Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The term ostomy originates from the Latin word stoma, meaning “opening” or “origin,” and from the Greek word stomat, meaning “mouth.” Historically it is unclear when and how the first ostomies were created, although evidence suggests that the earliest use of fecal diversion was probably related to traumatic fecal fistulas. The first mention of stomas in the surgical literature is by Littre in the early eighteenth century, yet stomas did not become part of surgical practice until decades later, with the creation of ventral and lumbar colostomies for the treatment of imperforate anus and obstructing cancers.
Ileostomies have their origins in the late nineteenth century, when they were used as a means of managing ulcerative colitis. Although the ileostomy was potentially life saving in the treatment of advanced disease, it was soon discovered that the same principles of maturation that were applied to colostomies could not be applied to ileostomies. Early ileostomies that were left to mature spontaneously caused significant morbidity and mortality as a result of serositis, with subsequent development of strictures of the stoma and fluid and electrolyte losses. This constellation of symptoms later became known as “ileostomy dysfunction.” The work of Turnbull and Brooke in the early 1950s was instrumental in resolving these complications. The key was recognition of the causal role of serositis; the cure was to cover the serosa, either with a skin graft (Turnbull) or primary eversion of the bowel (Brooke). The Brooke technique continues to be the standard technique for the creation of ileostomies.
In addition to the many clinicians who have greatly contributed to the development of ostomy surgery and care over the years, enterostomal therapists have contributed hugely to the field. The first school of enterostomal therapists was established in 1961 as a collaboration between Turnbull and one of his former patients, Mrs. Norma Gill. Seven wound, ostomy, and continence nursing accredited programs currently exist throughout the United States, and their contributions to the care of patients with stomas and the management of ostomy complications are invaluable.
The temptation exists for surgeons to regard stoma construction as part of wound closure, which may mean that it is performed by residents. In reality, stoma construction is an important determinant of outcome because an improperly constructed stoma can lead to unnecessary inconvenience, stress, and financial expenditures for the patient. Although ostomy complications are relatively common, in most cases, further surgery is not required for correction. This chapter describes important principles in minimizing the incidence of ostomy complications and covers the specific complications themselves.
Prevention of ostomy complications starts before they are created. Complications are less frequent when stomas are performed electively (37%) than in an emergency (55%). This difference can be explained not only by the difficulties posed by an emergency operation, such as peritonitis/contamination and a dilated bowel, but also by the lack of appropriate preoperative planning. Despite the indication for the stoma or the type of stoma, certain basic steps in the process should always be followed.
Appropriate informed consent and preoperative education is very important. As with any procedure, a full discussion of risks and benefits should be undertaken preoperatively. This step is especially important for ostomy surgery because of the psychological hurdles involved. Many resources are available to patients through the American College of Surgeons and the United Ostomy Associations of America.
Many complications of a dysfunctional ostomy originate in poor placement. A poorly located stoma is prone to hernia, prolapse, skin excoriation from leakage, bleeding from appliance trauma, and parastomal sepsis. Preoperative marking is usually performed by the enterostomal therapist, but any surgeon operating on the bowel should be able to do it himself or herself. The standard locations are within the confines of the rectus abdominis muscle on either side of the midline, at a height that is visible to and accessible by the patient, in a flat area of skin without scars or dimples. This site usually ends up being just lateral and most often inferior but in some cases superior to the umbilicus ( Fig. 90-1 ). Initially the location is chosen with the patient supine, but it is also essential to evaluate the site with the patient standing and sitting.
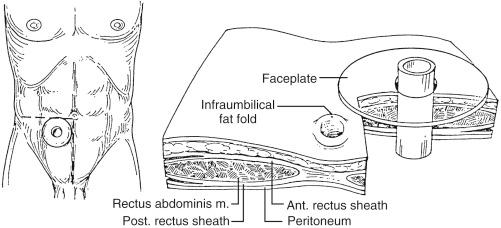
Although various unique situations can lead to difficulty in proper siting of a stoma ( Box 90-1 ), the most common situation encountered is obesity. Extreme care must be taken in assessing the site to avoid placement within a crease or an area where the patient is unable to see or properly care for the stoma. In an obese abdomen, the ostomy is generally placed slightly on the upside of a fold. A more superior location provides better accessibility. Ideally there should be 2 inches of flat skin around the stoma to allow the appliance to adhere properly.
Obese patients
Bilateral paramedian incisions
Pelvic exenteration requiring both fecal and urinary diversions
Radiation of skin-grafted abdominal wall
Disturbed or absent rectus muscles (e.g., transverse rectus abdominis myocutaneous/vertical rectus abdominis myocutaneous flaps and bladder exstrophy)
To set up for the stoma construction, Kocher clamps should be clipped onto the cut edge of the anterior rectus sheath as it is displayed in the incision, and on the dermis. The clamps should be vertically aligned one over the other and kept in line so that the aperture is straight. A folded gauze pack is placed immediately under the site of the intended stoma and held there by the surgeon’s nondominant hand.
