Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Epidermal nevi are of the following three subtypes, which are histologically identical and differ only in the degree of clinical involvement:
nevus verrucosus,
nevus unius lateris,
ichthyosis hystrix (this has no relationship to ichthyosis).
Lesions, which may be present at birth or develop during childhood, are usually yellowish-brown warty papules or plaques with irregular margins. They commonly affect the trunk or limbs and vary from trivial small lesions to very extensive areas of involvement that may cause the patient great cosmetic embarrassment ( Fig. 24.1 ). They can follow a Blaschkoid distribution. The sex incidence is equal and there is no racial predilection. Familial cases may rarely be seen and are transmitted in an autosomal dominant fashion.
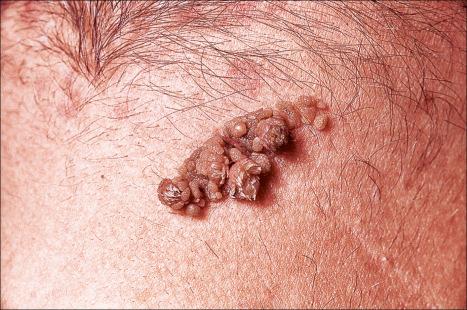
Nevus verrucosus refers to solitary or multiple localized lesions, nevus unius lateris refers to a more severe unilateral linear distribution, and ichthyosis hystrix refers to the most extreme example with a bilateral or generalized distribution ( Figs 24.2 and 24.3 ). Rare but important complications are development of basal cell and squamous cell carcinoma in addition to keratoacanthoma, eccrine syringofibroadenoma, syringocystadenoma papilliferum, and clear cell acanthoma. Unusual presentations include onset in adulthood; involvement of the maxilla, palm, or oral mucosa; and a bilateral symmetric distribution. Association with a number of diseases and syndromes has been reported including KID (keratitis-ichthyosis-deafness) syndrome, CHILD (congenital hemidysplasia with ichthyosiform nevus and limb defects) syndrome, CLOVE (congenital lipomatous overgrowth, vascular malformations, and epidermal nevi) syndrome, SCALP (nevus sebaceous, central nervous system malformations, aplasia cutis congenital, limbal dermoid and pigmented nevus) syndrome, Gardner syndrome, Rubinstein-Taybi syndrome, precocious puberty, hypophosphatemic vitamin D-resistant rickets, digital constrictions, divided fingers, localized cranial defects, hemimegalencephaly, temporal lobe enlargement, vascular anomalies and malformations, renal artery stenosis, polyostotic fibrous dysplasia, choristomas, hypermelanosis and chronic hyponatremia, segmental hypermelanosis, trichilemmal and proliferating trichilemmal cysts, central nervous system (CNS) lipomas, mandibular ameloblastoma, chondroblastoma, rhabdomyosarcoma, transitional cell carcinoma, multiple apocrine adenomas, and malignant eccrine poroma. Epidermal nevi may also present together with nevus sebaceous, woolly hair nevus, and nevus comedonicus. They may also rarely be complicated by a dermatitis such as psoriasis.
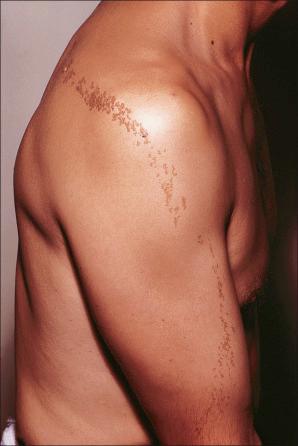
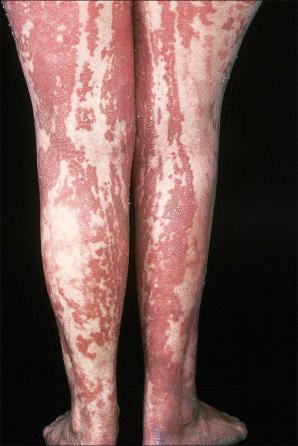
Patients with the epidermal nevus syndrome show a variety of systemic manifestations. They also have an increased incidence of café-au-lait macules, congenital hypopigmented macules, congenital as well as Spitz melanocytic nevi, and a range of vascular malformations. Visceral features particularly affect the skeletal, ocular, and central nervous systems. These include kyphoscoliosis, bone cysts, genu valgum, skull abnormalities, limb reduction defects, strabismus, mental retardation, delayed motor milestones, cranial nerve palsies and nonfebrile seizures. Patients with the epidermal nevus syndrome may have an increased incidence of systemic malignancy. More recent studies suggest that the epidermal nevus syndrome is a heterogeneous group of disorders that can be separated by clinical and pathological as well as genetic criteria. Happle has suggested nine distinct syndromic entities, each associated with distinct epithelial nevi. Others have recently suggested largely overlapping but not identical groupings.
This is a rapidly evolving area and increased discovery of mosaic mutational genotypes is informing the definition of discrete entities. It is increasingly recognized that many epidermal nevi are manifestations of mosaic RASopathy as will be discussed further below. Other genes such as FGFR3 , PTEN , AKT1 , PIK3CA , PTEN and others can also be involved in mosaic fashion. We briefly present some of the distinguishing features of 12 relatively well-defined syndromes with prominent epidermal nevi:
Schimmelpenning syndrome (nevus sebaceous syndrome),
nevus comedonicus syndrome,
pigmented hairy epidermal nevus syndrome (Becker nevus syndrome),
angora hair nevus syndrome,
Proteus syndrome,
type 2 segmental Cowden disease,
FGFR3 epidermal nevus syndrome,
CHILD syndrome,
porokeratotic adnexal ostial nevus,
phakomatosis pigmentokeratotica,
inflammatory linear verrucous epidermal nevus syndrome,
cutaneous-skeletal hypophosphatemia syndrome.
Schimmelpenning syndrome (Schimmelpenning-Feuerstein-Mims syndrome, organoid nevus phakomatosis) is characterized by unilateral nevus sebaceous of the head and neck in combination with cerebral, ocular, cardiac, vascular, and skeletal abnormalities. It is believed to represent a lethal autosomal inherited condition with survival dependent upon a mosaic state. It appears to be driven by postzygotic activating mutations in either HRAS , KRAS , or NRAS recently coined as “mosaic RASopathy.” A dominant variant presenting in one of two monozygotic twins is compatible with de novo postzygotic mosaicism. Neurological abnormalities include mental retardation, convulsions, hemiparesis, cranial asymmetry, and hydrocephalus. Oral involvement has also been documented. Patients may present with gingival papillomata, hemihypertrophy of the tongue, bone cysts, aplasia of teeth, and hypoplastic or absent enamel as well as pigmented malformed teeth, multiple odontomas, bilateral maxillary fibro-osseous lesions, recurrent central giant cell granulomas of the jaw, and adenomatoid odontogenic tumor. Ocular manifestations take the form of microphthalmos, eyelid coloboma, nystagmus, ptosis, dermoids, and teratomas of the conjunctiva. Skeletal abnormalities include skull asymmetry, exostoses, and scoliosis.
The nevus comedonicus syndrome consists of nevus comedonicus, cataract, and skeletal defects.
The pigmented hairy epidermal nevus syndrome comprises Becker nevus in association with ipsilateral hypoplasia of the breast and other cutaneous as well as skeletal anomalies.
The exceedingly rare angora hair nevus syndrome (Schauder syndrome) shows a nevus with prominent soft white hair that occurs along Blaschko lines. Associated cerebral and ocular malformations and dysfunctions can occur along with skeletal deformations and facial features. The white hair and lack of breast hypoplasia distinguishes it from Becker nevus syndrome.
Proteus syndrome is an exceedingly rare hamartomatous condition that can be very disfiguring and is associated with an increased risk of malignancy. It is sporadic and is thought to result from mosaicism for a mutation that is lethal in the nonmosaic state. Males are more frequently affected than females and the syndrome is associated with an increased risk of premature death. A subset has been linked to PTEN mutations, thereby displaying genetic in addition to clinical overlap with other hamartomatous conditions including Cowden syndrome and Bannayan-Riley-Ruvalcaba syndrome. This group is now termed the PTEN hamartoma tumor syndromes. Recent mutational analyses of patients with ‘bona fide’ Proteus syndrome, however, failed to detect mutation in the PTEN gene and the contribution of PTEN mutations remains an issue of ongoing debate. Rather than PTEN , very recent data suggest constitutive and mosaic activating mutations in PIK3CA and AKT1 , encoding critical kinases in the PTEN/PIK3CA/AKT signaling pathway. It is now considered to be part of the PIK3CA-related overgrowth syndrome (PROS) group rather than the related PTEN hamartoma tumor syndromes. Proteus syndrome is a complex disorder comprising malformations and overgrowth of multiple tissues in addition to epidermal nevi. The latter are flat, soft, and of nonorganoid type and are present in about two-thirds of cases. They are associated with other cutaneous anomalies such as connective tissue nevi, cystic lymphangiomas, hemangiomas, lipomas, and fibromas. Cerebriform hyperplasia of the plantar connective tissue (moccasin lesion) is a characteristic finding. A hallmark of Proteus syndrome is asymmetrical hypertrophy affecting the face, limbs, and trunk including macrocephaly and hemihypertrophy of the body. Macrodactyly is thought to be characteristic.
Other noncutaneous manifestations include bony exostoses, kyphoscoliosis, spinal canal stenosis, hydrocephalus, hemimegancephaly, CNS cysts, seizures, epibulbar tumors, enlargement of the eye, cataract and strabismus, paraovarian endometrioid cystic tumors, genitourinary abnormalities, and nephrogenic diabetes insipidus. Patients are at increased risk for a number of tumors including testicular papillary adenocarcinoma, ovarian cystadenoma, meningioma, parotid monomorphic adenoma, astrocytoma, optic nerve tumor, leiomyoma, and endometrial carcinoma.
Linear Cowden nevus syndrome is associated with non-organoid epidermal nevus that is soft and thick with distinctly papillomatous features. This occurs in the setting of PTEN loss of function mutation heterozygote that undergoes embryonal loss of heterozygosity. It lacks the cerebriform hyperplasia of the palms and soles seen in Proteus syndrome.
Two patients from families with Cowden syndrome have been described with a unique phenotype related to bi-allelic inactivation of PTEN . These patients showed classic features of Cowden syndrome in addition to segmental overgrowth, lipomatosis, arteriovenous malformation, and linear epidermal nevus for which the term SOLAMEN syndrome has been proposed. These are likely identical to type 2 segmental Cowen disease. It is possible that biallelic PTEN loss might result in levels of PIK3CA and AKT activity that resemble that seen from the direct mutation activation of these genes in Proteus syndrome and thus partially phenocopy Proteus syndrome. A small subset of Cowden patients are also reported to harbor activating PIK3CA and AKT1 mutations instead of the characteristic inactivating PTEN mutations.
A mosaic FGFR3 mutation was detected in a patient with epidermal nevus syndrome with cerebral involvement. Underlying neurological and structural deficits can be seen in this syndrome. FGFR3 epidermal nevus syndrome (Garcia-Hafner-Happle syndrome) shows a soft velvety epidermal nevus specifically driven by mosaic activating mutations in FGFR3 (usually R284C). This same activating mutation is seen in up to one-third of keratinocytic nevi that are nonepidermolytic in type as well as some sporadic seborrheic keratoses. FGFR3 and PIK3CA activating mutations are also seen in familial seborrheic keratosis.
CHILD syndrome is an X-linked dominant disorder almost exclusively affecting females and is characterized by a unique epidermal nevus involving one side of the body in addition to ipsilateral defects of the limbs and internal organs. Mutations in the NSDHL (NADPH steroid dehydrogenase-like protein) gene, which is located on Xq28 and is involved in the cholesterol synthesis pathway, have been identified in this syndrome. The CHILD nevus is a unilateral, circumscribed, inflammatory, ichthyosiform nevus typically presenting at birth. It is erythematous and covered by yellow, waxy scales. Frequently, the body folds are affected. It may be linear and follow the lines of Blaschko. Disease presentation can be mild and familial, affecting multiple generations.
