earlier workers did not clearly state, however, that Taussig-Bing heart is different from the heart with classic DORV with subaortic VSD, not only with respect to relationships of the VSD but also with respect to position and interrelations of great arteries and infundibular (outlet) septum. Early reports of successful surgical treatment were published in 1967 and 1969. Other early reports were by Patrick and McGoon in 1968 and by Kawashima and colleagues in 1971.
The other types of DORV with AV concordant connection began to be clarified in the classic paper by Lev and colleagues in 1972. Successful correction of unusual forms was reported in the 1970s and early 1980s.
Although controversies developed concerning categorization of hearts with DORV and their basic morphologic features, these are now straightforward because of numerous detailed morphologic and clinical studies. The basic categorization of Lev and colleagues forms the basis of most surgical thought about this anomaly, but the terms they used, such as “subaortic” and “subpulmonary,” are relational ones. Confusion arises when their terms are used as morphologic ones for actual location of the VSD (see “Location in Septum and Relationship to Conduction System” under Morphology in Section I of Chapter 35 ).
Actual categorization of DORV and related conditions (specifically, Taussig-Bing heart, transposition of the great arteries with VSD, and double outlet left ventricle) is less important than a generalized surgical plan for their management. Even so, development of a valid body of knowledge concerning surgical methods and outcomes requires accurate categorization of morphologic details and other patient characteristics. Even with the goal of accurate morphologic categorization and description, problems remain. Although a conus (or infundibulum ) is easy to define as the presence of muscle between a semilunar and AV valve, the muscle strip may vary from a few millimeters to a few centimeters wide. An aorta that is to the right and side by side with the pulmonary trunk may seem essentially normal in position to one observer or in D-malposition to another. These matters complicate categorization accuracy and precision.
Complex categorization points to a unifying hypothesis of morphogenesis put forth in a series of papers by the Van Praaghs, summarized recently by Richard Van Praagh. He hypothesizes that “the distal or subsemilunar part of the infundibulum or conus arteriosus performs an arterial switch during cardiogenesis,” with the development stage similar to the Taussig-Bing heart. The developmental steps that avoid double outlet right ventricle relate to asymmetric conal free wall enlargement. Van Praagh proposes that failure of this morphologic step leads to such entities as double outlet right and left ventricle, various transposition entities, and isolated atrial and ventricular discordant connections.
The VSD is usually large, but in about 10% of cases it is smaller than the aortic root and flow restrictive. It may be multiple; rarely, it is absent.
In most DORV hearts, the VSD is conoventricular, lying between the limbs of the trabecula septomarginalis (TSM; septal band). However, such defects vary in their relationships with the great arteries. Therefore, the VSD is discussed in relational categories .
The subaortic VSD and TSM lie more posteriorly in the ventricular septum than subpulmonary and doubly committed VSDs, and are tucked beneath the infundibular (conal) septum ( Fig. 53-2 ). Distance between the VSD and aortic valve varies, depending on presence and length of the subaortic conus (infundibulum); this determines whether the aorta overrides the VSD and hence whether the VSD is juxtaaortic.

When there is aortic-mitral fibrous continuity, absence of a subaortic conus, and a typical juxtaaortic VSD, the posterosuperior margin of the VSD is formed by the left aortic cusp or base of the anterior mitral leaflet, depending on degree of overriding. The ventriculoinfundibular fold and rightward posterior division of the TSM may form the posterior margin of the VSD. Alternatively, the VSD may reach the tricuspid anulus (opposite the anteroseptal leaflet commissure), resulting in mitral-tricuspid continuity, and the VSD is perimembranous (see “Perimembranous Ventricular Septal Defect” under Morphology in Section I of Chapter 35 ). In this event, the rightward posterior division of the trabecula septomarginalis is deficient, and the bundle of His lies along the posteroinferior border of the VSD and is at risk during surgical repair ( Fig. 53-3 ). Occasionally the VSD may extend farther inferiorly beneath the septal leaflet of the tricuspid valve. Inferiorly, the VSD is bordered by the trabecula septomarginalis and anteriorly by the infundibular septum.

