Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Adequate understanding of the underlying pathophysiological disease processes associated with the range of obstetric and gynaecological presentations is essential for the rational evaluation of appropriate investigations, therapies and outcomes. Huge volumes of literature are available on almost all of the topics covered in this chapter, but the most important essential points are summarised in the sections below. A basic understanding of general pathological principles is covered in the first section of the chapter, with the pathologies of some important examples of obstetric and gynaecological entities described later.
There is a limited cellular repertoire of response to injury from a variety of causes including hypoxia (lack of oxygen supply), ischaemia (lack of blood supply), metabolic insults, mechanical trauma, immunological reactions, infections and toxins. Such insults may cause either a temporary impairment of cellular function followed by complete recovery, structural cellular damage with survival but ongoing impairment or, if severe or prolonged, may result in widespread cell death. Control of cellular proliferation and death is also essential for normal tissue turnover regulation and all aspects of embryonic development. The maintenance of normal tissue architecture, whether normal or neoplastic, is dependent upon the balance between cellular proliferation and cell death. At the basic cellular level there are two major types of cell death which may occur in association with the type, severity and timing of insult, namely necrosis and apoptosis.
Necrosis essentially represents a process of severe widespread cellular damage with marked cell swelling and rupture of the membrane. It usually affects sheets of adjacent cells causing disruption of normal tissue architecture with release of mediators and associated inflammation; necrosis is always pathological. Apoptosis, in contrast, essentially represents the controlled or selective death of individual or selected cells within tissues, without significant tissue destruction or associated inflammatory response, and is an essential process in both embryonic development and normal tissue turnover. The process of necrosis is mediated within the cell by rising intracellular calcium concentration, with massive cellular swelling and uncontrolled activation of intracellular enzymes, whereas apoptosis is mediated by controlled activation of specific intracellular enzyme pathways (caspases, transglutaminases and endonucleases) which result in a controlled destruction of the cell and its subsequent phagocytosis and removal.
Following injury due to any mechanism, at a tissue, rather than cellular, level, there are three basic tissue responses which may be stimulated depending on the type and severity of the insult: acute inflammation, wound healing and chronic inflammation.
Acute inflammation is the common and stereotyped tissue response to injury from a wide range of insults. Five classical clinical features are described including redness, heat, swelling, pain and loss of function. The acute inflammatory response is mediated by the activation of a range of vasoactive and chemotactic pathways which result in local vasodilatation, with increased blood flow to the affected area resulting in redness and heat; increased vascular permeability, resulting in exudation of fluid into the interstitial tissue and swelling; and release of numerous mediators which recruit further inflammatory cells to the site and cause pain and loss of function. The primary inflammatory cell mediator of acute inflammation is the neutrophil in the early stage, followed by the macrophage with resolution. Huge numbers of mediators have now been described in association with acute inflammation including histamine, prostaglandins, leukotrienes, bradykinins and complement components in addition to an ever-expanding list of cytokines produced by the inflammatory cells themselves, such as interleukin and tumour necrosis factor families. With removal or reduction of the inciting agent, the later stages of acute inflammation merge imperceptibly with the process of tissue repair and wound healing described below. Fig. 6.1 shows acute inflammation in fetal membranes in a pregnancy complicated by chorioamnionitis.
