Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
![]() Access video lecture content for this chapter online at Elsevier eBooks+
Access video lecture content for this chapter online at Elsevier eBooks+
The process of facial aging can be broken down into three major categories: (1) structural or gravitational changes; (2) correction of deflation or loss of volume; and (3) treatment of wrinkles, texture, and skin quality. The first two categories are very familiar to practitioners and the bulk of clinical and academic activities involve these areas.
The treatment of well-established wrinkles and aging textural changes has received much less attention, and since surgeons seem less well equipped to deal with them, it is simply ignored. This is regrettable because even the best performed facelift with “old” skin will still look old. Moreover, we surgeons know that surgery has no effect on perioral rhytids and a facelift can make them more noticeable because of the contrast that is created. Also, aging changes of the skin itself can have greater importance to patients than jowls or loose skin.
Why the reluctance to resurfacing? It is our contention that this is mainly due to lack of exposure and especially misconceptions about deep chemical peeling and misinformation that is still seen in professional publications. Our purpose in this chapter is to consider medium-depth trichloroacetic acid (TCA) peels and the deeper, more versatile, croton oil peels. Both authors are experienced deep peelers and PPR, a dermatologist, will share his knowledge with TCA peels. Of note, both authors are in agreement that croton oil peels offer the best solution for deeper, more established wrinkles. Regarding deep chemical peels, the topic will be distilled to its essence and give detailed practical instruction so that practitioners may consider this terrific technique and then be able to provide their patients with a more complete result. The role of facelifting is considered and, especially, the synergy of lipofilling and peeling is discussed as a particularly favorable combination.
TCA peels are the most commonly used medium-depth chemical peels, and are the most common for dermatology residents to be trained in. Their popularity over the more effective croton oil is due to three factors. First, it has not been linked to cardiac toxicity and thus does not require cardiac monitoring. Second, it does not require mixing and can be bought in different strengths. Third, it is moderately effective for mild to moderate photoaging, acne scars, skin pre-cancers (actinic keratoses), and other skin conditions. Achieving a medium-depth injury must meet both clinical and histologic criteria, as described below. Some TCA peels are used to treat superficial skin conditions, usually applied as a single agent and in low concentration (%). For example, 10–15% TCA (one coat) is used to treat melasma and acne vulgaris. Many commercial peels with TCA (usually in combination with lactic acid, salicylic acid or even phenol), produced a superficial, or at most, a superficial to medium injury. We will not cover these peels here but focus instead on a true medium-depth TCA peel, where the injury reaches the upper reticular dermis (URD).
Medium-depth TCA peels include the augmented 35% TCA peels, where Jessner’s solution (Dr. Gary Monheit ) or carbon dioxide “dry ice” (Dr. Harold Brody ) are used to increase the penetration and depth of TCA. Jessner’s solution (JS) contains 14% salicylic, 14% lactic acid, and 14% resorcinol. Two very similar peels, Obagi’s “Blue Peel” and Z.O.’s “Controlled Depth Peel” (CDP), were both developed by Dr. Zein Obagi. In these, a blue/green dye is used to help the peeler find the right depth of injury by using multiple applications of either 20% or 26% TCA, until a desired depth is found. These also contain a propriety emulsifying/surfactant agent to help penetration. Most dermatologists buy TCA from Delasco (Delasco.com, Plano, TX), which uses the weight/volume method to formulate their TCA peels.
Brody compared the depth of injury from JS or carbon dioxide/dry ice plus 35% TCA (CO 2 /TCA 35%), using one to three coats, at different times post peels. Three days post peel with JS or CO 2 followed by three applications of TCA, the epidermis has full-thickness necrosis, ghost cells with re-epithelization, and mixed dermal infiltrate of neutrophils and lymphocytes. The papillary dermal collagen fibers have been disrupted, and there is edema with increased ground substance extending to the upper reticular dermis. Thirty days post peel with a single application of TCA, there is a hyperplastic epidermis, mean of about 7 cells thick. A thickened papillary dermis is present, and there are increased collagen fibers in the upper reticular dermis. Thirty days post peel by triple application of TCA, there is a very hyperplastic epidermis (about 10 cells thick). A thickened papillary dermis, and many new collagen fibrils and increased ground substance are present in the upper reticular dermis.
