Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
The authors wish to thank Rajiv Varma and Shelley D. Williams for their work on this chapter in the previous edition.
The primary objective of the neurologic examination is to assess the functional integrity of the central nervous system (CNS) and the peripheral nervous system (PNS) and to detect and localize any sites of neurologic dysfunction. Techniques and interpretation of the pediatric neurologic examination are based largely on knowledge of normal growth and development. The examination is preceded by a thorough history of the presenting problem, including timing and mode of onset; course; and a past medical history that focuses on the antenatal, perinatal, and neonatal periods for possible prior insults (e.g., bleeding, infection, hypoxia, drugs, and/or trauma). Abnormalities of birth weight; the need for resuscitation after delivery; early neonatal problems with hypoglycemia, hypocalcemia, or severe jaundice; and abnormalities in activity or difficulty feeding shortly after birth often serve as red flags. This is followed by a detailed history of behavior; growth and development with attention to evidence of delay, slowing, cessation, or regression of developmental milestones; and any possible association with prior illness or trauma. Obtaining a family history of neurologic, neuromuscular, or developmental problems is also important.
The systematic neurologic evaluation proceeds from assessment of mental status and language functions through evaluation of cranial nerves, gross motor function, muscle strength, gait and station, balance and coordination, sensory systems, and deep tendon reflexes. It is applicable to older children and adolescents without significant modification from the evaluation geared to the adult. Tools essential to the neurologist include the reflex hammer, bright penlight, ophthalmoscope, and stethoscope. For evaluation of the primary sensory modalities of light touch, pain, temperature, and vibration, wisps of cotton, sterile broken cotton tipped applicators, and a tuning fork are used. A collection of small, common objects (e.g., coins, buttons, keys) to be identified by feel alone are useful for assessment of cortical sensations of stereognosis. Derangements of primary sensory function may be present with lesions at the level of the nerve roots, plexuses, or peripheral nerves. If a particular area of decreased sensation is identified in part of a limb, careful delineation of its boundaries often suggests root (dermatomal), plexus, or peripheral nerve involvement ( Fig. 16.1 ).
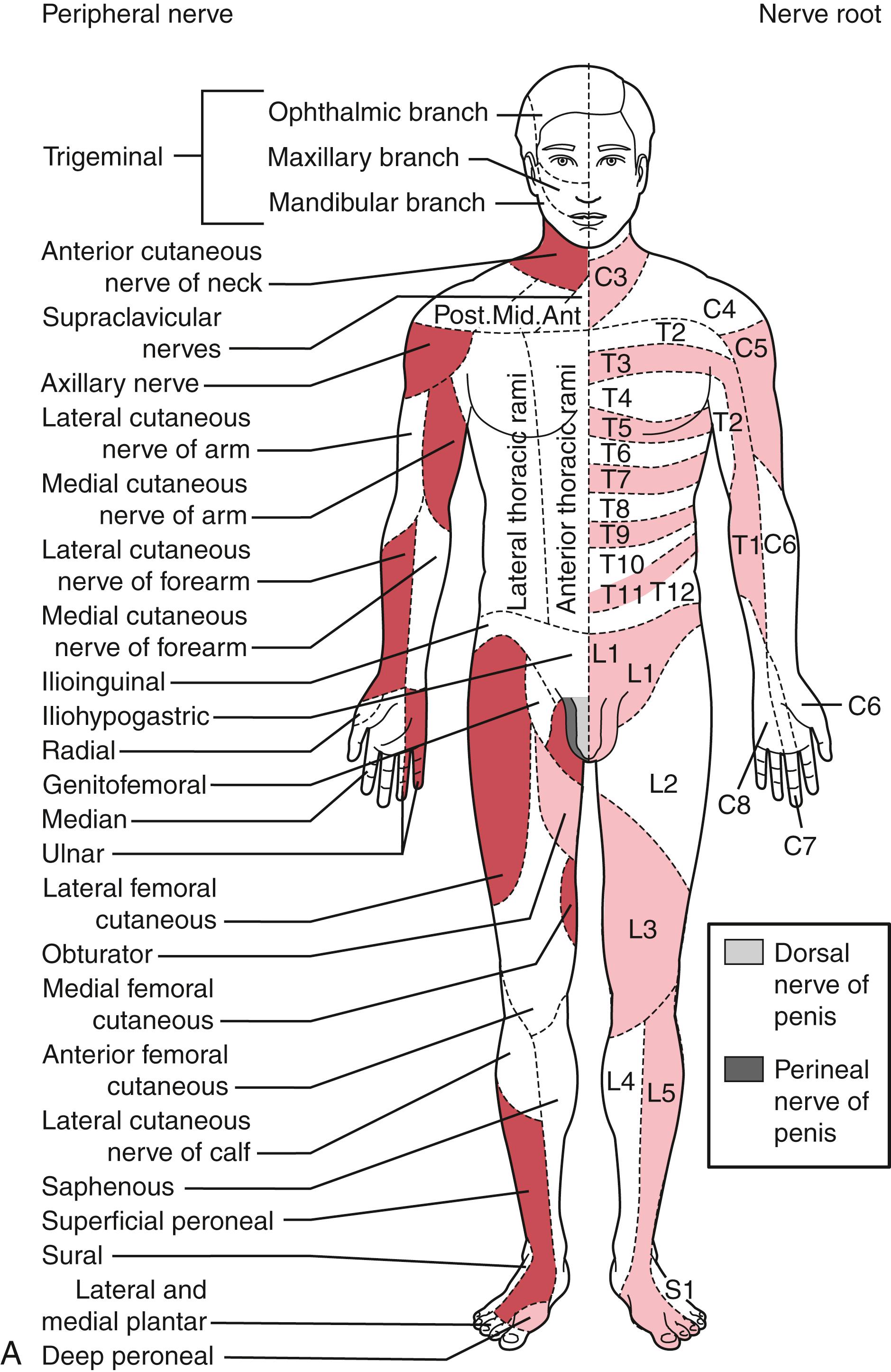
Neurologic examination of the younger child requires flexibility and a gentle, staged approach. The first stage consists of observation, much of which can be done while taking the history as the infant sits in the parent’s lap or while the toddler or older child plays with toys. The child’s level of alertness and interest in people and the environment are assessed. Facies, head shape, body habitus, spontaneous movements, position, and posture are noted, along with spontaneous vocalizations and quality and pitch of cry in infants. In the child old enough to walk, stance and gait, as well as the ability to run, stoop, and recover; climb onto a stool; and rise from the floor (when developmentally appropriate) are observed. These observations provide a good general impression of the child’s developmental level and abilities.
Much of the remainder of the neurologic examination also lends itself to play, and in the second stage of observation a more detailed assessment of mental status, language, handedness, and fine and gross motor skills is performed by engaging the child in play. A selection of rattles, keys, spinning and mechanical toys, dolls, cars, small blocks, noise makers, tennis balls, hand puppets, crayons, and picture books supplement the traditional instruments. If further observation of gait is necessary, the examiner can have the child walk to or with the parent. Children older than 4 years old love to show what they can do when asked to walk on their heels or toes, hop, or do tandem gait along a line. Pat-a-cake games are popular for testing rapidly alternating movements with young children. Then, with the child comfortable and rapport established, the hands-on examination is initiated with the child still dressed and in the parent’s lap. Trying to catch the otoscope light as it is shown over various parts of the body can act as the prologue to following the light with the eyes and looking at it. For infants and toddlers, following a face or spinning toy is still better for testing extraocular movements. Having a parent jingle keys at the child’s eye level and asking the child to look at the object assists the ophthalmoscopic examination in older preschool and young school-age children. Asking young children to make faces, stick out their tongues, and blow up balloons is another helpful technique in assessing cranial nerves.
Tone is assessed by observing resistance to passive motion. Then active motion and motion against resistance are checked (strength). Older preschoolers and school-age children love showing their muscles, and push/pull games can be used to test muscle strength, especially when the child’s efforts are admired. Deep tendon reflexes can often be tested at this time with only the shoes off. These are normally brisk, or 3+, in the young infant, becoming 2+ by 6 months old. If directly tapping on the tendon seems upsetting to the child, it may help to place a finger over the tendon to be percussed and tap that. In infants and toddlers, it is often easier to elicit the ankle jerk by placing a finger over the ball of the child’s foot and gently dorsiflexing it before percussing the Achilles tendon. Preschoolers and young children love having the examiner express surprise and pleasure when reflexes are elicited.
Finally the parent is asked to help undress the child, and the remainder of the examination proceeds with the parent providing reassurance and assistance as needed. During this stage, head circumference is measured in the infant and toddler, and the head, midline of the neck and back, and skin are carefully examined for abnormalities. Muscles are inspected for symmetry, and extremity circumference is measured a set distance from a bony landmark if asymmetry is suspected, and abnormal muscle movements are noted. The appropriate disappearance or persistence of primitive reflexes is determined in infants (see Chapter 3 ). The Babinski reflex is difficult to elicit and interpret during the first year of life because stroking the sole of the foot may simply stimulate withdrawal or plantar flexion. Evaluation of sensation is difficult in the younger child and is generally limited to appreciation of light touch and pinprick. These may be assessed using a sterile broken cotton tipped applicator.
Neurologic examination of the newborn is highly specialized. The essential components of the neonatal examination include assessment of gestational age, growth patterns, dysmorphic features, motor tone, postures, spontaneous activity, cry, respiratory patterns, brainstem reflexes, response to bright light, response to noxious stimuli, developmental reflexes, and deep tendon reflexes (see Chapter 2 ). Normal findings vary with gestational age. The immaturity of the newborn’s CNS, with functioning largely at a subcortical reflex level, may conceal all but the most severe neurologic deficits—hence the often-deceptive normal examination of the newborn with hydranencephaly.
The most prevalent neurologic disorders in childhood are related to CNS infection, ingestions, congenital malformations, perinatal insults, trauma (including abuse), progressive neurodegenerative or neuromuscular processes, and metabolic disorders. This chapter concentrates on selected neurologic disorders accompanied by physical signs that can be detected on visual inspection.
The neurocutaneous syndromes or phakomatoses are congenital disorders with prominent cutaneous and neurologic manifestations, often arising from identified defects in specific gene loci. The simultaneous involvement of the skin and nervous system, both derivatives of embryonic ectoderm, suggests that these disorders may be caused by an unknown abnormality of the embryonic epiblast. Although the clinical and pathologic features of the phakomatoses are diverse, these syndromes share a propensity for malformations and hamartomatous tumors of multiple organs. Among the more frequently encountered phakomatoses are neurofibromatosis, tuberous sclerosis (TS), Sturge-Weber syndrome, ataxia-telangiectasia, and linear sebaceous nevus.
Neurofibromatosis 1 (NF-1; previously known as von Recklinghausen disease ) is the most common of the neurocutaneous syndromes and affects about 1 in 3000 individuals. Although usually inherited as an autosomal dominant disorder, up to 50% of cases may be sporadic. Molecular genetic testing for mutations of the NF1 gene is clinically available and is able to detect up to 90% of gene mutations. The NF1 gene has been localized to chromosome 17q. Neurofibromin, its gene product, acts as a tumor suppressor of the RAS/MAPK pathway, and its function is altered in affected patients. Characteristic clinical manifestations include multiple hyperpigmented skin macules (café-au-lait spots), axillary or inguinal freckling, multiple skin neurofibromas, and iris hamartomas (Lisch nodules). Associated abnormalities may include optic gliomas; other CNS tumors of glial or meningeal origin; neurofibromas of spinal or peripheral nerves; pheochromocytoma, macrocephaly, and cognitive impairment; and bony abnormalities. Diagnostic criteria for NF-1 are summarized in Box 16.1 .
Diagnostic criteria are met if two or more of the following are found:
Six or more café-au-lait macules >5 mm in greatest diameter in prepubertal children and >15 mm in greatest diameter in postpubertal individuals
Two or more neurofibromas of any type or one plexiform neurofibroma
Axillary or inguinal freckling
Optic glioma
Two or more Lisch nodules (iris hamartomas)
A distinctive osseous lesion, such as a sphenoid dysplasia or thinning of long bone cortex with or without pseudarthrosis
A first-degree relative (i.e., parent, sibling, or child) with NF-1, according to these criteria
Multiple café-au-lait spots, the most frequently encountered cutaneous abnormality, are brown hyperpigmented macules with smooth margins, usually most numerous over the trunk ( Fig. 16.2A ; and see Fig. 8.123 ). Other abnormalities of cutaneous pigmentation may include axillary or inguinal freckling or extensive areas of hyperpigmentation (see Fig. 16.2B and C ). Hyperpigmented skin lesions almost always precede neurologic symptoms and often increase in size and number with advancing age. They are not necessarily present at birth and may be inconspicuous in early childhood, becoming more prominent at puberty. Ninety-seven percent of patients with NF-1 have at least five café-au-lait spots by 20 years old.
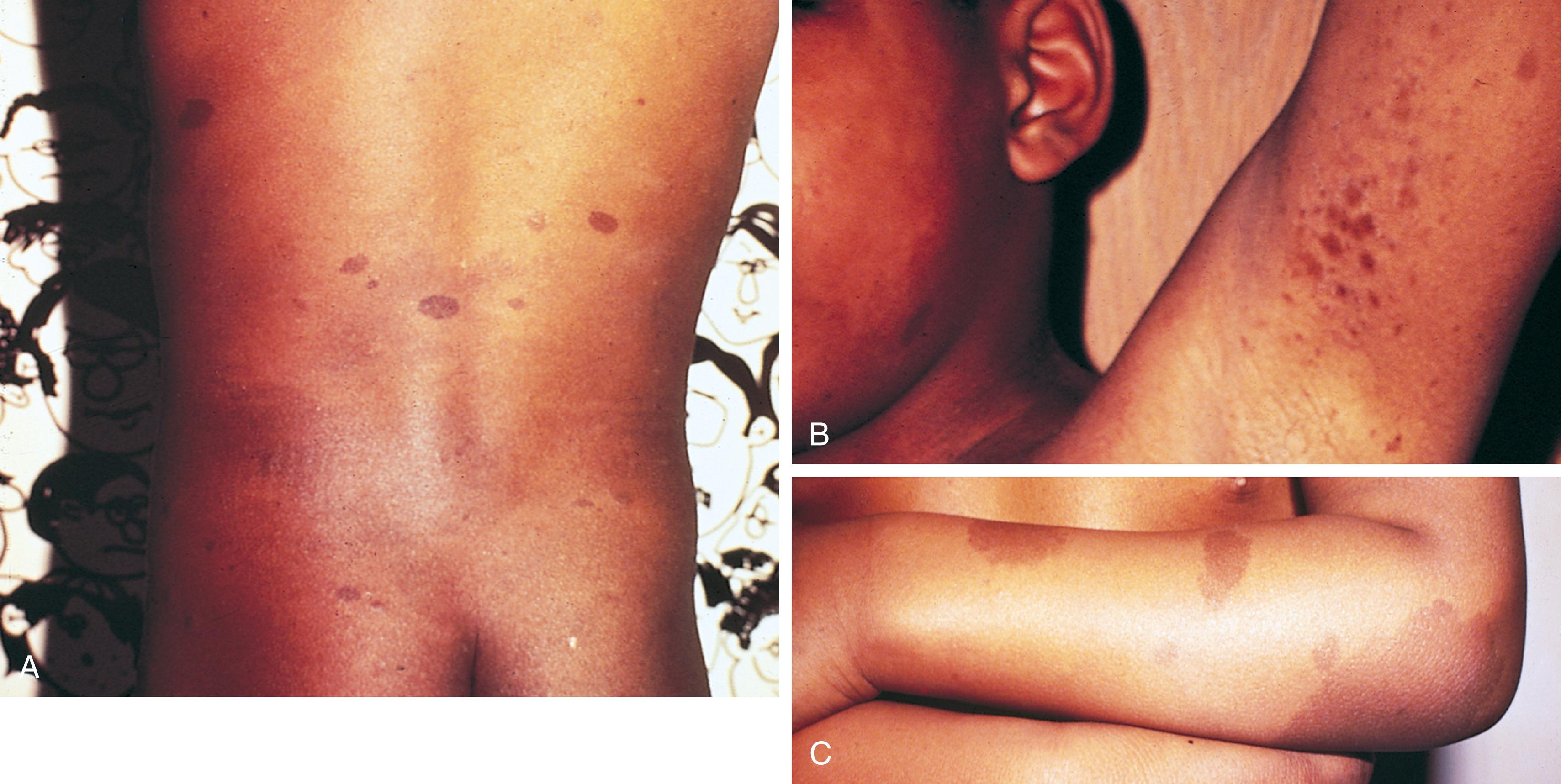
Although multiple café-au-lait spots are a clinical hallmark of NF-1, they may also occur as an autosomal dominant trait unassociated with the other features of neurofibromatosis. Genetic investigations in such families have excluded linkage to the NF1 locus on chromosome 17, indicating a distinctly different genetic association. Multiple café-au-lait spots can be found, as well, in a variety of other conditions ( Table 16.1 ). Legius syndrome involves a mutation in the SPRED1 gene also involved in the RAS/MAPK pathway. Legius syndrome is associated with the same cutaneous markers (café au lait macules and freckling) as NF1 and learning disabilities, but not the tumorigenesis. Café au lait spots are a prominent feature of McCune-Albright syndrome, the additional manifestations of which include skeletal dysplasia and endocrine abnormalities. Those seen in McCune-Albright syndrome are often large and have irregular (“coast of Maine”) margins (see Fig. 8.123 D), in contrast to the smooth (“coast of California”) borders characteristic of the hyperpigmented lesions of NF-1. Café-au-lait spots also may be encountered in TS and neurofibromatosis 2 (NF-2) but are seldom prominent. They are present in about 10% of the general population (typically four or less in number) and are not by themselves a sign of disease.