Histologically, the cutaneous manifestations are characterized by psoriasiform epidermal hyperplasia, and features reminiscent of verruciform xanthoma may be present. Ultrastructural data suggest that the formation of the cutaneous lesion may be due to abnormal lipid metabolism. Although CHILD nevus has a distinctive presentation there is considerable overlap with inflammatory linear verrucous nevus (ILVEN). Other clinical findings in CHILD syndrome include ipsilateral hypoplasia or aplasia of limbs and other skeletal structures. Neurological defects may include hypoplasia of a cerebral hemisphere or cranial nerve but mental development is typically unimpaired. Cardiovascular, renal, and pulmonary anomalies may be present. Development of a cutaneous squamous cell carcinoma has been reported.
This syndrome is characterized by the presence of a nevus sebaceous following the lines of Blaschko in addition to a speckled lentiginous nevus (nevus spilus) typically in a segmental distribution with a checkerboard pattern. Extracutaneous manifestations are typically but not invariably present. They comprise predominantly skeletal, neurological, and ocular abnormalities and the most consistent extracutaneous finding is hemiatrophy. Neurological findings include hyperpathia, dysesthesia, hyperhidrosis, seizures, deafness, ptosis, strabismus, and mild mental retardation. Other associations include hypophosphatemic vitamin D-resistant rickets, hemihypertrophy, linear connective tissue nevus, juvenile onset hypertension, aortic stenosis, scoliosis, dermoid cysts, nephroblastoma, pheochromocytoma, and rhabdomyosarcoma. A melanoma arising in a nevus spilus has been documented and the organoid nevus may be complicated by the development of multiple basal cell carcinomas. This syndrome is also a mosaic RASpathy.
Inflammatory linear verrucous epidermal nevus (ILVEN) syndrome shows a linear verucous nevus with a distinct inflammatory characteristics usually described as eczematous or psoriasiform. Some have likened it to the rare linear form of psoriasis in presentation. While some have suggested that an ILVEN syndrome exists with various additional malformations, others do not consider this to be a well-defined association. A single case of ILVEN was associated with a GJA1 mutation, encoding a gap junction protein, though this is probably best considered as a postzygotic and mosaic form of erythrokeratoderma variabilis et progressiva which is normally autosomal dominant. There is an entire family of autosomal dominant and recessive syndromes with mutations in GJA1 and other gap junction and connexin encoding genes. It has also been suggested that ILVEN is a primary inflammatory condition rather than an epidermal nevus. It also shares features with the lesions seen in CHILD syndrome.
This mosaic RASopathy shows epidermal nevi with a profound hypophosphatemia that is not present at birth, but has a later onset and leads to osteomalacia. Other skeletal defects can also be seen and are not usually correlated with overlying epidermal nevi.
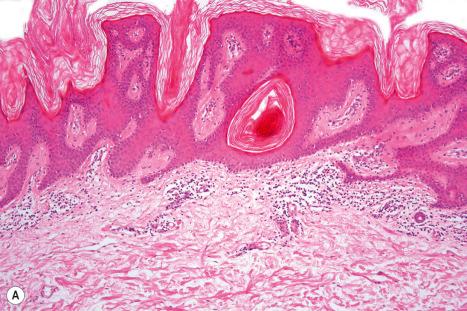
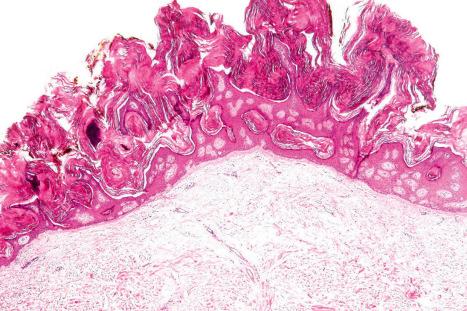
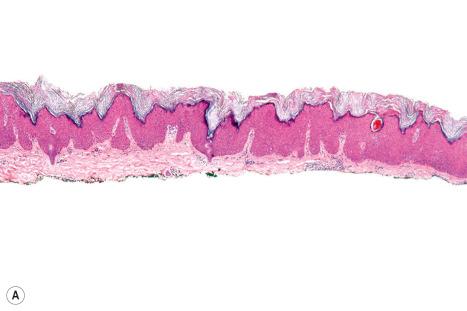
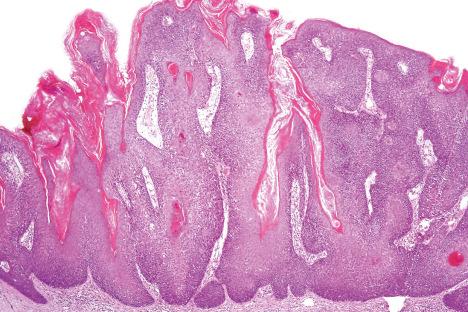
Epidermal nevi represent developmental abnormalities limited to proliferation of the epidermis, sometimes accompanied by anomalous terminal differentiation. Although they are related to sebaceous (organoid) nevi and frequently coexist, it is convenient to consider them separately. Commonly, they show the features of a sharply demarcated simple squamous cell papilloma ( Fig. 24.4 ). They, therefore, manifest hyperkeratosis, papillomatosis, acanthosis, and elongation of the rete ridges ( Fig. 24.5 ). The histologic features are often subtle and occasionally resemble acanthosis nigricans or a seborrheic keratosis. Rarely, the lesions show focal acantholytic dyskeratosis, acrokeratosis verruciformis-like features, cornoid lamellae formation, epidermolytic hyperkeratosis, an associated lichenoid tissue reaction or cutaneous horn formation. Acantholytic dyskeratosis in epidermal nevi is thought by some authors to represent zosteriform Darier disease. The presence of epidermolytic hyperkeratosis may be indicative of mosaicism for bullous ichthyosiform erythroderma as further supported by the identification of keratin 1 and 10 mutations.
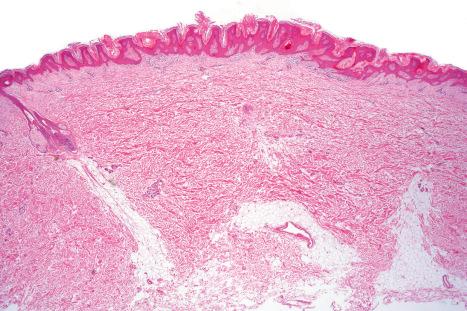
Epidermal nevi in Proteus syndrome are characterized by hyperorthokeratosis, acanthosis and papillomatosis in the absence of adnexal hyperplasia or epidermolytic hyperkeratosis.
The CHILD nevus is characterized histologically by marked acanthosis with overlying parakeratosis admixed with areas of hyperorthokeratosis. Intraepidermal neutrophils, also forming aggregates similar to Munro abscesses, are sometimes present. The dermis shows a lymphohistiocytic infiltrate. Dermal papillae may be filled with foamy histiocytes reminiscent of verruciform xanthoma.
ILVEN show epidermal psoriasiform hyperplasia with hyperkeratosis, parakeratosis and sometimes Muro abscesses. A prominent mixed perivascular dermal inflammatory infiltrate is present associated with dilated capillaries. There is considerable overlap with the lesions of CHILD syndrome, but ILVEN lacks the NSDHL mutations and X-linked dominant inheritance of CHILD syndrome.
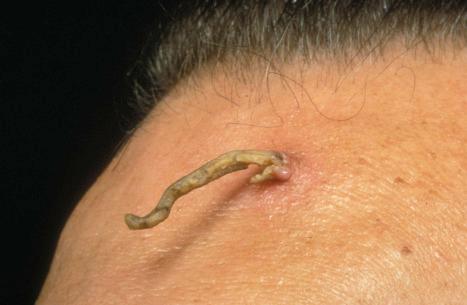
Cornu cutaneum (cutaneous horn) is a clinical diagnosis based upon the presence of a large protuberant mass of keratin ( Fig. 24.6 ). They can occur at virtually any body site, but are typical on the sun-exposed areas of the face and head, and can also involve other upper torso and extremity sites. It may complicate a variety of conditions and accurate diagnosis depends upon histologic examination of tissue from the base of the lesion. Cutaneous horns may complicate solar keratosis, viral wart, seborrheic keratosis, squamous cell carcinoma, keratoacanthoma, lichenoid keratosis, and basal cell carcinoma. It has been noted that these horns are considerably more likely to arise from benign or premalignant lesions (more than 80%) rather than invasive malignancies (less than 20%).
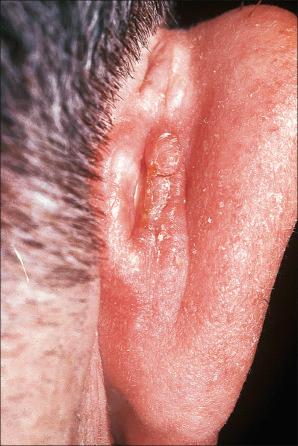
Acanthoma fissuratum (spectacle frame acanthoma) is a benign epidermal ‘tumor’ which develops as a result of chronic irritation from spectacles. It presents as an erythematous or flesh-colored, sometimes tender, nodule situated on the bridge of the nose or behind the ears ( Fig. 24.7 ). Typically, the center of the lesion shows a linear groove. The importance of this entity is that it is clinically frequently misdiagnosed as a basal cell or squamous cell carcinoma. An analogous lesion termed granuloma (epulis) fissuratum has been described in the mouth as a result of poorly fitting dentures. An exceptional case involved the penis with tight fitting undergarments. What is described as “vulvar granuloma fissuratum” is a fissuring process that complicates a variety of vulvar dermatoses with dyspareunia and other discomforts. This seems to represent a different lesion altogether.
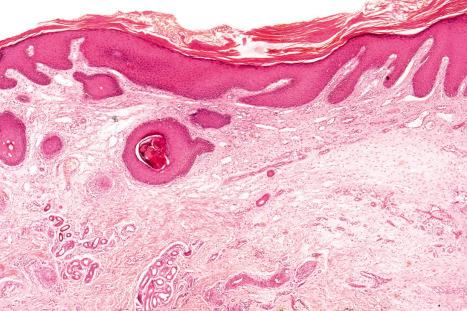
The histopathology is not specific, diagnosis being dependent upon knowledge of the clinical history. Its features usually include acanthosis (sometimes amounting to pseudoepitheliomatous hyperplasia) with hyperkeratosis and patchy parakeratosis, particularly at the edges of the fissure ( Fig. 24.8 ). The underlying dermis is edematous, fibrosed, and hyalinized. A chronic inflammatory cell infiltrate of variable severity is commonly present.
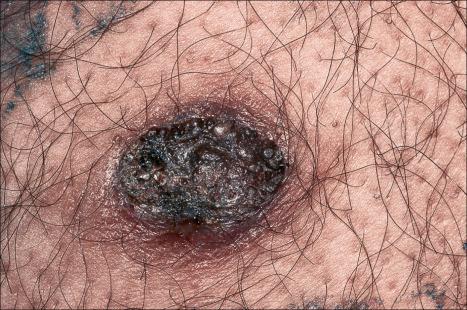
Seborrheic keratoses are very common lesions, developing in the middle aged and elderly. They are frequently numerous and appear as sharply delineated, round or oval, flesh-colored or brown-black warty plaques with a rather greasy texture ( Figs 24.9 and 24.10 ). Sometimes they are dome-shaped with a smooth surface and occasionally they may show an inflammatory halo or eczema-like features (Meyerson phenomenon). Although they may be found anywhere on the body (except for the palms and soles), they are particularly common on the face, chest, and back. The conjunctiva may also be involved.