Chordal attachments of anterior and septal tricuspid leaflets are variable; they may be anomalously attached around the edge of the VSD and seriously interfere with placing of the tunnel patch ( Fig. 53-4 ).

When DORV is associated with L-malposition of the aorta, the VSD is usually juxtaaortic and thus also subaortic. VSD and TSM, within whose limbs the VSD is cradled, lie more anteriorly and superiorly than when the aorta is to the right. The TSM and its limbs form inferior and posterior margins of the defect, as does the aortic valve superiorly. The VSD occasionally extends to the tricuspid anulus and is perimembranous.
Taussig-Bing heart is the typical example of DORV and subpulmonary VSD. It may be considered a form of DORV in which the VSD is subpulmonary and associated with malalignment of the infundibular septum.
The VSD and TSM lie more superiorly and anteriorly in the ventricular septum, directly beneath the pulmonary conus or valve, than they do in subaortic VSD with right-sided aorta, but in a position similar to that of subaortic VSD with aortic L-malposition. If there is a subpulmonary conus, infundibular (conal) muscle forms the superior margin of the defect. If there is no subpulmonary conus, there is pulmonary-mitral and occasionally pulmonary-tricuspid continuity, and the VSD is juxtapulmonary with the pulmonary valve overriding it ( Fig. 53-5 ). The posterosuperior margin of the VSD is formed by the zone of fibrous continuity or by the pulmonary cusps, depending on degree of pulmonary valve overriding, or by the subpulmonary conus if present. As with subaortic VSD, the defect may extend to the tricuspid anulus posteroinferiorly and be perimembranous (see Fig. 53-5 ), but often it does not. The infundibular septum is usually sagittally oriented and is then not a part of the interventricular septum.

In doubly committed VSD, an uncommon variant, the VSD and TSM lie more superiorly in the septum than subaortic or subpulmonary VSDs. This, plus absence (or severe hypoplasia) of the infundibular septum and consequent confluence of the aortic and pulmonary valves, place the defect in a juxtaarterial position. The semilunar valves are related to posterior and superior boundaries of the defect. Anterior and inferior boundaries are formed by the TSM and its left anterior division; posteroinferior boundaries are formed by the posterior division. This muscle band usually separates the VSD from the tricuspid valve anulus. There is usually no conus, but if present it is very narrow, and there may be aortic-tricuspid and pulmonary-mitral continuity ( Fig. 53-6 ).

The VSD and its relationships resemble those of isolated juxtaarterial VSD (see Chapter 35 ), tetralogy of Fallot with juxtaarterial VSD (see Chapter 38 ), and some types of double outlet left ventricle (see Chapter 54 ). Both semilunar valves usually lie over the RV, but it can be difficult to decide whether this is the case or whether they lie mostly over the LV. At times, they may arise equally over both ventricles, a condition that can be called double outlet both ventricles.
Trabecular VSDs are not related to the TSM and its divisions, as are VSDs of most hearts with DORV, and they are clearly away from the semilunar valves. However, an inlet septal VSD (see Morphology in Section I of Chapter 35 ) may be sufficiently remote from the great arteries as to be considered noncommitted ( Fig. 53-7 ).
