Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The hand is an incredibly designed structure with complex anatomy and precise biomechanics. The hand must be able to produce adequate force to allow performance of activities of daily living. Furthermore, it must ensure coordination of the fingers for precise prehension and fine motor tasks.
In order to achieve an optimal functional and aesthetic outcome in patients requiring hand surgery, it is thus essential to fully understand the detailed bone, muscle–tendon, aponeurotic, vascular, nerve, and lymphatic components.
Additional challenges arise from the range of possible movements of various articular surfaces, assisted by muscle action and ligamentous support.
In this chapter, we present the various elements that compose the hand as well as explanations of the biomechanical principles. These are updated according to the latest literature. Additionally, clinical examples will be used to illustrate anatomic principles.
Access video and video lecture content for this chapter online at Elsevier eBooks+ ![]()
![]()
During the Renaissance, Vesalius corrected early misconceptions and brought gross anatomy into proper focus. Since that time, many investigators have embellished the basic structural studies with functional, physiologic, and philosophical observations. The forearm and hand have been prominently included in those observations. Sir Charles Bell (1834), in his thought-provoking volume The Hand – Its Mechanism and Vital Endowments as Evincing Design , presented a concept of hand anatomy that places it in proper context with the position of humans in the animal kingdom. Duchenne (1867) carried out detailed analysis of muscular function by isolated electrical stimulation, described in his classic volume Physiologie des Mouvements . Frederick Wood-Jones (1920) probed more extensively into comparative anatomy and anthropology in his excellent work The Principles of Anatomy as Seen in the Hand . Allen B. Kanavel (1925) published his monograph Infections of the Hand , which reported detailed analysis of the spaces and synovial sheaths. Surgery of the Hand by Sterling Bunnell (1944) became an indispensable reference during World War II. Emanuel B. Kaplan (1953) produced the nicely illustrated, detailed volume Functional and Surgical Anatomy of the Hand . Detailed studies of the integration of the intrinsic and extrinsic muscles operating the polyarticular digits may be found in the work of Landsmeer, Kaplan, Eyler and Markee, Stack, Tubiana and Valentin, and others. More recently, newer flaps intrinsic to the hand and upper extremity have been developed from more detailed investigation into vascular anatomy. Lastly, Berger, Viegas et al ., and others have expanded our knowledge of the ligamentous anatomy of the wrist.
As a functional puppet, the hand responds to human desires; its motor performance is initiated by the contralateral cerebral cortex. The conscious demands relayed to the hand and forearm from the central nervous controlling mechanism are sent as movement commands. At subconscious levels, such a movement command is broken down, regrouped, coordinated, and sent on as a signal for fixation, graded contraction, or relaxation of a specific muscular unit. The degree of contraction or relaxation is then modified by relayed evidence that the motion created is that desired by the person. The modifying factors arrive centrally from a multiplicity of sensory sources such as the eye, peripheral sensory end organs, and muscle or joint sensory endings.
The surgeon planning reconstructive surgery on the upper extremity must be aware not only of the complex anatomy of the hand and arm, but also of the physiologic interplay of balanced muscular functions under the influence of complex central nervous coordination. The maintenance of physiologic viability by the central and peripheral circulatory and lymphatic systems must also concern the reconstructive surgeon.
This chapter addresses the fundamentals of hand and upper extremity anatomy and highlights clinical pearls, new anatomic descriptions that may aid surgery of the hand, and the fundamentals of biomechanics relevant to the hand surgeon. Illustrations and dissection videos are included for the reader to review important anatomic concepts.
There is great disparity in the character of the skin and soft-tissue envelope covering the dorsum of the hand and that covering the palm. Dorsal skin is thin and pliable, anchored to the deep investing fascia by loose, areolar tissue. These characteristics, coupled with the fact that the major venous and lymphatic drainage in the hand courses dorsally, serve to explain why hand edema is first evident dorsally. The prominent, visible veins in the subcutaneous tissue make it the standard site in which to evaluate venous filling and limb venous pressure on physical examination. The same characteristics make the dorsum of the hand vulnerable to skin avulsion injuries.
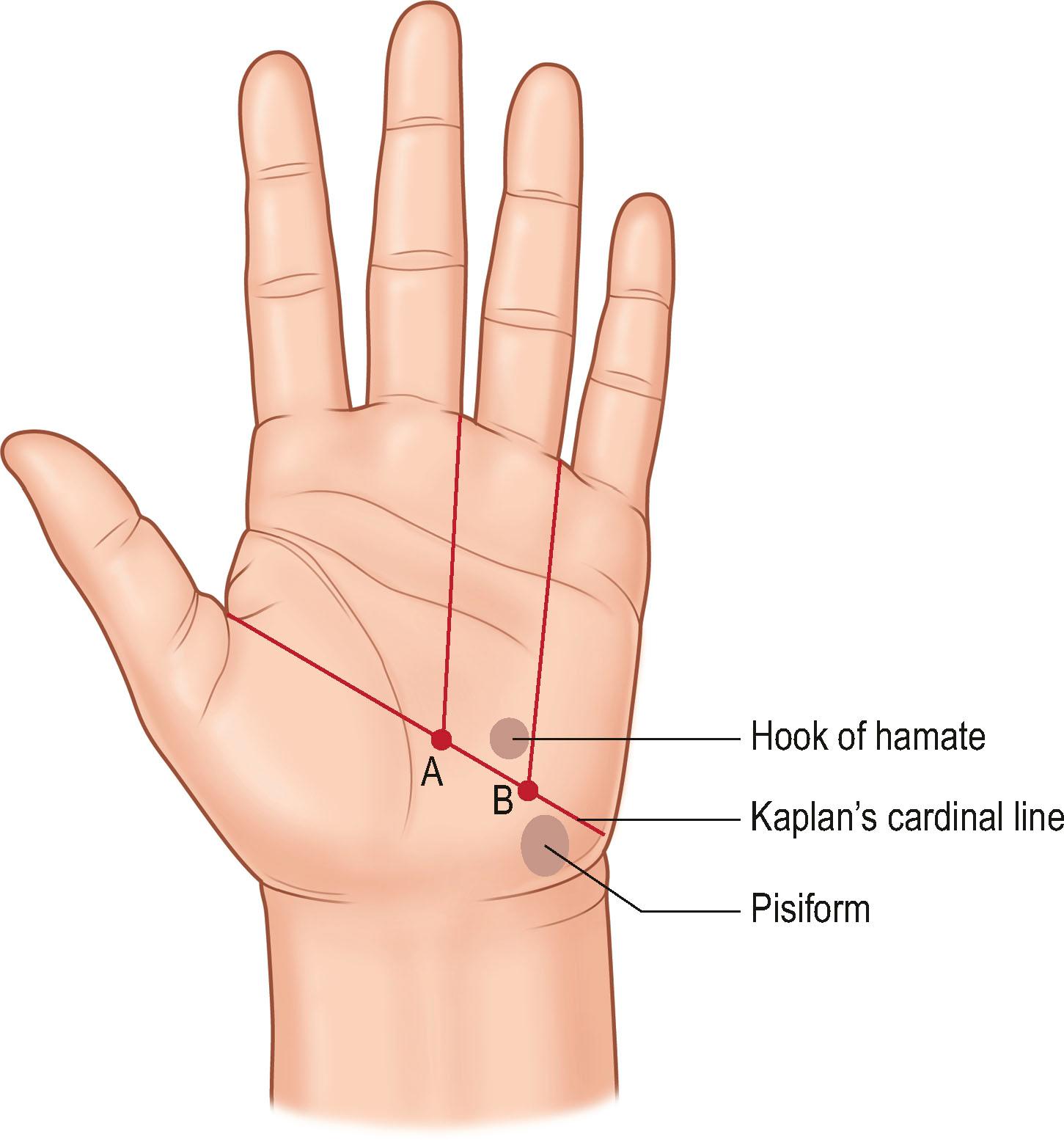
Palmar skin, in contrast, is characterized by a thick dermal layer and a heavily cornified epithelial surface. The skin is not as pliable as dorsal skin, and it is held tightly to the thick fibrous palmar fascia by diffusely distributed vertical fibers between the fascia and dermis. Stability of palmar skin is critical to hand function. At the same time, if scar fixation or loss of elasticity occurs in palmar skin, contractures and functional loss result. The skin of the palm is laden with a high concentration of specialized sensory end organs and sweat glands. The surgeon must understand the relationship of the palmar skin creases and the underlying joints in order to plan precise placement of skin incisions for exposure of joints and their related structures ( Box 1.1 & Fig. 1.1 ).
Hand anatomist Emanuel Kaplan described specific surface lines that would aid surgeons in locating key structures in the palm of the hand. The cardinal line has often been misquoted; therefore we refer to Kaplan's classic hand text, Functional and Surgical Anatomy of the Hand . Kaplan's cardinal line is drawn from the apex of the first webspace to the distal edge of the pisiform bone (see Fig. 1.1 ). Two longitudinal lines are drawn from the ulnar aspect of the middle finger and the ulnar aspect of the ring finger. These will cross the cardinal line. The intersection of the cardinal line and the longitudinal line from the ulnar side of the middle finger corresponds to the motor branch of the median nerve. The intersection of the cardinal line and the longitudinal line from the ulnar side of the ring finger corresponds to the hook of the hamate. The motor branch of the ulnar nerve is found on the cardinal line, equidistant between the hamate and pisiform. See Kaplan's original text for additional surface markings.
Examination of hand skin during normal ranges of motion in various planes is important in planning incisions or geometrically rearranging lacerations that might result in disabling scar contractures. Most loss of elasticity and some longitudinal shortening are compensated for adequately by mobility and elasticity of the uninjured dorsal skin. On the palmar aspect, however, scar shortening and inelasticity of the skin may result in contracture. The nature of palmar skin, its stabilizing fixation to the palmar fascia, and its position on the concave side of the hand are the bases for such contractures. Littler outlined the specific sites in the palm where a longitudinal scar would impede extension. For example, in each digit, the geometry has been worked out by noting each joint axis and the kissing surfaces of the palmar skin in full flexion. These diamond-shaped skin surfaces should not be shortened and rendered inelastic by longitudinal scars if limitation of extension is to be avoided ( Fig. 1.2 ).