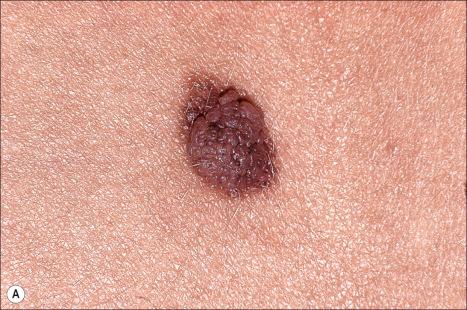
Other unusual clinical presentations include distribution along skin cleavages, involvement of the areola or the back of elderly patients (raindrop seborrheic keratosis), as well as a distribution along the lines of Blaschko. Occasionally, deeply pigmented or traumatized lesions are mistaken clinically for melanoma. The irritated seborrheic keratosis (inverted follicular keratosis) presents as a small warty papulonodule ( Fig. 24.11 ). It commonly affects middle-aged or elderly males and shows a predilection for the face. Multiple inverted follicular keratoses have been reported as a presenting sign in a patient with Cowden syndrome.
Sudden onset of numerous seborrheic keratoses (Leser-Trélat sign) has been reported in association with internal malignancy, most commonly adenocarcinoma of the stomach. Other tumors which may be present include lymphoma (particularly mucosis fungoides and Sézary syndrome), leukemia, metastatic melanoma, malignant solitary fibrous tumor, bronchial and breast carcinoma, cholangiocarcinoma, carcinoma of the ampulla of Vater, the pancreas and the esophagus, adenocarcinoma of the rectum, renal cell carcinoma, endometrial adenocarcinoma, transitional cell carcinoma, and anaplastic ependymoma ( Fig. 24.12 ). Leser-Trélat sign has also been described after treatment with chemotherapy, as well as in association with a benign Leydig cell tumor. The relationship of seborrheic keratosis and malignancy, however, has been questioned. Although neoplasia and seborrheic warts are both common in the elderly, we believe that a sudden eruption of the latter should still warrant careful investigation. Spontaneous regression of multiple seborrheic keratoses has also been reported in association with malignancy. Multiple eruptive seborrheic keratoses have been observed in a background of erythroderma, at a postoperative site, and with leprosy. Eruptive seborrheic keratosis has been reported with the use of the hepatitis C virus protease inhibitor telaprevir and also rarely with adalimumab anti-tumor necrosis factor (TNF)-α therapy for rheumatoid arthritis. In some cases, no underlying cause is found despite exhaustive clinical investigation.
Disappearance or fading of pigmented seborrheic keratoses has been reported with use of immune checkpoint inhibitor therapy (PD-1 inhibitor) for metastatic melanoma.
This benign epidermal tumor is definitely monoclonal in nature and represents a true neoplasm rather than epidermal hyperplasia. It has become clear that a subset of seborrheic harbor activating mutations oncogenes. The first noted was FGFR3 (usually R284C or S249C). The rates of FGFR3 mutations in patients with multiple to many seborrheic keratosis ranges from about 25% of lesions to almost 90%. Multiple oncogenic mutations were seen in different lesions from the same patients. These few patients had many seborrheic keratoses occurring in the genetic background of the rare anaphoric dysplasia and severe achondroplasia with developmental delay and acanthosis nigricans syndrome. There is increased incidence of these mutations with older patient age and location in head and neck region. Activating PIK3CA somatic mutations have also been noted (usually E542K or E454K). In a small subset of cases, both PIK3CA and FGFR3 mutations are encountered simultaneously. Either FGFR3 or PIK3CA mutation has been seen limited to the lesions in the setting of familial seborrheic keratoses. Interestingly, studies of human skin explants into mice indicate that FGFR3 is insufficient to drive seborrheic keratosis tumor formation in that model and other data suggest that FGFR3 signaling in keratinocytes provides more of a senescence than oncogenic impetus. Other model systems indicate FGFR3 mutation is associated with increased proliferation and reduced apoptosis in keratinocytes with little effect on senescence. Examining broader panels of genes have reviewed rare mutations in additional oncogenes including KRAS , HRAS , EGFR and AKT1 . Mutational signatures suggest ultraviolet (UV) exposure and very recently TERT and DPH3 promoter mutations have been noted in older patients in lesions from the head and neck region. More work is needed to understand how these various drivers work in these neoplasms that so rarely progress to malignancy.
Seborrheic keratosis is characterized by proliferation of basaloid cells with a variable degree of squamoid differentiation. There is a range of histopathological patterns, including: hyperkeratotic (papillomatous), adenoid or reticulated variants, acanthotic or solid keratosis, clonal or nested, inflamed, and irritated seborrheic keratosis (inverted follicular keratosis).
The keratotic (papillomatous) variant has a verrucous appearance with variable proliferation of basaloid and squamoid cells ( Fig. 24.13 ). The lesion shows acanthosis, papillomatosis, and hyperkeratosis, often with the development of pseudohorn cysts ( Fig. 24.14 ).
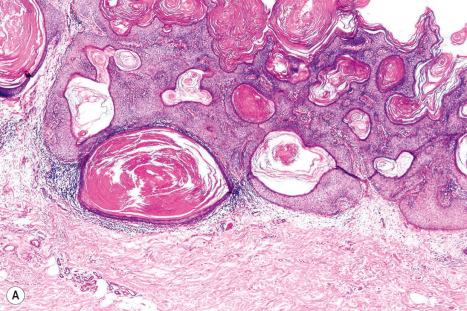
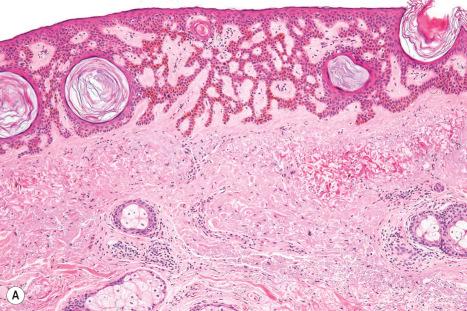
In the adenoid type of seborrheic keratosis, the lesion is typified by thin proliferating strands of basaloid cells arising from the epidermis ( Fig. 24.15 ). These lesions may be highly pigmented and pseudohorn cysts are less often evident.
In the acanthotic variant, the surface of the tumor is hyperkeratotic, rounded, and smooth ( Figs 24.16 and 24.17 ). Melanocytic proliferation is not uncommon. When marked, the designation melanoacanthoma is sometimes applied ( Fig. 24.18 ). Pigmentation in seborrheic keratosis has been linked to increased expression of keratinocyte-derived endothelin 1 mediated by TNF-alpha and endothelin-converting enzyme 1 alpha (ECE1 alpha).
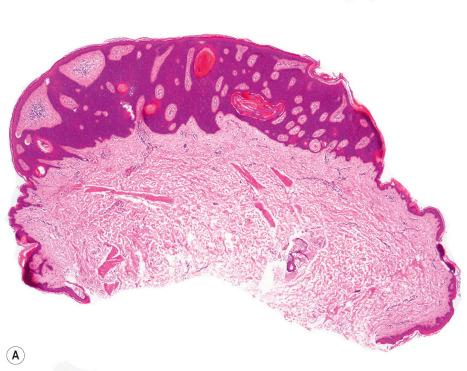
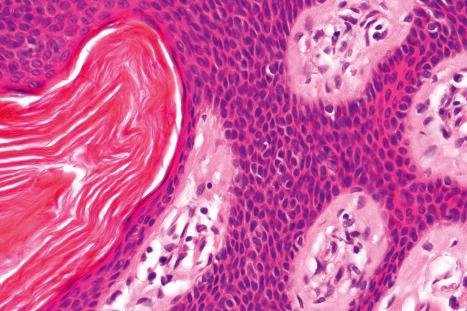
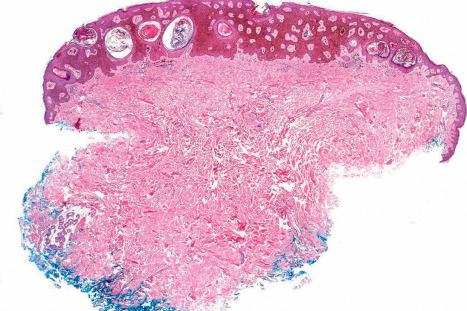
Many seborrheic keratoses show a mixture of the patterns described above. Occasionally, intraepithelial nesting gives rise to the Borst-Jadassohn appearance (so-called clonal seborrheic keratosis) and some variants barely protrude above the adjacent epidermis (flat seborrheic keratosis) ( Figs 24.19–24.21 ). Rare patterns include the adamantinoid variant characterized by intercellular mucin and pseudorosette formation due to a radial arrangement of basal keratinocytes around central small empty spaces. Bowenoid seborrheic keratosis has a predilection for sun-exposed areas, has intraepidermal atypia, and is seen in only about 1% of excised cases. Some have reported an association with human papillomavirus (HPV) with Bowenoid transformation. The presence of numerous basal cells with abundant clear cytoplasm is a rare finding and may lead to an erroneous diagnosis of melanoma in situ within a seborrheic keratosis on H&E-stained sections. By immunohistochemistry, these basal clear cells are, however, positive for cytokeratins and negative for markers of melanocytic differentiation, confirming their epithelial nature. The etiology of marked clear cell change is unclear but appears unrelated to glycogen deposition. A desmoplastic variant is characterized by nests and strands of bland-appearing basaloid epithelium within a dense desmoplastic stromal response. Analogous to desmoplastic trichilemmoma, the tumor shows an exophytic growth pattern, is well-demarcated, and lacks cytological atypia. Stromal amyloid deposition may occasionally be evident, and an accumulation of xanthomatized histiocytes within dermal papillae reminiscent of verruciform xanthoma has been reported.
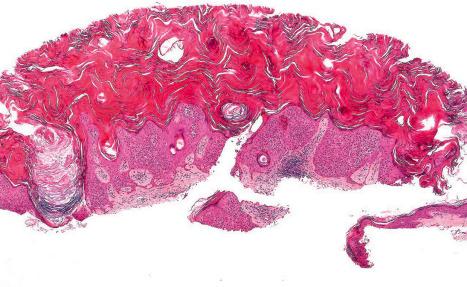
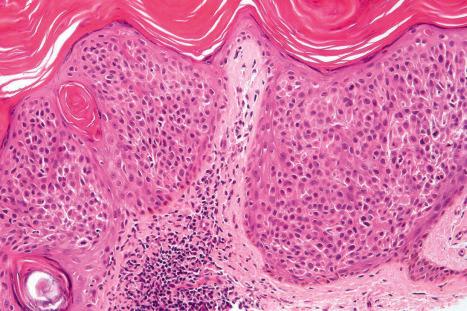
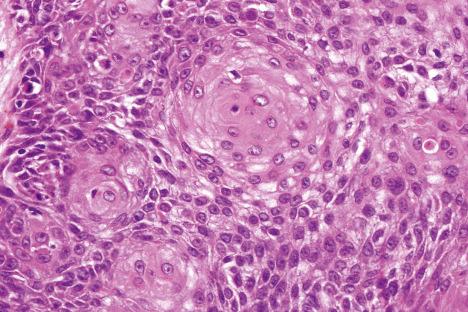
Seborrheic keratosis is sometimes characterized by an intradermal or ‘inverted’ type of proliferation known as inverted follicular keratosis ( Fig. 24.22 ). In this variant, characteristic whorls of maturing squamous epithelium (squamous eddies) are particularly evident ( Figs 24.23 and 24.24 ). These tumors are usually seen arising close to a hair follicle ostium and squamous eddies have been shown to be related to follicular units. Mitotic figures are sometimes conspicuous, but are invariably normal. Some of the lesions contain large numbers of horn cysts and are frequently accompanied by an intense chronic inflammatory cell infiltrate, hence its alternative designation, ‘irritated seborrheic keratosis.’ Conspicuous apoptosis is sometimes present in areas of squamous differentiation.