![Figure 53-7, Specimen of double outlet right ventricle (RV) with noncommitted ventricular septal defect (VSD). A, Right ventricular outflow tract, opened through pulmonary valve (PV) and banded pulmonary trunk (PT) and aortic valve (AoV) . A well-developed subsemilunar conus separates aortic and pulmonary valves from tricuspid valve (TV) and VSD, which is partly obscured by tricuspid valve. Aortic and pulmonary valves are joined (i.e., infundibular [conal] septum is absent). Aorta (Ao) and pulmonary trunk (PT) lie side by side, with their valves at the same level. B, View from opened left ventricle (LV) . The only exit is via the VSD (which is of inlet septal type) through which tricuspid valve tissue can be seen. Anterior mitral valve leaflet is cleft. Key: ant MV, Anterior mitral leaflet. Figure 53-7, Specimen of double outlet right ventricle (RV) with noncommitted ventricular septal defect (VSD). A, Right ventricular outflow tract, opened through pulmonary valve (PV) and banded pulmonary trunk (PT) and aortic valve (AoV) . A well-developed subsemilunar conus separates aortic and pulmonary valves from tricuspid valve (TV) and VSD, which is partly obscured by tricuspid valve. Aortic and pulmonary valves are joined (i.e., infundibular [conal] septum is absent). Aorta (Ao) and pulmonary trunk (PT) lie side by side, with their valves at the same level. B, View from opened left ventricle (LV) . The only exit is via the VSD (which is of inlet septal type) through which tricuspid valve tissue can be seen. Anterior mitral valve leaflet is cleft. Key: ant MV, Anterior mitral leaflet.](https://storage.googleapis.com/dl.dentistrykey.com/clinical/DoubleOutletRightVentricle/6_3s20B978141606391900053X.jpg)
In general, hearts with DORV may have bilateral conuses, one beneath the aortic valve and one beneath the pulmonary valve, or a single conus beneath either semilunar valve, or no conus. About three fourths of hearts with subaortic VSD have bilateral conuses, and about one fourth have only a subpulmonary conus ( Table 53-1 ). An operative experience, however, may reflect a nonrepresentative prevalence of morphologic features. For example, in 350 patients operated on at Madras Medical Mission, the distribution of conal morphology was weighted far more toward absent conus (86%); prevalence of subaortic VSD was 57% (KM Cherian; personal communication, 2000) ( Table 53-2 ). Hearts with subpulmonary VSD (Taussig-Bing hearts) have either bilateral conus or a single conus beneath the aortic valve, in about equal proportions. Hearts with doubly committed VSDs may have a single common conus beneath the two semilunar valves (“doubly committed”), or there may be fibrous continuity between one of the semilunar valves and one of the AV valves, associated with absence of a conus.
| Type of Conus | |||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Bilateral | Subpulmonary Only | Subaortic Only | Absent | ||||||||||
| Relationship of VSD | n | No. | % of n | CL (%) | No. | % of n | CL (%) | No. | % of n | CL (%) | No. | % of n | CL (%) |
| Subaortic | 22 | 17 | 77 | 64-87 | 5 | 23 | 13-36 | 0 | 0 | 0-8 | 0 | 0 | 0-8 |
| (63 | 51-74) | (100 | 68-100) | (0 | 0-19) | (0 | 0-85) | ||||||
| Subpulmonary | 11 | 5 | 45 | 27-65 | 0 | 0 | 0-16 | 6 | 55 | 35-73 | 0 | 0 | 0-16 |
| (19 | 11-29) | (0 | 0-32) | (67 | 44-85) | (0 | 0-85) | ||||||
| Doubly committed | 3 | 2 | 67 | 24-96 | 0 | 0 | 0-47 | 0 | 0 | 0-47 | 1 | 33 | 4-76 |
| (7 | 2-17) | (0 | 0-32) | (0 | 0-19) | (100 | 15-100) | ||||||
| Noncommitted | 6 | 3 | 50 | 24-76 | 0 | 0 | 0-27 | 3 | 50 | 24-76 | 0 | 0 | 0-27 |
| (11 | 5-21) | (0 | 0-32) | (33 | 15-56) | (0 | 15-100) | ||||||
| T otal | 42 | 27 | 64 | 55-73 | 5 | 12 | 7-19 | 9 | 21 | 15-30 | 1 | 2 | 0.3-8 |
| P (χ 2 ) b | .3 | .16 | .0007 | ||||||||||
a Data based on study at GLH of 42 autopsy specimens. Specimens with atrial isomerism or L-malposition of the aorta are excluded.
