Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The need for and mode of transporting an injured athlete is determined after primary and secondary evaluations by the first responder. It must always be executed so that further injury is prevented.
Planning the mode of transport and necessary equipment can help ensure that an appropriate technique is used (see Chapter 4 : “Sideline Preparedness and Emergencies”).
An athlete with a suspected spinal injury should not be moved by anyone other than certified medical personnel with appropriate stabilization. An ambulance should be contacted immediately (see Chapter 46 : “Neck Injuries”), if not already present.
If a serious fracture, such as that of the tibia, femur, or pelvis, is suspected, the safest and most efficient mode of transportation for a short distance is by means of a stretcher that is taken onto a utility vehicle or preferably by an ambulance.
Suspected extremity fractures must be immobilized before transport ( Fig. 58.1 ).
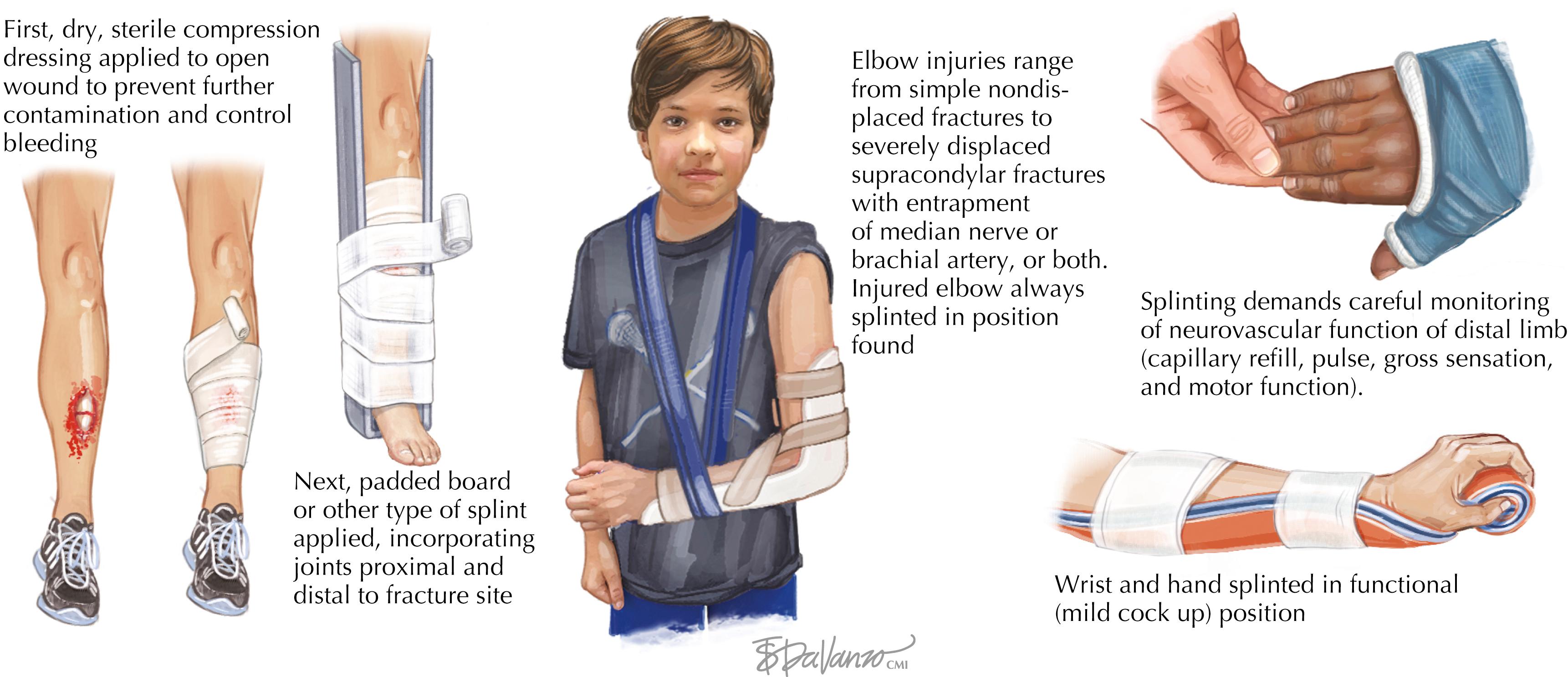
The ability to take care of an acute fracture in an athlete is directly related to one’s level of preparedness and experience.