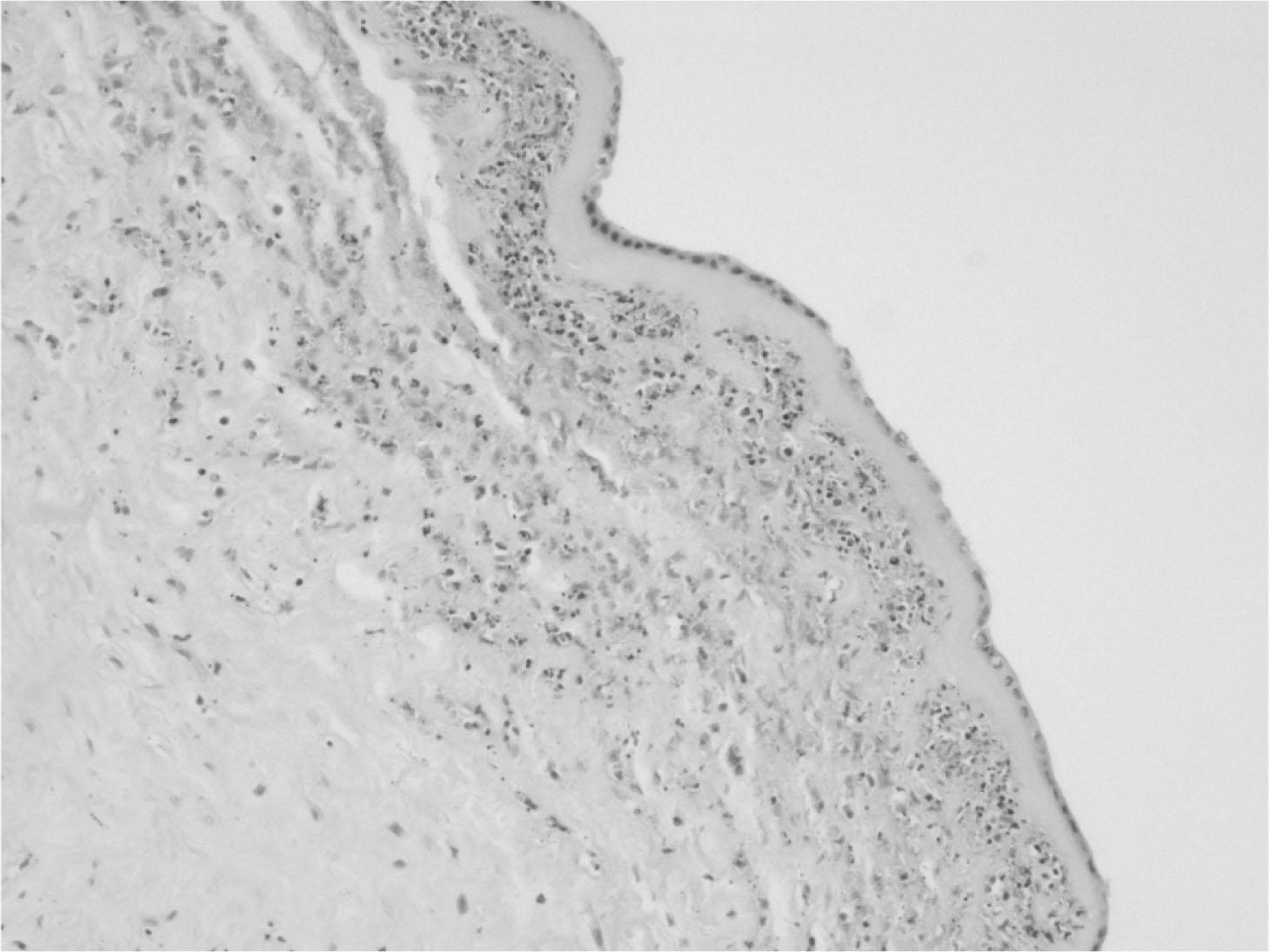
The process of tissue repair or healing may involve either regeneration of the tissue to its original state by replacement of dead or damaged cells by proliferation of cells of the same type, or repair and organisation, in which new connective or scar tissue replaces the original tissue. The type of process to occur depends upon the timing, severity and extent of the insult, in addition to the underlying characteristics of the tissues involved.
An example of this process is the healing of skin wounds. In wounds with closely opposed edges, healing can occur by first intention, in which an initial blood clot forms followed by cellular proliferation and migration of the marginal epidermis across the clot to bridge the defect with proliferation of blood vessels and fibroblasts into the wound edges in the underlying connective tissue to form loose granulation-type tissue which is then remodelled over time. In skin wounds in which the edges are widely separated (healing by secondary intention), there is similar, but more extensive, formation of granulation tissue but since the epithelial proliferation cannot rapidly bridge the defect, there is ongoing remodelling, with wound contraction secondary to the presence of myofibroblasts and replacement of the original tissue by scarring. The process of wound healing is further influenced by additional factors such as the local blood supply, the presence of infection or foreign bodies, excessive movement at the site or other systemic factors such as metabolic abnormalities. Defective wound healing may therefore result in either inadequate union and wound dehiscence or excessive production of scar tissue such as hypertrophic scars or keloid formation. It is clear that the control of the process of wound healing is complex and dependent upon large numbers of mediators such as transforming growth factor beta and epidermal growth factor, the manipulation of which may allow novel interventions in the future. It should also be noted that there are marked differences in the potential responses to injury between different tissues and at different stages in development, with fetal wound healing and remodelling, for example, occurring very rapidly.
Histologically, chronic inflammation is defined as an inflammatory process that is occurring simultaneously with attempted healing, rather than a simple sequential process following acute inflammation. It should therefore be noted that it may often be clinically impossible to distinguish between ongoing acute and chronic inflammation, the two potential mechanisms being persistence of a low-grade inflammatory stimulus that initially induced an acute inflammatory response, or a process involving chronic inflammation from its outset. The characteristic histopathological features of chronic inflammation are the presence of predominant mononuclear inflammatory cells, in particular lymphocytes, plasma cells and macrophages, in association with fibroblast proliferation. Many immunological diseases are associated with such chronic inflammatory responses from their outset. A specific type of chronic inflammation is termed granulomatous inflammation, which represents prominent collections of epithelioid macrophages within tissues as a consequence of either an immunological reaction or the presence of foreign organisms or material which cannot be digested and removed by macrophages ( Fig. 6.2 ). It should be noted that granulomatous inflammation and granulation tissue are entirely different processes.
