Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
In the United States trauma is the leading cause of death in people aged 1 through 44. Blunt trauma accounts for the majority of trauma mortality overall, but in urban settings penetrating trauma, including firearm-related injuries, accounts for an increased proportion of trauma deaths. In 2013, more than 33,000 firearm-related deaths occurred in the United States, with many victims arriving at the emergency department (ED) in extremis.
Severe traumatic injuries can be associated with a very high mortality rate. However, on rare occasions an aggressive approach involving the use of emergency department thoracotomy (EDT) leads to survival in patients with impending or recent traumatic arrest. EDT is a dramatic, heroic intervention performed outside the operating room and often in the absence of trained cardiothoracic or trauma surgeons. Though supported as a potential lifesaving procedure, EDT is not a mandated standard of care nor a procedure that is expected to be performed in most EDs. The first successful thoracotomy was reported more than 100 years ago, and the first EDT was reported in 1966. Since then, multiple studies have reported outcomes, indications, techniques, and risks associated with the procedure. In 2003, the National Association of EMS Physicians Standards and Clinical Practice Committee and the American College of Surgeons Committee on Trauma (ACSCOT) proposed specific guidelines for EDT. Several other guidelines have been published without consensus guidelines on the ideal candidates for EDT.
Given the circumstances surrounding the procedure and the associated injuries, few patients survive. The poor overall survival rates, however, should not discourage performance of the procedure in the correct setting and when appropriate surgical backup is available for definitive care.
EDT is not a simple procedure ( ). Identifying specific structures within a chest cavity filled with blood, coupled with a collapsed lung and an injured heart and major vessels, can be formidable. Localizing the injuries that can be reversed quickly and safely is even more difficult.
This chapter focuses on three major objectives: (1) identifying possible indications for and contraindications to EDT, (2) describing the technical aspects of the procedure and adjunctive maneuvers to repair specific injuries, and (3) recognizing the associated risks and complications.
Because of the controversies surrounding EDT, every institution should have guidelines for its appropriate use. An institutional plan for chest wound management and postprocedural care should also be established with the service that will provide backup when members of the surgical team cannot be on site at the time of resuscitation. Debate regarding who should perform EDT is not necessary because everyone who is licensed to perform resuscitative thoracotomy should be trained, competent, and prepared for the technical and initial critical care aspects of patient management. Patient care needs in the event of successful resuscitation should be considered in advance and the surgical and intensive care teams notified so that they can mobilize the appropriate supplies, equipment, and personnel.
In the ED the vast majority of thoracotomies are performed on penetrating trauma patients in cardiac arrest. Beall and coworkers initially proposed EDT for the treatment of penetrating cardiac injuries in 1966. Since then it has been expanded to include extrathoracic injuries, blunt trauma, and nontraumatic pathology. Studies show wide variation in survival rates and outcomes. Taking 50 years of collective EDT data into account, the survival rate of patients undergoing EDT for blunt trauma is nearly 2%, whereas that for penetrating trauma is nearly 10%, but these survival rates depend on many variables and are not applicable to every situation. There is a paucity of data concerning survival rates in patients with EDT performed for nontraumatic causes, and it is not recommended that this procedure be regularly used in these settings.
Make the decision to perform EDT quickly based on whether the patient is likely to benefit from the procedure, has a reasonable chance of survival, and cannot tolerate a delay in operative intervention. In addition, consider the risks associated with performing the procedure. Trauma researchers have identified several factors that are considered crucial when determining who will benefit from EDT ( Box 18.1 ).
Mechanism of injury
Location of injury
Initial cardiac rhythm
Resuscitation (cardiopulmonary) time
Signs of life
The first assessment is made in the prehospital setting, where determination of the mechanism of injury and the presence or absence of a pulse is critical. Multiple guidelines recommend against EDT in patients without a pulse, blunt traumatic mechanisms, and without signs of life. Such patients do not survive, regardless of the intervention. In one of the largest EDT series to date, Branney and coworkers reviewed 868 consecutive patients over a 23-year period. They found that no blunt trauma patients survived EDT when they had no vital signs in the field, but that 2.5% of blunt trauma patients survived EDT when vital signs were present in the field. In 2000 Rhee and colleagues examined 4620 cases of EDT from 24 studies over a 25-year period. The overall survival rate after blunt trauma was just 1.4%, which led to EDT falling out of favor for this indication. Recent articles have challenged the idea of limiting EDT to those in cardiac arrest from penetrating injury only.
