Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Lumbar interbody fusion (LIF) is a well-accepted treatment for spinal pathologies. Traditionally, LIF is performed using posterior approaches. These open strategies require broad dissection of the paraspinal musculature and nerve root retraction to access the disk space for interbody fusion. A more refined minimally invasive method, transforaminal lumbar interbody fusion (TLIF), approaches the disk space through a tube via a more posterior oblique trajectory. Access to the disk space is gained through the Kambin’s triangle. This posterior variant approach preserves the contralateral musculoligamentous elements and avoids excessive manipulation of the dural sac. Therefore, many of the complications associated with traditional open posterior approaches are mitigated. TLIF remains an important interbody fusion strategy. Nonetheless, the technique relies on a small surgical window—a particularly limiting factor when attempting more extensive diskectomy, graft placement, and fusion.
Anterior lumbar interbody fusion (ALIF) affords the most impressive fusion area of any surgical technique. The improvements in arthrodesis can be attributed to superb visualization of the disk space. This allows for robust removal of the disk and placement of the graft with maximal biological footprint. Other theoretic benefits of ALIF include avoidance of the spinal canal and the potential for more impressive degrees of correction via sectioning of the anterior longitudinal ligament (ALL). Nonetheless, ALIF is not without significant risks. ALIF requires entry in the abdominal cavity, which may be intraperitoneal or retroperitoneal, and careful dissection of important vascular structures. This puts the patient at risk for potentially devastating hollow-viscous and large-vessel injuries (including the iliac and great vessels). Other important considerations include ureteral injury, sexual dysfunction, and the need for a secondary access surgeon.
Various strategies have been proposed to improve on ALIF. These include laparoscopic, endoscopic, and mini-open approaches. Although strong proponents of these respective methods remain, many now consider laparoscopic strategies as historical stepping-stones. Laparoscopic methods, however, have laid the foundation for the more modern lateral lumbar interbody fusion strategies (LLIF). These include a number of synonyms, namely the direct lateral (DLIF) and extreme lateral (XLIF) approaches.
The LLIF technique allows for lateral exposure of the disk space through a retroperitoneal route. The traditional approach is a transpsoas approach, which allows for clearance of the disk tissue in the anterior column. This approach affords access to the disk space, avoiding the spinal canal posteriorly, and abdominal cavity and large vessels anteriorly. Other benefits of LLIF include no need for a secondary access surgeon, reduced incidence of ileus, preservation of the ALL, lack of bony resections, reduced operative time, reduced hospital stay, and reduced analgesic requirements. These features have slowly made the LLIF an acceptable method for lumbar interbody fusion. Nonetheless, certain issues remain if the transpsoas LLIF is to be embraced as a gold-standard interbody fusion strategy. Chief among them include injury to the lumbar plexus with neurologic injury and access to the lumbosacral junction. In a broader sense, it remains to be seen whether minimally invasive (MIS) techniques such as this can, as a whole, accomplish comparable metrics in global coronal and sagittal alignment.
In this chapter, we discuss an alternative lateral interbody approach, the pre-psoas (oblique) lateral interbody fusion (OLIF) technique. We review anatomic considerations of the approach including the rationale for the shift from a transpsoas to a pre-psoas trajectory and limitations of accessing the L5-S1 disk space via the lateral approach. Our discussion offers a step-by-step description of the technique including patient positioning, preoperative planning, operative procedure, and closure. We discuss common complications and management strategies. In our discussion, we review the available literature for preliminary outcome data and discuss future endeavors moving forward. Finally, we introduce relatively new techniques, such as lordotic cages, used to improve global alignment—a primary limiting factor in MIS correction.
A thorough anatomic understanding is a vital tool in the spinal surgeon’s armamentarium. This is particularly important given the shift toward minimally invasive methods. Surgeons once trained in posterior approaches must now familiarize themselves with the novel anatomic landscape of OLIF.
A comprehensive review must not overlook key anatomic landmarks. The intercrestal line is the theoretic plane between respective superior iliac crests. The landmark classically represents the L4-5 interspace. Surgeons must be weary of variations based on abdominal circumference, body mass index, age, gender, and degree of flexion. Furthermore, the intercrestal line denotes the lower limit of the minimally invasive transpsoas lateral approach as the iliac crest hinders lateral L5-S1 disk space entry. An oblique anterior pre-psoas approach (OLIF) allows surgeons access to the lumbosacral junction avoiding the iliac crest and this could be a distinct advantage of OLIF over LLIF.
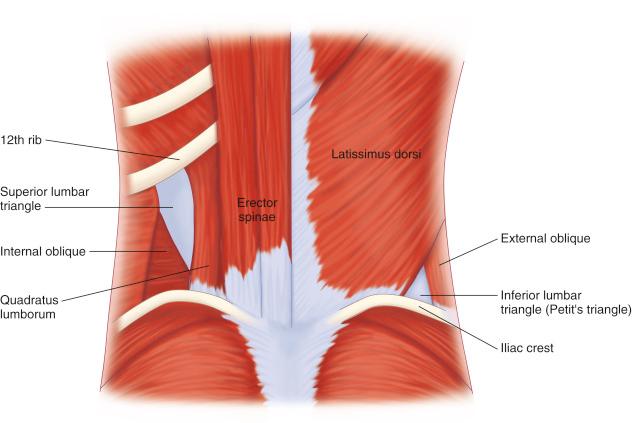
The abdominal musculature consists of the external oblique, internal oblique, and transverse abdominis from superficial to deep. It is important to note the direction of the respective muscle fibers. In particular, the external oblique travels diagonally from the superior-lateral to the inferior-medial direction. This plane is followed during superficial dissection in order to improve cosmesis with closure. Another important consideration is the inferior lumbar triangle, also known as Petit’s triangle ( Fig. 12.1 ). This anatomic space is bordered by the iliac crest inferiorly, latissimus dorsi posteriorly, and external abdominal oblique anteriorly. The area could be targeted during the initial dissection in order to gain access to the retroperitoneal space.
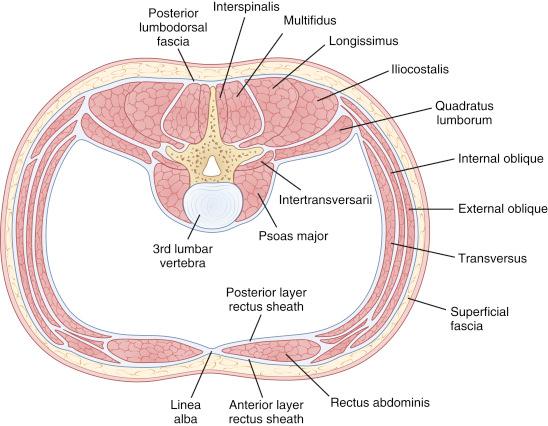
The psoas muscle lies posterior to the retroperitoneal space. It traverses on the lateral surface of vertebral bodies and intervertebral spaces and originates from the anterior surface of the transverse processes from T12 to L5 and eventually inserts inferiorly on the lesser trochanter of the femur. Embedded within the muscle fibers of the psoas run key components of the lumbosacral plexus. Careful attention must be given in order to avoid damage to these neuronal structures. Another important deep muscle is the quadratus lumborum. This spinal stabilizer attaches to the transverse processes, 12th rib, and iliac crest. Fig. 12.2 illustrates the musculature of the lumbar spine.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here