b P values along bottom of table refer to difference in prevalence of type of conus within the various relationships of the VSD.
| VSD Position | No. | % | Conus | No. | % | Position of Aorta in Relation to Pulmonary Trunk | No. | % |
|---|---|---|---|---|---|---|---|---|
| Subaortic | 199 | 57 | Subaortic | 32 | 9.1 | Normal | 232 | 66 |
| Subpulmonary | 37 | 11 | Subpulmonary | 6 | 1.7 | D-Malposed | 51 | 15 |
| Doubly committed | 21 | 6 | Bilateral | 10 | 2.9 | L-Malposed | 29 | 8.3 |
| Noncommitted | 93 | 27 | Noconus | 302 | 87 | Anteroposterior | 38 | 11 |
a Data from study of 350 patients with double outlet right ventricle operated on at the Institute for Cardiovascular Disease, Madras Medical Mission, 1989-2000. (Cherian KM; personal communication, 2000.)
There is a pattern of relations between conus and position of the great arteries ( Table 53-3 ). As a general rule, presence of conus beneath a semilunar valve tends to result in an anterior position of the valve and great artery. Absence of conus links semilunar valve and artery to the mitral valve with fibrous continuity, resulting in a posterior position of valve and artery. As a result, degree of conal development beneath the aortic and pulmonary valves fairly well predicts position and relationship of the great arteries. This can be inferred from the Madras experience (see Table 53-2 ), in which there is a high prevalence of normally related great arteries and subaortic or absent conus. Anterior position (D-malposition) of the aorta is uncommon (26%) when there are bilateral conuses, but common (67%) when there is only a subaortic conus. An anterior position has not been observed to occur with only subpulmonary conus or with no conus. An aorta side by side with or posterior to the pulmonary trunk occurs in all conal patterns.
| Aortic Position Relative to Pulmonary Trunk | ||||||||
|---|---|---|---|---|---|---|---|---|
| Side by Side or Posterior b | Anterior c | |||||||
| Type of Conus | n | No. | % of n | CL | No. | % of n | CL | P d |
| Bilateral | 27 | 20 | 74 | 63-83 | 7 | 26 | 17-37 | |
| (69 | 58-79) | (54 | 36-71) | .3 | ||||
| Subpulmonary only | 5 | 5 | 100 | 68-100 | 0 | 0 | 0-32 | |
| (17 | 10-28) | (0 | 0-14) | .14 | ||||
| Subaortic only | 9 | 3 | 33 | 15-56 | 6 | 67 | 44-85 | |
| (10 | 5-20) | (46 | 29-64) | .009 | ||||
| Absent | 1 | 1 | 100 | 15-85 | 0 | 0 | 0-85) | |
| (3 | 0.4-11) | (0 | 0-14) | .7 | ||||
| T otal | 42 | 29 | 69 | 60-77 | 13 | 31 | 23-40 | |
| P (χ 2 ) | .04 | .4 | ||||||
a Data and presentation are as described for Table 53-1 .
b Side by side or posterior refers to aorta being to the right and beside or slightly posterior to pulmonary trunk, with the great arteries more or less normally interrelated.
c Anterior refers to D-malposition, with aorta anterior and more or less to the right.
d P -value column refers to difference in occurrence of the given VSD position in the two great artery positions.
Both great arteries may lie over the RV in their entirety in the rare instances of DORV with intact ventricular septum and noncommitted VSD. This is often the situation as well when the VSD is subaortic. When the VSD is doubly committed or subpulmonary, there is usually a variable degree of overriding of one or both great arteries over the VSD.