| Disorder | Clinical Features |
|---|---|
| Neurofibromatosis | Most common in NF-1, rare in NF-2 (see sections on NF-1 and NF-2 and Box 16.2 ) |
| Tuberous sclerosis (TS) | See Box 16.3 |
| McCune-Albright syndrome | Polyostotic fibrous dysplasia, precocious puberty, endocrine dysfunction |
| Watson syndrome | Features of Noonan syndrome (webbed neck, hypertelorism with antimongoloid slant, low-set ears, pulmonic stenosis, low intelligence), plus meets criteria for NF-1 |
| Epidermal nevus syndrome | Verrucous skin lesions, scoliosis, aortic coarctation, intellectual disability |
| Bloom syndrome | Severe intrauterine and postnatal growth retardation, photosensitivity, telangiectatic erythema of cheeks/face |
| Ataxia-telangiectasia | Ataxia, conjunctival telangiectasia, recurrent sinopulmonary infections |
| Silver syndrome | Intrauterine growth retardation, hemihypertrophy, syndactyly, triangular facies, premature sexual development |
| Gaucher disease | Opisthotonos, splenomegaly, cranial nerve dysfunction, regression of motor milestones |
| Turner syndrome | Short stature, webbed neck, coarctation of aorta, delayed puberty |
| Fanconi anemia | Aplastic anemia, hyperpigmentation, short stature, intellectual disability, congenital anomalies of bone, heart, eye, kidney |
| Multiple lentigines (LEOPARD) syndrome | Multiple small lentigines, hypertelorism, pulmonic stenosis, cryptorchidism, mild growth retardation, sensorineural deafness |
Additional cutaneous manifestations of NF-1 may include extensive plexiform neuromas at the terminal distribution of nerve fibers ( Fig. 16.3 and see Fig. 8.84 ) or small subcutaneous nodules—neurofibromas—scattered along the course of nerve trunks ( Fig. 16.4 ).
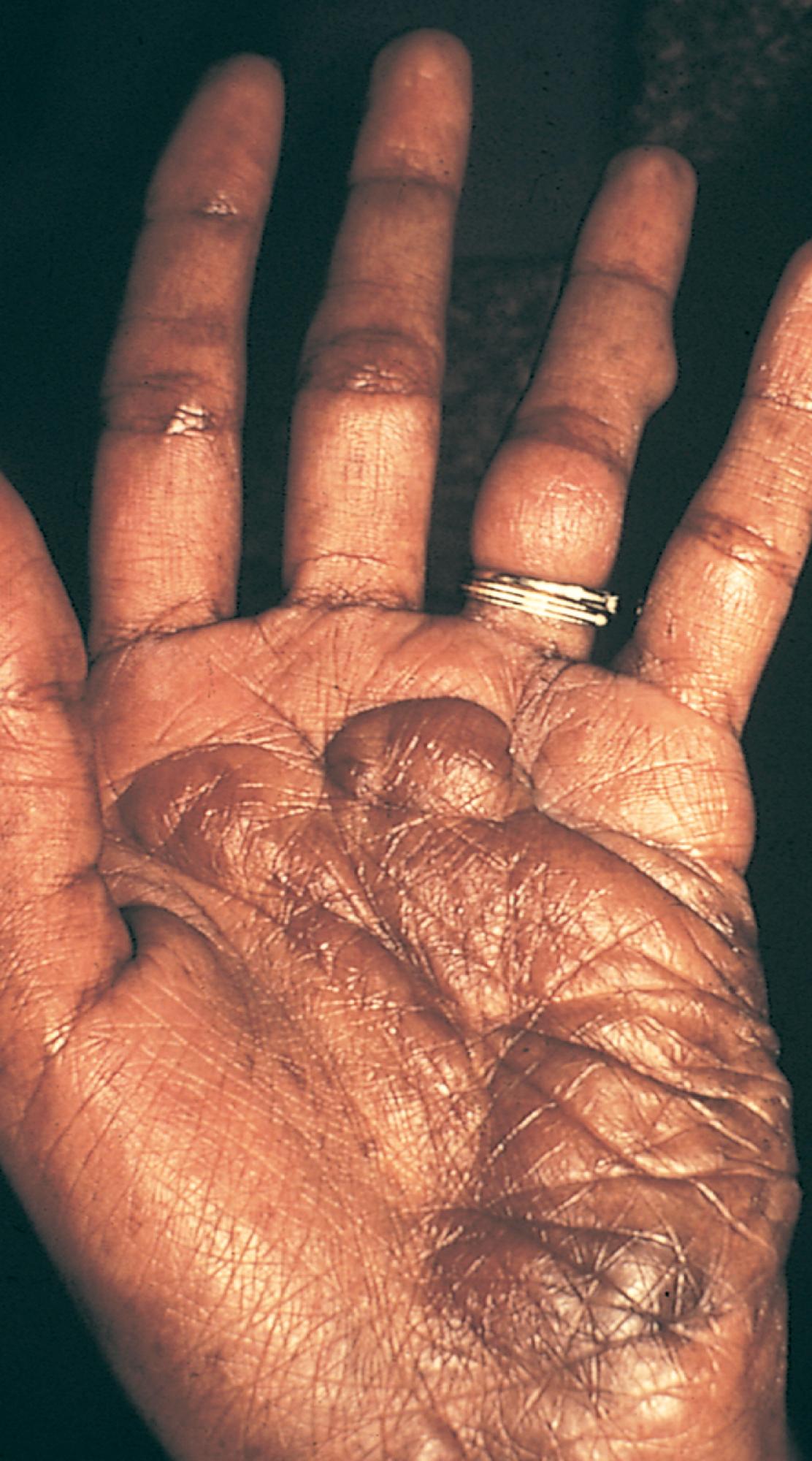
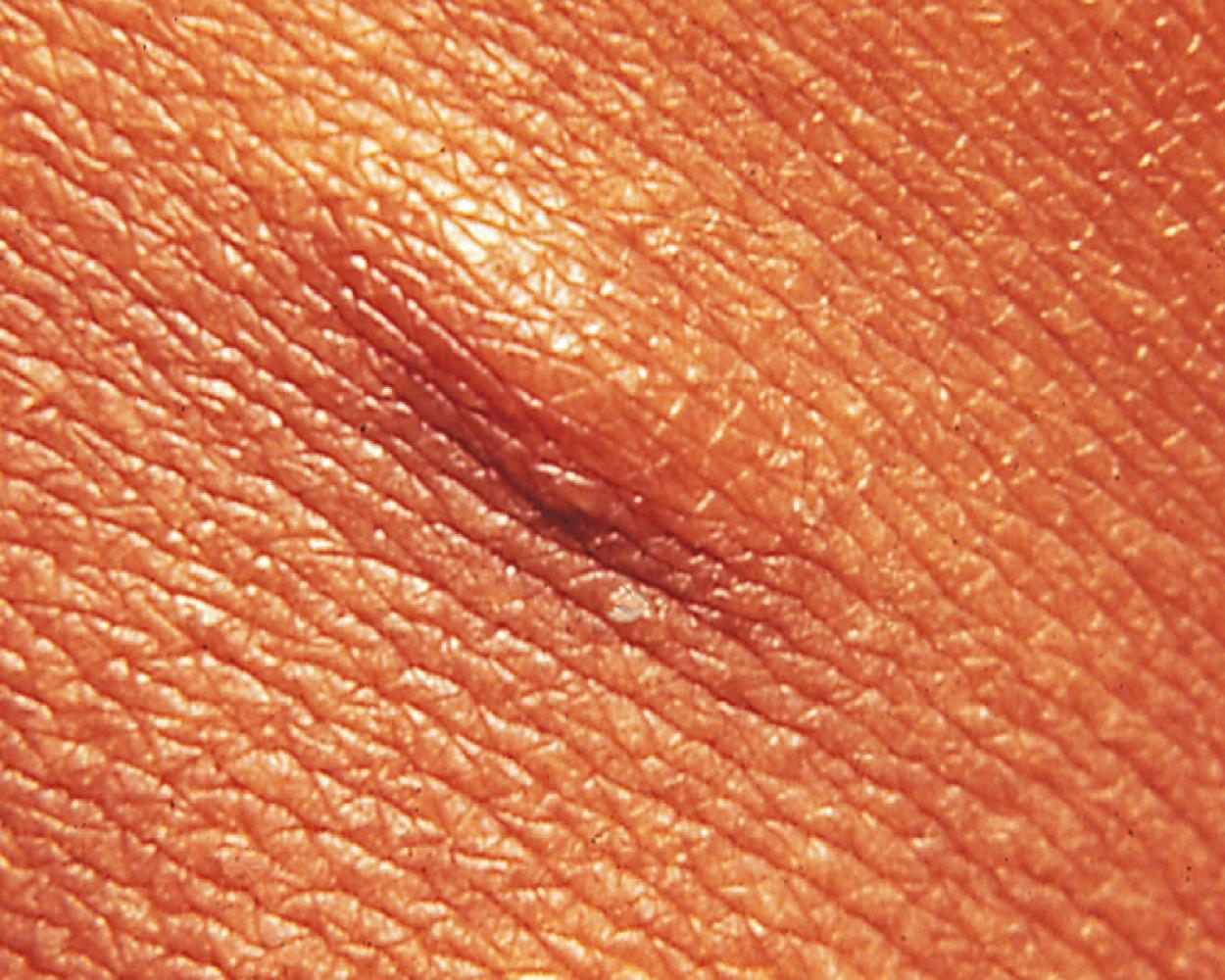
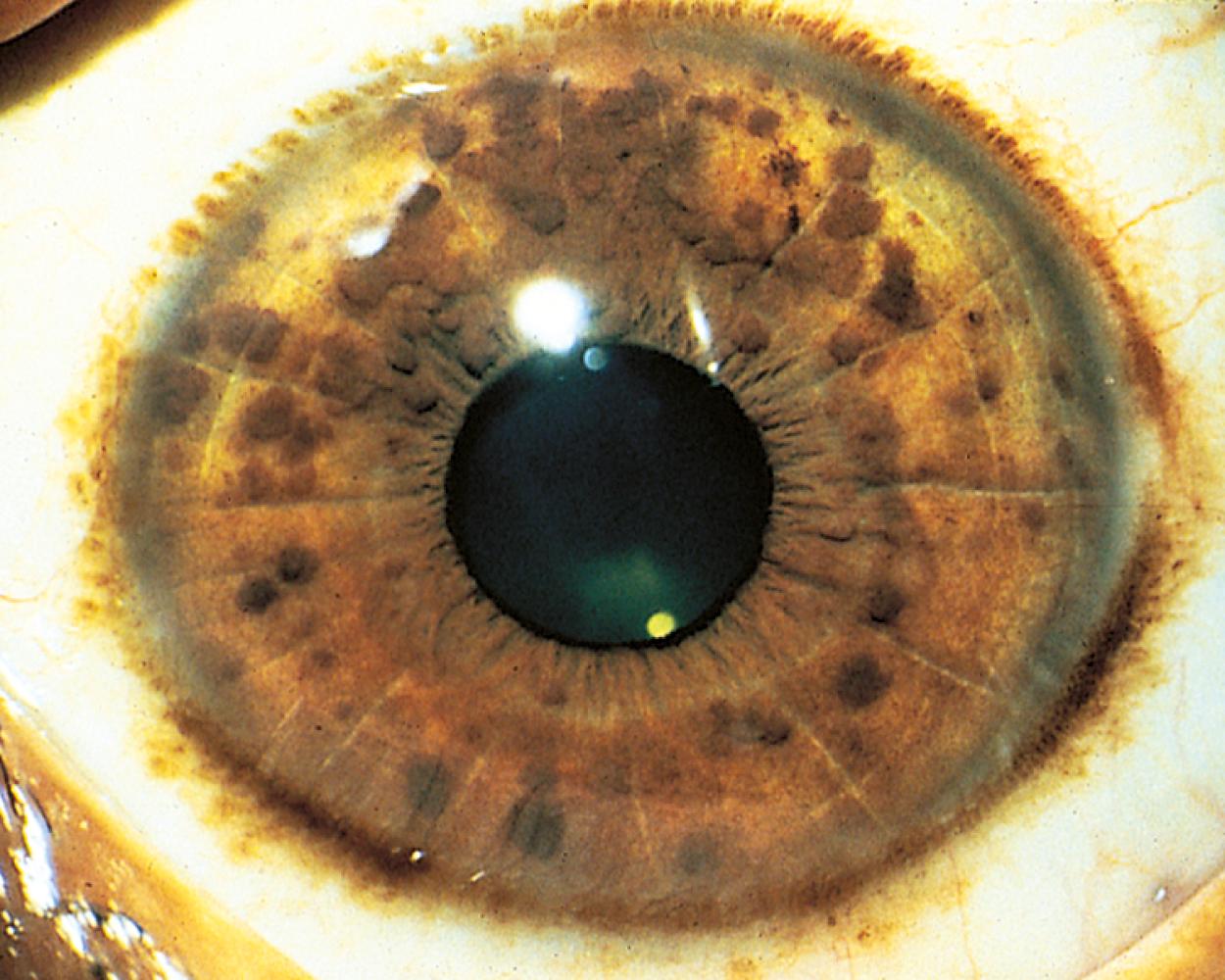
Pigmented hamartomas of the iris, or Lisch nodules, are seen in more than 90% of patients with NF-1 who are older than 6 years old and can be found in nearly one-third of younger individuals ( Fig. 16.5 ). They do not occur in the normal population. Although these hamartomas are asymptomatic and do not correlate with the extent or severity of other manifestations, they are helpful in establishing the diagnosis.
