Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The previous chapter reviewed the lung CT AI methods to assess normal and diseased lung structure using a single TLC chest CT scan. COPD, ILD, and asthma can all produce small and large airway disease. This chapter will look at how lung CT AI can be used to assess lung ventilation by obtaining two chest CT scans with each scan taken at a different lung volume. This approach can be viewed as a dynamic assessment of the lungs that can provide information on lung function by assessing lung ventilation. Functional lung CT imaging can provide indirect information on the function of small airways, <2 mm in diameter, that cannot be measured directly by currently available CT scanners. Direct imaging of the airway tree can provide structural information on normal and diseased airway tree geometry (e.g., lumen area, wall area) at different generations from the trachea, generation 1, to subsegmental airways out to airway generation 6. Direct imaging of the airway tree by chest CT will be discussed later in this chapter.
Obtaining a chest CT scan at a lower lung volume, FRC or RV, can be used to assess air trapping in the lung, areas of the lung where air cannot freely be exhaled. The process of exhaling air out of your lungs decreases the volume of your lung by decreasing the amount of air per unit volume and since the tissue per unit volume is approximately constant, the overall density of the lung tissue normally increases when you exhale ( Fig. 6.1 ). The normal expiratory CT scan obtained at either FRC or RV shows increased density throughout both lungs due to the decrease in air volume in the lung without substantially changing the tissue volume. The lung decreases in size and the density of the lung increases to the extent that air is exhaled from each region of the lungs. This decrease in air is greater in the lower lobes than the upper lobes and is greater in the dependent portions of the lungs compared to the nondependent portions of the lungs ( Fig. 6.1 ).

