Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The term “chronic stable angina” refers to angina that has been stable in frequency and severity for at least 2 months and with which the episodes are provoked by exertion or stress of similar intensity. Chronic stable angina is the initial manifestation of coronary artery disease (CAD) in about half of patients; the other half initially experience unstable angina, myocardial infarction (MI), or sudden death.
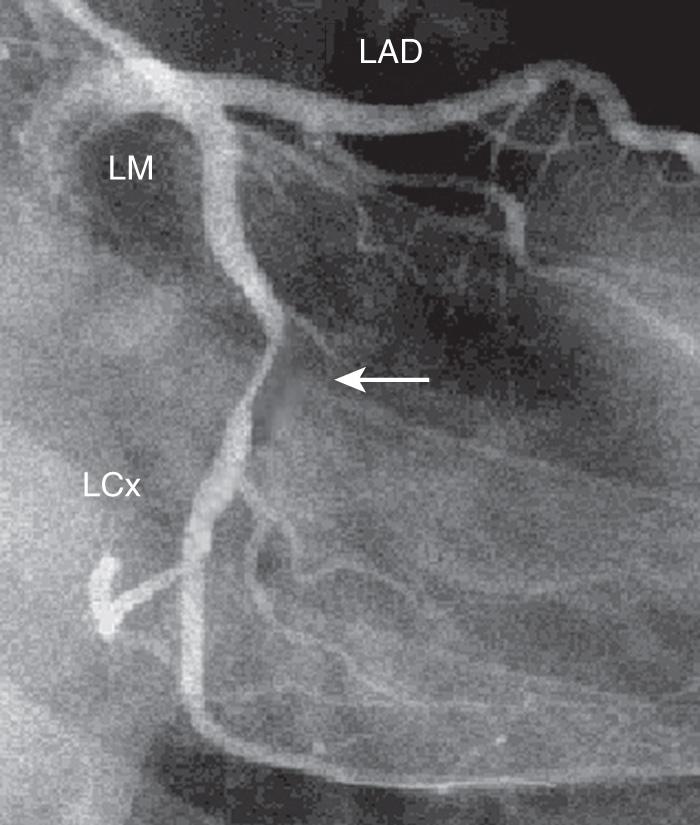
Angina occurs when myocardial oxygen supply is inadequate to meet the metabolic demands of the heart, thereby causing myocardial ischemia. This is usually caused by increased oxygen demands (i.e., increase in heart rate, blood pressure, or myocardial contractility) that cannot be met by a concomitant increase in coronary arterial blood flow, due to narrowing or occlusion of one or more coronary arteries ( Fig. 15.1 ).
Chronic coronary syndrome is a concept that was recently introduced by the 2019 European Society of Cardiology. Recognizing the dynamic nature of CAD and the various clinical presentations by which it can manifest, it is salient to distinguish between acute coronary syndrome (ACS) or chronic coronary syndrome (CCS). This has important implications for management of these patients. Conceptually, CCS is akin to the term “stable ischemic heart disease,” which is likely more familiar to US practitioners. The term includes both those with typical angina, as well as those with ischemia-mediated dyspnea on exertion or silent ischemia. CCS encompasses those with not only significant epicardial CAD but microvascular CAD as well.
The most commonly used system is the Canadian Cardiovascular Society system, in which angina is graded on a scale of I to IV. These grades and this system are described in Table 15.1 . This grading system is useful for evaluating functional limitation, treatment efficacy, and stability of symptoms over time.
|
|
|
|
After a careful history and physical examination, the laboratory tests for the patient with suspected angina should include a measurement of creatinine, hemoglobin, hemoglobin A1c, fasting lipids (i.e., serum concentrations of total cholesterol, high-density lipoprotein [HDL] cholesterol, triglycerides, and calculated low-density lipoprotein [LDL] cholesterol), and a 12-lead electrocardiogram (ECG).
Ameliorate angina.
Prevent major cardiovascular (CV) events, such as heart attack or cardiac death.
Identify “high-risk” patients that would benefit from revascularization.
Beta-blockers.
Nitrates.
Calcium channel blockers.
Ranolazine.
The initial approach should be focused upon eliminating unhealthy behaviors such as smoking and effectively promoting lifestyle changes that reduce CV risk such as maintaining a healthy weight, engaging in physical activity, and adopting a healthy diet. In addition, annual influenza vaccination reduces mortality (by ~35%) and morbidity in patients with underlying CAD. Tight glycemic control was thought to be important in patients with diabetes, but this approach actually increases the risk of CV death and complications.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here