Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Early postoperative ischemia (<30 days) is frequently due to graft occlusion or stenosis, and percutaneous coronary intervention (PCI) is often feasible.
Unstable angina or ST–segment–elevation myocardial infarction (STEMI) years after coronary artery bypass grafting (CABG) is most often due to a saphenous vein graft (SVG) lesion; in such cases, native vessel PCI is preferred whenever possible.
Embolic protection reduces the risk of atheroembolic myocardial infarction during SVG PCI and should be used in the treatment of most de novo SVG lesions that occur years after CABG.
Multiple diseased or occluded SVGs, reduced left ventricular (LV) function, and available arterial conduits favor repeat CABG; a patent left internal mammary artery (LIMA) to the left anterior descending (LAD) coronary artery favors PCI.
Drug-eluting stents (DESs) reduce restenosis in native coronary arteries and have become the default strategy in SVGs for many operators in spite of reduced efficacy in SVGs compared with native vessels. Five randomized trials of DESs and bare-metal stents (BMSs) in SVGs yielded conflicting results.
Coronary artery bypass grafting (CABG) is a commonly performed surgical procedure whose efficacy has been enhanced by the use of arterial grafts, off-bypass procedures, and minimally invasive surgical techniques. In addition, attempts have been made to improve graft longevity with antiplatelet agents and lipid-lowering therapy. In spite of these efforts, the temporary nature of the palliative effect of CABG remains a significant health care problem. Severe myocardial ischemic syndromes occur in 3% to 5% of patients immediately after surgery; thereafter, recurrent ischemic symptoms appear in 4% to 8% of post-CABG patients annually. Saphenous vein graft (SVG) attrition, the most common cause, is up to 40% during the first year; 1% to 2% of grafts occlude annually 1 to 5 years after surgery, and 5% occlude each year over the next 5 years. At 10 years, one half of all SVGs are occluded, and half of the patent SVGs are diseased.
In experience at Emory University Hospital and the Cleveland Clinic, reoperation was required in about 3% of patients by 5 years, 15% by 10 years, and 30% by 15 years. For reoperation, even in the most experienced centers, the risk of in-hospital death and nonfatal Q-wave myocardial infarction (MI) is triple that of the initial operation. In the state of New York, in-hospital mortality was 4.1% for initial operations but 11%, 25%, and 39% for first, second, and third reoperations, respectively. In addition to being more risky, reoperative surgery was associated with less complete anginal relief and reduced graft patency, probably attributable to more advanced disease and poorer graft conduits. These factors have promoted a conservative approach to reoperation and have favored the use of percutaneous coronary intervention (PCI). In addition, many symptomatic patients who are candidates for percutaneous methods would not be considered for reoperation because of a limited amount of myocardial ischemia, risk to patent grafts, lack of suitable conduits, poor left ventricular (LV) function, advanced age, or coexisting medical problems. Recently published data from the Society of Thoracic Surgery (STS) national database showed that among patients aged 65 years and older who survived following an initial CABG operation, rates of repeat revascularization at 1, 5, 10, and 18 years were 2%, 8%, 16%, and 25%, respectively, and that the mode of revascularization was mostly PCI (93%). Factors associated with a higher rate of repeat revascularization included female sex, diabetes, prior PCI, dialysis, and incomplete revascularization. In the past decade at Emory, approximately 10% of the patients who underwent PCI had had a prior CABG, and bypass graft intervention was the most common indication. It is in this difficult group of patients, those who require bypass graft intervention, that decision making is particularly critical owing to the increased up-front risk and reduced long-term benefit of such intervention.
Patients who experience recurrent ischemia after coronary bypass surgery have diverse anatomic problems; therefore selection for PCI must be based on careful analysis of the projected outcomes of competing strategies. The status of the left anterior descending (LAD) and its graft significantly influences revascularization choices because of its impact on long-term outcome and the lack of survival benefit of reoperative surgery to treat non–LAD-related ischemia. Factors that favor surgical revascularization include multiple-vessel involvement, severe vein graft disease, poor LV function, total occlusions of native coronary arteries, and the availability of arterial conduits. Because the choice among percutaneous methods and the relative effectiveness of each are often influenced by the time elapsed since surgery, indications are considered relative to this factor.