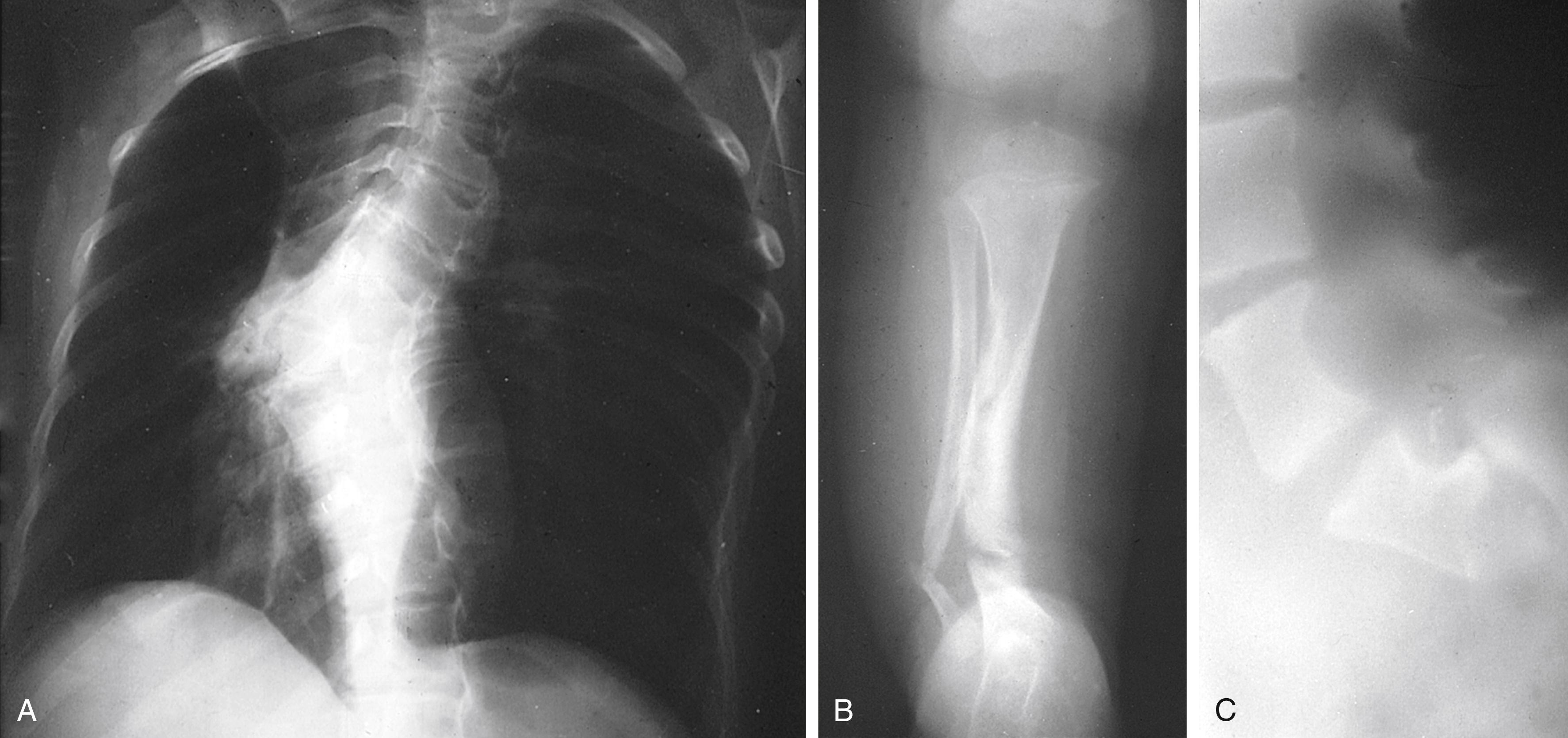
Short stature and macrocephaly are common in patients with NF-1, and skeletal abnormalities are found in 51% ( Fig. 16.6 ). Osseous lesions, if present, usually appear in the first year of life. The characteristic findings include the following:
Severe angular scoliosis with dysplasia of the vertebral bodies (see Fig. 16.6A )
Defects of the posterior superior wall of the orbit
Congenital bowing and thinning of the cortices of long bones and pseudarthrosis of the tibia, fibula (see Fig. 16.6B ), femur, or clavicle
Disorders of bone growth associated with elephantoid hypertrophy of overlying soft tissue
Erosive bony defects produced by contiguous neurogenic tumors
Scalloping of the posterior margins of the vertebral bodies corresponding to saccular areas of dilation of the spinal meninges (see Fig. 16.6C )
Patients with NF-1 can be affected with various tumors of the brain, spinal cord, spinal nerve roots, and peripheral nerves. Optic nerve glioma is the most common CNS tumor and affects 20% of patients with NF-1, usually occurring by 18 months to 7 years old. It often presents as progressive visual loss with optic atrophy and tends to be less aggressive than in patients without NF-1. Ependymomas, meningiomas, brainstem gliomas, and astrocytomas also have been reported.
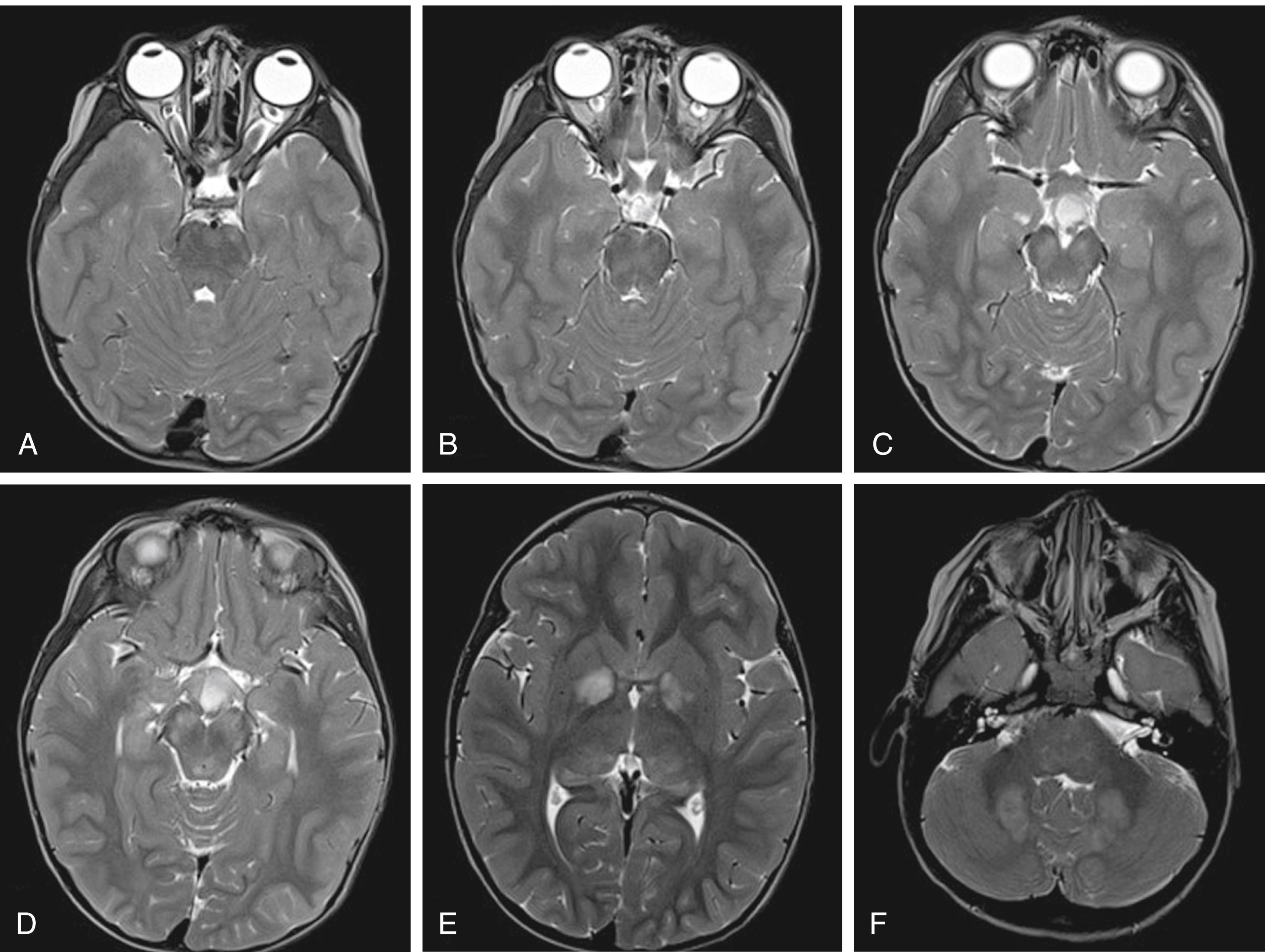
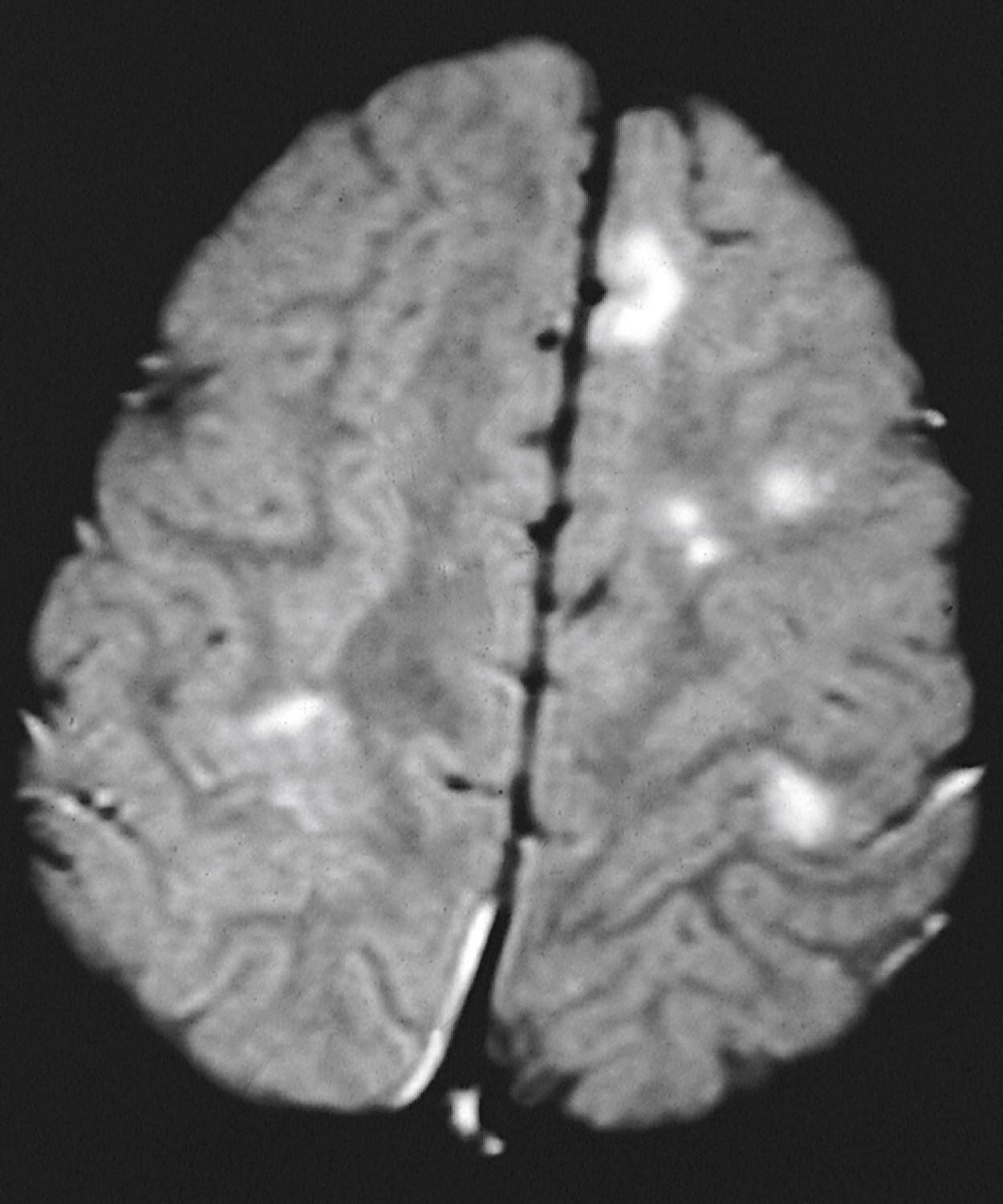
Magnetic resonance imaging (MRI) scans frequently show areas of increased signal intensity on T2-weighted images of the globus pallidus, brainstem, or cerebellar white matter ( Fig. 16.7 ). These are commonly termed unidentified bright objects (UBOs) or hamartomas and are believed to represent increased fluid within the myelin associated with dysplastic glial proliferation representing dysmyelination. The dysmyelination does not appear to correlate with neurologic dysfunction. However, their presence helps confirm the diagnosis of NF-1. Computed tomography (CT) seldom demonstrates corresponding abnormalities and should be avoided to limit ionizing radiation due to the loss of function of a tumor suppressing gene.
Learning disabilities and behavior problems are common and may affect up to 40% of patients with NF-1. Although their full-scale intelligence quotient is generally lower than that of the general population, severe intellectual disability is rare. Approximately 10% of patients with NF-1 have seizures.
A small percentage of patients with NF-1 have dysplasia of the renal or carotid arteries. Renal artery stenosis can cause systemic hypertension, and adult patients with NF-1 may develop pheochromocytoma with concomitant hypertension. Cerebral artery dysplasia can include moyamoya syndrome with abnormal vessels of the circle of Willis, predisposing to cerebral infarction in children and cerebral hemorrhage in adults.
NF-2 (also known as bilateral acoustic neurofibromatosis ) is a distinct genetic disorder characterized by autosomal dominant inheritance of bilateral acoustic neuromas with a penetrance of more than 95%. NF-2 occurs in approximately 1 in 50,000 people. It results from a mutation of the NF2 gene on the long arm of chromosome 22. The NF2 gene product, merlin or schwannomin, serves to suppress tumor formation, and its dysfunction leads to the common occurrence of CNS tumors in patients with NF-2. Most patients eventually develop bilateral acoustic neuromas (vestibular schwannomas).
Symptoms usually first appear in the teens or early 20s when pressure on the vestibulocochlear or facial nerve complex results in impaired auditory discrimination, hearing loss, tinnitus, unsteadiness, or facial weakness. Presenile lens opacities, found in half the patients examined, may precede the onset of symptoms referable to acoustic neuroma. Other Schwann cell tumors of cranial nerves, spinal roots, or the spinal cord, as well as multiple CNS tumors of meningeal or glial origin, may develop. Cutaneous manifestations such as café-au-lait spots, cutaneous neurofibromas, and axillary or inguinal freckling are less common in NF-2 than in NF-1, and Lisch nodules are not typical. Diagnostic criteria for NF-2 are summarized in Box 16.2 .