The survival rate of pulseless trauma patients sustaining penetrating injury is significantly higher than that of blunt trauma patients. Several penetrating injury subtypes have been studied as follows: firearm injuries, stab wounds, and penetrating explosive injuries. Thoracic stab wounds consistently show the highest rates of survival after EDT. This is theoretically as a result of the decreased amount of tissue damage related to the weapon and the ability to quickly identify anatomic structures and injuries. Penetrating firearm injuries are more likely to result in death because of increased tissue damage from the missile and concussive surrounding forces. Patients with firearm injuries are more likely to have multiple wounds, and the depth of penetration is increased in comparison to stab wounds. One published cohort of combat casualties from explosive penetrating injuries reported similar survival rates to those after firearm-related penetrating injuries.
The location of the penetrating injury helps determine the futility of EDT. A trend toward increased survival rates in patients with thoracic injuries was found in historical data. Isolated cardiac wounds have the highest survival rate after EDT, with approximately 17% of patients surviving the procedure. Penetrating abdominal injuries have beneficial outcomes when EDT is performed to cross-clamp the aorta, with survival rates in the midteens. Extremity injuries rarely require EDT because the use of a tourniquet can control the hemorrhaging until the patient can be transported to the operating room. When EDT is used for traumatic extremity exsanguination survival rates range from 10% to 25%. Patients in cardiac arrest associated with head injuries, especially those with open cranial wounds, have dismal survival rates and are considered poor candidates for further resuscitative efforts, including EDT.
The type of cardiac electrical activity can be helpful in determining who may benefit from EDT. Battistella and colleagues reviewed 604 patients undergoing cardiopulmonary resuscitation (CPR) for traumatic cardiopulmonary arrest and found that of the 212 patients who were in asystole, none survived. Fulton and associates found that of patients in traumatic arrest, survival was improved when the patients exhibited ventricular fibrillation, ventricular tachycardia, or pulseless electrical activity rather than asystole or an idioventricular rhythm. In another study of EDT for traumatic arrest, asystole, idioventricular rhythm, or severe bradycardia was indicative of poor outcomes or an unsalvageable patient.
The duration of pulselessness prior to EDT has traditionally been used as a decision point. With traumatic injury, survival rates and meaningful neurologic outcomes diminish as the duration of CPR increases. The traditional dogma is that any trauma patient who has undergone CPR for longer than 15 minutes has an exceedingly dismal survival rate and further resuscitation should be considered futile. Guidelines from 2013 have questioned the 15-minute dogma and consensus timing on futility of the procedure remains elusive. It is recommended that each institution should develop protocols directing futility decision as it pertains to timing of pulseless activity prior to arrival of the patient in the ED.
Perhaps the most critical determinant of the appropriateness of EDT is whether the patient demonstrates “signs of life.” Signs of life are objective physiologic parameters that are present in patients who survive EDT. They include pupillary response, extremity movement, cardiac electrical activity, measurable or palpable blood pressure, spontaneous ventilation, or the presence of a carotid pulse. The presence of one or more of these indicators has been associated with good neurologic outcomes and increased rates of survival.
Although survival remains the ultimate gauge of the effectiveness of EDT, it is also essential to consider quality of life, especially neurologic function of the patient. It is somewhat surprising that survivors of EDT generally have good neurologic outcomes. Rhee and colleagues reported that 280 of 303 (92.4%) patients discharged after EDT were neurologically intact. It is not possible to accurately predict which patients are likely to survive intact, but the study by Branney and coworkers demonstrated that all survivors with full neurologic recovery had respiratory effort at the scene, and 75% still had respiratory effort on arrival at the ED. The presence or absence of a palpable pulse was not an absolute prognostic indicator in this study. The first 24 hours after EDT rapidly demonstrates which patients are likely to become long-term survivors. Baker and associates showed that with 168 emergency thoracotomies for mixed trauma, most patients with fatal injuries died within 24 hours. Of patients surviving the first 24 hours, 80% (33 of 41) lived and were discharged from the hospital. Full neurologic recovery occurred in 90% of these survivors. Overall only 2.4% (4 of 168) remained severely disabled or in a persistent vegetative state. Guidelines from 2015 show 90% of penetrating trauma patients surviving EDT were neurologically intact on discharge, although this rate falls to near 60% in blunt trauma.
