Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Epidemiological studies on sport injuries occurring at the foot and ankle are not consistent and lack uniformity in published outcomes in Brazil. Current literature on sports injuries in the country indicates that soccer is the most frequently investigated and the first source of injury. Research has shown that soccer players have a 1000-fold increased risk of injury compared to industrial workers. Approximately 15.3 million people in Brazil play soccer, which represents 39.3% of all sports practiced in the country. Barefoot sports such as beach soccer and beach volleyball have also been gaining participants due to Brazil’s advanced placements in recent international tournaments.
Among sport injuries, after the thigh, the foot and ankle are the most common locations for injury. In one epidemiological study, severe ankle and foot problems occurred in 33% of the 200 healthy soccer players over 2 years of prospective observation. Direct player-to-player contact (32%) and overuse (26%) are the most commonly cited mechanisms of injury. Of these, by far the most common injuries are sprains (80%) (which includes foot sprains such as Lisfranc lesions), followed by bruises (9%–49%) and tendon lesions (2%–23%). Fractures are rare and account for only 1% of all ankle injuries in soccer. Except for Achilles tendinopathies, which are higher during the preseason, most injuries occur during competition.
Here, we briefly describe some of the most common injuries that are seen in our clinics, including subtle Lisfranc injury, sand-toe, posterior ankle impingement, and loose bodies of the ankle joint.
In athletes, Lisfranc lesions are mostly the result of indirect trauma, occurring as plantar flexion or abduction injuries. Plantar flexion injuries often occur when the player suffers a slide tackle and an axial load is applied to a plantar flexed foot while the toes are dorsiflexed through the metatarsophalangeal (MTP) joints. The ligamentous complex at the tarsometatarsal (TMT) joints usually fails dorsally as rotational forces are applied to the midfoot, with resulting subtle joint subluxation or dislocations. Abduction pattern injuries are also common in Brazil and occur when the forefoot is suddenly abducted relative to a fixed hindfoot, such as in equestrian sports in which riders have their feet stuck in the stirrup and may suddenly be thrown out of the saddle.
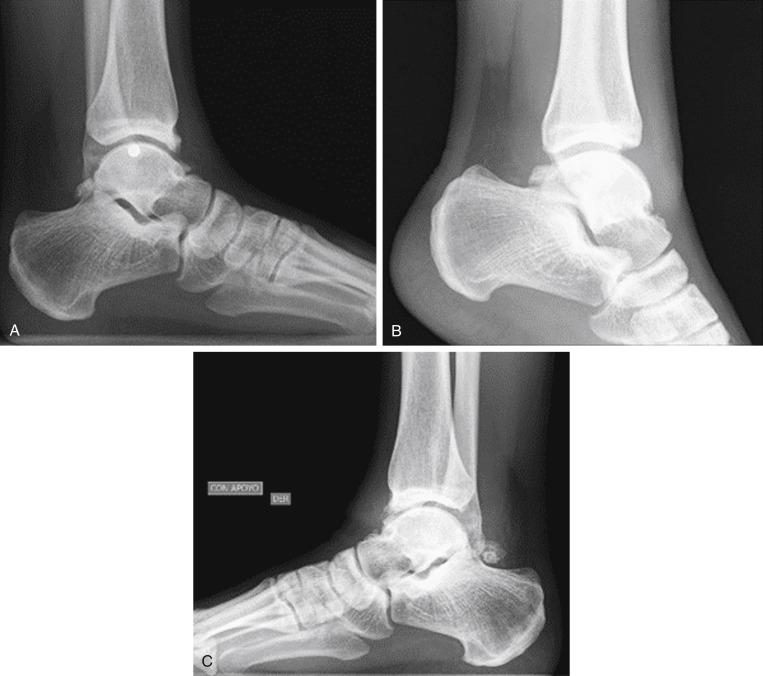
Early diagnosis of Lisfranc injuries is critical to allow for appropriate treatment and a speedier return to play. Misdiagnosis or maltreatment of these potentially career-ending injuries may not only prolong return to competitive play but can also lead to posttraumatic degenerative changes and pain that limit activity and quality of life in the future. Patients with subtle Lisfranc complex injuries may present with varied degrees of swelling throughout the midfoot, though they reliably report pain with attempted weight-bearing activity. Several tests are described, but a high index of suspicion is paramount for diagnosing these injuries. Radiographic studies are critical. If it is too painful for patients to cooperate with adequate standing x-rays, a couple of days of rest or intra-articular local anesthetic can be administered ( Fig. 25.1 ).
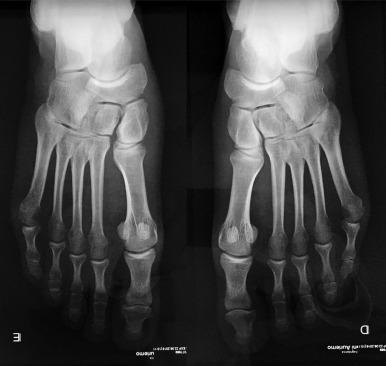
Excellent results have been reported with nonoperative treatment when less than 2 mm of diastasis occurs. However, a low tolerance for displacement should be accepted in elite players, as some recent studies have shown a trend that a surgical approach results in an earlier return to play.
The intraoperative finding of proximal extension of a Lisfranc injury into the intercuneiform area and naviculocuneiform joints is not uncommon. Small intercuneiform diastasis can be misdiagnosed and represents a less stable injury pattern that demands adequate open reduction and internal fixation ( Figs. 25.2 and 25.3 ).
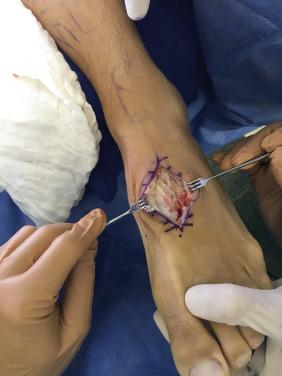
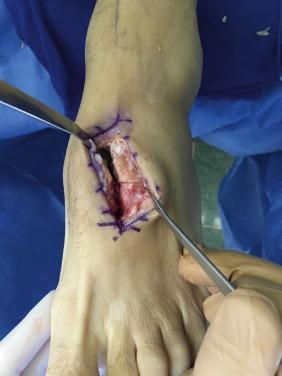
Subtle Lisfranc lesions in athletes are not typically associated with a severe degree of swelling. Therefore, in subtle lesion cases swelling would not limit the ability to proceed with surgery as soon as feasible. The authors generally attempt to avoid penetrating cartilage surfaces at internal fixation up to 3 months after injury. In cases where the initial diagnosis was missed, or treatment is delayed for more than 6 weeks, open reduction of the involved joints is required to remove the thickened scar tissue between the joints, preventing a stable closed reduction. Dorsal bridging plates with or without a C1M2 screw may be a better option for high-impact athletes and contact players ( Fig. 25.4 ).