Bilateral eighth nerve masses seen with appropriate imaging techniques (e.g., CT, MRI)
or
A first-degree relative with NF-2 and a unilateral eighth nerve mass
or
Two of the following:
Neurofibroma
Meningioma
Glioma
Schwannoma
Juvenile posterior subcapsular lens opacity
TS is inherited as an autosomal dominant trait. Two genes appear to cause the disorder: TSC1 located on chromosome 9q and TSC2 on chromosome 16p. Their gene products (hamartin for TSC1 and tuberin for TSC2) have tumor suppressor activity, which is dysfunctional in affected patients. Both genes produce similar phenotypes when expressed. Genetic testing is available and currently detects nearly 80% of cases. Although 1 in 6000 to 9000 people in the population carry a TS gene, expression is highly variable and full expression of disease is seen in only 1 in 150,000 members of the population. Most carriers have hypopigmented macules (ash-leaf spots) as their only manifestation. Spontaneous mutation appears to account for the majority of newly diagnosed cases, and in up to 2% of patients without a positive family history, the disorder may be the result of germline mosaicism.
The more prominent features of this neurocutaneous disorder include seizures (96%), intellectual disability (60%), autism (50%), intracranial calcification (49%), tumors of various organs (including the brain, heart, liver, and kidneys), and cutaneous lesions. Seizures are the most frequent presenting symptom. Clinical expression can be quite variable even among affected members of the same family. Diagnostic criteria are summarized in Box 16.3 .
Two major features or one major and two or more minor features
Either one major feature or two or more minor features
Angiofibromas (>3) or fibrous forehead plaque
Nontraumatic ungual or periungual fibroma (>2)
Hypomelanotic macules (i.e., ash-leaf spots [≥3], at least 5 mm diameter)
Shagreen patch (connective tissue nevus)
Multiple retinal hamartomas
Cortical dysplasias (includes tubers and cerebral white matter radial migration lines)
Subependymal nodule
Subependymal giant cell astrocytoma (SEGA)
Cardiac rhabdomyoma, single or multiple
Lymphangiomyomatosis
Renal angiomyolipoma (≥2)
Multiple randomly distributed pits in dental enamel (>3)
Gingival/intraoral fibromas (≥2)
Nonrenal hamartoma
Retinal achromatic patch
“Confetti” skin lesions
Multiple renal cysts
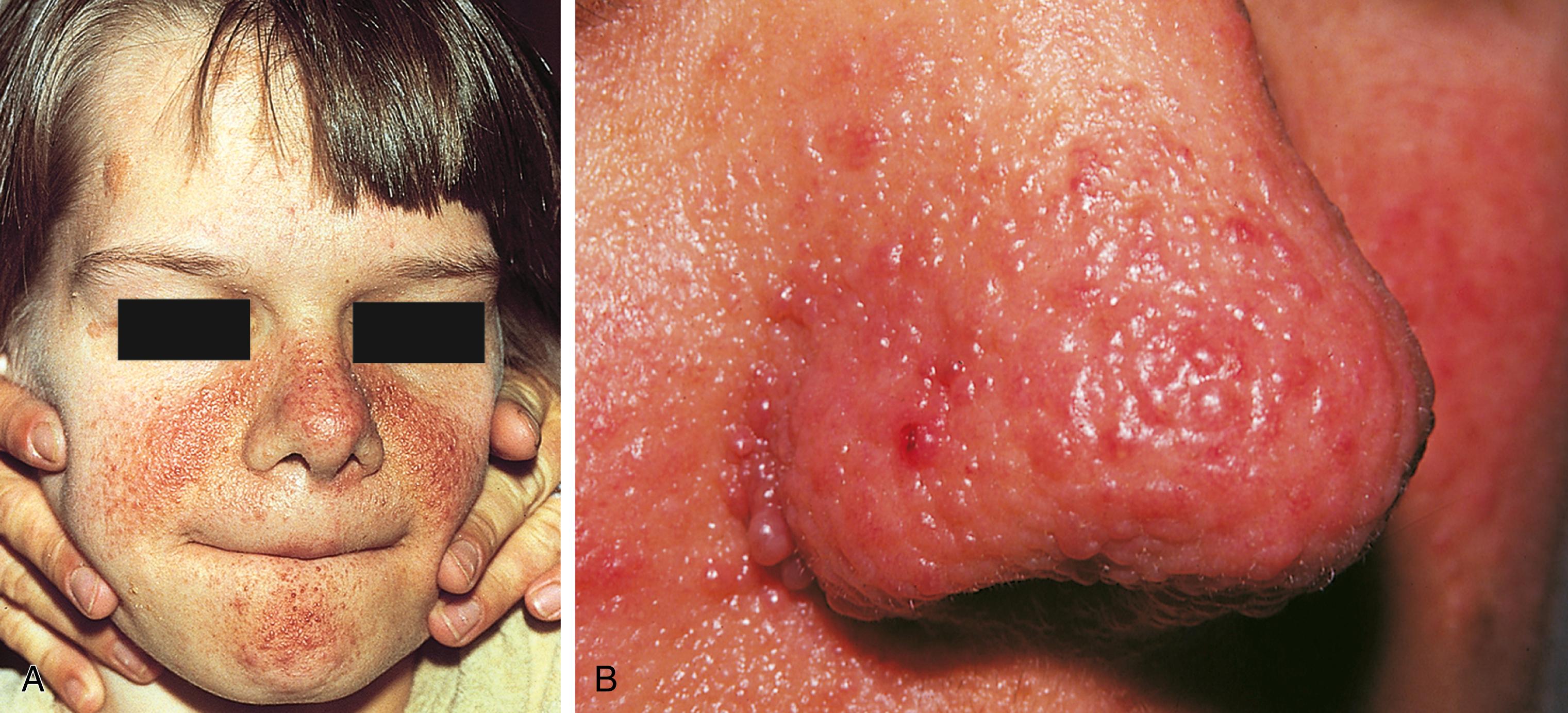
The characteristic skin lesion of TS is the angiofibroma (adenoma sebaceum). These are seen as erythematous papules distributed over the nose and malar region of the face ( Fig. 16.8 ). Approximately 40% of children with TS demonstrate these lesions by 3 years old.
Hypomelanotic macules with irregular borders, termed ash-leaf spots, are another common cutaneous manifestation ( Fig. 16.9 ). These generally appear earlier than adenoma sebaceum and may be present at birth. They are detectable by 2 years old in more than half of affected children. They resemble vitiligo but differ in that they are not completely devoid of melanin. In fair-skinned infants, these nevi may be demonstrable only under Wood lamp light.
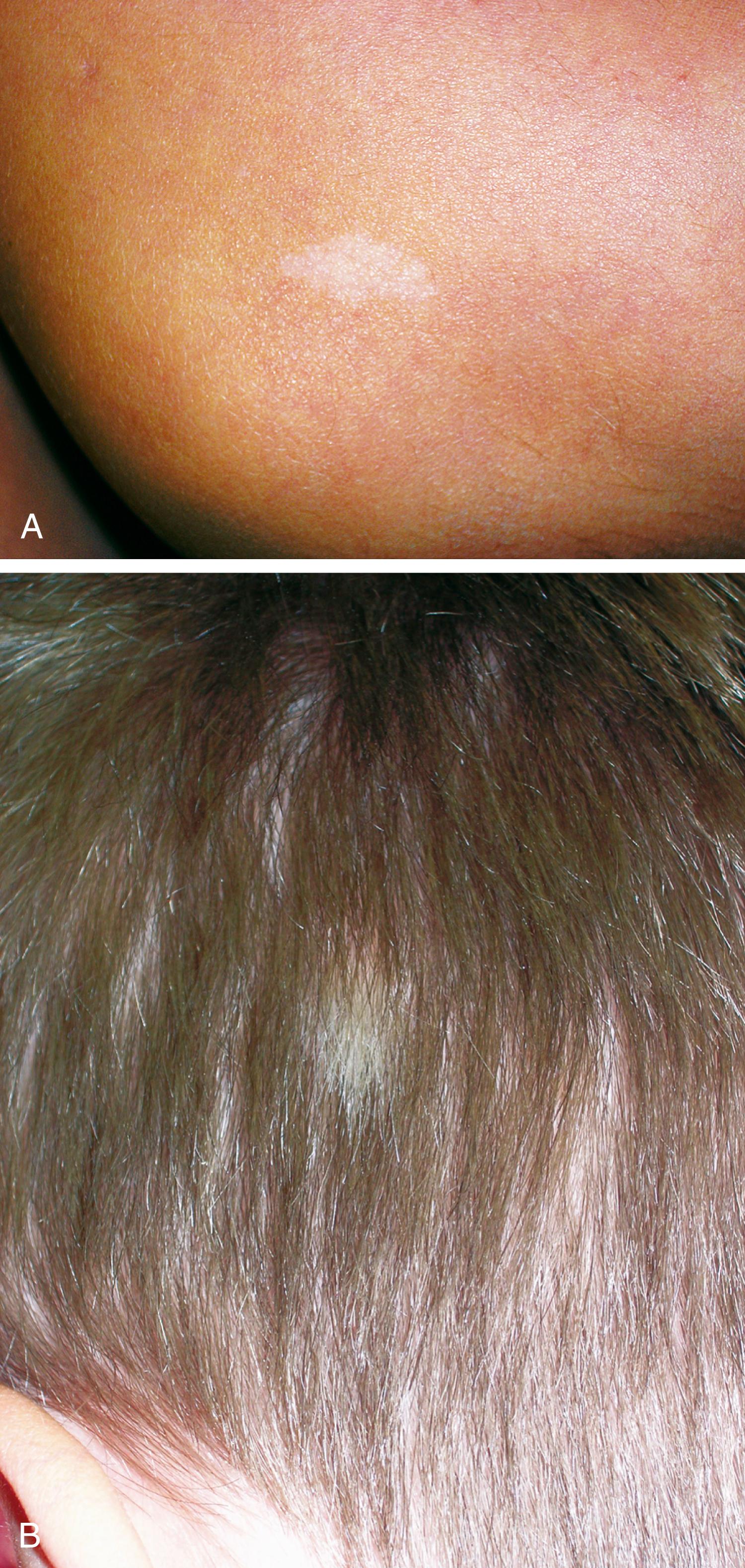
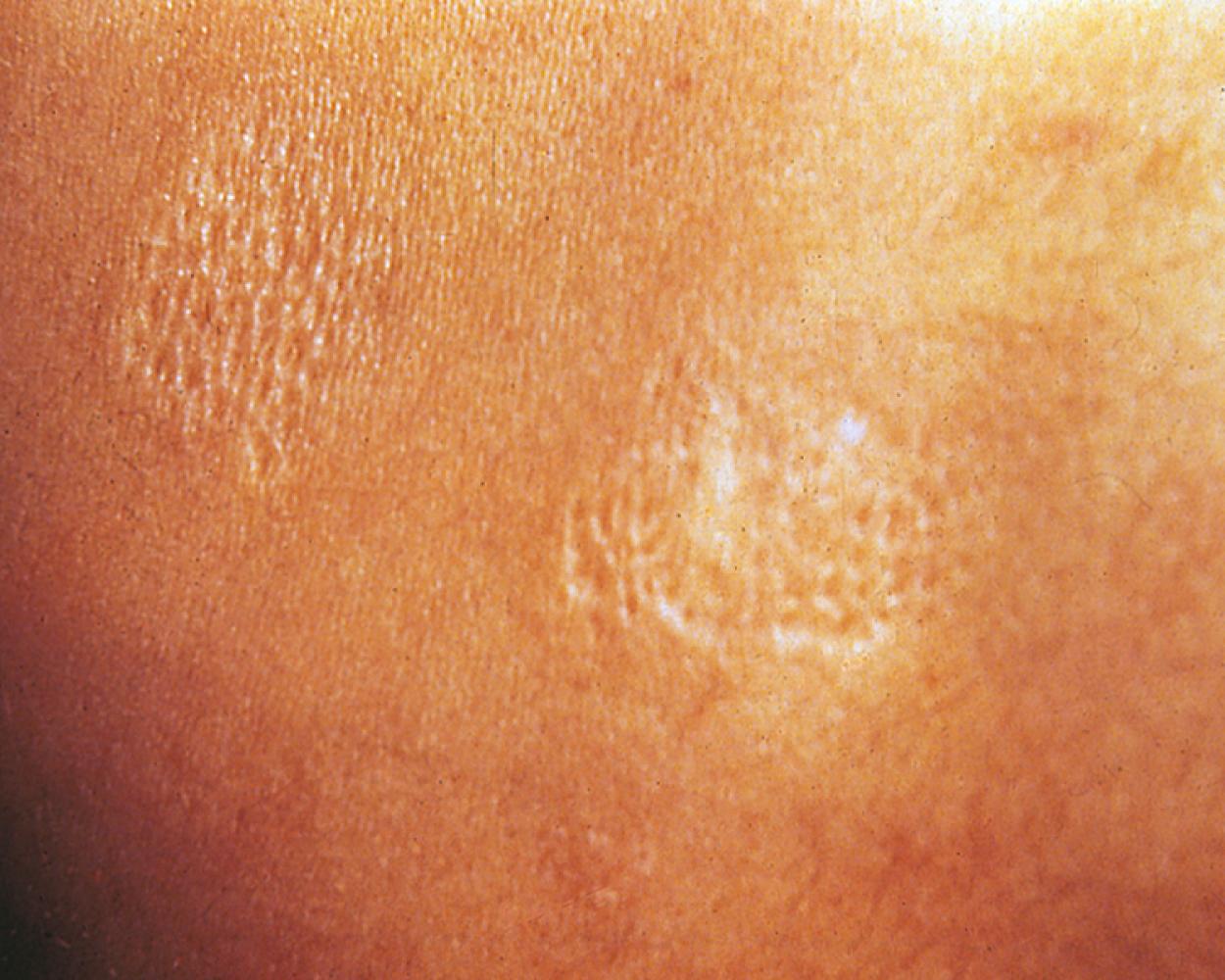
Another valuable cutaneous marker is the shagreen patch, a plaque of thickened skin with a cobblestone or orange-peel texture often seen on the dorsal aspect of the trunk ( Fig. 16.10 ). Histologically, the shagreen patch is a connective tissue nevus.