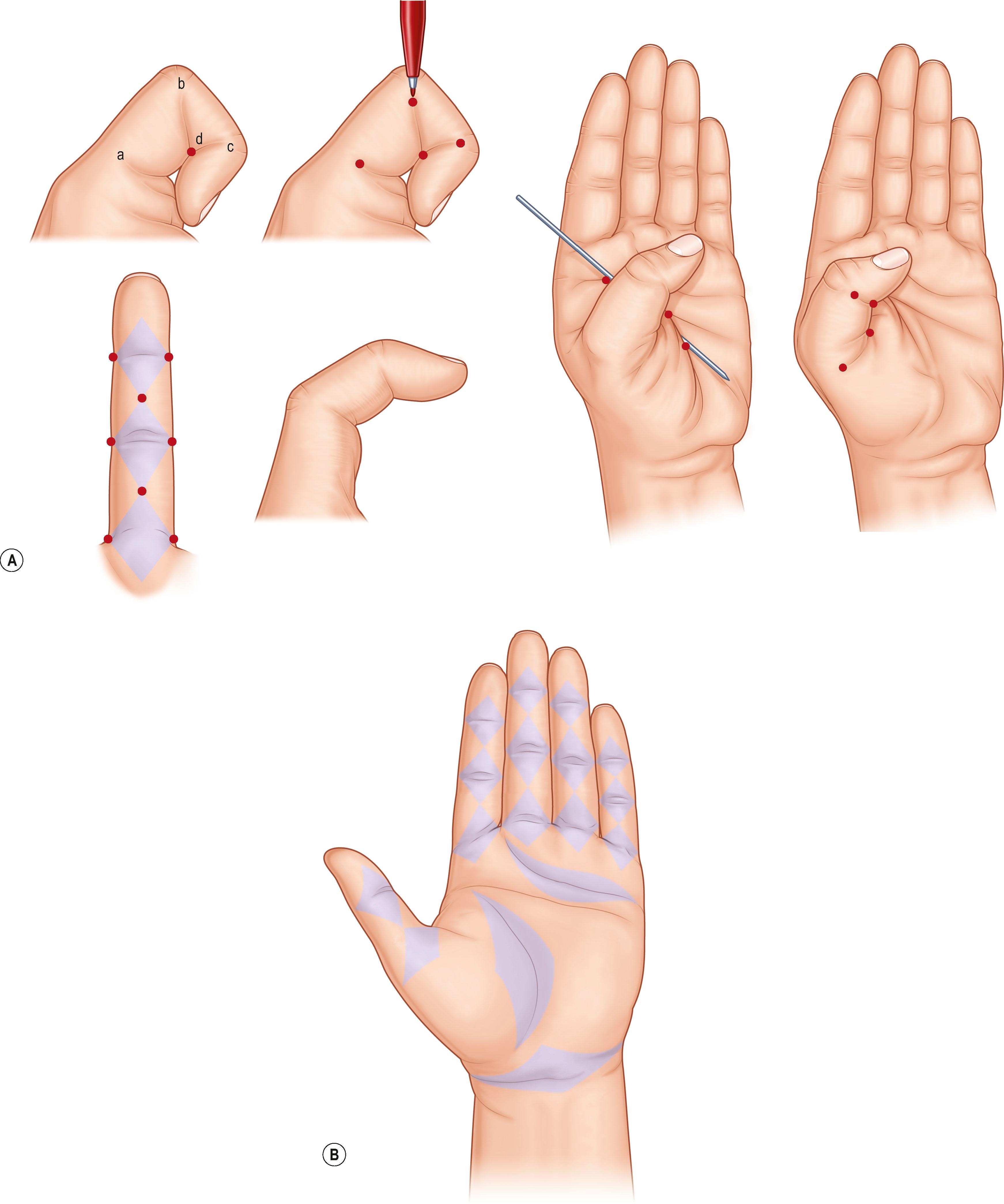
The palmar fascia consists of resistant fibrous tissue arranged in longitudinal, transverse, oblique, and vertical fibers ( Fig. 1.3 ). The longitudinal fibers concentrate at the proximal origin of the palmar fascia at the wrist, taking origin from the palmaris longus when it is present (in about 80–85% of individuals). The fascia at this level is separable from the underlying flexor retinaculum/carpal ligament, being identified by the longitudinal orientation of its fibers in contrast to the transverse fibers of the retinaculum. The palmar fascia fibers fan out from this origin, concentrating in flat bundles to each of the digits. Generally, the fibers spread at the base of each digit and send minor fibers to the skin and the bulk of fibers distal into the fingers, where they attach to tissues making up the fibrous flexor sheath of the digits. There are attachments of the fascia to the volar plate and intermetacarpal ligaments at each side of the flexor tendon sheath at the level of the metacarpal heads.
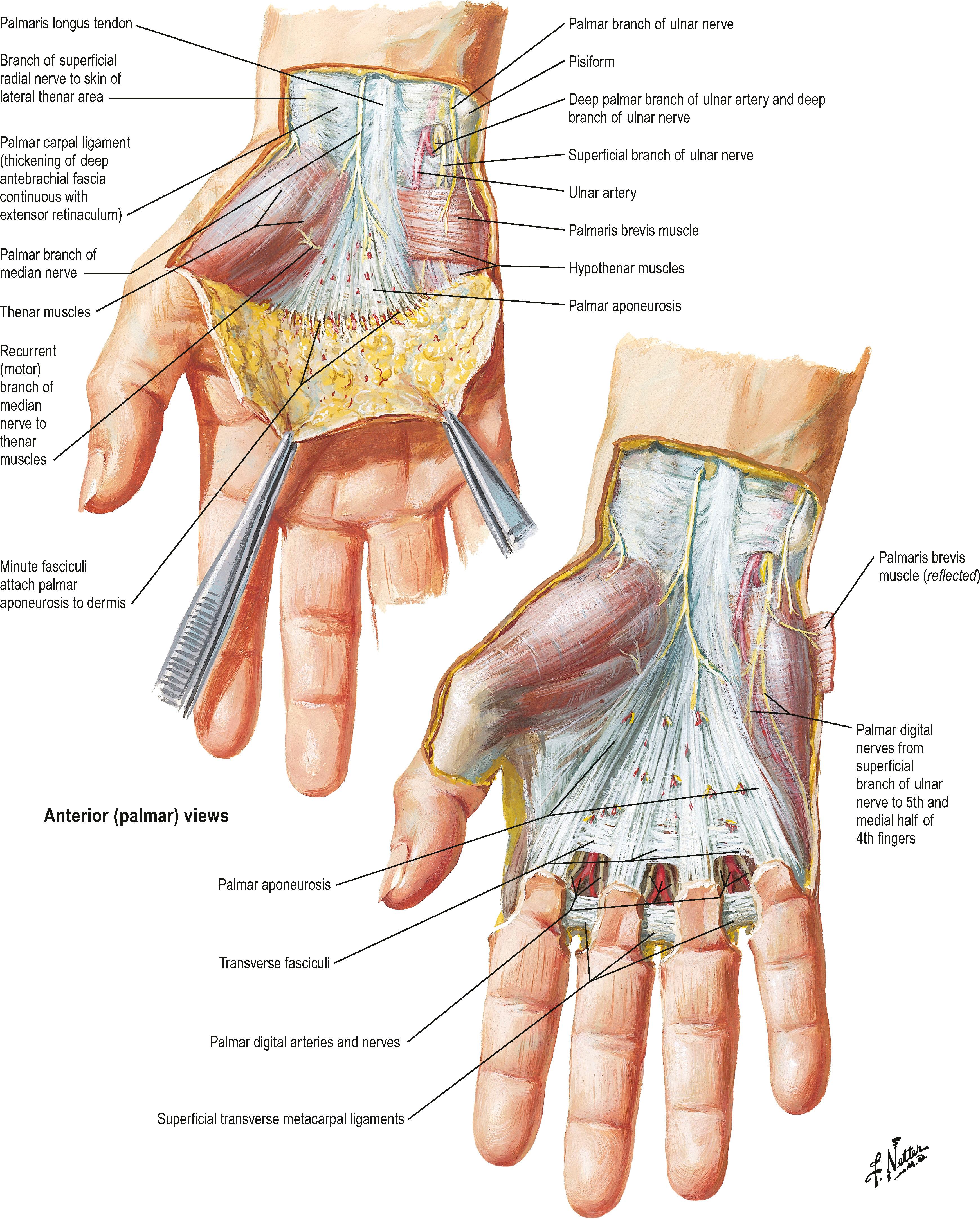
Transverse fibers are concentrated in the midpalm and the webspaces. The midpalmar transverse fibers, although intimately associated with the longitudinal bundles, lie deep to them and are inseparable from the vertical fibers that concentrate into septa between the longitudinally oriented structures passing to the fingers. This system of palmar transverse fibers makes up what Skoog (in 1967) called the transverse palmar ligament. In fact, the transverse fibers form the roof of tunnels at this point that act as pulleys for the flexor tendons proximal to the level of the digital pulleys. Biomechanical evaluation of the palmar aponeurosis pulley has demonstrated that isolated sectioning did not change the work of flexor tendons or load efficiency. Nevertheless, this pulley has been implicated as contributing to the etiology of trigger finger.
Longitudinal fibers pass toward the palmar surface of the thumb, but these fibers are generally less numerous and sometimes difficult to identify. The thumb fibers blend into the deep fascia overlying the thenar muscles. The ulnar extreme palmar fascia blends with the hypothenar fascia. The proximal one-third of this border is the attachment site of the palmaris brevis muscle. Laterally, the muscle attaches to the hypothenar skin and hypothenar fascia.
