Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Discuss the constituents and various functions of saliva.
Understand the mechanisms leading to the formation of saliva.
Explain the processes resulting in the tonicity of saliva and concentrations of its various ions.
Describe the regulation of salivary secretion.
Although the salivary glands are not essential to life, their secretions are important for the hygiene and comfort of the mouth and teeth. The functions of saliva may be divided into those concerned with lubrication , protection , and digestion . An active process produces saliva in large quantities relative to the weight of the salivary glands. Saliva is hyposmotic at all rates of secretion, and in contrast to the other gastrointestinal (GI) secretions, the rate of secretion is almost totally under the control of the nervous system. Another characteristic of this regulation is that both branches of the autonomic nervous system (ANS) stimulate secretion. However, the parasympathetic system provides a much greater stimulus than does the sympathetic system.
The lubricating ability of saliva depends primarily on its content of mucus . In the mouth, mixing saliva with food lubricates the ingested material and facilitates the swallowing process. The lubricating effect of saliva is also necessary for speech, as evidenced by the glass of water normally found on the podium of a public speaker.
Saliva exerts its effects through a variety of different mechanisms. It protects the mouth by buffering and diluting noxious substances. Hot solutions of tea, coffee, or soup, for example, are diluted and cooled by saliva. Foul-tasting substances can be washed from the mouth by copious salivation. Similarly, the salivary glands are stimulated strongly before vomiting. The corrosive gastric acid and pepsin that are brought up into the esophagus and mouth are thereby neutralized and diluted by saliva. Dry mouth, or xerostomia, is associated with chronic infections of the buccal mucosa and with dental caries. Saliva dissolves and washes out food particles from between the teeth. Certain specialized constituents of saliva have antibacterial actions. These include the following: a lysozyme , which attacks bacterial cell walls; lactoferrin , which chelates iron and thus prevents the multiplication of organisms that require it for growth; and the binding glycoprotein for immunoglobulin A (IgA), which in combination with IgA forms secretory IgA, which in turn is immunologically active against viruses and bacteria. Various inorganic compounds are taken up by the salivary glands, concentrated, and secreted in saliva. These include fluoride and calcium (Ca 2+ ), which are subsequently incorporated into the teeth.
The contributions made by saliva to normal digestion include dissolving and washing away food particles on the taste buds to enable one to taste the next morsel of food eaten. Saliva contains two enzymes, one directed toward carbohydrates and the other toward fat. An α-amylase called ptyalin cleaves internal α-1,4-glycosidic bonds present in starch. Exhaustive digestion of starch by this enzyme, identical to pancreatic amylase, produces maltose, maltotriose, and α-limit dextrins, which contain the α-1,6 branch points of the original molecule. Salivary amylase has a pH optimum of 7, and it is rapidly denatured at pH 4. However, because a large portion of a meal often remains unmixed for a considerable length of time in the orad stomach, the salivary enzyme may account for the digestion of as much as 75% of the starch present before it is denatured by gastric acid. In the absence of salivary amylase, there is no defect in carbohydrate digestion because the pancreatic enzyme is secreted in amounts sufficient to digest all the starch present.
The serous salivary glands of the tongue secrete the second digestive enzyme, lingual lipase , which plays a role in the hydrolysis of dietary lipid. Unlike pancreatic lipase, lingual lipase has properties that allow it to act in all parts of the upper GI tract. Thus the ability of lingual lipase to hydrolyze lipids is not affected by surface-active detergents such as bile salts, medium chain fatty acids, and lecithin. It has an acidic pH optimum and remains active through the stomach and into the intestine.
The salivary glands are a collection of somewhat dissimilar structures in the mouth that produce a common juice (the saliva), although the composition of the secretion from different salivary glands varies. The largest of the salivary structures are the paired parotid glands , located near the angle of the jaw and the ear. They are serous glands, secrete a fairly watery juice rich in amylase, and account for approximately 25% of the daily output of saliva. The smaller bilateral submandibular and sublingual glands are mixed glands, containing both serous and mucous cells. They elaborate a more viscid saliva and secrete most of the remaining 75% of the output. Other, still smaller glands are present in the mucosa covering the palate, buccal areas, lips, and tongue.