Timely application of a splint to a fractured extremity minimizes the overall surrounding soft tissue injury and allows for safe transportation of the athlete for definitive care.
Sports medicine providers (physician and trainers) should carry lightweight, easy-to-apply splint material in their sport medicine bag (see Chapter 4 : “Sideline Preparedness and Emergencies”).
Basic mobile splint kit for a medicine bag ( Table 58.1 ):
Arm sling/shoulder immobilizer (medium and large sizes)
Alumafoam padded splints (several lengths that can be cut to size)
Structural aluminum malleable (SAM) splint
Knee immobilizer (universal size)
Webril (cast padding) and Ace wraps (4 inch [10.16 cm] and 6 inch [15.24 cm])
Plaster or fiberglass splinting material for self-made splints (prepackaged splints are available)
| Clavicle and Acromioclavicular (AC) Joint | Arm sling |
| Shoulder and Proximal Humerus | Arm sling and a 6-inch Ace wrap swathe |
| Distal Humerus and Elbow | Air or vacuum splint |
| Forearm and Wrist | Fiberglass/plaster splint, structural aluminum malleable (SAM) splint, prefabricated orthosis |
| Hand | Buddy taping, Alumafoam splint |
| Spine | Cervical collar and spine board |
| Hip and Femur | Femoral traction splint |
| Knee and Proximal Tibia | Knee immobilizer |
| Tibial Shaft, Ankle, and Foot | Air or vacuum splint |
Advanced facility kit (available at all high-volume sports complexes or via emergency medical services [EMS]):
Extremity vacuum splints or air splints (total body kits)
Cervical collar
Spine board
Femoral (Hare) traction splint
Crutches
Braces or orthoses stop or limit range of motion, facilitate movement, or guide a joint through an arc of motion.
Splints are used to immobilize and position one or several joints (see Fig. 58.1 ).
Splints and braces are prescribed after a fracture to protect a partially healed fracture or to prevent the pain and soft tissue damage that occur with motion.
A cast is a stress-sharing device, allowing limited fracture motion and callus formation because of secondary bone healing. The joints above and below a fracture should be immobilized to prevent rotation and translation of the fracture fragments.
Splints are beneficial because they provide some stabilization at the fracture site, but they may be removed for rehabilitation treatment.
After a cast is initially removed, splints are frequently used during activity or at night to reduce pain and discomfort and allow additional fracture consolidation.
Joint stiffness is common after cast removal and resolves after weeks to months of aggressive, but appropriate, rehabilitation.
Immobilization of the joints above and below the fracture site often leads to stiffening and the need for a prolonged rehabilitation program.
A cast brace can provide partial immobilization while allowing some range of motion and weight bearing on a limb.
Once a fracture achieves an appropriate degree of stability as a result of callus formation, the cast can be replaced with a splint or brace, allowing motion of the joints proximal and distal to the fracture, without compromising the support at the fracture site.
Immediately after an athlete sustains a fracture or dislocation, the neurologic and vascular status must be evaluated and documented.
Temporary immobilization measures should be employed as the patient is transported to the hospital (see Fig. 58.1 ).
The mechanism of injury can provide clues regarding what type of injury has occurred.