The diameter of the stoma aperture is a key to constructing an effective stoma. An ileostomy should protrude about an inch from the abdominal skin as a bud, which means that at least 2 inches of bowel should protrude, tension free, before maturation. To assist in stabilizing the bud, the skin aperture must not be too loose. It should just grip the bowel without narrowing it. Therefore, the diameter depends on the diameter of the bowel itself. A colostomy need not protrude more than 5 mm, and because the bowel is larger than the ileum, the aperture can be more generous. A stoma aperture that is too tight can produce a postoperative bowel obstruction that may appear to be an ileus.
The following steps should be performed:
Incise the subcutaneous fat vertically in the middle of the aperture, using small retractors to deepen the wound to the fascia. Do not remove fat, which is needed to support the stoma.
Incise the anterior rectus sheath vertically. If the bowel is big, small cruciate incisions can be made on either side ( Fig. 90-2 ).
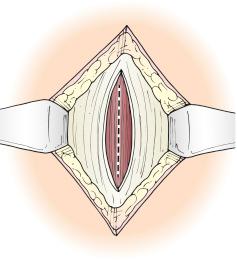
Using a Kelly clamp, separate the rectus fibers in the middle of the wound. Make sure the posterior fascia/peritoneum is visible for the entire length of the incision ( Fig. 90-3 ).
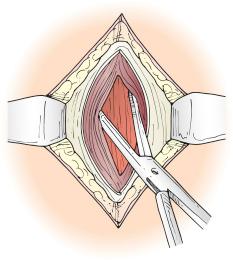
Incise the posterior sheath/peritoneum, pushing up from underneath with the folded sponge. Be careful around the deep epigastric vessels.
Pass a Kelly clamp through the aperture onto the sponge and then into the abdomen. Holding up on the end of the clamp, inspect the inside of the abdominal wall for bleeding ( Fig. 90-4 ).
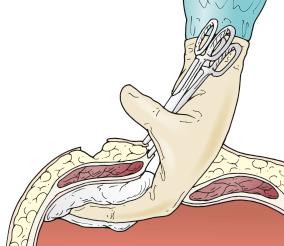
Pass one or two fingers into the aperture and check for diameter. The aperture should match the size of the bowel and its attached mesentery. For an ileostomy, a two-finger aperture is a good size, whereas for a colostomy, a three-finger aperture is usually required ( Fig. 90-5 ).
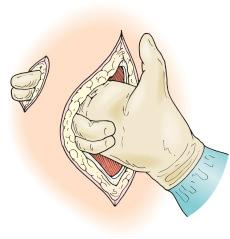
For an ileostomy, the choice of an end stoma versus a loop end is determined prior to making the aperture and is based on the thickness of the abdominal wall and the configuration of the mesentery of the bowel—that is, whether it will allow the end of the ileum to protrude enough to make a satisfactory bud. A trial pull through is part of the decision-making process.
For an end ileostomy, bulky mesenteric fat can be carefully debrided. The bowel is pulled through with the mesenteric edge cephalad. At least 5 to 6 cm should protrude. If the skin aperture is too large it can be narrowed, or supporting sutures can be used (described in the next section).
For a loop ileostomy, pass a tonsil clamp adjacent to the mesenteric margin of the bowel at the apex of the chosen site for the stoma and then bring an umbilical tape through the mesentery, which is used to pull the loop through the abdominal wall. Tag afferent and efferent ileum with different colored sutures. At maturation, the incision in the bowel is just above skin level in the downstream (efferent) limb. This incision needs to be from one mesenteric border to the other. The full thickness of the downstream (diverted) bowel is then sewn to the dermis. No suture that is used to mature an ileostomy should traverse the epidermis because of the risk of the development of mucosal implants, which can produce mucus and encourage lifting of an appliance. The upstream bowel maturation sutures are then placed and tightened while the stoma is gently everted. Sutures are then tied.
If the stoma aperture is too large (i.e., it is not gently gripping the bowel), supporting 0 chromic sutures can be placed between subcutaneous fat and the serosa of the bowel, laterally, and the antimesenteric edge. Alternatively, these sutures can be incorporated into the maturation stitch (“Brooking”). With maturation, subcuticular sutures are used for ileostomies to avoid mucosal implants.
An end ileostomy is a fixed point around which loops of bowel can volve. This can be avoided by sewing the terminal ileal mesentery to the anterior abdominal wall and falciform ligament.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here