Most of the salivary glands are ectodermal in origin. The combined secretion of the parotid and submandibular glands constitutes 90% of the volume of saliva, which in a normal adult can amount to a liter daily. The specific gravity of this mixed juice ranges from 1.000 to 1.010.
The microscopic structure of the salivary glands combines many features observed in another exocrine gland, the pancreas. A salivary gland consists of a blind-end system of microscopic ducts that branch out from grossly visible ducts. One main duct opens into the mouth from each gland. The functional unit of the salivary duct system, the salivon , is depicted in Fig. 7.1 . At the blind end is the acinus , surrounded by polygonal acinar cells. These cells secrete the initial saliva, including water, electrolytes, and organic molecules such as amylase. The solutes and fluid move out of the acinar cell into the duct lumen to form the initial saliva. The acinar cells are surrounded in turn by myoepithelial cells . The myoepithelial cells rest on the basement membrane of acinar cells. They contain an actinomycin and have motile extensions. The next segment of the salivon is the intercalated duct , which may be associated with additional myoepithelial cells. Contraction of myoepithelial cells serves to expel formed saliva from the acinus, oppose retrograde movement of the juice during active secretion of saliva, shorten and widen the internal diameter of the intercalated duct (thereby lowering resistance to the flowing saliva), and prevent distention of the acinus (distention of the blind end of the salivon would permit back-diffusion of formed saliva through the stretched surface of the acinus). Thus the myoepithelial cells support the acinus against the increased intraluminal pressures that occur during secretion.
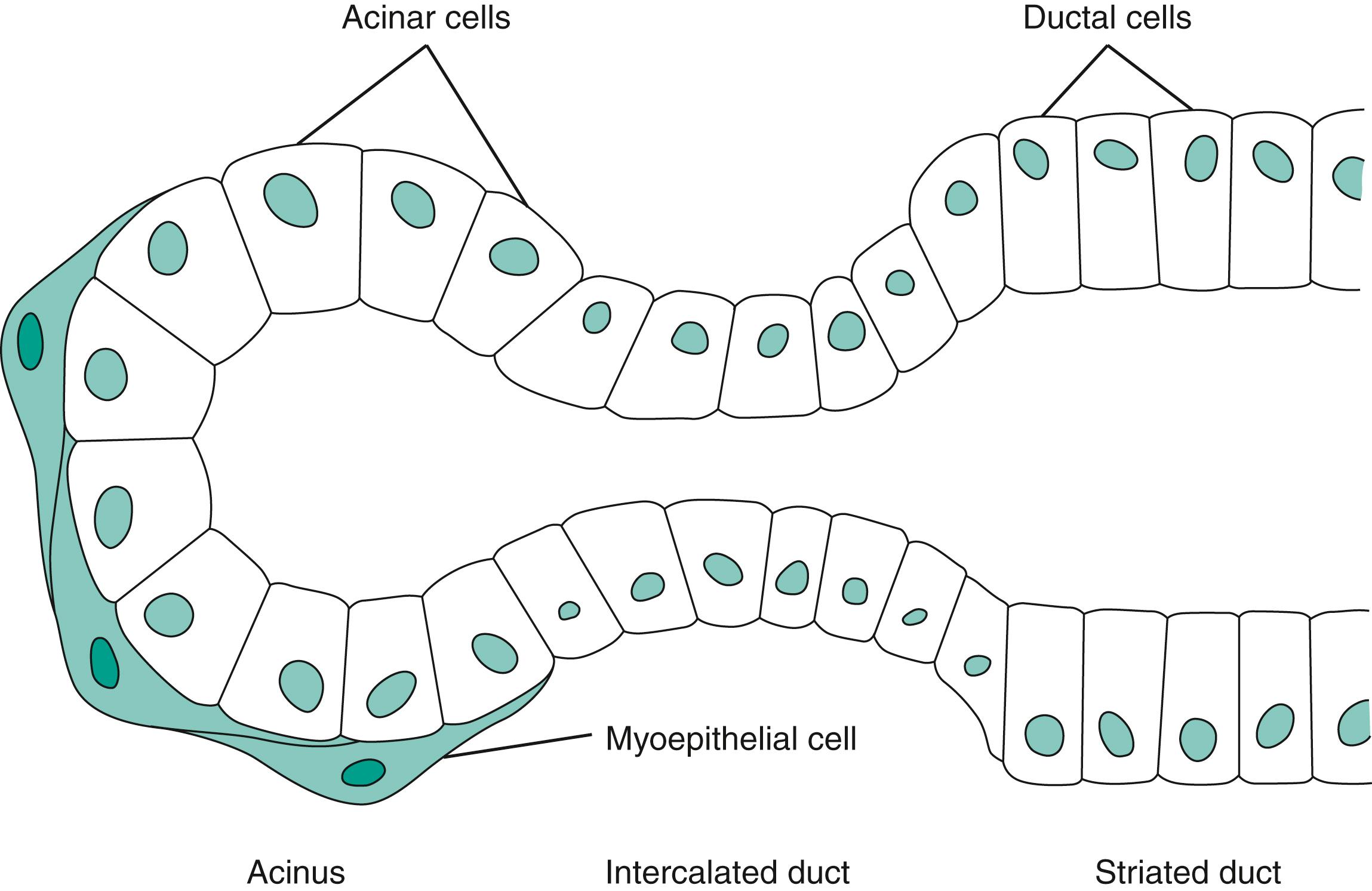