Positional interrelationships of the great arteries are variable in hearts with DORV. Interrelationships are normal or near-normal in most patients with DORV, with the aorta located rightward and posterior relative to the pulmonary trunk ( Table 53-4 ). Less often, the great arteries are side by side, with the aorta to the right. D-malposition may be present in hearts with DORV, with the aorta anterior and to the right of the pulmonary trunk or at times directly anterior. Rarely, it is anterior and to the left. Occasionally there is L-malposition, with aorta to the left but side by side with the pulmonary trunk.
Although in 77% of hearts with subaortic VSD the aorta is to the right and either side by side or posterior to the pulmonary trunk (more or less normally related), it is anterior (D-malposition) in 23% of cases (see Table 53-4 ). Furthermore, more or less normally related great arteries are not unique to hearts with subaortic VSD; those with subpulmonary VSD have normally related great arteries in similar frequency ( P for difference = .8).
Only in hearts with noncommitted VSD is the frequency of more or less normally related great arteries less (33%) ( P for difference = .06; see Table 53-4 ). Although D-malposition of the aorta may be considered characteristic of ordinary transposition (see “Great Arteries” under Morphology in Chapter 52 ) and by implication Taussig-Bing heart, hearts with DORV and subpulmonary VSD are associated with typical D-malposition in a minority of cases (see Table 53-4 ).
Hearts with doubly committed VSD tend to have more or less normally related great arteries. Observing great artery position at cineangiography or operation does not permit a reasonably accurate inference as to the position and category of the VSD (see Table 53-4 ). There is no greater certainty that the VSD is subaortic when the great arteries are more or less normally interrelated than when in D-malposition ( P = .2). When the aorta is in D-malposition, there is no greater certainty that the VSD will be subpulmonary than subaortic ( P = .8).
Pulmonary stenosis is common in hearts with a subaortic VSD. It is most often infundibular ( Fig. 53-8 ), but it may be valvar, with or without a small pulmonary valve ring. Thus, all types of pulmonary stenosis observed in hearts with tetralogy of Fallot may be seen in DORV. Rarely, infundibular stenosis may be of the isolated low-lying variety, producing a two-chambered RV.

Pulmonary stenosis is also common in hearts with doubly committed VSD (five of five in the GLH experience). It is uncommon in association with Taussig-Bing heart and in hearts with a noncommitted VSD.
The AV node is in its normal position in the AV septum, and the bundle of His penetrates the right fibrous trigone in the usual way. Thus, the course of the bundle of His relative to the VSD is the same as in primary VSD and in tetralogy of Fallot (see Chapter 35, Chapter 38 ). The bundle is at risk of damage during repair when the defect reaches the tricuspid anulus (and becomes perimembranous). This is true whether the defect is subaortic or subpulmonary and whether the ascending aorta is right or left sided. However, as in other conditions with clockwise rotation and dextroposition of the aorta, the bundle is more on the LV side of the septum than usual. Furthermore, the trigone is often attenuated in DORV when there is a subaortic conus, which removes the aortic anulus from the central fibrous skeleton of the heart.
When a complete AV septal defect coexists, the node and bundle course are altered accordingly (see “Conduction System” under Morphology in Chapter 34 ).
Coronary artery pattern depends on position of the great arteries. In most varieties of DORV, it is similar to normal except that the aortic sinuses are rotated in a clockwise direction (viewed from below), such that the right coronary arises anteriorly and the left coronary posteriorly. When the aorta is anterior and rightward, the pattern is usually similar to that in transposition of the great arteries (see “Coronary Arteries” under Morphology in Chapter 52 ), with the right coronary artery arising from sinus 2 (right posterior facing sinus). In 15% of cases, a single coronary ostium may arise either anteriorly or posteriorly that supplies left and right sides of the heart. The branching pattern is also usually normal, except for occasional origin of the left anterior descending from the right coronary artery, with this vessel crossing the RV outflow from right to left as in tetralogy of Fallot (see Chapter 38 ). This anomaly was found in 25% of the DORV hearts reported in the early Mayo Clinic series, but it was not encountered in 42 GLH autopsy cases.