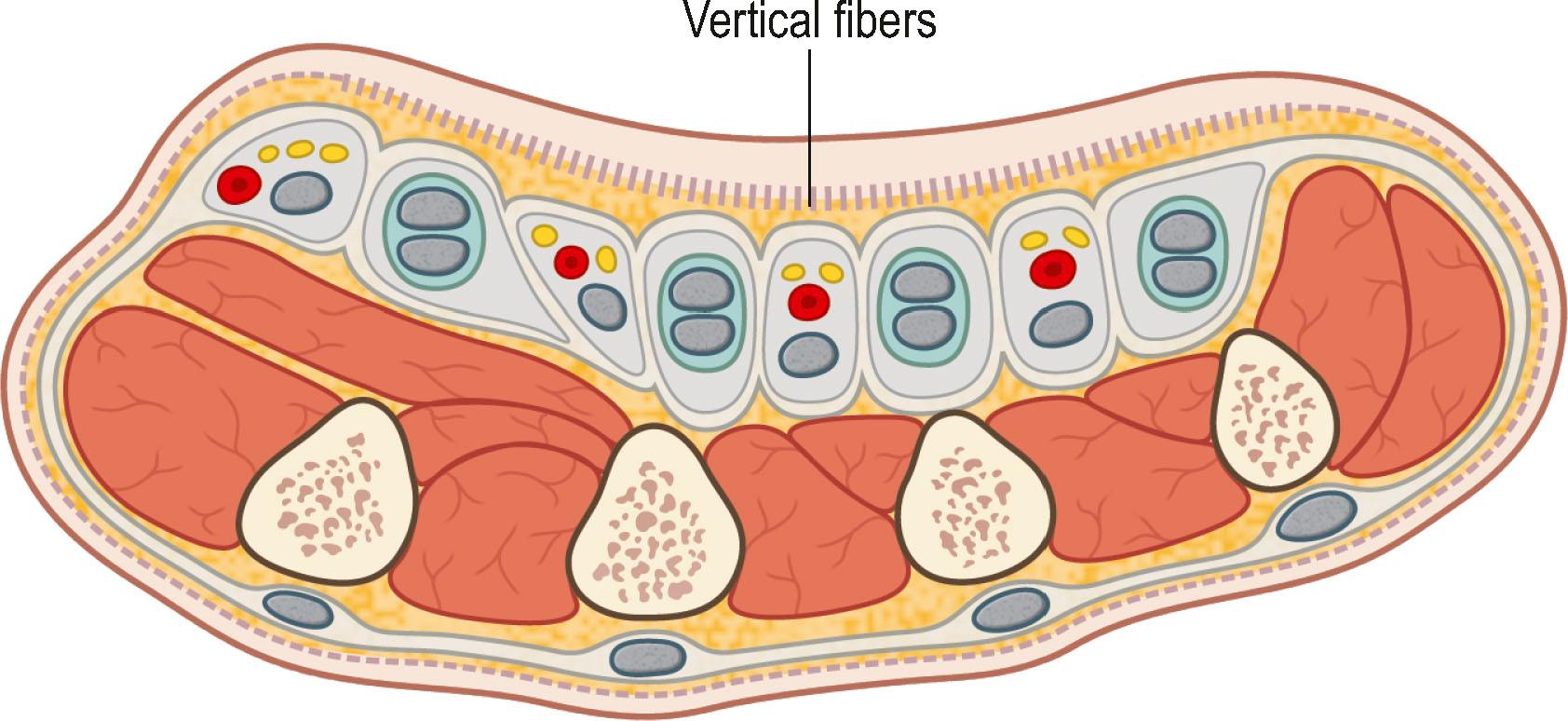
The vertical fibers of the palmar fascia, which lie superficially to the tough triangular membrane made up by the longitudinal and transverse fibers, consist of abundant vertical fibers to the palm dermis ( Fig. 1.4 ). Deep to the palmar fascia, the vertical fibers coalesce into septa, or the “perforating fibers of Legueu and Juvara”, forming compartments for flexor tendons to each digit and separate compartments for the neurovascular bundles together with the lumbrical muscles. There are eight such compartments which extend proximally to about the midpalm. Proximal to this, there is a common central compartment. The marginal septa extend more proximally than the seven intermediate septa closing the central compartment laterally and medially. The major septum between the index flexor tendons and the neurovascular and lumbrical space to the third interspace attaches to the third metacarpal, dividing the thenar or adductor space from the midpalmar space. Knowledge of these vertical compartments aids dissection and identification of structures in operations such as trigger-finger release, sympathectomy, and Dupuytren's fasciectomy ( Fig. 1.5 ).
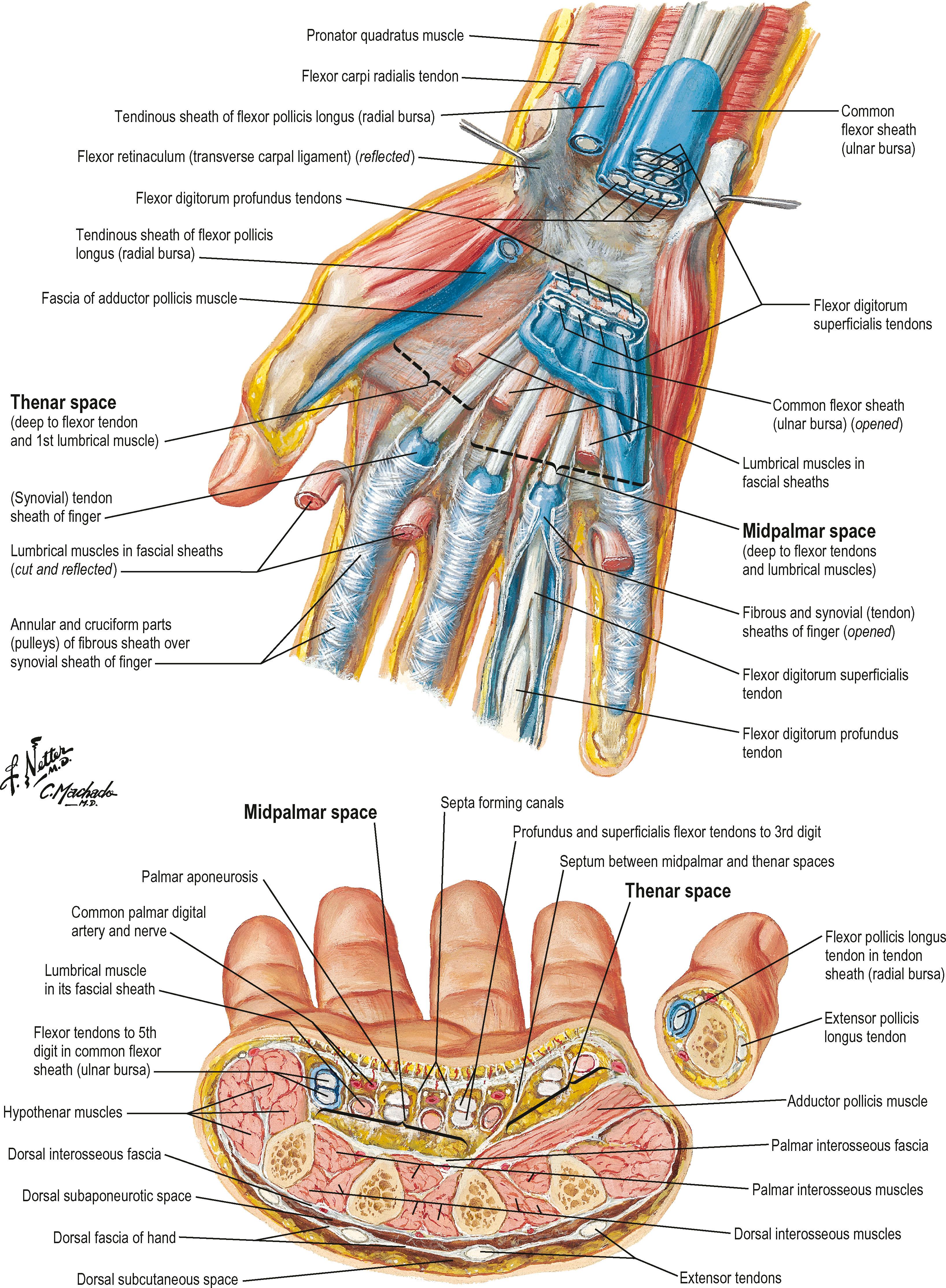
In the fingers, two important bands of fascia are named Grayson's ligaments and Cleland's ligaments. Grayson's ligaments are volar to the neurovascular bundles and are quite flimsy. The much stouter Cleland's ligaments are dorsal to the neurovascular bundles. These two fascial sheets help contain and protect the ulnar and radial digital arteries and nerves ( Fig. 1.6 ).