In all upper extremity fractures, assess the following:
Open or closed fracture
Pain, swelling, or paresthesias
Vascular status distal to the injury
Active and passive range of motion of wrist and/or digits
Radial, median, and/or ulnar nerve function and possible compression; axillary nerve function should also be documented with shoulder injuries
In all lower extremity fractures, assess the following:
Open or closed fracture
Patient complaints of pain, swelling, or paresthesias
Vascular status distal to the injury
Active and passive range of motion of all metatarsophalangeal and interphalangeal joints
Nerve function and possible compression
Overview: Uncommon, accounting for approximately 1% of fractures in trauma registries ( Fig. 58.2C ).
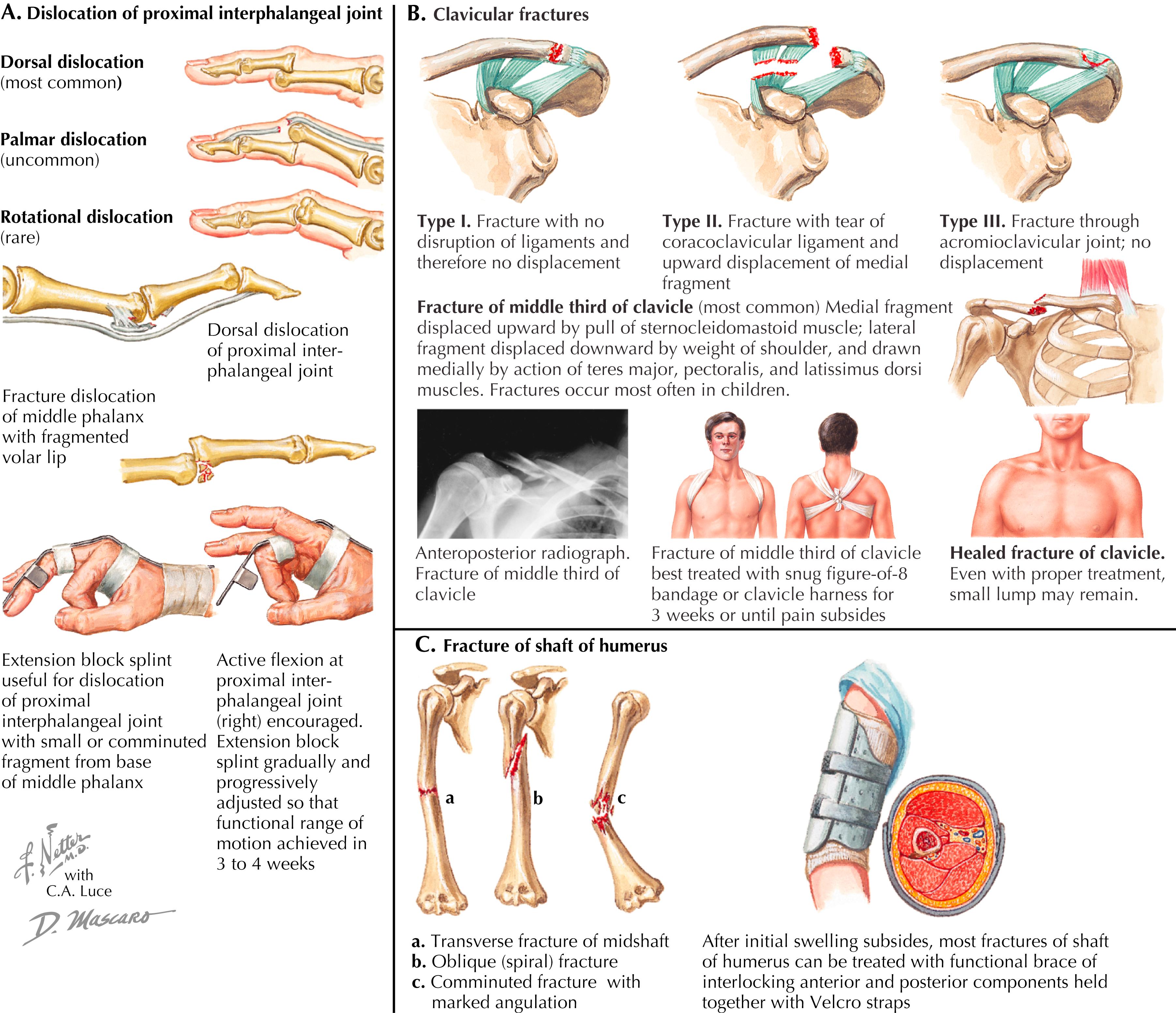
Mechanism of injury: More frequently from a fall onto the involved extremity but can occur from a direct blow. On occasion, rotational injuries can also occur in some sports such as arm wrestling.