When the aorta is to the left in L-malposition, the right coronary artery passes to the right from the anterior sinus of the leftward anterior aorta to reach the AV groove in front of the pulmonary trunk. Its position prohibits extensive anterior patching across the pulmonary “anulus.”
Major associated cardiac anomalies, in addition to pulmonary stenosis of the tetralogy of Fallot type, may coexist. Coarctation of the aorta may be present, particularly in Taussig-Bing variant, and may require repair in the neonatal period; rarely, discrete subvalvar aortic stenosis may coexist. Various other cardiac anomalies coexist in about 30% of patients coming to intracardiac repair of DORV with a subaortic or doubly committed VSD ( Tables 53-5 and 53-6 ).
| Associated Cardiac Anomalies | No. | Percentage of Total ( n = 70) |
|---|---|---|
| Multiple VSDs | 9 | 13 |
| Patent ductus arteriosus | 8 | 11 |
| Pulmonary artery distribution deficiencies or post-shunt stenoses | 9 | 13 |
| Pulmonary atresia | 2 | 3 |
| LV hypoplasia + MV hypoplasia or regurgitation | 2 | 3 |
| Congenital mitral stenosis | 1 | 1.4 |
| Subaortic stenosis | 2 | 3 |
| Tricuspid regurgitation (severe) | 2 | 3 |
| Unroofed coronary sinus syndrome | 3 | 4 |
| Azygos continuation of IVC | 1 | 1.4 |
| Right aortic arch | 1 | 1.4 |
| Aberrant right subclavian artery | 1 | 1.4 |
| Origin of right coronary from left coronary artery | 1 | 1.4 |
| Juxtaposed atrial appendages | 1 | 1.4 |
| Situs inversus totalis (Van Praagh S,L,L) | 2 | 3 |
| No associated anomalies | 41 | 59 |
a Data combine the experience at UAB (1967-1982; n = 42) and GLH (1958-1984; n = 28). Because some patients had multiple anomalies, total is not cumulative, nor is list mutually exclusive.
| Associated Cardiac Anomalies | n | Percentage of Total ( n = 15) | Hospital Deaths |
|---|---|---|---|
| Hypoplasia of LV and MV | 1 | 7 | 1 |
| Congenital mitral stenosis | 1 | 7 | 1 |
| Two-storied heart | 2 | 13 | 1 |
| Dextrocardia | 2 | 13 | 0 |
| Juxtaposed atrial appendages | 3 | 20 | 1 |
| LSVC to CS | 3 | 20 | 1 |
| Coarctation of aorta | 1 | 7 | 0 |
| MV override or straddling | 1 | 7 | 1 |
| TV override or straddling | 1 | 7 | 0 |
| Hypoplastic RV and TV | 1 | 7 | 0 |
| AV discordant connection (Van Praagh S,L,L) | 3 | 20 | 0 |
| Multiple VSDs | 2 | 13 | 2 |
| ASD (moderate or large) | 6 | 40 | 2 |
| No associated anomalies (apart from PS or small ASD) | 5 | 33 | 1 |
a Data from experience with surgical correction at GLH (1964-1984; n = 15). Because most patients had multiple anomalies, total is not cumulative, nor is list mutually exclusive.
The phrase simple DORV connotes the commonly occurring and easily repaired type of DORV in which the VSD is subaortic and the aorta is to the right, usually by the side of the pulmonary trunk or slightly posterior to it, or which in about 20% of cases is somewhat anterior to the pulmonary trunk (see Table 53-4 ). The aorta may spiral around the pulmonary trunk as it leaves the heart, or the great arteries may course parallel to each other. Usually there is a conus (infundibulum) beneath both the aorta and pulmonary valve, but in some cases there may be no subaortic conus (see Table 53-1 ). Coronary arterial anatomy is normal.
In borderline cases, this type of DORV merges with the type in which a perimembranous VSD demonstrates inlet extension and appears to be noncommitted and, on the other hand, the type in which the VSD demonstrates outlet extension and appears to be doubly committed.