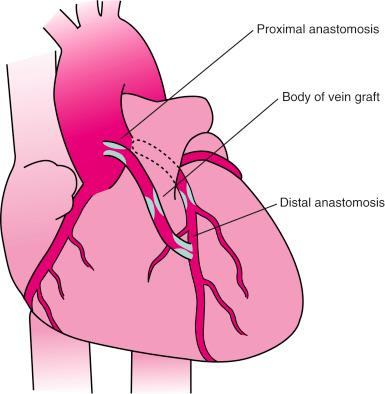
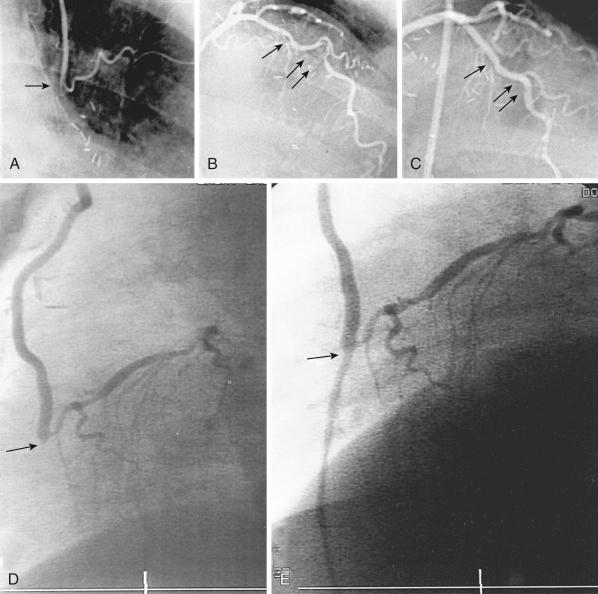
The performance of routine intraoperative angiography at the conclusion of CABG at one center and four recent trials in which routine angiography was performed at 12 months to assess graft patency have provided sobering insights regarding contemporary CABG. Among 366 consecutive patients who underwent intraoperative completion angiography, Zhao and colleagues found that 12% of bypass grafts had defects important enough to require intervention (open surgical revision, 3.4%; open-chest PCI, 6%; and minor adjustment, 2.8%). In a randomized trial in over 100 high-volume U.S. centers that included over 3000 patients in whom modern surgical techniques and medications were utilized, graft failure at 1 year occurred in 41.6% of SVGs with a single distal anastomosis and 50.6% with multiple distal anastomoses. In the PRAGUE-4 (randomized comparison between off-pump and on-pump surgery) trial, angiographic follow-up at 1 year revealed that 40% of SVGs and 9% of left internal mammary artery (LIMA) grafts were occluded. In the Veterans Affairs Randomized On/Off Bypass (ROOBY) study, 23% of SVGs and 11% of LIMA grafts performed off-pump failed at 1 year. In the DACABG trial conducted in 2014 to 2015, patients undergoing elective CABG and treated with aspirin postoperatively experienced a 24% rate of SVG failure. Graft failure was associated with death, new MI, or repeat revascularization in 26% of patients. Recurrent ischemia within days of surgery is usually related to acute vein graft thrombosis due to endothelial damage during harvesting and initial exposure to arterial pressure. However, stenosis may exist at proximal or distal anastomoses ( Fig. 27.1 ); a bypass graft may be kinked; the wrong vessel may have been bypassed; or the revascularization may have been rendered incomplete as a result of diffuse disease, stenoses distal to graft insertion, or inaccessible intramyocardial position of a recipient artery. To determine the cause of severe early postoperative myocardial ischemia and define therapeutic options, coronary arteriography has been carried out within a few hours of surgery in 3% to 4% of patients in some centers, and this strategy is recommended. PCI in patients with early ischemia after CABG is a class I indication in the American College of Cardiology(ACC)/American Heart Association (AHA)/Society for Cardiovascular Angiography and Interventions (SCAI) PCI guidelines and the European guidelines on revascularization. Although 44 of 145 patients (30%) catheterized because of ischemia early after surgery had no apparent cause for ischemia, many patients had correctable problems; 30 patients had emergency reoperation and 44 underwent