Presentation: Painful, unstable extremity with swelling and bruising.
Physical examination: Gentle palpation of the shaft of the humerus should be performed, noting any areas of malalignment and severe pain.
Associated injuries: Associated nerve injuries are relatively common and should be documented; radial nerve injuries are most common. Most common fracture type associated with a nerve injury is a transverse mid-diaphyseal fracture. Document a motor neurologic examination of the axillary, musculocutaneous, radial, median, and ulnar nerves. Skin should also be examined to rule out an open fracture. Shoulder and elbow joint should be examined and imaged.
Diagnostics: Anteroposterior (AP) and lateral radiographs of the entire humerus should be obtained. Additionally, radiographs of the shoulder and elbow should be taken.
Treatment: In most cases, nonoperative management of midshaft fractures is appropriate. Treat with functional bracing to allow active flexion and extension of the elbow during the healing process to prevent elbow stiffness; motion helps reduce the fracture and aids in the healing process. Isometric muscle exercises in the functional brace can aid in maintaining alignment and assist in fracture healing. Patients who have sustained significant nerve injuries that prevent active range of motion are not candidates for functional bracing. The humerus can heal with angulation of up to 30 degrees and shortening of 2 to 3 cm without functional problems in most patients. However, the functional needs of a high-performance athlete are different, and accepting that degree of malalignment is discouraged. If functional bracing is elected to treat an athlete, great care should be taken to follow the healing process and evaluate the alignment. If alignment is not maintained in the dominant arm of a skill athlete, consideration should be given to surgical stabilization of the fracture. Surgical treatment usually involves either plating or use of an intramedullary nail (see Fig. 58.2C ). Shoulder pain is the most frequent complication after intramedullary nailing. It is important to warn an athlete of the risk of shoulder pain if intramedullary nailing is elected.
Prognosis and return to play: Prognosis for healing and good functional return after isolated humerus shaft fractures is good. Patients who have associated nerve injuries or shoulder dislocations have a less favorable prognosis, but still may be able to return to competition if the nerve injury resolves.
Fractures that have minimal displacement and are in near anatomic alignment can be treated with casting or splinting if they are stable enough to allow early elbow motion.
Elbow stiffness and permanent motion loss are significant risks after elbow trauma.
Cast or splint treatment of these injuries should initially allow no motion at the elbow.
Most distal humerus fractures require surgical stabilization, followed by early functional motion of the elbow.
Minimally displaced fractures of the olecranon with <2 mm displacement and intact elbow extensor mechanism can be treated with cast or splint immobilization.
Early elbow motion is necessary for good functional results.
The cast should be adequately padded to avoid skin breakdown at the edges of the cast or splint.
The cast should volarly extend to the proximal palmar crease and dorsally to the metacarpophalangeal joints to allow full motion at the interphalangeal and metacarpophalangeal joints.
Once there is early evidence of healing, the elbow should be mobilized to prevent stiffness.
An elbow-hinged brace can protect the fracture and maintain motion of the elbow. Often, some terminal extension is lost, but functional range of motion is maintained.
Aggressive rehabilitation is critical, as the loss of some terminal extension may have implications on athletic performance even if it does not affect activities of daily living.
Displaced fractures of the olecranon require open reduction and internal fixation (ORIF), followed by early elbow range of motion to minimize the development of elbow stiffness.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here