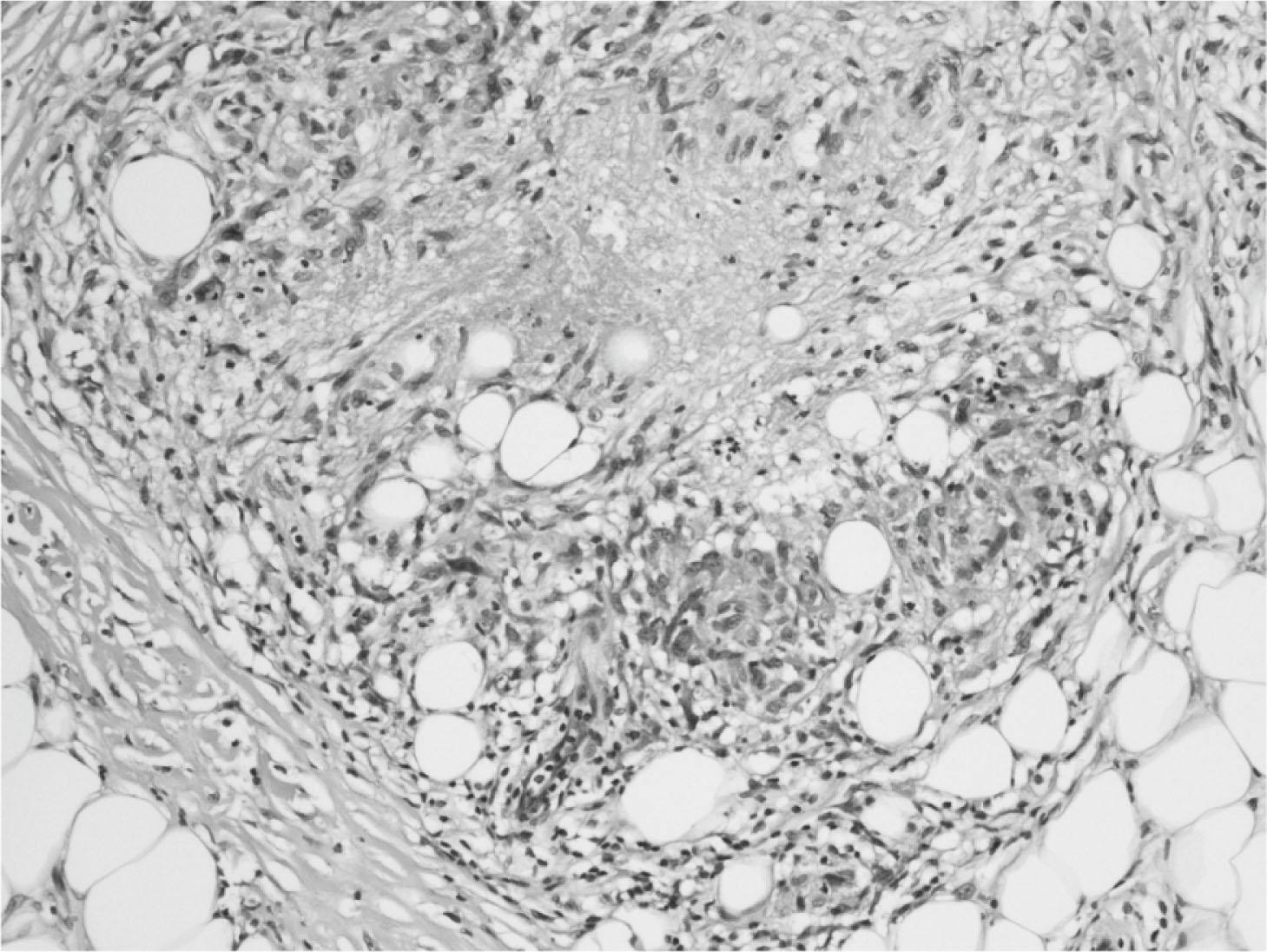
In normal tissue there is very strict control of cellular growth, proliferation, death and differentiation. Several types of abnormal tissue response may occur.