When compared to the histology of croton oil peels, the biggest difference is the latter’s significant thicker band of neocollagenesis. Recent studies by Dr. Carlos Wambier et al . showed the NETosis, or a strong neutrophilic response to phorbol esters, was responsible for this neocollagenesis, rather than simply depth of injury (mid-reticular dermis).
The clinical endpoint of these peels varies. With the JS/TCA 35%, the endpoint is an even white frost with some erythema (2+ frost), and without erythema, in the background (3+ frost) ( Figs. 8.5.1–8.5.3 ). With CO 2 /TCA 35% the endpoint is also an even frost, but it will be accompanied by more edema and erythema afterwards, revealing a deeper injury ( Figs. 8.5.4–8.5.6 ). With the Obagi peels, the endpoint is an even blue edematous color and texture to the skin. The edema is such that when pinching the skin, there is no wrinkling or epidermal sliding. In all of these peels, the skin becomes edematous and red for the first 2 days. The skin dries out, with reddish tones, which then become dark brown. These sheets begin to exfoliate regionally, beginning around day 5 and around the mouth. Healing takes around 7–10 days, revealing a pink re-epithelialized fresh epidermis. Note improvement with CO 2 /TCA 35%, 30 days later ( Fig. 8.5.7 ).
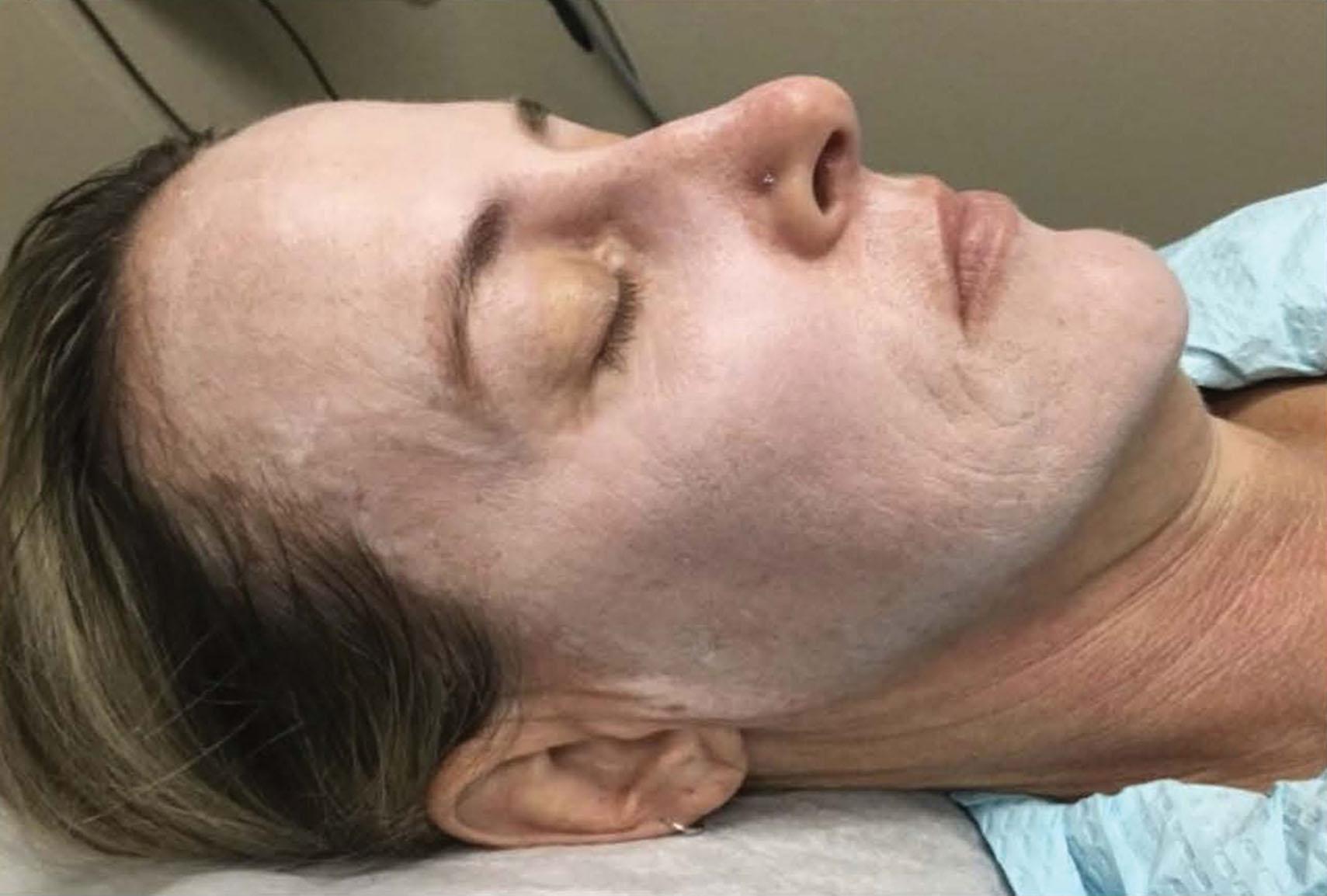
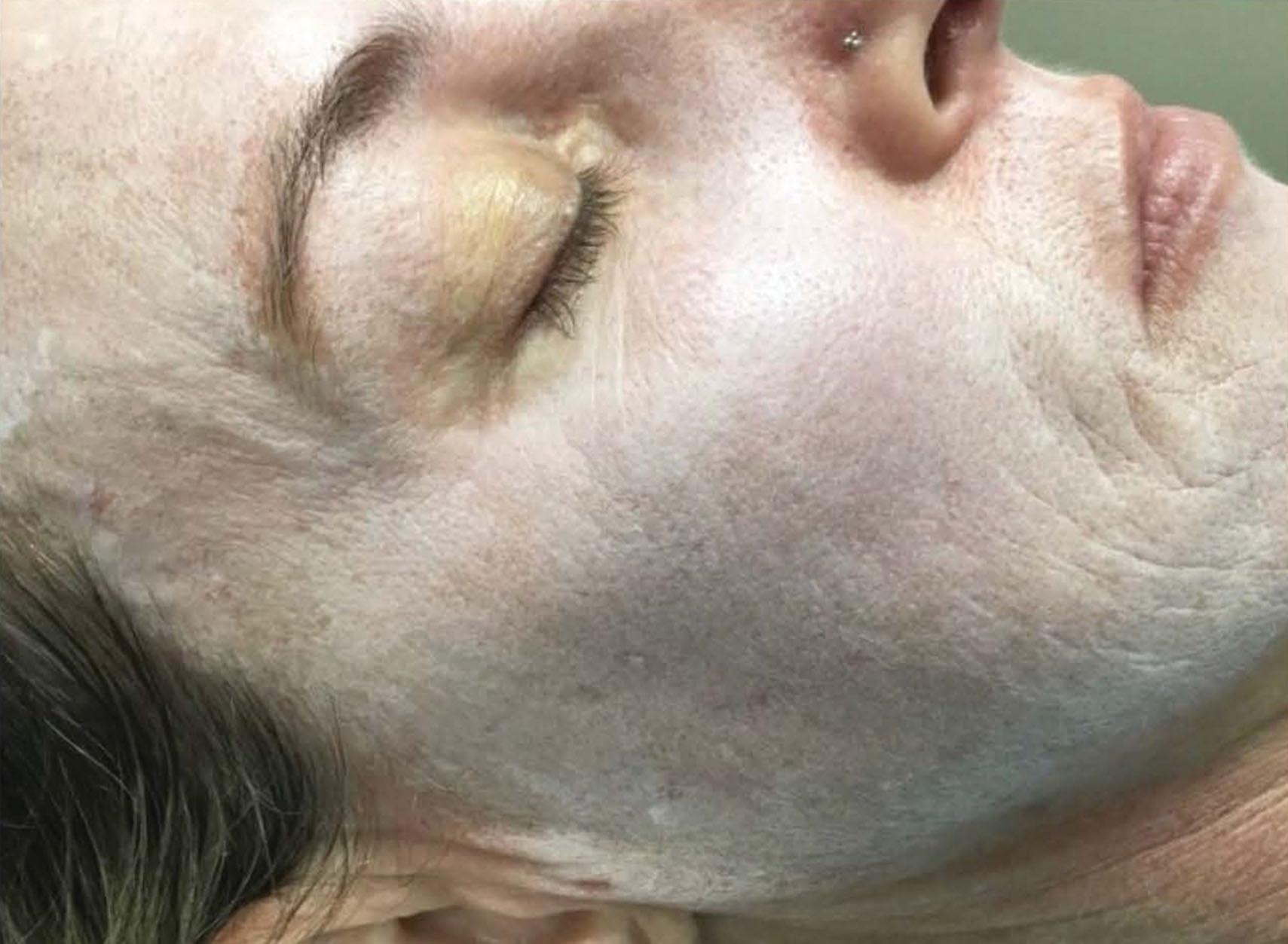
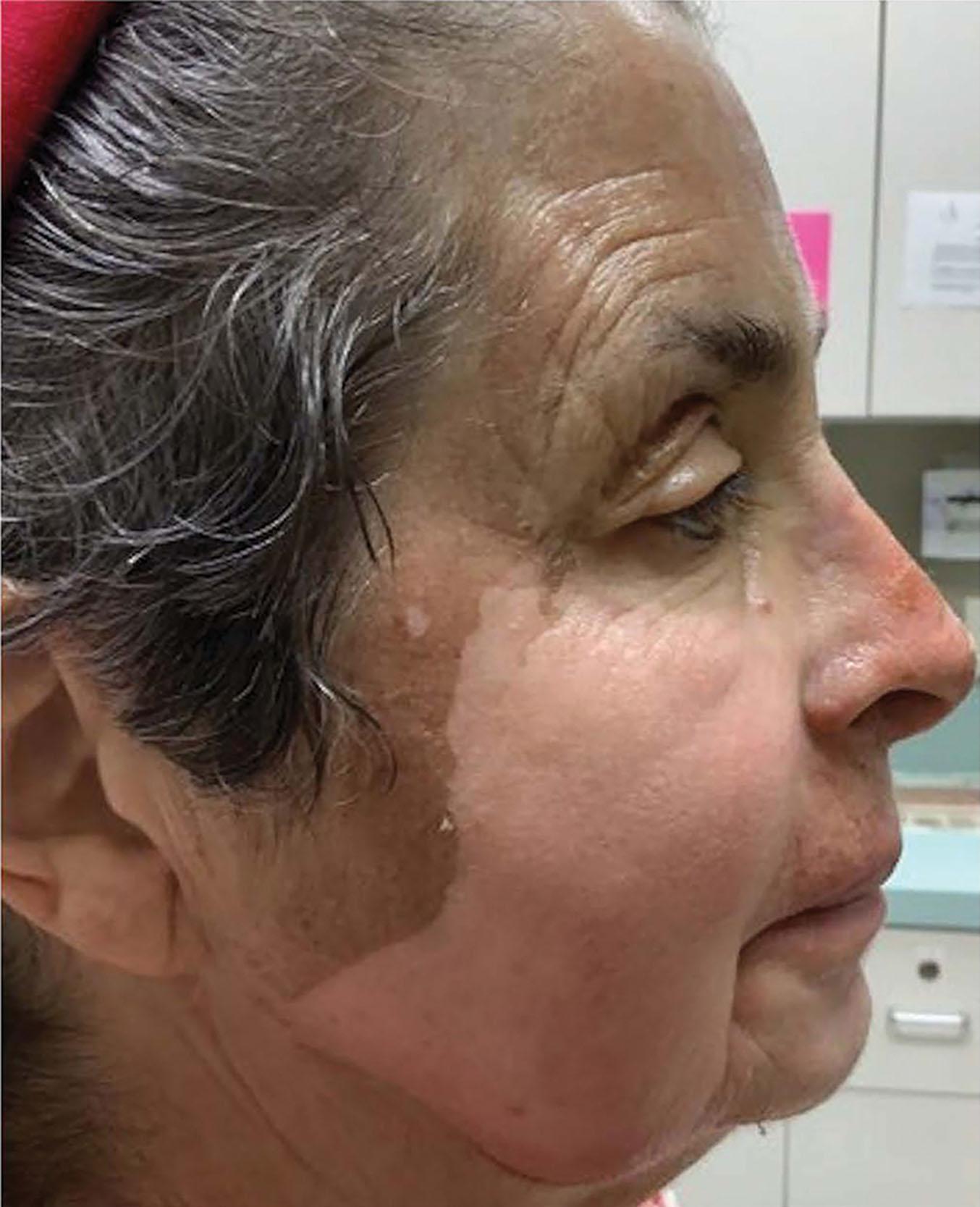
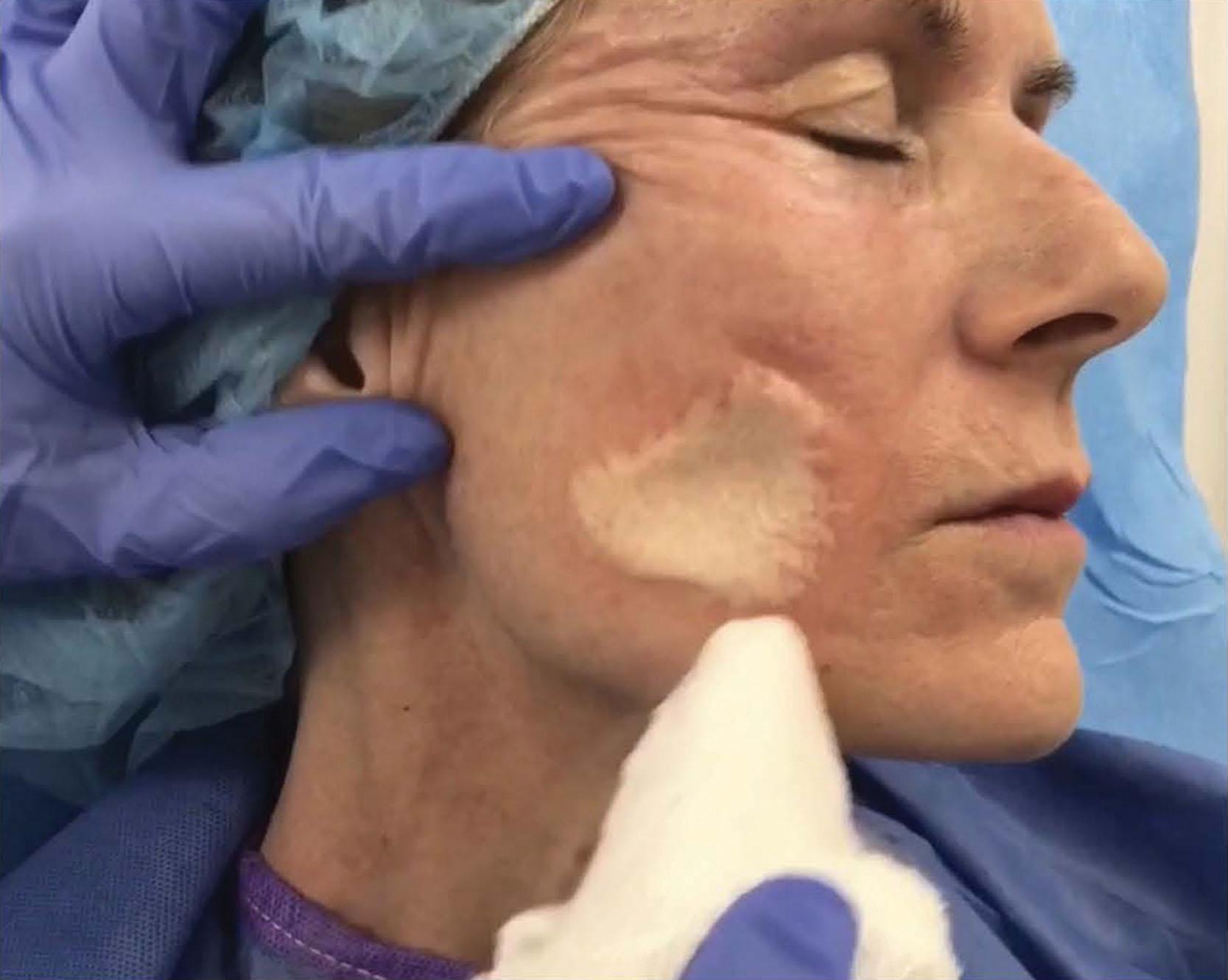
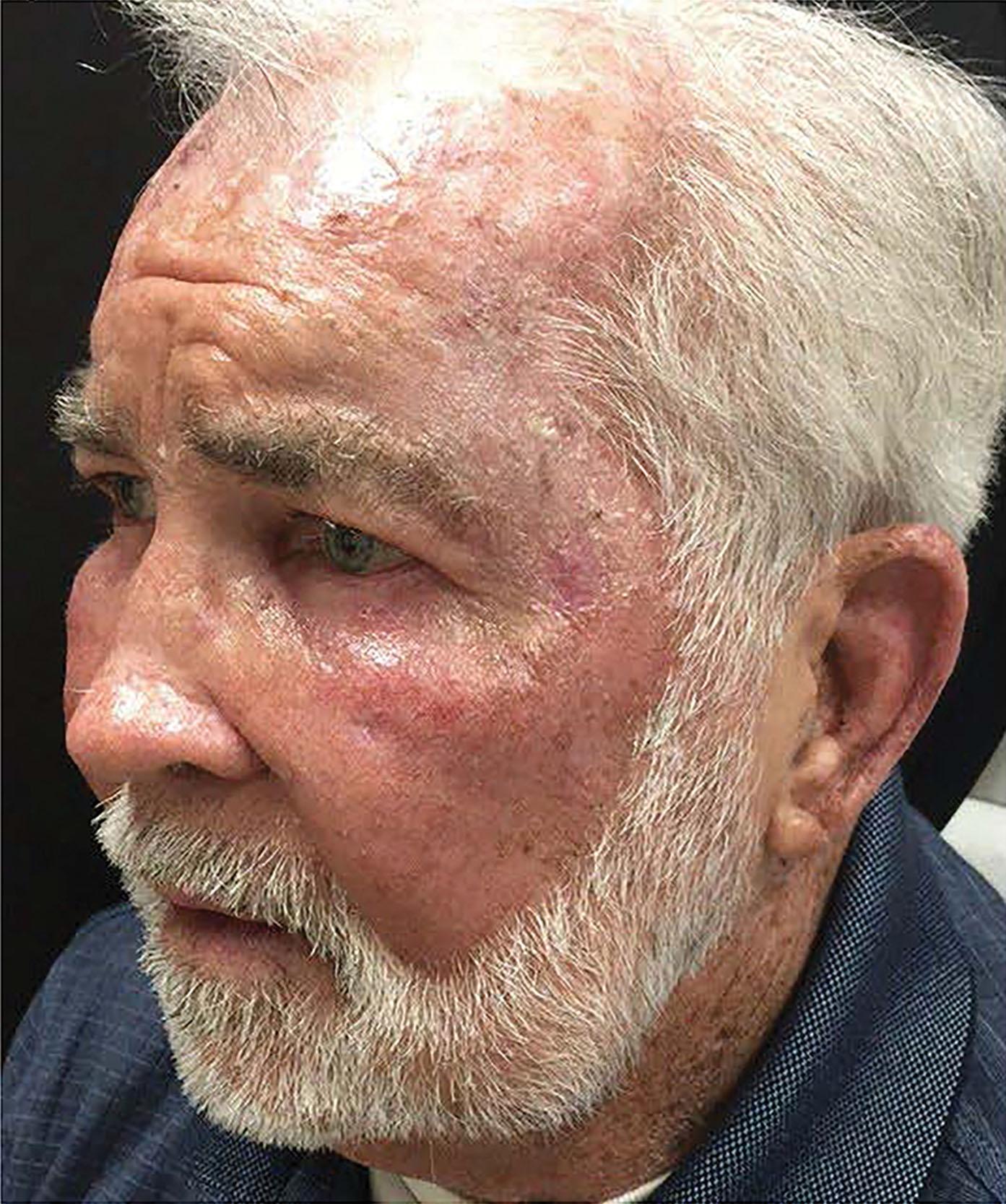

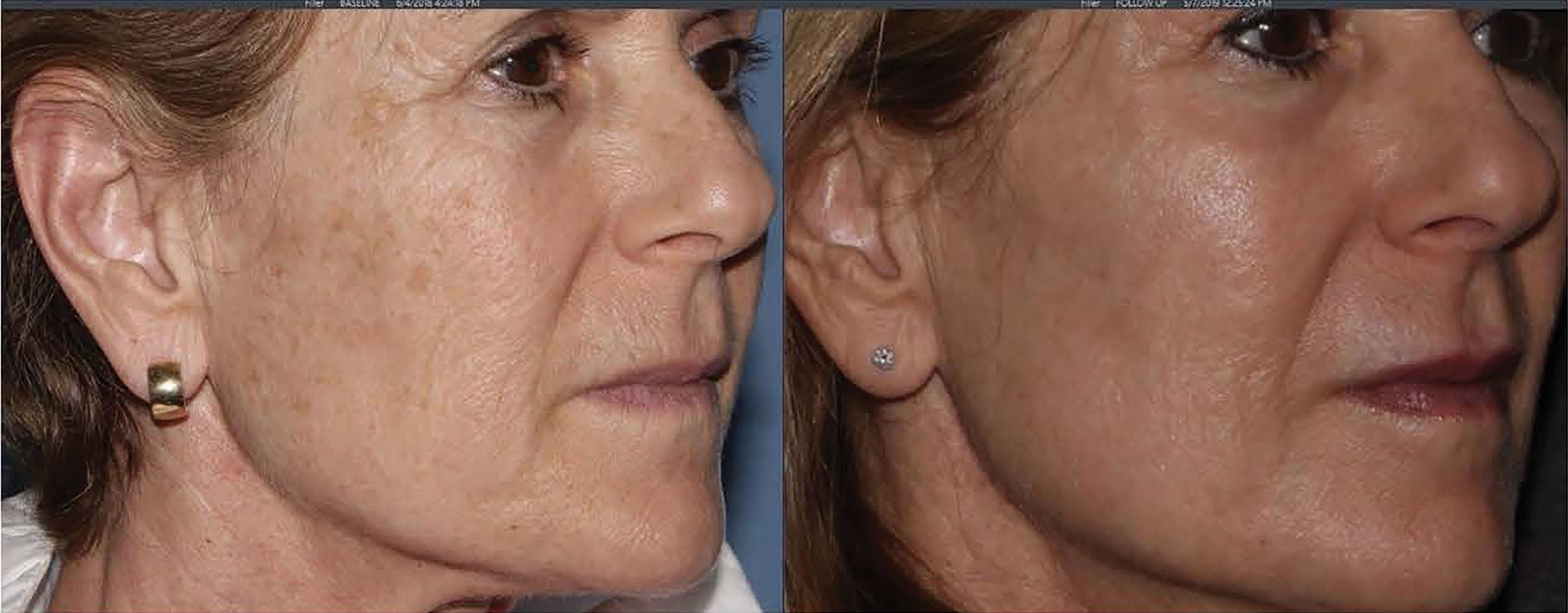
Use retinoid creams to increase cell turnover (which reduces the risk of post-inflammatory hyperpigmentation [PIH] and leads to faster healing), and to thin the stratum corneum (which enhances peel evenness and penetration). Prescribe antivirals (valacyclovir) for 10 days starting the day before peel; and instruct the home aide on the use of cold-water compresses and possible analgesics. Hydroquinone