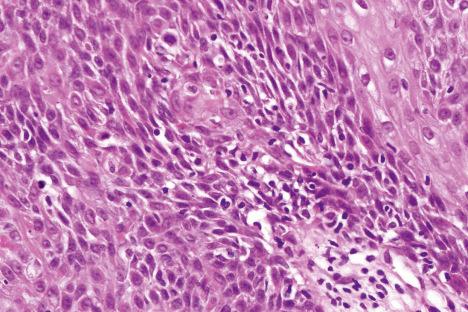
Acantholysis is not uncommon in seborrheic keratoses, particularly in the ‘irritated’ variant.
Malignant change within a seborrheic keratosis is very rare, but has occasionally been documented. Usually this represents an in situ change, but basal cell carcinoma and squamous cell carcinoma have also been reported. Both elevated UV exposure and immunosuppression can play a role in malignant transformation. More frequently (in up to 5% of tumors) other neoplasms arise in association with seborrheic keratoses, sometimes referred to as collision tumors. The most frequent association is with superficial basal cell carcinoma but squamous cell carcinoma and melanoma have also been reported. Unusual combined tumors that have very occasionally been documented include cutaneous ganglioneuroma, melanocytic nevi, sebaceoma, eccrine poroma, and trichilemmoma in addition to adenocarcinoma.
In contrast to nongenital lesions, seborrheic keratoses arising on genital skin are frequently (in approximately 70%) related to HPV. These HPV-positive lesions are probably better regarded as condyloma acuminatum rather than true seborrheic keratoses.
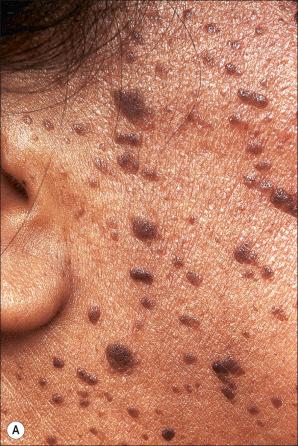
Dermatosis papulosa nigra is an extremely common condition in which adults of Afro-Caribbean origin develop multiple, small, darkly pigmented papules, predominantly on the face, particularly the cheek. The neck, chest, and upper back may also be involved. There is a female preponderance of 2 : 1, and a family predisposition has been identified in the majority of patients. Very rarely, children may be affected and exceptionally the disorder presents in the white races. An eruptive presentation has been reported in a patient with a colonic adenocarcinoma analogous to eruptive seborrheic keratoses associated with internal malignancy (Leser-Trélat sign).
The lesions are indistinguishable from seborrheic keratoses ( Fig. 24.25 ). Like seborrheic keratoses, activating mutations in both FGFR3 and PIK3CA have been documented. There is hyperkeratosis, acanthosis with a reticulated pattern, and ‘horn cyst’ formation. The epithelium shows abundant melanin pigmentation. A chronic inflammatory cell infiltrate may be present in the superficial dermis.
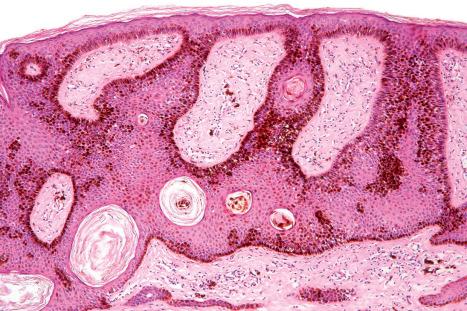
Actinic lentigines (also known as lentigo senilis, solar lentigo, senile freckle, senile lentigo, liver spot) are benign, irregular, macular lesions that commonly develop on sun-damaged skin of the middle aged and elderly people, and are therefore most numerous on the face and dorsal aspects of hands and forearms ( Figs 24.26A and 24.26B ). Both acute and chronic sun exposure have been implicated in their pathogenesis. An increased incidence in the setting of type 2 diabetes has recently been noted. It has been proposed that actinic lentigines, especially those that are large, irregularly sized, and located on the upper back and shoulders, serve as a clinical marker of past severe sunburn.
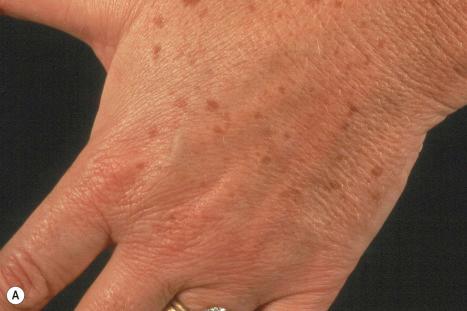
Actinic lentigines measure 0.1–1.0 cm or more in diameter, have a tendency to coalesce, and vary from light to dark brown. Caucasians are particularly affected. The lesions may be clinically mistaken for lentigo maligna.
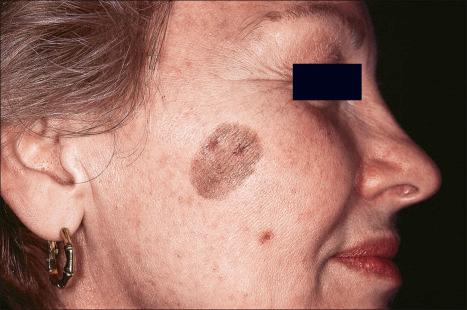
Unstable solar lentigo is a variant of solar lentigo, often presenting as a solitary irregularly pigmented macule and is usually darker and larger than classical solar lentigines. It has been hypothesized that unstable solar lentigo could be a precursor lesion to lentigo maligna.
Actinic lentigo usually develops against a background of solar elastosis. There may be slight hyperkeratosis. The epidermis shows extension of the rete ridges to form budlike processes expanding into the papillary dermis (see Fig. 24.26C ). The inter-ridge epithelium is often atrophic. The melanocytes may be normal or slightly increased in number, but appear to be functionally hyperactive because there is a marked increase in the amount of melanin production (see Fig. 24.26D ). A pivotal role for fibroblast-derived growth factors in regulating hyperpigmentation has recently been suggested. Mild nuclear hyperchromatism and nuclear irregularity are sometimes seen as a reflection of the chronic actinic exposure. Similar changes may be evident in apparently normal skin from sun-exposed sites. Vacuolar degeneration of basal keratinocytes has also been reported to be a fairly consistent histologic abnormality. Unstable solar lentigo is characterized by melanocytic hyperplasia not extending beyond the confines of the lesion. Although melanocytes may be somewhat larger, they nevertheless lack nuclear atypia and hyperchromasia.
In some examples, epidermal proliferation may lead to a reticular pattern due to the formation of anastomoses between adjacent attenuated ridges. Occasionally, formation of small horn cysts can result in histologic overlap with seborrheic keratosis. Interestingly, similar genetic alterations, namely activating mutations in both FGFR3 and PIK3CA pathways, have been demonstrated in both actinic lentigo and seborrheic keratosis, suggesting a possible relationship at the molecular level. Altered fibroblasts in the underlying dermis may also trigger changes in keratinocytes. Local cytokine and keratinocyte functional dysregulation likely also contribute. Gene expression studies support the primary keratinocytic nature of these lesions. Genome-wide association studies suggest a role for the immunoregulatory pathways as well as melanocytic pigmentation function as predisposition factors. Actinic lentigo is increasingly viewed primarily as a keratinocytic lesion and it is therefore included in this chapter.
Actinic lentigo is sometimes associated with a slight increase in collagen within the papillary dermis. Pigmentary incontinence is often evident and a slight chronic inflammatory cell infiltrate is usually seen in the adjacent dermis. Dermal melanophages are also often seen. A study demonstrated significant increase in dermal vessel density. Some (but not all) authors believe that actinic lentigo may evolve into large cell acanthoma (see tumors of the surface epithelium) or that the latter represents a variant of solar lentigo with cellular hypertrophy.
Ultrastructurally, the melanocytes contain increased numbers of morphologically normal melanosomes.
Large cell acanthoma presents as a discrete scaly papule or plaque up to 1 cm or more in diameter and is most commonly found on the head, arms, trunk, and lower limbs in decreasing order of frequency ( Fig. 24.27 ). Conjunctival involvement is rarely described. Lesions, which are sharply demarcated, are often single, but multiple acanthomas have occasionally been documented. The papules are commonly hyperpigmented or flesh colored, although achromic lesions have also been described. The sex incidence is equal and patients are usually elderly. Large cell acanthoma does not therefore have distinctive clinical features, most examples being submitted as seborrheic keratoses, actinic keratoses or actinic lentigines.
The precise nature of this curious lesion is unknown. It has been variably described as a distinct entity, a variant of actinic keratosis or Bowen disease, a form of stucco keratosis, or a subtype of solar lentigo; we favor the latter interpretation. The recent finding of aneuploidy in this clinically benign acanthoma suggests that it merits separate classification. HPV type 6 has been identified from lesional skin in one patient with multiple disseminated large cell acanthomata. Characterization for FGFR3 or PIK3CA mutations as seen in some seborrheic keratoses is of interest, but not yet reported.
Histologically, large cell acanthoma is composed of keratinocytes measuring about twice normal size ( Fig. 24.28 ). Hyperkeratosis is usual and not associated with parakeratosis and the acanthotic epithelium shows bulbous epidermal ridges. Keratinocytes contain enlarged and rounded nuclei and the cytoplasm is abundant. Cytological atypia is not a feature and mitotic activity is limited to basal keratinocytes. Lesions may be hyperpigmented, normally pigmented, or achromic. Verrucous variants reminiscent of stucco keratoses have also been described. Some large cell acanthomas can recede in the form of benign lichenoid keratoses.
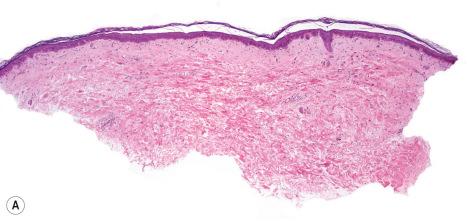
When pigmented, large cell acanthoma may be confused with actinic lentigo. However, actinic lentigo is composed of small basaloid cells aggregated within narrow, elongated epidermal ridges.
Stucco keratoses are warty lesions found on the extremities of elderly people and are more common in males than in females. They are small (1–2 mm), sharply defined, round or oval verrucous papules of gray or brown coloration, commonly located around the foot, ankle, and dorsum of the hand ( Fig. 24.29 ). The extensor surface of the forearm is also often affected. The lesions are typically numerous, often in excess of 100. The papules appear stuck to the underlying skin but can be easily scratched off, leaving an intact undersurface with a scaly collarette. Xerosis is often present and patients may also show scattered seborrheic keratoses. An eruptive case associated with esophageal cancer has been reported.
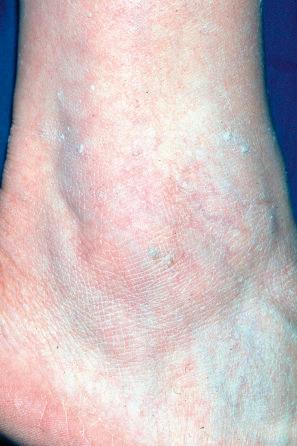
Ultrastructural studies have shown normal epidermal differentiation without evidence of intracellular viral particles. Two patients with disseminated eruptive lesions demonstrated HPV DNA. Activating mutations in FGFR3 and PIK3CA have been documented, suggesting a pathogenetic relationship with seborrheic keratosis.
The lesions are typified by dense orthokeratosis and ‘peaked’ or church-spire acanthosis ( Fig. 24.30 ). Basaloid cell proliferation and horn cyst formation as seen in seborrheic keratosis are characteristically absent. There are no significant inflammatory changes.
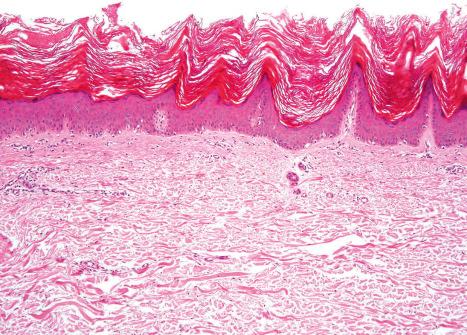
The histology of stucco keratosis is indistinguishable from acrokeratosis verruciformis. In contrast to the latter condition, stucco keratoses are not associated with Darier disease.