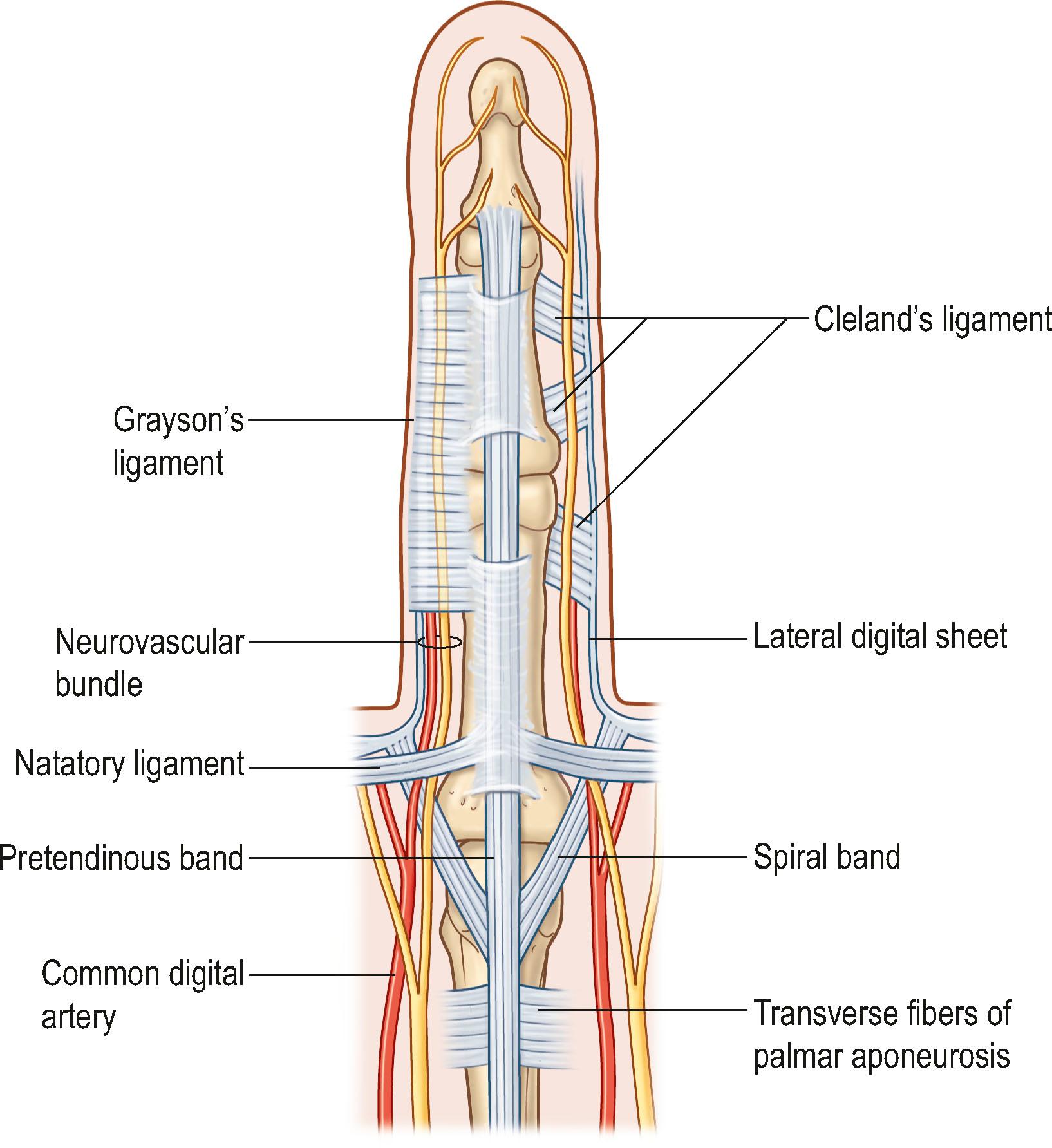
The ability of the hand to resist and create powerful gross action, combined with its capacity to perform intricate fine movements in multiple planes, reflects the masterful construction of its supporting architecture. Reducing the hand to its supporting skeleton and its restraining ligaments reveals the architectural basis for its varied function. A study of the range of joint motions in the hand and forearm with all motor elements removed discloses the full range and limitations that the skeleton imposes on hand function.
The hand skeleton is divisible into four elements:
The fixed unit of the hand, consisting of the second and third metacarpals and the distal carpal row.
The thumb and its metacarpal with a wide range of motion at the carpometacarpal joint. Five intrinsic muscles and four extrinsic muscles are specifically influential on thumb positioning and activity.
The index digit with independence of action within the range of motion allowed by its joints and ligaments. Three intrinsic and four extrinsic muscles allow such digital independence.
The third, fourth, and fifth digits with the fourth and fifth metacarpals. This unit functions as a stabilizing vise to grasp objects for manipulation by the thumb and index finger, or in concert with the other hand units in powerful grasp ( Fig. 1.7 ).
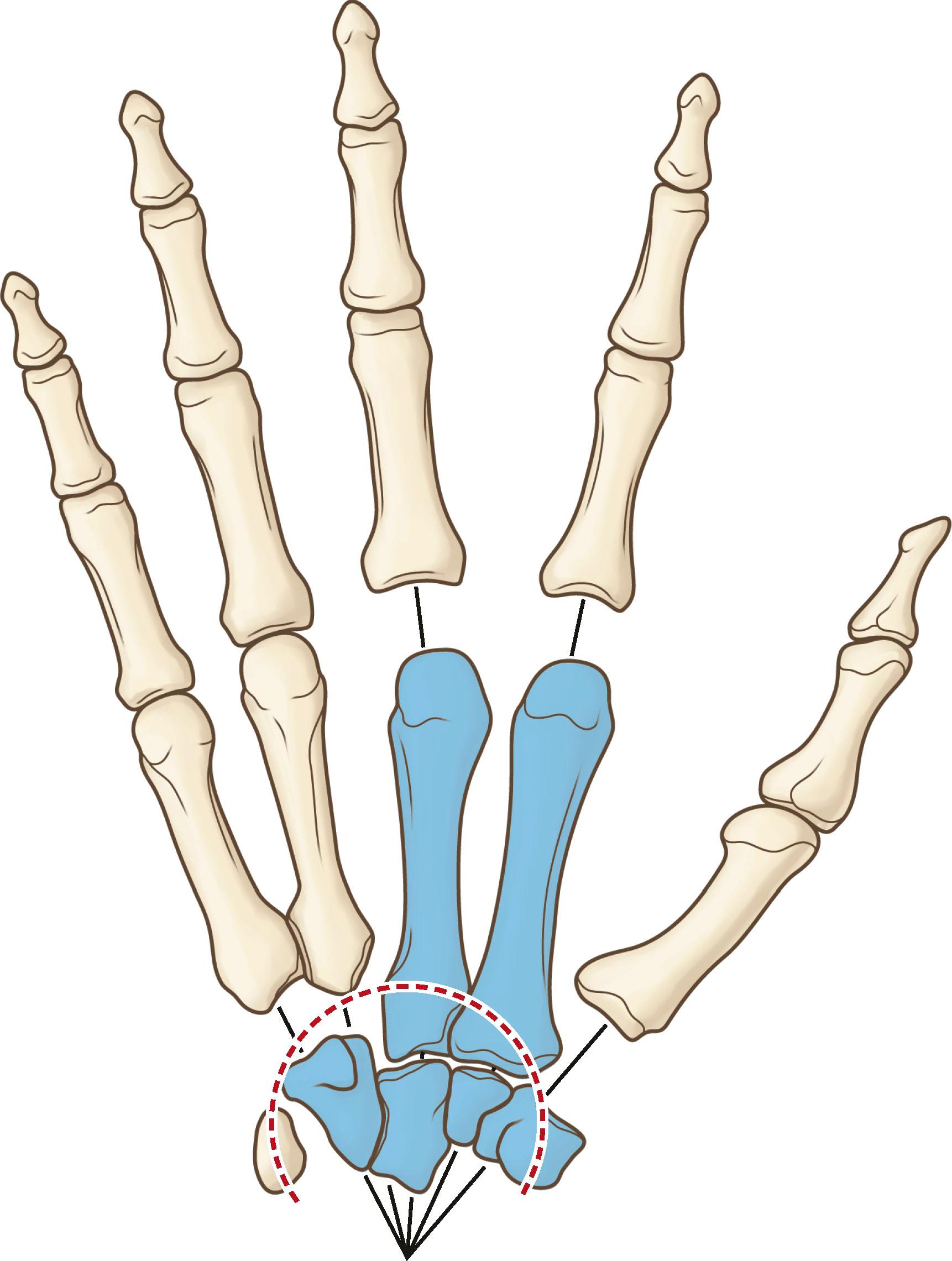
The distal row of carpal bones forms a solid architectural arch with the capitate bone as the keystone. The articulations of the distal carpals with one another, the intercarpal ligaments, and the important transverse carpal ligament (flexor retinaculum) maintain a strong, fixed transverse carpal arch. Projecting distally from the central third of this arch are the fixed central metacarpals, the second and third. Littler called this the “fixed unit of the hand”. It forms a fixed transverse arch of carpal bones and a fixed longitudinal arch created by the anatomic convexity of the metacarpals. As a stable foundation, this unit creates a supporting base for the three other mobile units. This central beam moves as a unit at the wrist under the influence of the prime wrist extensors (the extensor carpi radialis longus and brevis) and the prime wrist flexor, the flexor carpi radialis. These major wrist movers insert on the second and third metacarpals. Thus, the fixed central unit is positioned for activity of the adaptive elements of the hand around it.
The distal row of carpal bones constitutes a fixed transverse arch. At the level of the metacarpal heads, the transverse arch of the hand becomes mobile, which is possible because the first metacarpal moves through a wide range of motion at the saddle-like carpometacarpal joint. The loose capsular ligaments and the shallow saddle articulation between the first metacarpal and the trapezium allow circumduction of the mobile first metacarpal. Its range of motion is checked by these capsular ligaments, including the volar beak ligament, and by its attachment to the fixed hand axis through the adductor pollicis, the first dorsal interosseous, and the fascia and skin of the first webspace. The mobile fourth and fifth metacarpal heads move dorsally and palmarly in relation to the central hand axis by limited mobility at the carpometacarpal joints. These metacarpal heads are tethered to the central metacarpals by the intermetacarpal ligaments. The latter unite adjacent metacarpophalangeal volar plates, which are an intimate part of the joint capsules.
When the head of the first metacarpal is palmar-abducted by thenar muscles innervated by the median nerve, and the fourth and fifth metacarpals are palmar-abducted by the hypothenar muscles innervated by the ulnar nerve, a volar, concave, transverse metacarpal arch is created, approximating a semicircle. The mobile metacarpal heads are pulled dorsally by extrinsic extensor tendons when the thenar and hypothenar muscles relax. It is obvious that a flaccid paralysis of the intrinsic muscles of the hand in median and ulnar nerve palsy will produce a flattened or even reversed transverse metacarpal arch. The active production of a semicircular transverse arch by the thenar and hypothenar muscles creates the proper circumferential arrangement of the metacarpophalangeal joints for convergence of the fingers in flexion. In this position the fingers, flexing at the metacarpophalangeal joints only, converge, forming with the thumb a cone, the apex of which lies over the anatomic center of the hand ( Fig. 1.8 ). A vertical line dropped from the apex of the cone to the center of its base will strike the third metacarpophalangeal joint. This point at the apex of the transverse metacarpal arch is the anatomic center of the hand. With the fingers fully abducted, the tips form radii of equal length from the anatomic center of the hand. The same radius projected proximally falls at the wrist joint.