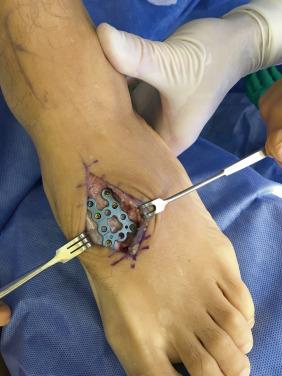
Our postoperative care consists of a below-knee nonweight-bearing boot used for 6 weeks. Foot and ankle range-of-motion (ROM) exercises are initiated at 3 weeks. At 2 months, patients are allowed to wean out of the boot as tolerated. Plates and screws are routinely removed during the fourth month, and patients are permitted to fully weight bear on the limb.
Barefoot sports seem to have a surprisingly low number of injuries, sometimes even lower than the rates for athletes wearing shoes and doing the same or similar activities. For instance, in beach volleyball, injury rates have been found to be fourfold lower during competition on the sand compared to indoors.
Competing barefoot on a sand interface may pose a unique risk for injury that is mainly exclusive to beach volleyball, known as “sand toe.” The mechanism of this injury is a hyper-plantarflexion sprain of the great toe, which usually occurs when the player steps down unsteadily and shifts forward, catching the big toe in the sand ( Fig. 25.5 ). This stresses the dorsal capsule of the MTP joint. This is essentially the opposite mechanism of injury of turf toe. Clinically, athletes present with tenderness at the dorsum of the MTP joint capsule and pain in the same area with toe plantarflexion, which is worse with passive stretching. Active dorsiflexion is not as painful, and strength is typically intact.
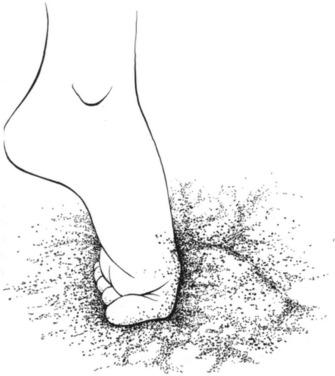
Diagnosis is made clinically, but x-rays should rule out fractures or avulsions. A magnetic resonance image (MRI) should be reserved for severe lesions with likely extensor hallucis longus (EHL) weakness, when dorsiflexion strength does not get better after 6 to 8 weeks.
Treatment starts with taping that is typically continued for the remainder of the competitive season, or until the toe can be plantarflexed passively and fully without pain. On the other hand, rupture of the dorsal hood resulting in EHL subluxation may result in pain that is most pronounced with resisted dorsiflexion and may need surgical repair. In a series of 12 patients, the average player took 6 months to fully recover from the injury. Beach volleyball players will probably benefit most if they do some portion of their rehabilitation on an uneven sand surface, since this is the surface on which they will be returning to play.
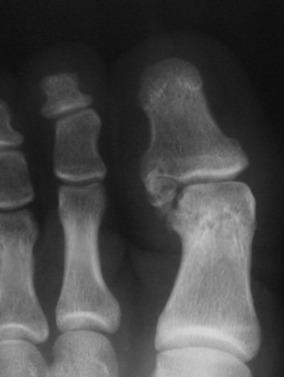
In beach soccer, most injuries occur in the feet and toes (36.4%), followed by the Achilles tendon (18.2%). A specific clinical syndrome characterized by progressive pain and swelling in the dominant (kicking side) hallux MTP or interphalangeal (IP) joints can lead to an osteochondral injury of the hallux ( Fig. 25.6 ). Hyperextension or hyperflexion with repetitive trauma of the hallux MTP or IP joints is the postulated mechanism of injury. Radiographic evaluation can show a marginal, often sclerotic, bony fragment within the lateral or medial aspect of the symptomatic MTP or IP joints. This fragment usually represents marginal osteonecrosis that can be confirmed with MRI. When a symptomatic bony fragment is identified within the MTP or IP joints of the hallux, simple excision has been reported to predictably relieve symptoms.
Posterior ankle impingement syndrome (PAIS) is a clinical disorder defined as a painful limitation of ankle ROM—more specifically, forced plantarflexion—usually caused by repetitive stress. Causes include neurovascular lesions that involve the Stieda process, malunion fractures of the posterior malleolus or talus, os trigonum syndrome, flexor hallucis longus stenosing tendinitis ( Figs. 25.7 and 25.8 ), osteochondral lesions (OCLs), and retrocalcaneal bursitis.
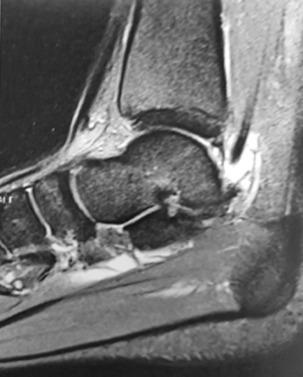
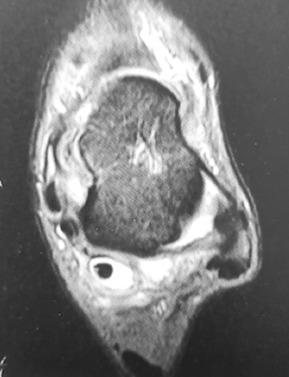
Among soccer players, PAIS symptoms arise more commonly when the soccer player sprints or hits the ball, which results in forced plantarflexion of the ankle. Approximately 60% of conservatively treated athletes show improvement of their symptoms by changing sports habits and wearing braces to limit plantarflexion.
Os trigonum is present in 8% to 13% of the general population and can impinge against the tibia and calcaneus, especially in ballet dancers and soccer players. When symptoms cannot be relieved by conservative measures, athletes tend to compensate the loss of plantarflexion by placing the foot in a suboptimal position in order to diminish symptoms, which leads to further injuries. Therefore, surgical treatment should not be delayed in order to avoid other related lesions ( Fig. 25.9 ).
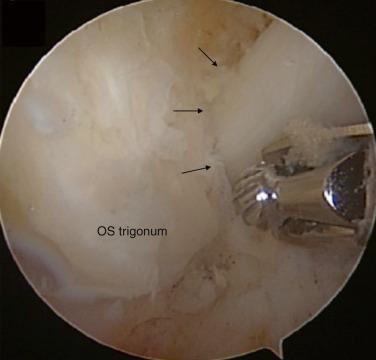
We prefer to endoscopically treat these patients through two para-Achilles portals previously described in the literature, because we believe faster return to play can be achieved. Return to play usually occurs around 40 days. Full weight bearing with crutches is allowed immediately, and after 1 week can be done without crutches or a cane. Sports activity is resumed on their second postoperative week and field training with their respective teams from week 4 thereon.