is useful in patients with risk of PIH. Stop the retinoids 4–7 days before the peel. Another tip is to remove crusts such as actinic keratoses or seborrheic keratoses before starting the peel. The author 8likes to administer 1 mg of alprazolam and 10 mg of zolpidem pre peel as oral sedatives.
Degrease the skin after washing it with a foaming cleanser, using isopropyl alcohol and acetone (pre-mixed or separately). Jessner’s is applied multiple times until a light frost is achieved, ensuring that the stratum corneal layer has been weakened. Using a non-woven 2 × 2 gauze, begin applying 35% TCA (in a metal cup), starting along the perimeter of the face like the mandibular skin and hairlines. This lets you assess the permeability and responsiveness of the skin. Then continue onto the midface, beginning in the periorbital skin and then the upper lip. Step back and let the frost develop (helps refrain from overapplying TCA). Observe. Repeat the TCA where the frost has not become confluent. Step back and observe. When satisfied, apply a very cold washcloth immersed in ice-water. Zimmer Cooler or personal electric fans help. Rarely are more than three layers of TCA needed. Beginner peelers can opt to achieve a less-dense white frost as their endpoint.
On the day of the peel, purchase an inexpensive block of dry ice (readily available in supermarkets, adjacent to the ice bags). With a small hammer, cut off a handful-size piece of ice and wrap it with a towel. Prepare a bowl with a 1 : 3 ratio of isopropyl alcohol and acetone (used to dip the dry ice right before every time it is rubbed onto the face). After thoroughly degreasing the skin, begin rubbing the dry ice in a quick rotating movement to cosmetic unit (about 10 strokes) followed by the TCA, using 2–3 strokes to achieve a frosting. Rub the dry ice lighter over bone and harder over acne scars. Use same pain control measures as for Jessner’s/TCA above.