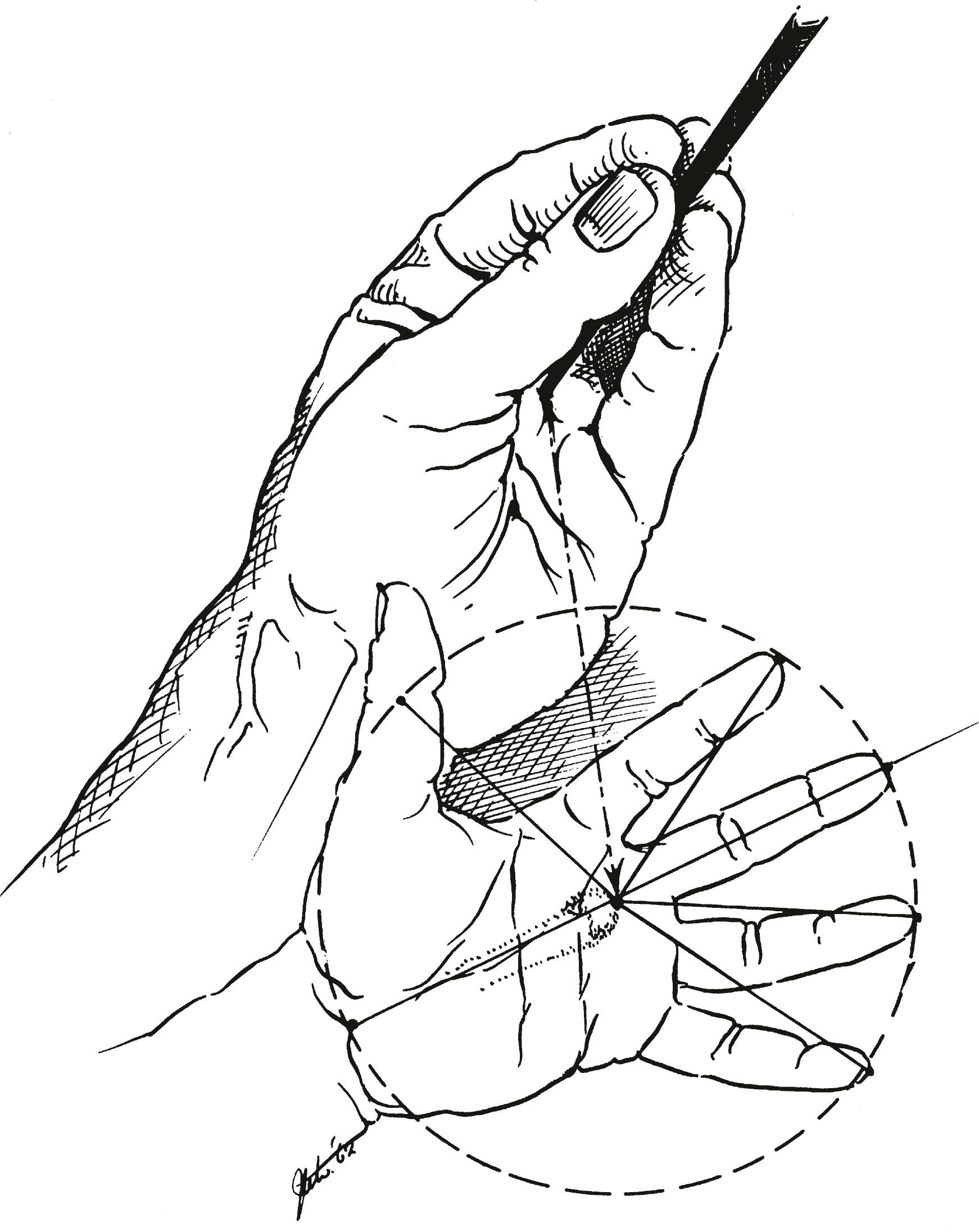
The most important single motor operating the central hand beam at the wrist level is the extensor carpi radialis brevis, which works against gravity, positioning the pronated hand into extension. In the absence of any other motors it pulls the central third metacarpal into extension, making it the apex of the passively created transverse metacarpal arch.
The wrist joint is the site for major postural change between the arm beam and the working hand end piece ( Fig. 1.9 ). It has a multiarticulated architecture that creates a potentially wide range of motion in flexion, extension, radial deviation, ulnar deviation, and circumduction. The distal radioulnar joint allows pronation and supination of the hand as the radius rotates around the head of the ulna. The proximal row of carpal bones (scaphoid, lunate, triquetrum, pisiform) articulates with the distal radius and ulna, providing the ability to flex and extend the hand and perform radial and ulnar deviation. The distal carpal row (trapezium, trapezoid, capitate, and hamate), along with the second and third metacarpals, forms the “fixed unit” of the hand.
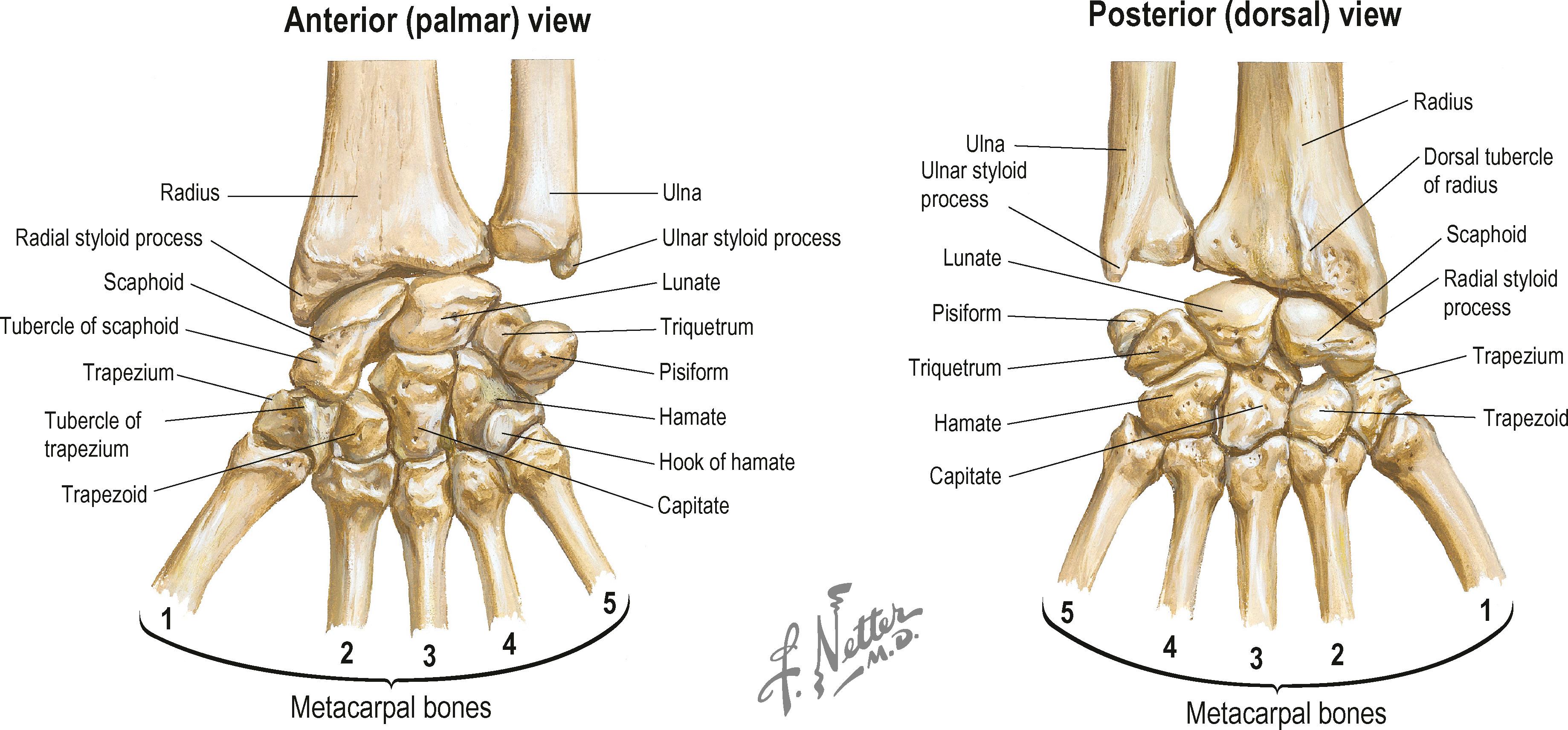
The radiocarpal joint includes the carpal bones and the distal radius ( Fig. 1.10 ). The principal articulation of the carpus is with the distal surface of the radius. The articular surface of the radius slopes in several planes. In the radial-to-ulnar plane, the radius exhibits an average slope of 22°. In the dorsal-to-palmar plane, the articular surface of the radius slopes 12° with the dorsal surface more distal than the palmar surface. Fractures of the distal radius frequently result in a loss of the normal radiocarpal configuration in one or both planes. A loss of the normal dorsal-to-palmar tilt of the articular surface will result in a change in the biomechanical properties of the wrist joint, which may lead to degenerative arthritis.