When resecting the Os Trigonum, one should release all bands involving the flexor halluces longus (FHL), since a constricting effect may arise from scar tissue there ( Figs. 25.10 and 25.11 ).
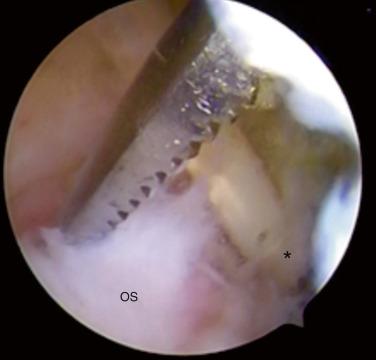
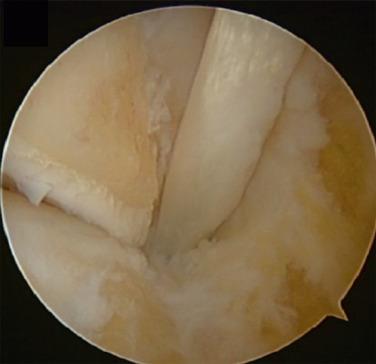
Loose fragments of the ankle joint in athletes usually result from anterior bone impingement with fracture of the anterior osteophytes ( Fig. 25.12 ). The mechanism of loose bodies is related to recurrent ball impact or the repetitive hyper-dorsiflexion, which occurs in high-impact sports, such as volleyball and running. The classic presentation is anterior ankle pain (especially with compression of the soft tissues against the anteromedial aspect of the ankle), restriction of dorsiflexion, and swelling. When fracture of the osteophytes occurs, pain may go away and loose bodies may deposit into lateral or medial gutters.
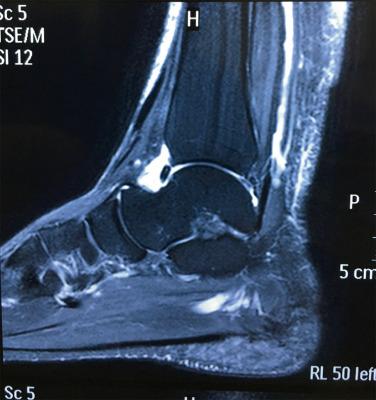
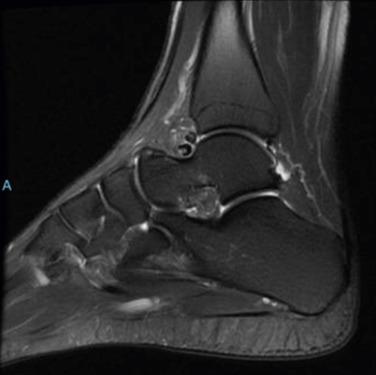
Lateral ankle radiographs reveal osteophytes on the anterior tibia and talar neck (kissing osteophytes). The diagnostic value of an oblique radiograph in addition to a lateral radiograph has been shown. When the lateral radiograph was combined with an oblique anteromedial radiograph, the sensitivity and specificity of the method were high. MRI is useful to rule out any associated soft tissue lesions ( Fig. 25.13 ).
We have a low threshold to maintain athletes in conservative treatment. Arthroscopy is usually indicated when diagnosis is confirmed. Results of ankle arthroscopic soft-tissue debridement and osteophyte resection are good, satisfaction is high (94% to 98%), and the rate of major complications is as low as 1%.
Postoperatively, the ankle is immobilized with a bandage, and partial weight bearing is applied for 3 to 5 days. Full weight bearing is allowed 5 days after surgery, and postoperative rehabilitation is started. Athletes usually return to complete activity after 4 weeks.
Fifth metatarsal stress fractures account for less than 2% of metatarsal fractures in college football players, but can be a source of significant temporary disability and loss of playing time.
Athletes typically report an acute episode of lateral foot pain that, in some cases, follows a 1- to 2-month prodromal history of a lateral foot “ache.” They also often report mild to moderate pain with ambulation but intense, sharp pain at the base of the fifth metatarsal with attempts to run, jump, cut on the involved foot, roll up on the lateral side, or land on the lateral side of the foot.
The mechanism of injury is rarely from a direct blow or crush injury that may occur in actions such as a pileup. Some have described the position of 30 degrees to 50 degrees of foot supination as the most likely position for maximal strain on the fifth metatarsal base. Whether any prodromal symptoms existed or not, the athletes report acute pain in the lateral foot at the metaphyseal-diaphyseal junction of the fifth metatarsal. Commonly, the athlete is unable or lacks confidence to continue full play.
Fifth metatarsal stress fractures typically involve the proximal to mid diaphysis, characteristically occurring more distal than a traumatic base of fifth metatarsal tuberosity avulsion fracture.
Physical examination confirms mild to moderate swelling localized to the lateral midfoot and sharp tenderness at the base of the fifth metatarsal. It is important to examine the athlete, both sitting and standing, to assess the full lower leg alignment, especially the hindfoot and midfoot alignment. Cavus midfoot or varus hindfoot can be present but is not uniform. More recent studies have demonstrated an everted rearfoot and inverted forefoot alignment were associated with fifth metatarsal stress fractures.
Weight-bearing anteroposterior (AP), lateral, and oblique radiographic imaging of the involved foot is mandatory. Additional specialty imaging, such as a bone scan, MRI, or computed tomography (CT), is used in unique circumstances.
Radiographic and MRI findings of fifth metatarsal stress fractures include features of both diaphyseal (cortical-predominant) and metaphyseal (trabecular-predominant) stress fractures given its location at the junction of the metaphysis and diaphysis. Initial radiographic findings include periosteal reaction, with the degree of intramedullary sclerosis increasing in healing and chronic fractures. Important prognostic findings include the presence of a plantar gap at the fracture site, which is associated with poorer healing. MRI demonstrates periosteal and intramedullary edema, with a cortical fracture line evident in higher-grade injuries.
Significant medical workup for athletes with Jones fractures is not routinely needed. However, vitamin D deficiency, low calcium intake, and general nutritional evaluation are helpful in athletes at all levels. Vitamin D deficiency has been shown to occur in up to 50% of Division I athletes and is noted in some studies to be higher in African American populations.