In the most representative cases, the Taussig-Bing heart is similar from heart to heart. The VSD is anterior and superior and subpulmonary. The left main coronary artery is anterior to the pulmonary trunk. The pulmonary trunk arises biventricularly over the VSD, and the aorta is to the right and slightly anterior to or alongside it (see Table 53-4 ). The first portions of aorta and pulmonary trunk are parallel rather than tending to spiral as do normally positioned great arteries. The infundibular septum is in the sagittal plane and is not part of the interventricular septum. Lev and colleagues were able to use specific morphologic features within the RV as the hallmark of Taussig-Bing heart, but this is rarely possible clinically or surgically.
Subaortic stenosis, from narrowing of the subaortic infundibulum, may develop in Taussig-Bing heart. Pulmonary stenosis is uncommon. The mitral valve may straddle across the subpulmonary VSD, and in such cases the LV may be hypoplastic. Associated coarctation of the aorta is common (about 50% of cases). This contrasts with the 6% prevalence in transposition with VSD.
In borderline cases, this type of DORV merges with transposition of the great arteries and large VSD and, on the other hand, may merge with DORV and noncommitted VSD of the trabecular type.
In DORV with doubly committed VSD, an uncommon syndrome, the VSD is immediately beneath both aorta and pulmonary trunk and is juxta-arterial.
When the VSD is in the trabecular septum and clearly far removed from the great arteries, the anomaly is easily categorized into this subset. When the VSD is in the inlet septum and up against the tricuspid valve, categorization as DORV with noncommitted VSD can be questioned, but at least the defect is further removed from the aorta than in most hearts with DORV and subaortic VSD.
DORV with L-malposition usually has a subaortic VSD (rarely extending back to the tricuspid anulus) and pulmonary stenosis and presents a rare but distinctive clinical and surgical syndrome. Rarely the VSD may be perimembranous and extend up toward the pulmonary valve, or it may be truly subpulmonary. The VSD may, contrariwise, extend into the inlet septum and be noncommitted. Mehrizi has reported DORV with L-malposition and doubly committed VSD.
In cases of DORV with complete AV septal defect, the interventricular communication is large and usually extends deeply beneath a bridging left superior leaflet (see “Atrioventricular Valves” under Morphology in Chapter 34 ) to be subaortic in position. Occasionally, however, the interventricular communication does not extend in this manner and is noncommitted.
In most hearts with this ventricular position, there is a ventricular L-loop, atrial situs solitus, and AV discordant connection (see Chapter 55 ). Uncommonly, in DORV with atrial situs solitus, AV concordant connection, and D-ventricular loop, there is a positional anomaly termed superior-inferior ventricles (over-and-under ventricles , upstairs-downstairs ventricles) (see “Cardiac and Arterial Positions” under Terminology and Classification of Heart Disease in Chapter 1 ). The RV is superior (and sometimes a little posterior) and the LV inferior. There may be D- or L-malposition of the aorta. The VSD is usually perimembranous and in the inlet portion of the septum. The right AV valve is usually more superiorly placed than usual relative to the left AV valve, and either AV valve may straddle the VSD (see “Ventricular Septal Defect with Straddling or Overriding Tricuspid Valve” under Morphology in Chapter 35 ). Severe LV hypoplasia may be present, and pulmonary stenosis is common.
Clinical features of patients with this morphologically highly variable anomaly are necessarily also highly variable. In general, patients with a large VSD and no pulmonary stenosis or severe pulmonary vascular disease are not clinically cyanotic. This is because pulmonary blood flow ( ![]() ) is high and the resultant mixture of blood in the RV has a high enough oxygen saturation to prevent clinically evident cyanosis; however, there is some arterial desaturation.
) is high and the resultant mixture of blood in the RV has a high enough oxygen saturation to prevent clinically evident cyanosis; however, there is some arterial desaturation.