The Borst-Jadassohn epithelioma refers to a histopathological appearance rather than a precise clinicopathological entity. It had initially been regarded as a distinctive clinicopathological entity. The histologic findings, however, are seen in a number of lesions of different etiology such as Bowen disease, actinic keratosis, hidroacanthoma simplex, and seborrheic keratosis; it is therefore preferable to regard this as a histologic pattern rather than a distinct entity. Histologically, it is characterized by nests of neoplastic cells situated within and surrounded by normal keratinocytes ( Fig. 24.31 ).
Porokeratoma is an entity characterized by histologic features of porokeratosis presenting as a solitary lesion. It shows a marked male predominance and affects adults with a mean age of 57 years. One case showed an association with HPV type 16. The clinical presentation is of a hyperkeratotic plaque or nodule that may appear verrucous. A wide range of anatomic sites is affected but there is a predilection for distal extremities. There is no underlying or associated porokeratosis and behavior is benign.
Histologically, porokeratoma is well circumscribed and characterized by marked epidermal hyperplasia and papillomatosis showing prominent distinct or broad and confluent cornoid lamella formation with dyskeratosis and loss of the granular cell layer. There is an abrupt transition with areas of adjacent hyperorthokeratosis. The dermis shows a non-specific chronic inflammatory infiltrate and mild vascular dilatation.
Psoriasiform keratosis typically presents as solitary and occasionally multiple erythematous scaly papules or plaques measuring between 0.5 and 3 cm. The anatomic distribution is wide and there is a predilection for the extremities. Adults are affected, with a mean age at presentation of 66 years. The gender distribution is roughly equal and there is no history of psoriasis. Behavior is benign. HPV type 6 was identified in a single case.
The histologic findings are at least somewhat reminiscent of psoriasis. There is sharp lesional circumscription and marked irregular, verrucous epidermal acanthosis with overlying hyperparakeratosis. Focal to confluent mounds of parakeratosis contain collections of neutrophils and there is an absence or diminution of the granular cell layer in these areas. Prominent and dilated vessels are present within the papillary dermis, accompanied by a chronic inflammatory infiltrate predominantly containing lymphocytes. A fungal etiology is excluded by PAS staining.
This solitary keratosis presents in adulthood with a median age of 59 years. Trunk and extremities are mainly affected and, based on the limited information available, there is a slight female bias.
The histologic hallmark is the presence of keratinocytes showing conspicuous granular parakeratosis as observed in granular parakeratosis. The lesion is otherwise circumscribed, with an endophytic growth pattern reminiscent of the adenoid pattern in seborrheic keratosis showing infundibular pseudocyst formation. There is a florid accompanying chronic inflammatory infiltrate within the superficial dermis and lichenoid features may be present. Eosinophils and histiocytes are admixed.
Clear cell acanthoma (of Degos) is an uncommon, usually solitary, tumor occurring in the middle aged or elderly but which may rarely present in younger patients. Occasional multiple or disseminated eruptive variants have been described. It is most commonly found on the lower limbs and presents as a circumscribed pink to bright red or brown oval-shaped papule or nodule measuring 1–4 cm in diameter ( Fig. 24.32 ). Rarely, lesions have been described at other sites including the face, forearm, hand, finger, trunk, inguinal region, scrotum, buttocks, hallux, and nipple.
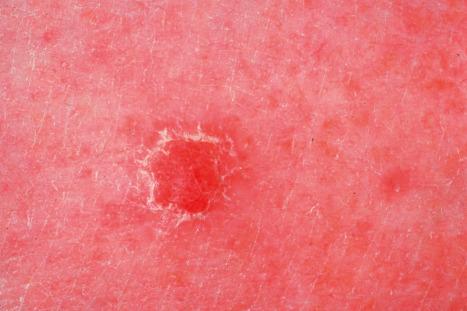
Occasionally, clear cell acanthoma presents as a polypoid lesion and large variants measuring up to 6 cm have been reported. Rare pigmented variants are also recognized. It often shows a collarette of scale, and erythematous puncta that bleed with minor trauma are commonly present on the surface. Clinically, it may resemble a lobular capillary hemangioma (pyogenic granuloma) or an eccrine poroma. Individual case reports describe clear cell acanthoma arising within an epidermal nevus, in association with a melanocytic nevus, in a split-thickness skin graft and within a psoriatic plaque. Multiple lesions have been reported in association with ichthyosis. A case of Cowden syndrome associated with multiple clear cell acanthomas has been reported.
The precise nature of the clear cell acanthoma is unknown. Although variably regarded as an inflammatory epithelial hyperplasia, a hamartoma, or a variant of a seborrheic keratosis, most authors believe it to be a benign neoplasm, although the cell of origin is subject to dispute. Derivation from epidermal, sebaceous, and sweat gland epithelium have all been proposed. The high glycogen content coupled with keratin and involucrin positivity and carcinoembryonic antigen (CEA) negativity has led some authors to suggest an origin from the follicular outer root sheath. However, considering the characteristic follicular sparing this seems an unlikely hypothesis. The presence of striking epithelial membrane antigen (EMA) expression could suggest an eccrine acrosyringeal derivation. However, immunohistochemical studies on cytokeratin, involucrin, and filaggrin expression support an epidermal derivation and raise the possibility that clear cell acanthoma could represent an inflammatory dermatosis rather than a true neoplasm. This hypothesis is further supported by studies suggesting that, similar to psoriasis, keratinocyte growth factor (KGF) upregulation may be responsible for keratinocyte hyperproliferation in clear cell acanthoma.
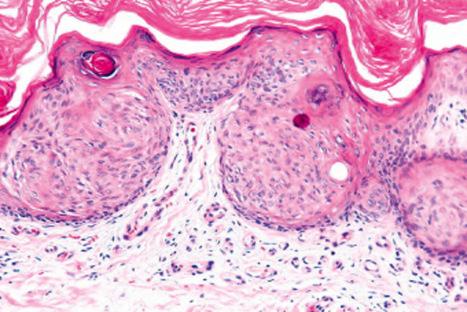
Clear cell acanthoma is composed of markedly acanthotic (often psoriasiform) epithelium, which has a characteristically clearly demarcated lateral border ( Fig. 24.33 ). The epidermal ridges are commonly fused. Individual cells have clear cytoplasm due to the presence of abundant glycogen, best demonstrated with a periodic acid-Schiff (PAS) reaction ( Fig. 24.34 ). Variably pigmented, dendritic melanocytes are sometimes present, both along the basal epithelial layer and also intermingled with keratinocytes in the upper layers of the lesion. This latter feature appears to be more common in patients of Mediterranean ancestry. In cases where pigmentation is clinically apparent, the confusing term clear cell melanoacanthoma (cf. seborrheic keratosis) or pigmented clear cell acanthoma has sometimes been applied. Typically, the intraepidermal portions of the adnexae are spared. Intralesional neutrophils are characteristic and are often evident within an overlying parakeratotic scale. The underlying dermal papillae commonly contain dilated capillaries, and an inflammatory cell infiltrate with a predominance of neutrophils is often present. These latter features show considerable overlap with psoriasis.
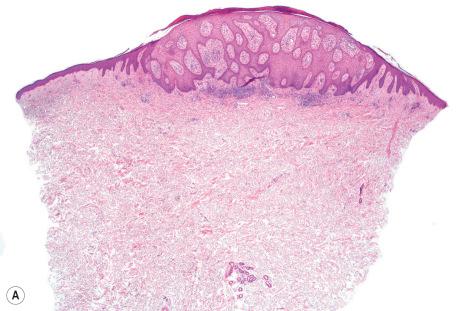
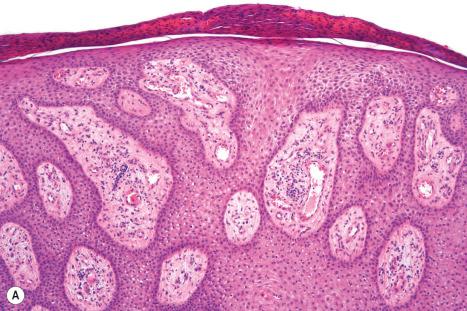
Rarely, so-called atypical or malignant clear cell acanthoma has been documented in which cellular pleomorphism and mitotic activities are features. Whether, in reality, this represents a true variant is uncertain.
Pseudoepitheliomatous (pseudocarcinomatous) hyperplasia represents an extreme degree of acanthosis, which histologically mimics squamous cell carcinoma. It may be seen in association with:
chronic venous stasis,
ulceration,
chronic inflammatory conditions, such as pyoderma gangrenosum, lupus vulgaris, syphilis and fungal infections (e.g., blastomycosis), hypertrophic lichen planus, insect bite granuloma and bromoderma.
CD30 positive lymphoproliferative disorders and more rarely in reactive conditions rich in CD30 positive cells.
It is occasionally found in the epithelium overlying neoplasms such as granular cell tumor and fibrous histiocytoma.
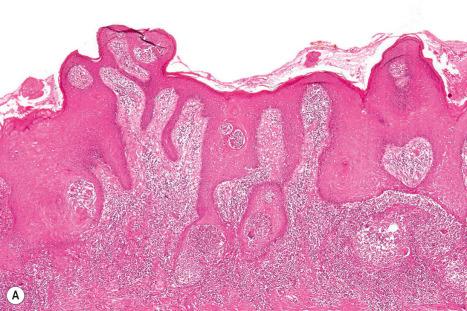
The histologic features of pseudoepitheliomatous hyperplasia vary from a marked degree of irregular acanthosis to changes highly suggestive of squamous cell carcinoma ( Fig. 24.35 ). In such instances, distinction from the latter can be very difficult. The diagnosis of this entity depends on awareness of the condition and on a careful survey of the surrounding dermis to find a predisposing lesion.
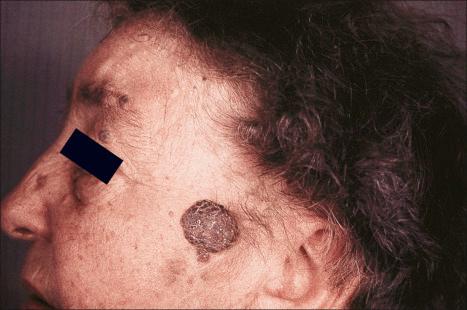
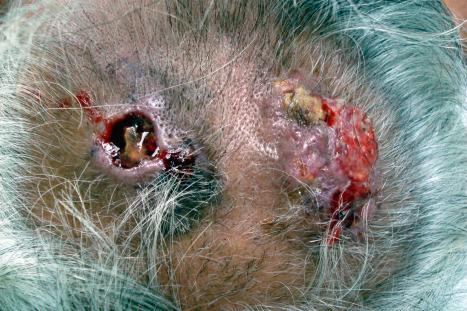
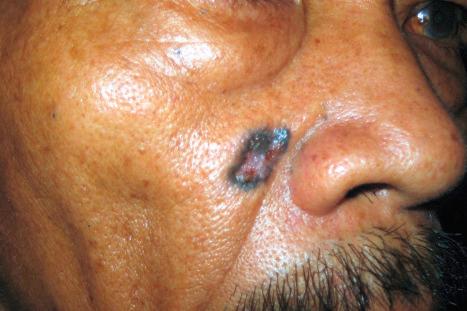
Nonmelanoma skin cancer – consisting predominantly of basal cell carcinoma (BCC) and squamous cell carcinoma (SCC) – is the most prevalent cutaneous malignant neoplasm in the United States with an estimated incidence broadly ranging from 600,000 to 2,800,000 persons affected per year. However, since basal cell carcinoma is not a reportable disease in the United States, reliable estimates are challenging to obtain and differ based on methodology. Basal cell carcinoma constitutes well over 70% of skin cancers and one-third of all cancers in the United States,and its incidence outnumbers melanoma by a factor of approximately 20-40. Thus while not as deadly as melanoma, it constitutes a huge public health concern and population screening remains a priority. Basal cell carcinoma (epithelioma) is the most common cutaneous malignant neoplasm, being four to five times more frequent than squamous cell carcinoma, and the incidence appears to be rising at a rate of 3–10% annually. Accurate current data are not available, but the incidence of basal cell carcinoma in the United States in 1977–78 was approximately 180 per 100,000 of the population and estimated at 191 per 100,000 in 1990. Based on a study from 1994, the estimated incidence of basal cell carcinoma in the United States was as high as 407 per 100,000 for men and 212 per 100,000 for women. Estimated differently based on procedure data, the total burden of non-melanoma skin cancer in the United States is suggested to be as high 5.4 million cases and 3.3 million patients per year. There is marked regional variation in incidence. A slightly lower figure has been reported in Northern Europe in contrast to a drastically increased incidence in Australia. Basal cell carcinoma is slightly more common in men than in women and it is very rare in blacks. Basal cell carcinoma in the Oriental population is frequently pigmented (55–75% of BCC), while this phenomenon is much less prevalent in India (around 20%). The term carcinoma is preferred to epithelioma because, although these tumors metastasize exceptionally rarely, locally advanced cases are capable of gross tissue destruction, particularly those lesions arising on the head, which may erode the nose or orbital contents and even extend into the brain ( Fig. 24.36 ).