In the female athlete, a history of menstrual cycle irregularity should be investigated, as low estrogen and other hormonal imbalances may lead to a higher risk of delayed unions or nonunions. Dual-energy x-ray absorptiometry (DEXA) scan evaluation is reserved for the athlete with multiple stress fractures or recurring nonunions, as well as the middle-aged and older athlete. Newer-technology DEXA scanning allows for a more detailed evaluation of trabecular bone abnormalities despite normal, generalized bone.
Fractures of the proximal fifth metatarsal that occur in the proximal diaphysis (greater than 1.5 cm from the tuberosity) have an increased risk of poor healing, which is believed to be due, at least partially, to the relative lack of blood supply of the proximal diaphysis. In contrast to the metaphysis, which is supplied by a rich network of metaphyseal arteries, the proximal diaphysis is supplied by a sole nutrient artery, which may be disrupted in proximal diaphyseal fractures.
In a recent review of the literature, it is described that operative treatment of fifth metatarsal stress fractures results in a smaller number of delayed unions or nonunions, compared to conservative treatment. Also, the goals of early surgical management are to minimize the risk of nonunion and recurring fracture, and to decrease the time to return to sport. Foot anatomy must be taken into consideration, and additional procedures such as the lateralizing calcaneal osteotomy for a cavovarus foot should be considered.
Internal fixation with a solid stainless-steel IM screw has become the procedure of choice. The patient is kept nonweight bearing for 3 weeks; then partial weight bearing is allowed with a removable boot, and stationary bicycle and pool therapy is initiated. Transition to full weight bearing begins at 5 weeks. In general, return to activity is allowed 2 months after surgery, depending on the resolution of pain and radiographic evidence of healing.
The Andes Mountains is the world᾽s longest mountain range extending from north to south for 4498 miles across seven countries: Venezuela, Colombia, Ecuador, Peru, Bolivia, Argentina, and Chile. The chain has an average height of 12,000 feet and a width of 149 miles, giving shape to the landscape and scenery of most of western South America.
Providing a stunning backdrop to almost the entire Chilean territory, the Andes mountains contribute with approximately 3000 miles of natural border running down from the arid Atacama Desert to the Glaciers of the Patagonia. The above, added to the narrowness of Chile᾽s geography, makes the mountains accessible from almost every point of the country and usually can be planned as a day trip from almost every major city. This unique feature facilitated since the 1930s the development of numerous ski areas and world-class resorts throughout the central and south regions, being the firsts of their kind in South America and making Chile nowadays an internationally renowned winter sports destination ( Fig. 25.14 ).

Skiing and snowboarding are the most popular activities during the regular winter season that runs usually from May until October. These sports have been growing in popularity among the Chilean population during the last 20 years, as they are more accessible and are no longer perceived as elite activities. Professional skiing has also seen great advances in the current decade with consistent World Cup and Olympic participation ( Fig. 25.15 ).

Injuries affecting skiers and snowboarders have been widely described. The most common injuries in skiers involve the knee, specifically the anterior cruciate ligament and medial collateral ligament, with a prevalence reported between 27% and 33% of all injuries. On the other hand, snowboarders usually sustain upper extremity injuries especially involving the wrist and shoulder, corresponding to almost 20% of all injuries.
Foot and ankle injuries are far less frequent in these disciplines. Nevertheless, there are several sport-specific injuries in this category presenting unique characteristics that physicians in charge of these winter sports athletes must consider for prevention and adequate treatment.
The basic modern skiing equipment considers the use of a boot-binding-ski system. This spring-actuated mechanism attaches the boot to the ski in a fixed position until the bindings are released in response to torsional and upward forces ( Fig. 25.16 ). Release is determined by the spring tensions in two adjustable toe and heel pieces. A significant decrease in foot and ankle injuries during downhill skiing has been evidenced after the 1970s due mainly to the breakthrough of better-designed and -engineered ski boots and binding systems, transmitting the torque forces more proximally in the lower limb. These advances also included improved materials for harder boot shells and weight/height-specific bindings that optimize the detaching process following falls and twisting forces.

However, the current popularity of snowboarding has meant an increase in foot and ankle injuries due to the use of softer boots that allow better control and maneuverability ( Fig. 25.17 ). In line with this trend, there are several studies showing that 12% to 38% of snowboarding lesions are ankle-related, in comparison to only 1.7% to 6% of all skiing injuries. Several different types of boot-binding combinations exist nowadays, but the most commonly used is a soft “pack-type” boot, with a nonreleasable strap binding. Although less popular, hybrid and hard ski boots are also used with either releasable or nonreleasable bindings. Kirkpatrick and collaborators compared snowboarding injuries of the foot and ankle in relation to the type of boot used (soft, hybrid, or hard) and found no significant correlation between boot type and overall injury rate. Nevertheless, in their study, hard boots appeared to be protective for ankle fractures not involving the lateral process of the talus (LPT).

Ankle sprains and fractures are the most prevalent injuries of the foot and ankle segment reported both in skiers and snowboarders. Differential diagnosis is crucial in patients sustaining an ankle sprain in this context, especially because there are similar clinical findings on fractures of the LPT or peroneal tendon injuries that can be easily misdiagnosed.
The most frequent mechanism of fractures of the lower leg and ankle usually involves a fall in skiers, while a greater proportion of snowboarders has jump-related injuries. Concerning the level of injury, skiers present most commonly with oblique or spiral distal tibial fractures at the edge of the skiing boot, or “Boot-Top-Fractures.” On the other hand, malleolar fractures are more common among snowboarders, with isolated fibula fractures almost exclusively seen in this discipline. Ishimaru and colleagues reported that most ankle fractures in snowboarders were supination-external rotation type II injuries as described by the Lauge and Hansen classification.
Pilon fractures are common in the context of vertical impact and axial load, especially in skiers landing from a high-altitude jump. Energy tends to dissipate when the athlete lands on a slope and then continues in a downhill direction. In cases where the landing is effected on a flat surface, the energy is not capable of dissipating, and this can result in a tibial plafond injury.
Management of these injuries is no different from lesions occurring outside of the ski/snowboard context. Emphasis should be on rehabilitation and complete healing of the fracture site with a period of at least 12 weeks following open reduction and internal fixation before returning to practice.
Fractures of the LPT are a specific type of injury that was rarely seen before the snowboard era but has become more prevalent mimicking snowboarding popularity, which has contributed to its current name, “Snowboarder´s fracture.” Kirkpatrick in his series reported a talar fracture incidence of 17% within all snowboarding injuries around the foot and ankle. LPT fractures were particularly high, accounting for almost 95% of these injuries.
The LPT is a wedge-shaped prominence that comprises the most lateral aspect of the talar body, being part of the talofibular and subtalar joints and serving for various ligamentous attachments.