Sixty percent to 80% of cardiac stab wounds result in pericardial effusion regardless of the presence of shock. Tamponade can occur if the wound is smaller than 1 cm in size, depending on which chamber is involved. Wounds larger than 1 cm usually continue to bleed regardless of which chamber is involved. Low-pressure atrial wounds generally form a thrombus before tamponade develops. The thicker-walled left ventricle may spontaneously seal stab wounds up to 1 cm in length. As little as 60 to 100 mL of blood acutely filling the pericardium will impede diastolic filling, reduce stroke volume, decrease cardiac output, and increase release of catecholamine. Catecholamine release may mask the severity of illness because it maintains blood pressure through an increase in peripheral vascular resistance. In penetrating cardiac injury, the right ventricle is the chamber most likely to be involved because of its anterior location, followed by the left ventricle and the atria.
The progression from compensated cardiac function to uncompensated tamponade can be sudden and profound. Although one may suspect tamponade based on well-described signs, clinical diagnosis of pericardial tamponade in an unstable trauma patient is difficult because of the combined effect of hemorrhagic and cardiogenic shock. The classic signs of Beck's triad (distended neck veins, hypotension, and muffled heart sounds) described in 1926 have limited diagnostic value for acute penetrating cardiac trauma. The most reliable signs of tamponade are elevated central venous pressure, hypotension, and tachycardia.
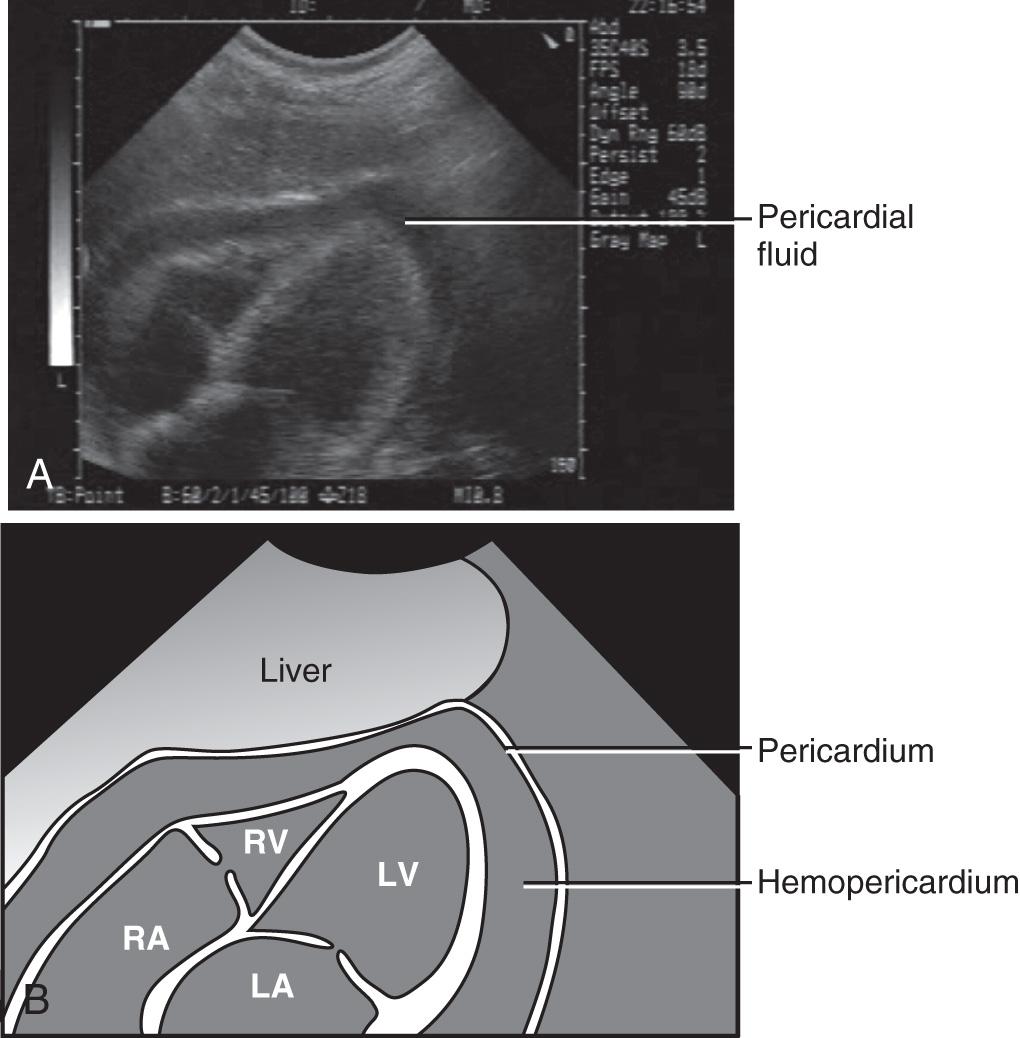
The advent of ultrasound and the focused assessment with sonography in trauma (FAST) examination has improved the diagnosis of pericardial effusion and tamponade. Findings indicative of tamponade include the presence of pericardial fluid with right atrial or ventricular collapse during diastole ( Fig. 18.1 ). FAST is a rapid bedside screening examination used to detect hemopericardium and hemoperitoneum and is now important in the evaluation of unstable trauma patients. From data collected in 1540 patients, Rozycki and associates reported 100% sensitivity and specificity in detecting pericardial and peritoneal fluid in a hypotensive, unstable trauma patient. Ultrasound can have rare false-negative results when pericardial fluid from a cardiac injury decompresses into the thoracic cavity through a wound in the pericardium. A 2015 study by Inaba and colleagues showed a high sensitivity and negative predictive value of FAST exam in determining which patients will not benefit from EDT. In this study the likelihood of survival if pericardial fluid and cardiac motion were both absent was zero.