When there is a narrowing of the small airways in the lung or a reduced number of small airways in the lung or both, the lungs will not exhale as much air as they normally would in the regions of the lung where there are abnormal small airways. The areas of lung where there is incomplete emptying of the air will decrease the density of the lung in those regions, compared to the adjacent normal lung tissue, on expiratory chest CT scans. This is referred to as air trapping and is seen on FRC/RV chest CT scans as regions of relative decreased density compared to normal areas of higher density on the expiratory CT scan ( Fig. 6.2 ). The trapped air can be quantitated in several ways and at different scales, including assessing both lungs together, individual lungs, lung lobes, and at the level of the individual lung voxel. Assessing air trapping at progressively smaller scales can increase spatial information that is lost when the air-trapping analysis is done by assessing both lungs together.
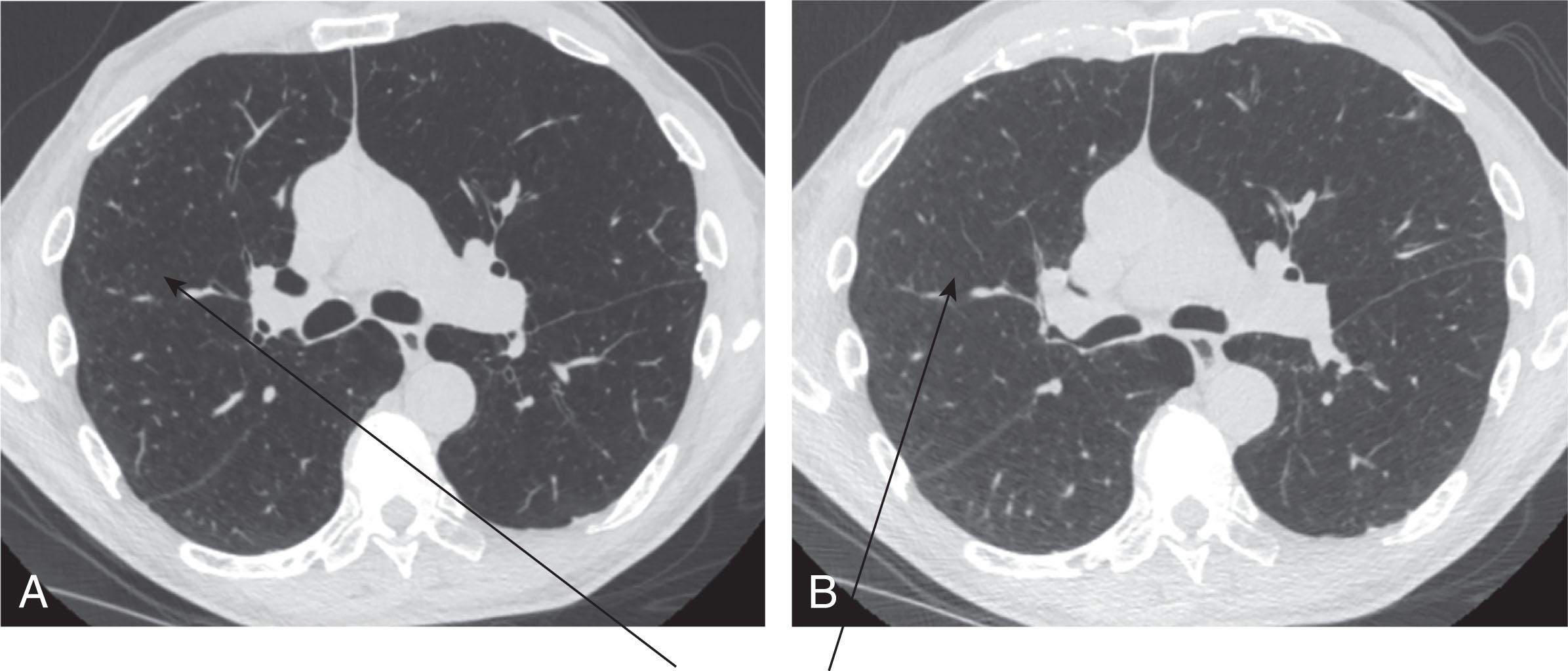
The mean lung density on expiration, FRC/RV, CT scans can be used to assess air trapping. Similar to the LAA and HAA measures described in Chapter 5 , the amount of lung that is lower than a defined threshold HU value on an FRC/RV lung CT can assess the amount of air trapping in the lung ( Fig. 6.3 ). The ratio of the mean lung density on expiration to the mean lung density on inspiration can also be used to assess the amount of air trapping present in the lung. Air trapping can also be assessed in the lung by taking the ratio of the CT lung volume at FRC to the CT lung volume at TLC. A much more powerful way to assess the air trapping in the lung is to use nonrigid registration methods to compare voxel by voxel the differences in lung attenuation between the TLC and RV chest CT scans. Two well-known published methods that use image registration to assess air trapping at the voxel level: the parametric response map (PRM) and the disease probability map (DPM). The different methods to determine air trapping in the lung are summarized in Box 6.1 .
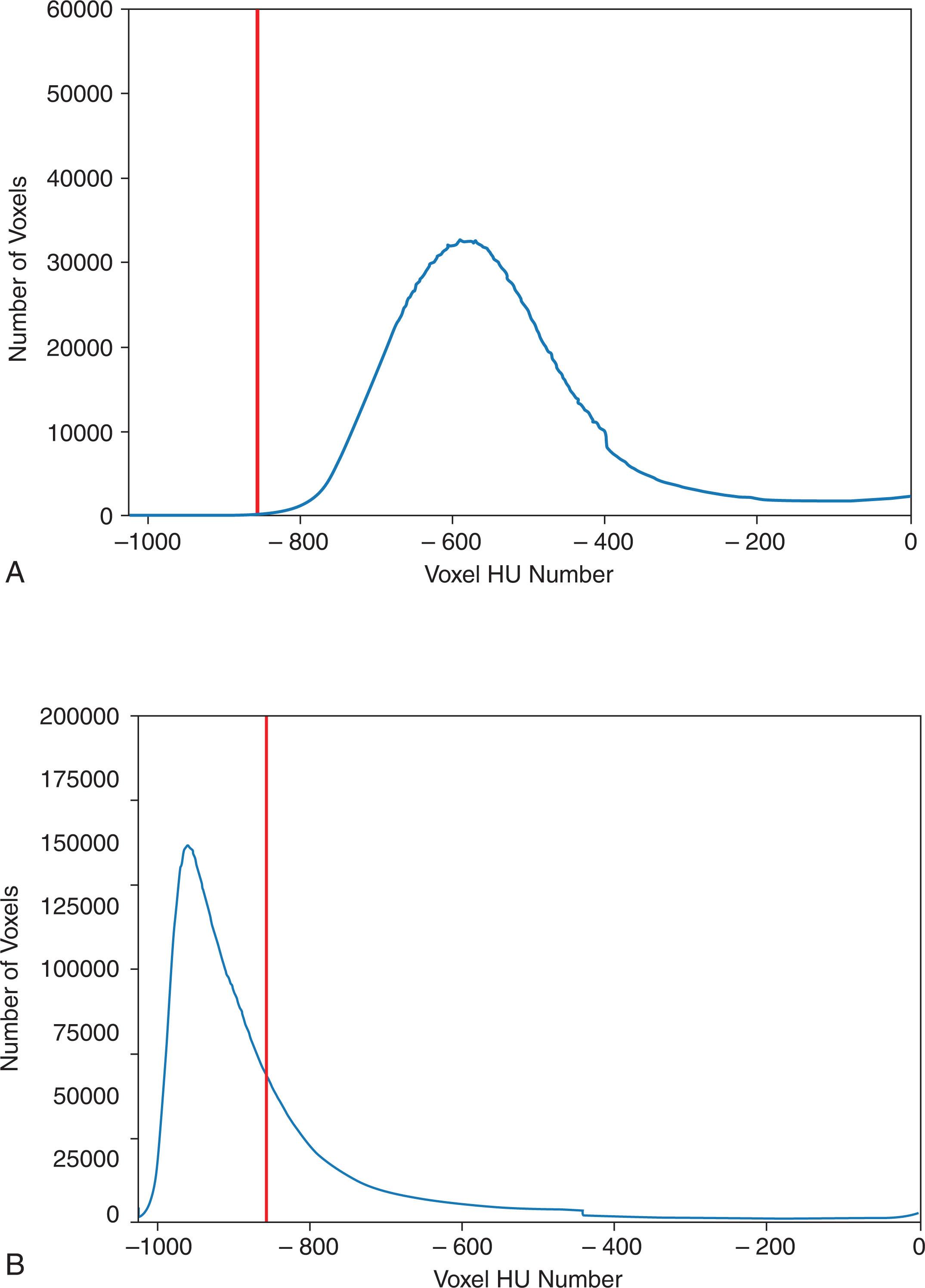
Mean value of the lung CT voxels on an FRC lung CT
This is referred to as the expiratory mean lung density (MLD expiration )
Determine the percentage of FRC or RV lung CT voxels that are <−856 HU
This is referred to as the LAA −856
Ratio of the FRC lung CT MLD to the TLC lung CT MLD
MLD expiration /MLD inspiration
Ratio of the FRC CT lung volume to the TLC CT lung volume
CT FRC /CT TLC
Determine the difference between TLC CT lung volume and RV CT lung volume
CT TLC -CT RV
Functional small airway disease using PRM or DPM
fSAD