Even though the mechanism of injury is controversial, the most common accepted explanation for LPT fractures is an axial impaction in dorsiflexion with the hindfoot in inversion and in an externally rotated position. This axial impaction is typically seen after landing from a height in snowboard jumping.
In 1965, Hawkins described three types of LPT fractures :
Type I, Simple (42%): Extends from the talofibular articular surface and the posterior subtalar facet.
Type II, Comminuted (34%): Involves both articular surfaces and the entire lateral process.
Type III, Chip (24%): Normally compromising only the subtalar joint, variable size.
Clinical presentation resembles an ankle sprain and may result in pain and disability if not recognized and treated, especially because up to 41% of LPT are missed on initial presentation. Typically, there will be local ecchymosis, edema, and tenderness to perifibular palpation, with variable weight-bearing ability. ROM can be limited by pain, though deformity is usually not seen in these kind of injuries.
Imaging study includes x-rays to rule out other more prevalent injuries such as ankle fractures. LPT fractures can be identified more clearly on the Mortise view. However, there is a general agreement that the best diagnostic accuracy is obtained with CT-Scan, allowing classification of the type of fracture and assessment of articular involvement, thus guiding the treatment plan.
Treatment of LPT fractures is guided by the topographical Hawkins classification and the amount of displacement involved. Valderrabano proposed a treatment algorithm based on their series of 20 cases. Large displaced fragments (type I) should be surgically treated in order to restore articular congruity and diminish long-term morbidity ( Fig. 25.18 ). For nondisplaced fragments, a nonsurgical approach can be made but with a higher risk of future morbidity. For type II and III, treatment depends on the amount of displacement; nonoperative management if no displacement is seen, and surgical debridement if there is any displacement. In general, this approach appears to be reasonable and is accepted by the vast majority of authors.
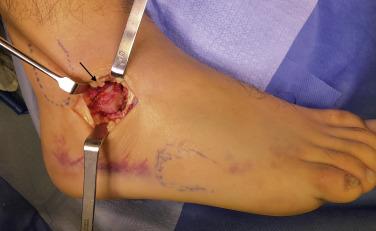
Outcomes for type I fractures treated operatively, regardless of the method of fixation, are fairly good. Perera and colleagues reported that 88% of their patients presented mild or no symptoms during follow-up. On the other hand, up to 38% of the patients treated conservatively persist with moderate or severe symptoms. 42 Poor prognosis has to be expected if diagnosis is missed initially, which is a common reason for nonsurgical treatment. For patients with continued pain and morbidity, depending on the type of fracture, excision or articular fusion may be indicated. Common complications include chronic pain, nonunion, ankle instability, and subtalar arthritis.
Erroneously classified as a neuroma, this entity is one of the most common causes of metatarsalgia. Morton᾽s neuroma is an entrapment neuropathy causing an interdigital neuralgia secondary to perineural fibrosis. This condition is frequent in skiers, in relation to narrow hard boots producing increased pressure on the forefoot. This leads to traction of the interdigital nerves, which subsequently produces perineural fibrosis. Other factors influencing the condition is repetitive trauma and stresses over the MTP joints producing swelling of underlying metatarsal bursa and causing greater compression of the interdigital nerve against the intermetatarsal ligament.
Clinical features include pain and tingling at the involved web space. Numbness may be present. Patients often describe a shooting electrical sensation during or after skiing that usually alleviates by taking the boot off. Ultrasound and MRI examination have been described to confirm the diagnosis. However, clinical findings still have the highest accuracy for Morton᾽s neuroma diagnosis.
Conservative treatment options include ski boot modifications, inserts to reduce pressure beneath the metatarsal heads, or lidocaine/steroid injections. Surgical excision is indicated with persistent symptoms and has been shown to have between 70% to 85% success in literature.
Skier᾽s toe or subungual hematoma is produced by excessive compression of the toes against a narrow boot or by a repetitive trauma of the affected toe secondary to a loose boot. The most affected toe is the hallux, and patients usually complain of progressive pain due the increased pressure produced by the hematoma on the nail bed.
Another factor related to skier᾽s toe is improper skiing technique. Sitting back on the skis forces the toes against the roof of the boot, while maintaining forward pressure on the shins diminishes this pressure on the toes. Long toenails also act as a lever, increasing pressure on the respective toes. We recommend keeping toenails short when skiing or snowboarding in order to avoid this complication.
Treatment of the subungual hematoma includes conservative measures such as applying ice and nonsteroid antiinflammatory drugs (NSAIDs). In cases of persistent pain or complete involvement of the nail bed, aseptic fenestration of the nail to drain the hematoma is indicated.
Chilblains, or pernio, is an injury that develops with prolonged exposure (1 to 5 hours) to frigid or near-freezing temperature. This condition appears as erythematous, well-defined, and tender papules typically on the hands or feet of susceptible skiers and snowboarders.
Treatment involves removing wet clothes or constrictive boots, gentle washing and drying of the area, and covering the skin with dry and loose clothing. Nifedipine may decrease pain and accelerate resolutions of symptoms.
There are many traditional sports and performances that are still popular in China at present, such as shuttlecock kicking ( Figs. 25.19 and 25.20 ), flipping in various Chinese local operas ( Figs. 25.21 and 25.22 ), and the Chinese martial art “wushu,” which is also called Kung Fu ( Figs. 25.23 and 25.24 ). Usually, the Chinese do traditional sports for health purposes and personal fulfillment. Thus there are infrequent opportunities for the traditional Chinese sports to be competitive. However, it is not unusual to see foot and ankle injuries caused by these traditional sports in clinic. Soft-tissue injuries are much more common than a real fracture.






The most common reason for the shuttlecock players suffering a foot or ankle injury is players performing a trick. When there is uneven ground, there is more likely to be an accident. Ankle sprain occurs and may lead to chronic ankle instability several years later. Furthermore, injury may occur as a result of increasing body weight or decreasing strength of the ligament. Flipping is often performed in many kinds of traditional local Chinese operas. This maneuver is more skillful and always performed by professional actors. Since the calf contracts suddenly and strongly when doing this, Achilles tendon injury (partial or complete rupture) may occur. Chronic injury is seen in Chinese wushu players when they continue to practice wushu exercises for decades after a primary injury.
There are many different kinds of foot and ankle injuries caused by these traditional Chinese sports and performances, including ankle sprain, fifth metatarsal avulsion fracture, Achilles tendon rupture, diastasis of syndesmosis, MTP joint capsular injury, instability of the ankle, and medial and lateral malleolus fracture.
Many Chinese believe in traditional treatment and traditional medicine when they have foot and ankle problems. There are some special, traditional treatments for soft-tissue injuries of the ankle joint in China that have a long history. These treatments include acupuncture, Chinese herb ointment, poultices, foot massage, and so on ( Figs. 25.25 through 25.28 ).