After EDT for penetrating cardiac wounds, survival is also related to the mechanism of injury. Patients with stab wounds fare better than do patients with gunshot wounds. Rhee and colleagues noted that 16.8% of patients with stab wounds survived to hospital discharge after EDT. Branney and coworkers reported a 29% survival rate in stab wound patients with tamponade, and a 15% survival rate in those without tamponade.
In contrast, gunshot wounds are often large injuries unable to seal themselves; tamponade occurs in only 20%. Patients with penetrating cardiac injuries from gunshot wounds are more likely to initially be seen with profoundly compromised hemodynamics. In addition, the increasing popularity of larger-caliber weapons has made it more difficult to resuscitate patients with gunshot wounds to the chest. Of 112 patients with gunshot wounds to the heart, only 2% survived neurologically intact.
Blunt trauma to the heart can range from minor contusion to cardiac rupture. The most common cause of death after nonpenetrating cardiac injuries is myocardial rupture, and in approximately 25% of such patients the ascending aorta is ruptured simultaneously. Branney and coworkers observed a 2% survival rate in blunt trauma patients resuscitated with EDT. Those who survived had vital signs present in the field. The poor outcomes associated with this type of injury are a result of the poor cardiac function caused by myocardial contusion, even if the hemorrhage has been treated.
Pulmonary injuries can be divided into three types: parenchymal, tracheobronchial, and large vessel. Parenchymal and tracheobronchial injuries rarely require EDT because they are either rapidly fatal or treated initially by tube thoracostomy. Tracheobronchial injury is more common in blunt than in penetrating trauma. Bertelsen and Howitz reviewed 1128 patients at autopsy and found only three to have this injury. The airway is usually maintained, even with complete transection. The stiff tracheobronchial cartilage tends to hold the lumen open, and the paratracheal and parabronchial fasciae preserve the relationship of the proximal to distal bronchi. Ninety percent of tracheobronchial tears occur within 2.5 cm of the carina and most commonly involve the main stem bronchi. Complete division of the trachea is extremely rare. Depending on the size and location of the injury, patients may have massive hemoptysis, airway obstruction, pneumomediastinum, pneumothorax, or tension pneumothorax. Massive subcutaneous emphysema and pneumomediastinum are usually seen, although up to 10% of patients with this injury have no abnormal findings on the initial radiograph. If hemorrhage is profuse or if the site of the injury can be determined, use of a bifid endotracheal tube or unilateral intubation of a main stem bronchus will help secure the airway.