Hyperplasia represents an increase in the number of cells in a tissue or organ, which may be physiological, such as during pregnancy, or pathological, such as with oestrogen-induced endometrial hyperplasia
Hypoplasia is a reduction in cell number within an organ or tissue, which may also be physiological or pathological
Atrophy represents a potentially reversible reduction in mass of the tissue, with atrophic cells usually being smaller than normal. This may also be physiological, such as in postmenopausal endometrial atrophy, or pathological, such as tissue atrophy following damaged nerve or blood supply
Hypertrophy represents a potentially reversible increase in cell size, which may be physiological, such as the uterus in pregnancy, or pathological, such as myocardial hypertrophy in hypertension
Metaplasia represents the change in cellular phenotype from one fully differentiated state to another, and usually occurs from stem cells in epithelia, the most common example being columnar to squamous metaplasia of the transformation zone of the cervix (see later)
Epithelial dysplasia represents the presence of cytological changes associated with malignancy but in the absence of abnormalities of underlying tissue architecture with an intact basement membrane. For many tumours, there is thought to be a clear pathway of progression from low-grade to high-grade dysplasia through to invasive carcinoma, the primary example of which being cervical intraepithelial neoplasia (CIN) as a forerunner of invasive squamous cell carcinoma of the cervix (see later)
Neoplasia represents the process of new growth of cells
Tumour represents a distinct mass lesion, and hence not all tumours are neoplasms
Tumours may be simply classified as benign or malignant, and primary (arising at the site) or secondary (metastatic from another site), with specific subtyping, grading and staging on the basis of clinical and histopathological features.
Neoplasms may be benign or malignant. In general terms, benign neoplasms are usually localised, do not exhibit local destructive infiltration, do not metastasise and are often composed of relatively well differentiated cells. Malignant neoplasms demonstrate local destructive invasion of the surrounding normal tissue and the ability to metastasise (grow at sites distant from the site of origin). Despite these apparently clear-cut definitions, in a range of clinical situations, the precise distinction between a benign and malignant neoplasm may be extremely difficult, although most of these are not of significance to the obstetrician and gynaecologist.
The terminology commonly used for many neoplasms implies their benign or malignant nature from the nomenclature. For example, benign mesenchymal neoplasms usually have the suffix ‘oma’, such as a leiomyoma, whereas malignant mesenchymal neoplasms usually have the suffix ‘sarcoma’, such as a leiomyosarcoma. Malignant epithelial neoplasms are termed carcinomas and many paediatric malignancies that mimic embryonal tissues are termed blastomas. Malignant neoplasms of haematological stem cells in the bone marrow are termed leukaemias, whereas other malignancies of lymphoid tissue are termed lymphomas. There are well described specific and detailed classification systems and staging systems (extent of spread) for all described malignancies from the World Health Organization (WHO) and, in the context of gynaecological malignancies, the International Federation of Gynecology and Obstetrics (FIGO).
Malignancies are defined histopathologically on the basis of abnormalities of tissue architecture and cytological features. There is loss of the normal well-defined microarchitecture, with destruction of the underlying basement membrane in the case of carcinomas, and invasion of the surrounding tissue by malignant cells. Cytological features of malignancy in general include abnormal nuclear shape and size, abnormal mitoses and an increased nuclear to cytoplasmic ratio. In addition, many malignant cells demonstrate reduced or abnormal differentiation. (It should be noted here that the cell of origin of a tumour is not necessarily the same as the phenotype to which it is differentiating.) Neoplasms are a consequence of abnormalities in the normal cellular proliferation and differentiation control mechanisms, the majority of which are associated with either activation of oncogenes or loss of function of tumour suppressor genes.
The female genital tract essentially almost entirely develops from the müllerian duct system embryologically, with part paired and part fused areas, resulting in development of the fallopian tubes, uterus, cervix and upper vagina, in addition to the embryologically distinct ovaries. The female genital tract is lined by a range of different types of epithelium along its length ranging from vaginal squamous epithelium, through uterine columnar epithelium and tubal ciliated epithelium. The ovary is composed of a mixture of germ cells (oocytes) among ovarian stroma and covering epithelium. The range of pathologies encountered may therefore be related to any of the above elements depending on the specific site, age and other aetiological factors, with the most common tumours being related to the underlying histological structures.
The male genital tract is also composed of paired gonads, with germ cells surrounded by epithelium and connective tissue, connected to the external by a tubal system, but in males the müllerian ducts regress, the functional ductal system being developed from the wolffian system. Therefore, although the potential spectrum of pathologies which may affect male and female gonads is similar, the specific types and distributions of neoplasms significantly differ; for example, across all ages in males, testicular germ cell tumours in younger men represent the most common neoplasms, whereas the predominant neoplasm in females is ovarian carcinoma in older women.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here