Whenever there is an abrupt need for saliva in the mouth (e.g., immediately before vomiting), myoepithelial cell contraction propels the secretion into the main duct of the gland. Other exocrine glands, such as the mammary glands and the pancreas, also possess myoepithelial cells.
The intercalated duct soon widens to become the striated duct , lined by columnar epithelial cells that resemble the epithelial components of the renal tubule in both shape and function. The saliva in the intercalated duct is similar in ionic composition to plasma. Changes from that composition occur because of ion exchanges in the striated duct. As saliva traverses the striated duct, sodium (Na + ) is actively reabsorbed from the juice, and potassium (K + ) is transported into it. Ca 2+ also enters secreting duct cells during salivation. Similarly, anionic exchange occurs; chloride (Cl − ) is reabsorbed from the saliva, and bicarbonate (
) is added to it.
The striated duct epithelium is considered to be a fairly “tight” sheet membrane. That is, its surface is fairly impermeable to the back-diffusion of water from the saliva into the tissue, and osmotic gradients develop between the saliva and interstitial fluid through the reabsorption of Na + and Cl − . The result is hypotonic saliva.
The blood supplied to the salivary glands is distributed by branches of the external carotid artery. The direction of arterial flow within each salivary gland is opposite the direction of flowing saliva within the ducts of each salivon. The arterioles break up into capillaries around the acini, as well as in nonacinar areas. Blood from nonacinar areas passes through portal venules back to the acinar capillaries, from which a second set of venules then drains all the blood to the systemic venous circulation. The rate of blood flow through resting salivary tissue is approximately 20 times that through muscle. This blood flow in part accounts for the prodigious amounts of saliva produced relative to the weight of the glands.