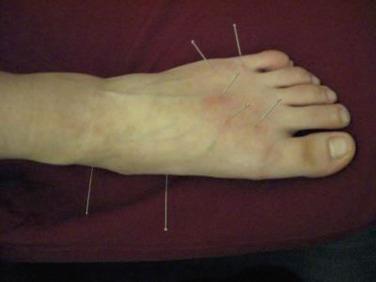

Chinese herb ointment and sometimes a semirigid splint made of bark are the usual management modalities for soft-tissue injury in the early stage. Chinese herb ointment can decrease the swelling effectively and quickly. Poultices, acupuncture, and massage, accompanied by functional exercises, are the treatments for subacute injury.
Acupuncture and massage are important components of restoring balance to the person’s vital energy channels, which form the basis behind traditional Chinese medicine. The channels are a system of conduits throughout the body that carry and distribute “Qi,” which can be considered as vital energy. Disease is present when the flow of vital energy through the channels is disrupted. This may occur when the integrity of the channels themselves is damaged by a sprain. The Chinese describe this as a disease of “Bi,” or pain, caused by a localized disruption to the flow of “Qi.”
The traditional Chinese explanation for soft-tissue injury is that the channel running through the damaged tissue has been physically disrupted, resulting in local pain, a disease of “Bi.” To treat the pain, the integrity of the channel and the flow of vital energy through the channel must be restored. This can be achieved by the selective use of points on the damaged channel, thereby restoring the flow of “Qi” and relieving the pain.
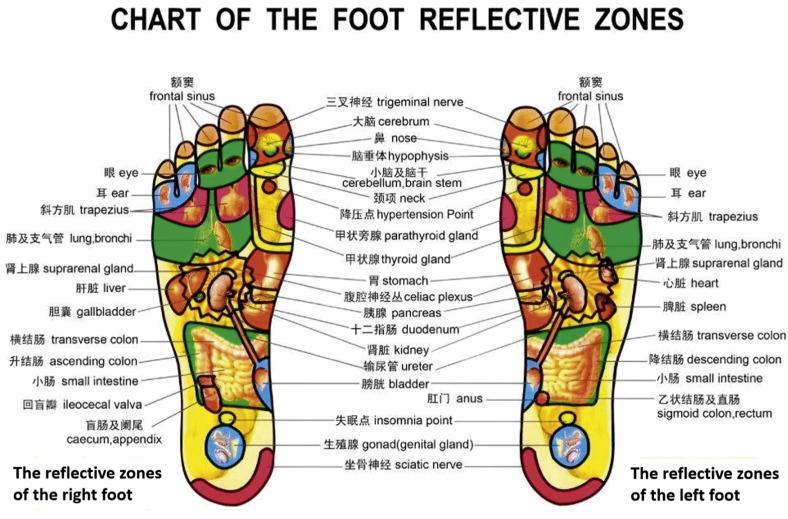
The foot plantar surface is an important place for the body because there are many points of channels, which represent many internal organs. Therefore foot massage not only treats the injury of foot but also can treat diseases anywhere in the body. In China, foot massage is looked on as a good method for preventing and treating diseases and is popular throughout the whole country.
Foot massage is used to stimulate the points of the channels that can activate the gates of the body, which are opened and closed to adjust circulation in the channels. Foot massage has four functions: it can enhance the blood circulation, so as to accelerate the metabolism of the body ; it can regulate the nervous system; because there are many nerves endings in the foot, one can stimulate the reflex zone of the foot to regulate the corresponding tissues and organs ; it can mobilize “Qi,” moisture, and blood and promote proper function of the muscles, nerves, vessels, glands, and organs ; and it brings the efficacy of release and relaxation.
Chinese traditional treatments for acute foot and ankle injury are similar to modern treatments in some aspects, such as rest, relieving the pain, and diminishing the swelling. The treatments of acupuncture and foot massage are helpful to the patients during rehabilitation. Nowadays, the modern treatment and rehabilitation methods have been widely accepted and used throughout the country. The traditional method and modern method supplement each other.
Colombia has a varied geography and a variety of sports and recreational activities. The most popular sport is soccer, which is a widespread activity throughout the country, and professional dancing has a special place in some regions of the country. Athletic activities including 5, 10, 21, and 42 km racing competitions, and cycling in two modalities (mountain biking and road biking) is also very popular sports sometimes associated with foot and ankle conditions. Since Colombia has no seasons, these sports and recreational activities can be practiced year-round, leading to frequent overuse syndromes.
Related to soccer, the most frequent injuries are ankle sprains and anterior ankle impingement. Soccer is played on turf, which can be soft in the rainy season and hard in the dry season. The uneven grounds are also related to the frequency of ankle sprains. Indoor soccer played on synthetic turf has also a very high frequency of ankle sprains, due to shear forces on ankle and knee joints. Radiological evaluation of regular soccer players shows frequently medial, lateral, and anterior osteophytes associated with the repetitive trauma to the ankle. In recent literature, the origin of the tibial and talar osteophytes is related to ankle instability or repetitive trauma at or near the joint line. Thus, these are called osteophytes and not enthesophytes. The traction theory is no longer valid as cited by Johannes et al.
Patients with a history of frequent soccer games in the past present with multiple sprains and painful episodes after games. They may have had an initial severe sprain that received medical attention with adequate management. However, after ongoing sprains, patients do not search for medical attention until symptoms evolve either with instability or limitation in motion and impingement symptoms. In cases of ankle anterior impingement on physical exam, patients may complain of ankle reduced dorsiflexion compared to the contralateral side. Palpation on the anterior ankle joint can elicit pain, and depending on the size of the osteophyte, these can often be palpated. Stability testing of the ankle is carried out, and sometimes instability findings can be associated. Patients must also be tested for peroneal tendon pathology and subtalar symptoms, which are to be ruled out. Eversion strength and gastrocsoleus muscle contracture are also evaluated.
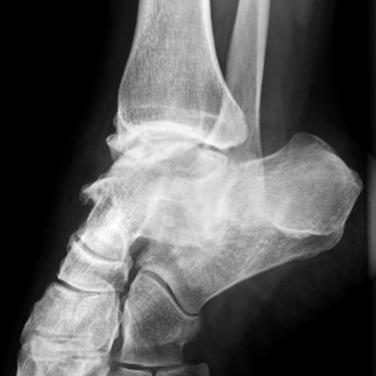
Antero-posterior, lateral, and mortise standing comparative views are taken in routine fashion ( Fig. 25.29 ), and if a small osteophyte is seen, an additional van Dijk᾽s view is taken ( Fig. 25.30 ). Only if any other instability-generating factor is suspected will a CT or MRI be ordered.