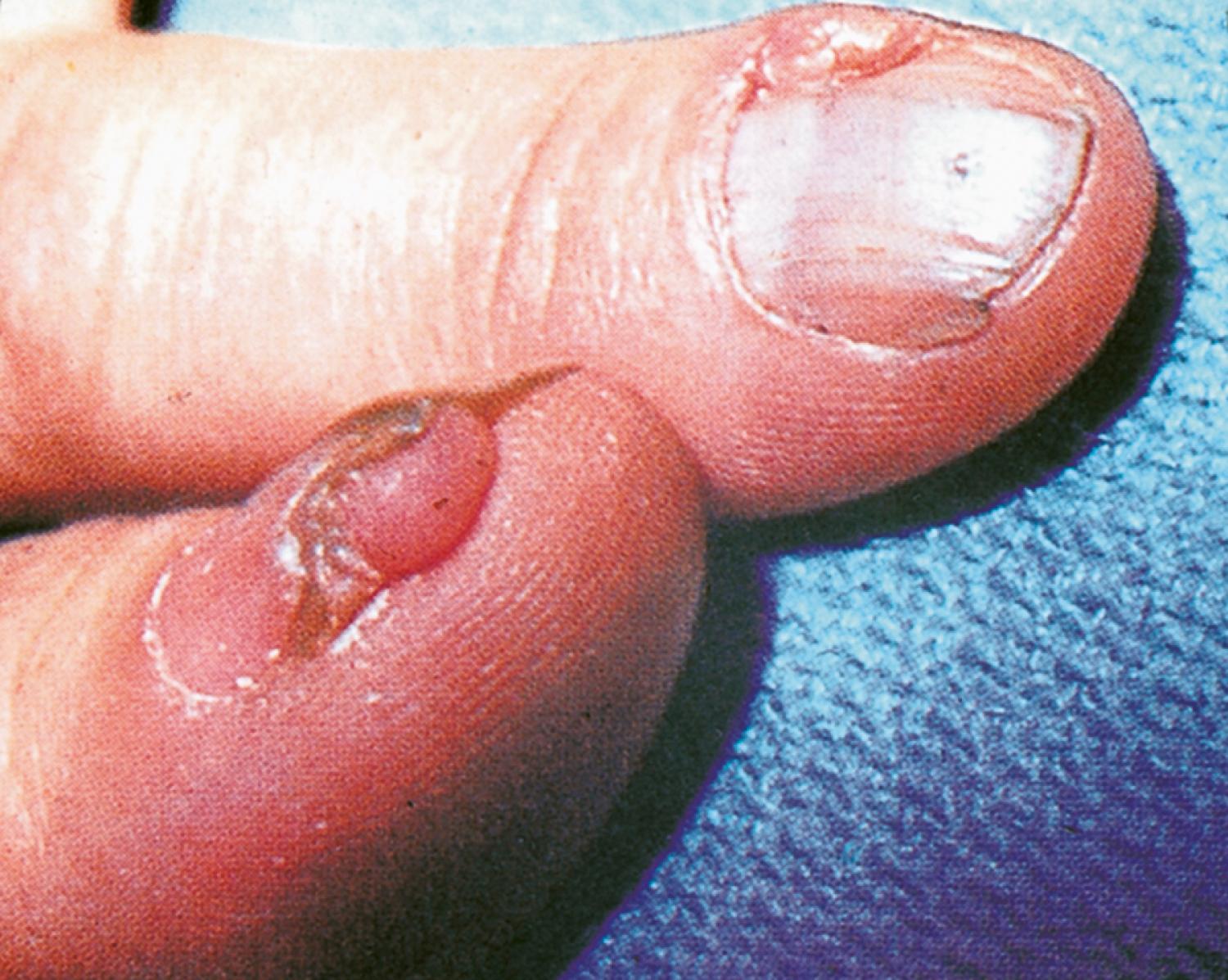
Additional dermatologic manifestations of TS include periungual fibromas ( Fig. 16.11 ) and macular areas of hyperpigmentation. Recognition of the cutaneous features can suggest an etiologic diagnosis in some patients with intellectual disability or seizures. Oral examination may reveal pitting of dental enamel.
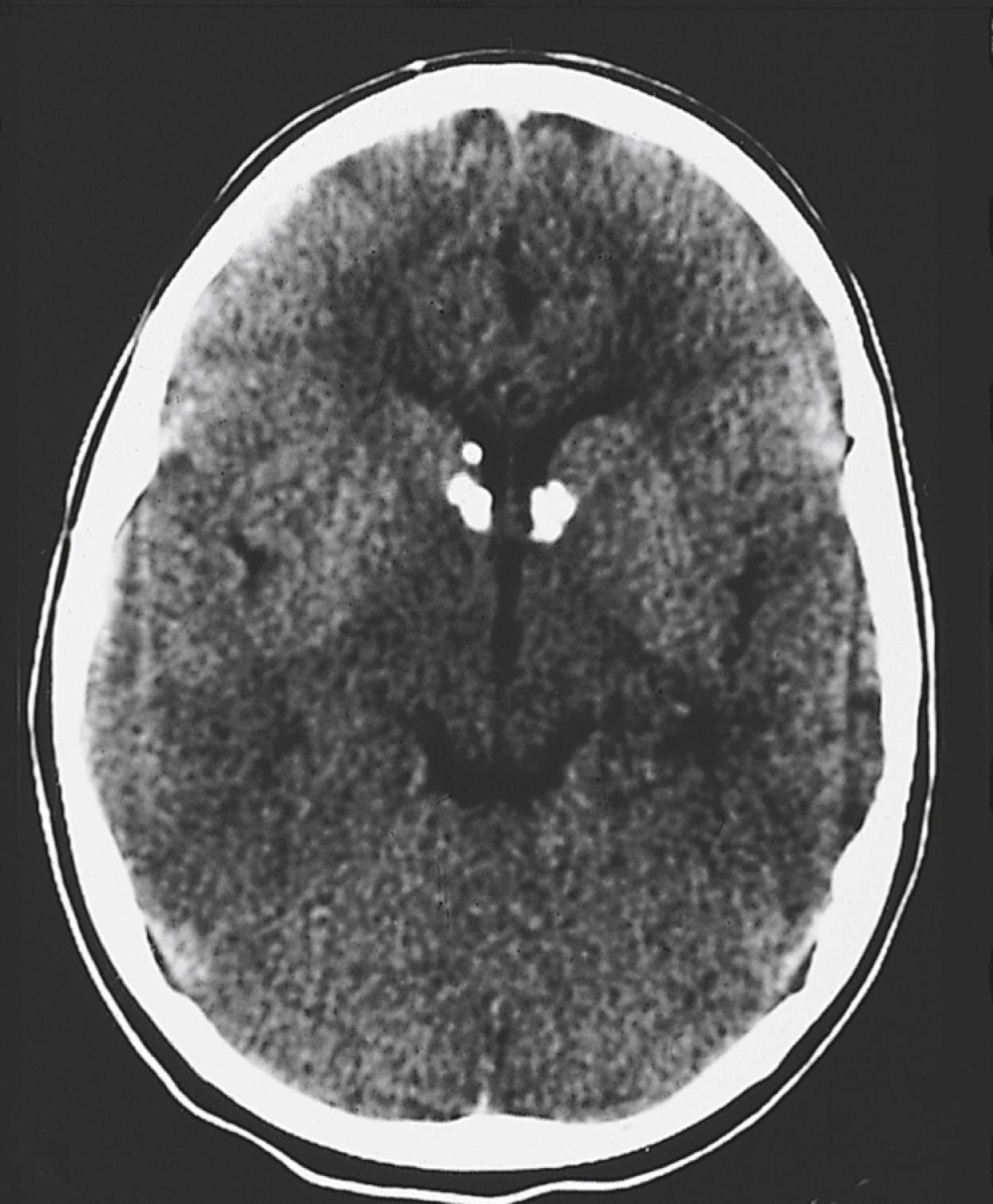
In patients with TS, CT scans often demonstrate subependymal nodules seen as intracranial calcifications that appear as multiple scattered areas of increased density adjacent to the walls of the lateral and third ventricles ( Fig. 16.12 ). CT is superior to MRI for demonstration of small calcifications. No relationship has been established between the extent of periventricular calcification and clinical severity as judged by developmental function or seizure frequency. CT may also demonstrate asymptomatic but typical intracranial calcifications in individuals who lack external manifestations of the disorder. This can help identify subclinical cases and improve the accuracy of genetic counseling in affected families.
The characteristic gross abnormality of the brain in TS is the presence of multiple gliotic nodules (hamartomas) of varying size, which constitute the tubers for which this disorder is named. These are located over the convolutions of the cerebral hemispheres and beneath the ependymal lining of the lateral and third ventricles. Heterotopic nodules of identical structure may be found in the cerebral white matter as well. Although cortical tubers are rarely apparent on CT scans, they are readily identified by MRI studies ( Fig. 16.13 ). Severely affected patients have a greater number of cerebral cortical lesions detected by MRI scans, suggesting that MRI may be useful in predicting eventual clinical severity in young children with newly diagnosed TS. Tumors may arise from cortical or subependymal tubers, complicating the course of the disease by producing increased intracranial pressure and other symptoms associated with intracranial mass lesions.
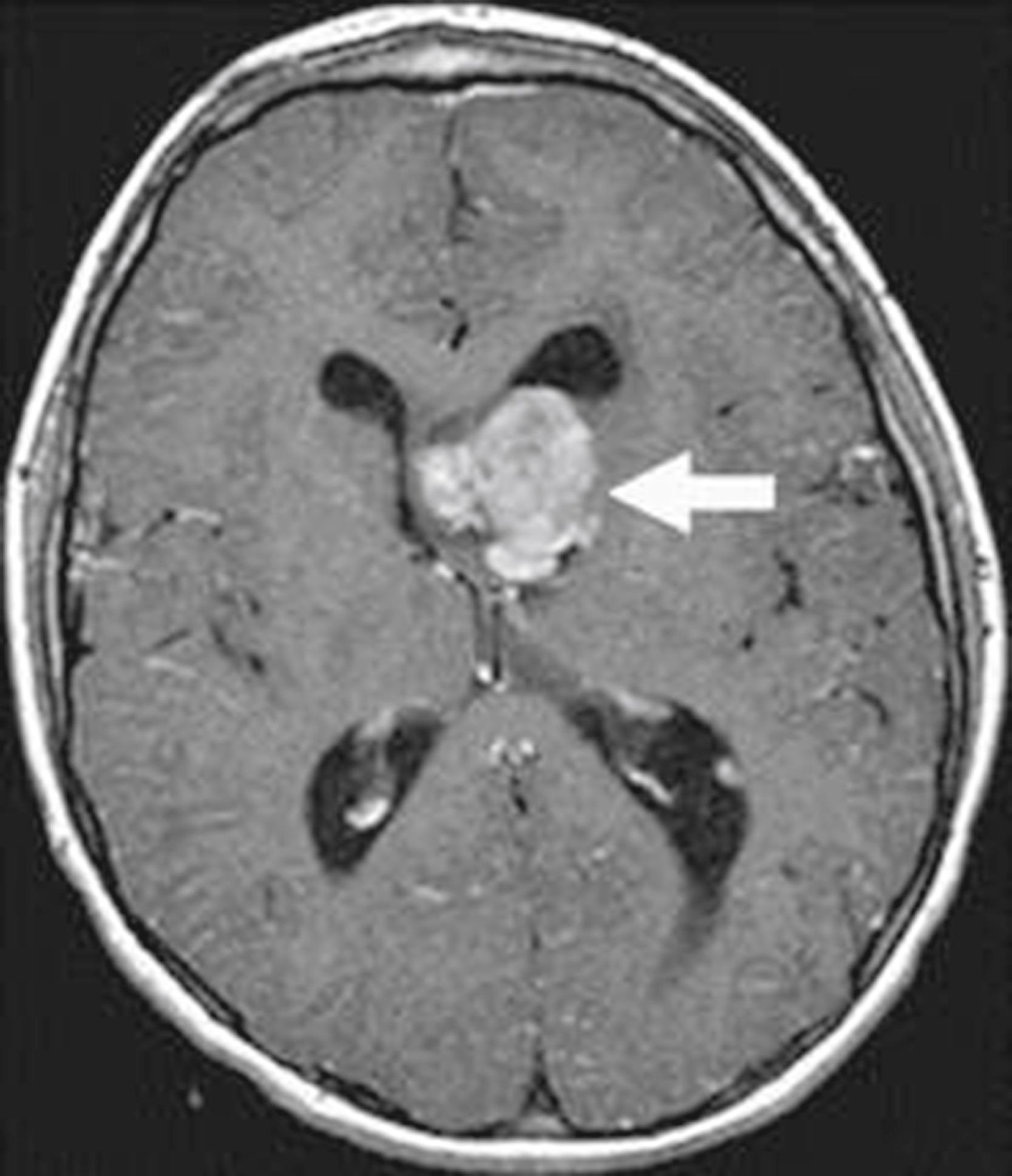
Subependymal giant cell astrocytomas (SEGAs) ( Fig. 16.14 ) can affect 15% to 20% of patients with TS and are clinically manifested by symptoms of obstructive hydrocephalus. The site of obstruction is often at the level of the foramen of Monro in the lateral ventricles. Such patients may present with signs of increased intracranial pressure (headache, vision changes, and/or papilledema), behavior change, or worsening seizure control. Up to 80% of patients with TS develop seizures of variable types that are often difficult to control. Infantile spasms are common and may be the presenting symptom leading to diagnosis. Patients with a history of infantile spasms should be evaluated for TS, because those who develop other types of seizures when very young tend to have more severe seizure disorders and poorer cognitive function.
Visceral lesions associated with TS include cardiac rhabdomyoma, renal angiomyolipomas, pulmonary lymphangiomyomatosis, and hepatic hamartoma. Cardiac rhabdomyomas occur in up to two-thirds of patients and may be multiple. They tend to regress over the first few years of life and are usually asymptomatic, although occasionally an affected newborn may have obstructive congestive heart failure. About three-fourths of patients with TS have renal angiomyolipomas, which are often bilateral and multiple. Most remain clinically silent, but tumors greater than 4 cm in size are more likely to be symptomatic and may cause hematuria or proteinuria. Renal disease is the most common cause of death in adults with the disease and may manifest as flank pain, hematuria, or retroperitoneal hemorrhage. Renal cysts occur earlier and less often than angiomyolipomas. Rarely, children with TS can present in infancy with polycystic kidney disease. Chronic renal failure and malignant transformation of renal tumors are rare. Pulmonary lymphangiomyomatosis affects less than 2% of patients, mostly females, and is rare before the adult years. Symptoms include dyspnea, spontaneous pneumothorax, and hemoptysis. Hepatic hamartoma is clinically insignificant.