PCI. In a recent report, emergency coronary angiography was performed in 118 of 5427 CABG patients, of whom 57% had graft failure and 60% underwent repeat revascularization. In seven patients, focal stenosis was present in a venous or arterial graft distal anastomosis, and balloon dilation across suture lines was safe in these patients. However, in our experience ( Fig. 27.2 ) and in that of others, extreme care is warranted within a few hours after surgery to ensure an intracoronary position of the steerable guidewire, indicating that the guidewire has not penetrated a suture line. In addition, balloon sizing should be conservative; we are aware of unreported cases of suture-line disruption and severe hemorrhagic complications. It is noteworthy that European guidelines advise against PCI of a graft anastomosis early after CABG because of this risk of perforation. Immediate access to a covered stent is essential, should suture line perforation occur. Mild to moderate imperfections at the anastomosis observed in the early postoperative period should not be dilated because they frequently disappear on subsequent angiography, suggesting the presence of edema. Some have attributed these observations to the self-reparative ability of the LIMA. If a thrombosed graft is discovered, PCI of the native coronary artery is recommended, but mechanical thrombectomy can be attempted—or a return to the operating room may be considered—if the jeopardized vessel is of significant importance. Use of thrombolytic agents or glycoprotein (GP) IIb/IIIa inhibitors in the early postoperative period carries substantial risk of bleeding. Patients at increased risk for early postoperative ischemia include those undergoing minimally invasive and “off-bypass” techniques and those who receive noninternal mammary arterial grafts.
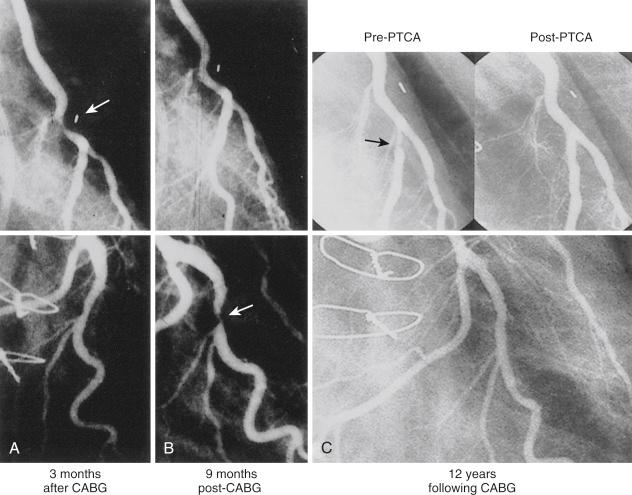
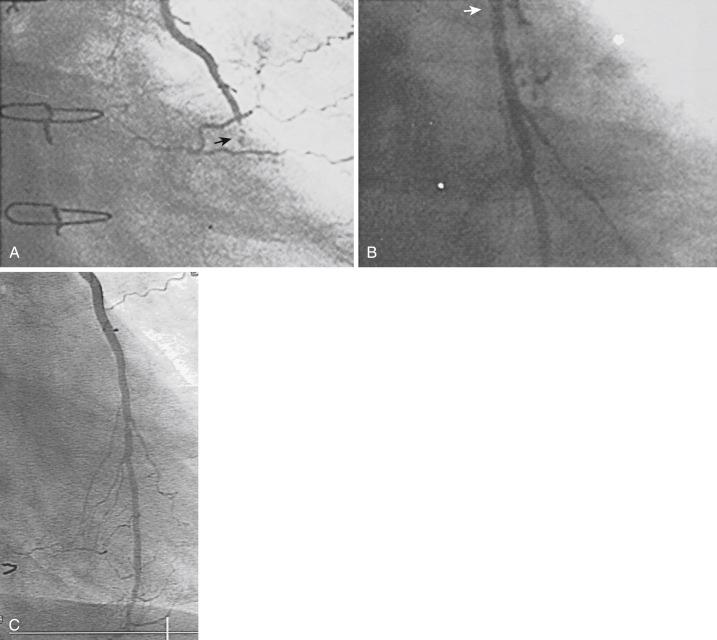
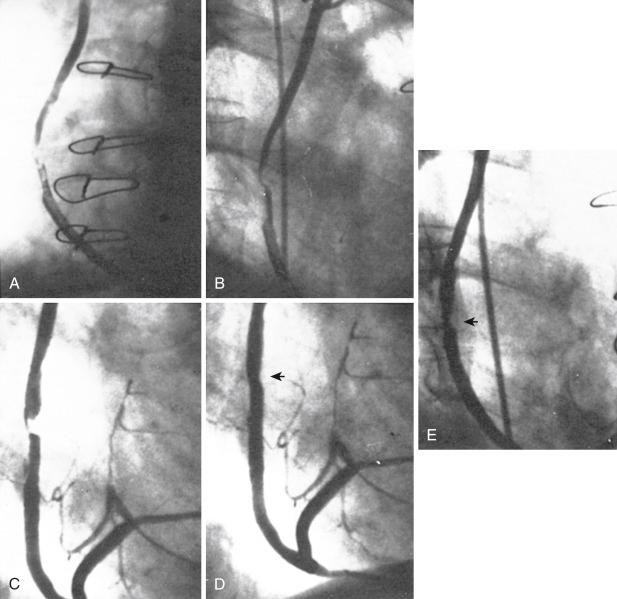
When ischemia recurs 1 to 12 months after surgery, perianastomotic stenoses are among the most common problems ( Fig. 27.3 ). Stenotic lesions of the distal anastomosis of saphenous vein or arterial grafts can be successfully dilated with balloon angioplasty at this time with little morbidity and good long-term patency in 80% to 90% of patients without stent implantation. Among 34 patients with distal anastomosis lesions reported from our early experience, 25 (74%) presented within 1 year of CABG. Thirty-two were successfully dilated, and three of four restenosis lesions redilated. A total of 30 of 32 patients were asymptomatic at 10 months. Stenoses, or in some cases total occlusions, of the middle or distal portions of the internal mammary artery (IMA) or radial artery grafts may be dilated successfully ( Fig. 27.4 ), especially when the presence of a short occlusion can be documented. Stenotic lesions of mid-SVGs that occur within a year of surgery are usually the result of intimal hyperplasia; these lesions can be dilated with balloon angioplasty and/or stented with little risk of distal embolization, but recurrence has been noted in about 50% of cases in our experience, and periprocedural graft perforation has been observed. Stents, directional coronary atherectomy, and excimer laser angioplasty have all been tried for the treatment of proximal anastomotic lesions that occur within a year of surgery with excellent initial results but significant rates of restenosis. Data are sparse regarding the use of drug-eluting stents (DESs) at this site.
Patients with recurrent ischemia 1 to 3 years after surgery frequently have new stenoses in graft conduits and native coronary arteries that are amenable to percutaneous intervention. Whenever possible, native coronary lesions are targeted. The ACC/AHA/SCAI PCI guidelines consider focal ischemia–producing graft lesions in patients 1 to 3 years after CABG with preserved LV function to be a class IIa indication (“conflicting evidence, weight of evidence/opinion in favor of usefulness”).
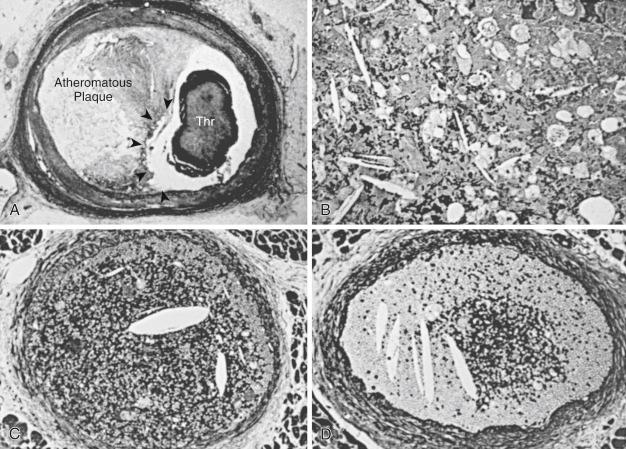
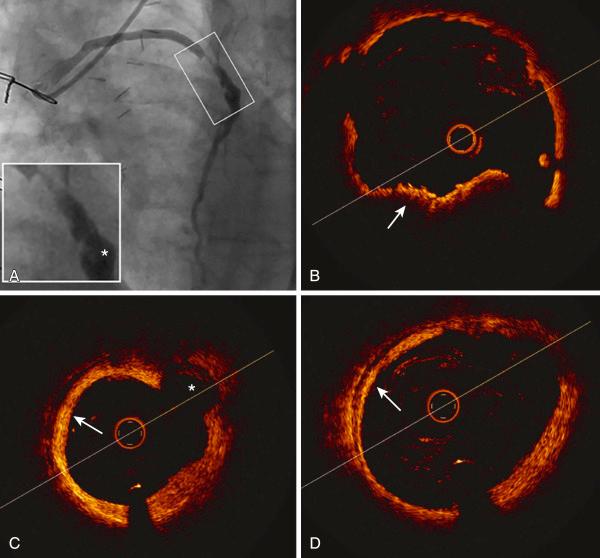
Beginning about 3 years after implantation, atherosclerotic lesions appear in vein grafts with increasing frequency. Unstable ischemic syndromes are common, and aggressive invasive evaluation and therapy are indicated. In about 70% of post-CABG patients who present with an acute coronary syndrome (ACS), the culprit lesion is located in an SVG. Atherosclerotic plaques in vein grafts contain foam cells, cholesterol crystals, blood elements, and necrotic debris, with less fibrocollagenous tissue and calcification than are present in native coronary arteries ( Fig. 27.5 ). Consequently, the plaques in older vein grafts may be softer and more friable, as well as being larger than those observed in native coronary arteries, and they frequently have thin fibrous caps and associated thrombus formation ( Fig. 27.6 ). Recently published optical coherence tomography (OCT) studies of older SVGs in patients with stable angina surprisingly documented the presence of thrombus in most patients and in patients with ACSs revealed the enormous complexity of SVG lesions ( Fig. 27.7 ). Atheroembolism related to graft intervention may have catastrophic consequences. Consequently, bulky vein graft lesions (those with a large potential atheroma mass) should be avoided if possible. Improved initial outcome has been reported with stent placement compared with balloon dilation in SVGs. However, long-term results in SVGs have been disappointing. Data on long-term outcomes with DESs in SVGs are limited (see Drug-Eluting Stents in Vein Grafts section), and the role of percutaneous techniques in totally occluded SVGs is controversial.
