Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
hidradenitis suppurativa
interleukin
neodymium-doped yttrium-aluminum-garnet laser
metabolic syndrome
inflammatory bowel disease
odds ratio
standardized incidence ratios
quality of life
standard deviation
socioeconomic status
National Ambulatory Medical Care
National Hospital Ambulatory Medical Care Survey
intimate partner violence
Crohn’s disease
ulcerative colitis
squamous cell carcinoma
United States
While the overall US prevalence of hidradenitis suppurativa (HS), obtained through US claims data, has been reported to be 0.10% or 98 per 100,000 persons, HS disproportionally affects women (137 per 100,000), African Americans (296 per 100,000), and biracial (African American/Caucasian) (218 per 100,000) patient groups. In comparison, the rates of HS among white patients are closer to the overall reported US prevalence at 95 per 100,000 persons. Conversely, HS affects Asians, Pacific Islanders, Native Americans, Latin Americans, and Native Hawaiians at much lower rates, with a standard prevalence of 0.04%. However, these prevalence rates may be underestimations due to underdiagnosis and the inability to capture those who did not seek care in the healthcare systems included in the databases analyzed. Further, adult patients with HS may have symptoms for up to 7 years before diagnosis. Consequently, if the same is true among children with HS, then prevalence in younger age groups may also be underestimated.
Classical teachings have supported this claim that people of African descent have a higher incidence than those of European descent. However, the majority of previously published studies on HS report prevalence and incidence in a largely Caucasian cohort. Recently, additional retrospective studies have emerged supporting the classical teachings, demonstrating that African Americans appear to be more commonly affected and with higher severity of HS. The true prevalence of HS in the general US population may likely be higher due to limitations in diagnosis, underdiagnosis, misdiagnosis, and patient reluctance to seek treatment. This may be especially true in skin of color populations due to limited access to medical care, implicit biases, anatomical differences, genetics, and increased prevalence of lower socioeconomic status (SES) among these groups.
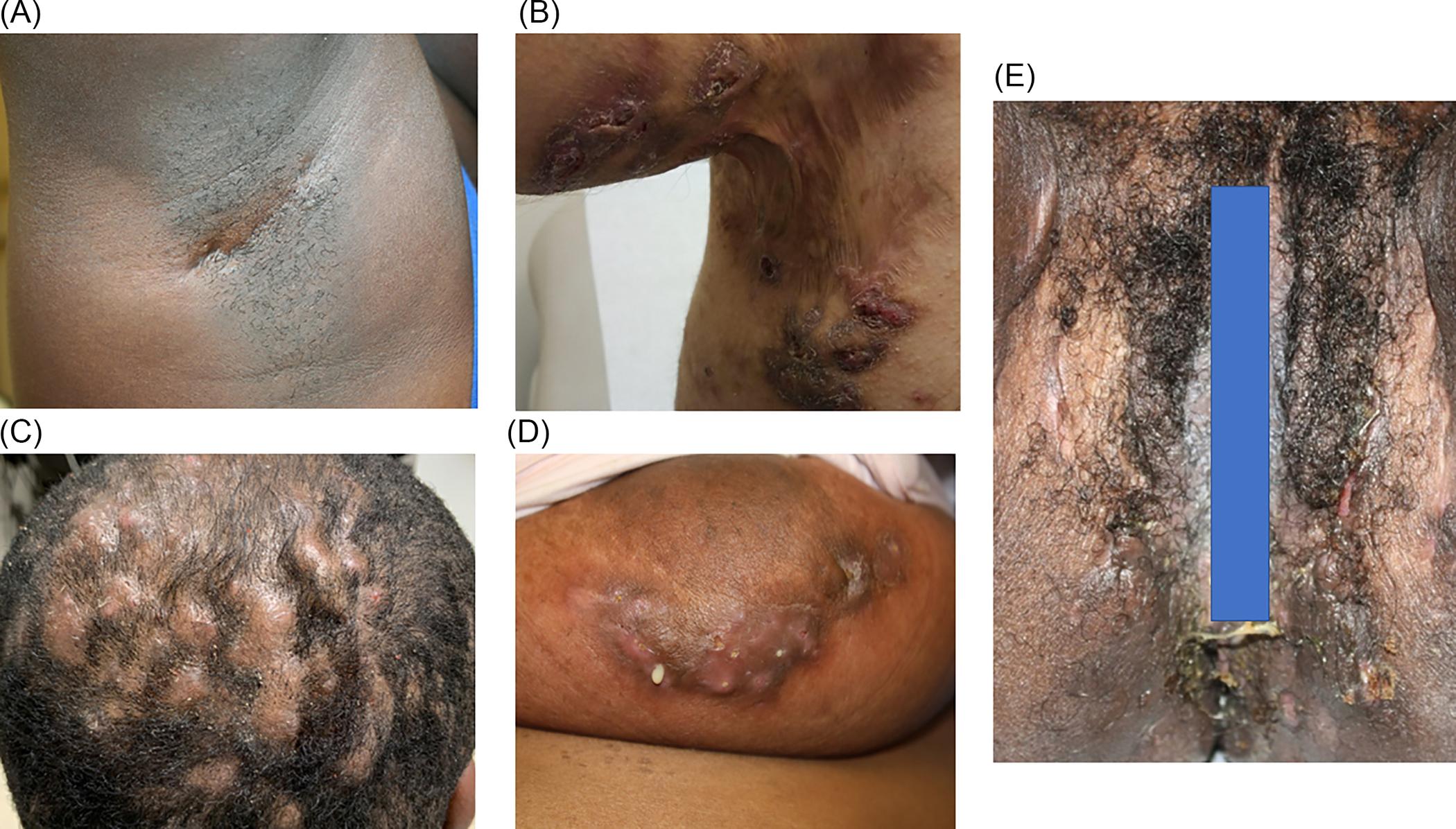
HS presents with painful, erythematous, and often malodorous abscesses, nodules, dermal tunnels, double- and multi-ended comedones, along with scar formation followed by hyperpigmentation in apocrine gland-bearing skin such as the axillae, inguinal, perianal, and perineal regions. Further, HS lesions in skin of color patients may be purplish in color, more hyperpigmented, and the erythema and tunnels may be more difficult to identify in comparison to Caucasian patients. Gentle palpation can be used to help identify them( Fig. 30.1 ).