The cardinal manifestations of Sturge-Weber syndrome are as follows:
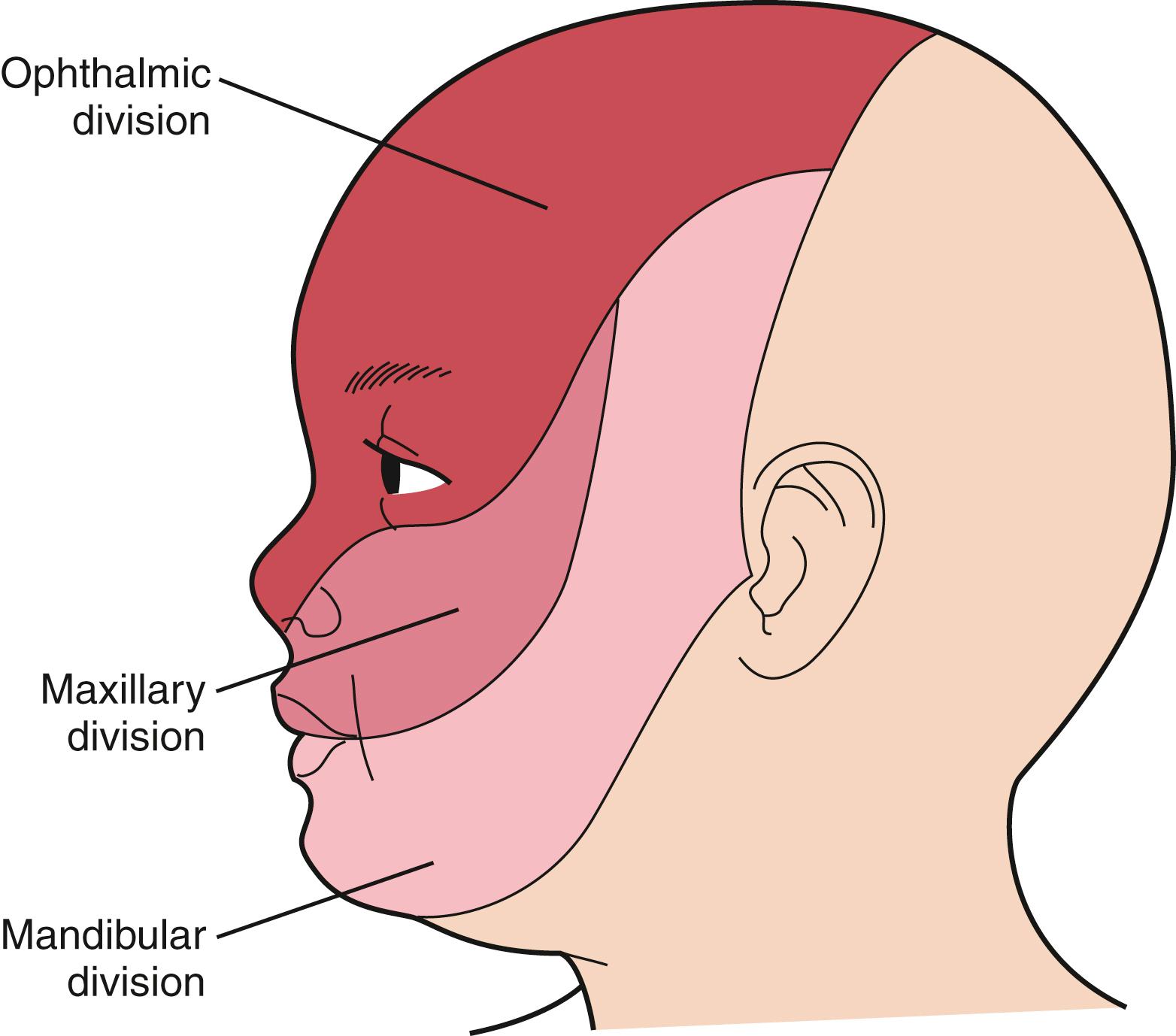
A vascular malformation or port-wine stain over the face that involves the cutaneous distribution of the ophthalmic division of the trigeminal nerve
Ipsilateral leptomeningeal angiomatosis with associated intracranial calcifications
A high incidence of intellectual disability and ipsilateral ocular complications
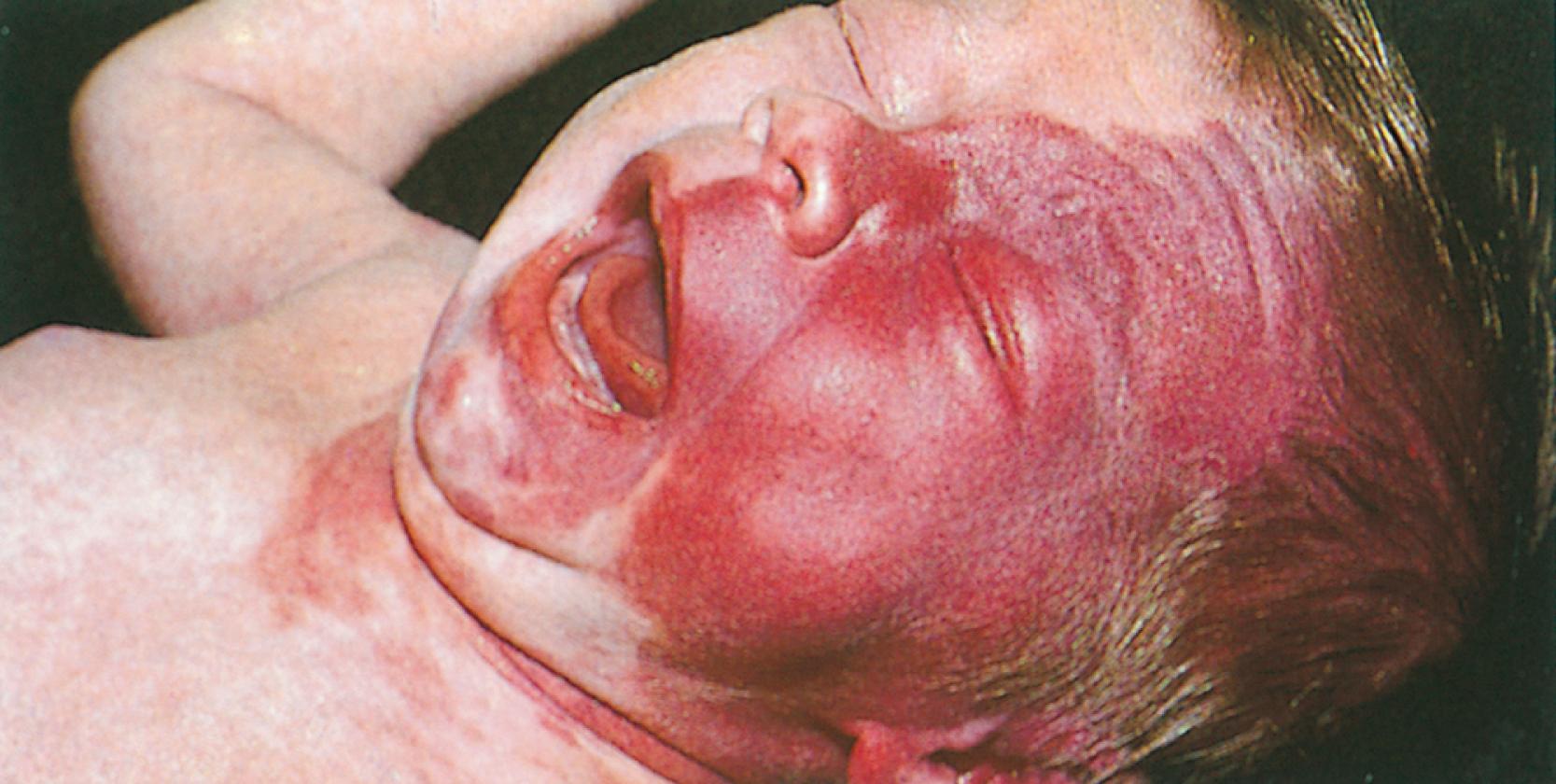
The port-wine stain ( Fig. 16.15 ) is usually present at birth and consists of a pink-to-purple macular cutaneous vascular malformation. Only patients with lesions involving the cutaneous distribution of the ophthalmic division of the trigeminal nerve (i.e., forehead and upper eyelid) are at risk for associated neuro-ocular complications ( Fig. 16.16 ). Repeated ophthalmologic and CT or MRI examinations are indicated only in this high-risk group, which has a 10% to 20% incidence of associated intracranial angiomas.
The coincidence of seizures and a facial vascular nevus should suggest the diagnosis of Sturge-Weber syndrome, which can be confirmed by CT scan or MRI ( Fig. 16.17 ). These scans may be normal at birth but subsequently show areas of gyriform contrast enhancement corresponding to the leptomeningeal angiomatosis. Serial examinations often demonstrate progressive ipsilateral cerebral atrophy. Additional findings may include serpiginous calcifications of brain parenchyma underlying vascular malformations of the pia. These intracranial calcifications are first seen on CT scan but become evident on plain skull films by the end of the second decade.
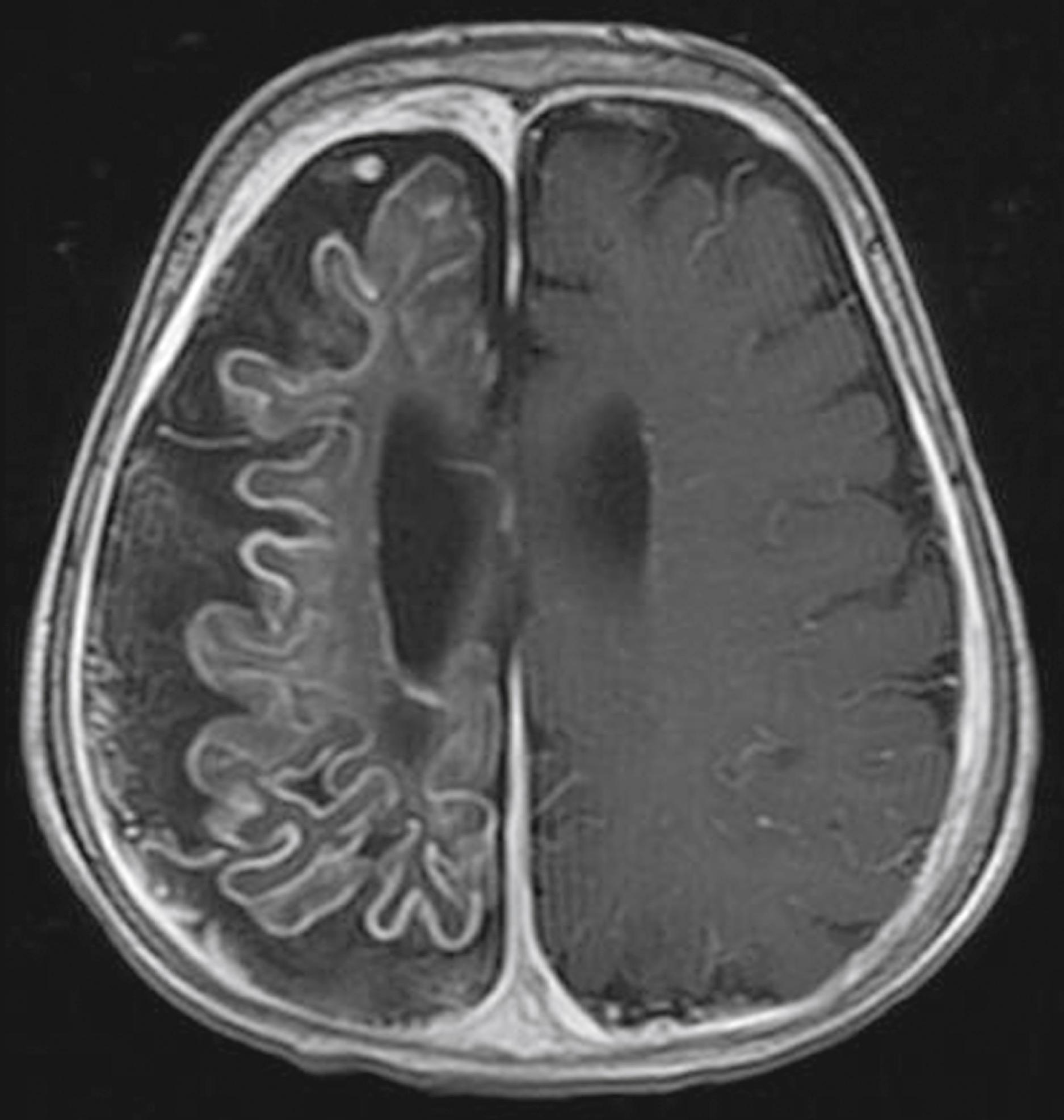
Associated ocular abnormalities are often encountered. Buphthalmos (corneal enlargement) or colobomata may be present at birth, and glaucoma frequently develops in infancy or later childhood ( Fig. 16.18 ). Dilated vessels in the sclera, conjunctiva, and retina are common, and angiomatous malformations of the choroid occasionally occur.
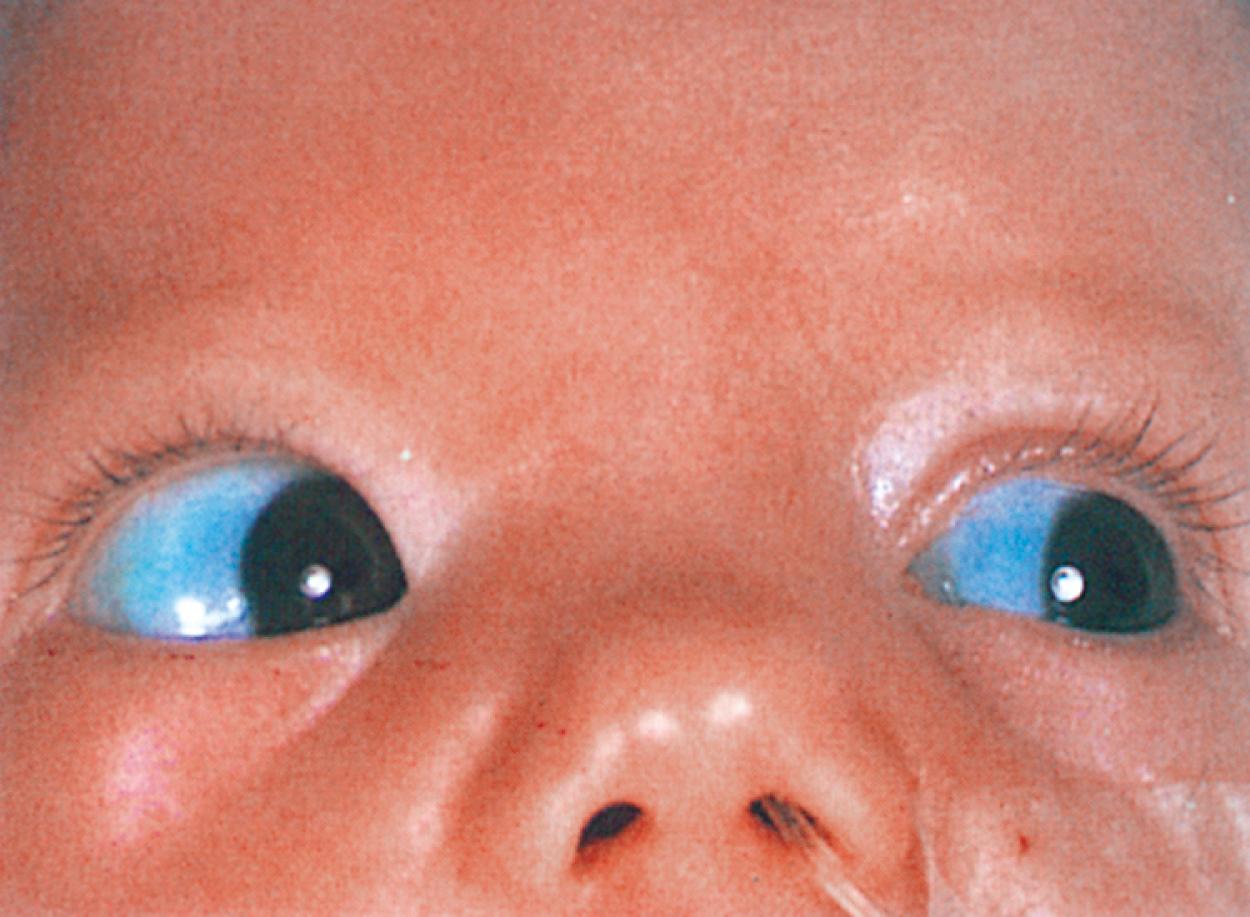
The estimated incidence of facial cutaneous angioma is 1 in 5000, and the estimated frequency of the complete syndrome is 1 in 30,000. Among patients with the complete syndrome, seizures occur in 90%, and contralateral hemiparesis eventually develops in one-third. Early developmental milestones are often normal, but about 50% develop cognitive difficulties ranging from mild to severe. Behavioral problems are common. Patients with refractory epilepsy are more likely to be more severely delayed. Although most cases are sporadic, genetic determination has not been ruled out. However, no cases of direct inheritance from a parent to child have been reported.