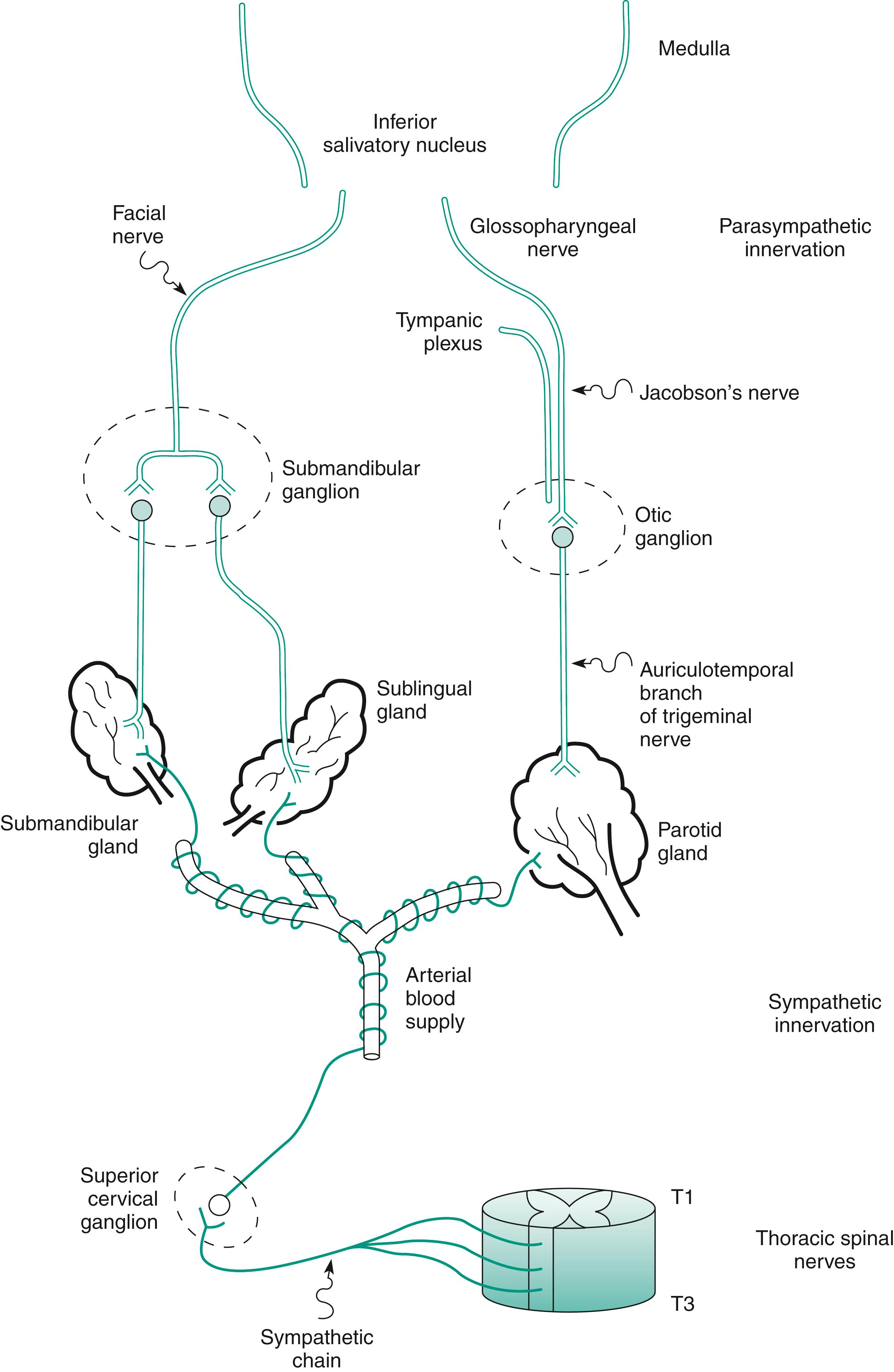
Both components of the ANS reach the salivary glands. The parasympathetic preganglionic fibers are delivered by the facial and glossopharyngeal nerves to autonomic ganglia, from which the postganglionic fibers pass to individual glands. The sympathetic preganglionic nerves originate at the cervical ganglion, whose postganglionic fibers extend to the glands in the periarterial spaces (these relationships appear in Fig. 7.2 ). Parasympathetic and sympathetic mediators regulate all known salivary gland functions to an extraordinary degree. Their influence includes major effects, not only on secretion but also on blood flow, ductular smooth muscle activity, growth, and metabolism of the salivary glands.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here