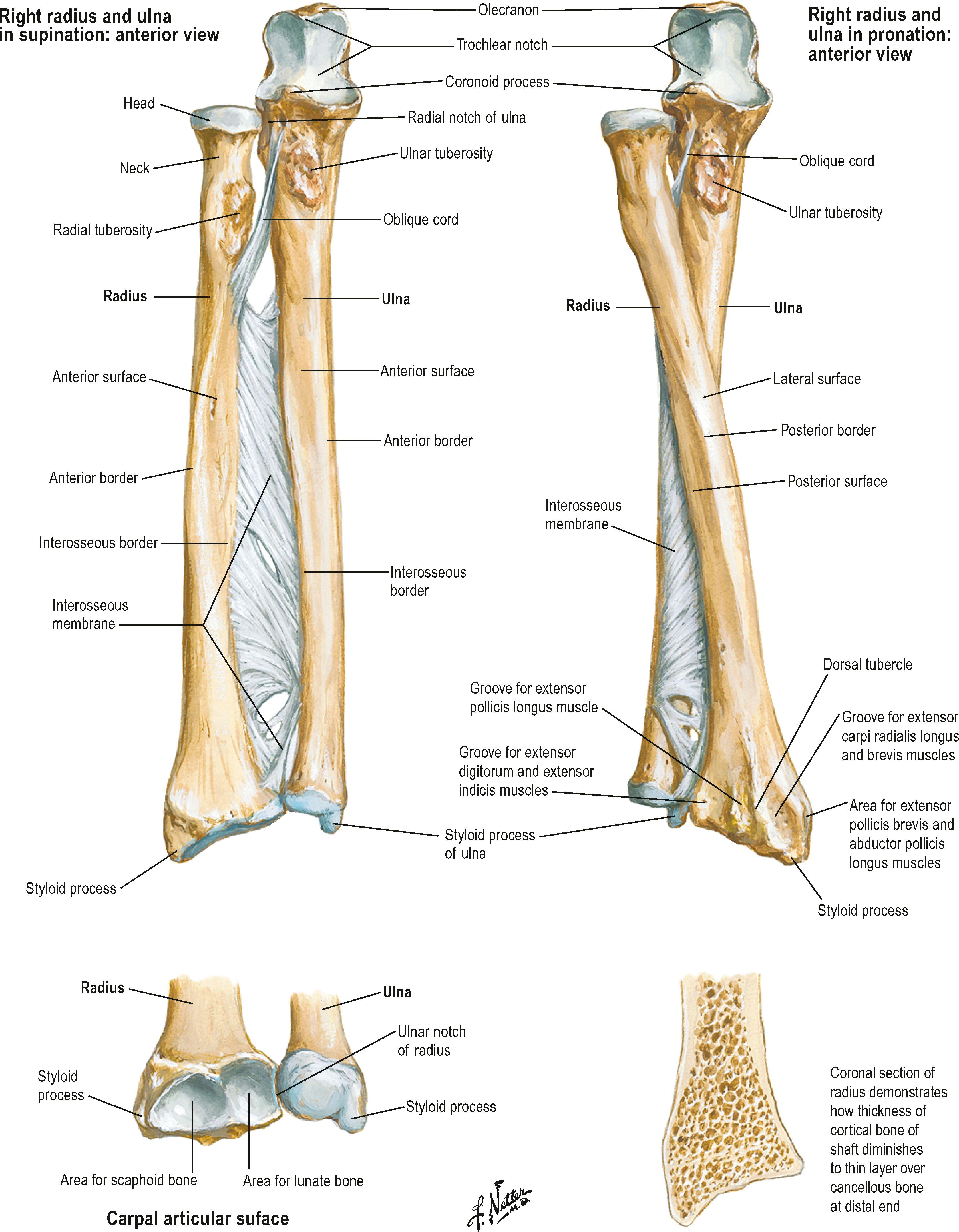
The relationship of the length of the radius to the length of the ulna is fairly constant in individuals and is termed ulnar variance. The distal ulna will complete the curve of the articular surface of the radius. If the end of the ulna falls short of this curvature, the condition is termed ulnar negative variance. If the ulna extends distal to this imaginary extension, the condition is termed ulnar positive variance. Either condition may lead to wrist problems. Ulnar negative variance is associated with a higher incidence of Kienböck's disease, avascular necrosis of the lunate. Ulnar positive variance greater than 2–3 mm is associated with ulnar impaction ( Fig. 1.11 ).
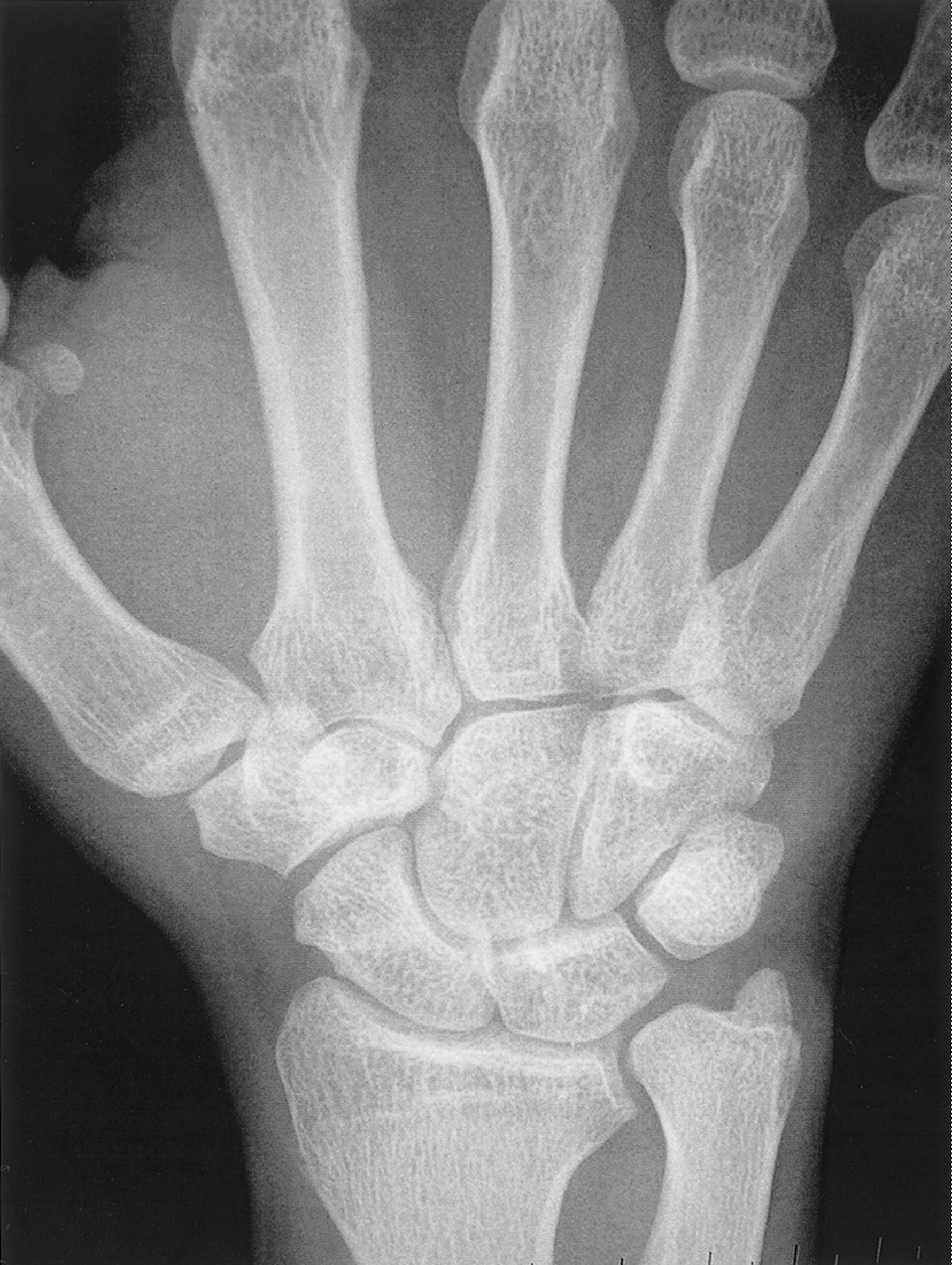
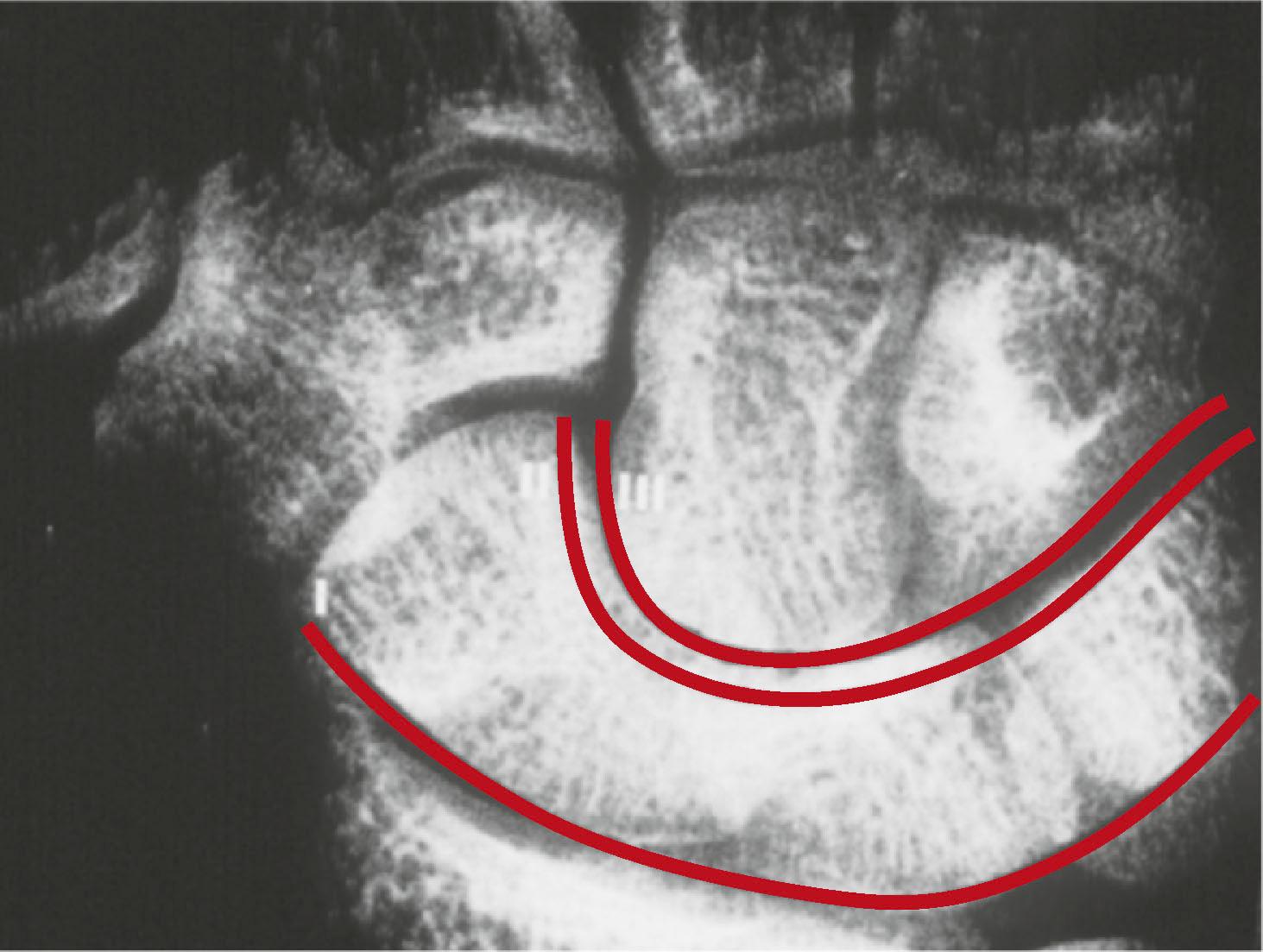
Gilula and others have described several anatomic features that denote normal extracarpal and intracarpal architecture. A line that follows the proximal articular contours of the proximal row of carpal bones circumscribes a smooth arc, termed the greater arc ( Fig. 1.12 ). A disruption in the smooth appearance of this arc is one of the signs of carpal abnormality, such as abnormal rotation of one of the bones of the proximal carpal row, as would be seen with disruption of the scapholunate ligament. Similarly, the joint line between the proximal and distal row of carpal bones circumscribes another smooth arc, termed the lesser arc. The presence of abnormalities in either of these arcs may be an indication of carpal pathology, either acute or chronic.