Sa o 2 is also affected by streaming of blood within the RV, which is determined by the relationship of the semilunar valves to the VSD and the position and presence of the infundibular septum. Thus, in simple DORV, flow of highly oxygen-saturated LV blood through the VSD is directed preferentially beneath the infundibular septum into the adjacent aorta (particularly when the subaortic conus is short or absent), whereas systemic venous blood passes largely out of the pulmonary trunk. As a result, patients with this arrangement present in infancy with high ![]() in heart failure without cyanosis and cannot be clinically distinguished from infants with a large VSD (see Clinical Features and Diagnostic Criteria in Section I of Chapter 35 ).
in heart failure without cyanosis and cannot be clinically distinguished from infants with a large VSD (see Clinical Features and Diagnostic Criteria in Section I of Chapter 35 ).
When the VSD is subpulmonary, as in Taussig-Bing heart, flow through it of highly saturated LV blood is directed into the adjacent pulmonary trunk by the vertically positioned infundibular septum. Spa o 2 is then higher than Sa o 2 , with systemic venous blood from the RV tending to flow more into the aorta. This situation is aggravated when there is overriding of the pulmonary trunk onto the LV. Thus, these infants present in a fashion similar to patients with transposition of the great arteries with large VSD in heart failure with mild cyanosis (see “Large Ventricular Septal Defect, Large Patent Ductus Arteriosus, or Both [Good Mixing]” under Morphology in Chapter 52 ).
Pulmonary vascular disease may be more rapid in onset in patients with DORV without pulmonary stenosis than in patients with simple large VSD, particularly in Taussig-Bing heart (see “Pulmonary Vascular Disease” under Natural History in Section I of Chapter 35 ). The resultant reduction in ![]() has a more marked influence on Sa o 2 than in simple VSD, because it reduces the amount of highly saturated blood in a common mixing chamber.
has a more marked influence on Sa o 2 than in simple VSD, because it reduces the amount of highly saturated blood in a common mixing chamber.
When important pulmonary stenosis is present, cyanosis becomes severe, and the clinical features and presentation are similar to those of patients with tetralogy of Fallot (see Chapter 38 ).
On physical examination, no clinical signs distinguish patients with DORV with and without pulmonary stenosis from the conditions that they mimic. The electrocardiogram (ECG) is not diagnostic, nor is the chest radiograph. However, in those uncommon instances in which there is L-malposition of the aorta, the aorta may be evident on the posteroanterior chest radiograph as it ascends vertically from the cardiac silhouette in the left upper mediastinum ; this finding is not specific, however (see Clinical Features and Diagnostic Criteria in Chapter 57 ).
Two-dimensional echocardiography provides a considerable amount of information regarding size of the VSD, relationship of the VSD to the semilunar valves, presence of subvalvar conus, and AV valve abnormalities. Position of the great arteries and conus are usually apparent ( Fig. 53-9 ). The coronary arterial anatomy can also generally be defined accurately in neonates and infants by echocardiography alone.

Because echocardiographic assessment of morphology is reliable, cardiac catheterization before surgical intervention is not routinely required in neonates and young infants. In older infants and children, it may be needed to assess hemodynamics such as pulmonary vascular resistance and ventricular end-diastolic pressure, and to define extracardiac morphology such as the peripheral pulmonary vasculature and presence of aortopulmonary collateral vessels. Cineangiography can be used when necessary to define intracardiac morphology ( Fig. 53-10 ). The whole of the ventricular septum must be profiled so that its upper part can be projected cranially. In this way, great vessel positions can be assessed relative to the two ventricles, and location of the VSDs determined. VSD size can be judged ( Fig. 53-11 ) and subsets such as Taussig-Bing heart identified ( Fig. 53-12 ). Cineangiography is of particular value in assessing the complex interrelationships present in DORV with superior-inferior ventricles and criss-cross hearts.



Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here