Lacerations of the lung parenchyma that are not accompanied by injury to major vessels generally respond to tube thoracostomy. If the initial chest tube drainage is more than 1500 mL or if there is persistent hypotension or cardiac arrest, consider immediate thoracotomy. For pulmonary injuries, survival after EDT is also related to the mechanism of injury. Branney and coworkers reported a 17% survival rate after pulmonary stab wounds, 3% after gunshot wounds, and 5% after blunt trauma.
Air embolism is a complication of pulmonary parenchymal injuries that may require immediate thoracotomy if the patient is hemodynamically unstable. The development of air embolism after penetrating injuries of the lung is often insidious, and the diagnosis is usually made at the time of thoracotomy. Preoperative and postmortem diagnosis of air embolism is difficult, and it is likely that most air emboli are not detected. Air embolism is confirmed at thoracotomy by needle aspiration of a foamy air-blood mixture from the left or right ventricle or by visualization of air within the coronary arteries.
Air embolism may appear in either the right or the left side of the circulatory system. Involvement of the right side of the circulation is referred to as venous or pulmonary air embolism. Generally, venous air is well tolerated, but death can occur when the volume of air reaches 5 to 8 mL/kg. The rate at which air moves into the circulation and the body's position are important determinants of the volume that can be tolerated. If the body's position allows dispersion of air into the peripheral circulation, more air can be tolerated, although the damage to peripheral structures and end-organs can be extensive. Rapid death usually results from obstruction of the right ventricle or the pulmonary outflow tract. Injuries to the vena cava or the right ventricle can also create portals of entry into the right circulatory system.
Air embolism involving the left side of the circulatory system is referred to as arterial or systemic air embolism. The lethal volume depends on the organs to which it is distributed. As little as 0.5 mL of air in the left anterior descending coronary artery can lead to ventricular fibrillation. Two milliliters of air injected into the cerebral circulation can be fatal. The formation of traumatic bronchovenous fistulas creates potential entry points for air to move into the left side of the circulatory system. The only requirement is the formation of an air-blood gradient conducive to the inward movement of air. Although lowered intravascular pressure from hemorrhage is a risk factor, the most important element in all reports of air embolism has been the use of positive pressure ventilation.
In a review of 447 cases of major thoracic trauma, Yee and coworkers found adequate chart data to suggest the diagnosis of air embolism in 61 patients. Approximately 25% of patients with air embolism have blunt trauma, with associated lung injury secondary to multiple rib fractures or hilar disruption. The overall mortality is higher than 50%.
The diagnosis of air embolism is easily overlooked because the signs and symptoms are similar to those of hypovolemic shock. Two valuable signs that are present in 36% of patients are hemoptysis and the occurrence of cardiac arrest after intubation and ventilation . The development of focal neurologic changes, seizures, or central nervous system dysfunction in the absence of head injury is also suggestive of the diagnosis. Overall, the diagnosis is subtle and must be considered when there is no evidence of the more common causes of extremis in a trauma patient.
In the setting of penetrating abdominal injury, thoracotomy with cross-clamping of the thoracic aorta has been advocated as a means of controlling hemorrhage, redistributing blood flow to the brain and heart, and reducing blood loss below the diaphragm. Unfortunately, aortic cross-clamping can also have detrimental effects. Kralovich and colleagues studied the hemodynamic consequences of aortic occlusion in a swine model of hemorrhagic arrest. There was no difference between groups in return of spontaneous circulation; however, the occluded aorta group experienced statistically greater impairments in left ventricular function and systemic oxygen utilization in the postresuscitation period. Branney and coworkers found that 8 of 76 patients undergoing EDT for penetrating abdominal injury survived neurologically intact. More recently, Seamon and colleagues achieved a 16% survival rate with good neurologic outcomes (8 of 50 patients) when EDT was used before laparotomy for abdominal exsanguination from trauma. Of note, none of the survivors in this study were in cardiac arrest at the time of EDT, but they did have severe hemorrhagic shock, and six of the eight had unmeasurable blood pressure. The resurgence of resuscitative endovascular balloon occlusion of the aorta (REBOA) has changed many institutional trauma algorithms dealing with exsanguinating abdominal and pelvic hemorrhage. Current recommendations suggest that EDT be performed judiciously in patients with abdominal trauma as an adjunct to definitive repair of the abdominal injury.