The ankle sprains are managed initially with the rest, ice, compression, elevation (RICE) protocol and after a short immobilization period sent to physiotherapy. We put great value in a thorough rehabilitation program looking for a total restoration of full eversion strength, Achilles tendon flexibility, and proprioception. Most of these patients get back to regular sports after 6 to 8 weeks, and only those who continue having giving-way symptoms and recurrent pain are treated surgically with the open Bröstrom-Gould procedure.
Other patients who have an instability sensation in more chronic cases can have an anterior impingement syndrome, which affects their proprioceptive condition. In these cases, the surgical procedure is focused on the resection of the anterior osteophytes of the tibia and the dorsum of the talar neck. This procedure is preferably performed either with a 40-mm arthroscope or with a mini-open technique. The joint is inspected first with a thorough complete ankle joint evaluation, with special attention to the medial and lateral gutters and at the horizontal joint line. Temporary distraction of the ankle is performed for inspection. The main procedure is performed without traction, and we proceed to resect the osteophytes on both sides (tibia and talus). The extent of the resection is checked under fluoroscopy. Careful resection of the inflamed synovial tissue of the anterior joint space is also performed. These patients are operated as outpatients under peripheral nerve block and sedation. Postoperatively they are immobilized with a soft dressing and 48 hours bed rest and elevation. Weight bearing is allowed after 2 days to tolerance, and sutures are removed after 12 to 15 days. A rehabilitation protocol centered on dorsiflexion recovery, strength, and proprioception is begun at that time.
On follow-up, we have experienced what the literature describes as recurrence of the osteophytes in a large percentage of our cases, but less than a third of those patients have recurring symptoms. If instability persists, the recurrence is greater (see Fig. 25.30 ).
Our main problems with surgical treatment of ankle instability, are neuropathic pain with superficial peroneal nerve lesion, arthrofibrosis, and medial or residual lateral instability. The multimodal pain management or in combination with nerve blocks with the aid of ultrasound and open neurolysis are the common approaches to this clinical entity. Arthrofibrosis is not frequent after open or arthroscopic ligament reconstruction. If there is a mild to moderate case, physical therapy has been beneficial. Uncommonly there are severe cases of arthrofibrosis that may require open debridement.
The residual instability of ankle is described more often in the recent literature, and the medial component of this pathology has had more focus in the last years. We are focusing on this clinical problem and see it with a more prevalent frequency in our clinical practice. When rupture of the deltoid ligament in an acute setting is present, a repair of the ligament is performed. In acute or chronic spring ligament ruptures, and an MRI with positive findings, our choice is a repair with suture anchors in acute settings or debridement of scar tissue and direct repair in the chronic lesions.
Achilles tendon ruptures are increasing and causing morbidity in our young population. These young adults are more involved in indoor and outdoor soccer without a physical training program, which renders more lesions than in the professional players. High frequency of games throughout the week (3–4 times) generate overuse syndromes that predispose to tendinopathy and tendon ruptures. These lesions can be caused by either indirect or direct trauma to the tendon. Patients can present with some prodromal symptoms before the acute rupture. Occasionally our patients have had previous visits with paratendonitis or paratendonitis with tendinosis that were not treated adequately.
These patients come in to the emergency room with an acute onset of pain and a sudden snapping or popping sensation at the Achilles tendon during sports activity. On occasions, a previous history of Achilles tendon pain can be obtained from the patient.
On physical exam the patient walks with a limp and variable edema around the rupture site. A positive Thompson test and a palpable gap are typical of a complete rupture ( Fig. 25.31 ). The plantar flexion strength can be diminished. In cases of doubt we order an ultrasound or an MRI, but these are not routinely performed.
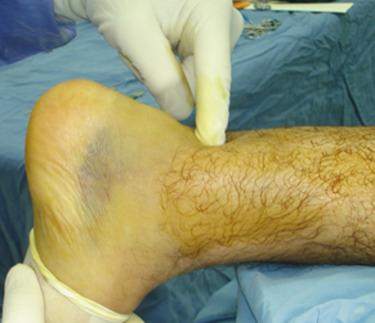
If the rupture is a palpable gap within 7 cm of the posterosuperior calcaneal tuberosity with a positive Thompson test, we proceed to perform a minimal incision repair within the first 10 days. If the rupture does not have a clear gap, but a positive Thompson test, an ultrasound or an MRI is ordered to define the type of rupture to plan the surgical approach. The mini-invasive technique has a lower complication rate with respect to the soft-tissue complications in simple ruptures (horizontal), but in massive and irregular tears, an open reparative technique is preferred.
The patient is positioned prone with both legs prepped for comparison of foot position at final tendon repair ( Fig. 25.32 ). A 4-cm skin incision is performed horizontally 1 cm above the gap, and careful incision of the paratenon is also performed. The stumps are localized and pulled through the incision, and a commercial tendon repair kit is used to perform the repair on both sides of the ruptured tendon. Three strands of reinforced nonabsorbable suture are knotted with the foot in a similar or slightly more plantar-flexed ankle position as the contralateral limb ( Fig. 25.33 ). Suture of the paratenon and skin incision are performed. A bulky dressing with the foot in plantar flexion and a posterior splint is applied for 12 days nonweight bearing. On day 12, the sutures are removed and a walker boot with a 40-mm heel lift is applied with permission for progressive weight bearing. Physiotherapy with the Mendelbaum protocol is started.
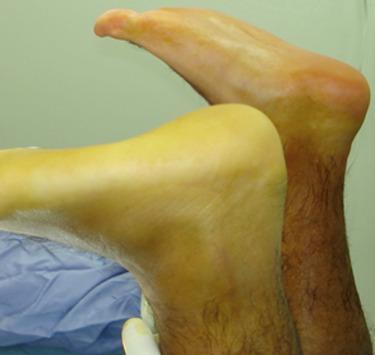
For all chronic lesions, either partial or complete, with more than three months evolution, we use the FHL transfer deep to the Achilles insertion, fixed with anchor sutures or biotenodesis screws. We have used this transfer tendon technique in more than 80 patients with solid results at this time.
In other activities performed in Colombia, like dancing, cycling, or horseback riding, trauma to the foot and ankle can involve torsional forces that generate these sprains and have a relative high incidence and are not properly diagnosed in local emergency rooms. Sometimes these lesions are detected in patients in a late form with residual pain and problems at their midfoot. Persistent pain after 4 to 6 weeks of injury, with edema present at the TMT point of first and second rays, with initial ecchymosis described on the first visit at the emergency room, can be indicative of severe ligament or soft-tissue damage.