Patients with Klippel-Trénaunay syndrome (KTS) are born with a port-wine stain that is usually located over the lateral aspect of one leg. Less often an arm and a leg may be affected. In rare instances, more extensive, even bilateral, involvement is seen. The surface lesion is associated with an underlying vascular malformation, which provides an unusually rich blood supply to soft tissue and bony structures that results in hypertrophy (usually hemihypertrophy) and lymphedema ( Fig. 16.19 ). These features are often evident in the newborn, and progressive enlargement occurs during the first few years. Most cases are sporadic. However, a few cases have been reported to be autosomal dominant.
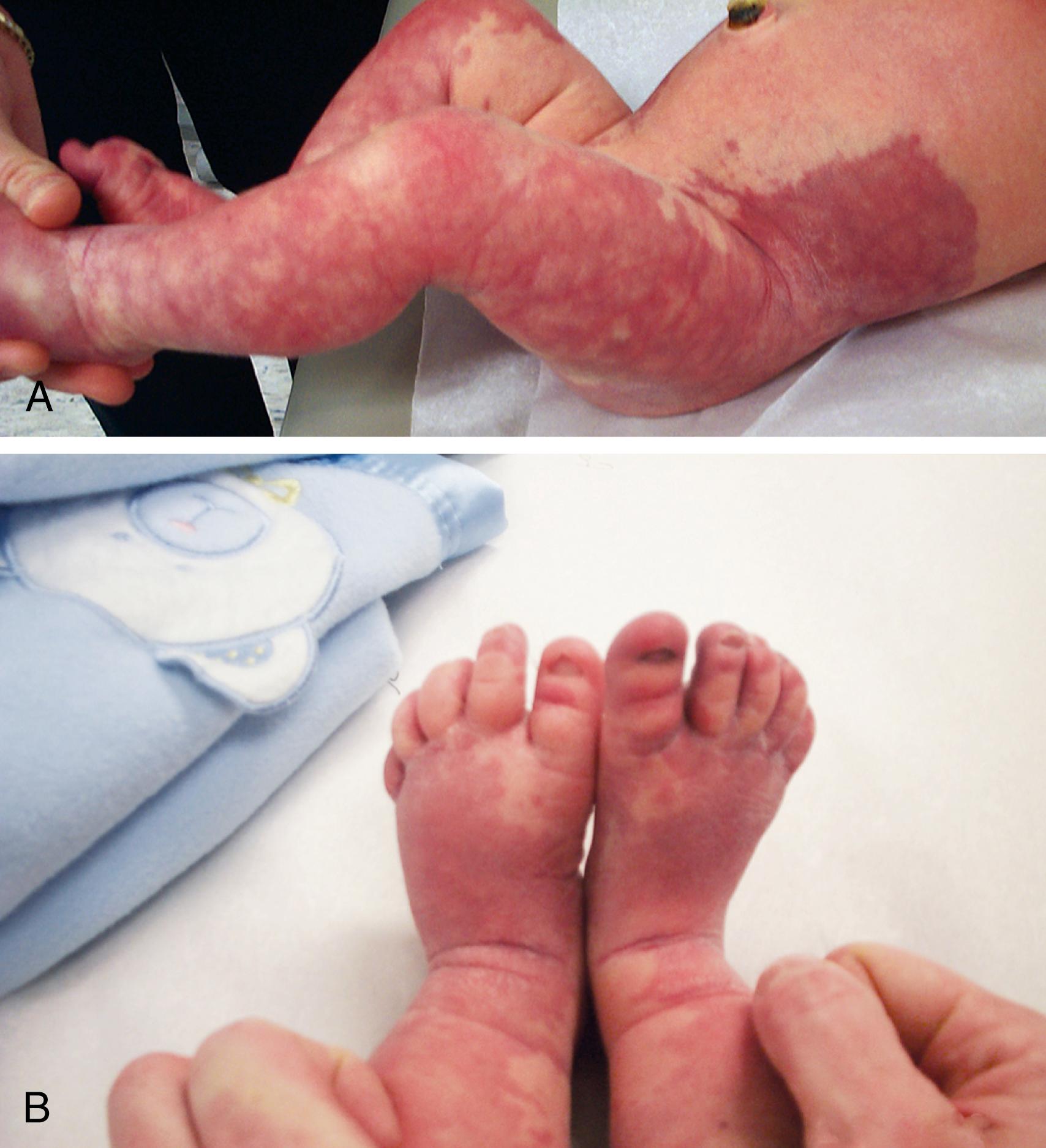
Ataxia-telangiectasia is a multisystem, autosomal recessive degenerative disorder characterized by ataxia, oculocutaneous telangiectasia, immunodeficiency, and a high incidence of neoplasia. The nature of the basic underlying defect is unknown. Affected individuals are extremely sensitive to ionizing radiation and have defective deoxyribonucleic acid (DNA) repair mechanisms. Molecular genetic testing for ATM (ataxia telangiectasia mutated), the only gene associated with ataxia-telangiectasia, is clinically available. Ataxia is the usual presenting feature, and the course of the neurologic disturbance is rather stereotypic. Tremors of the head may be seen before 1 year old, and unsteadiness of gait is evident when the child first walks. Progressive global ataxia and slurred, scanning, dysarthric speech are typical during the early school-age years. Loss of deep tendon reflexes and impairment of position and vibratory sensation are evident by the end of the first decade. Adolescence is marked by choreoathetosis, dystonic posturing, gaze apraxia, and progressive dementia. Nonclassic forms of ataxia-telangiectasia have included adult-onset cases and presentations with early dystonia.
The characteristic cutaneous manifestations of this disorder appear by 6 years old. Telangiectases first appear on the bulbar conjunctivae ( Fig. 16.20 ) and develop later over the malar regions, ears, antecubital fossae, neck, and upper chest.
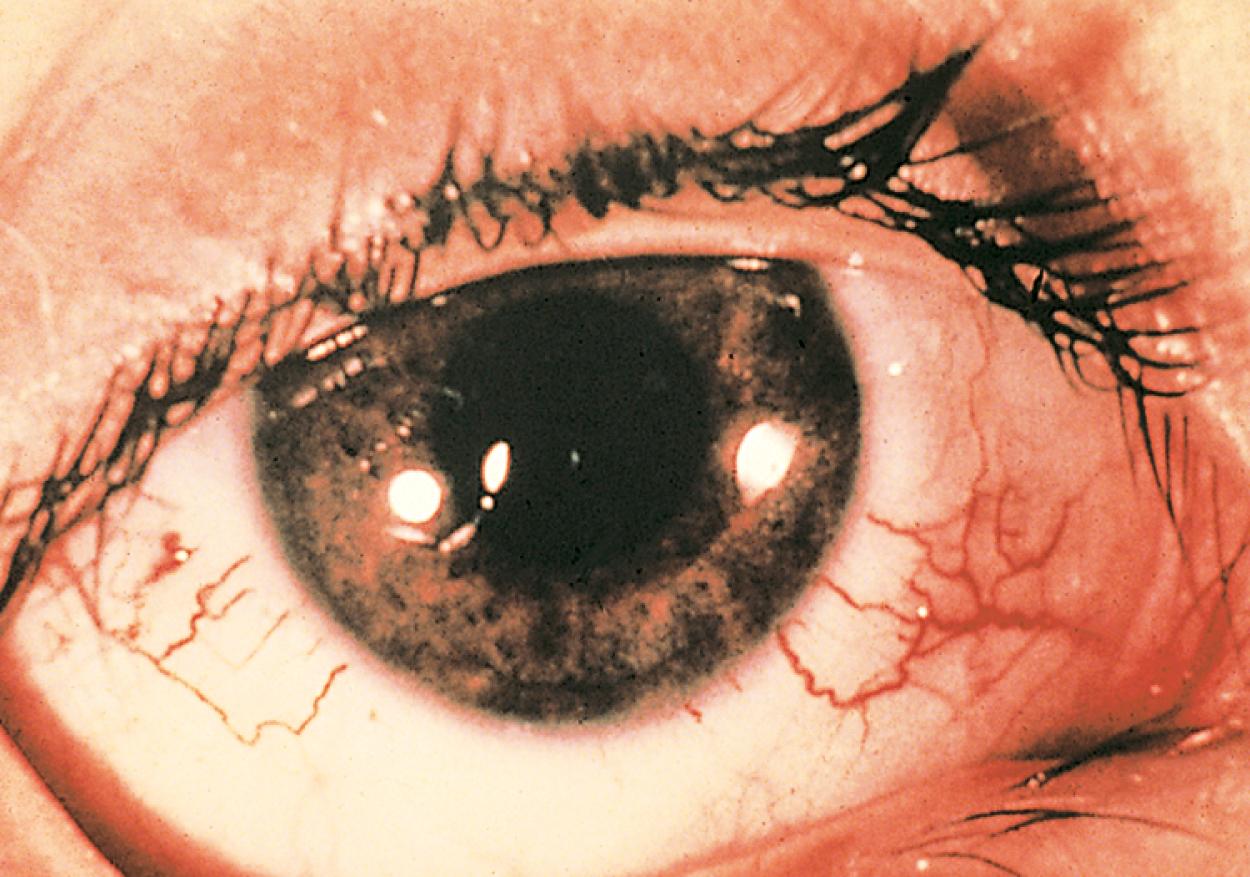
Neuropathologic changes are widespread, with the cerebellum being the site of maximal degeneration. Loss of Purkinje and basket cells, thinning of the granular cell layer, and mild changes in the molecular layer are characteristic findings.
Systemic manifestations include major defects in cellular and humoral immunity. Deficiencies of immunoglobulin A (IgA) and immunoglobulin M (IgM) are characteristic and together with impaired cellular immunity contribute to susceptibility to the recurrent sinus and pulmonary infections that mark this disorder, as well as to the tendency to develop malignancies of the lymphoreticular system (most commonly acute lymphoblastic leukemia or lymphoma) during adolescence or early adulthood (see Chapter 12 ). Serum α-fetoprotein levels are elevated, which serves as a nonspecific marker. Adult family members of patients, especially mothers, may also be susceptible to malignancy—breast and lung cancer being the most common.
The nevus sebaceus of Jadassohn is usually present at birth, manifest as a yellowish-tan, waxy, linear lesion ( Fig. 16.21 ) that contains a papillomatous excess of sebaceous glands. This nevus may be found on the scalp, face, neck, trunk, or extremities. With time, the lesion becomes disfiguring. This eventuality and a 15% to 20% risk of malignant degeneration have led practitioners to recommend early surgical excision. Although usually seen as an isolated abnormality in otherwise normal individuals, an association with seizures and intellectual disability has been reported. The risk of neurologic abnormalities is greatest when the cutaneous lesion is located in the midfacial area.
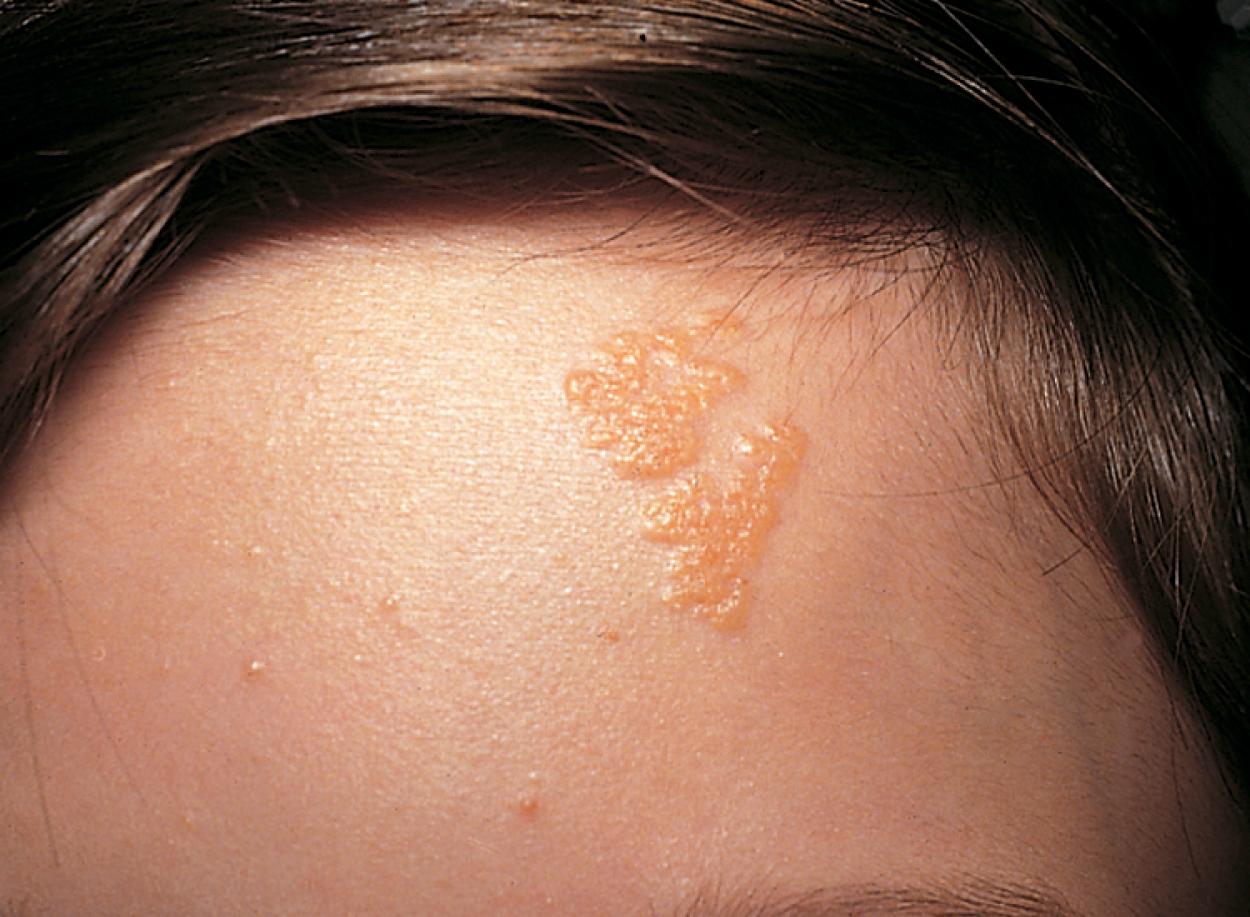
Epidermal nevus syndrome is a congenital neurocutaneous disorder in which an epidermal nevus is seen in association with neurologic dysfunction. The latter may include seizures, paresis, intellectual disability, and developmental delay. Unilateral hemimegalencephaly with intractable seizures is the commonest CNS abnormality. Disorders of segmentation/migration and multiple other structural CNS anomalies have been reported. Extra-CNS congenital defects may involve connective tissues, especially the skeleton, as well as ocular, cardiac, and genitourinary systems. The skin lesions are hamartomatous (derived from embryonic ectoderm) and characterized by hyperplasia of the epidermis and adnexal structures. They are usually present at birth, although some may appear later in the first year. They appear as raised, often warty hyperpigmented lesions typically in a linear pattern ( Fig. 16.22 ). They may enlarge subsequently but tend to stabilize in size by puberty. Most cases are sporadic, although a small number are autosomal dominant.