The scaphoid and lunate bones of the proximal carpal row form the convex articular counterparts of the concave distal radius for the major wrist articulation. In fact, the articular surface of the radius is divided into scaphoid and lunate fossae ( Box 1.2 ). The triquetrum articulates with the lunate in the proximal row, and with the hamate across the midcarpal joint. The pisiform is essentially a floating bone, unimportant for carpal stability.
Investigations by Gelberman and Menon have described two main vessel systems that perfuse the scaphoid via ligamentous attachments. The superficial palmar branch of the radial artery contributes a volar blood supply that feeds the distal scaphoid. The dorsal carpal branch of the radial artery contributes a dorsal blood supply that also primarily feeds the distal scaphoid. Therefore, the proximal scaphoid is poorly vascularized and is susceptible to nonunion after proximal pole fracture.
All four of the bones in the distal carpal row present articular surfaces for junction with the metacarpals. The distal carpal row forms a solid architectural arch with the central capitate as the keystone. The nature of the articulations of the distal carpals with one another, and of the carpal ligament (flexor retinaculum), is such that they make up a strong and fixed transverse carpal arch ( Box 1.3 & Fig. 1.13 ).
The tubercle of the scaphoid is found at the distal flexion crease of the wrist joint, lateral to the tendon of the flexor carpi radialis. It is an important skeletal landmark in evaluating digital malrotations. Normally, each finger points to the scaphoid tubercle when individually flexed. A finger that points away from the tubercle may do so because of destructive flattening of the carpal arch. More commonly, it may result from malrotation following a metacarpal or phalangeal fracture ( Fig. 1.13 ).
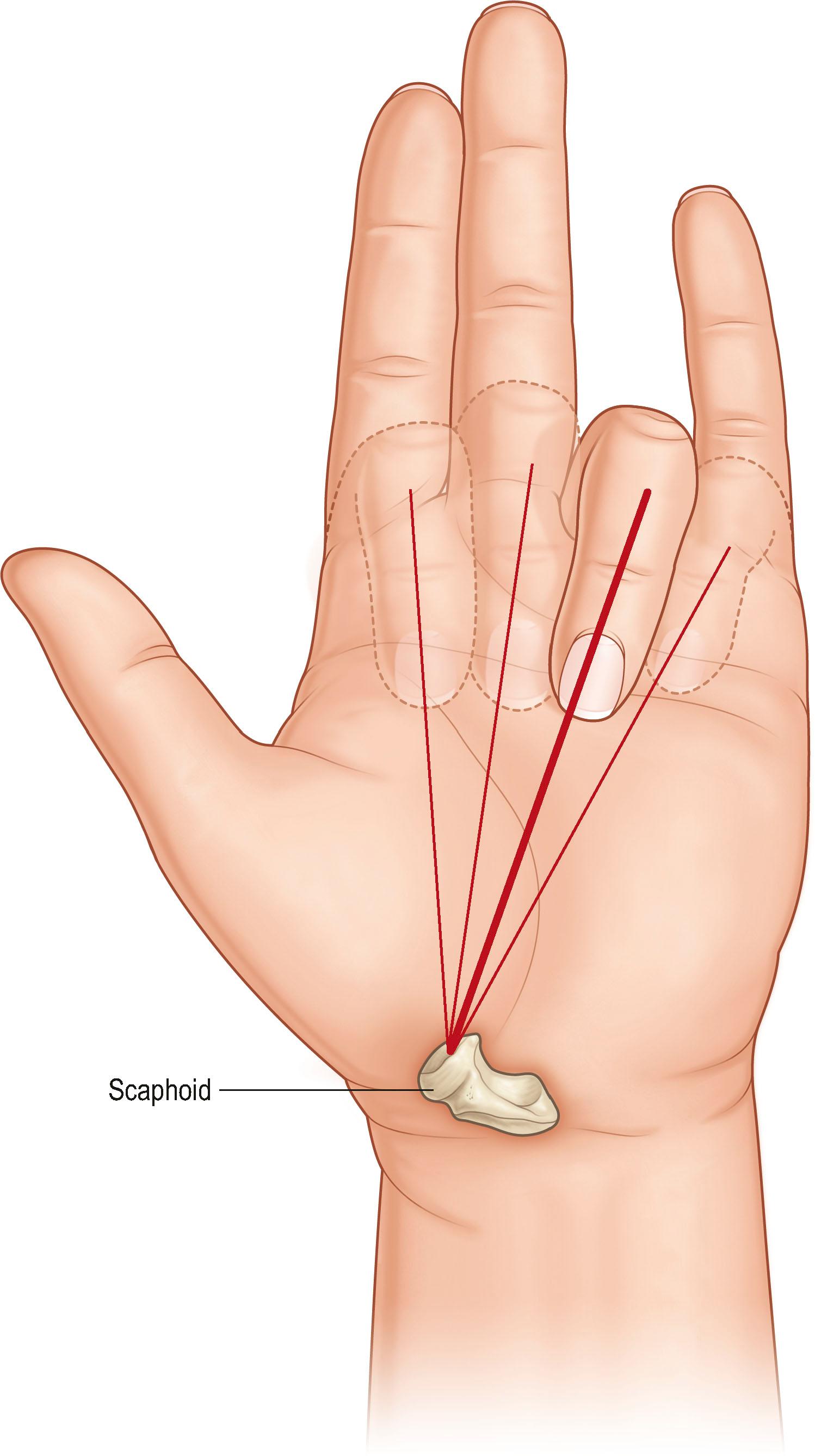
The complex motions of the wrist are a product of the collected movements of the carpal bones in various planes and degrees of rotation relative to one another. The motion of any one carpal bone is a consequence of several factors. The first factor is the contour of the bone and the arrangements of its articular surfaces. The second is the degree of freedom afforded by intrinsic ligaments, which are ligaments originating from one carpal bone and inserting on another carpal bone, and by extrinsic ligaments, which are ligaments arising from the radius or ulna and attaching to a carpal bone or bones. This complex set of ligaments and the shape of the intercarpal and radiocarpal articulations control movement because no muscles arise or insert on any of the carpal bones except for the pisiform. This unique adaptation of nature avoids the need for a thickly muscled wrist and hand unit. It permits great flexibility in positioning the hand in space without the need for sets of muscle agonists and antagonists to control the several degrees of freedom of movement.
The proximal row of carpal bones is anchored to the radius by a series of stout palmar ligaments arising primarily from the radius and by an additional set of stout ligaments arising from the ulna and the palmar portion of the triangular fibrocartilage complex (TFCC). The TFCC separates the distal end of the ulna from the ulnar-sided carpal bones and serves to suspend the distal ulna to the radius at the distal radioulnar joint. These primary extrinsic palmar ligaments take the form of an inverted “V” with its apex pointed distally.
The three most predominant nerves innervating the TFCC are the dorsal cutaneous branch of the ulnar nerve (100%), the medial antebrachial cutaneous nerve (91%), and the volar branch of the ulnar nerve (73%). Other nerves play a minor role in the innervation of the triangular fibrocartilage complex: the anterior interosseous nerve, the posterior interosseous nerve, and the palmar branch of the median nerve.
Dorsally, the extrinsic radiocarpal ligament complex is thinner and is primarily a condensation of capsular tissues, except for two stout structures, the dorsal intercarpal ligament joining the distal pole of the scaphoid and the triquetrum, and the dorsal radiocarpal ligament. According to work by Viegas, these two dorsal ligaments form a unique lateral “V” configuration that allows variation in length by changing the angle of the “V” while maintaining a stabilizing force on the scaphoid during wrist range of motion.