In less sunny climates, basal cell carcinoma represents a tumor of the elderly, commonly presenting in patients in their sixth decade or older. Exceptions to this include those with xeroderma pigmentosum, albinism, the nevoid basal cell carcinoma syndrome, and Bazex syndrome. In sunny climates, presentation may be at a much younger age, and even children without associated genetic disorders may be affected. Basal cell carcinoma presenting at an early age has been thought to behave more aggressively, a view that has recently been challenged. Tumors are often multiple; a recent study from Australia demonstrated that 46% of patients with an initial diagnosis of basal cell carcinoma suffered from more than one tumor over a 10-year period. Data from the United States are similar.
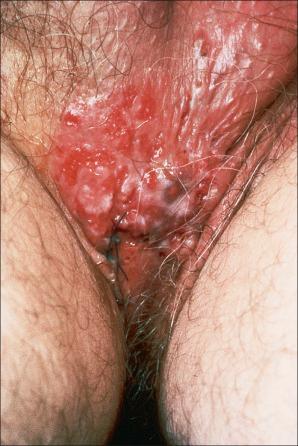
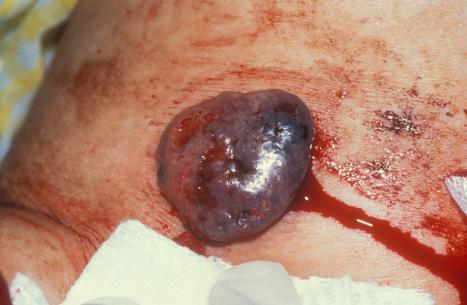
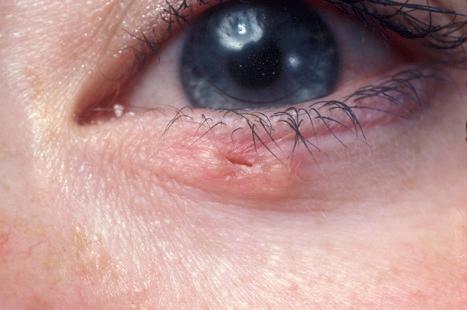
Although the face is most commonly involved, the tumors being particularly related to excessive sunlight, lesions are not usually seen on the dorsal aspects of the hands. Less often, basal cell carcinoma presents on the neck, trunk, and proximal extremities. Lesions affecting the lower leg are rare and have been suggested to ulcerate more frequently. Other unusual and rare locations include the vulva, penis, scrotum, perineum, buttock, nipple, areola, umbilicus, subungual region, soles, palms, axilla, conchal bowl, caruncle, lacrimal duct, and the oral mucosa. Lesions of the scrotum are of particular importance because of an associated high rate of metastasis (13%) ( Fig. 24.37 ). Occasionally, basal cell carcinoma may complicate venous stasis ulcers. These are particularly significant as they may mimic granulation tissue. The rolled margin, however, is the diagnostic clue. Basal cell carcinoma has also been reported to arise in scars of variable etiology, such as surgical, burn, and postvaccination, in addition to scars which have followed healed infectious diseases such as leishmania and chickenpox. An increased risk for the development of basal cell carcinoma has also been documented at the site of prior radiation therapy with potential for more aggressive behavior and higher local recurrence as well as distant metastasis rates. Basal cell carcinoma that has been described in association with nevus sebaceous and dermatofibroma are better regarded as variants of trichoblastoma.
Basal cell carcinoma may also arise in association with melanoma either in the form of a collision tumor or as a melanoma metastasis to a basal cell carcinoma. The intimate association of melanoma cells and basaloid epithelial proliferations has recently been reported as ‘basomelanocytic tumor’. Whether this truly represents a distinct entity rather than colonization of basal cell carcinoma by melanoma cells is a topic of current debate and awaits further study.
Basal cell carcinoma may also complicate other lesions such as dilated pore of Winer, port-wine stain, Marjolin ulcer, arteriovenous malformation, rhinophyma, pilonidal sinus, lupus vulgaris, multiple trichoepitheliomas, and hair and skin graft transplantation sites. Basal cell carcinoma may also show involvement by underlying systemic disorders such as chronic lymphocytic leukemia. An increased incidence of basal cell carcinoma has been reported in young females who smoke and use tanning beds and there appears to be a similar sex predilection for tumors arising on the upper lip.
It is convenient to divide basal cell carcinoma into five main clinical subtypes, which to some extent correlate with their general growth pattern and treatment. Nodular and morpheaform basal cell carcinomas are most frequently located in the head and neck area whereas those lesions on the trunk are predominantly of the superficial subtype.
nodular/ulcerative (45–60%),
diffuse (infiltrating and morpheaform) (4–17%),
superficial (15–35%),
pigmented (1–7%),
fibroepithelioma of Pinkus.
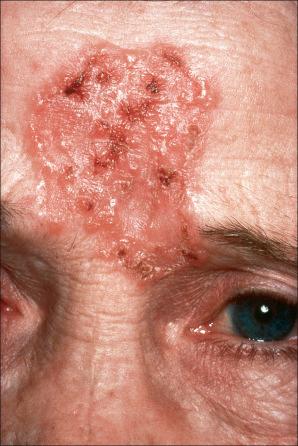
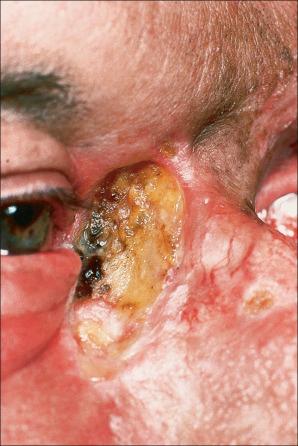
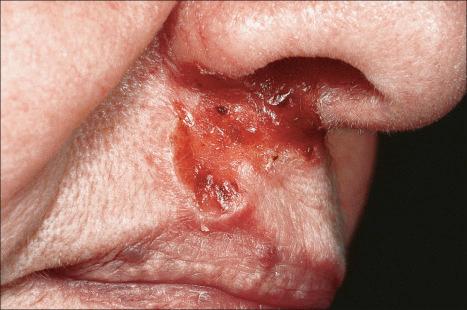
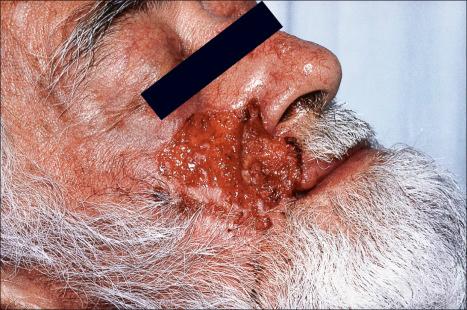
Ulcerative basal cell carcinoma (rodent ulcer) commences life as a small translucent papule, which may be yellow or pink or have a pearly appearance. The epidermis is thinned and is stretched over the surface of the tumor and often a few telangiectatic vessels are evident. As the lesion enlarges, central erosion or ulceration develops ( Figs 24.38–24.44 ). A history of an ulcer that never quite heals is characteristic. An established rodent ulcer is sharply demarcated and typically has a rolled margin.
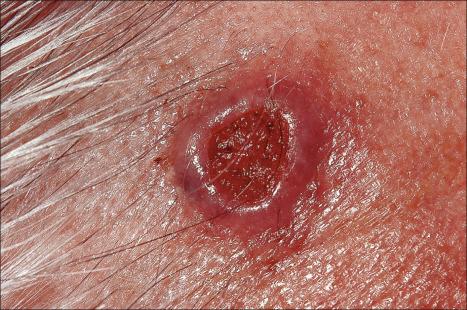
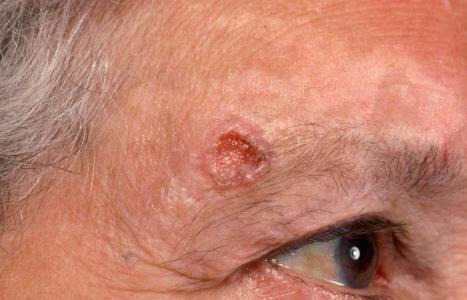
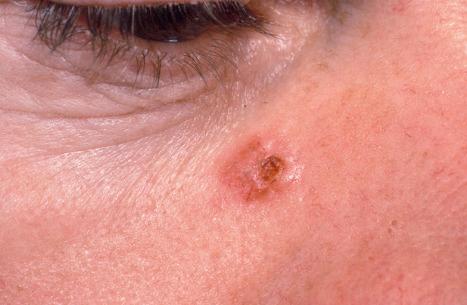
The nodulocystic variant is lobulated and usually does not ulcerate; it may therefore be mistaken for a simple cutaneous cyst. The tumor may grow quite large, measuring 2 cm or more in diameter, and presents as a smooth pearly nodule that is frequently associated with telangiectatic vessels ( Figs 24.45 and 24.46 ).
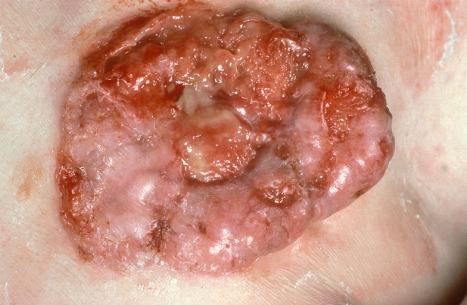
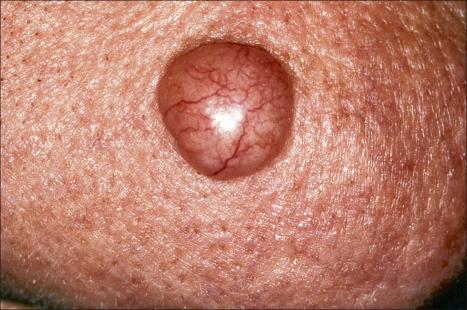
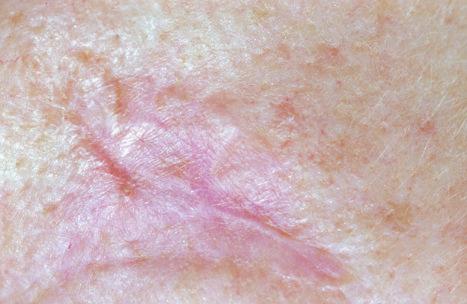
The diffuse type comprises several patterns, all of which are associated with a poorly demarcated clinical margin. The prototype is the morpheaform or sclerosing basal cell carcinoma. This is a flat, whitish-pink plaque, which feels indurated and tethered and slowly enlarges over the course of several years ( Fig. 24.47 ). In contrast to the noduloulcerative tumors, the morpheaform variant is not usually associated with obvious translucency. Sometimes, however, in examples where the fibrous component is less dense, some translucency may be present and is best highlighted by stretching the skin under a good light. Erosions, crusting, or ulceration are common, with the center of the lesion showing either a cicatrized or healed regressed area. Morpheaform basal cell carcinomas are notoriously difficult to treat, the pathological extent of the tumor often being greatly in excess of the clinical impression.