After coronary bypass surgery, approximately 3% of patients experience ST-segment elevation myocardial infarction (STEMI) annually. Because these patients were excluded from early reperfusion trials, therapy has been based on clinical experience and remains controversial. In a majority of patients, the culprit vessel has been found to be a vein graft, and considerable lesion-associated thrombus was a common accompaniment (see Fig. 27.6 ). Intravenous thrombolytic therapy is relatively ineffective in SVGs. Most investigators currently favor emergency coronary arteriography and the option of more specific intervention, including thrombectomy and mechanical recanalization. Among approximately 1000 patients with STEMI and a history of prior CABG reported from the National Cardiovascular Data Registry (NCDR), post-CABG patients were older, had more lesion complexity, and had lower likelihood of a door-to-balloon time ≤90 minutes (76%). This delay to treatment warrants a “call to action” in the post-CABG patient with STEMI. Among almost 80,000 patients undergoing primary PCI in England and Wales between 2007 and 2012, 2658 had prior CABG, and these patients had more comorbidities and higher mortality at 30 days and 1 year. The culprit vessel was a bypass graft in 56% and native coronary artery in 44%. Recent reports indicate that both acute and long-term results of PCI in SVGs for treatment of STEMI are inferior to those of native vessel PCI for STEMI. In a study of 2240 consecutive patients with STEMI, Brodie and colleagues observed that patients who underwent SVG PCI were sicker (had poorer LV function, more three-vessel disease, and prior MI) than patients who underwent native vessel PCI. Patients with SVG occlusion had lower rates of thrombolysis in myocardial infarction (TIMI) grade 3 blood flow, higher in-hospital mortality (21% vs. 8%, P = .0004), and worse 10-year survival (49% vs. 76%, P < .0001). SVG patency was 64% at 1 year. In the Mayo Clinic STEMI experience, treatment of an SVG was independently associated with adverse cardiac events. In a report of 192 post-CABG patients with acute MI, 30-day mortality with SVG PCI was significantly higher than that with native vessel PCI (14.3% vs. 8.4%, P = .03). The ACC/AHA Task Force Report on Early Management of Acute Myocardial Infarction classified PCI for vein graft recanalization as a class IIa intervention: “acceptable, of uncertain efficacy and may be controversial; weight of evidence in favor of usefulness/efficacy.”
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here