The intrinsic ligaments are broad, stout structures that link one carpal bone to another, either within the proximal or distal row, or linking one carpal row to the other. The two most significant intrinsic ligaments are the scapholunate ligament and the lunotriquetral ligament. The scapholunate ligament anchors the scaphoid to the lunate to allow these two carpal bones to move in synchrony. Berger has subdivided this U-shaped structure into three regions: dorsal, proximal, and palmar. The dorsal region is thick and controls scapholunate stability. The proximal portion, composed mainly of fibrocartilage, and the palmar region, with thin and obliquely oriented fibers, are less important for stability. The lunotriquetral ligament is also composed of dorsal, proximal, and palmar portions. There is less motion between these two carpal bones. Disruption of either the scapholunate or lunotriquetral ligaments may lead to wrist instability because the normal restraints on synchronous motion are removed.
The bony anatomy of the hand is presented in Fig. 1.14 . Normal metacarpophalangeal joint motion in the fingers ranges from 0 to 90°. Lateral activity in the metacarpophalangeal joints is limited by the rein-like collateral ligaments. These ligaments are loose and redundant when the metacarpophalangeal joints are in extension, allowing maximal medial and lateral deviation. As the metacarpophalangeal joint is flexed, the cam effect of the eccentrically placed ligaments and the epicondylar bowing of the collateral ligaments result in tightening and strict limitation of lateral mobility ( Fig. 1.15 ). The fingers that have been fixed in extension during a period of healing have had the stage set for collateral ligament shrinkage and locking of the metacarpophalangeal joints in hyperextension.
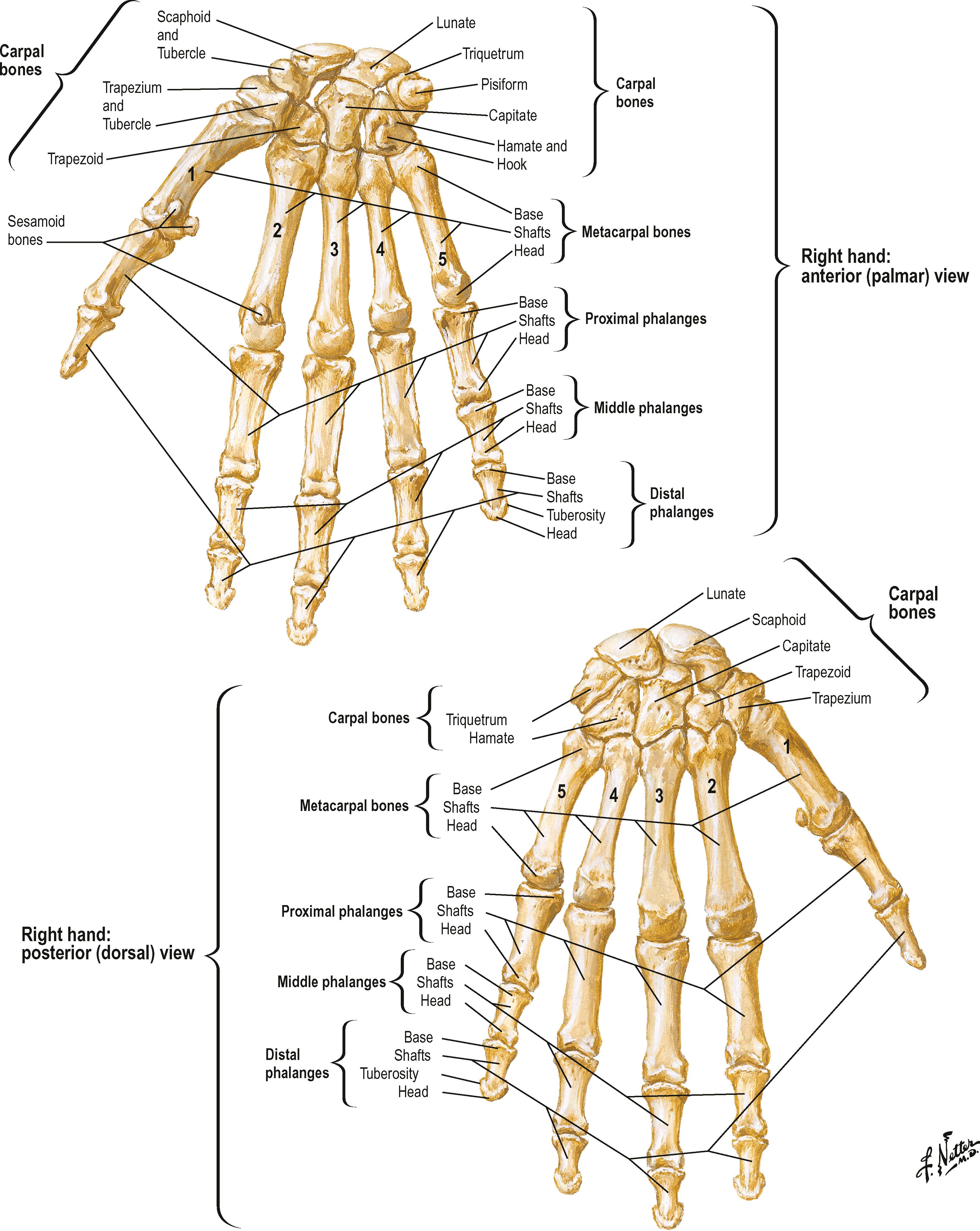
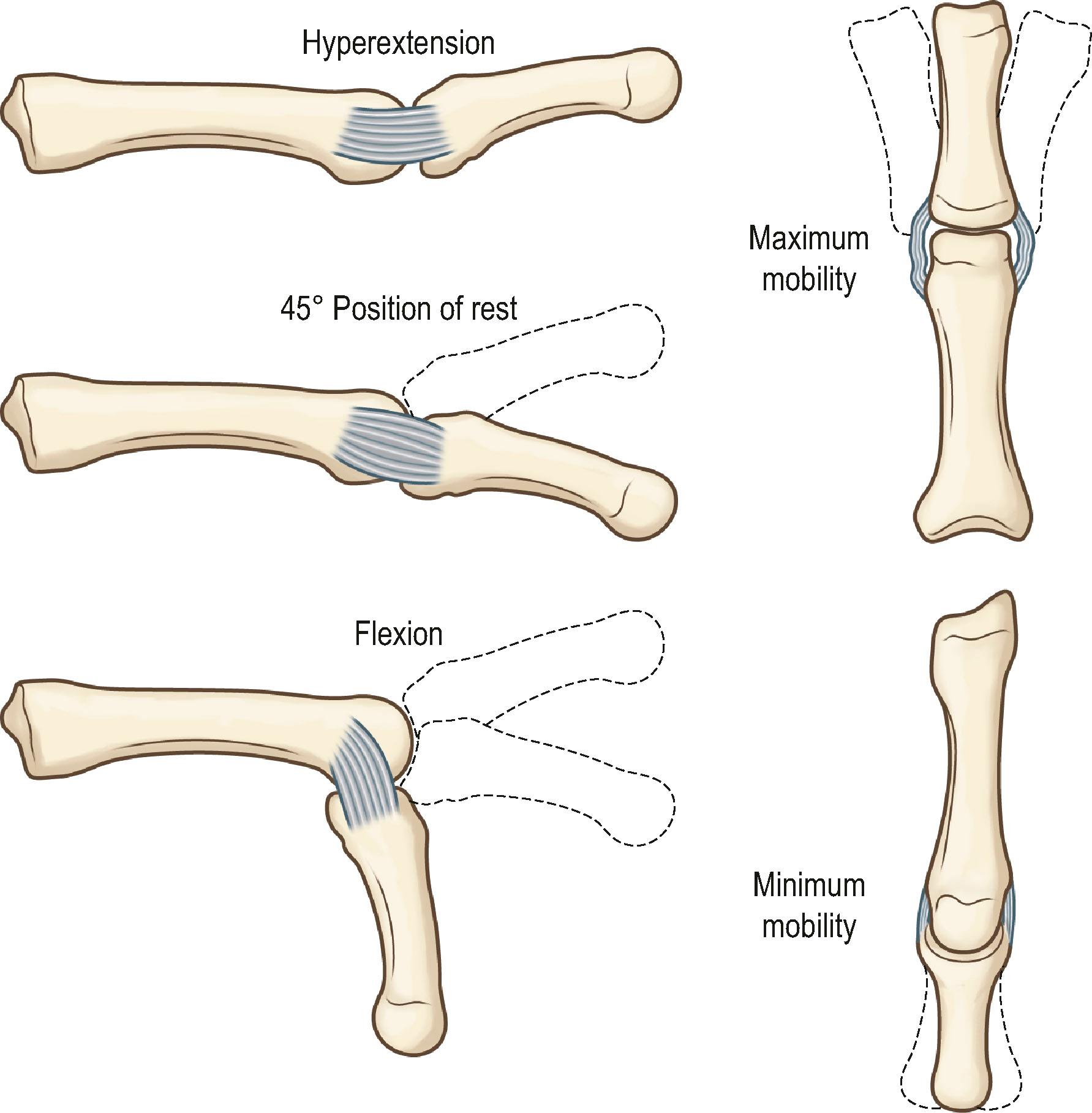
The proximal interphalangeal joint can be pushed to 110° of flexion, but extension usually cannot be carried beyond 5° of hyperextension because of the ligamentous volar plate, which is an inseparable part of the joint capsule. The medial and lateral collateral ligaments are a part of the capsule. They are radially fixed in a manner that allows no medial or lateral deviation of the joint in any position. The shape of the articular joint surface also strongly contributes to this stability in lateral motion.
The distal interphalangeal joints of the fingers can be pushed into about 90° of flexion before they are limited by the dorsal joint capsule and extensor mechanism. The distal interphalangeal joints extend to 30° of hyperextension. There is no lateral mobility in these joints with the collateral ligaments intact. The collateral ligaments of the distal interphalangeal joints are simply thickened medial and lateral portions of the joint capsule.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here