These peels must be purchased as kits. You will also need 30% TCA. Pump the Blue Dye 4 times into a cup, followed by either 4 mL or 30% TCA (generates a 20% peel), or 8 mL of 30% (to generate a 26% peel). Once you stir this mixture, begin the peel using the same technique as the Jessner’s/TCA technique. Achieving the “total blue face” endpoint takes longer than with Jessner’s. Beginner peelers can opt to achieve a less- dense blue frost as their endpoint. Patients find it amusing to see their face turn blue. Use the same pain control measures as for Jessner’s/TCA above.
Ice-cold water compresses and over-the-counter (OTC) analgesics, like acetaminophen and ibuprofen, are usually adequate to control post-peel burning, which can last 4–8 hours. These are the most important skin care items needed initially. Once burning subsides, topical agents like Alastin Serum Nectar (Alastin Skincare, Inc., Carlsbad, CA) and Aquaphor (Beiersdorf, Inc., Stamford, CT) are the author’s (PPR) favorite agents. Aquaphor is used once the peeling begins. Alastin is used initially and after the peeling occurs, to help reduce the redness faster. Patients can resume the use of retinoids, hydroquinone, and other agents once the skin is not sensitive (around 2–3 weeks after the peel). Sunscreens with zinc oxide and iron oxide can be used as tolerated, usually 2 weeks post peel. Patients should avoid sweating and possible sunbathing for 3–4 weeks.
The history of deep chemical peels is a fascinating one, mainly involving lay peelers using “secret” formulas and shrouded in mystery. The first instance of a practical formula came from Thomas Baker, a plastic surgeon from Miami in 1961. This formula, presumably obtained from a lay peeler, was simple and could be easily reproduced. It included four ingredients: liquid phenol, three drops of croton oil, water, and a surgical soap Septisol to act as a surfactant to allow miscibility of the aqueous and oily components. The presumption was that the phenol was the peeling agent and it was unclear what the croton oil did.
In 1962, Dr. Baker halved the volume of the formula, presumably for convenience, while keeping the three drops of the croton oil unchanged. This change appeared inconsequential, but it elevated the concentration of the croton oil to 2.1% and affected the course of chemical peeling. This formula was published nationally and became the standard for decades. This peel worked very well in improving severe wrinkles, but it also caused significant and predictable hypopigmentation. The results were certainly there, but patients developed an unnatural porcelain look that necessitated the permanent use of make-up. Due to this, the Baker peel, as it became known, was reserved for older, light-eyed individuals.
It was believed that phenol had an “all-or-none” phenomenon that was out of the surgeon’s control. Phenol also had the reputation of being cardiotoxic, requiring careful timing and strict cardiac monitoring. For these reasons, “phenol peels” carry a negative reputation that persists to this day and has limited their acceptance despite more recent improvements.
The crucial step in the development of modern chemical peels came about from the work of Gregory Hetter. Hetter, a plastic surgeon in Las Vegas, frustrated by his options of resurfacing, took a scientific approach in the hope of better understanding the Baker formula. Hetter experimented by performing a number of peels with different combinations of the ingredients and discovered that phenol alone has little effect. Adding croton oil to the phenol at different concentrations resulted in deeper peels proportional to the concentrations of the croton oil. An analysis of the classic Baker formula showed for the first time that the croton oil concentration was very high at 2.1% – responsible for the results as well as the hypopigmentation. Recognizing that croton oil, not phenol, was the peeling agent, Hetter could now alter the concentration so as to give the clinical result without negatively altering the quality of the skin. An important observation was that the “all-or-none” phenomenon ascribed to phenol was simply that the croton oil concentration was so high that it immediately peeled to the point of hypopigmentation. This may seem a small difference but it is actually a fundamental change that ushered in the modern era of chemical peeling. Being able to choose the croton oil concentration allowed the procedure to be performed superficially or deep and made it applicable to all ages and skin types. An important improvement was that different croton oil concentrations could be used in different areas of the face depending on skin thickness and clinical need. A critical change was that with weaker croton oil concentrations, the application technique became an important factor in determining the depth reached. The entire process is slowed down so that the surgeon can observe the skin changes and stop at the depth deemed appropriate. In this manner, the surgeon is in precise control and the process becomes orderly and predictable.
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here