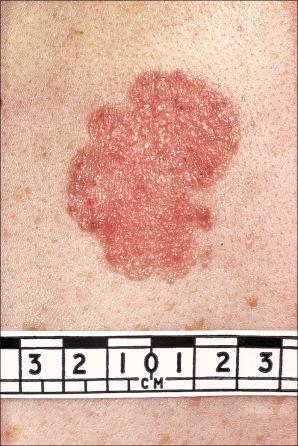
Superficial basal cell carcinoma presents mainly on the trunk as a slowly enlarging, scaly red patch that has usually been present for years ( Fig. 24.48 ). Lesions, particularly when multiple, may be clinically confused with psoriasis. The surface in the center of the lesion may occasionally be eroded, but more often it is intact. Careful examination sometimes reveals a delicate rolled thin translucent border that greatly facilitates establishing the diagnosis. Multiple superficial basal cell carcinomas are a known complication of arsenic ingestion (and also actinic keratosis and Bowen disease).
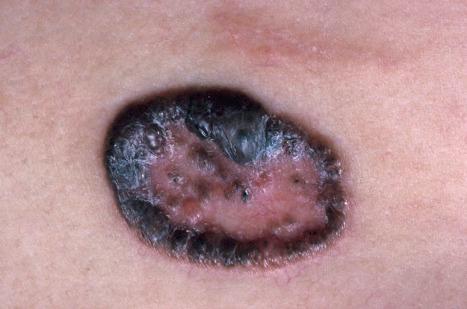
Both superficial and localized basal cell carcinomas may contain pigment, which is distributed patchily or evenly and may therefore cause clinical confusion with melanoma – pigmented basal cell carcinoma ( Figs 24.49–24.51 ).
Giant basal cell carcinoma, by definition measuring 10 cm or more in diameter, is preferentially found on the trunk ( Fig. 24.52 ). It is thought to be a high-grade variant with a high metastasis rate (30%) and significant mortality, although some studies do not detect any evidence of metastasis. It is usually associated with neglect. There is a high incidence of alcoholism as well as cigarette smoking.
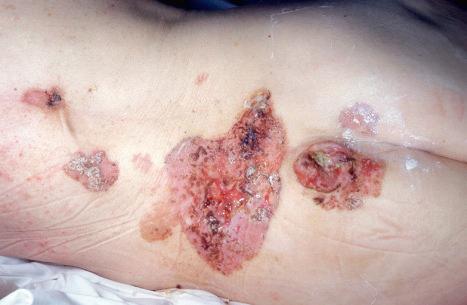
Other less frequent clinical presentations include linear as well as unilateral basal cell carcinoma, polypoid basal cell carcinoma, and pedunculated basal cell carcinoma.
Linear basal cell carcinoma presents predominantly on the neck, eyelid, and medial canthus in the elderly as an ill-defined linear lesion.
Polypoid basal cell carcinoma has been described recently and presents in the elderly as an exophytic, polypoid lesion connected by a stalk. The most prevalent sites are the scalp, ear, and genital area but only limited data are available. A patient with multiple infundibulocystic basal cell carcinomas in a unilateral distribution around the mouth and with indolent clinical behavior has also been reported.
The reported recurrence rates are very variable (1–8.7%) and depend upon the location, size, histologic subtype and form, and adequacy of primary therapy. Facial tumors, especially those around the nose, eye, lip, and ear, are most likely to recur, particularly when greater than 2 cm in diameter ( Fig. 24.53 ). Morpheaform, metatypical, and infiltrative variants have the highest recurrence rates. Superficial basal cell carcinoma is also associated with a high risk of recurrence due to difficulty in assessing the anatomical limits of the tumor. Patients with chronic lymphocytic leukemia appear to have a higher risk for local recurrence following Mohs surgery independent of other prognostic factors such as tumor type and thickness.
Systemic spread of basal cell carcinoma is rare, quoted incidences having ranged from 0.0028% to 0.55%. Metastases are more common in men and average age at presentation is younger (45 years) than that of nonmetastatic tumors (61 years). Most tumors have arisen on the scalp, ear, and neck and there may be a past history of antecedent radiotherapy for an unrelated dermatosis or unsuccessful previous radiation treatment for the neoplasm. The majority of tumors are large and often deeply invasive and may show evidence of lymphovascular invasion. The most common sites of metastasis include lymph nodes (65%), lung (34%), bone (18.5%), and skin (18.5%). Other sites of metastasis include the parotid gland, liver, oral cavity, and auditory meatus. Secondary amyloidosis has been reported to occur in the setting of metastatic basal cell carcinoma. The prognosis has been very poor, but targeted therapies that address the driving pathogenic mechanism of basal cell carcinoma are now available.
A basal cell carcinoma consists of a dual population of a fibrous stroma surrounding islands of dependent cells that resemble those of the basal layer of the epidermis and hair follicle. The tumor is believed to be derived from an undifferentiated pluripotent epithelial germ cell. These cells arise from interfollicular basal cells or from germ cells in hair follicles or sebaceous glands and immunohistochemically and ultrastructurally share many features with follicular matrix cells. Because of the stromal dependence and the capacity of basal cell carcinomas for differentiation towards any skin appendage, their pathogenetic mechanism possibly represents flawed rehearsal of embryological differentiation. Animal dermal–epidermal recombination experiments show that dermis from a given site is responsible at a given time-window for the presence or absence of appendage development in heterotopic epidermis. Basal cell carcinomas have developed over the fibrosis of venous stasis, and it seems likely, though unproven, that dermal damage with secondary induction of basaloid epidermal changes is the mechanism of development of many basal cell carcinomas.
Overexposure to UV radiation and the inadequate protection provided by fair skin correlates best, though not completely, with the distribution of up to 80% of tumors on the head and neck. The relationship to sunlight, however, is complex and incompletely understood. Basal cell carcinoma correlates particularly with the degree of freckling and a positive history of severe sunburn in childhood, in addition to excessive recreational exposure in the first two decades of life. This last is particularly evident in children who tend to burn rather than tan. The relationship to cumulative and occupational sun exposure and adult recreational sun exposure is less certain. Red hair is associated with an increased incidence of basal cell carcinoma whereas Southern European ancestry has a protective effect. Similar to squamous cell carcinoma, basal cell carcinoma may also be a complication of psoralen plus UV light of A wavelength (PUVA) therapy.
Skin damage from irradiation, grenz rays, burns, tattoos, and other forms of physical injury has also been incriminated. Basal cell carcinoma is sometimes a complication of chronic arsenic ingestion or exposure to coal tar derivatives. Immunosuppressed patients following organ transplantation, with human immunodeficiency virus (HIV) infection or leukemia/lymphoma have a higher incidence of basal cell carcinoma. Although the tumor has been described as a complication of nevus sebaceous, this is more likely in most instances to represent a trichoblastoma. Rarely, it may develop within a linear epidermal nevus.
Basal cell carcinoma is driven by mutations that activate the hedgehog (HH) pathway, involved in embryonic patterning and development. Genetic studies on patients with the nevoid basal cell carcinoma syndrome (Gorlin-Goltz syndrome) who present with multiple basal cell carcinomas at an early age have identified germline mutations in PTCH1 (9q22.32), PTCH2 (1p34.1), and SUFU (10q24.32), all in the HH pathway as underlying defects. Mutations in PTCH1 or PTCH2 have also been identified in about two-thirds of sporadic basal cell carcinomas with SUFU mutations being more rare (2-5%). Another gene in this pathway, SMO (9q32.1), was mutated in 10% of sporadic cases and can be linked to inherited basal cell carcinoma susceptibility independently of Gorlin-Goltz syndrome. All mutations are inactivating, confirming that each is indeed a tumor suppressor gene. PTCH1 is a transmembrane protein, as is the much less mutated homolog PTCH2 , and serves as a receptor for sonic hedgehog (SHH) ligand. PTCH forms a receptor complex with smoothened (SMO), a seven-span transmembrane protein. Upon ligand binding of SHH, the inhibitory function of PTCH1 upon SMO is released which leads to subsequent activation of the zinc-finger transcription factor GLI1. In the HH pathway, PTCH inhibits SMO which inhibits SUFU which inhibits GLI1. Overall, at least 85% of basal cell carcinomas have a relevant mutation in the an SHH pathway member.
As an indicator of the importance of the HH pathway, GLI1 has been found to be overexpressed in virtually all sporadic basal cell carcinomas examined. Its homolog GLI2 also promotes epidermal proliferation and tumorigenesis. Transgenic mice with loss of one Ptch1 gene develop basal cell carcinomas after UV irradiation. In contrast, epidermal proliferations resembling basal cell carcinoma can be induced by overexpression of Shh or Smo in transgenic mice and overexpression of Gli1 results in several skin tumors including hair follicular tumors as well as basal cell carcinoma.
The sonic hedgehog pathway has been linked to the Wnt signaling cascade. Activation of this pathway leads to nuclear translocation of beta-catenin, which then functions as a transcription factor. Nuclear localization of beta-catenin was observed in over 50% of basal cell carcinomas analyzed. More recent data confirm that Wnt/beta-catenin signaling is induced by constitutively active SHH signaling and that this is a requirement for tumor formation in basal cell carcinoma. Epigenetic gene silencing also helps to coordinate these two pathways in tumor development.
An additional pathway involved in the tumorigenesis of basal cell carcinoma involves mutations in the tumor suppressor gene TP53 . Mutations in TP53 are observed in a multitude of human cancers including squamous cell, basal cell carcinomas, and less frequently in melanoma. In basal cell carcinomas, TP53 mutations have been detected in nearly two-thirds of cases. Signatures of UVB irradiation are common in TP53 , and seen across all subtypes. Patients with basal cell carcinoma appear to have a reduced capacity to repair UV-induced DNA damage. These findings provide further molecular evidence linking development of basal cell carcinoma to UV irradiation. In contrast, the UV signature has been reported in only 40% of PTCH1 mutations in sporadic basal cell carcinoma. This lower incidence of UV signature mutations implies that there are mutagenic events other than solely UV irradiation. Characteristic mutations in the TERT gene promoter conferring increased expression and thus promoting tumorigenesis by preventing the senescence that can be invoked by increased cell proliferation has been described. These mutations are also linked to UV exposure. Recent genomic profiling of a large cohort of almost 300 basal cell carcinomas revealed mutations in the RAS and MYC pathways as well as many other oncogenes and tumor suppressors seen across many other forms of cancer.
Gene expression microarray data demonstrate that basal cell carcinoma shows distinctive gene expression patterns compared to surrounding epidermal basal cell keratinocytes and that histologic variants associated with more aggressive disease (i.e., morpheaform basal cell carcinoma) display a gene expression profile distinctly different from more indolent variants such as nodular and superficial basal cell carcinoma. Recently, use of inhibitors of SMO have been helpful in the rare cases of basal cell carcinoma not amenable to a surgical approach, though developmental resistance remains an issue.
Basal cell carcinomas frequently show an origin from the overlying epidermis ( Fig. 24.54 ). They are composed of small cells with uniform round or oval darkly staining nuclei and minimal cytoplasm ( Fig. 24.55 ). Intercellular bridges are not evident. Mitoses and apoptosis are commonly seen ( Figs 24.56 and 24.57 ).