Clinical findings, AP, lateral, and oblique standing bilateral views can sometimes be sufficient to view subtle differences of both feet to make the diagnosis. The fleck sign, which indicates Lisfranc’s avulsion fracture, must also be considered. CT scan or MRI can be indicated in cases of doubt, but they are usually not ordered in a routine fashion. The open reduction and internal solid fixation are mandatory in all displaced fracture-dislocations.
For low-grades lesions and symptomatic sprains, we use the Nunley and Vertullo classification, with good and excellent results in the 89% of our patients with surgical treatment in grade II and III lesions with transarticular screws or the endo button technique.
In Egypt, soccer is the most common sport practiced both on professional and recreational levels. People of all age groups play soccer, and it is currently played on different terrains including turf mostly, but also sand and concrete. An array of foot and ankle injuries has been associated with soccer, including but not limited to ankle sprains, Achilles tendon ruptures, turf toes, FHL tendinitis, Lisfranc injuries, ankle impingement, and OCLs of the talus. Other popular sports include squash, wrestling, and martial arts. Recently, cycling and marathon running have gained popularity and attracted a good proportion of the youth population.
One thing to mention is the delayed presentation of many of our patients. This is partly due to limited access to health care at some areas. Moreover, patients tend to ignore their complaints and try natural remedies and alternative medicine long before they seek medical advice. This reflects on the chronicity of the case and therefore decision-making and available options to treat such problems.
We here report on our experience with management of some of the aforementioned injuries and our preferred surgical techniques.
It is estimated to occur in 2%–6% of ankle sprains; however, more than 80% of lesions are missed or diagnosed in a delayed fashion. Many factors have to be considered when discussing surgical management of these injuries. These can be classified into patient factors (age, body mass index [BMI], activity level, and comorbidities) and lesion factors (size, containment, condition of surrounding cartilage and subchondral bone). Treatment strategies can generally be grouped into two major categories:
Reconstruction techniques: fixation or reattachment of OCLs and autograft or allograft osteochondral transplantation
Repair techniques or marrow-stimulation techniques: microfracture and drilling (with or without biologic augmentation), autologous or allogeneic cell implantation
While we have performed many of these options, our results have been inconsistent and not fully satisfactory. This is in line with data showing no superiority of one cartilage repair technique over others. We recommend performing microfracture for lesions <10 mm 2 . Lesions larger then 10 mm 2 are treated with either microfracture supplemented with biological augmentation (bone marrow aspirate concentrate [BMAC] or platelet-rich plasma [PRP]) or osteochondral autologous transplantation (OATs) with allografts reserved for critically sized lesions that are not amenable to autografts.
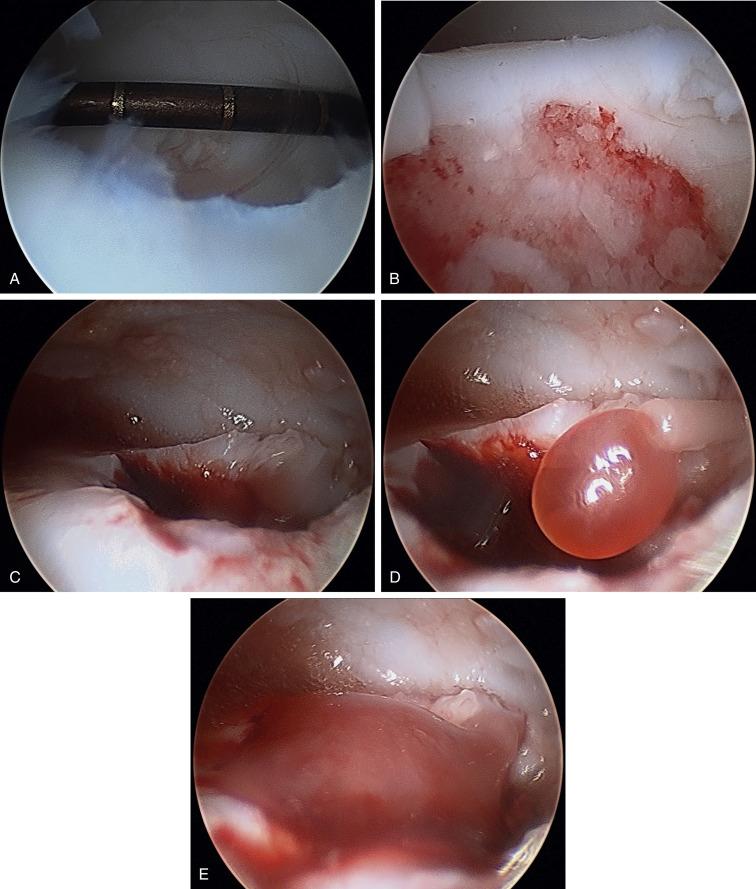
Recently, the senior author (AH) reported on the use of culture-expanded bone marrow–derived mesenchymal stem cells (MSCs) in treatment of large OCLs of the femoral condyle. Their preliminary results were promising, and they noted improvement in patient outcomes and MRIs. We subsequently decided to use the same technique with OCLs of the talus. We started using second-generation bone marrow MSC implantation, which entailed culture-expanded MSCs, implanted on platelet-rich fibrin glue (PR-FG) scaffold. This mixture was injected via all-arthroscopic technique into the base of critical-sized OCLs, and patients were made nonweight bearing for 6 weeks postoperatively ( Fig. 25.34 ). We reported on a small case series of 16 patients treated with this technique with an average size of OCL of 3.74 cm 2 ± 1.12 and mean follow-up of 18 months. Briefly, autologous bone marrow aspirate was acquired from patients in a first-stage procedure. This was transferred to the Tissue Engineering Unit at the Department of Biochemistry, Cairo University College of Medicine, where MSCs were isolated and culture expanded for a minimum of five passages. The plasma was processed to create PR-FG. In a second-stage all-arthroscopic procedure, the base of the defect was curetted to a stable healthy rim of cartilage and underlying bleeding subchondral bone. Defects deeper than 8 mm were grafted with autologous calcaneal bone graft. The culture-expanded MSCs were then mixed with the autologous PR-FG and injected in the base of the defect after establishing dry arthroscopy. The mixture was let to clot and ankle ROM was tested under arthroscopy for stability of the implant. Immobilization for 2 weeks was followed by active and passive ROM exercise while maintaining nonweight-bearing status for 6 weeks, followed by progressive weight bearing. Our study showed improvement in postoperative AOFAS scores compared to preoperatively, but this improvement did not reach statistical significance.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here