At present, less than 6% of CPR attempts conducted outside hospital special care units result in survival. The first case of a human survivor of open-chest cardiac massage (OCCM) was reported in 1901. In 1960, Kouwenhoven and associates published favorable survival rates with closed-chest CPR as opposed to OCCM. After further refinement by Pearson and Redding, closed-chest CPR gradually became the preferred method of cardiac compression.
The goal of CPR is to restore coronary perfusion pressure (CPP), which is the prime determinant for return of spontaneous circulation as established in animal models. Paradis and associates found that humans need a minimal CPP of 15 mm Hg to achieve return of spontaneous circulation. Although a CPP of 15 mm Hg does not guarantee return of spontaneous circulation, there is 100% failure of resuscitation if CPP is below this level. Despite the limited number of human studies on OCCM, its hemodynamic superiority over closed-chest CPR is compelling. Del Guercio and coworkers measured cardiac output during both closed-chest CPR and OCCM in in-hospital cardiac arrest patients. OCCM produced a mean cardiac index of 1.31 L/min per m 2 as opposed to 0.6 L/min per m 2 during closed-chest CPR. Boczar and colleagues further examined 10 patients who were unresponsive to closed-chest CPR and measured CPP during closed-chest CPR followed by OCCM. Mean CPP in the closed-chest group was 7.3 mm Hg versus 32.6 mm Hg in the open-chest group. All patients achieved a CPP of at least 20 mm Hg at some time during their OCCM phase. This easily surpassed the minimal CPP required for return of spontaneous circulation. Outcomes after OCCM have not been well established. Animal models suggest not only improved hemodynamic parameters, but also a possible increase in 24-hour survival rates. However, neurologic outcomes are unknown, and the American Heart Association guidelines for CPR do not promote the regular use of OCCM in patients with out-of-hospital cardiac arrest.
At present, the precise indications for open-chest resuscitation after nontraumatic arrest are not well defined, and the procedure is not considered the standard of care. Despite demonstrated hemodynamic superiority in both animal and human models of open-chest versus closed-chest CPR, outcome benefit is lacking. There is a paucity of human data evaluating the window of time during which this treatment can be effective.
In the setting of cardiac arrest from hypothermia, one can consider the use of EDT and OCCM. Cardiopulmonary bypass (CPB) or extracorporeal membrane oxygenation are the most rapid methods of core rewarming, but these methods are sometimes not available immediately. Open thoracotomy with mediastinal irrigation has been used successfully in cases of severe hypothermia with cardiac arrest. Brunette and McVaney reported 11 patients with hypothermic cardiac arrest, 7 of whom underwent EDT with OCCM and mediastinal rewarming. Five patients survived, and all had positive neurologic outcomes despite cardiac arrest times of between 10 and 90 minutes (although one patient died of gastrointestinal hemorrhage and sepsis following resuscitation; the other four patients survived with full neurologic recovery). The other four patients who did not undergo EDT did not survive despite being taken promptly to the operating room for CPB rewarming. Although the number of cases is limited, this study is evidence that OCCM can provide prolonged hemodynamic support and good neurologic outcomes. It should be noted that similar case reports also exist in which closed-chest CPR was maintained for prolonged periods and resulted in successful hypothermic resuscitation. EDT with mediastinal irrigation can produce core rewarming rates as fast as 8°C/hr, with the heart and lungs preferentially being rewarmed first. Mediastinal irrigation involves heating sterile saline in a microwave oven to 40°C and then pouring it slowly over the heart and into the thorax. Performing a thoracotomy for hypothermic arrest does not preclude the use of CPB inasmuch as it was subsequently used after EDT in three of the survivors from the Brunette and McVaney study.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here