This discrepancy in reporting HS prevalence amongst skin of color patients also appears to extend to clinical trials. Using Clinicaltrials.gov and PubMed, Price et al. examined the race and ethnicity demographics in phase II and phase III HS treatment trials published from 2000 to August 2019. Fifteen trials were included in the analysis. Among these trials, 669 (68.0%) of the participants were Caucasian and 138 (14.0%) were of African descent. Asians, American Indian or Alaskan Natives, and Native Hawaiian or other Pacific Islanders comprised 29 (2.9%), 3 (0.3%), and 1 (0.1%) participants, respectively. Only 15 participants were reported as Hispanic, as only three trials reported ethnicity data. While these percentages may reflect the breakdown of the US population in terms of race/ethnicity, they do not reflect the disproportionate rates of HS in African Americans. The remaining 144 (14.6%) participants were recorded as “other/unspecified” (36 self-identified, 108 lacked race reporting). None of the trials included a sub-analysis of treatment efficacy based on race or ethnicity.
Adalimumab is the only currently approved systemic medication for the treatment of HS. However, clinical trials for adalimumab did not sufficiently examine the treatment response in patients with skin of color. One study was conducted solely in Caucasian and Romany individuals, while another study consisted of 80% to 85% Caucasians. Further, none of the trials reported the percentage of patients that were Hispanic/Latino or stratified the responses to adalimumab by race. The other systemic biologic agent trials for HS (e.g., etanercept, infliximab, anakinra, and ustekinumab) either did not report race or largely had a Caucasian population. Reduced enrollment in clinical trials by skin of color populations may be due to distance from clinical trial sites, lack of education regarding clinical trials, lack of awareness that clinical trials are available for the particular disorder, language barriers, and mistrust of researchers from historical experiences such as the Tuskegee Syphilis Study. Moreover, these results suggest that populations represented in clinical trials may not truly reflect the diverse patient populations affected by HS, and that these medications may only work in a subset of HS patients.
In HS treatment, there are differences in dosing for standard phototherapeutic options in patients with skin of color. In randomized controlled trials, typical settings used for the neodymium-doped yttrium-aluminum-garnet laser (Nd:YAG) were generally a 10-mm spot size with a 20-ms pulse duration and 40 to 50 J/cm 2 in patients with Fitzpatrick skin type I to III and a 35-ms pulse duration and 25 to 35 J/cm 2 in patients with skin types IV to VI. This treatment is discussed further in Chapter 25 . Carbon dioxide laser excision and marsupialization has also been shown to be an effective therapy for the management of Hurley Stage II or III disease. Notably, it has been our experience in clinical practice that the risk of keloid formation following the excision of HS lesions has rarely been seen. Due to this observation, the authors strongly suggest that this modality be offered to skin of color patients. Additional light-based treatment options for HS include photodynamic therapy (PDT) and intense pulsed light. However, these treatment modalities are not well-studied in skin of color HS patients and their general efficacy appears to be very limited.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here