Air trapping is a hallmark of patients with asthma. Busacker et al. in 2009 reported the results of assessing air trapping in severe asthma subjects enrolled in the Severe Asthma Research Project (SARP) using quantitative assessment of chest CT scans obtained at FRC. Air trapping was defined to be significant in this study if 9.66% or more of the lung tissue was <−850 HU, LAA −850 , on the expiratory chest CT scans obtained at FRC. The quantitative chest CT assessment of LAA −850 in this study identified severe asthma subjects that were at increased risk for asthma-related hospitalizations, ICU visits, and mechanical ventilation. Multivariate analysis showed that those subjects with an LAA −850 >9.66% had an increased risk of asthma, pneumonia, high levels of airway neutrophils, and airflow obstruction measured by FEV1/FVC ratio and atopy.
Schroeder et al. in 2013 reported the results of doing TLC and FRC quantitative CT scans to assess air trapping and emphysema in 4062 COPD subjects enrolled in the COPDGene research study. The quantitative CT metric of air trapping was defined as the percent or fraction of lung tissue <−856 HU, LAA −856 , on the expiratory FRC CT scan ( Fig. 6.3 ). The results of this study showed that the LAA −856 metric of air trapping strongly correlated with decreases in airflow measured by spirometry, FEV1 R = −0.77 and FEV1/FVC R = −0.84, in this large group of COPD subjects. The corresponding LAA −950 metric of emphysema derived from the TLC chest CT scans (see Chapter 5 ) did not correlate as strongly with decreases in airflow, FEV1 R = −0.67 and FEV1/FVC R = −0.76.
As we discussed in Chapter 5 , the COPDGene 2019 Classes of COPD are determined by first defining four novel criteria to diagnose COPD: “Exposure, Symptoms, CT Structural Abnormality, Spirometry”. The CT structural criteria include having one or more of the following lung CT AI QCT metrics: LAA −950 equal to 5% or greater on a TLC chest CT scan (QCT structural measure of Emphysema), LAA −856 ≥15% on expiratory CT scan (QCT functional measure of air trapping), Pi10 equal to 2.5 mm or greater (QCT structural measure of airway wall thickening). The presence of 15% or more of air trapping on an expiratory FRC CT using the QCT metric LAA−856 in a patient with a 10-pack-year or greater smoking history, means they have at least possible COPD using the COPDGene 2019 Classes of COPD (see Chapter 5 ).
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here