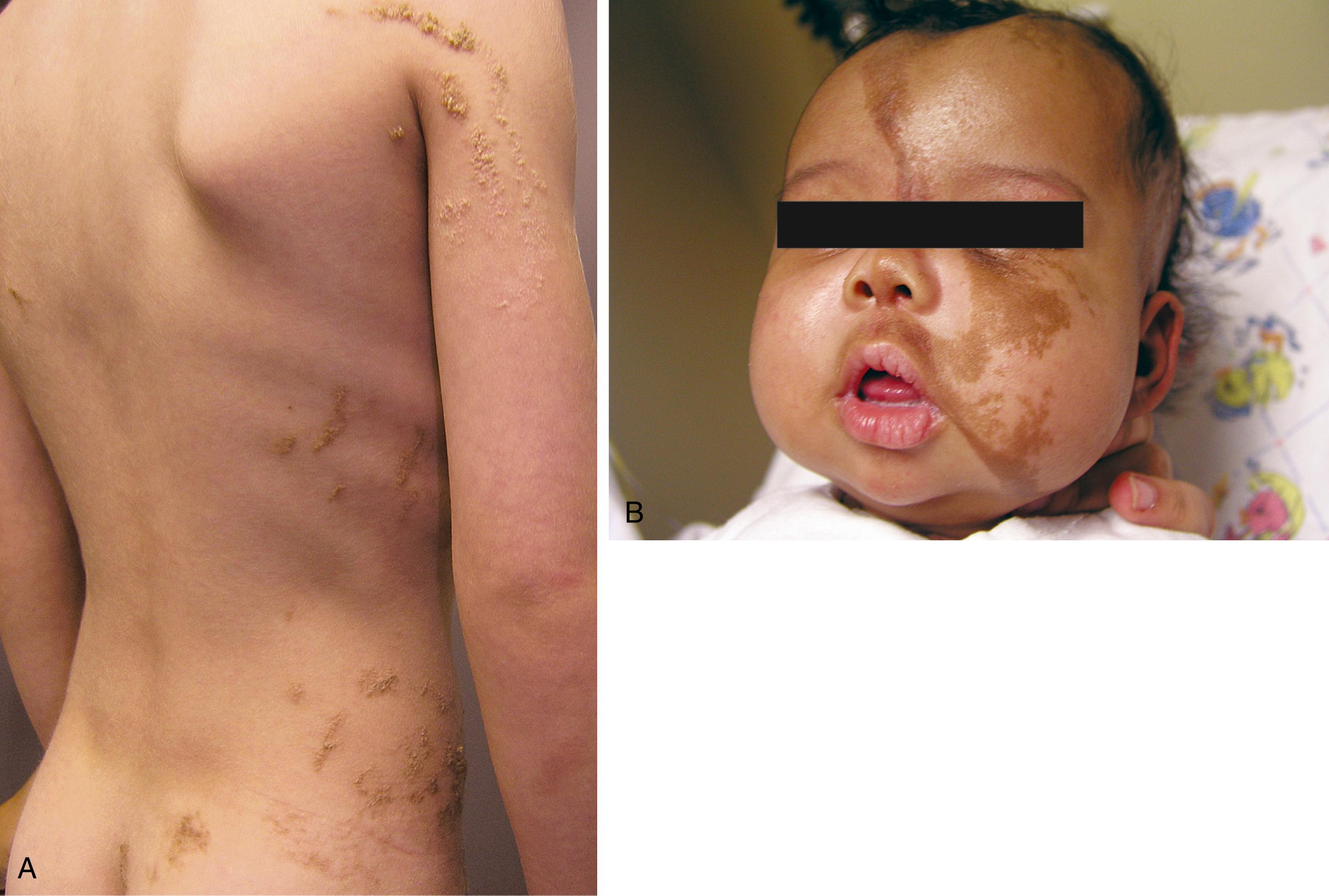
Incontinentia pigmenti is a rare, X-linked dominant syndrome with cutaneous, neurologic, ophthalmologic, and dental manifestations. It is caused by a mutation in the NEMO gene.
Neurologic and ophthalmologic problems often become manifest during early infancy and are reported to occur in about 30% of patients. They may include seizures, cerebrovascular accidents, developmental delay, intellectual disability, and microcephaly. Cutaneous features are described in Chapter 8 (see Fig. 8.100 ).
Malformations of the CNS are a leading cause of neurologic and developmental disability in infants and children. Although CNS malformations are not necessarily accompanied by external dysmorphic features, disturbances of cranial volume, abnormalities of head shape, and skin and visceral lesions in the dorsal midline should alert the physician to the possibility of associated CNS dysmorphogenesis.
Macrocephaly is defined as a head circumference more than 2 standard deviations above the mean for age, gender, and gestation. This abnormality can be caused by a myriad of conditions ( Table 16.2 ), including hydrocephalus (excessive accumulation of cerebrospinal fluid [CSF]), intracranial mass lesions (i.e., tumors, subdural effusions), thickening or enlargement of the skull (primary skeletal dysplasias), and a true increase in brain substance (megalencephaly). The latter is seen in Soto syndrome, achondroplasia, neurocutaneous syndromes, and certain lipidoses, leukodystrophies, and mucopolysaccharidoses. Primary megalencephaly may occur as a benign familial trait.
| Early Infantile (Birth to 6 Months Old) |
Late Infantile (6 Months Old to 2 Years Old) |
Early to Late Childhood (After 2 Years Old) |
|---|---|---|
|
|
|
Evaluation of the child with a head that is abnormally large or appears to be growing at an excessive rate should include the following:
Serial measurements of head circumference
Measurement of the parents’ head circumferences and exploration of family history for evidence of macrocephaly or neurologic and cutaneous abnormalities
Developmental history
Careful examination for evidence of increased intracranial pressure, developmental delay, skeletal dysplasia, abnormal transillumination, cranial bruits, ocular abnormalities, or organomegaly
Plain skull radiographs may detect primary skeletal dysplasias. CT or MRI scans allow assessment of ventricular size and permit detection of intracranial mass lesions and chronic subdural effusions. CT is the method of choice for demonstrating intracranial calcification (as seen with congenital cytomegalovirus infection in Fig. 16.23 ) and detecting fresh blood.
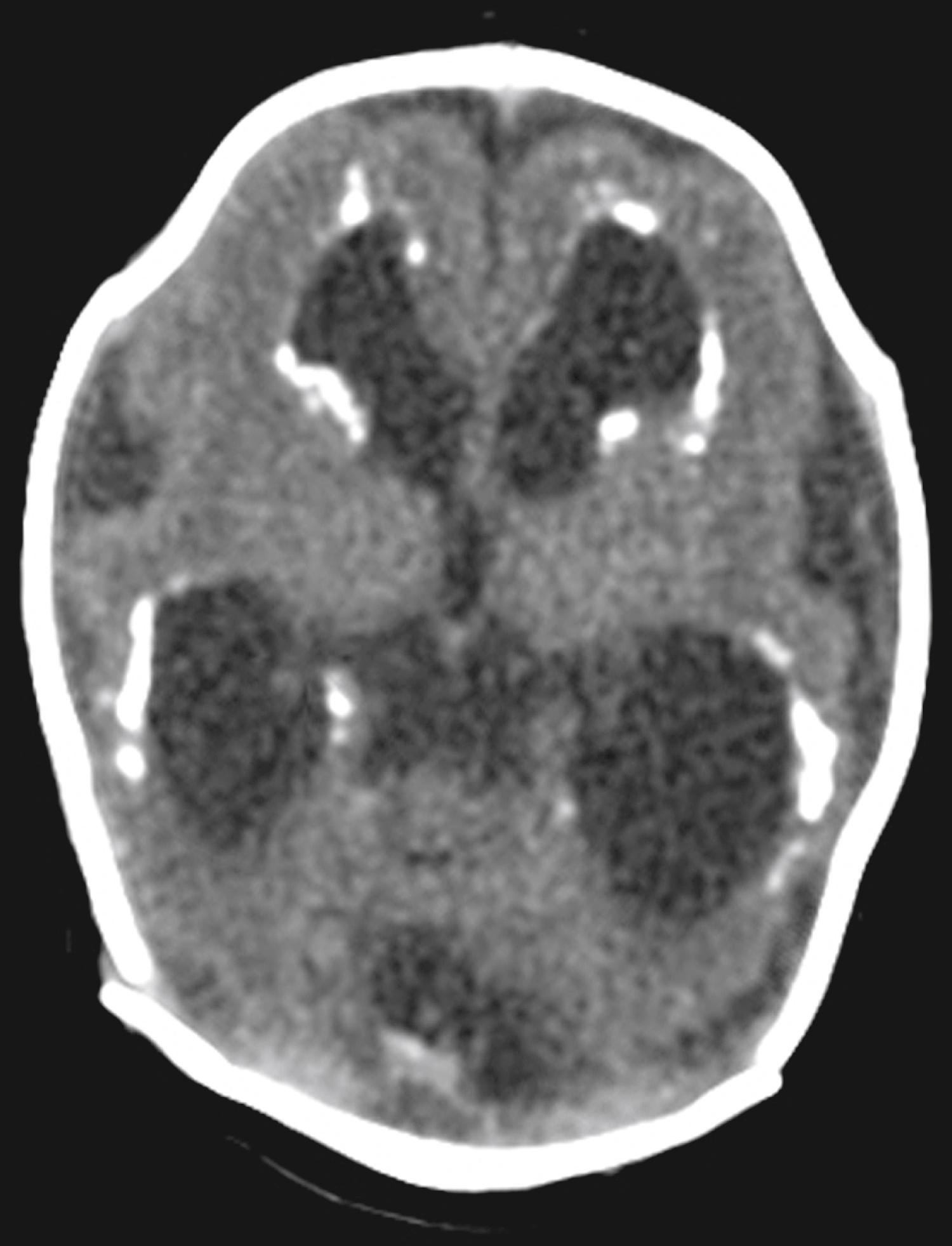
Hydrocephalus is caused by an imbalance between CSF production and resorption that is of sufficient magnitude to result in a net accumulation of fluid within the ventricular system. Impaired CSF resorption may occur secondary to obstruction of CSF pathways within the ventricular system (noncommunicating hydrocephalus) or as a result of obstruction of the subarachnoid space (communicating hydrocephalus). Hydrocephalus secondary to CSF overproduction is rare but does occur in some cases of choroid plexus papilloma (see Fig. 16.38 ). Noncommunicating hydrocephalus is often due to aqueductal stenosis or congenital malformations of the fourth ventricle, and it is a common complication of tumors or vascular malformations of the posterior fossa that compress the cerebral aqueduct or obstruct outflow from the fourth ventricle. Causes of communicating hydrocephalus include intracranial hemorrhage, meningitis, cerebral venous or dural sinus thrombosis, and diffuse infiltration of the meninges by malignant cells.
The clinical manifestations of hydrocephalus in infancy are stereotypic. The head is excessively large at birth or grows at an abnormally rapid rate, becoming macrocephalic over the first few months. The forehead is disproportionately large, and the face appears small in relation to the calvarium. The scalp is thin and glistening, and its veins are distended, often becoming strikingly dilated when the infant cries. The anterior fontanelle is large, tense, and non-pulsatile, and the sutures are excessively wide ( Fig. 16.24A ). Divergent strabismus, abducens nerve paresis, and impaired upward gaze are important ocular findings. With severe hydrocephalus, there may be forced, conjugate downward deviation of the eyes so that the inferior half of the iris is hidden by the lower eyelid, producing the “sunsetting sign” (see Fig. 16.24B ). Neurologic abnormalities include developmental delay, persistence of early infantile automatisms, and spasticity and hyperreflexia of the lower extremities. CT or MRI scans demonstrate enlargement of the ventricular system and thinning of the cortical mantle and may provide additional anatomic information concerning the etiology (see Fig. 16.24C , D ).
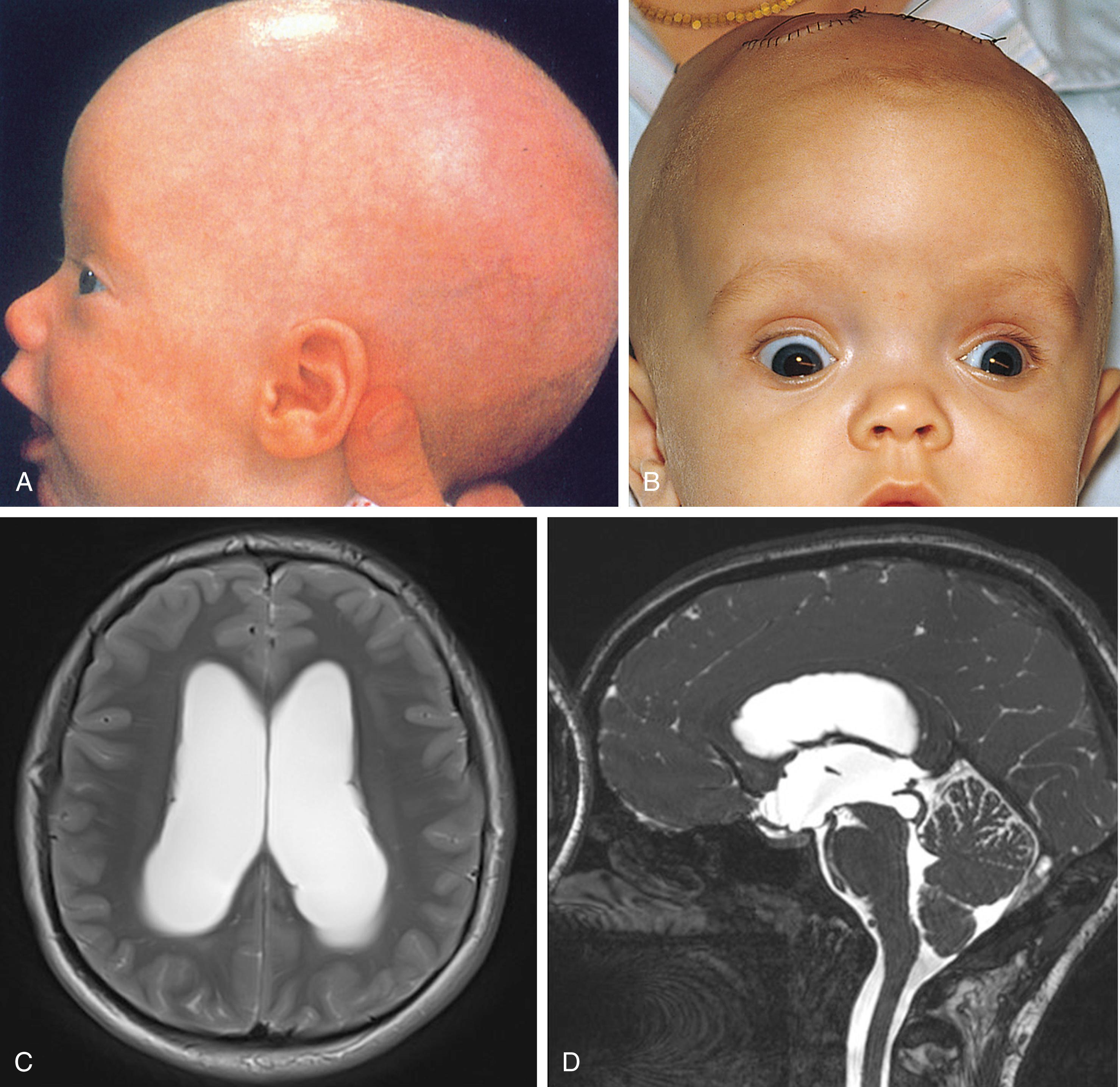
Infantile hydrocephalus must be distinguished from other causes of macrocephaly in infancy, such as chronic subdural hematoma, expanding porencephalic cyst, and certain degenerative disorders that may produce abnormal enlargement of the head (see Table 16.2 ). In premature infants with suspected hydrocephalus, the normally rapid rate of postnatal head growth must be taken into account.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here