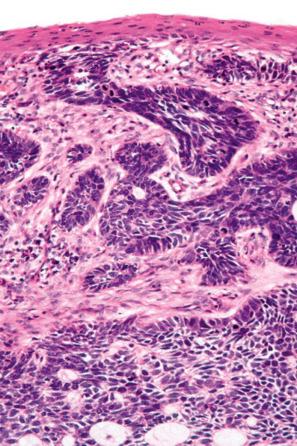
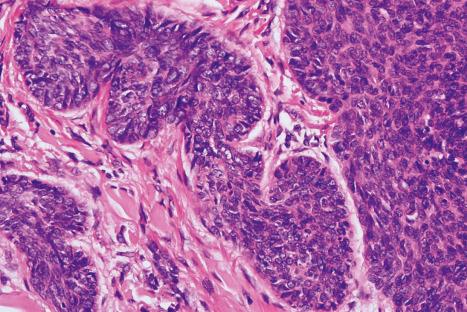
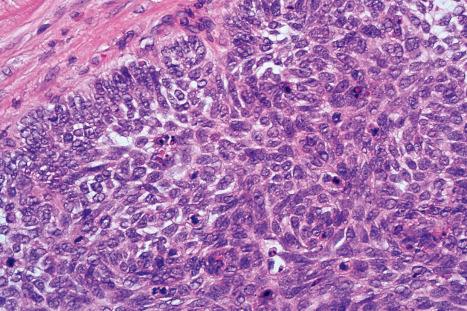
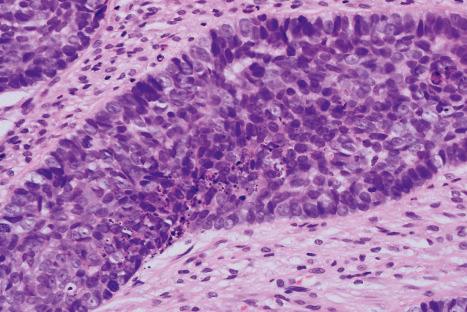
A variety of histologic subtypes are recognized, as follows.
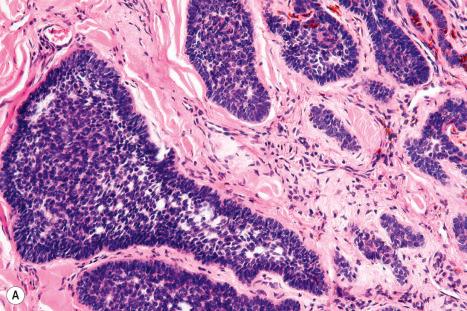
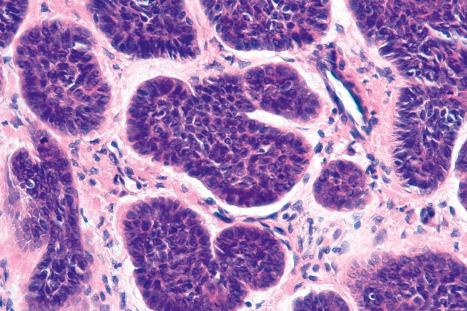
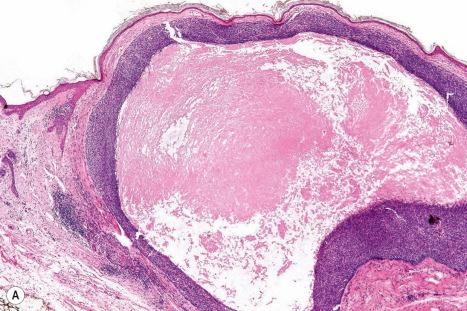
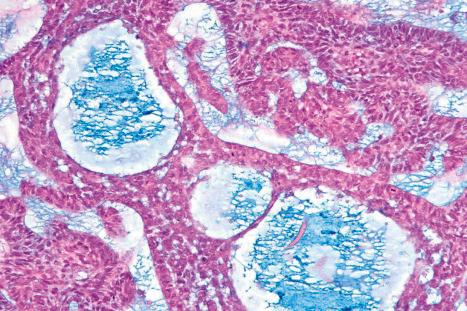
Approximately 75% of all basal cell carcinomas fall into the nodulocystic category in which large basaloid lobules of varying shape and size form a relatively circumscribed mass ( Figs 24.58–24.60 ). A peripheral palisade is typically present around the rim of the lobule, which may be solid or show central cystic dilatation ( Figs 24.61–24.64 ). The stroma surrounding these lobules varies in quality and quantity, but is usually loose and rich in mucin, predominantly hyaluronic acid. Fixation often results in mucin shrinkage; the resultant separation of the tumor lobules from their associated stroma is characteristic of this tumor. Retraction, however, is also related to basement membrane abnormalities of adhesion, including diminished expression of bullous pemphigoid antigen and reduced numbers of hemidesmosomes and anchoring fibrils.
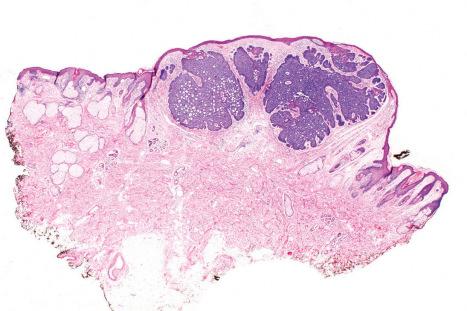
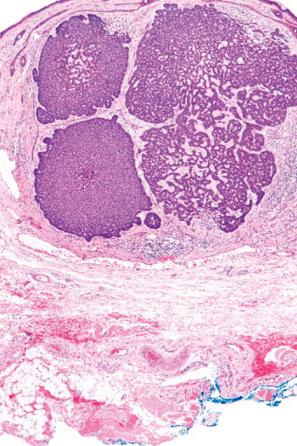
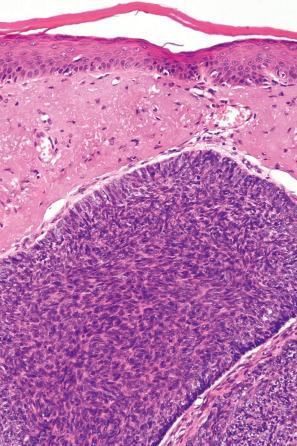
Amyloid may be present in the stroma in from 66% to 75% of basal cell carcinomas, usually at the advancing edge ( Fig. 24.65 ). It may be found in all subtypes and is probably formed from keratin as a consequence of apoptosis. Rarely, metaplastic bone formation is observed.
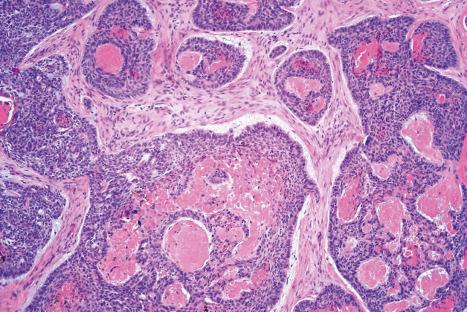
A reticulate pattern of basaloid cells may combine with an almost pure mucinous stroma to form the adenoid variant of basal cell carcinoma, which on occasion mimics glandular formation ( Fig. 24.66 ).
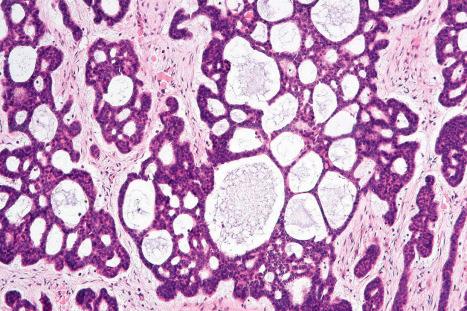
The micronodular variant is characterized by a basaloid cellular proliferation arranged in small nests ( Figs 24.67 and 24.68 ). Peripheral palisading is frequently less prominent than in the nodulocystic type and a retraction artifact is usually absent. This variant may often diffusely infiltrate the dermis and extend into the subcutis. It is therefore associated with a higher local recurrence rate.
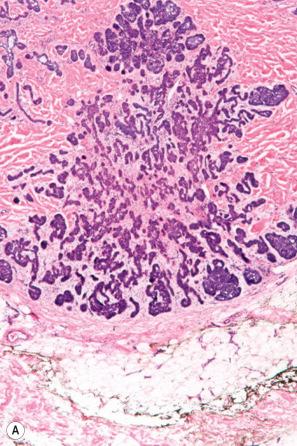
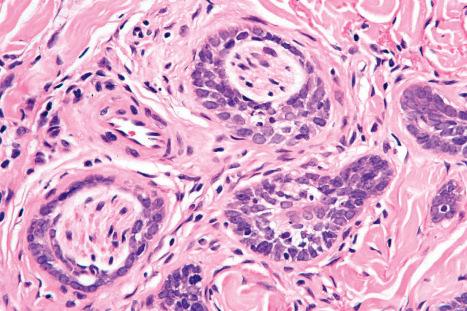
The infiltrative basal cell carcinoma is characterized by small irregular clumps of basaloid cells with a jagged border and limited peripheral palisading ( Fig. 24.69 ). In contrast to the morpheaform variant, the stroma often appears rather loose and mucin may be prominent. The tumor usually shows extensive spread, and involvement of the perineural space is not uncommon. An infiltrative component may also be a feature of noduloulcerative variants.
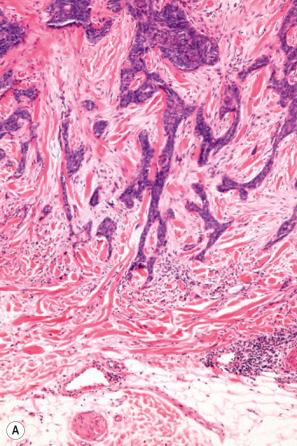
Similar to the infiltrating type, morpheaform basal cell carcinoma is composed of thin strands and nests of basaloid cell showing only limited peripheral palisading. The surrounding stroma is dense and sclerotic, giving rise to the indurated appearance clinically resembling morphea ( Fig. 24.70 ). Extensive spread and perineural infiltration are not infrequent.
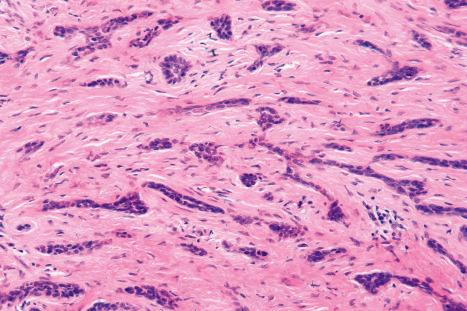
Keratinization is a rare feature of basal cell carcinoma, presenting horn cyst formation ( Fig. 24.71 ). The keratotic variant of basal cell carcinoma may be indistinguishable from a familial trichoepithelioma. Where doubt exists, particularly in the elderly, it is advisable to treat the lesion as basal cell carcinoma.
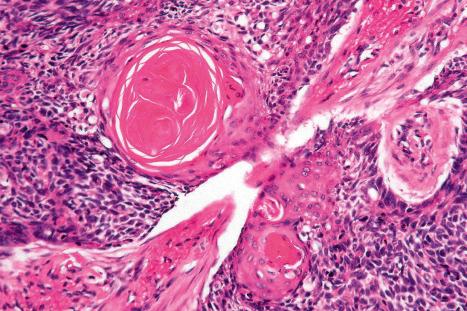
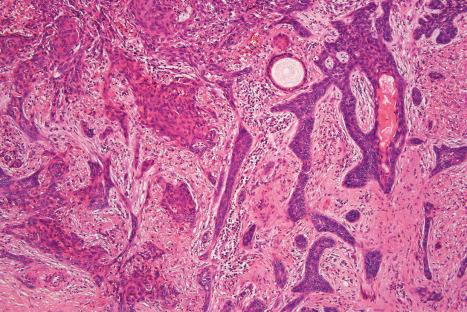
When foci of neoplastic squamous differentiation occur, the tumors are labeled basosquamous or ‘metatypical’ and, because of their usual infiltrative growth pattern, are associated with a poorer outlook including increased risk of distant metastasis ( Fig. 24.72 ).
Become a Clinical Tree membership for Full access and enjoy Unlimited articles
If you are a member. Log in here